Back to Journals » Journal of Pain Research » Volume 12
Rethinking the criteria for fibromyalgia in 2019: the ABC indicators
Authors Stewart JA , Mailler-Burch S, Müller D, Studer M, von Känel R , grosse Holtforth M, Schwegler K , Egloff N
Received 14 February 2019
Accepted for publication 16 May 2019
Published 10 July 2019 Volume 2019:12 Pages 2115—2124
DOI https://doi.org/10.2147/JPR.S205299
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Michael Schatman
Julian A Stewart,1 Simone Mailler-Burch,1 Darius Müller,1 Martina Studer,1 Roland von Känel,2,3 Martin grosse Holtforth,1,4 Kyrill Schwegler,1 Niklaus Egloff1,2
1Department of Neurology, Bern University Hospital, University of Bern, Bern, Switzerland; 2Department of Clinical Research, Bern University Hospital, University of Bern, Bern, Switzerland; 3Department of Consultation-Liaison Psychiatry and Psychosomatic Medicine, University Hospital Zurich, University of Zurich, Zurich, Switzerland; 4Department of Psychology, University of Bern, Bern, Switzerland
Purpose: Diagnostic criteria for fibromyalgia have been subject to debate and controversy for many years. The preliminary diagnostic criteria introduced in 2010 and 2011 have been criticized for different reasons, including questionable diagnostic specificity and a lack of an etiopathogenetic foundation. The “ABC indicators” presented in this study reflect a further development of the 2011 criteria and refer to (A) algesia, (B) bilateral, axial-symmetric pain distribution, and (C) chronic distress.
Patients and methods: We compared the diagnostic performance of the ABC indicators with that of the 2011 criteria by analyzing the data of 409 inpatients with chronic functional pain divided into two subgroups of pain patients: Those with whole-body pain and those with pain not involving the whole body. Under the premise that FM phenotypically represents a whole-body pain disorder, sensitivity, specificity, correct classification and diagnostic odds ratios were calculated.
Results: The 2011 criteria demonstrated a specificity of 68.1%, a sensitivity of 75.5%, a correct classification of 71.0% and a diagnostic odds ratio of 6.56 (CI: 4.17–10.31). The ABC indicators achieved a specificity of 88.3%, a sensitivity of 62.3%, a correct classification of 78.6%, and a diagnostic odds ratio of 12.47 (CI: 7.30–21.28).
Conclusion: The ABC fibromyalgia indicators demonstrated better specificity, lower sensitivity, and better overall diagnostic effectiveness than the original 2011 criteria.
Keywords: chronic pain, diagnostic criteria, widespread pain, hyperalgesia, psychological distress, Complex Generalized Pain Syndrome (CGPS)
Introduction
The ongoing problem with diagnosing fibromyalgia by the ACR criteria
Since their inception in 1990, criteria for the diagnosis of the fibromyalgia syndrome (FM) have been discussed controversially.1–4 Recent literature has highlighted current uncertainty and skepticism of the diagnosis of FM in the general medical community.5,6 Aiming to overcome previous shortcomings, experts proposed new diagnostic criteria for FM to the American College of Rheumatology (ACR) in 2010, with a revised version subsequently published in 2011.7,8 Both the 2010 and 2011 criteria are based on satisfying one of two numerical cut-off combinations of the Widespread Pain Index (WPI) and the Symptom Severity Score (SSS). The WPI is an inventory of the occurrence of pain in 19 defined body locations. The SSS contains the four items fatigue, non-restorative sleep, cognitive symptoms and an item comprising a multiplicity of other concomitant symptoms.7,8
Even though the 2010/2011 criteria are easy-to-administer, uncertainty remained regarding its clinical validity.9 Concerns raised were a) the lack of any pathophysiological disease concept underlying the criteria; b) exclusive reliance on self-reported symptoms; c) inconclusive recommendations for their use in overlapping rheumatological diseases, and d) insufficient diagnostic specificity and differentiation from localized functional pain syndromes.10
In a previous study, the limitations of the ACR criteria 2010/2011 were examined in relation to other functional pain syndromes.10 By realizing the latter diagnostic deficit of the ACR criteria 2010/2011, Wolfe and colleagues aimed to increase specificity by (re-)defining FM as a generalized pain syndrome in 2016.11,12 Additively to the SSS and WPI scores, they reintroduced a widespread pain criterion (whole-body pain with pain in at least 4 of 5 defined body regions), while retaining the arguably redundant WPI-limit, which overlaps with the reintroduced widespread pain criterion. To summarize, in 2016 FM still appears as a “non-clinical diagnosis”, emerged out of 3 checklists (with many redundancies) and without any visible underlying pathophysiological concept. Therefore, we fear that the acceptance and communicability of FM criteria remain limited.5,6 We believe that despite the ACR’s decision in 2015 “to cease funding and endorsing research on further diagnostic criteria”, the FM diagnosis still needs optimization.13
Alternatives in diagnosing FM are needed
Analogous to the Complex Regional Pain Syndromes (CRPS), we support the paradigm which defines FM as a Complex Generalized Pain Syndrome (CGPS). Neurogenic inflammatory modulation processes have been demonstrated to play a role in both CRPS and FM.14 However, for both pain disorders there is no generally accepted neurochemical surrogate-marker to identify the disorders (yet). Subsequently, the diagnosis must further be made phenotypically. Analogous to the “Budapest Criteria” for CRPS, the “ABC Indicators” presented in this study introduce a method to diagnose FM phenotypically. By retaining the SSS, they reflect a possible further development of the 2011 ACR criteria.
However, before proposing new ways to optimize FM diagnosis, the function of the medical-diagnostic process of FM criteria must undoubtedly be clarified: As experts share the opinion that FM may occur alongside, for example, rheumatological diseases, FM may neither represent an exclusion diagnosis, nor a residual category within rheumatological diseases (Figure 1).12–14
 |
Figure 1 The fibromyalgia syndrome and the ABC indicators within the context of functional pain syndromes and rheumatological diseases. |
Based on the above-mentioned possibility of a comorbid rheumatological disorder, peripheral biomorphologic pain correlates must be identified or ruled out in clinical practice, as is the case with any other complex pain syndrome.
Additionally and independent of this first step, patients should be tested specifically for FM symptoms. In absence of a simple diagnostic surrogate-marker-test for FM, patients should be tested for positive clinical characteristics of FM. These clinical indicators should be in line with the current medical understanding of the syndrome. The combination of the indicators should capture the clinical phenotype of FM as accurately as possible and correctly identify it within the spectrum of other pain syndromes.
ABC indicators refer to the pathophysiology
The current understanding of FM focusses primarily on altered neuronal perception resulting in generalized heightened sensitivity to various stimuli due to changes in the central nervous, neuroendocrine and autonomic nervous systems. 13,15–25 Several neurogenic neuroinflammatory processes may contribute to the Symptoms of FM.14 Some studies also describe additive peripheral nerve dysfunction in some FM subgroups.26 Based on these essential mechanisms of generalized hypersensitivity, the enhanced proprioception of musculoskeletal segments typically occurs in an axial-symmetric (bilateral) pain distribution pattern, similar to muscle pain experienced with influenza (see Figure 2).27
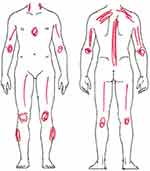 |
Figure 2 Pain drawing example of bilateral axial-symmetric pain distribution. |
Altered stress-related processing likely accounts for the high prevalence of comorbid vegetative, affective and cognitive (psychological) symptoms in FM.25 Recent research demonstrated higher levels of stress to be associated with reduced pressure pain-thresholds.28 In animal models of FM, rodents repeatedly exposed to stress exhibited changing signal pathways in central and peripheral pain processing, resulting in hyperalgesia.29–33 Accordingly, the term stress-induced hyperalgesia has been coined for this crucial pathophysiological link between chronic stress-exposure and generalized pain sensitization in FM.34,35
Based on these pathogenetic mechanisms, the “ABC indicators of FM” circumscribe the following key features of FM:
Indicator A: Algesia (hyperalgesia operationalized through pain pressure algometry),
Indicator B: Bilateral, multilocular, axial-symmetric pain distribution pattern (operationalized through pain drawings or clinical examination), and
Indicator C: Chronic distress symptoms (operationalized through standardized questionnaires or SSS 2011).
In detail, the clinical indicators (A, B, and C) serve slightly different steps in the diagnostic process: (See Figure1). While indicator A (algesia) and indicator C (chronic distress) are also common positive characteristics in other functional pain syndromes (eg irritable bowel syndrome), the additional need for indicator B (bilateral, axial-symmetric pain) aids the selection of FM as generalized pain disorder within this spectrum of functional pain syndromes.36 Due to ubiquitously lowered thresholds in proprioception, FM consequently appears predominantly as “whole-body-pain”, identifiable with its typical multilocular axial-symmetric bilateral pain-pattern.
Methodologically, the concept of the ABC indicators is consistent with recent IMMPACT recommendations explicitly advocating use of various psychosocial and psychophysical (quantitative sensory testing) instruments for phenotyping pain disorders.37
Aims of the present study
To evaluate the diagnostic application of the ABC indicators within the spectrum of functional pain syndromes, we compared the diagnostic parameters of the FM 2011 criteria with the ABC indicators. Since no gold-standard exists to validate different FM-criteria concepts, indirect test methods are implemented: Based on the pathophysiological aspect of generalized hyperalgesia, we predict FM to be a “complex generalized pain syndrome” within the spectrum of functional pain syndromes. This paradigm of generalized pain is congruent with the recent re-adaptations of Wolfe and colleagues in 2016, reintroducing a widespread pain criterion.12,13
More specifically, we aimed to compare ACR criteria 2011 and the ABC indicators in their capacity to select whole-body-pain in a cohort of over 400 patients with functional pain syndromes. We define whole-body-pain as pain in at least 4 of 6 defined body areas (extremities, trunk, and head). We consequently define “false-positive” cases as fulfilling the FM criteria, despite not having whole-body-pain (eg, a patient fulfilling the 2011 FM criteria while only reporting pain in the left arm and right leg would be considered a false-positive case).
In consequence to these premises we expect (I) significantly higher values of the clinical indicators (A, B & C) in the whole-body-pain group compared to the non-whole-body-pain group as well as healthy controls. Since bilateral, axial-symmetric pain distribution (indicator B) is viewed as an explicit key criterion for generalized hyperalgesia, we expect (II) indicator B to be predominantly observed in the whole-body-pain group, in which we assume FM to be represented. Furthermore, as FM is considered a stress-related syndrome, we hypothesize particularly high levels of distress in patients with the whole-body-pain disorders (III). With respect to the ACR criteria 2011 we expect significant correlations between the SSS and other measures of psychological distress (IV).
The aims of the present study are summarized as follows:
- To examine the ABC indicators when comparing the whole-body-pain group to the non-whole-body-pain group
- To examine the rate of bilateral, axial-symmetric pain distributions in the whole-body pain group compared to the non-whole-body-pain group
- To examine the levels of psychological distress in the whole-body-pain group compared to the non-whole-body-pain group
- To examine the association between the SSS and the measures of psychological distress
Materials and methods
Participants
Data were collected from 409 consecutively admitted inpatients with different chronic functional pain syndromes at admission to a multimodal interdisciplinary treatment program in a tertiary university pain clinic as part of a standard clinical assessment. Patients with acute psychosis or severe addiction were excluded from participation in study. Furthermore, patients with primarily neurological or primarily inflammatory diseases were excluded from participation in study. Patients were over 18 years of age, suffered from ≥1 functional pain syndromes. All patients provided written informed consent for the reuse of their health data for research purposes. The study performed in compliance with the Declaration of Helsinki and was approved by the local institutional review board (Kantonale Ethikkomission Bern, 2018–00467). All available information from hospital charts, previous clinical assessments, as well as radiological and serological data were thoroughly reviewed at admission, and further assessments were performed as needed in order to specify the pain syndrome origin.
All patients were examined by internal medicine residents and supervised by board-certified internists and psychiatrists trained in pain medicine. The physicians conducted a structured interview about the patient’s medical history including information on various pain characteristics (intensity, type and dynamics of pain, factors modulating pain intensity, pain localization, concomitant symptoms and effects of analgesics) and rated the Symptom Severity Score (SSS). A second, semi-structured part of the interview focused on demographic data and adverse life events. Psychiatric comorbidities were identified with diagnostic instruments and further validated through observation over the course of inpatient treatment. Diagnoses were classified according to ICD-10 criteria.38
Measures
The German version of the Hospital Anxiety and Depression Scale (HADS) was used for the assessment of anxiety and depression symptoms experienced admission.39 The HADS consists of two scales with seven items each ranging from 0 to 21. Both scores have a cut-off at ≥8 points for clinically relevant symptoms.40 The sum of the anxiety and depression scores can be used to measure “total distress” with a cut-off ≥15.41 The German version of the Brief Symptom Inventory (BSI), containing 53 items, was used to self-rate psychopathological symptoms and emotional distress subscales.42 Cronbach’s alpha yielded good to excellent internal consistency for all scales used in the present study (BSI total: 0.96; BSI anxiety: 0.81; BSI depression: 0.84; HADS total: 0.87; HADS anxiety: 0.80; HADS depression: 0.82).
A standardized and validated pressure-pain provocation test was applied To assess hyperalgesia.43 This method represents a cost-saving and reliable alternative to electronic measurement instruments.44 Since this test is not subject to a patent, it can be implemented and easily reproduced all over the world.43,44 The method is easy-to-administer and has been implemented in several studies.10,27,36,43–45,56 Selected by means of spring balances, the pegs used for pain provocation are set with an exact clamping force of 10N, at an extension of 5 mm (Type Algopeg, size 78×10 mm, polypropylene and nickel). The test is administered at both right and left earlobes (without touching ear cartilage) and middle fingers (without touching the nailfold). After a duration of 10 seconds the peg was removed and patients were asked to report the intensity of the provoked pain on a numerical rating scale (NRS) of 0–10 (0= “no pain”, 10= “most intense pain imaginable”). After computing the average value of the right and left middle fingers and ear lobes, we obtained the following variables: Pain level middle finger (NRS 0–10), pain level earlobe (NRS 0–10). “Hyperalgesia” was defined clinically as a reported pain level of ≥3 at the middle finger or a pain level of ≥8 at the earlobe. This definition of hyperalgesia is based on reference data from 676 healthy subjects. For healthy central European subjects, the mean pain sensitivity at the middle finger is 1.6 (SD 1.5) and the mean pain sensitivity at the earlobe is 5.6 (SD 2.3) (www.algopeg.ch).
Each patient was carefully instructed to provide a detailed pain drawing (PD) of his/her pain sensations. PD is an important and easy-to-administer tool for obtaining additional non-verbal information about an individual’s pain distribution pattern.24 Patients were given an empty body diagram showing the human outlines from all four perspectives (front, back, left, and right). For detailed documentation, PDs additionally included enlarged pictures of the head, hands and feet, shown from different angles. Investigators instructed patients to mark all painful sensations using a red pencil. Patients were free to depict their pain sensations how they felt was most accurate, using lines, circles, crosses, arrows, hatches, solidified areas, etc. PDs were systematically analyzed according to defined variables, which have demonstrated their differential diagnostic utility in previous studies (eg number of marks, length of longest mark, and axial symmetry etc.).27 Examples of variables derived from the pain drawings are: WPI (amount of marks fulfilling WPI criteria) and indicator B (multilocular bilateral pain-patterns) fulfilled, when there were ≥3 pairs of axial-symmetric marks. Different pain distribution pattern categories have been documented in previous literature, upon which predominantly localized pain syndromes (non-whole-body variants) are differentiated from predominantly generalized pain syndromes (whole-body variants) in the present study.27,46 Whole-body pain was defined as pain distribution affecting at least 4 of 6 body segments (including the extremities, trunk and head)
Statistical analyses
SPSS 21 (SPSS Inc., Chicago, IL, USA) was used for statistical analyses. Normal data distribution was tested with the Kolmogorov–Smirnoff test and if not fulfilled, non-parametric statistical analyses were applied. Descriptive statistics were used to compare patient groups on sociodemographic data, clinical symptoms, pain history, and psychiatric comorbidity. Group comparisons for categorical variables used Pearson’s chi-squared test or Fisher’s exact test where appropriate. The Mann–Whitney test or an independent sample t-test was used to compare continuous variables. The significance level was set at p<0.05 (two-tailed). The Pearson product-moment correlations coefficient were used to test associations between SSS, WPI, psychopathological distress scales (HADS; BSI), algometric data and baseline pain measurements. Spearman’s rho correlation coefficients were used for respective non-parametric analyses. Regarding psychometric data, sum or mean scores of subscales and total scores were used respectively. To determine the discriminative ability of the different binary diagnostic sets, diagnostic odds ratios (DOR) and correct classification rates were calculated.47
Results
409 patients with functional pain syndromes were included. Table 1 shows demographic and basic pain characteristics of the sample across both pain distribution subgroups. 169 patients (41.3%) had whole-body pain and 240 patients (58.7%) had non-whole-body pain. Patients with non-whole-body pain had diagnoses such as chronic cervical pain syndromes; atypical chronic limb syndromes; functional pain associated hemi-disorders; quadrant-specific pain syndromes; chronic chest, trunk, or low back pain and chronic tension headache. Additive comorbid pain disorders were chronic temporomandibular disorder; chronic atypical facial pain syndrome; chronic abdominal pain and chronic pelvic pain syndromes. 62.3–75.5% of patients with whole-body pain had FM-like disorders, 1 patient suffered from cenesthesia, the other patients in the whole-body pain group exhibited pain, which was best described as “combinations of several local pain syndromes”. About half of all the patients with functional pain syndromes (196/397, 47.9%) fulfilled the FM criteria when diagnosed with the 2011 criteria, of which 76 (31.9%) represented non-whole-body pain syndromes. Whereas ABC indicators are more selective: Less than a third of all patients with functional pain syndromes (112/360, 31.1%) would receive the FM diagnosis.
 |
Table 1 Health characteristics of 409 patients with functional pain syndromes according to their anatomical pain distribution patterns |
Taking FM as a distinct phenotype with generalized pain, we expected significantly different clinical profiles for whole-body compared to non-whole-body variants. Table 2 shows the results of comparisons on the different indicators. Overall, statistically significant differences emerged among all individual indicators (A, B & C). Generally, the whole-body pain group displayed a significantly higher frequency of symptoms in all areas. Indicator B (bilateral axial symmetric pain pattern) has, as expected, the best effect size (Cohen’s d) to distinguish the whole-body from the non-whole-body group. The non-whole-body pain group showed significantly higher HADS anxiety (p<0.001, d=0.92) and depression (p<0.001, d=0.96) levels compared to healthy normal controls.48 The whole-body pain group also showed significantly higher HADS anxiety (p<0.001, d=1.17) and depression (p<0.001, d=1.07) levels compared to healthy normal controls.48 Yet, between the subgroups, statistically significant differences emerged in all algometric and psychometric aspects except for the depression-scores. Notably, concerning distress (Indicator C), both the HADS and the BSI total scores showed statistically significant differences. With regard to indicator C, the SSS 2011 showed the largest effect for a difference based on Cohen’s d.
 |
Table 2 Differences in FM characteristics between non-whole-body and whole-body variants |
Table 3 displays the correlations of the SSS 2011 with the various measures of distress. All distress measures correlated significantly with the SSS 2011 with values between r =0.3 and 0.42, indicating moderate associations.
 |
Table 3 Pearson correlations among SSS 2011 and indicator C (distress) measures |
Table 4 shows the results of the specificity, sensitivity and DOR in identifying FM using either the FM 2011criteria or the ABC indicators. The specificity of the ABC indicators was substantially higher than that of the FM 2011 criteria, whereas the sensitivity of the ABC indicators was lower than that of the FM 2011 criteria. As a measure of overall diagnostic performance, the diagnostic odds ratio of the ABC indicators was substantially higher than that of the FM 2011 criteria.
 |
Table 4 Sensitivity, specificity, correct classification and DOR |
Discussion
The proposed ABC indicators are a clinically based further development of the 2011 FM criteria. The indicators have been developed based on the current pathophysiological understanding of FM as a complex generalized pain syndrome. “A” stands for Algesia, “B” for Bilateral, axial-symmetric pain distribution, and “C” for Chronic distress.
We evaluated the diagnostic accuracy of the ABC indicators compared to the FM 2011 criteria (WPI and SSS 2011) analyzing data of 409 chronic functional pain patients. The ABC indicators increased the specificity of the FM diagnosis by 20% to 88.3% (compared to 68.1% with the conventional 2011 criteria), and the DOR increased by 90.0% from 6.56 to 12.47, indicating superior diagnostic performance.
Crucially, our data emphasize the notion that FM represents a distinct phenotype within the spectrum of functional pain disorders. Accordingly, patients in the whole-body pain group showed significantly higher pain sensitivity (Indicator A), higher rates of bilateral axial-symmetric pain pattern (Indicator B) and higher levels of distress symptoms (Indicator C), compared to patients with non-whole-body pain (Table 2). Notably, levels of anxiety differed significantly between both groups, too (HADS and BSI). In line with previous findings, high anxiety levels may also be a distinctive feature of FM.49 Finally, the lowered pain, stress, and anxiety thresholds in FM may be expressions of the same underlying central hypersensitivity mechanism.50 Notably, research has established the understanding of the overlap between stress and anxiety in their underlying neurobiological processes, a finding that supports our results.51 Animal models have demonstrated, that the anterior cingulate cortex plays a central role in the sensitization, long-term potentiation, and emulsification of chronic pain and anxiety.52 Exposure to adverse experiences may contribute to the synergetic processes of pain and anxiety in FM.34
The correlations between SSS 2011 and psychological distress measures (HADS, BSI) in this sample additionally corroborates previous research demonstrating significant correlations of SSS 2011 with psychological distress.10 These results support retaining the SSS 2011 as an easy-to-administer clinical screening measure of distress symptoms (Indicator C) within the ABC indicators.
Even if the SSS 2011 appears to be a viable instrument for screening stress-related symptoms (Indicator C), the conventional application of the 2011 FM criteria (WPI and SSS 2011) to our patient sample yielded questionable specificity: Nearly half of all patients with functional pain syndromes were diagnosed with FM, and 2 out of 5 patients with local functional pain syndromes received an FM diagnosis according to the 2011 criteria despite lacking whole-body-pain.
In brief, “generalized pain”, the central aspect upon which our study is methodologically founded, is represented as whole-body-pain in our sample. The proposition to support the notion of “generalized pain” is in line with recent revisions of the ACR FM criteria in 2016.11,12 We emphasize this profile of FM as a generalized pain syndrome in distinction from CRPS, hemi-body pain syndromes, myofascial pain syndromes and many other localized functional pain syndromes.10,53,54 One inclusion can arguably be made regarding early stages of FM, ie incomplete FM Syndromes, which may do not (yet) exhibit a “whole-body” distribution of pain.55 However, we surmise that even incomplete FM syndromes would correspond to our indicators of hyperalgesia (indicator A), bilateral axial-symmetric pain distribution (indicator B), and chronic stress symptoms (indicator C).
A methodological limitation of the ABC indicators is that, similar to the ACR criteria, they rely considerably on patients’ self-report ratings. However, an important difference to the ACR criteria is that indicator A is implemented through a clinical algometric assessment of the patient. A necessary clinical assessment is arguably expedient for a credible classification and subsequent treatment of FM patients.
As a preliminary limitation of the proposed ABC FM indicators we need to emphasize that the present study analyzed data of one sample of inpatients with functional pain disorders, so we cannot yet generalize the diagnostic accuracy to other settings and patient groups. Importantly, the utility of the ABC indicators needs to be further evaluated in outpatient settings and other patient groups (eg orthopedic pain patients) as well, in order to establish generalizability.
Conclusion
With the ABC indicators, the specificity of FM diagnosis is substantially above that of the 2011 criteria, which tend to “over-diagnose” FM. Additionally, while the sensitivity is 13.2% below the 2011 criteria’s sensitivity, the overall discriminative ability (DOR) of the proposed clinical indicators is substantially higher than that of the 2011 criteria. An eminent difference between the 2011 criteria and the proposed ABC indicators lies in its completely different clinical approach: ACR criteria 2011 diagnose FM by exclusion and based on 2 linear scales of self-administered symptoms. In contrast, the ABC indicators regard FM as a tangible and complex clinical disease-entity with generalized hyperalgesia, which should be diagnosed face-to-face by a physician in a structured clinical assessment in search of positive clinical indicators. More importantly, the underlying pathophysiological concept of the ABC indicators allows for a suitable and viable communication of this pain disorder to patients as well as to medical students and health professionals due to its etiopathogenetic underpinning. We hope to stimulate international discourse on the improvement of the understanding of FM through our proposed ABC indicators and encourage future research to investigate their utility and validation in further clinical settings.
In summary, we recommend the following approach for identifying FM:
- Clinical examination and serological or radiological screens for the verification/exclusion of lesion-based or inflammatory comorbid components (according to rheumatology standards).
- Indicator A: Testing for generalized hyperalgesia by quantifying hyper-perceptive components of pain sensation using a standardized algometric measure.
- Indicator B: Examining, eg with pain drawings, the fulfilment of a bilateral axial-symmetric pain distribution (fulfilled, when there are ≥3 pairs of WPI marks).
- Indicator C: Use of the SSS 2011 as a brief Stress Symptom Screen with the cutoff of ≥5. Decide whether a more detailed exploration of psychological distress is required.
- If a patient exhibits all three indicators, the fulfilment of the FM syndrome can be communicated and explained, and care according to current guidelines a multimodal therapy should be recommended.
Acknowledgment
We thank clinical practitioner colleagues for their constructive feedback regarding this project.
Disclosure
NE has developed a method of peg algometry. Importantly, the here implemented method is not patentable (since the peg existed beforehand) and is replicable anywhere without extensive technical effort.43 The authors report no other conflicts of interest in this work.
References
1. Wolfe F, Smythe HA, Yunus MB, et al. The American College of Rheumatology 1990 criteria for the classifcation of Fbromyalgia. Report of the Multicenter Criteria Committee. Arthritis Rheum. 1990;33(2):160–172.
2. Bennett RM, Goldenberg DL. Fibromyalgia, myofascial pain, tender points and trigger points: splitting or lumping? Arthritis Res Ther. 2011;13(3):117. doi:10.1186/ar3357
3. Goldenberg DL. Fibromyalgia syndrome a decade later: what have we learned? Arch Intern Med. 1999;159(8):777–785.
4. Wolfe F. Stop using the American College of Rheumatology criteria in the clinic. J Rheumatol. 2003;30(8):1671–1672.
5. Kumbhare D, Ahmed S, Watter S. A narrative review on the difficulties associated with fibromyalgia diagnosis. Ther Adv Musculoskelet Dis. 2018;10(1):13–26. doi:10.1177/1759720X17740076
6. Kumbhare D, Ahmed S, Sander T, et al. A survey of physicians’ knowledge and adherence to the diagnostic criteria for fibromyalgia. Pain Med. 2017;19(6):1254–1264. doi:10.1093/pm/pnx271
7. Wolfe F, Clauw D, Fitzcharles MA, et al. The American college of rheumatology preliminary diagnostic criteria for fibromyalgia and measurement of symptom severity. Arthritis Care Res. 2010;62(5):600–610. doi:10.1002/acr.20140
8. Wolfe F, Clauw DJ, Fitzcharles MA, et al. Fibromyalgia criteria and severity scales for clinical and epidemiological studies: a modification of the ACR preliminary diagnostic criteria for fibromyalgia. J Rheumatol. 2011;38(6):1113–1122. doi:10.3899/jrheum.100594
9. Smythe HA. Unhelpful criteria sets for ‘diagnosis’ and ‘assessment of severity’ of fibromyalgia. J Rheumatol. 2011;38(6):975–978. doi:10.3899/jrheum.110142
10. Egloff N, von Känel R, Muller V, et al. Implications of proposed fibromyalgia criteria across other functional pain syndromes. Scand J Rheumatol. 2015;44(5):416–424. doi:10.3109/03009742.2015.1010103
11. Wolfe F, Clauw DJ, Fitzcharles MA, et al. 2016 Revisions to the 2010/2011 fibromyalgia diagnostic criteria. Semin Arthritis Rheum. 2016;46(3):319–329. doi:10.1016/j.semarthrit.2016.08.012
12. Wolfe F, Egloff N, Häuser W. Widespread pain and low widespread pain index scores among fibromyalgia positive cases assessed with 2010/2011 fibromyalgia criteria. J Rheumatol. 2016;43(9):1743–1748. doi:10.3899/jrheum.160153
13. Aggarwal R, Ringold S, Khanna D, et al. Distinctions between diagnostic and classification criteria? Arthritis Care Res. 2015;67(7):891–897. doi:10.1002/acr.22583
14. Littlejohn G, Guymer E. Neurogenic inflammation in fibromyalgia. Semin Immunopathol. 2018;40(3):291–300. doi:10.1007/s00281-018-0672-2
15. Fitzcharles MA, Shir Y, Ablin JN, et al. Classification and clinical diagnosis of fibromyalgia syndrome: recommendations of recent evidence-based interdisciplinary guidelines. Evid Based Complement Alternat Med. 2013;2013:528952.
16. Bellato E, Marini E, Castoldi F, et al. Fibromyalgia syndrome: etiology, pathogenesis, diagnosis, and treatment. Pain Res Treat. 2012;2012:426130.
17. López-Solà M, Woo CW, Pujol J, et al. Towards a neurophysiological signature for fibromyalgia. PAIN. 2016;158(1):34–47. doi:10.1097/j.pain.0000000000000707
18. Mease P. Fibromyalgia syndrome: review of clinical presentation, pathogenesis, outcome measures, and treatment. J Rheumatol. 2005;75:6–21.
19. Meeus M, Nijs J. Central sensitization: a biopsychosocial explanation for chronic widespread pain in patients with fibromyalgia and chronic fatigue syndrome. Clin Rheumatol. 2007;26(4):465–473. doi:10.1007/s10067-006-0433-9
20. Staud R, Smitherman ML. Peripheral and central sensitization in fibromyalgia: pathogenetic role. Curr Pain Headache Rep. 2002;6(4):259–266.
21. Sommer C, Alten R, Bär J, et al. Drug therapy of fibromyalgia syndrome. [Article in German]. Schmerz. 2017;31(3):239–245. doi:10.1007/s00482-017-0202-5
22. Yunus MB. Fibromyalgia and overlapping disorders: the unifying concept of central sensitivity syndromes. Semin Arthritis Rheum. 2007;36(6):339–356. doi:10.1016/j.semarthrit.2006.12.009
23. Yunus MB. Central sensitivity syndromes: a new paradigm and group nosology for fibromyalgia and overlapping conditions, and the related issue of disease versus illness. Semin Arthritis Rheum. 2008;37(6):339–352. doi:10.1016/j.semarthrit.2007.09.003
24. Yunus MB. Editorial review: an update on central sensitivity syndromes and the issues of nosology and psychobiology. Curr Rheumatol Rev. 2015;11(2):70–85.
25. Martinez-Lavin M. Biology and therapy of fibromyalgia: stress, the stress response system, and fibromyalgia. Arthritis Res Ther. 2007;9(4):216. doi:10.1186/ar2172
26. Uceyler N, Häuser W, Sommer C. Systematic review with meta-analysis: cytokines in fibromyalgia syndrome. BMC Musculoskelet Disord. 2011;12(1):245. doi:10.1186/1471-2474-12-181
27. Egloff N, Cámara RJ, von Känel R, Klingler N, Marti E, Ferrari ML. Pain drawings in somatoform-functional pain. BMC Musculoskelet Disord. 2012;13(1):257. doi:10.1186/1471-2474-13-63
28. Hven L, Frost P, Bonde JPE. Evaluation of pressure pain threshold as a measure of perceived stress and high job strain. PLoS One. 2017;12(1):e0167257. doi:10.1371/journal.pone.0167257
29. Alvarez P, Green PG, Levine JD. Stress in the adult rat exacerbates muscle pain induced by early-life stress. Biol Psychiatry. 2013;74(9):688–695. doi:10.1016/j.biopsych.2013.04.006
30. Green PG, Chen X, Alvarez P, Ferrari LF, Levine JD. Early-life stress produces muscle hyperalgesia and nociceptor sensitization in the adult rat. PAIN. 2011;152(11):2549–2556. doi:10.1016/j.pain.2011.07.021
31. Khasar SG, Burkham J, Dina OA, et al. Stress induces a switch of intracellular signaling in sensory neurons in a model of generalized pain. J Neurosci. 2008;28(22):5721–5730. doi:10.1523/JNEUROSCI.0256-08.2008
32. Khasar SG, Green PG, Levine JD. Repeated sound stress enhances inflammatory pain in the rat. PAIN. 2005;116(1–2):79–86. doi:10.1016/j.pain.2005.03.040
33. Quintero L, Moreno M, Avila C, Arcaya J, Maixner W, Suarez-Roca H. Long-lasting delayed hyperalgesia after subchronic swim stress. Pharmacol Biochem Behav. 2000;67(3):449–458.
34. Egle UT, Egloff N, von Känel R. [Stress-induced hyperalgesia (SIH) as a consequence of emotional deprivation and psychosocial traumatization in childhood: implications for the treatment of chronic pain]. [Article in German]. Schmerz. 2016;30(6):526–536. doi:10.1007/s00482-016-0107-8
35. Jennings EM, Okine BN, Roche M, Finn DP. Stress-induced hyperalgesia. Prog Neurobiol. 2014;121:1–18. doi:10.1016/j.pneurobio.2014.06.003
36. Egloff N, Cámara RJ, von Känel R, Klingler N, Marti E, Ferrari ML. Hypersensitivity and hyperalgesia in somatoform pain disorders. Gen Hosp Psychiatry. 2014;36(3):284–290. doi:10.1016/j.genhosppsych.2014.01.011
37. Edwards RR, Dworkin RH, Turk DC, et al. Patient phenotyping in clinical trials of chronic pain treatments: IMMPACT recommendations. PAIN. 2016;157(9):1851–1871. doi:10.1097/j.pain.0000000000000602
38. World Health Organization. The ICD-10 Classification of Mental and Behavioural Disorders. Clinical Descriptions and Diagnostic Guidelines. Geneva: World Health Organization; 1992.
39. Herrmann C, Buss U, Snaith RP. [Hospital Anxiety and Depression Scale]. [Manual in German]. Bern: Hans Huber; 1995.
40. Bjelland I, Dahl AA, Haug TT, Neckelman D. The validity of the hospital anxiety and depression scale. An updated literature review. J Psychosom Res. 2002;52(2):69–77.
41. Ibbotson T, Maguire P, Selby P, Priestman T, Wallace L. Screening for anxiety and depression in cancer patients: the effects of disease and treatment. Eur J Cancer. 1994;30(1):37–40. doi:10.1016/S0959-8049(05)80015-2
42. Franke GH. [Brief Symptom Inventory of L.R. Derogatis: Shortform of the SCL-90-R]. [Manual in German]. Weinheim: Belz; 2000.
43. Egloff N, Klingler N, von Känel R, et al. Algometry with a clothes peg compared to an electronic pressure algometer: a randomized cross-sectional study in pain patients. BMC Musculoskelet Disord. 2012;12(1):174. doi:10.1186/1471-2474-12-174
44. Cámara RJ, Merz C, Wegmann B, Stauber S, von Känel R, Egloff N. Cost-saving early diagnosis of functional pain in nonmalignant pain: a noninferiority study of diagnostic accuracy. Pain Res Treat. 2016;2016:5964250.
45. Ferrari MLG, Thuraisingam S, von Känel R, Egloff N. Expectations and effects of a single yoga session on pain perception. Int J Yoga. 2015;8(2):154–157. doi:10.4103/0973-6131.158486
46. Löfvander M, Lindström MA, Masich V. Pain drawings and concepts of pain among patients with “half-body” complaints. Patient Educ Couns. 2007;66(3):353–360. doi:10.1016/j.pec.2007.01.011
47. Glas AS, Lijmer JG, Prins MH, Bonsel GJ, Bossuyt PM. The diagnostic odds ratio: a single indicator of test performance. J Clin Epidemiol. 2003;56(11):1129–1135.
48. Hinz A, Brähler E. Normative values for the hospital anxiety and depression scale (HADS) in the general German population. J Psychosom Res. 2011;71(2):74–78. doi:10.1016/j.jpsychores.2011.01.005
49. Thieme K, Turk DC, Flor H. Comorbid depression and anxiety in fibromyalgia syndrome: relationship to somatic and psychosocial variables. Psychosom Med. 2004;66(6):837–844. doi:10.1097/01.psy.0000146329.63158.40
50. Egloff N, Hirschi A, von Känel R. Traumatization and chronic pain: a further model of interaction. J Pain Res. 2013;6:765–770. doi:10.2147/JPR.S52264
51. Shin LM, Liberzon I. The neurocircuitry of fear, stress, and anxiety disorders. Neuropsychopharmacology. 2009;35(1):169–191.
52. Koga K, Descalzi G, Chen T, et al. Coexistence of two forms of LTP in ACC provides a synaptic mechanism for the interactions between anxiety and chronic pain. Neuron. 2015;85(2):377–389. doi:10.1016/j.neuron.2014.12.021
53. Egloff N, Maecker F, Stauber S, et al. Nondermatomal somatosensory deficits in chronic pain patients: are they really hysterical? Pain. 2012;153(9):1847–1851. doi:10.1016/j.pain.2012.05.006
54. Egloff N, Sabbioni ME, Salathé C, Wiest R, Juengling FD. Nondermatomal somatosensory deficits in patients with chronic pain disorder: clinical findings and hypometabolic pattern in FDG-PET. Pain. 2009;145(1–2):252–258. doi:10.1016/j.pain.2009.04.016
55. Yunus MB, Aldag JC. The concept of incomplete fibromyalgia syndrome: comparison of incomplete fibromyalgia syndrome with fibromyalgia syndrome by 1990 ACR classification criteria and its implications for newer criteria and clinical practice. J Clin Rheumatol. 2012;18(2):71–75. doi:10.1097/RHU.0b013e318247b7da
56. Studer M, Stewart J, Egloff N, et al. Psychosocial stressors and pain sensitivity in chronic pain disorder with somatic and psychological factors (F45.41). Schmerz. 2017;31(1):40–46. doi:10.1007/s00482-016-0159-9
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
