Back to Journals » Substance Abuse and Rehabilitation » Volume 9
Review of the effects of self-stigma and perceived social stigma on the treatment-seeking decisions of individuals with drug- and alcohol-use disorders
Authors Hammarlund R, Crapanzano KA , Luce L , Mulligan L , Ward KM
Received 9 August 2018
Accepted for publication 23 October 2018
Published 23 November 2018 Volume 2018:9 Pages 115—136
DOI https://doi.org/10.2147/SAR.S183256
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Li-Tzy Wu
R Hammarlund,1 KA Crapanzano,2 L Luce,2 L Mulligan,2 KM Ward2
1Our Lady of the Lake Division of Academic Affairs, Baton Rouge, LA, USA; 2Department of Psychiatry, Louisiana State University Health Sciences Center, Baton Rouge, LA, USA
Abstract: Substance-use disorders are a public health crisis globally and carry with them significant morbidity and mortality. Stigma toward people who abuse these substances, as well as the internalization of that stigma by substance users, is widespread. In this review, we synthesized the available evidence for the role of perceived social stigma and self-stigma in people’s willingness to seek treatment. While stigma may be frequently cited as a barrier to treatment in some samples, the degree of its impact on decision-making regarding treatment varied widely. More research needs to be done to standardize the definition and measurement of self- and perceived social stigma to fully determine the magnitude of their effect on treatment-seeking decisions.
Keywords: self-stigma, perceived social stigma, substance-use disorders, treatment seeking
Introduction
Alcohol-use disorders (AUDs) and drug-use disorders (DUDs) are issues of great concern to public health officials around the world. According to the World Drug Report, 31 million adult drug users across the globe suffer from a DUD, and the number of deaths from drug overdose has been rising.1 Indeed, in the USA alone, deaths from overdoses of heroin or other opioids have quadrupled since 2010.2 Although much of this trend is attributable to increases in the use of pharmaceutical opioids, legal substances, such as alcohol, are also problematic. Globally, 16% of individuals 15 years of age or older reported participating in episodes of heavy alcohol consumption in 2014, and 5.9% of all deaths that year were caused by alcohol use.3 In the USA, 15.1 million adults over the age of 18 years had an AUD in 2015.4
Despite the potentially lethal consequences of DUDs and AUDs, it has been estimated that fewer than one in six individuals worldwide receives treatment each year.1 Within the USA, the National Epidemiologic Survey on Alcohol and Related Conditions estimated that rates of treatment seeking during the first year of disorder onset were 13% for drug dependence, 2% for drug abuse, 5% for alcohol dependence, and 1% for alcohol abuse.5 Previous work has identified a number of treatment barriers that contribute to these low utilization rates. These barriers include systematic issues (ie, features endemic to the health care system), such as high costs of treatment, poor coordination among health care providers, inconvenient service hours, delays in access (ie, lengthy waiting times to see providers and lengthy waits for acceptance into treatment programs), and shortages of programs.6–13 Nonsystematic treatment barriers (ie, characteristics of individuals rather than the health care system) include denial of a problem,8,14–16 lack of knowledge of treatment options,6–9 and dislike of available treatment options stemming either from doubts about the treatment model being offered or the perceived daily burden of participating in treatment.6 Perceived burden is a particularly common complaint among opioid users in methadone maintenance treatment, which requires a daily time commitment to participate successfully.17
One type of barrier that is believed to be particularly impactful for those in need of treatment for AUDs and DUDs is stigma. Stigma is a complex construct that can come from many sources and may manifest as a barrier in several ways. Perceived social stigma is one type of stigma in which a person recognizes and believes that their society holds prejudicial beliefs that will result in discrimination against them.18 Perceived social stigma can act as a systematic barrier when those to whom substance users turn for help (eg, primary-care providers) react with negative judgments and even disgust. Indeed, there is evidence not only that primary-care providers do not feel prepared to deliver appropriate care to those with substance-use issues, such as AUD and DUD,19 but also that health care professionals in general may have negatively biased views of these individuals that include beliefs that such individuals are violent, manipulative, and poorly motivated to change.20 Such reactions to substance users may be so subtle that they are felt by the substance user, but are otherwise ineffectual, or they may be accompanied by more direct disparities in care (eg, differential care patterns after acute myocardial infarction).21 These attitudes may also directly impact the behaviors of drug and alcohol users, as research has shown that individuals who experience discrimination are much more likely to engage in behaviors that are harmful to their health.22 Finally, perceived social stigma may become internalized and result in self-stigma (ie, the personal endorsement of stereotypes about oneself and the resulting prejudice and self-discrimination).18
Various types of stigma can also act as nonsystematic barriers. Public stigma against substance abuse is common23 and can deter people with a variety of mental health conditions, including substance-related conditions, from seeking help, due to feelings of embarrassment or shame.1,5,16 Self-stigma can also deter treatment when it results in loss of self-respect and questioning the point of trying to get better.24 At least one review has found that attitudinal barriers, a category including stigma, were more important in predicting nontreatment than financial barriers.25 However, note that this review was limited in scope to papers produced from one nationwide longitudinal study, while there have been a number of other studies that have examined this issue. The purpose of the current paper is to provide a broader review of the literature examining the impact of perceived social stigma and self-stigma on treatment-seeking decisions, including expressed desire to enter treatment.
Methods
Search strategy
A systematic search of the literature was carried out to identify articles related to perceived social stigma and self-stigma related to seeking treatment for AUDs and DUDs. The PubMed, Scopus, and PsycInfo databases were searched first in September 2016. Our initial search used the following terms: (“social stigma” OR self-stigma) AND (dependence, addiction, OR abuse). We then expanded our PubMed search by adding the MeSH terms “shame” and “substance-related disorders”, producing the following search string: (“shame” [MeSH] OR “social stigma” OR self-stigma OR stigma) AND “substance-related disorders” (MeSH). We then also expanded our PsycInfo and Scopus searches to the following: (shame OR “social stigma” OR self-stigma OR stigma) AND “substance-related disorders” OR “drug abuse” OR “drug dependence” OR “alcohol abuse” OR “alcohol dependence” OR addiction OR “substance abuse”. References identified within publications and thought to be relevant were added to the corpus of articles for further screening. Due to the time lapse between the initial search and finalization of the manuscript, the search was repeated on July 27, 2018.
Selection of literature
After discarding of duplicates and articles not available in English (due to lack of translation resources), at least two people examined the title and abstract of each article for relevance to the review questions. Next, the bodies of the remaining papers were reviewed. Opinion pieces, conference abstracts, case reports, case series, commentaries, and review articles or book chapters without original research reported were excluded, as were studies that did not have people who used psychoactive substances as subjects or that did not explicitly link social or self-stigma to treatment seeking. We included articles that were original empirical work and explicitly linked stigma (of any type, as terminology varied or was vague in many studies, ie, did not specify a type of stigma) or stigma-like constructs (ie, shame,1 embarrassment, need for secrecy) to either the desire to seek treatment or actually seeking treatment for alcohol or drug use. Stigma-like constructs were included because in many articles stigma was a loosely defined concept that was discussed in terms of being ashamed or embarrassed for others to find out about problematic drug or alcohol use, but not necessarily precisely worded during measurement. We also included both articles that specified diagnoses of AUD or DUD and those that referenced problematic alcohol or drug use in the absence of an official diagnosis. We did not screen articles based on the legality of the substance. We did exclude studies that looked solely at nicotine dependence, as this was not the target of this review. Because we aimed to be as inclusive as possible, we did not exclude articles based on quality of evidence, but rather critiqued articles as appropriate in our analysis.
All authors participated in initial screening before the primary author and KC reviewed them again to ensure completeness. Disagreements, if any, were resolved through discussion and consensus. The PRISMA flowchart for selection of articles is shown in Figure 1.
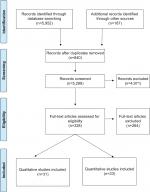  | Figure 1 PRISMA flow diagram. |
Data extraction
Tables 1 and 2 contain overall summaries of all articles. For each article, we extracted reference information, location, sample size, participant demographics, relevant constructs measured in the study, and results relevant to this review. For qualitative articles (Table 1), we extracted analysis approach, while for quantitative articles (Table 2), we extracted construct-measurement tools.
  | Table 1 Summary of characteristics of included qualitative publications related to treatment seeking Abbreviations: AA, Alcoholics Anonymous; OST, opioid-substitution therapy. |
Results
Figure 1 illustrates the literature-identification and -screening process. Of 6,139 articles considered, 64 were included in the final review. A total of 31 qualitative articles are summarized in Table 1, and 33 quantitative articles are summarized in Table 2. Note that “perceived stigma” is based upon subjective reports, and thus does not bear on this issue of whether or not such stigma was objectively present. Also of note, the etiology of reports of stigma from health care professionals could be debated as a version of structural stigma, the process of institutions having a culture of stigmatizing policies and practices (with employees representing the policies and attitudes of the places in which they work), or public stigma (with their attitudes representing their own core beliefs). We chose to interpret it as the latter, and instances of this are noted as perceived health care-professional stigma, a subset of perceived social stigma, in the tables. Not all studies used the exact constructs of self-stigma or perceived social stigma in their work. However, the constructs we included were those that were most closely related to these types of stigma and measured some aspect of one or the other.
Qualitative stigma experiences
A number of qualitative studies (see Table 1) have provided an overview of the stigma experiences of those in need of treatment for substance abuse. Feelings of shame,26–28 embarrassment,26,29,30 and guilt26 were reported. Problem substance users also reported a need for secrecy about both their use and any attempts to seek treatment.27,28,31 This secrecy was linked to perceptions of stigma from health care providers in general practice and emergency settings, who may be the first source of help available, and thus the need for secrecy was said to lead to delays in treatment seeking.29–33 Two studies suggested that these feelings and need for secrecy stemmed from a strong desire to avoid accepting the identity of “addict” or “junkie”,34,35 while two more found that even those who had attempted to seek treatment may disengage when identity conflicts arise.17,36 On the other hand, participants in one study said they had sought help from a general practitioner specifically to avoid stigma from social sources,33 while those in other studies said that emotional support from loved ones had facilitated seeking formal help for substance abuse.37,38
Frequency of stigma as a barrier
Of the 33 quantitative studies summarized in Table 2, 23 shed light on the frequency with which stigma was perceived as a barrier to treatment relative to other barriers. Stigma-as-barrier frequencies ranged from just 2%39 up to 92%40 (mean 30.39%, SD 19.46%). Using 50% frequency as a cutoff to differentiate between high (≥50%) and low (<50%) stigma-frequency studies, only four40–43 fall into the high-frequency category (mean 67.00%, SD 11.37%). All these high-frequency studies were cross-sectional. Among the low-frequency studies (mean 31.33%, SD 19.99%), three reported high stigma frequencies in certain subsets of their sample.7,44,45 Bisexuals (compared to heterosexual and homosexual,44 but see also Green,42 who found heterosexuals reported stigma more often than homosexual and bisexual individuals), people with many barriers (compared to few barriers),45 and alcohol users (compared to drug users)7 all reported stigma as a barrier >50% of the time, whereas their comparison groups did not. In a primarily qualitative study of illicit-stimulant users, less than half had entered drug-abuse treatment and most did not feel they needed help; social stigma was cited only by a few as a barrier to treatment.46 The remaining 16 studies all reported low frequencies for stigma (mean 18.99, SD 8.59). These studies were both longitudinal (n=10) and cross-sectional (n=6).
Relative to other barriers, the frequencies reported in the 23 studies put stigma (or stigma-relevant constructs) in ordinal ranks ranging from most to 13th-most frequently reported (see Table 3). Overall, stigma (or a stigma-like construct) was in the top-three most frequent barriers in 17 studies. These studies also reported the frequencies of other treatment barriers. “Should handle alone” was the most frequent barrier in seven studies,8,13,14,44,45,47,48 stigma (or stigma-relevant constructs) in six studies,7,39–41,43,49 denial of a problem in five,13,39,42,50,51 “not ready to quit” in three,10,12,52 cost and access barriers in four,10–12,53 role responsibilities in two,44,54 and treatment attitudes in one.11 Note that barriers tied for most frequent in several studies, and that the rank order of barriers often varied by participant group (eg, men vs women). See Table 3 for more details.
  | Table 3 Summary of barrier frequency rankings in articles with frequency data Abbreviation: NA, not applicable/not available. |
Only five qualitative articles in Table 1 reported frequency of stigma as a barrier, ranging from 15%55 to 90%56 (mean 55.75%, SD 29.90). The highest frequency was from a study where stigma was associated with a national drug-user registration system that led to lifelong consequences.56 The second-highest frequency, 78% for female substance users, actually reflects the number of women who felt compounded stigma for being both female and a user.6 The remaining three frequencies were <50%,55,57,58 and one of these duplicates data from an article in Tables 2 and 3.54,55
Degree of influence of stigma
In addition to frequency, three quantitative studies directly asked participants to rate the degree of influence stigma had on their decisions about treatment seeking. In the first, mean ratings (on a scale from 1 [not influential] to 5 [very influential]) were 3.7 for alcohol users and 3.4 for drug users.7 These values were the seventh- (for alcohol users) and eighth- (for drug users) highest influence ratings: the most influential barrier for alcohol users was being unaware of treatment options, while for drug users it was being in denial of a problem. In the second study, the mean stigma-influence rating for alcohol users was 0.72 (on a scale from 0 [not influential] to 3 [very influential]), with stigma being the third-most influential barrier of nine.42 In this study, denial of a problem was the most influential barrier. Finally, the third study found that problem drinkers’ mean stigma-influence rating was 2.7 (on a scale from 1 [not influential] to 5 [very influential]), with stigma being the most influential of six barriers.43
Stigma as a statistical predictor of treatment
Twelve studies that did not ask participants to rate directly the influence of stigma on their treatment-seeking decisions did use statistical methods to determine whether or not stigma predicted treatment motivation and/or utilization.13,15,42,54,59–66 Of these, five found stigma to be a positive predictor or copredictor,54,60,63–65 three found it to be a negative predictor or copredictor,15,61,62 and three found it not to be a predictor at all.13,42,59
The first study that found stigma to be a positive predictor found that stigma barriers significantly predicted treatment utilization at 3-month follow-up for cocaine users seen in the emergency room, while other types of treatment barriers did not.60 The second study found that pregnant women in a detoxification program who reported an acceptability barrier (a category that included stigma) had increased treatment-motivation scores, while gestational age of the fetus was a negative predictor.54 The third and fourth studies were different analyses of the same data. The third study found stigma consciousness to be a positive predictor of current treatment utilization for women only,64 while the fourth found it to be a significant positive predictor for “colored” participants only.63 The final study found that person-related barriers (a category that included stigma, but also “wanting to handle the problem on your own” and not having motivation or reasons to stop drinking) positively predicted currently being in treatment. Sex and education level were also positive predictors, while intrapersonal consequences and emotional distress were negative predictors.65
The first study that found stigma to be a negative predictor found that higher alcohol-related stigma (controlling for disorder severity, sex, age, race, ethnicity, income, education, and marital status) was related to less lifetime use of any treatment option.15 The second study found that drug stigma was related only to 12-month treatment utilization in those who also had high HIV stigma.61 The third study was conducted with psychology students, and found that more stigma was related to less interest in seeking help.62
Finally, one study that did not find stigma to be a significant predictor found that alcohol-related stigma did not predict treatment seeking 1 year later.13 A second study found that alcohol-related stigma was related to race, but that race did not predict treatment seeking 1 year later.59 The third study grouped stigma with all perceived barriers, and found it did not predict having a history of treatment use.42
Compounding effects of multiple stigmas
A total of 29 studies reported on the combined effects of multiple stigmas on treatment-seeking decisions.6,8,11,12,30,37,39,41,44,45,50,55–57,59,61,63,64,67–78 Generally speaking, individuals with more barriers to treatment were found to be less likely to seek treatment than those with fewer barriers in one study.45 More specifically, participants across various studies reported compounded effects on treatment decisions of being both substance users and older,57,67 a member of a racial or ethnic minority,8,50,59,64,68,69 HIV-positive,61 dually diagnosed with depression,11 or female.6,30,37,50,54,56,64,70–74 Females in several studies had a number of additional stigmas, including that of being pregnant,54 incarcerated,72 or black.74 Stigmas were particularly influential on women when their substance use and/or usage of treatment services had implications for child-custody arrangements.30,37 Other institutional influences also increased the influence of stigma. Studies in countries with drug-user registries showed that fears of the consequences of the registration process affected decisions to seek treatment for many.50,56,75,76 Country of origin also impacted the influence of stigma in the absence of such programs, likely via social and cultural expectations.39 Additionally, sexual orientation (bisexuality compared to homo- and heterosexuality)44 and some chosen careers (nursing and army soldiers)41,77,78 increased the influence of stigma in some studies.
Congruently with these findings, a study that did not specifically measure multiple stigmas, but did look at the ability of demographic variables to predict treatment use longitudinally, found that being a woman, a minority, married, college-educated, employed, and having a higher income all decreased the odds of having sought treatment in the past year.12
Discussion
The articles reviewed here provide a mixed picture as to the influence of stigma on treatment decisions in those with a need for treatment for alcohol or drug use. Seventy percent of quantitative studies that provided frequency information for stigma as a treatment barrier reported low rates, with stigma ranging between the most and 13th-most frequently cited barrier. All studies reporting high frequency for stigma were cross-sectional and thus incapable of prospective prediction of treatment utilization, whereas ten of the studies with low frequency were longitudinal in nature.
That said, frequency itself is not necessarily the variable of most interest. A barrier might occur only in a small number of people and yet be highly influential for those individuals. Only three studies in this review asked participants to rate the influence of stigma on their treatment-seeking decisions: in these, stigma ranged from the most influential to eighth-most influential barrier. The study where stigma was rated as most influential included only 39 alcohol users,43 while the other two studies included 21842 and 346 individuals.7 With so few studies, such low sample sizes, and such mixed findings of influence strength, it is unwise to make strong claims about the ultimate influence of stigma on treatment decisions in the larger population of substance users.
Statistical prediction of treatment utilization also showed mixed results in the studies reviewed. Five studies found that stigma was a positive predictor or copredictor, three that it was negative predictor or copredictor, and three that it was not a predictor at all. Of the positive (co)predictor studies, two looked at stigma within a larger category of barriers,54,65 two probed the stigma of being a user (as opposed to the stigma of getting into treatment),63,64 and one looked at individuals who had experienced a significant health event related to their use.60 It stands to reason that measuring stigma within a larger category loses some specificity in terms of the direct impact of stigma on treatment-seeking decisions. Additionally, probing stigma of use is quite different from probing the stigma of getting treatment. It is easy to understand why someone might feel pressure to get help if it were known they had a problem with drugs or alcohol, whereas due to secretive coping strategies, many users may actually be able to maintain a degree of privacy concerning their use that would be lost by seeking treatment. Therefore, this collection of studies does not provide strong evidence of a positive influence of stigma on treatment seeking.
In terms of negative (co)predictor studies, the first was cross-sectional data from a longitudinal study.15 Another article from the same longitudinal study, but using two waves of data, found that stigma was not a predictor of treatment use,13 calling into question the utility of cross-sectional data in assessing this relationship. The second negative study found stigma was influential only when present for two statuses (ie, user and HIV-positive),61 supporting the idea that confounded multiple stigmas may be highly influential, but not providing good evidence of a singular effect of substance-related stigma. Finally, the third negative study was conducted in college students (as opposed to a sample of only those with substance-use disorders) and measured only “help-seeking interest”, not actual use of services,62 making this study a measure of theoretical attitudes, rather than actual behavior in a population in need of treatment. As such, these studies are not particularly convincing either.
Of the studies that found no relationship between treatment seeking and stigma, two were longitudinal13,59 and one was not.42 One of the longitudinal studies only looked at stigma as a predictor indirectly through its relationship to race,59 and the cross-sectional study grouped stigma with all perceived barriers to treatment.42 The remaining longitudinal study13 is somewhat more convincing, in that it is a report from a nationwide study and contains two waves of data. On balance, however, this group of studies is no more convincing than those that found a relationship between stigma and treatment-seeking decisions.
On more steady ground is the finding that multiple stigmas together can have compounded influence on treatment-seeking decisions. Thirty studies (47%) found evidence of the increased influence of compounded stigmas or a relationship between stigmatized demographic variables (ie, being a woman or minority) and treatment-seeking decisions. However, recognition of this fact may have contributed to the development of more culturally appropriate treatment programs for people with these compounded stigmas,79 and thus the gap for sex and racial groups to access care, while still present, may have narrowed in recent years.80
The mixed results reported in this review are somewhat disheartening, given the number of studies included. However, as previously alluded to, one major factor in this problem is likely related to varying definitions and measurement of the constructs of interest. Stigma is a complex construct, and is thus difficult to define and measure. There are different sources of stigma, including social institutions, public opinion, and the self. Moreover, these sources are all interconnected. For example, self-stigma is thought to develop as external stigma internalized by the individual.81 It is also the case that stigma can range from extremely subtle perceptions, which themselves may arise from objectively observable external sources or from subjective inner perceptions, to blatant discrimination practices. In terms of drug and alcohol use, there are also different targets of the stigma: there is the stigma of being a user itself, there is the entirely separate stigma of being someone who needs help with their use, which is activated when one seeks treatment services, and there is differentiated stigma, depending on the substance being used.82 Finally, there is also the problem of multiple compounded stigmas. Many people who fall into one stigmatized category (eg, drug user) also fall into other such categories (eg, incarcerated individual, bisexual, female). Locating the boundary between one stigma and the next is difficult, if not impossible, and thus their impact must often be assessed together, rather than individually.
Beyond simply defining stigma, researchers have measured it in a number of ways, making it somewhat difficult to pull all the literature together coherently. Some measured stigma within a larger category (eg, acceptability of treatment), some measured one type or the other (eg, social stigma vs self-stigma) alone, others measured components of stigma that they had defined in various ways (eg, perceived devaluation), and still others measured stigma-related concepts (eg, fear of what others think or embarrassment). This lack of standardization must be considered when attempting to determine why one study may find a relation between (whatever they are calling) stigma and treatment seeking, while another does not. A secondary consequence is that there are not a large number of studies with the same measure of stigma to aggregate in a meta-analysis, which would be the best way to determine the strength of the evidence for any effect.
In addition to the complexity in defining and measuring stigma, there is the complexity of human motivation to consider. In a number of studies, the most frequently cited reasons not to seek treatment were not being ready to stop using,10,12,52 not accepting that there was a problem with use,13,39,42,50,51 or other attitudes about treatment.8,11,14,44,45,47,48 Stages of readiness to change must be considered when looking at the impact of stigma,60,62,83 as it stands to reason that someone who does not recognize they have a problem with drug or alcohol use at all will not be particularly influenced by perceived stigma against substance-use treatment, as the idea of getting treatment does not enter their consciousness. In other words, if one wishes to measure the influence of stigma on treatment seeking, first one must know where the sample falls in terms of problem recognition. Indeed, modern substance-use-treatment approaches are centered on the stages-of-change model.
Another factor to consider is treatment history. Notley33 suggests that studies in this area should consider those who have a previous treatment history separately from those who have not. Having been through the process before exposes one to actual experiences of various types of stigma, as opposed to the anticipation of stigma in those who have not yet sought any treatment. Indeed, veterans who had attended at least nine mental health-treatment sessions had higher stigma scores than those who had not,84 a finding that one might reasonably suspect would be relevant in the case of drug- and alcohol-use treatment. Therefore, stigma may have a different level of influence in each population. Relatedly, a common theme in a number of studies in this review was that the source of stigma matters. In particular, it seems that nonjudgmental acceptance from staff at health care and substance-treatment facilities might be instrumental in overcoming negative emotions, self-stigma, and perceived social stigma associated with treatment, whereas staff who propagate stigma in populations with drug- or alcohol-use problems discourage these individuals from seeking or remaining in treatment.
In summary, this review of the literature found that while stigma may be frequently cited as a barrier to treatment in some samples, it is unclear if it is a particularly influential one. Clearly in some cases it is highly influential, such as when multiple stigmas are compounded, or when the stigma is being experienced or anticipated from staff at rehabilitation facilities or programs. But there are also clearly times when stigma is not the main concern, most especially when the user does not recognize their use as problematic. In a similar vein, sometimes stigma is not perceived as such directly, but can be seen in indirect ways (eg, worried about what others will think, feelings of embarrassment). Without concentrated efforts to standardize the definition and measurement, the exact magnitude of the effect of stigma on treatment-seeking decisions, if any, will almost certainly remain unknown.
Acknowledgment
The authors would like to thank Richard Vath, MA, for his invaluable help in the conceptualization and early organization of the paper.
Disclosure
The authors report no conflicts of interest in this work.
References
World Drug Report 2018 (United Nations publication SNEX). Available from: https://www.unodc.org/wdr2018. Accessed July 3, 2018. | ||
Centers for Disease Control and Prevention, National Center for Injury Prevention and Control, Division of Unintentional Injury Prevention. Heroin Overdose Data; Updated January 26, 2017. Available from: https://www.cdc.gov/drugoverdose/data/heroin.html. Accessed May 21, 2017. | ||
Chestnov O. Global Status Report on Alcohol and Health 2014. Switzerland: World Health Organization; 2014. | ||
(SAMHSA) SAaMHSA. 2015 National Survey on Drug Use and Health (NSDUH) Table 5.6A – Substance Use Disorder in Past Year among Persons Aged 18 or Older, by Demographic Characteristics: Numbers in Thousands, 2014 and 2015; 2015. Available from: https://wwwsamhsagov/data/sites/default/f iles/NSDUH-DetTabs-2015/NSDUH-DetTabs-2015/NSDUH-DetTabs-2015htm#tab5-6b. Accessed November 12, 2018. | ||
Blanco C, Iza M, Rodríguez-Fernández JM, Baca-García E, Wang S, Olfson M. Probability and predictors of treatment-seeking for substance use disorders in the U.S. Drug Alcohol Depend. 2015;149:136–144. | ||
Copeland J. A qualitative study of barriers to formal treatment among women who self-managed change in addictive behaviours. J Subst Abuse Treat. 1997;14(2):183–190. | ||
Cunningham JA, Sobell LC, Sobell MB, Agrawal S, Toneatto T. Barriers to treatment: why alcohol and drug abusers delay or never seek treatment. Addict Behav. 1993;18(3):347–353. | ||
Grant BF. Barriers to alcoholism treatment: reasons for not seeking treatment in a general population sample. J Stud Alcohol. 1997;58(4):365–371. | ||
McCutcheon JM, Morrison MA. Injecting on the Island: a qualitative exploration of the service needs of persons who inject drugs in Prince Edward Island, Canada. Harm Reduct J. 2014;11(1):10. | ||
Ali MM, Teich JL, Mutter R. Reasons for not seeking substance use disorder treatment: variations by health insurance coverage. J Behav Health Serv Res. 2017;44(1):63–74. | ||
Chen LY, Strain EC, Crum RM, Mojtabai R. Gender differences in substance abuse treatment and barriers to care among persons with substance use disorders with and without comorbid major depression. J Addict Med. 2013;7(5):325–334. | ||
Choi NG, Dinitto DM, Marti CN. Treatment use, perceived need, and barriers to seeking treatment for substance abuse and mental health problems among older adults compared to younger adults. Drug Alcohol Depend. 2014;145:113–120. | ||
Mojtabai R, Crum RM. Perceived unmet need for alcohol and drug use treatments and future use of services: results from a longitudinal study. Drug Alcohol Depend. 2013;127(1–3):59–64. | ||
Cohen E, Feinn R, Arias A, Kranzler HR. Alcohol treatment utilization: findings from the National Epidemiologic Survey on Alcohol and Related Conditions. Drug Alcohol Depend. 2007;86(2–3):214–221. | ||
Keyes KM, Hatzenbuehler ML, McLaughlin KA, et al. Stigma and treatment for alcohol disorders in the United States. Am J Epidemiol. 2010;172(12):1364–1372. | ||
Cumming C, Troeung L, Young JT, Kelty E, Preen DB. Barriers to accessing methamphetamine treatment: a systematic review and meta-analysis. Drug Alcohol Depend. 2016;168:263–273. | ||
Radcliffe P, Stevens A. Are drug treatment services only for ‘thieving junkie scumbags’? Drug users and the management of stigmatised identities. Soc Sci Med. 2008;67(7):1065–1073. | ||
Corrigan PW, Rao D. On the self-stigma of mental illness: stages, disclosure, and strategies for change. Can J Psychiatry. 2012;57(8):464–469. | ||
Miller NS, Sheppard LM, Colenda CC, Magen J. Why physicians are unprepared to treat patients who have alcohol- and drug-related disorders. Acad Med. 2001;76(5):410–418. | ||
van Boekel LC, Brouwers EP, van Weeghel J, Garretsen HF. Stigma among health professionals towards patients with substance use disorders and its consequences for healthcare delivery: systematic review. Drug Alcohol Depend. 2013;131(1–2):23–35. | ||
Li Y, Glance LG, Lyness JM, Cram P, Cai X, Mukamel DB. Mental illness, access to hospitals with invasive cardiac services, and receipt of cardiac procedures by Medicare acute myocardial infarction patients. Health Serv Res. 2013;48(3):1076–1095. | ||
Richman LS, Lattanner MR. Self-regulatory processes underlying structural stigma and health. Soc Sci Med. 2014;103:94–100. | ||
Room R, Rehm J, Paglia A, Ustun TB. Cross cultural views on stigma, valuation, parity, and societal views towards disability. In Ustun TB, editor. Disability and culture. Seattle: Hogrefe & Huber Publishers; 2001:247–291. | ||
Corrigan PW, Bink AB, Schmidt A, Jones N, Rüsch N. What is the impact of self-stigma? Loss of self-respect and the “why try” effect. J Ment Health. 2016;25(1):10–15. | ||
Hasin DS, Grant BF. The National Epidemiologic Survey on Alcohol and Related Conditions (NESARC) Waves 1 and 2: review and summary of findings. Soc Psychiatry Psychiatr Epidemiol. 2015;50(11):1609–1640. | ||
Jakobsson A, Hensing G, Spak F. The role of gendered conceptions in treatment seeking for alcohol problems. Scand J Caring Sci. 2008;22(2):196–202. | ||
Finn SW, Bakshi AS, Andréasson S, Consumption A. Alcohol consumption, dependence, and treatment barriers: perceptions among nontreatment seekers with alcohol dependence. Subst Use Misuse. 2014;49(6):762–769. | ||
Wieczorek Ł. Barriers in the access to alcohol treatment in outpatient clinics in urban and rural community. Psychiatr Pol. 2017;51(1):125–138. | ||
Haighton C, Wilson G, Ling J, McCabe K, Crosland A, Kaner E. A Qualitative study of service provision for alcohol related health issues in mid to later life. PLoS One. 2016;11(2):e0148601. | ||
Neale J, Tompkins C, Sheard L. Barriers to accessing generic health and social care services: a qualitative study of injecting drug users. Health Soc Care Community. 2008;16(2):147–154. | ||
Dyson J. Experiences of alcohol dependence: a qualitative study. J Fam Health Care. 2007;17(6):211–214. | ||
Kozloff N, Cheung AH, Ross LE, et al. Factors influencing service use among homeless youths with co-occurring disorders. Psychiatr Serv. 2013;64(9):925–928. | ||
Notley C, Maskrey V, Holland R. The needs of problematic drug misusers not in structured treatment – a qualitative study of perceived treatment barriers and recommendations for services. Drugs. 2012;19(1):40–48. | ||
Gilchrist G, Moskalewicz J, Nutt R. Understanding access to drug and alcohol treatment services in Europe: a multi-country service users’ perspective. Drugs. 2014;21(2):120–130. | ||
Khadjesari Z, Stevenson F, Godfrey C, Murray E. Negotiating the ‘grey area between normal social drinking and being a smelly tramp’: a qualitative study of people searching for help online to reduce their drinking. Health Expect. 2015;18(6):2011–2020. | ||
Gourlay J, Ricciardelli L, Ridge D. Users’ experiences of heroin and methadone treatment. Subst Use Misuse. 2005;40(12):1875–1882. | ||
Gueta K. A qualitative study of barriers and facilitators in treating drug use among Israeli mothers: an intersectional perspective. Soc Sci Med. 2017;187:155–163. | ||
McCann TV, Mugavin J, Renzaho A, Lubman DI. Sub-Saharan African migrant youths’ help-seeking barriers and facilitators for mental health and substance use problems: a qualitative study. BMC Psychiatry. 2016;16(1):275. | ||
Probst C, Manthey J, Martinez A, Rehm J. Alcohol use disorder severity and reported reasons not to seek treatment: a cross-sectional study in European primary care practices. Subst Abuse Treat Prev Policy. 2015;10(1):32. | ||
Stepanyan K. Methamphetamine Users and Gender Differences in their Acceptance of Long-Term Substance Abuse Treatment Programs. College of Social and Behavioral Sciences, Walden University. 2016. Available from: http://scholarworks.waldenu.edu/dissertations. Accessed November 7, 2018. | ||
Cares A, Pace E, Denious J, Crane LA. Substance use and mental illness among nurses: workplace warning signs and barriers to seeking assistance. Subst Abus. 2015;36(1):59–66. | ||
Green KE. Client-Guided Treatment Development for Problem Drinkers of Various Sexual Orientations. New Brunswick, NJ: Department of Psychology, Rutgers University; 2008. | ||
Tucker JA, Vuchinich RE, Gladsjo JA. Environmental events surrounding natural recovery from alcohol-related problems. J Stud Alcohol. 1994;55(4):401–411. | ||
Allen JL, Mowbray O. Sexual orientation, treatment utilization, and barriers for alcohol related problems: findings from a nationally representative sample. Drug Alcohol Depend. 2016;161:323–330. | ||
Schuler MS, Puttaiah S, Mojtabai R, Crum RM. Perceived barriers to treatment for alcohol problems: a latent class analysis. Psychiatr Serv. 2015;66(11):1221–1228. | ||
Sexton RL, Carlson RG, Leukefeld CG, Booth BM. Barriers to formal drug abuse treatment in the rural south: a preliminary ethnographic assessment. J Psychoactive Drugs. 2008;40(2):121–129. | ||
Hingson R, Mangione T, Meyers A, Scotch N. Seeking help for drinking problems; a study in the Boston Metropolitan Area. J Stud Alcohol. 1982;43(3):273–288. | ||
van der Pol P, Liebregts N, de Graaf R, Korf DJ, van den Brink W, van Laar M. Facilitators and barriers in treatment seeking for cannabis dependence. Drug Alcohol Depend. 2013;133(2):776–780. | ||
Pal HR, Yadav S, Joy PS, Mehta S, Ray R. Treatment nonseeking in alcohol users: a community-based study from North India. J Stud Alcohol. 2003;64(5):631–633. | ||
Zemore SE, Mulia N, Yu Ye, Borges G, Greenfield TK. Gender, acculturation, and other barriers to alcohol treatment utilization among Latinos in three National Alcohol Surveys. J Subst Abuse Treat. 2009;36(4):446–456. | ||
Gates P, Copeland J, Swift W, Martin G. Barriers and facilitators to cannabis treatment. Drug Alcohol Rev. 2012;31(3):311–319. | ||
Wu LT, Blazer DG, Li TK, Woody GE, Lt W, Tk L. Treatment use and barriers among adolescents with prescription opioid use disorders. Addict Behav. 2011;36(12):1233–1239. | ||
Mojtabai R, Chen LY, Kaufmann CN, Crum RM. Comparing barriers to mental health treatment and substance use disorder treatment among individuals with comorbid major depression and substance use disorders. J Subst Abuse Treat. 2014;46(2):268–273. | ||
Jackson A, Shannon L. Examining barriers to and motivations for substance abuse treatment among pregnant women: does urban-rural residence matter? Women Health. 2012;52(6):570–586. | ||
Jackson A, Shannon L. Barriers to receiving substance abuse treatment among rural pregnant women in Kentucky. Matern Child Health J. 2012;16(9):1762–1770. | ||
Bobrova N, Rhodes T, Power R, et al. Barriers to accessing drug treatment in Russia: a qualitative study among injecting drug users in two cities. Drug Alcohol Depend. 2006;82(Suppl 1):S57–S63. | ||
Ayres RM, Eveson L, Ingram J, Telfer M. Treatment experience and needs of older drug users in Bristol, UK. J Subst Use. 2012;17(1):19–31. | ||
Naughton F, Alexandrou E, Dryden S, Bath J, Giles M. Understanding treatment delay among problem drinkers: what inhibits and facilitates help-seeking. Drugs. 2013;20(4):297–303. | ||
Smith SM, Dawson DA, Goldstein RB, Grant BF. Examining perceived alcoholism stigma effect on racial-ethnic disparities in treatment and quality of life among alcoholics. J Stud Alcohol Drugs. 2010;71(2):231–236. | ||
Fortney JC, Tripathi SP, Walton MA, Cunningham RM, Booth BM. Patterns of substance abuse treatment seeking following cocaine-related emergency department visits. J Behav Health Serv Res. 2011;38(2):221–233. | ||
Calabrese SK, Burke SE, Dovidio JF, et al. Internalized HIV and drug stigmas: interacting forces threatening health status and health service utilization among people with HIV who inject drugs in St. Petersburg, Russia. AIDS Behav. 2016;20(1):85–97. | ||
Cellucci T, Krogh J, Vik P. Help seeking for alcohol problems in a college population. J Gen Psychol. 2006;133(4):421–433. | ||
Myers B. Barriers to alcohol and other drug treatment use among Black African and Coloured South Africans. BMC Health Serv Res. 2013;13(1):177. | ||
Myers B, Louw J, Pasche S. Gender differences in barriers to alcohol and other drug treatment in Cape Town, South Africa. Afr J Psychiatry. 2011;14(2):146–153. | ||
Saunders SM, Zygowicz KM, D’Angelo BR. Person-related and treatment-related barriers to alcohol treatment. J Subst Abuse Treat. 2006;30(3):261–270. | ||
Semple SJ, Grant I, Patterson TL. Utilization of drug treatment programs by methamphetamine users: the role of social stigma. Am J Addict. 2005;14(4):367–380. | ||
Conner KO, Rosen D. “You’re nothing but a junkie”: multiple experiences of stigma in an aging methadone maintenance population. J Soc Work Pract Addict. 2008;8(2):244–264. | ||
Browne T, Priester MA, Clone S, Iachini A, Dehart D, Hock R. Barriers and facilitators to substance use treatment in the rural south: a qualitative study. J Rural Health. 2016;32(1):92–101. | ||
Smye V, Browne AJ, Varcoe C, Josewski V. Harm reduction, methadone maintenance treatment and the root causes of health and social inequities: an intersectional lens in the Canadian context. Harm Reduct J. 2011;8(1):17. | ||
Gunn A, Guarino H. “Not human, dead already”: perceptions and experiences of drug-related stigma among opioid-using young adults from the former Soviet Union living in the U.S. Int J Drug Policy. 2016;38:63–72. | ||
Otiashvili D, Kirtadze I, O’Grady KE, et al. Access to treatment for substance-using women in the Republic of Georgia: socio-cultural and structural barriers. Int J Drug Policy. 2013;24(6):566–572. | ||
van Olphen J, Eliason MJ, Freudenberg N, Barnes M. Nowhere to go: how stigma limits the options of female drug users after release from jail. Subst Abuse Treat Prev Policy. 2009;4(1):10. | ||
Small J, Curran GM, Booth B. Barriers and facilitators for alcohol treatment for women: are there more or less for rural women? J Subst Abuse Treat. 2010;39(1):1–13. | ||
Jones LV, Hopson L, Warner L, Hardiman ER, James T. A qualitative study of black women’s experiences in drug abuse and mental health services. Affilia. 2015;30(1):68–82. | ||
Bojko MJ, Mazhnaya A, Makarenko I, et al. “Bureaucracy & beliefs”: assessing the barriers to accessing opioid substitution therapy by people who inject drugs in Ukraine. Drugs. 2015;22(3):255–262. | ||
Lembke A, Zhang N. A qualitative study of treatment-seeking heroin users in contemporary China. Addict Sci Clin Pract. 2015;10(1):23. | ||
Freeman-McGuire M. An Investigation into the Barriers to Treatment and Factors Leading to Treatment and Long-Term Recovery from Substance Abuse among Registered Nurses. Santa Barbara (CA): The Fielding Graduate University. 2010. | ||
Gibbs D, Rae Olmstead K, Brown J, Clinton-Sherrod AM. Dynamics of stigma for alcohol and mental health treatment among army soldiers. Military Psychology. 2011;23:36–51. | ||
Bloom AW. Advances in substance abuse prevention and treatment interventions among racial, ethnic, and sexual minority populations. Alcohol Res. 2016;38(1):47–54. | ||
Schmidt LA. Recent Recent developments in alcohol services research on access to care. Alcohol Res. 2016;38(1):27–33. | ||
Smith LR, Earnshaw VA, Copenhaver MM, Cunningham CO. Substance use stigma: reliability and validity of a theory-based scale for substance-using populations. Drug Alcohol Depend. 2016;162:34–43. | ||
Crapanzano K, Vath RJ, Fisher D. Reducing stigma towards substance users through an educational intervention: harder than it looks. Acad Psychiatry. 2014;38(4):420–425. | ||
Diclemente CC, Schlundt D, Gemmell L. Readiness and stages of change in addiction treatment. Am J Addict. 2004;13(2):103–119. | ||
Hoerster KD, Malte CA, Imel ZE, Ahmad Z, Hunt SC, Jakupcak M. Association of perceived barriers with prospective use of VA mental health care among Iraq and Afghanistan veterans. Psychiatr Serv. 2012;63(4):380–382. |
 © 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2018 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

