Back to Journals » International Medical Case Reports Journal » Volume 13
Retinal Vasculitis with Macular Infarction: A Dengue-related Ophthalmic Complication
Received 24 May 2020
Accepted for publication 7 August 2020
Published 25 August 2020 Volume 2020:13 Pages 363—366
DOI https://doi.org/10.2147/IMCRJ.S264324
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Lalit Agarwal,1 Nisha Agrawal2
1Vitreoretina Department, Biratnagar Eye Hospital, Biratnagar, Nepal; 2Pediatric Ophthalmology and Strabismus Department, Taparia Eye Care, Biratnagar, Nepal
Correspondence: Lalit Agarwal Biratnagar Eye Hospital, Rani, Atithi Marg, Biratnagar, Nepal
Tel +977-9852027817
Email [email protected]
Introduction: Dengue-associated ocular complications are increasing owing to the rising global burden of dengue fever. We intend to highlight a rare and sight-threatening complication of this disease.
Case Details: A 44-year-old male, with prior history of dengue fever, presented with diminution of vision in both eyes for 10 days. At presentation, his best-corrected visual acuity was 1/60 in the right eye and 6/18 in the left eye. Anterior segment findings were unremarkable. Fundus examination revealed vitritis, perivascular exudates, intraretinal hemorrhages, macular edema, peripapillary retinal whitening and cotton wool spots in both eyes suggestive of vasculitis, with additional retinal whitening affecting the right macula. Fundus fluorescein angiography revealed disc and perivascular leakage limited to posterior pole along with patches of blocked fluorescence. In addition, there was capillary nonperfusion due to occlusion of multiple small arterioles supplying the macula of right eye confirming macular ischemia. Macular edema with subretinal fluid in both eyes was evident on optical coherence tomography. Treatment was attempted with intravenous methylprednisolone which was futile even after three days of administration.
Conclusion: We report a case of retinal vasculitis with macular infarction attributed to dengue fever. Although uncommon, dengue-associated ocular complications can lead to irreversible visual loss. Therefore, clinicians should keep this disease entity in mind while evaluating febrile patients with visual complaints in dengue endemic regions.
Keywords: dengue fever, vasculitis, retinal artery occlusion, macular infarction, thrombocytopenia
Introduction
Dengue fever is now endemic in several countries of different WHO regions. America, South-East Asia, and Western Pacific regions are highly influenced. Among them, Asia alone represents 70% of the disease burden.1 The number of individuals affected with this disease has increased by 15-fold in the past two decades, maximum number of cases were reported globally in the year 2019.1 Ophthalmic manifestation of dengue is rare but diverse. The symptoms are usually self-limiting with good recovery of vision.2 Usually the posterior segment of the eye is involved in the form of maculopathy, macular edema, optic neuropathy, vasculitis, and vein occlusion.3 We report a rare ocular complication of dengue fever as bilateral retinal vasculitis with macular ischaemia not responding to systemic steroid and leading to refractory loss of vision.
Case Report
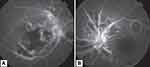
A 44-year-old male presented with sudden onset, diminution of vision in both eyes for 10 days. He gave history of fever, myalgia, and weakness one week prior to onset of ocular problem. He was previously healthy, not known to have diabetes mellitus or hypertension. There was no relevant family or social history of medical significance. During clinical evaluation and laboratory investigation for fever; typhoid, malaria, tuberculosis, syphilis, collagen vascular disease and bleeding disorders were absent. He was diagnosed to have dengue fever as NS1 antigen and IgM antibody were positive. After conservative management, his platelet count had improved from 49⨰103/µL to 176⨰103/µL (normal range, 150–450⨰103/µL) over a week period. At presentation, his best-corrected visual acuity was 1/60 in the right eye (OD) and 6/18 in the left eye (OS). Anterior segment findings were normal. Fundus examination revealed vitritis, perivascular exudates, intraretinal hemorrhages, macular edema, peripapillary retinal whitening, and cotton wool spots in both eyes, with additional retinal whitening affecting the right macula (Figure 1). Fundus fluorescein angiography revealed disc and perivascular leakage limited to posterior pole along with patches of blocked fluorescence. In addition, there was capillary nonperfusion due to occlusion of multiple small arterioles supplying the macula of the right eye confirming macular ischemia (Figure 2). Optical coherence tomography of both eyes demonstrated macular edema with subretinal fluid. A diagnosis of bilateral retinal vasculitis with right eye macular infarction was made. Echocardiography and carotid Doppler studies revealed normal cardiac and carotid artery status. The patient was treated with intravenous methylprednisolone which was futile even after three days of treatment. Then he was counseled for treatment with immunoglobulin, which the patient refused and left for a second opinion without returning back to us.
Discussion
Dengue-associated ocular complications are increasing owing to the rising global burden of this infection.4–9 They can manifest in various forms in the eye. Common presenting symptoms are diminution of vision, scotoma, metamorphopsia, micropsia, altered colour vision, pain, and redness.2,10 Anterior segment involvement of the eye is less common and seen in the form of subconjunctival hemorrhage, uveitis and rarely angle closure glaucoma.2,10 Posterior segment involvement has been reported more frequently in the form of vitritis, maculopathy (10%), vasculitis, chorioretinitis, choroidal effusion, and optic neuropathy.2,3
Many researchers have published many reports of dengue-related ocular involvement in various forms in the recent years.4–9 Cases of branch retinal vein occlusion and rarely isolated retinal artery occlusion have also been found to be associated with dengue fever.6,9 Recent reports have also suggested acute macular neuroretinopathy as a manifestation of dengue maculopathy which can lead to persistent central scotomas.7 Our patient manifested as bilateral retinal vasculitis with multiple macular retinal arteriolar occlusions.
There are many critical determinants in the classification of vasculitis such as etiology (infective and noninfective), caliber of vessels involved (large/medium/small caliber), types of vessel affected (artery/veins/mixed) and level of impedance to blood flow (occlusive or nonocclusive).11,12 A precise categorization is desirable as it can play a crucial role in clinching a diagnosis. Infective causes of vasculitis include viruses like herpes simplex, human immunodeficiency virus, cytomegalovirus, varicella zoster and dengue, syphilis, tuberculosis, and toxoplasmosis.12 Among them, dengue is a rarely encountered infective etiologic cause of vasculitis, affecting both artery and vein.9,12
Retinal vasculitis is also found in association with other forms of noninfective uveitis, eg Vogt–Koyanagi–Harada syndrome or birdshot choroidopathy.12 Rheumatic disorder is a major subset among which Behçet’s disease, multiple sclerosis and sarcoidosis are consistently associated with retinal vasculitis.11,12 Our patient did not have any systemic features suggestive of these diseases.
The pathogenesis behind ocular involvement in dengue fever is not completely understood. Scientists have proposed that these organisms may affect vessels either by direct infiltration or by delayed hypersensitivity to antigens, commonly seen with tuberculosis.13 Arboviruses have a tropism to the central nervous system and small caliber vessels which could be a reason for ocular involvement in dengue fever.13,14 Immune mediated hypersensitivity is a more widely accepted mechanism of affection. Ocular complications usually develop one week after the onset of dengue fever.2,3,9 Similar was the interval in our patient who developed symptoms after a week of onset of fever and at the nadir of thrombocytopenia. This delay is also in favor of the proposed mechanism of immune mediated pathologic process rather than direct invasion by the virus.
Overall, dengue-related ocular complications have a good natural course.2,3,9 Visual recovery is usually seen within one week to three months.2,9 Tan et al reported good visual recovery in a case of dengue-related bilateral retinal vasculitis with macular edema.5 Persistent visual loss can be seen due to extensive macular vasculitis, optic neuropathy, outer retinal damage or foveolitis like acute macular neuroretinopathy.2,7–9 Location of the affected retinal vessel is the most important determinant of visual prognosis.8,11,12 Vasculitis affecting vessels near the macula often affects visual acuity due to edema or infarction, while vasculitis of peripheral retinal vessel may remain asymptomatic for a long time.11,12 OCT angiography study in a case of dengue-related maculopathy has revealed loss of capillaries in the superficial and deep capillary plexus.15 Sharief et al found macular ischemia to increase the risk of vision loss in vasculitis eyes,11 similar to our patient who developed macular infarction leading to irreversible loss of vision.
Spontaneous resolution is common during the course of dengue retinopathy. Persistently symptomatic patients and those with poor or deteriorating vision need intervention.10 The majority of patients respond well to treatment with steroids. Those presenting with posterior segment involvement in the form of vasculitis usually respond to oral prednisolone. Nonresponsive cases, require intravenous methylprednisolone therapy.4,10,16 A rare subset of recalcitrant patients who fail to respond to intravenous steroids, require intravenous immunoglobulin therapy and may show miraculous results with visual gain.3,4 Our patient’s vision unfortunately remained limited despite systemic steroid treatment due to the severity of the retinal involvement. Immunoglobulin trial could not be given to him, which is a limitation of our report.
Conclusion
We report a case of retinal vasculitis with macular infarction attributed to dengue fever. Although uncommon, dengue-associated ocular complications can lead to irreversible visual loss. Therefore, clinicians should keep this disease entity in mind while evaluating febrile patients with visual complaints in dengue-endemic regions.
Ethical Clearance
Ethical approval regarding publication of the case details was obtained from the Institutional Review Board of Biratnagar Eye Hospital.
Patient Consent
Written informed consent for patient information and images to be published was provided by the patient.
Funding
No funding or grant support was received.
Disclosure
The authors report no conflicts of interest in this work.
References
1. World Health Organization. Dengue and severe dengue -Fact sheet. 2020; Available at: https://www.who.int/news-room/fact-sheets/detail/dengue-and-severe-dengue.
2. Yip VC, Sanjay S, Koh YT. Ophthalmic complications of dengue Fever: a systematic review. Ophthalmol Ther. 2012;1(1):2. doi:10.1007/s40123-012-0002-z
3. Ng AW, Teoh SC. Dengue eye disease. Surv Ophthalmol. 2015;60(2):106–114. doi:10.1016/j.survophthal.2014.07.003
4. Bacsal KE, Chee SP, Cheng CL, Flores JV. Dengue associated maculopathy. Arch Ophthalmol. 2007;125:501–510. doi:10.1001/archopht.125.4.501
5. Tan CSH, Teoh SCB, Chan DPL, Wong IBY, Lim TH. Dengue retinopathy manifesting with bilateral vasculitis and macular oedema. Eye. 2007;21:875–877. doi:10.1038/sj.eye.6702748
6. Kanungo S, Shukla D, Kim R. Branch retinal artery occlusion secondary to dengue fever. Indian J Ophthalmol. 2008;56:73–74. doi:10.4103/0301-4738.37606
7. Li M, Zhang X, Ji Y, Ye B, Wen F. Acute macular neuroretinopathy in dengue fever: short-term prospectively followed up case series. JAMA Ophthalmol. 2015;133(11):1329–1333. doi:10.1001/jamaophthalmol.2015.2687
8. Fang PP, Pfau M, Holz FG, Finger RP. Persistent visual loss in dengue fever due to outer retinal damage. Clin Experiment Ophthalmol. 2017;45:747–749. doi:10.1111/ceo.12960
9. Somkijrungroj T, Kongwattananon W. Ocular manifestations of dengue. Curr Opin Ophthalmol. 2019;30(6):500–505. doi:10.1097/ICU.0000000000000613
10. Teoh SC, Chan DP, Nah GK, et al. Eye institute dengue-related ophthalmic complications workgroup. A re-look at ocular complications in dengue fever and dengue haemorrhagic fever. Dengue Bull. 2006;30:184–193.
11. Sharief L, Lightman S, Blum-Hareuveni T, Bar A, Tomkins-Netzer O. Clinical outcome of retinal vasculitis and predictors for prognosis of ischemic retinal vasculitis. Am J Ophthalmol. 2017;177:206–212. doi:10.1016/j.ajo.2017.02.028
12. Rosenbaum JT, Sibley CH, Lin P. Retinal vasculitis. Curr Opin Rheumatol. 2016;28(3):228–235. doi:10.1097/BOR.0000000000000271
13. Yacoub S, Mongkolsapaya J, Screaton G. The pathogenesis of dengue. Curr Opin Infect Dis. 2013;26:284–289. doi:10.1097/QCO.0b013e32835fb938
14. Laurence B, Harold M, Thierry D. Ocular complications of dengue fever. Ophthalmology. 2008;115(6):1100–1101. doi:10.1016/j.ophtha.2008.02.017
15. Tavassoli S, Carreno E, Teoh SC, et al. Optical coherence tomography angiography (OCTA) findings in dengue-related maculopathy: a case report. Ophthalmic Surg Lasers Imaging Retina. 2016;47:1057–1060. doi:10.3928/23258160-20161031-12
16. Lim WK, Mathur R, Koh A, Yeoh R, Chee SP. Ocular manifestations of dengue fever. Ophthalmology. 2004;111(11):2057–2064. doi:10.1016/j.ophtha.2004.03.038
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.