Back to Journals » Clinical Epidemiology » Volume 13
Risk Scoring Systems Including Electrolyte Disorders for Predicting the Incidence of Acute Kidney Injury in Hospitalized Patients
Authors Chen X, Xu J, Li Y, Xu X, Shen B, Zou Z, Ding X, Teng J, Jiang W
Received 17 March 2021
Accepted for publication 21 April 2021
Published 27 May 2021 Volume 2021:13 Pages 383—396
DOI https://doi.org/10.2147/CLEP.S311364
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Vera Ehrenstein
Xin Chen,1,* Jiarui Xu,1,* Yang Li,1 Xialian Xu,1 Bo Shen,1 Zhouping Zou,1 Xiaoqiang Ding,1,2 Jie Teng,1,2 Wuhua Jiang1
1Department of Nephrology, Zhongshan Hospital, Fudan University; Shanghai Institute of Kidney Disease and Dialysis (SIKD), Shanghai Laboratory of Kidney Disease and Dialysis, Shanghai Medical Center of Kidney Disease, Shanghai, People’s Republic of China; 2Department of Nephrology, Xiamen Branch, Zhongshan Hospital, Fudan University, Xiamen, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Xiaoqiang Ding; Wuhua Jiang
Department of Nephrology, Zhongshan Hospital, Fudan University ; No.108, Fenglin Road, Xuhui District, Shanghai, People’s Republic of China
Tel +86-21-64041990
Email [email protected] x
Introduction: Electrolyte disorders are common among hospitalized patients with acute kidney injury (AKI) and adversely affect the outcome. This study aimed to explore the potential role of abnormal electrolyte levels on predicting AKI and severe AKI.
Methods: In this retrospective, observational study, we included all hospitalized patients in our hospital in China from October 01, 2014, to September 30, 2015. Since only a few patients had arterial blood gas analysis (ABG), all subjects involved were divided into two groups: patients with ABG and patients without ABG. Severe AKI was defined as AKI stage 2 or 3 according to KDIGO guideline.
Results: A total of 80,091 patients were enrolled retrospectively and distributed randomly into the test cohort and the validation cohort (2:1). Logistic regression was performed in the test cohort to analyze risk factors including electrolyte disorders and elucidate the association. The test data (derivation cohort) led to AUC values of 0.758 (95% CI: 0.743– 0.773; AKI with ABG), 0.751 (95% CI: 0.740– 0.763; AKI without ABG), 0.733 (95% CI: 0.700– 0.767; severe AKI with ABG), 0.853 (95% CI: 0.824– 0.882; severe AKI without ABG). Application of the scoring system in the validation cohort led to AUC values of 0.724 (95% CI: 0.703– 0.744; AKI with ABG), 0.738 (95% CI: 0.721– 0.755; AKI without ABG), 0.774 (95% CI: 0.732– 0.815; severe AKI with ABG), 0.794 (95% CI: 0.760– 0.827; severe AKI without ABG). Hosmer–Lemeshow tests revealed a good calibration.
Conclusion: The risk scoring systems involving electrolyte disorders were established and validated adequately efficient to predict AKI and severe AKI in hospitalized patients. Electrolyte imbalance needs to be carefully monitored and corrections should be made on time to avoid further adverse outcome.
Keywords: acute kidney injury, electrolyte disorders, risk score
Introduction
Acute kidney injury (AKI) is prevalent in hospitalized patients, particularly in the intensive care unit. The incidence of AKI varies widely according to different diagnostic criteria and study populations. Recent meta-analysis, adopting KDIGO definition, reported that the incidence rates of AKI was 21.6% and the AKI-associated mortality rate was 23.9% in adults.1 While in China, the incidence and mortality rate of AKI were 3.19% and 19.68%, respectively.2 Early identification of patients with high risk of developing AKI is helpful for prevention.
Most of the AKI scoring system focused on specific patients, including patients undergoing cardiac surgery, contrast medium exposure, major surgery and critically ill patients.3–8 To date, there were limited reliable studies that focused on scoring system for a wider range of inpatients. Actually, the occurrence of AKI in hospitalized patients is notable and AKI leads to prolonged hospital stay and increased financial burden.9 Therefore, it is of great clinical significance to analyze the risk factors of hospitalized patients and establish a predictive scoring system for early identification of AKI and avoidance of aggravating impaired renal function.
Renal function is critical to maintain internal electrolyte balance. Severe electrolyte and acid-based disorders are considered as important indicators for renal replacement treatment and cause of death. One national report in the UK stated that one-fifth of the in-hospital AKI could be avoidable, if only they received better monitoring of electrolytes, recognition of risk factors, and prompt management.10 Previous studies have revealed the relationship between AKI and specific electrolyte disorders, including hypernatremia, hyperchloremia and hypomagnesemia.11–14 The sample size in previous studies was relatively small. Compared with other risk factors such as age and comorbidities, which are irreversible, electrolyte disorders deserve more attention. However, as far as we know, few risk models contained acid-base or electrolyte disorders to predict AKI. The research in predicting AKI among ICU patients concluded that PH<7.30 was an important indicator.8 Electrolyte and acid-base disorders were included in risk scoring system to predict mortality rates.15 Therefore, we might be one of the innovative articles to include electrolytes in predicting AKI and severe AKI. Therefore, it might be of clinical significance to include unprecedented electrolyte disorders in the predicting system. This study set out to 1) investigate the relationship between electrolyte disorders and AKI; 2) develop a predictive scoring system for the onset of AKI.
Materials and Methods
Design Overview
Patients included in the study were divided into test and validation cohorts randomly. In the test cohort, risk factors for AKI including electrolyte disorders were investigated. After that, the novel and dynamic risk scores for the assessment of AKI and severe AKI were developed. Then, we evaluated the predicting efficiency of the risk scores in validation cohort. The study aimed to identify AKI and severe AKI in their early stages and guide the clinical practice on reversible risk factors including the correction of disordered electrolyte.
Study Population
In this retrospective, observational study, we included all subjects admitted to Zhongshan Hospital, Shanghai Medical college, Fudan University from October 01, 2014 to September 30, 2015. Patients younger than 18 years and those without any data on electrolytes and serum creatine level were excluded. This study was approved by the Ethical Committee of Zhongshan Hospital, Fudan University (B2018-175) and written informed consents from all participants were provided. The study was conducted in accordance with the Declaration of Helsinki.
We investigated the potential risk factors indicated by baseline analysis for further observation and evaluated them to predict AKI and severe AKI in the test cohort. PH was highly valued in the previous studies8,16 and considered as a potential risk factor to predict AKI and severe AKI in our study. However, PH is available only in patients who underwent arterial blood gas analysis (ABG), so we divided the patients into two groups: patients with ABG and patients without ABG.
Data Collection
Data were collected from an electronic medical records database and blood tests were taken on the admission day. All data were checked twice by medical personnel (postgraduate and resident doctor) before being admitted to the database. We collected data of hospitalized patients including sex, age, weight and height; comorbidities including hypertension, diabetes mellitus, chronic kidney disease (CKD), coronary heart disease (CHD), heart failure, stroke and cancer; laboratory reports within the first 24 hours of the hospitalization including routine blood and urinary tests, renal and liver function, electrolytes and glucose levels. AKI and severe AKI were served as the main endpoints. Patients who already had AKI at the time of admission were excluded. The short-term outcomes included renal replacement therapy (RRT), in-hospital mortality, length of stay and hospital expenses.
Definitions
Electrolyte magnitude were measured in the clinical laboratory department of the hospital using standard methods on an automatic biochemical analyzer (Hitachi 7600, Japan). In this hospital setting, the standardized normal ranges for serum sodium (Na), potassium (K), chlorine (Cl), calcium (Ca), phosphorus (P), and magnesium (Mg) levels were 135–145 mmol/L, 3.5–5.5 mmol/L, 98–110 mmol/L, 2.15–2.55 mmol/L, 0.8–1.45 mmol/L, and 0.67–1.04mmol/L, respectively. Values beyond these normal ranges were considered indicative of electrolyte disorders. The sodium level was adjusted using the formula: Adjusted total serum sodium level (mmol/L) = measured total sodium level (mmol/L) + (glucose (mmol/L)–5.6)÷5.6×2.4. The calcium level was adjusted using the formula: Adjusted total serum calcium level (mmol/L) = measured total calcium level (mmol/L) + 0.02*(40-albumin concentration (g/L)). Anion gap (AG) was calculated by the standard formula: AG=[Na+]-[Cl-]-[HCO3-], with an elevated AG defined as greater than or equal to 16 mmol/L.17
AKI was defined according to the KDIGO guideline18 as any of the following: an increase in SCr ≥0.3 mg/dL (≥26.5 μmol/L) within 48 hours; or an increase in SCr to ≥1.5 times the baseline that is known or presumed to have occurred within the prior 7 days. For the purpose of the research, all the patients involved in the study have tested twice for the serum creatinine level. If patients presented with increased SCr at admission but decreased SCr during hospitalization and the injury occurred before admission, we considered the highest value as the maximum value and the lowest value from the second to the nth as the baseline. If patients presented with elevated creatinine and did not recover, we would retrieve their outpatient records and record baseline SCr. For patients who tested SCr more than twice, we considered the nadir of the first three as baseline and the maximum of the second through nth as peak.2 Patients with no further monitoring or change in SCr was regarded as non-AKI. Patients with AKI at baseline were defined as the increase in creatinine level or decrease in urine output before the hospital admission or within 48 hours of admission and those with AKI during the hospitalization were not included. Classification of AKI was performed according to KDIGO guideline18 (stage 1, 2 and 3) without including urinary output criteria. Severe AKI was considered as AKI stage 2 or 3, which referred to an increase in SCr of 2.0 and 2.9-fold of baseline or 3.0-fold of baseline or increased SCr level to 353.6 μmol/L or initiation of renal replacement therapy. Serum creatinine was used as an indicator of the glomerular filtration rate. Renal function was regarded as normal with SCr less than 1.4 mg/dl (<124 μmol/L), moderately impaired with SCr from 1.4 to 2.5 mg/dl (124–220 μmol/L) and severely impaired with SCr more than 2.5 mg/dl (>220 μmo/L) or more.19,20 The level of eGFR was calculated by using the chronic kidney disease epidemiology collaboration (CKD-EPI) creatinine equation.21 When eGFR is greater than 90 mL/min/1.73m2, it is defined as normal renal function. When eGFR is between 60 and 89 mL/min/1.73m2, it is defined as renal function is slightly impaired. When eGFR is between 30 and 59 mL/min/1.73, it is defined as moderately impaired renal function. When eGFR is less than 29 mL/min/1.73m2, it is defined as severely impaired renal function. The definition of CKD following KDIGO guidelines was based on declined eGFR and laboratory abnormalities of more than three months.22 Hyperuricemia is defined as uric acid level of more than 420 µmol/L (7 mg/dL).
Statistical Analyses
Statistical analyses were carried out by SPSS statistics for Windows (Version 20.0. IBM Corp, Armonk, NY). Continuous variables were expressed as mean±SD and analyzed by unpaired t tests, with Welch adjustment when necessary. Continuous variables that violated the normality assumption were expressed as median and 25th to 75th percentiles and analyzed by a Mann–Whitney U-test. Categorical variables were expressed as absolute (n) and relative (%) frequency and were analyzed by the Pearson 2-test or the Fisher exact test whenever appropriate. Missing data were noted in <8% of records. The missing values of variables were replaced using multiple imputations.23 Compared with P value, the confidence interval (CI) better describes effect size and precision.24 Therefore, CI was described instead of P value. Univariate analysis was carried out for patient data, and multivariate analysis by logistic regression was used to find out the risk factors. In the multivariate analysis, the results were expressed by the odds ratio and the 95% CI. The regression β of those variables obtained from logistic regression were used to develop scoring system to predict AKI and severe AKI. The area under the receiver operating characteristic curves (AUROC) as well as Hosmer-Lemeshow goodness-of-fit test were applied to estimate the reliability of the scoring system.
Results
A total of 80,091 eligible patients were enrolled in this study. The flow chart of this study was presented in Figure 1. The test cohort consisted of 53,394 patients, and 26,697 patients were enrolled in the validation cohort. The characteristics of both cohorts are shown in Table 1. The incidences of in-hospital AKI, severe AKI and mortality in the test cohort were 7.7% (n=4108), 1.7% (n=918) and 1.1% (n=594), whereas in the validation cohort they were 7.5% (n=1994) and 1.7% (n=465) and 0.9% (n=230). There was no statistical difference of AKI stage and mortality rate between two groups.
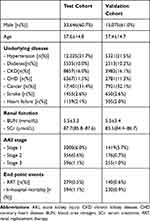 |
Table 1 Clinical Characteristics of Test and Validation Cohort |
 |
Figure 1 Flow chart. Abbreviations: *AKI, acute kidney injury; ABG, arterial blood gas analysis; Na, sodium; K, potassium; Cl, chlorine. |
Baseline Characteristics and Electrolyte Disorders
The characteristics of the test cohort are presented in Table 2. AKI group contained more male and elder people and obtained higher proportion of underlying diseases, such as hypertension, diabetes, CKD, CHD, cancer, stroke and heart failure. Patients in AKI group had a higher level of white blood cell (WBC), blood urea nitrogen (BUN), serum creatinine (SCr), uric acid (UA) and higher proportion of anemia and hypoproteinemia. Each patient involved has tested major electrolytes, such as Na, K, Cl and about 68.8% patients tested for electrolytes like Ca, Mg, P. Only 14.5% patients took ABG test. AKI group had a greater proportion of electrolyte disturbance in either increased or decreased levels of Na, K, Cl, Ca, Mg, P, Carbon dioxide binding capacity (CO2CP), AG, PH and HCO3− compared with non-AKI group (Table 2).
 |
Table 2 Clinical Characteristics of the Patients in Test Cohort |
Logistic Regression Analysis for the Risk Factors of AKI and Severe AKI
The risk factors in predicting AKI in patients with ABG included admission in cardiac surgery or ICU, underlying disease such as heart failure, elevated Aspartate aminotransferase (AST) level, hypoalbuminemia, renal dysfunction measured by increased BUN and UA levels and reduced eGFR level and electrolyte and acid-base disorders measured by decreased Mg, PH and HCO3− levels (Table 3). In patients without ABG, underlying disease as heart failure, elevated AST and Scr, anemia, hypoalbuminemia, hyperuricemia, hyponatremia, hypokalemia, hypocalcemia, hyperphosphatemia, hyperchloremia and reduced CO2CP were concluded as risk factors (Table 4).
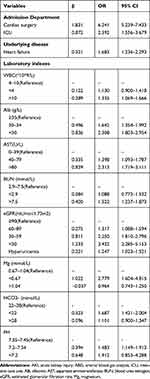 |
Table 3 Multivariate Logistic Regression Analysis of Risk Factors for AKI Among Patients with ABG |
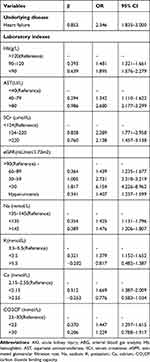 |
Table 4 Multivariate Logistic Regression Analysis of Risk Factors for AKI Among Patients without ABG |
The risk factors in predicting severe AKI in patients with ABG included admission in cardiac surgery, underlying disease such as CKD, potential inflammation or malnutrition presented as elevated WBC level and hypoalbuminemia, renal dysfunction tested by increased SCr level and electrolyte disorders such as hyponatremia and hyperphosphatemia (Table 5). In patients without ABG, elevated WBC, BUN and SCr, hyponatremia, hyperphosphatemia and hypermagnesemia were considered as risk factors (Table 6).
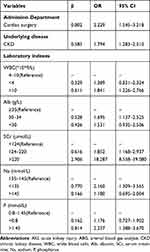 |
Table 5 Logistic Multivariate Regression Analysis Containing Risk Factors for Severe AKI in AKI Patients with ABG |
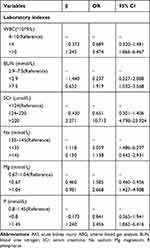 |
Table 6 Logistic Multivariate Regression Analysis Containing Risk Factors for Severe AKI in AKI Patients without ABG |
Score Development
Next, we developed risk scoring systems for predicting AKI (Table 7) and severe AKI (Table 8) occurrence with the regression coefficient data from the multivariable regression analyses of the test cohort patients. For predicting the occurrence of AKI, two sets of scoring systems were established according to whether ABG was performed. The AUC for predicting AKI was 0.758 with ABG (95% CI: 0.743–0.773) and 0.751 without ABG (95% CI: 0.740–0.763), as shown in Figure 2. The calibrations resulted from Hosmer-Lemeshow statistics were good with the P values of 0.821 and 0.365. Another two sets of scoring systems were established to predict severe AKI and the risk factors were similar. AUC for predicting severe AKI was 0.733 with ABG (95% CI: 0.700–0.767) and 0.853 without ABG (95% CI: 0.824–0.882) (Figure 2). The calibrations were good with P values of 0.663 and 0.333.
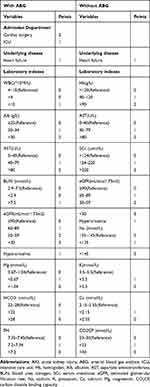 |
Table 7 Factor Scoring for Predicting of AKI Incidence |
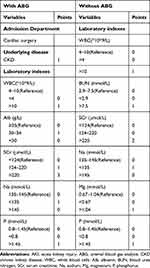 |
Table 8 Factor Scoring for Predicting of Severe AKI Incidence |
Score Validation
The clinical characteristics of the 26,697 patients in the validation cohort are shown in Table 1. The AUC for predicting AKI was 0.724 with ABG (95% CI: 0.703–0.744) and 0.738 without ABG (95% CI: 0.721–0.755). AUC for predicting severe AKI was 0.774 with ABG (95% CI: 0.732–0.815) and 0.794 without ABG (95% CI: 0.760–0.827) (Figure 2).
For clinical practice, the risk scoring system was categorized into low, moderate and high risk of AKI. LR+ (likelihood ratio of positive) was applied to estimate the issue. LR+ greater than 10 means that a positive test is good at ruling in a diagnosis.25 The predictive risks of AKI occurrence in patients with ABG were low with 0 to 1 point (pt) (10.0%), medium with 2 to 7 pts (27.7%) and high with more than 8 pts (74.5%) with LR+ 10.46. That is to say, in patients who scored higher than 8 points, the incidence of AKI was 74.5%. In patients without ABG, the predictive risks of AKI occurrence were low with 0 to 1 pt (2.1%), medium with 2 to 8 pts (6.9%) and high with more than 9 pts (50.0%) with LR+ 18.87. (Table 7). The predicting risks of severe AKI occurrence in patients with ABG were low with 0 to 1 pts (10.7%), medium with 2 to 3 pts (29.1%) and high with more than 4 pts (69.3%) with LR+ 9.87. In patients without ABG, the predictive risks were low with 0 to 1 pts (12.8%), medium with 2 pts (26.7%) and high with more than 3 pts (74.2%) with LR+ 18.45.
There was no statistically significant difference between either AKI or severe AKI frequency in test and validation cohorts as is shown in Figure 3.
Discussion
In the present study, we enrolled a total of 80,091 patients, including 53,394 patients in the test cohort and 26,697 in the validation cohort, in a large, tertiary hospital in East China. The study has found that the relationship between electrolyte disturbance and AKI was of statistical importance. Based on that, point-scoring systems were established to predict AKI and severe AKI in hospitalized patients. In the validation cohorts, AUC values of scoring systems were 0.724 (AKI with ABG), 0.738 (AKI without ABG), 0.774 (severe AKI with ABG), 0.794 (severe AKI without ABG). All these findings indicated the reliability of the novel risk scores for evaluation and monitoring the risk factors, so as to guide the in-time corrective measures to irreversible risk factors and prevent the occurrence and progression of AKI.
KDIGO guideline has established the definition of AKI and pointed out that limited measures were useful for treatment. Therefore, it is critical to identify the high-risk patients and perform early intervention. A study in America extracted data from electronic health records in a tertiary care, academic hospital.26 Risk models were established to predict AKI, the AUC values for AKI Risk and AKI Injury according to RIFLE criteria were 0.75 and 0.78, separately. The KDIGO AKI definition outperformed RIFLE criteria as proved in the former study.27 Our risk scoring system followed the latest definition guideline of AKI and obtained the comparable results. The AUC values were not greatly improved, partly because the study did not include new biomarkers to predict AKI. Given the new biomarkers were not widely applicable in clinical practice, this scoring system were adequately convenient and effective identify the high-risk patients in advance before they have already developed AKI or severe AKI. We considered this risk scoring system could be applied to all hospitalized patients since it was mainly based on blood tests and highly available before undergoing other expensive imaging or invasive inspection.
The multiple risk factors contained in our risk scoring systems have already been highly valued in previous studies. Patients in cardiac surgery and ICU are more likely to develop AKI compared with other admission departments and corresponding risk prediction scores were established.3,4,8 Underlying diseases like chronic kidney disease and heart failure have been involved in risk scoring systems in predicting AKI in ICU patients.7 The renal function was indicated with BUN, SCr and eGFR, and impaired renal function on the admission day was associated with AKI.20 Hypoproteinemia,7 hyperuricemia28 and elevated AST level26 would increase the risk of AKI. Despite these important factors, our study emphasized more on the formerly neglected electrolyte disorders.
Our research suggests that in patients undergoing blood gas analysis, the reduction of PH and HCO3- is associated with AKI; in patients without blood gas analysis, the reduction of CO2CP level is associated with AKI. A multicenter prospective cohort study showed that PH≤7.30 was identified as independent predictors of AKI in ICU patients.8 To obtain PH level and diagnose acid-base disturbances, patients need to undergo ABG analysis. But since it is an invasive procedure, patients hesitate to take the test and only a small portion of them receive ABG in clinical practice (14.5% in our study). CO2CP is much easier and widely accepted for patients to obtain from intravenous blood sampling. ABG. Although most patients have not measured ABG and PH level, with reduced CO2CP level, they might suffer from the potentially acidic inner environment. Most often, decreased CO2CP signifies the presence of metabolic acidosis. Similar to our study, another retrospective study has concluded that decreased CO2CP was considered as an independent risk factor for AKI.16 Moreover, our study illustrated that PH level severed as a promising predictive factor for AKI, but it was not associated with severe AKI. Previous study concluded the same result by suggesting that arterial blood PH was not associated with the progression of acute kidney injury in critically ill patients.29
Hypernatremia, hyponatremia, hypokalemia and hypocalcemia were associated with AKI in patients without ABG. Similar results were revealed in previous studies focus on the relationship between AKI and specific electrolyte disorders. A retrospective cohort study suggested that hypernatremia was a risk factor for AKI in patients with subarachnoid hemorrhage. The risk of AKI increased by 5.4% (95% CI 1.4–9.7%) for every 1 mEq/L increase in serum sodium.11 In critically ill patients, a U-shaped relationship was revealed between serum sodium and potassium magnitudes and the incidence of AKI.12 Hyponatremia, hypernatremia, hypokalemia, and hyperkalemia were related to the 90-day mortality rate and hyperkalemia predict a worse clinical outcome among patients with hyponatremia. Hypocalcemia was not fully evaluated in previous studies. Insufficient effective circulating blood volume (such as vomiting) or fluid overload (such as heart failure) might cause the decrease in calcium level. Further basic research is necessary to explain the pathophysiology mechanism.
Hyperphosphatemia was associated with high risk of developing severe AKI in our study. The renal function was of essential importance when related to phosphorus regulation. Previous studies have already demonstrated that hyperphosphatemia was associated with increasing risks of AKI, end-stage renal disease (ESRD) and mortality irrespective of previous kidney function.30 The mechanisms might involve calcification of smooth muscle cells, disrupted endothelial function and secretion of fibroblast growth factor.31,32
Hypomagnesemia was associated with AKI, while hypermagnesemia was associated with AKI progression. It was demonstrated that the prevalence of hypomagnesaemia was significantly higher in AKI patients.14 In an animal study, hypomagnesaemia might induce a decrease in the glomerular filtration rate and renal blood flow.33 Hypomagnesemia was considered as independent risk factors for non-recovery of renal function in critically ill patients.34 In this way, magnesium supplement might be highly suggested, but hypermagnesemia might also lead to serious commodities such as prolonged QT interval, bradycardia and even cardiac arrest.35 A study emphasized on patients presented with severe hypermagnesemia and subsequently underwent emergency hemodialysis.36 The associated AKI incidence was 60% and it was recommended that elder patients should regularly measure serum magnesium value when taking oral magnesium oxide. Our study suggested that hypermagnesemia was associated with severe AKI (AKI 2 or 3 stage) at hospital admission. A retrospective study found the similar results by establishing a U-shape curve between AKI and admission magnesium, indicating that both hypomagnesemia and hypermagnesemia were associated with increased risks of AKI in adult patients.37 However, it remained unknown whether the presence of hypermagnesemia is simply a reflection of AKI and other serious comorbidities or severed as a direct contributor to AKI. Further prospective studies are necessary for developing the causal relationship.
The study contains several limitations. Firstly, since it was a retrospective, single-center cohort study, the external validity or generalized ability of our results might need further evaluation. Besides, it was suggested that the predictive performance should be tested in an independent cohort of patients with the same and different ethnic backgrounds. We used data of electrolyte disorders on the admission day of patients and the fluctuation of electrolyte levels are necessary to be followed in future study. In addition, damage may occur before reaching the AKI threshold of changes in SCr or urine output, reflecting delay in these functional markers or the presence of renal reserve. This suggested the importance of developing biomarkers. The best-studied and most widely available biomarkers in the clinical setting are urinary or plasma neutrophil gelatinase-associated lipocalin (NGAL) and tissue inhibitor of metalloproteinases-2* insulin-like growth factor-binding protein 7 (TIMP2*IGFBP7). Urine NGAL was found to be an early predictive biomarker of AKI in clinical settings38 and was particularly associated with the severity of kidney injury NGAL.39 TIMP2*IGFBP7 showed the best accuracy and stability among all biomarkers, especially in cardiac surgery-associated AKI.40 This is the limitation of our studies for not including these biomarkers, since they were mostly tested in research and have not widely used in clinical practice. Lacking promising biomarkers might also explain that AUC level was not significantly promoted in our study. However, we pointed out that the accessible electrolyte lab results were promising in predict AKI and if not intervened in time, they might cause seriously adverse outcomes. Lastly, since it is a study based on observational data, we can draw the association between electrolyte disorders and AKI, further clinical and basic studies are required to elucidate the causality.
In conclusion, this study established the risk predicting systems for early identification of AKI and critical AKI in hospitalized patients. Most importantly, a variety of electrolyte disorders were reversible, and clinical monitoring should be timely and necessary measures should be taken to prevent the occurrence and development of AKI.
Statement of Ethics
This study was approved by the Ethical Committee of Zhongshan Hospital affiliated to Fudan University (No. B2018-175).
Funding
Shanghai Municipal Hospital Frontier Technology Project supported by Shanghai ShenKang Hospital Development Center (No. SHDC12018127), Shanghai “Science and technology innovation plan” Technology Standard Project (No.19DZ2205600), Xiamen Science and Technology Plan in 2018 (3502Z20184009), and Youth Foundation of Zhongshan Hospital (No.2020ZSQN44).
Disclosure
The authors have no conflicts of interest to declare.
References
1. Susantitaphong P, Cruz DN, Cerda J, et al. World incidence of AKI: a meta-analysis [J]. Clin J Am Soc Nephrol. 2013;8(9):1482–1493. doi:10.2215/CJN.00710113
2. Fang Y, Ding X, Zhong Y, et al. Acute kidney injury in a Chinese hospitalized population [J]. Blood Purif. 2010;30(2):120–126. doi:10.1159/000319972
3. Jiang W, Teng J, Xu J, et al. Dynamic predictive scores for cardiac surgery-associated acute kidney injury [J]. J Am Heart Assoc. 2016;5(8). doi:10.1161/JAHA.116.003754.
4. Thakar CV, Arrigain S, Worley S, et al. A clinical score to predict acute renal failure after cardiac surgery [J]. J Am Soc Nephrol. 2005;16(1):162–168. doi:10.1681/ASN.2004040331
5. Mehran R, Aymong ED, Nikolsky E, et al. A simple risk score for prediction of contrast-induced nephropathy after percutaneous coronary intervention: development and initial validation [J]. J Am Coll Cardiol. 2004;44(7):1393–1399. doi:10.1016/j.jacc.2004.06.068
6. Kheterpal S, Tremper KK, Heung M, et al. Development and validation of an acute kidney injury risk index for patients undergoing general surgery: results from a national data set [J]. Anesthesiology. 2009;110(3):505–515. doi:10.1097/ALN.0b013e3181979440
7. Chawla LS, Abell L, Mazhari R, et al. Identifying critically ill patients at high risk for developing acute renal failure: a pilot study [J]. Kidney Int. 2005;68(5):2274–2280. doi:10.1111/j.1523-1755.2005.00686.x
8. Malhotra R, Kashani KB, Macedo E, et al. A risk prediction score for acute kidney injury in the intensive care unit [J]. Nephrol Dial Transpl. 2017;32(5):814–822. doi:10.1093/ndt/gfx026
9. Chertow GM, Burdick E, Honour M, et al. Acute kidney injury, mortality, length of stay, and costs in hospitalized patients [J]. J Am Soc Nephrol. 2005;16(11):3365–3370. doi:10.1681/ASN.2004090740
10. Mayor S. UK report into acute kidney injury deaths recommends electrolyte checks in all emergency admissions [J]. BMJ 2009;338:b2370.
11. Kumar AB, Shi Y, Shotwell MS, et al. Hypernatremia is a significant risk factor for acute kidney injury after subarachnoid hemorrhage: a retrospective analysis [J]. Neurocrit Care. 2015;22(2):184–191. doi:10.1007/s12028-014-0067-8
12. Gao XP, Zheng CF, Liao MQ, et al. Admission serum sodium and potassium levels predict survival among critically ill patients with acute kidney injury: a cohort study [J]. BMC Nephrol. 2019;20(1):311. doi:10.1186/s12882-019-1505-9
13. Suetrong B, Pisitsak C, Boyd JH, et al. Hyperchloremia and moderate increase in serum chloride are associated with acute kidney injury in severe sepsis and septic shock patients [J]. Crit Care. 2016;20(1):315. doi:10.1186/s13054-016-1499-7
14. Chintala V, Prabhu VM, Boyanagari M, et al. Role of hypomagnesaemia in acute kidney injury [J]. J Clin Diagn Res. 2018. doi:10.7860/JCDR/2018/28073.11329
15. Wang Y, Hu J, Geng X, et al. A novel scoring system for assessing the severity of electrolyte and acid-base disorders and predicting outcomes in hospitalized patients [J]. J Invest Med. 2019;67(4):750–760. doi:10.1136/jim-2018-000900
16. Hu J, Wang Y, Geng X, et al. Metabolic acidosis as a risk factor for the development of acute kidney injury and hospital mortality [J]. Exp Ther Med. 2017;13(5):2362–2374. doi:10.3892/etm.2017.4292
17. Jindal SL. Clinical Physiology of Acid—Base and Electrolyte Disorders [M]. Can Med Assoc J. 1978;118(1):27–30.
18. Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group. KDIGO clinical practice guideline for acute kidney injury. [J]. Kidney Int. 2012;2(suppl):1–138.
19. Jones DC, Hayslett JP. Outcome of pregnancy in women with moderate or severe renal insufficiency [J]. N Engl J Med. 1996;335(4):226–232. doi:10.1056/NEJM199607253350402
20. Gibson CM, Pinto DS, Murphy SA, et al. Association of creatinine and creatinine clearance on presentation in acute myocardial infarction with subsequent mortality [J]. J Am Coll Cardiol. 2003;42(9):1535–1543. doi:10.1016/j.jacc.2003.06.001
21. Levey AS, Stevens LA, Schmid CH, et al. A new equation to estimate glomerular filtration rate [J]. Ann Intern Med. 2009;150(9):604–612. doi:10.7326/0003-4819-150-9-200905050-00006
22. Levey AS, Coresh J, Bolton K, et al.K/DOQI clinical practice guidelines for chronic kidney disease: evaluation, classification, and stratification [J]. Am j Kidney Dis. 2002;39(2Suppl 1):S1–266.
23. Vergouw D, Heymans MW, VAN DER WINDTDA, et al. Missing data and imputation: a practical illustration in a prognostic study on low back pain [J]. J Manipulative Physiol Ther. 2012;35(6):464–471. doi:10.1016/j.jmpt.2012.07.002
24. Rothman K. Disengaging from statistical significance [J]. J Eur J Epidemiol. 2016;31(5):443–444. doi:10.1007/s10654-016-0158-2
25. Grimes DA, Schulz KF. Refining clinical diagnosis with likelihood ratios [J]. Lancet (London, England). 2005;365(9469):1500–1505. doi:10.1016/S0140-6736(05)66422-7
26. Matheny ME, Miller RA, Ikizler TA, et al. Development of inpatient risk stratification models of acute kidney injury for use in electronic health records [J]. Med Decis Making. 2010;30(6):639–650. doi:10.1177/0272989X10364246
27. T-y TSAI, Chien H, Tsai F-C, et al. Comparison of RIFLE, AKIN, and KDIGO classifications for assessing prognosis of patients on extracorporeal membrane oxygenation [J]. J Formosan Med Assoc. 2017;116(11):844–851. doi:10.1016/j.jfma.2017.08.004
28. Xu X, Hu J, Song N, et al. Hyperuricemia increases the risk of acute kidney injury: a systematic review and meta-analysis [J]. BMC Nephrol. 2017;18(1):27. doi:10.1186/s12882-016-0433-1
29. Dunn WJ, Shimizu T, Santamaria N, et al. The effect of urinary and arterial blood pH on the progression of acute kidney injury in critically ill patients with systemic inflammatory response syndrome or sepsis and oliguria [J]. Aust Crit Care. 2016;29(1):41–45. doi:10.1016/j.aucc.2015.06.001
30. Moon H, Chin HJ, Na KY, et al. Hyperphosphatemia and risks of acute kidney injury, end-stage renal disease, and mortality in hospitalized patients [J]. BMC Nephrol. 2019;20(1):362. doi:10.1186/s12882-019-1556-y
31. Zhao MM, Xu MJ, Cai Y, et al. Mitochondrial reactive oxygen species promote p65 nuclear translocation mediating high-phosphate-induced vascular calcification in vitro and in vivo [J]. Kidney Int. 2011;79(10):1071–1079. doi:10.1038/ki.2011.18
32. Jung SY, Kim H, Park S, et al. Electrolyte and mineral disturbances in septic acute kidney injury patients undergoing continuous renal replacement therapy [J]. Medicine. 2016;95(36):e4542. doi:10.1097/MD.0000000000004542
33. Seguro AC, DE ARAUJO M, Seguro FS, et al. Effects of hypokalemia and hypomagnesemia on zidovudine (AZT) and didanosine (ddI) nephrotoxicity in rats [J]. Clin Nephrol. 2003;59(4):267–272. doi:10.5414/CNP59267
34. Alves SC, Tomasi CD, Constantino L, et al. Hypomagnesemia as a risk factor for the non-recovery of the renal function in critically ill patients with acute kidney injury [J]. Nephrol Dial Transpl. 2013;28(4):910–916. doi:10.1093/ndt/gfs268
35. Topf JM, Murray PT. Hypomagnesemia and Hypermagnesemia [J]. Rev Endocr Metab Disord. 2003;4(2):195–206. doi:10.1023/A:1022950321817
36. Nishikawa M, Shimada N, Kanzaki M, et al. The characteristics of patients with hypermagnesemia who underwent emergency hemodialysis [J]. Acute Med Surg. 2018;5(3):222–229. doi:10.1002/ams2.334
37. Cheungpasitporn W, Thongprayoon C, Erickson SB. Admission hypomagnesemia and hypermagnesemia increase the risk of acute kidney injury [J]. Ren Fail. 2015;37(7):1175–1179. doi:10.3109/0886022X.2015.1057471
38. Devarajan P. Emerging biomarkers of acute kidney injury [J]. Contrib Nephrol. 2007;156:203–212.
39. Bennett M, Dent CL, Ma Q, et al. Urine NGAL predicts severity of acute kidney injury after cardiac surgery: a prospective study [J]. Clin J Am Soc Nephrol. 2008;3(3):665–673. doi:10.2215/CJN.04010907
40. Wang Y, Zou Z, Jin J, et al. Urinary TIMP-2 and IGFBP7 for the prediction of acute kidney injury following cardiac surgery [J]. BMC Nephrol. 2017;18(1):177. doi:10.1186/s12882-017-0592-8
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.