Back to Journals » Integrated Pharmacy Research and Practice » Volume 7
Role of pharmacists in providing parenteral nutrition support: current insights and future directions
Authors Katoue MG
Received 7 January 2018
Accepted for publication 5 May 2018
Published 2 October 2018 Volume 2018:7 Pages 125—140
DOI https://doi.org/10.2147/IPRP.S117118
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Jonathan Ling
Video abstract presented by Maram Gamal Katoue
Views: 1438
Maram Gamal Katoue
Department of Pharmacology and Therapeutics, Faculty of Pharmacy, Kuwait University, Kuwait
Background: Parenteral nutrition (PN) therapy is a complex and critical therapy that requires special clinical knowledge, skills, and practice experience to avoid errors in prescribing, compounding, and clinical management of patients. Pharmacists with adequate clinical training and expertise in PN therapy can have pivotal role in the care of patients receiving PN therapy.
Objective: The aim of this systematic review was to describe and evaluate the different roles of pharmacists and their provided services related to PN therapy.
Materials and methods: A comprehensive systematic literature review on the topic was conducted via PubMed database using several keywords related to the topic (from 1975 to 2017). Additional resources included the standards of practice and clinical guidelines from recognized organizations such as the American Society for Parenteral and Enteral Nutrition (ASPEN) and the American Society of Health-System Pharmacists (ASHP).
Results: Pharmacists have diverse roles in relation to PN therapy including the following: the assessment of patients’ nutritional needs; the design, compounding, dispensing, and quality management of PN formulations; monitoring patients’ response to PN therapy; supervision of home parenteral nutrition (HPN) programs; education of patients, caregivers, and other health care professionals on nutrition support and conducting PN-related research and quality improvement activities. These services seem to be variable across clinical settings and among different countries depending on the practice environment and pharmacists’ clinical practice in these settings. However, each of these practice domains helps to support the delivery of safe and effective PN therapy to patients.
Conclusion: Pharmacists have been actively participating in providing PN-related services to patients. To fulfill the requirements of their essential role in this area of practice, pharmacists need adequate educational preparation and clinical training on nutrition support. Empowerment of pharmacists to assume a stronger leadership role in this dimension of pharmacy practice will enhance the quality of care provided to patients receiving PN therapy and improve PN services.
Keywords: nutrition support, nutrition support pharmacist, nutrition support team
Introduction
Parenteral nutrition (PN) therapy involves the intravenous administration of nutritionally sufficient and balanced formulations to supply essential nutrients to patients who are unable to tolerate oral or enteral feeding due to dysfunctional or inaccessible gastrointestinal (GI) tract. Over the years, PN has become an important primary and adjunctive therapy in various clinical conditions and disease states for both the acutely ill hospitalized patients and in the long-term setting for selected patients in the home.1,2 For example, PN formulations can serve as a life-sustaining option for premature infants and critically ill hospitalized patients and for patients who have permanent loss of the GI tract such as those with fistulas or short bowel syndrome.3,4
When all the daily nutritional requirements are exclusively supplied to the patient by PN formulations, the therapy is called total parenteral nutrition (TPN). In terms of their composition, PN formulations can either be of standard composition or tailored to the patient’s individual needs. Although standard PN formulations have been increasingly supplied by industry in some countries,5,6 PN formulations are still compounded in-house by pharmacy staff within the hospital pharmacies to cover patients’ needs in many countries.7
The PN formulations are complex admixtures that consist of multiple components, including both macronutrients (amino acids, dextrose, and intravenous fat emulsions [IVFEs]) and micronutrients (electrolytes, vitamins, and trace elements). In view of the complexity of their composition and direct administration into the blood stream, these formulations must be sterile and contain stable and compatible components to ensure the safety of patients receiving PN therapy.1,8,9 An incompatible, unstable, or contaminated intravenous infusion may result in harm to patients, including serious morbidity and even mortality.10 Therefore, PN formulations must be compounded under strict aseptic techniques according to validated pharmaceutical compounding procedures.1,11,12
Although being lifesaving for many patients, PN therapy is a high-risk feeding modality that can be associated with some complications.4,13,14 In the initial stages of PN therapy, electrolyte imbalance is usually the most common acute PN-related complication.13 In the long-term PN therapy, line complications such as line sepsis and occlusion, pulmonary embolism, and metabolic complications such as glucose intolerance, cholestatic liver disease, and micronutrients deficiencies/toxicity may occur.13 Another potential complication of PN therapy is the refeeding syndrome which results from feeding after a period of prolonged starvation.15 This can result in serious biochemical disturbance including a dramatic fall in phosphate levels with subsequent symptoms and signs of deterioration that may lead to death if not recognized and managed properly.13,15 In addition to these potential complications, supporting patients’ survival through the venous administration of nutrients is an expensive form of nutrition support.4
Pharmacists have unique constellation of competencies, including clinical knowledge and skills which place them in an ideal position to contribute to the delivery of nutrition support therapy to patients. Indeed, the professional roles of pharmacists have been evolving from the traditional compounding and dispensing of medications to the modern delivery of direct patient care within multidisciplinary health care teams. Pharmaceutical care (PC) is a practice philosophy, in which the pharmacist responsibly provides medication therapy to patients to achieve definite outcomes that improve their quality of life.16,17 There is cumulative evidence to support the positive impact of PC on patient care17 and health care costs.18,19
To adequately provide PC services, pharmacists must collaborate with other health care professionals and the patient in the design, implementation, and monitoring of a therapeutic plan to optimize patient’s clinical outcomes.17,19 Therefore, the effective execution of PC practice would require good collaboration between pharmacists and the other members of the health care team to optimize patients’ therapeutic outcomes. Likewise, PN therapy is optimally provided to patients as a multidisciplinary service in which the pharmacist collaborates with other health care professionals to optimize a patient’s nutrition care plan.20,21 Nutrition support team (NST) is an interdisciplinary team often composed of physicians, dieticians, pharmacists, and nurses who have specialty training in nutrition support with the responsibility to manage PN therapy following carefully designed protocols.14,22 Pharmacist provision of patient-oriented PC services to patients receiving PN therapy has been shown to improve the clinical outcomes of patients.23,24 Therefore, PN therapy presents an ideal avenue for the pharmacist to contribute as an active member of a multidisciplinary health care team in the provision of safe and effective nutritional and medical therapy to patients.
Development of nutrition support in clinical pharmacy
Most of the developmental milestones in pharmacy nutrition support were achieved in the USA. In 1968, Dudrick et al25 from the Hospital of University of Pennsylvania managed to nourish beagle puppies into full grown dogs by infusing nutrients through central venous access. Shortly after that, the therapy was initiated in infants with debilitating diseases or GI deformities, and then it was administered to adults. Stanely Serlick was the pioneer in pharmacy nutrition support as he managed to prepare sterile, stable, and compatible mixtures of nutrients that could be infused intravenously.26 By the early 1970s, commercial PN products were available and physicians were using the therapy in managing patients who required PN throughout the USA.27 As a result, there was a growing need to initiate a sophisticated system for ordering, preparing, and administering PN therapy with an increased attention to the development of measures to avoid PN metabolic and catheter-related complications.26 Since that early time, the interdisciplinary NSTs emerged as the preferred mode for the safe delivery of PN therapy and the pharmacists began to develop their knowledge and expertise in nutrition support.26,28 Their roles have been expanding beyond the preparation of the sterile, stable, and compatible PN admixtures to the clinical management of PN patients, as well as to PN-related research activities and safety improvement.26 In 1978, the American Society for Parenteral and Enteral Nutrition (ASPEN), which represents an interdisciplinary society of physicians, nurses, dieticians, pharmacists, and nonclinical researchers, was established with a mission to optimize nutrition support of patients during hospitalization and throughout recovery.26
The following two decades witnessed several advancements in PN therapy, such as the development of home parenteral nutrition (HPN) programs, improved quality of manufacturing macronutrients including amino acids and IVFE, advances in disposable administration devices, and introduction of automated compounding machines which enhanced the safety and precision of PN admixture compounding.2,26 Prior to that landmark achievement, the historical method of compounding these multicomponent admixtures was to manually use gravity-driven transfers for large volume additives, such as amino acids, dextrose, lipids, and sterile water, and to add small volume additives, such as electrolytes, trace minerals, multivitamins, and drugs using syringes.29 The manual method used to be labor intensive and required multiple manipulations of infusion containers, sets, syringes, and needles which can lead to poor accuracy of the compounding process and possible contamination of the final admixture.29 The evolution of automated compounding technology for PN admixture compounding with the aid of fluid pump technology and software that controls the compounder pump has led to potentially improved compounding accuracy and PN safety.26,29 It also reduced the time required to compound PN formulas and simplified the process of tailoring their composition to suit individual patient’s needs.26
In an attempt to achieve the best PN outcomes, there has also been increasing clinical research related to the proper use of PN in different clinical conditions and the management of PN-related complications.26 As the pharmacists’ role in nutrition support evolved, ASPEN published standards for nutrition support pharmacists (NSPs) in 1987.30 These standards were defined by ASPEN as a “benchmark representing a range of performance of competent care that should be provided to assure safe and efficacious nutrition care”.31 A year later, the Board of Pharmaceutical Specialties (BPSs) recognized NSPs as specialists.32 Collaborative efforts by ASPEN, the American Society of Health-System Pharmacists (ASHPs), and other organizations came to fruition with the development of Nutrition Care Standards by the Joint Commission on Accreditation of Health Care Organizations (JCAHO).33 These standards mandated the implementation of interdisciplinary nutrition care process and started to be surveyed in 1995.33 Since PN is considered as a high-alert medication, ASPEN in partnership with ASHP created a task force to develop safe practices for PN which were first published in 1998 and revised in 2004.1,34 These clinical guidelines include consensus recommendations to support safe practices related to PN ordering, labeling, compounding, administration, and quality control.
Roles of NSPs
In many developed countries, especially in North America and Europe, nutrition support pharmacy has been growing as a specialty in clinical pharmacy practice. The NSPs are trained and competent to provide several beneficial services related to PN therapy. Depending on their practice environment, their scope of practice may include, but it is not limited to the following: providing direct patient care to patients; consultations with other health care professionals including those in entrepreneurial/industry; supervision of the compounding and dispensing of PN formulations; education of patients, caregivers, students, postgraduate trainees, colleagues, and the public; and contribution to research activities and quality improvement related to nutrition support.21 Moreover, they can have administrative functions such as the management of nutrition support services in their institutions including development, documentation, implementation, and periodic review of organizational policies, procedures, and protocols related to nutrition support and the selection and review of suitable and cost-effective nutrition support formulary.21
Materials and methods
This systematic review outlines the various services that pharmacists can provide in relation to the delivery of PN therapy. A comprehensive literature review on the topic was conducted using different combinations of keywords including the following: parenteral nutrition, total parenteral nutrition, nutrition support, nutrition support pharmacist, clinical pharmacy practice, clinical pharmacist, pharmacist, intensive care unit (ICU), adults, and neonates. References were resourced in the literature indexed in PubMed database during the period from 1975 to 2017 and were accessed via the Health Sciences Center Library at Kuwait University.
The references used in this review were articles describing pharmacists’ role in PN therapy including clinical studies, review articles, and position statements related to pharmacists’ role in PN from recognized organizations such as ASPEN and ASHP. References were included in the final review only if the article focused on an area of pharmacy practice related to PN therapy, and/or the article reported pharmacists’ involvement in PN therapy and/or an intervention or assessment of PN-related services by pharmacists or comparison between services. Results were mainly full articles published in English. Due to the paucity in the literature describing pharmacists’ role in PN therapy, the abstracts of some studies published in other languages were also evaluated for evidence.
The review process initially identified all article titles and abstracts related to the topic which were reviewed to exclude duplicates and irrelevant articles. The titles and abstracts were then examined to determine the relevant articles that would be suitable for detailed examination. The next review cycle involved evaluating the remaining full articles to identify the content that met the inclusion criteria and exclude irrelevant articles. The articles were excluded from the final review if they were not reporting any intervention or involvement of the pharmacist in PN therapy or the full text could not be obtained. These articles were evaluated for content and subsequently classified according to the type of service provided by pharmacists in relation to PN therapy and the scope of pharmacists’ practice for that service. Figure 1 outlines the flowchart of the study selection process.
  | Figure 1 Flowchart of the study selection process. Abbreviation: PN, parenteral nutrition. |
Results
Pharmacists have diverse roles in relation to PN therapy including the assessment of patients’ nutritional needs; the design, compounding, dispensing, and quality management of PN formulations; developing and implementing of an individualized nutrition care plan and monitoring patients’ response to PN therapy. Other areas of pharmacists’ practice in relation to PN include supervision of HPN programs; education of patients, caregivers, and other health care professionals on nutrition support; and conducting PN-related research and quality improvement activities. Each of these practice domains helps to support the delivery of safe and effective PN therapy to patients. Figure 2 illustrates the different roles of pharmacists in relation to PN therapy. Table 1 summarizes the key findings of the relevant studies that were included in this review.
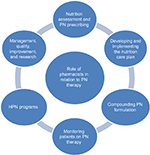  | Figure 2 Pharmacists’ different roles in relation to PN therapy. Abbreviations: HPN, home parenteral nutrition; PN, parenteral nutrition. |
Pharmacists’ role in nutrition assessment and PN prescribing
The PN formulations must meet the nutritional requirements of the patient according to patient age, energy expenditure, and clinical status to ensure that the appropriate nutrients are provided to patient and to avoid under- or overnutrition.1 The ASPEN’s standards of practice for NSPs state that the NSP providing direct patient care should participate in nutrition assessment of patients in collaboration with other health care professionals to identify patients who are at risk for malnutrition.21 The assessment is based on retrieving patient history through patient/caregiver interview, reviewing the patient’s medical record and evaluating nutrition-focused physical and biochemical assessment parameters.21,35 The NSP shall participate in the routine assessment of the patient’s energy, protein, fluid, vitamin, mineral, and electrolyte requirements according to age, clinical conditions, and medical therapy and in the assessment of patients’ candidacy for nutrient support.21,35 The NSP should participate in assessing the educational needs of patients, caregivers, health care professionals, and others regarding nutrition support therapy.21
The literature search revealed variable levels of pharmacists’ involvement in nutrition assessment and PN prescribing processes. However, the leading role of pharmacists in PN prescribing was described as early as the late 1970s.36 Greenlaw36 reported that the physician requested a consultation with the pharmacist to initiate PN therapy in a TPN program applied in a private nonteaching institution. The pharmacist was responsible for conducting the needed physical and nutrition assessment of the patient and writing all the TPN-related orders, with a resulting increase in the utilization of PN therapy and the physicians relying on pharmacists for this service.36
To prepare pharmacists for this role, adequate training was necessary, and a number of studies reported training of pharmacists on PN prescribing. For example, Faber37 described the development and implementation of an education and training program at a community hospital to enable staff pharmacists to become involved in the pharmacy-based TPN service and to write TPN orders and conduct TPN rounds. McDermott et al38 reported that training efforts were made to increase pharmacists’ involvement in nutrition support and physician prescribing at their institution. The increased involvement of pharmacists in the prescribing process resulted in more appropriate PN therapy, earlier shift from PN to enteral nutrition, acknowledging pharmacists as resources for physicians, and improved job satisfaction for pharmacists.38 In another study, Broyles et al39 reported the positive impact of pharmacists’ interventions on improving fluid balance in fluid-restricted ICU patients receiving PN. There is also available evidence to support pharmacists’ participation in nutrition consultations with physicians in different settings.40,41
Ragab et al3 conducted a literature review on pharmacist’s role as a prescriber for PN therapy as related to pharmacy practice. Their review revealed that the practice of pharmacist writing neonatal PN orders already exists, but seems to be limited compared to pharmacists’ role in writing adult PN orders which is more established in many countries.3 Nevertheless, they concluded that there is sufficient evidence to support pharmacists’ competencies in this area of practice.3
As part of the process of revision of ASPEN’s safe practices for PN guidelines, Seres et al42 conducted a web-based survey among ASPEN members to gain insight into PN practices including the processes for writing PN orders. Their findings showed that in general physicians (78%) were responsible for writing PN orders, but the dietitians and pharmacists were heavily involved in the order-writing process either as individuals or as members of a nutrition support service.42 Moreover, pharmacy staff were allowed to adjust certain electrolyte additives such as acetate or chloride in 62% of respondents’ organizations.42 In another web-based survey of PN practices in the USA by Boullata et al,43 28.3% of respondents reported that a pharmacist was prescribing PN at their settings. Similarly, Yang et al44 reported pharmacists’ involvement in confirming and adjusting the daily caloric content in the PN and enteral feeding orders of very low birth weight neonates receiving PN therapy. In another study, the specialty practice pharmacist was responsible for supervising the PN system throughout the entire health care system, while the unit-based pharmacist was responsible for the initiation and daily management of PN together with the primary service physicians.45 Pharmacists delivered nutrition support services have been proven to result in appropriate PN prescribing and a decline in the non-indicated use of PN.38,46
Pharmacists’ role in developing and implementing the nutrition care plan
The ASPEN’s standards of practice for NSPs state that the NSP shall participate in developing a customized nutrition care plan for the patient in collaboration with other health care professionals.21,35 This plan shall be based on the patient’s nutrition assessment, disease states, clinical conditions, and nutritional risk factors and shall include evidence-based literature.21 While developing this plan, the NSP shall review patient medications to determine their impact on the nutrition care plan and nutrient requirements.21 Other responsibilities of the NSP include the documentation of the nutrition care plan in the medical record, recommending the preferred route of administration of nutrition support therapy, recommending a patient-specific feeding formulation, rate of administration, and mode of administration based on the patient’s clinical information.21,35 Moreover, the NSP should recommend suitable medical therapy adjuncts to nutrition support therapy if needed.21 The NSP shall contribute to the implementation of the nutrition care plan to enhance appropriateness, safety, accuracy, resources’ efficiency and the delivery of fiscally responsible care.21,35 The NSP should recommend the necessary equipment and supplies and recommend strategies for the prevention, detection, and management of complications related to the feeding formulation(s) and feeding access device(s). The NSP shall also provide strategies for the prevention, detection, and management of interactions between drugs, dietary supplements and nutrients, and strategies to avoid the incompatibility or instability of the feeding formulations.21,35 The NSP should communicate the individualized nutrition care plan with other health care professionals within and outside the institution to promote continuity of care.21,35 One of the chief responsibilities of NSP is to provide appropriate education for the patients and caregivers regarding the nutrition care plan, for which they should develop written educational materials appropriate for the educational needs of the intended audience.21
As there has been a transition in pharmacy practice toward the provision of direct patient care services, the evidence on pharmacists’ participation in the development and management of nutrition care plans has been emerging in the literature. Gales and Riley47 reported a multidisciplinary consult-based NST including a pharmacist with direct interventions in the nutrition care plan in a large private tertiary care institution. The collaborative care provided by the NST resulted in more adequate nutrition care for patients and less metabolic complications compared to TPN therapy solely guided by a physician.47 Another study showed that pharmacist-led nutrition support service resulted in a decline in the incidence of metabolic and electrolyte abnormalities in the patients receiving PN.46 A clinical pharmacist-based nutrition support service has also been found to improve the nutritional status and clinical outcomes of patients undergoing hematopoietic stem cell transplantation.48 Accordingly, Mirtallo and Sacks49 proposed a paradigm move in pharmacy nutrition support practice to extend pharmacists’ role beyond PN and drug–nutrient interactions to become partners in the interdisciplinary approach to the implementation and monitoring of nutrition care plans.
A number of studies highlighted the specialized expertise of pharmacists in managing the medication-related changes associated with PN therapy. Giancarelli and Davanos documented several pharmacists delivered medication-related interventions in patients receiving PN therapy with a high overall acceptance rate by physicians. Some reports in the literature describe pharmacists’ role in the prevention, identification, and resolution of medication-related problems and PN complications in these patients with improved patient outcomes.23,24,50 These studies collectively provide evidence on the unique qualifications and perspectives of the pharmacists and potential areas in which pharmacists can educate the health care team and ensure proper medication use in this patient population.46,50
Pharmacists’ role in compounding PN formulations
In many developed countries, the safe practices for compounding and labeling PN admixtures have been well established.1,34 This is evident by the development of standards and practice guidelines that adequately govern these processes. The ASPEN’s standards of practice for NSPs state that NSP shall participate in the development, implementation, and adherence to policies and procedures related to the PN order verification process, PN order review process, and compounding safe and effective PN admixtures.21,35 Their duties shall also include participation in developing, implementing, and adhering to procedures for the detection and prevention of compatibility or stability problems associated with PN admixture during the compounding process.21 Obviously, pharmacists possess unique knowledge and skills in compatibility and stability as related to the PN formulations (e.g., calcium phosphate solubility, total nutrient admixture stability, and co-infusion of other medications with PN).51 In addition, NSP shall participate in developing, implementing, and adhering to quality control procedures related to compounding PN admixtures and policies and procedures related to labeling, delivery, and storage of PN admixtures prior to administration.21
The NSP should participate in training other pharmacists who verify and review PN orders and shall be involved in developing a competency-based educational curriculum for compounding PN admixtures and performing PN-related calculations. This includes training and monitoring pharmacy personnel regarding compounding PN admixtures and assessing their ability to perform the necessary calculations.21
The ASHP issued guidelines for the safe use of automated compounding devices for the preparation of PN admixtures and for quality assurance for pharmacy-prepared sterile products.11,29 The guidelines state that pharmacists are specifically trained and legally responsible for performing extemporaneously compounding parenteral formulations, including PN admixtures.29 The ASHP guidelines indicate that PN admixture compounding should be performed under the direct supervision of a pharmacist and in the appropriate environment.11 The guidelines also stress on the need for specific training of pharmacists, as well as other pharmacy personnel in the operation, maintenance, and quality assurance of the automated compounders and on performing periodic competency assessment on these responsibilities.29
Preparation of PN solutions has been reported as only one component of pharmacists’ role on the nutrition team and the pharmacists’ clinical responsibilities in managing and monitoring patients receiving PN have long been well established in developed countries.52 A cross-sectional study describing hospital pharmacists’ PN practices in Switzerland, France, and Belgium demonstrated the unique role of pharmacists in compounding PN formulas in hospital pharmacies as well as their participation in NST services.53 On the other hand, pharmacists’ role in PN therapy in many developing countries seems to be still limited to compounding PN admixtures. For example, Batani et al54 explored TPN practices in Universiti Sains Malaysia Hospital, Malaysia, and reported that pharmacists were merely responsible for compounding PN formulations and for the logistical aspects and integrity of the PN product lines. They identified high response rate of TPN-associated complications, especially in the electrolyte complications with a rate (56.5%) that seems to be higher compared to that reported in developed countries.3 Since pharmacists were only responsible for PN compounding in that study, this highlights the value of pharmacist monitoring of patients’ response to PN therapy to reduce the incidence of the metabolic and electrolyte complications as have been demonstrated in studies conducted in many developed countries.3,46,47 Likewise, Katoue et al7 explored TPN practices at hospital pharmacies in Kuwait. They reported that pharmacists were mainly performing technical roles such as PN order verification, PN compounding, and maintaining PN necessary supplies with limited clinical roles in providing direct patient care services.7,55 The pharmacists attributed their limited involvement in providing PC services to several professional and organizational barriers.55
Pharmacists’ role in monitoring patients on PN therapy
PN is a highly complex, therapeutic intervention, and patients receiving this therapy must be under close monitoring to avoid PN-related complications.13,14 It is important and specific to the role of the pharmacist to monitor the patient’s metabolic profile during PN therapy to early detect any feeding-related complications and prevent them from progressing to clinically significant disorders.2 The ASPEN’s standards of practice for NSPs state that the NSP shall monitor patients receiving nutrition support through reports or patient visits, as appropriate in collaboration with other health care professionals.21,35 The NSP shall determine the appropriate monitoring parameters consistent with the patient’s nutrition care plan to optimize therapy and achieve best outcomes.21 The NSP should routinely reassess the appropriateness of nutrition support therapy (e.g., feeding formulation, route of delivery, and delivery method) and evaluate the efficacy and safety of nutrition support therapy by using relevant monitoring parameters.21,35 Patient monitoring must also include careful review of the patients’ concurrent medications to avoid significant drug-induced metabolic disorders.2 Monitoring the levels of vitamins and trace elements in patients requiring specialized nutrition support is important and represents another area that can highlight the unique skills of pharmacists with additional nutrition support training.13,46
Undoubtedly, patients receiving long-term PN can greatly benefit from the experience and help of NSTs, so that the complications can be detected and managed promptly.13 Dodds et al14 performed retrospective analysis of a previously maintained NST database to identify the frequency of metabolic occurrences in hospitalized patients receiving TPN and managed by an NST. Their data showed that only 13 symptomatic events occurred in 11 patients in 2747 courses of TPN over 7 years (0.47%).14 Early recognition and prompt management of each of these events avoided long-term complications and patients’ death.14 This supports the positive impact of nutrition support service on avoiding serious metabolic complications in hospitalized patients receiving TPN.
Pharmacists’ participation in monitoring patients receiving PN therapy has long been proven to reduce costs and improve patients’ clinical outcomes38,56,57 and to prevent and resolve complications.36 Mutchie et al56 compared the outcomes of patients who received standard TPN solutions without pharmacist monitoring to the outcomes of patients whose TPN therapy was individualized and monitored by a pharmacist. Their findings revealed that pharmacist monitoring of patients receiving PN therapy resulted in improved patients’ clinical responses to TPN and reduced TPN-related costs.56 Similarly, Dice et al57 demonstrated that pharmacist monitoring of an individualized TPN in neonates resulted in a greater amount of nutrients to be provided and mean daily weight gain and was more cost-effective compared to the use of standardized TPN solutions without pharmacist monitoring. A report by Muller et al52 highlights the primary role of the pharmacist in monitoring the laboratory results of cancer patients receiving PN therapy and monitoring the medications that patients receive along with PN therapy. They recommended careful monitoring of the clinical status of these patients since medications and other treatment modalities can markedly influence the nutritional status and electrolyte balance in this patient population.52
Pharmacists’ role in HPN programs
Following the establishment, recognition, and reimbursement of PN therapy for hospitalized patients, consideration for payment for patients receiving therapy at home was sought and financially supported in the USA.26 This lead to the development of HPN programs supported by advancements in home infusion therapy industry.26 This has been found to be a useful alternative to improve nutrition in many patients especially those with short bowel syndrome, promote rehabilitation at home, and decrease long-term expenses compared to in-hospital PN therapy.58,59
To adequately provide HPN to patients and to guarantee the quality of service being provided, ASPEN published standards of practice for home nutrition support and ASHP published guidelines on the pharmacists’ role in home care.60,61 This was followed by home care accreditation program by the JCAHO which was the first to use pharmacists as surveyors, educators, and consultants.26 The JCAHO’s home care standards advocated the clinical management of patients by pharmacists.
Several reports in the literature document pharmacists’ involvement in the care of patients receiving HPN therapy. Gaffron et al58 described the organization and operation of HPN program at their hospital, in which the care was coordinated by a multidisciplinary team with a central role of the pharmacist in delivering this service to patients. Pharmacists were involved in patients’ education, provision of in-service training to nurses and house officers, coordination of patients’ transition to home care, testing and evaluating the equipment, development of a training manual, and editing a quarterly newsletter to patients on HPN.58 Similarly, Lees et al59 described pharmacists’ participation in patients training on HPN as part of a multidisciplinary team. Karnack et al62 conducted a national survey in the USA to investigate pharmacists’ role in HPN programs and documented their involvement in the preparation of PN solutions, patient education, and monitoring patients’ laboratory results in collaboration with physicians. There has also been some published literature describing pharmacists’ fundamental role in the care of patients receiving HPN from several countries including Kuwait, Japan, and Poland.55,63,64
Role of pharmacists as members in NSTs
The leadership role of pharmacists in NSTs is well established.36,46 There is considerable evidence to demonstrate the unique perspectives of pharmacists on NSTs and their valuable contribution to the delivery of effective and safe PN therapy.14,36,46 It has been evident that the care provided to patients by multidisciplinary NSTs involving pharmacists results in fewer metabolic and catheter-related complications compared to the care provided by a single physician.28,47,49 Several studies described pharmacists’ involvement in patient education and training on HPN programs as part of multidisciplinary NSTs with improved quality of care and cost-effectiveness of HPN.58,59,64
Pharmacists’ role in management, quality improvement, and research related to PN
According to the Board Certified Nutrition Support Pharmacist (BCNSP) criteria, management, quality improvement, education, and research related to PN therapy were included responsibilities of pharmacists in addition to the pharmaceutical aspects of PN and clinical management of nutrition support patients.26 The ASPEN’s standards of practice for NSPs state that the NSP should participate in the administrative management of the NST or services in collaboration with other members of the health care team.21 The NSP shall also develop collaborative relationships with health care professionals, students, postgraduate trainees, patients, and caregivers and should provide them with nutrition-related education. The NSP should participate in collaborative nutrition-related research activities and shall apply their findings and the best available evidence into practice.21
There have been some reports in the literature which describe some activities and initiatives by pharmacists to improve their practices and PN services. For example, in one study, the pharmacy services evaluated the quality of PN program applied in one hospital in Spain.65 Harbottle et al66 reported the findings of a clinical audit to evaluate PN use in Guernsey. Boitano et al67 reported a quality improvement collaboration to improve the safety and effectiveness of PN at their hospital which resulted in positive impact on the quality and cost of PN services as a result of implementing a set of process improvement strategies. McDermott et al68 described their experience in initiating a documentation system of clinical interventions in nutrition support with the aim to improve the workflow and quality of PN service. With regard to pharmacists’ role in the management of PN services, Martin69 highlighted the important role for consultant pharmacists in nutrition management in long-term care facilities.
Pharmacist’s specialization in nutrition support and continuing professional development (CPD)
As the pharmacy profession has been developing over the years, specialization was a logical outcome of this development. Specialization allowed those pharmacists with special clinical knowledge and skills to meet more in depth or more specific patient care needs.70 In 1988, the BPS recognized NSPs as specialists, thereby defining the scope of practice and the criteria for clinical competence for a pharmacist practicing in nutrition support.32 This certificate is provided to those pharmacists with adequate clinical experience in this area of practice and following rigorous assessment process to evaluate their clinical competencies in the broad area of nutrition support including PN therapy to become recognized as BCNSPs.71 A number of authors described and evaluated the NSP board certification process.70,72,73
The Certified Nutrition Support Clinician® (CNSC®) credential is another certification available for physicians, dietitians, pharmacists, physician assistants, and nurses who are involved in nutrition support.74 It is offered by the National Board of Nutrition Support Certification (NBNSC) which is an independent credentialing board established by ASPEN in 1984.74
Several professional organizations in the field of clinical nutrition also provide education, training, and CPD programs for pharmacists practicing in nutrition support in an effort to improve their practices. The European Society of Clinical Nutrition and Metabolism (ESPEN) offers a postgraduate qualification in clinical nutrition called the Life Long Learning (LLL) Program in Clinical Nutrition and Metabolism for medical doctors and other health care specialists.75 In this program, participants attend training online and at live courses, using several modern training methodologies and resources to provide them with adequate clinical experience in the field of nutrition support.75 Similarly, ASPEN provides wealth of educational resources and learning opportunities for pharmacists on topics related to clinical nutrition including webinars series, online courses, self-study programs, and conferences.76 In addition, some reports in the literature describe individual institutional efforts to conduct staff development programs for the education and training of pharmacists on PN support.37,38
Discussion
The literature presented in this review provides evidence to support pharmacists’ different roles and provided services in relation to PN therapy. These services include the nutrition assessment of patients and PN prescribing; developing and implementing the nutrition care plans; compounding and quality management of PN formulations and monitoring patients on PN therapy. Other areas of pharmacists’ practice included supervision of HPN programs; participation as members of NSTs; management of PN services and conducting PN-related research and quality improvement activities. Each of these practice domains helps to support the delivery of safe and effective PN therapy to patients. Nevertheless, it seems that the extent of pharmacists’ involvement in providing these services is variable across clinical settings and among different countries depending on the practice environment and pharmacists’ clinical practice in these settings. The clinical roles of pharmacists in providing direct patient care to patients requiring PN therapy are well established and documented in developed countries.23,24,46,47,52 Pharmacists practicing in nutrition support in these countries often collaborate with the other members of NST in the assessment of patient’s nutritional needs, development and implementation of an individualized nutrition care plan for the patient, and monitoring patient’s response to PN therapy. On the other hand, pharmacists’ roles in many developing countries are still limited to performing technical tasks such as the compounding, dispensing, and quality control of PN formulations with limited role in providing direct patient care services.7,54,55
The participation of pharmacists in the provision of TPN services has been described in the literature since the late 1970s and early 1980s.36,52,56,57 As there has been a paradigm shift of pharmacy practice from the provision of product-oriented services to the delivery of direct patient care, pharmacists’ practices related to PN therapy have been undergoing similar change as well. Pharmacists have been expanding their role beyond the preparation of PN admixtures to the clinical management of patients while practicing either as individuals or as part of NST services, therefore, emphasizing the philosophy of PC practice. The pharmacists can have clinical responsibilities which are of paramount importance such as following patient laboratory results and monitoring the impact of adjective medications on the nutrition care plan and nutrient requirements.21,52 Many patients receiving PN therapy are critically ill hospitalized patients, and they would be receiving multiple medications along with PN therapy. Being drug experts, pharmacists can have an essential role in the proper selection and monitoring of these mediations to guarantee optimal usage and avoid any interactions or incompatibility issues between these medications and PN therapy.21,46 Indeed, pharmacists have been shown to contribute effectively to the prevention, detection, and resolution of drug-related problems in patients receiving PN therapy with improved patients’ clinical outcomes.23,24,50 In some vulnerable patient populations such as cancer patients, medications and other treatment modalities (e.g., chemotherapy and radiotherapy) can markedly alter nutritional status and electrolyte balance, which highlights the important function of the pharmacist in following these patients.52 Pharmacist monitoring of neonates receiving PN therapy has also been found valuable for improving their clinical outcomes.57 Overall, the participation of pharmacists in providing direct patient care services to patients receiving PN therapy has been shown to improve patients’ nutritional status and clinical outcomes; to prevent and resolve PN-related complications and to save health care costs.48,56,57
Notably, most of the articles describing pharmacists’ interventions and roles in PN support were retrieved from the USA literature. This highlights a need to conduct more clinical studies evaluating pharmacists’ contributions to this area of practice in other countries, especially in developing countries where pharmacists are striving to establish clinical pharmacy services. The bulk of evidence on the benefits of NSTs on patient care has also been driven mainly from studies conducted in the USA.14,28,46,47 In view of the considerable evidence supporting their positive impact on nutrition support patients,14,28,47 the development of NSTs would be vital to enhance the effectiveness and safety of PN support services. This highlights a need to focus on advocating team approach to the management of patients receiving PN support in other countries and conducting good quality research to evaluate their services in these settings.
Transformation of traditional roles of pharmacists in compounding and dispensing PN admixtures into the clinical management of patients receiving PN therapy obviously offers several advantages but comes with substantial challenges. Pharmacists need adequate education and clinical training on nutrition support to enable them to provide these clinical services to patients. Several credentialing bodies and professional organizations including BPS, ASPEN, and ESPEN provide several certification options and CPD opportunities for pharmacists practicing in nutrition support to guarantee their clinical competence and to demonstrate their accountability for the critical role they play in patient care.
Continual improvement of the standards of practice, development of local PN protocols and practice guidelines to support pharmacists and to serve the local needs in different countries, standardization of PN-related practices and services, and empowerment of pharmacists to assume a stronger leadership role in this dimension of pharmacy practice are among the potential avenues of improvement in this area of clinical pharmacy practice.
Conclusion
Pharmacists have been actively participating in providing PN-related services to patients in different countries. Most of the evidence evaluating pharmacists’ role in PN support has been documented primarily from developed countries, but it is also being investigated in some developing countries. Pharmacists’ provision of clinical services for the management of PN support patients has been associated with adequate nutrition care and medical therapy; improved nutritional status and clinical outcomes of patients; prevention and resolution of PN-associated complications and reduced PN support-related health care costs. More involvement of pharmacists in the provision of direct care services to these patients will result in improved patient outcomes and enhanced quality of PN services. To fulfill the requirements of that role, pharmacists need adequate educational preparation and clinical training on nutrition support. The empowerment of pharmacists to assume a stronger leadership role in this dimension of pharmacy practice will enhance the quality of care provided to patients receiving PN therapy and improve PN services.
Disclosure
The author reports no conflicts of interest in this work.
References
Mirtallo J, Canada T, Johnson D, et al; Task Force for the Revision of Safe Practices for Parenteral Nutrition. Safe practices for parenteral nutrition. JPEN J Parenter Enteral Nutr. 2004;28(6):S39–S70. | ||
Driscoll DF. Hospital pharmacists and total parenteral nutrition: current status and trends. Eur J Hosp Pharm Sci Pract. 2008;14(1):64. | ||
Ragab MH, Al-Hindi MY, Alrayees MM. Neonatal parenteral nutrition: review of the pharmacist role as a prescriber. Saudi Pharm J. 2016;24(4):429–440. | ||
Worthington P, Balint J, Bechtold M, et al. When is parenteral nutrition appropriate? JPEN J Parenter Enteral Nutr. 2017;41(3):324–377. | ||
Kochevar M, Guenter P, Holcombe B, Malone A, Mirtallo J; ASPEN Board of Directors and Task Force on Parenteral Nutrition Standardization. ASPEN statement on parenteral nutrition standardization. JPEN J Parenter Enteral Nutr. 2007;31(5):441–448. | ||
Colomb V. Commercially premixed 3-chamber bags for pediatric parenteral nutrition are available for hospitalized children. J Nutr. 2013;143(12 suppl):2071S–2076S. | ||
Katoue MG, Al-Taweel D, Matar KM, Kombian SB. Parenteral nutrition in hospital pharmacies. Int J Health Care Qual Assur. 2016;29(6):664–674. | ||
Barnett MI, Cosslett AG, Duffield JR, Evans DA, Hall SB, Williams DR. Parenteral nutrition. Pharmaceutical problems of compatibility and stability. Drug Saf. 1990;5(suppl 1):101–106. | ||
Driscoll DF. Stability and compatibility assessment techniques for total parenteral nutrition admixtures: setting the bar according to pharmacopeial standards. Curr Opin Clin Nutr Metab Care. 2005;8(3):297–303. | ||
Lumpkin MM. Safety alert: hazards of precipitation associated with parenteral nutrition. Am J Hosp Pharm. 1994;51(11):1427–1428. | ||
American Society of Health-System Pharmacists. ASHP technical assistance bulletin on quality assurance for pharmacy-prepared sterile products. Am J Hosp Pharm. 1993;50(11):2386–2398. | ||
Ayers P, Adams S, Boullata J, et al; American Society for Parenteral and Enteral Nutrition. A.S.P.E.N. parenteral nutrition safety consensus recommendations. JPEN J Parenter Enteral Nutr. 2014;38(3):296–333. | ||
Meadows N. Monitoring and complications of parenteral nutrition. Nutrition. 1998;14(10):806–808. | ||
Dodds ES, Murray JD, Trexler KM, Grant JP. Metabolic occurrences in total parenteral nutrition patients managed by a nutrition support team. Nutr Clin Pract. 2001;16:78–84. | ||
Walmsley RS. Refeeding syndrome: screening, incidence, and treatment during parenteral nutrition. J Gastroenterol Hepatol. 2013;28(suppl 4):113–117. | ||
Hepler CD. The future of pharmacy: pharmaceutical care. Am Pharm. 1990;NS30(10):23–29. | ||
Hepler CD, Strand LM. Opportunities and responsibilities in pharmaceutical care. Am J Hosp Pharm. 1990;47(3):533–543. | ||
Berenguer B, La Casa C, de la Matta MJ, Martin-Calero MJ. Pharmaceutical care: past, present and future. Curr Pharm Des. 2004;10(31):3931–3946. | ||
American Society of Hospital Pharmacists. ASHP statement on pharmaceutical care. Am J Hosp Pharm. 1993;50:1720–1723. | ||
Howard P. Practical nutritional support: working together to make it happen. Proc Nutr Soc. 2001;60(3):415–418. | ||
Tucker A, Ybarra J, Bingham A, et al; American Society for Parenteral and Enteral Nutrition. American society for parenteral and enteral nutrition (ASPEN) standards of practice for nutrition support pharmacists. Nutr Clin Pract. 2015;30(1):139–146. | ||
DeLegge MH, Kelly AT. State of nutrition support teams. Nutr Clin Pract. 2013;28(6):691–697. | ||
Anoz Jimenez L, Borras Almenar C, Cavera Rodrigo E. Pharmaceutical procedures in patients under treatment with total parenteral nutrition. Farm Hosp. 2004;28(5):349–355. | ||
Sevilla Sanchez D, Placeres Alsina MM, Miana Mena MT, Lopez Sune E, Codina Jane C, Ribas Sala J. Pharmaceutical intervention with parenteral nutrition. Farm Hosp. 2010;34(1):9–15. | ||
Dudrick SJ, Wilmore DW, Vars HM, Rhoads JE. Long-term total parenteral nutrition with growth, development, and positive nitrogen balance. Surgery. 1968;64(1):134–142. | ||
Mirtallo JM. Advancement of nutrition support in clinical pharmacy. Ann Pharmacother. 2007;41(5):869–872. | ||
Flack HL, Gans JA, Serlick SE, Dudrick SJ. The current status of parenteral hyperalimentation. Am J Hosp Pharm. 1971;28(5):326–335. | ||
Nehme AE. Nutritional support of the hospitalized patient. The team concept. JAMA. 1980;243(19):1906–1908. | ||
American Society of Health-System Pharmacists. ASHP guidelines on the safe use of automated compounding devices for the preparation of parenteral nutrition admixtures. Am J Health Syst Pharm. 2000;57(14):1343–1348. | ||
American Society for Parenteral and Enteral Nutrition. Standards for nutrition support pharmacists. Nutr Clin Pract. 1993;8(3):124–127. | ||
Teitelbaum D, Guenter P, Howell WH, Kochevar ME, Roth J, Seidner DL. Definition of terms, style, and conventions used in A.S.P.E.N. guidelines and standards. Nutr Clin Pract. 2005;20(2):281–285. | ||
Holcombe BJ, Thorn DB, Strausburg KM, et al. Analysis of the practice of nutrition support pharmacy specialists. Pharmacotherapy. 1995;15(6):806–813. | ||
Dougherty D, Bankhead R, Kushner R, Mirtallo J, Winkler M. Nutrition care given new importance in JCAHO standards. Nutr Clin Pract. 1995;10(1):26–31. | ||
National Advisory Group on Standards and Practice Guidelines for Parenteral Nutrition. Safe practices for parenteral nutrition formulations. JPEN J Parenter Enteral Nutr. 1998;22(2):49–66. | ||
Rollins C, Durfee SM, Holcombe BJ, et al. Standards of practice for nutrition support pharmacists. Nutr Clin Pract. 2008;23(2):189–194. | ||
Greenlaw CW. Pharmacist as team leader for total parenteral nutrition therapy. Am J Hosp Pharm. 1979;36(5):648–650. | ||
Faber EM. Program for training staff pharmacists in total parenteral nutrition. Am J Hosp Pharm. 1991;48(5):980–986. | ||
McDermott LA, Albrecht JT, Good DH. Nutritional support: pharmacists’ influence on the prescribing process. Top Hosp Pharm Manage. 1994;14(3):30–39. | ||
Broyles JE, Brown RO, Vehe KL, Nolly RJ, Luther RW. Pharmacist interventions improve fluid balance in fluid-restricted patients requiring parenteral nutrition. DICP. 1991;25(2):119–122. | ||
Maclaren R, Devlin JW, Martin SJ, Dasta JF, Rudis MI, Bond CA. Critical care pharmacy services in United States hospitals. Ann Pharmacother. 2006;40(4):612–618. | ||
Pedersen CA, Schneider PJ, Scheckelhoff DJ. ASHP national survey of pharmacy practice in hospital settings: prescribing and transcribing--2010. Am J Health Syst Pharm. 2011;68(8):669–688. | ||
Seres D, Sacks GS, Pedersen CA, et al. Parenteral nutrition safe practices: results of the 2003 American Society for Parenteral and Enteral Nutrition survey. JPEN J Parenter Enteral Nutr. 2006;30(3):259–265. | ||
Boullata JI, Guenter P, Mirtallo JM. A parenteral nutrition use survey with gap analysis. JPEN J Parenter Enteral Nutr. 2013;37(2):212–222. | ||
Yang S, Lee BS, Park HW, et al. Effect of high vs standard early parenteral amino acid supplementation on the growth outcomes in very low birth weight infants. JPEN J Parenter Enteral Nutr. 2013;37(3):327–334. | ||
Mirtallo JM, Hawksworth K, Payne B. A nutrition support service web application to manage patients receiving parenteral nutrition. Nutr Clin Pract. 2009;24(4):447–458. | ||
Giancarelli A, Davanos E. Evaluation of nutrition support pharmacist interventions. JPEN J Parenter Enteral Nutr. 2015;39(4):476–481. | ||
Gales BJ, Riley DG. Improved total parenteral nutrition therapy management by a nutritional support team. Hosp Pharm. 1994;29(5):469–470,473–475. | ||
Mousavi M, Hayatshahi A, Sarayani A, et al. Impact of clinical pharmacist-based parenteral nutrition service for bone marrow transplantation patients: a randomized clinical trial. Support Care Cancer. 2013;21(12):3441–3448. | ||
Mirtallo JM, Sacks GS. A “call to action” for an expanded pharmacist role in influencing the quality of nutrition care. JPEN J Parenter Enteral Nutr. 2013;37(4):446–447. | ||
Cerulli J, Malone M. Assessment of drug-related problems in clinical nutrition patients. JPEN J Parenter Enteral Nutr. 1999;23(4):218–221. | ||
Rollins CJ. Pharmacist interventions: unique perspective versus taking the lead in nutrition support when knowledge and skills overlap with other healthcare disciplines. JPEN J Parenter Enteral Nutr. 2015;39(4):381–382. | ||
Muller RJ, Hoffman DM, Mulligan RM. Parenteral nutrition program in a major cancer center. Hosp Pharm. 1981;16(2):54–66. | ||
Maisonneuve N, Raguso CA, Paoloni-Giacobino A, et al. Parenteral nutrition practices in hospital pharmacies in Switzerland, France, and Belgium. Nutrition. 2004;20(6):528–535. | ||
Batani RA, Abdullah DC, Bahari MB. Evaluation of the total parenteral nutrition service at Universiti Sains Malaysia Hospital. E Spen Eur E J Clin Nutr Metab. 2007;2(6):e111–e115. | ||
Katoue MG, Al-Taweel D. Role of the pharmacist in parenteral nutrition therapy: challenges and opportunities to implement pharmaceutical care in Kuwait. Pharm Pract (Granada). 2016;14(2):680. | ||
Mutchie KD, Smith KA, MacKay MW, Marsh C, Juluson D. Pharmacist monitoring of parenteral nutrition: clinical and cost effectiveness. Am J Hosp Pharm. 1979;36(6):785–787. | ||
Dice JE, Burckart GJ, Woo JT, Helms RA. Standardized versus pharmacist-monitored individualized parenteral nutrition in low-birth-weight infants. Am J Hosp Pharm. 1981;38(10):1487–1489. | ||
Gaffron RE, Fleming CR, Berkner S, McCallum D, Schwartau N, McGill DB. Organization and operation of a home parenteral nutrition program with emphasis on the pharmacist’s role. Mayo Clin Proc. 1980;55(2):94–98. | ||
Lees CD, Steiger E, Hooley RA, et al. Home parenteral nutrition. Surg Clin North Am. 1981;61(3):621–633. | ||
Durfee SM, Adams SC, Arthur E, et al. A.S.P.E.N. Standards for nutrition support: home and alternate site care. Nutr Clin Pract. 2014;29(4):542–555. | ||
American Society of Health-System Pharmacists. ASHP guidelines on the pharmacist’s role in home care. Am J Health Syst Pharm. 2000;57(13):1252–1257. | ||
Karnack CM, Gallina JN, Jeffrey LP. Pharmacist involvement in home parenteral nutrition programs. Am J Hosp Pharm. 1981;38(2):215–217. | ||
Tomita I, Ishii S, Yonezawa M, Ito T, Hirai A, Mizuno K. Role of national insurance pharmacies in community complete home care networks--home TPN and home care supported by local national insurance pharmacies. Gan To Kagaku Ryoho. 2000;27(suppl 3):S683–S686. | ||
Pietka M, Watrobska-Swietlikowska D, Szczepanek K, Szybinski P, Sznitowska M, Klek S. Nutritional support teams: the cooperation among physicians and pharmacists helps improve cost-effectiveness of home parenteral nutrition (HPN). Nutr Hosp. 2014;31(1):251–259. | ||
Hernandez de la Figuera y Gomez T, Jimenez Torres NV, Ronchera Oms CL, Ordovas Baines JP. The participation of pharmacy services in evaluating parenteral nutrition programs. Nutr Hosp. 1989;4(3):149–153. | ||
Harbottle L, Brache E, Clarke J. Audit of parenteral nutrition use in Guernsey. Int J Pharm Pract. 2009;17(5):293–298. | ||
Boitano M, Bojak S, McCloskey S, McCaul DS, McDonough M. Improving the safety and effectiveness of parenteral nutrition: results of a quality improvement collaboration. Nutr Clin Pract. 2010;25(6):663–671. | ||
McDermott LA, Albrecht JT, Good DH, Stanford GG. Documentation of clinical interventions in nutritional support. Top Hosp Pharm Manage. 1993;13(2):32–45. | ||
Martin CM. The consultant pharmacist’s expanded role in nutrition management. Consult Pharm. 2009;24(6):414–421. | ||
Strausburg KM. Nutrition support pharmacist board certification process. Hosp Pharm. 1995;30(3):192–196,199–200,207. | ||
Board of Pharmacy Specilities [webpage on the Internet]. Nutrition Support Pharmacy. Available from: https://www.bpsweb.org/bps-specialties/nutrition-support-pharmacy/#1517761118361-6c02bae3-f5a015177800157771517854077689. Accessed April 27, 2018. | ||
Ebiasah RP, Schneider PJ, Pedersen CA, Mirtallo JM. Evaluation of board certification in nutrition support pharmacy. JPEN J Parenter Enteral Nutr. 2002;26(4):239–247. | ||
Durfee SM. Pharmacist specialty certification. JPEN J Parenter Enteral Nutr. 2012;36(2 suppl):51S–52S. | ||
The National Board of Nutrition Support Certification (NBNSC) [webpage on the Internet]. National Board of Nutrition Support Certification:multiple disciplines; a single standard of excellence. Available from: http://www.nutritioncare.org/NBNSC/Certification/Certification_Main_Page/. Accessed April 25, 2018. | ||
The European Society of Clinical Nutrition and Metabolism [webpage on the Internet]. The Life Long Learning (LLL) Programme in Clinical Nutrition and Metabolism. Available from: http://www.espen.org/education/lll-programme. Accessed December 15, 2017. | ||
American Society for Parenteral and Enteral Nutrition (ASPEN) [webpage on the Internet]. Continuing Education With ASPEN. Available from: https://www.nutritioncare.org/continuing-education/. Accessed March 20, 2018. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

