Back to Journals » Risk Management and Healthcare Policy » Volume 7
"It is the left eye, right?"
Authors Pikkel D, Sharabi-Nov A, Pikkel J
Received 15 January 2014
Accepted for publication 21 February 2014
Published 8 April 2014 Volume 2014:7 Pages 77—80
DOI https://doi.org/10.2147/RMHP.S60728
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Dvora Pikkel,1 Adi Sharabi-Nov,2,3 Joseph Pikkel4,5
1Risk Management and Patient Safety Unit, Assuta Hospital, Ramat Hachayal, Tel-Aviv, Israel; 2Research Wing, Ziv Medical Center, Safed, Israel; 3Tel-Hai Academic College, Upper Galilee, Israel; 4Department of Ophthalmology, Ziv Medical Center, Safed, Israel; 5Faculty of Medicine, Bar-Ilan University, Ramat Gan, Tel Aviv, Israel
Objective: Because wrong-site confusion is among the most common mistakes in the operations of paired organs, we have examined the frequency of wrong-sided confusions that could theoretically occur in cataract surgeries in the absence of preoperative verification.
Methods: Ten cataract surgeons participated in the study. The surgeons were asked to complete a questionnaire that included their demographic data, occupational habits, and their approach to and the handling of patients preoperatively. On the day of operation, the surgeons were asked to recognize the side of the operation from the patient's name only. At the second stage of the study, surgeons were asked to recognize the side of the operation while standing a 2-meter distance from the patient's face. The surgeons' answers were compared to the actual operation side. Patients then underwent a full time-out procedure, which included side marking before the operation.
Results: Of the total 67 patients, the surgeons correctly identified the operated side of the eye in 49 (73%) by name and in 56 (83%) by looking at patients' faces. Wrong-side identification correlated with the time lapsed from the last preoperative examination (P=0.034). The number of cataract surgeries performed by the same surgeon (on the same day) also correlated to the number of wrong identifications (P=0.000). Surgeon seniority or age did not correlate to the number of wrong identifications.
Conclusion: This study illustrates the high error rate that can result in the absence of side marking prior to cataract surgery, as well as in operations on other paired organs.
Keywords: wrong site surgery, wrong eye surgery, side marking, time out
Introduction
Though surgical confusions in ophthalmic surgeries are rarely mentioned in the medical literature, the results are always devastating; consequently, much effort has been invested in preventing them.1,2 The American Academy of Ophthalmology published a universal protocol in 2004 to prevent confusions of side in eye surgeries.3 The protocol recommends implementation of a consistent approach before surgeries, such as preoperative verification, site marking, and time-out procedures.
In a review of 106 cases of surgical confusions in ophthalmology, wrong intraocular lens implant occurred in 67, wrong eye surgery or block in 29, and wrong patient or procedure in ten. The author concluded that for 90 cases (84.9%) the confusion would have been prevented had the health care staff followed the universal protocol.4
Although confusion is more likely to happen in emergency operations, the Joint Commission on the Accreditation of Healthcare Organizations reported that 58% of surgical confusion occurred in ambulatory patients and 29% involved inpatients. Wrong-site confusions occurred in 76% of cases. In 13% percent of cases, it was the wrong patient; in 11%, it was the wrong procedure.5
In Canada, the number of lawsuits due to wrong-site surgery decreased by 65% during the 5 years following the implementation of a protocol that instructed orthopedic surgeons to mark operative sites prior to surgery.6 While this demonstrates that surgical confusion is preventable, some surgeons still resist following protocols and underestimate the importance of preventive measures to wrong-site operation. Only 48% of hand surgeons in Canada were found to mark surgical sites preoperatively; those who had made mistakes in the past were the most compliant.6
This study was designed to evaluate the frequency of mistakes that can occur in the absence of preoperative verification.
Methods
Ten cataract surgeons participated in the study. After receiving an explanation of the protocol and signing a consent form, they were asked to complete a questionnaire that accessed data about their age, sex, and seniority, and about their procedure for examining patients before cataract surgery. On the day of the operation, surgeons were asked – before entering the operating theater – to identify which eye was to receive the operation from the patient’s name only. They were then asked to stand at a distance of 2 meters from the patients’ faces (so they could not see which pupil was dilated) and to identify the side to be operated on. Patients then underwent a full time-out procedure, which included marking the operated side.
Statistical analysis was done using the Pearson product-moment correlation coefficient (Rp, between two continuous variables), the Spearman’s rank correlation coefficient (Rs, between two ordinal variables), and the chi-square test (between two binary variables). Values at P<0.05 were considered statistically significant. The study was approved by the local bioethics committee (ZIVHC 64/13).
Results
Ten surgeons participated in the study. Four surgeons were female; six were male. All were senior surgeons with 10–26 years of experience in ophthalmology. The total number of patients operated was 67. The surgeons correctly identified the operated side of the eye in 49 (73%) by the patients’ names (Table 1) and in 56 (83%) by looking at the patients’ faces (Table 2). Only one surgeon was able to identify the correct sides of all his patients by their names. This surgeon operated on five patients on one operating day. Four surgeons were able to do so when seeing their patients’ faces; they operated on few patients on the same day.
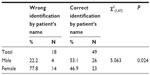  | Table 1 Accuracy of identification of operation side when looking at patients’ names |
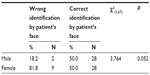  | Table 2 Accuracy of identification of operation side when looking at patients’ faces |
The number of days elapsed from the last preoperative examination correlated positively, with moderate power (Rs =0.671) to errors in identification of the operation side (P=0.034); the closer the last examination was to the operation, the less likely it was for a mistake in identification to occur. Younger surgeons tended to examine the patients closer to the operation day. The surgeons’ age correlated positively, with mild power (Rp =0.246), to the number of days between the last examination day and the operation day (P=0.045). For older surgeons, the time elapsed between the last examination day and the operation day tended to be longer. The number of operations per day correlated positively, and with high power (Rp =0.916), to wrong identification (in both the first and the second stage identifications) of the operation side (P=0.000; Rp =0.916); surgeons who operated more than the others (per day) tended to make more mistakes in identifying the operation side.
The surgeon’s sex, age, and experience did not correlate with the number of wrong-side identifications; experienced and less-experienced surgeons did not differ in their tendency to be wrong in side identification. Surgeons more often made erroneous identifications of women patients (with no correlation to the surgeon’s sex). The surgeons’ demographic data and results of identification of the operated side are given in Table 3.
  | Table 3 Surgeons’ data and results of identifications |
Discussion
Wrong-eye surgery or block occurs in about one-third of surgical confusions.4 Considering that ophthalmic surgeries are only one type of surgery done on paired organs highlights the importance of preoperative marking and time-out procedures.
In this study, well-experienced ophthalmic surgeons were tested for identifying the operation side, by either the patients’ names or by looking at their faces. Both the number of operations per day and the time elapsed from the last examination were found to correlate negatively with the correctly sited side of the operation. It seems expected that busy surgeons who operate on many patients in a day may find it more difficult to remember patients’ details, including the side of the operation. For more experienced surgeons, the time elapsed since their examination of their patients was relatively long. Though we did not find either seniority or experience to correlate directly with the wrong-side identification, this observation does suggest an indirect relationship; experienced surgeons may tend to wrong-side identification due to their tendency to examine patients a relatively long time before the day of operation. Age and sex of the surgeons did not correlate with the wrong-side identification. We do not have an explanation for the greater frequency of wrong-side identification among female patients; we suspect this may be a coincidental finding.
This study created an extreme scenario in which no marking of the operation side was done, no time-out procedure was performed, and the surgeons could not ask the patients which eye was to be operated on. Surgeons were obligated to use their memory alone to identify the side of the operation. Our study clearly shows that surgeons’ memories are no substitute to side marking and the proper time-out procedure, thus highlighting the importance of these two procedures.
Though this study was carried out with cataract surgeons and patients, side marking and time-out procedures are undoubtedly equally important in other paired organ surgeries.
In a recent cross-sectional study that included surgeons, anesthetists, nurse anesthetists, and operating room nurses, 38% of respondents had experienced uncertainty of patient identity, 81% had experienced uncertainty of the surgical site or side, and 60% had prepared for the wrong procedure. In these cases, the operating theater staff started to prepare the wrong equipment or operation site, but they eventually recognized the mistake preoperatively.7 Furthermore, that study found that only nurse anesthetists routinely performed identity checks prior to surgery and that 91% of the surgical team members supported implementation of a time-out protocol in their operating rooms.
In another study conducted in a public hospital, only 3% (three of 100) of the patients had the operation site marked for surgery; one incident of wrong-side surgery was recorded.8
Surgical errors recorded from 2002–2008 in a US medical liability insurance database revealed 107 wrong-site procedures with one death resulting from implantation of a pleural drain on the wrong side. Another 38 patients experienced significant harm (two of them had wrong-sided eye operations).9
The World Health Organization Surgical Safety Checklist and other means have been shown to be effective in preventing such errors, but the adoption of these means by health care professionals is inconsistent.3
The implications of the current study are that the side marking and time-out procedures are crucial to prevent wrong-site operations. In practice, surgical errors involving the wrong patient or wrong body site are preventable, and the operating theater personnel are responsible to follow appropriate protocols. The overall incidence of wrong-site surgeries decreased to one-half (0.14%–0.07%) after implementation of the universal protocol in the US.10 Surgical check lists were found to be effective in preventing these errors.11 Nevertheless, wrong-site surgery was found in 0.09–4.5 per 10,000 surgeries performed.12
There is no doubt that marking the operated side and performing a time-out procedure is a good tool in preventing errors; however, errors still happen, due to an unawareness of the health care staff to the importance of prevention procedures. Continued education and promoting awareness may be of benefit in preventing these adverse events.13
Conclusion
Side marking and time-out procedures are important in preventing wrong-site surgeries. This study shows that relying on surgeons’ memory alone may lead to further errors and wrong-site surgeries. Adhering to regulations, performing side marking, and implementing time-out procedures are all important to reduce these adverse events.
Disclosure
The authors report no conflicts of interest in this work.
References
Meakins JL. Site and side of surgery: getting it right. Can J Surg. 2003;46(2):85–89. French [with English abstract]. | |
Hadden OB. Which procedure, which eye. Clin Exp Ophthalmol. 2002;30(1):60. | |
Joint Commission on the Accreditation of Healthcare Organizations (JCAHO) JCAHO Universal Protocol for preventing wrong site, wrong procedure. JCAHO Perspective on Patient Safety. 2003;3:1–11. | |
Simon JW. Preventing surgical confusions in ophthalmology (an American Ophthalmological Society thesis). Trans Am Ophthalmol Soc. 2007;105:513–529. | |
A follow up review of wrong site surgery. Sentinel Event Alert. 2001;24:1–3. | |
Meinberg EG, Stern PJ. Incidence of wrong-site surgery among hand surgeons. J Bone Joint Surg Am. 2003;85–A(2):193–197. | |
Haugen AS, Murugesh S, Haaverstad R, Eide GE, Søfteland E. A survey of surgical team members’ perceptions of near misses and attitudes towards Time Out protocols. BMC Surg. 2013;13:46. | |
Sayed HA, Zayed M, El Qareh NM, Khafagy H, Helmy AH, Soliman M. Patient safety in the operating room at a governmental hospital. J Egypt Public Health Assoc. 2013;88(2):85–89. | |
Prevention of wrong-site and wrong-patient surgical errors. Prescrire Int. 2013;22(134):14–16. | |
Vachhani JA, Klopfenstein JD. Incidence of neurosurgical wrong-site surgery before and after implementation of the universal protocol. Neurosurgery. 2013;72(4):590–595. | |
Treadwell JR, Lucas S, Tsou AY. Surgical checklists: a systematic review of impacts and implementation. BMJ Qual Saf. Epub January 16, 2014. | |
Devine J, Chutkan N, Norvell DC, Dettori JR. Avoiding wrong site surgery: a systematic review. Spine (Phila Pa 1976). 2010; 35(Suppl 9):S28–S36. | |
Poore SO, Sillah NM, Mahajan AY, Gutowski KA. Patient safety in the operating room: I. Preoperative. Plast Reconstr Surg. 2012;130(5):1038–1047. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
