Back to Journals » Drug Design, Development and Therapy » Volume 13
Quizartinib (AC220): a promising option for acute myeloid leukemia
Received 20 December 2018
Accepted for publication 4 March 2019
Published 8 April 2019 Volume 2019:13 Pages 1117—1125
DOI https://doi.org/10.2147/DDDT.S198950
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Georgios Panos
Fang Zhou, Zheng Ge, Baoan Chen
Department of Hematology and Oncology (Key Department of Jiangsu Medicine), Zhongda Hospital, Medical School, Southeast University, Nanjing, Jiangsu Province, People’s Republic of China
Abstract: Quizartinib is an effective therapy for patients with FLT3-ITD acute myeloid leukemia (AML) by continuing to inhibit the activity of FLT3 gene, leading to apoptosis of tumor cells. Multiple clinical trials have proved that it is effective in relapsed or refractory AML with an FLT3-ITD mutation. In this review, we focus on the characteristics of FLT3/ITD mutations, the mechanism and pharmacokinetics of quizartinib, and the mechanisms of resistance to quizartinib. We also summarize clinical experiences and adverse effects with quizartinib and recommend crucial approaches of quizartinib in the therapy of patients with newly diagnosed AML and patients with relapsed/refractory AML, particularly those with FLT3-ITD mutation. Quizartinib presents its advantages as a very promising agent in the treatment of AML, especially in patients with FLT3-ITD mutations. FLT3/ITD mutation can lead to constitutive autophosphorylation of FLT3 and activation of its downstream effectors including RAS/RAF/MEK, MAPK/ERK, PI3K/AKT/mTOR and JAK/STAT5 signal pathways, while Quizartinib can inhibit these downstream pathways through specific FLT3 inhibition. Quizartinib has received US Food and Drug Administration breakthrough therapy designation in patients with relapsed/refractory FLT3-ITD AML based on clinical trials. A larger sample of clinical trials are needed to verify its safety and efficacy, and the efficacy of quizartinib combined with chemotherapy or allogeneic hematopoietic cell transplantation should also be estimated in clinical trials. Meanwhile, for the side effects of quizartinib, further studies are needed to find a way to reduce its toxicity.
Keywords: quizartinib, FLT3 inhibitor, FLT3-ITD mutation, AML, clinical trials, targeted therapy
Introduction
Acute myeloid leukemia (AML) is a heterogeneous disease characterized by multiple genetic aberrations.1 Some progress has been made in the pathogenesis of AML in recent years, there is a deeper understanding in molecular biology, immunology, clinical features and prognosis. Some breakthroughs have been made in the treatment of AML compared with the past. Traditional treatment regimens include the so-called “7+3” regimen, specifically 7 days of cytarabine +3 days of daunorubicin, and the 5-year survival rate of AML patients is still not optimistic. Besides, due to age and health conditions, many elderly patients find it difficult to adhere to the “7+3” treatment.2–4 Studies have shown that venetoclax in combination with the hypomethylating regimen can be used for the treatment of AML patients who ineligible for standard induction chemotherapy, with high response rate and long duration. Venetoclax in combination with the hypomethylating agent was approved by the US Food and Drug Administration (FDA) as a new treatment for the elderly.5,6 Moreover, approximately 20–30% of AML patients carry an internal tandem duplication (ITD) mutation in the FLT3 gene, carrying a dismal prognosis,7 and is considered as one of the adverse risk groups in the 2017 European LeukemiaNet risk stratification.8 All of these bring great challenges to the treatment of AML.
Quizartinib, a specific oral FLT3 inhibitor which can continue inhibiting the activity of FLT3 gene, leading to apoptosis of tumor cells.9–12 Currently, it has been granted as fast-track status to treat recurrent/refractory AML, as well as orphan status to treat AML by the US FDA and the European Drug Administration. In multiple clinical trials, quizartinib has shown its efficiency and security in patients with relapsed/refractory FLT3-ITD mutant AML or patients who have undergone transplantation or a second-line treatment.13,14 In this review, we address the characteristics of FLT3/ITD mutations, the mechanisms and pharmacokinetics of quizartinib and the mechanisms of resistance to quizartinib. We also review clinical studies and adverse effects with quizartinib and suggest critical approaches of quizartinib in the treatment of relapsed/refractory AML.
Characteristics of FLT3 mutations
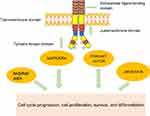
The human FLT3 gene (Fms Related Tyrosine Kinase 3) is a Protein-Coding gene which is located on band 13q12 and organized in 24 exons, and is ordinarily only expressed in primitive hematopoietic precursors, plays an important role in normal growth and differentiation of hematopoietic antecedent cells.15–18 It encodes a protein of 993 amino acids with four domains19,20 (Figure 1). Several different mutations can occur in the FLT3 gene and the ITD mutation on exon 14 is the most common mutation, which occurs in about 23% of de novo AML patients.21,22 ITD mutations occur in the juxtamembrane region of the receptor, which can damage its negative regulatory function, resulting in constitutive autophosphorylation of FLT3 and activation of its downstream effectors including RAS/RAF/MEK, MAPK/ERK, PI3K/AKT/mTOR and JAK/STAT5 signal pathways, all of which plays a significant role in the development of cell cycle progression, cell proliferation, survival, and differentiation, and cooperates with other recurrent molecular abnormalities to induce acute leukemia.21,23–28 ITD mutations range in length from 3 to 400 base pairs. It has been reported that the length of the ITD mutation has prognostic significance, and there is a correlation between the increase in ITD length and the decrease in overall survival.18,29,30
Mechanism and pharmacokinetics of quizartinib
FLT3 is an essential therapeutic target for the treatment of AML.31–35 It is a member of class III receptor tyrosine kinase family and is generally only expressed in primordial hematopoietic ancestors within the bone marrow.36,37 Tyrosine kinase inhibitors were incipiently developed for the therapy of solid neoplasms. The original intention of the researchers was to inhibit other kinases but then stumbled upon that they could also inhibit the activity of FLT3 gene. Therefore, in addition to inhibiting FLT3, the original tyrosine kinase inhibitors also inhibit other various kinases, resulting in poor specificity, high toxic side effects and low efficacy when used in the treatment of FLT3-ITD AML. And previous experiments have also shown that the pharmacokinetics of the first-generation tyrosine kinase inhibitors are not ideal enough to continue to exert inhibition.18,38,39 In order to solve the problem of tyrosine kinase production, the second generation of tyrosine kinase came into being. Quizartinib is the first drug designed as a selective FLT3 inhibitor with better pharmacokinetic characteristics, high specificity, more effective, better tolerance and other characteristics.30,40,41 The mechanism of quizartinib is that binding to FLT3 tyrosine kinase receptor isoform, thus leading to the inhibition of cancer cell proliferation and causes cancer cell death.38,42
Quizartinib is a selective and efficient FLT3 inhibitor with IC50 ≤1 nmol/L.43 Its half-life is relatively long, approximately more than 1.5 days.43 AC886 is a pharmacologically effective metabolite of quizartinib, which was recognized in early experiments. Like quizartinib, their systemic exposure was dose-dependent.43–45 Existing clinical trials have shown that for R/R AML patients, the maximum tolerated dose of quizartinib administered continuously is 200 mg/day. Previous clinical trials have also found that quizartinib can achieve plasma concentrations of 500–1000 nmol/L when administered at a dose of 60 mg/day, which can achieve continuous inhibition of FLT3-ITD phosphorylation in vivo.43,46
Preclinical studies
In the leukemia cell lines with a homozygous FLT3-ITD mutation and cell lines which expresse wild-type FLT3, AC220 has been proved to restrain FLT3 autophosphorylation and cell proliferation. In vivo, AC220 can significantly prolong survival at a dose of 1 mg/kg orally once a day and eradicate tumors at 10 mg/kg. It has also been demonstrated to inhibit FLT3 activity in primary leukemia cells. In a preclinical model using immortalized MV4-11 cells, quizartinib-treated mice showed rapid and complete tumor regression. In another leukemia model transplanted into the bone marrow, quizartinib achieved an increase in overall survival at 10 mg/kg, which was 25% longer than the control group.44
Clinical studies
AC220 has been studied in a number of clinical trials as a single drug, as well as in combination with chemotherapy drugs for the treatment of AML and satisfactory results have been reported in multiple clinical trial centers.47–53 (Tables 1 and 2)
 | Table 1 Summary of clinical trials using quizartinib as single agent |
 | Table 2 Summary of clinical trials of quizartinib in combination with chemotherapy |
Phase I
In a Phase I study,quizartinib was given as a single agent, 6 healthy male volunteers were treated at a dose of 60 mg oral solution, and the study confirmed that quizartinib has excellent safety and tolerance in healthy men.49 In another Phase I, multicenter dose-escalation research, Jorge et al conducted quizartinib at an escalating dose of 12–450 mg/day in 28-day cycles to 76 patients with R/R AML. Concomitant use of hydroxyurea was allowed for up to 5 days during the first 28 days of this study, up to a maximum dose of 5 g/day. This study revealed that the maximum-tolerated dose (MTD) was 200 mg/day.43 Besides, another Phase 1 study administered by Altman et al demonstrated that the MTD was 60 mg/day when combined with induction and strengthening chemotherapy.47 In another Phase I clinical trial of quizartinib monotherapy, quizartinib was used for supporting therapy in patients with AML after allogeneic hematopoietic stem cell transplantation. In this clinical trial, quizartinib was given orally in a 28-day cycle up to 24 cycles and the maximum dose of quizartinib for constant daily treatment is 60 mg.14 All of these clinical studies have shown that quizartinib has good tolerance and controllable safety. Whether as a single drug or in combination with chemotherapy or as supporting therapy after allogeneic hematopoietic stem cell transplantation, quizartinib showed a promising antileukemia activity in newly diagnosed AML patients and R/R AML patients, especially those with FLT3-ITD mutations.
Phase II
There have been six Phase II clinical studies of quizartinib for AML, five of them were for AML carrying the FLT3-ITD mutation and two were for relapsed/refractory AML. Furthermore, one of the six clinical trials have been completed and the other five are underway. Jorge et al divided 333 patients with relapsed/refractory AML into two groups to evaluate the effect of quizartinib. Patients aged 60 or older who received first-line treatment within 1 year were listed in group 1, and those aged 18 or older who received salvage chemotherapy or hematopoietic stem cell transplantation were listed in group 2, FlT3-ITD mutation was detected among all patients; the doses of quizartinib were 135 mg/d for male and 90 mg/d for female in 28-day treatment cycles continued until relapse. Among 332 evaluable patients, the composite complete remission rates were similar in patients with FLT3-ITD-positive and those with less than 10% allelic frequency, but lower in those with undetectable FLT3-ITD mutations (Figure 2). In patients with positive FLT3-ITD mutation, the median total survival was similar between the two groups, with 25+4 weeks in the first group and 24 weeks in the second group.50
In another randomized, open-label, two dosing regimens, Phase IIb clinical trial, the potency and security of quizartinib were estimated in 76 relapsed/refractory AML patients with FLT3-ITD mutations who had previously experienced a second-line remedial treatment or had received transplantation, and these patients were scheduled to take quizartinib at a dose of 30 mg or 60 mg per day according to randomization. The results demonstrated that the composite complete remission rates were 47% in both groups. The bridge to graft rate for the two group patients was 32% and 42%, the continuation of composite complete remission was 4.2 and 9.1 weeks and the median overall survival time was 20.9 and 27.3 weeks, respectively. It showed that a daily dose of 60 mg is more effective than a daily dose of 30 mg.51
Phase III
The current Phase III clinical trials of quizartinib as a promising drug for AML, compared the efficacy of quizartinib with induction/consolidation chemotherapy and salvage chemotherapy and further assessed the potency of quizartinib in maintenance treatment. A Phase III clinical trial conducted by Schlenk et al demonstrated that patients receiving quizartinib had a 24% lower risk of death than those receiving salvage chemotherapy. The median total survival time of patients receiving salvage chemotherapy was 6.2 months (95% CI 5.3–7.2 on both sides), and 4.7 months for patients receiving quizartinib (95% CI 4.0–5.5 on both sides). The 1-year survival rate for quizartinib was 27%, compared with 20% for patients receiving salvage chemotherapy.55
Mechanisms of resistance to quizartinib
Ordinarily, resistance to FLT3 inhibitors gives rise to treatment failure.56 Data obtained from clinical trials applying FLT3-TKI monotherapy illustrate the existence of primary resistance in almost 30% of FLT3-mutated AML patients.57 Current data have revealed that high expression of RUNX1 is one inference for emerging quizartinib-resistant FLT3/ITD+ cells. When RUNX1 was silenced, the emergence and proliferation of quizartinib-resistant FLT3/ITD+ cells became ineffective while quizartinib was applied.58
Some researchers have shown that re-activation of downstream FGF/Ras/ERK and Wnt signaling as a significant mechanism of resistance to quizartinib.59 FGF2 promoted resistance by activating FGFR1 and downstream MAPK effectors.60 p21Cdkn1a (p21) and pre-B cell leukemia transcription factor 1 (Pbx1), which can inhibit the proliferation of FLT3-ITD cells, are also important pathways involved in quizartinib resistance.61
The effect of FLT3 kinase domain mutation on drug resistance may be due to the disturbance of protein inactivation, which is necessary for drug binding, resulting in a reduction in drug affinity to mutant.62 The co-crystal structure of FLT3-quizartinib suggests that the combination of quizartinib depends on the basic aromatic interactions with the gatekeeper F691 residue and F830. Any changes in F691 and F830 may result in a significant loss of binding affinity.63 Furthermore, in most AML patients, FLT3-ITD mutations are activated when acquiring resistance to the FLT3 inhibitor quizartinib, accompanying enormous clonal diversity. Besides, great ancestral heterogeneity also destroys the response to the targeted therapeutics with quezatinib.56
Adverse effect
Quezatinib produces adverse effects, although it is reported to be ordinarily well tolerated by patients. But the adverse effects were considered manageable. Common adverse effects included febrile neutropenia, neutropenia, thrombocytopenia, anemia and QTcF prolongation.47,64–66
Conclusion and future directions
Quizartinib is an effective therapy for patients with FLT3-ITD AML, continuing to inhibit the activity of FLT3 gene, leading to apoptosis of tumor cells. In clinical trials, quizartinib presents its advantages as a very promising agent in the treatment of AML, though some side effects still happened in patients, and there was quizartinib resistance in clinical treatment. We mentioned that the high expression of RUNX1 leads to the emergence of quizartinib-resistant FLT3/ITD+ cells, so the development of targeted drugs for RUNX1 and the combination with quizartinib are the future considerations. In addition, it is worth noting that 30% of the FLT-WT cases have shown benefit with quizartinib therapy and so identifying a predictive biomarker of response in this population should become next focus. Furthermore, a larger sample of clinical trials is needed to verify its safety and efficacy, and the efficacy of quizartinib combined with chemotherapy or allogeneic hematopoietic cell transplantation should also be estimated in clinical trials. Meanwhile, for the side effects of quizartinib, further studies are needed to find a way to reduce its toxicity.
Acknowledgment
This work was supported by the National Natural Science Foundation of China (grant numbers 81170492 and 81370673), National High Technology Research and Development Program 863 of People’s Republic of China (grant number 2012AA022703), National Key Basic Research Program 973 of People’s Republic of China (grant number 2010CB732404), Key Medical Projects of Jiangsu Province (grant number BL2014078), Key Medical of Jiangsu Province (grant number ZDXKB2016020), Jiangsu Social Development Project (grant number BE2018711), and Postgraduate Research & Practice Innovation Program of Jiangsu Province (grant number SJCX18-0068).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Kornblau SM, Womble M, Qiu YH, et al. Simultaneous activation of multiple signal transduction pathways confers poor prognosis in acute myelogenous leukemia. Blood. 2006;108(7):2358–2365. Epub 2006/06/10. doi:10.1182/blood-2006-02-003475
2. Dohner H, Estey EH, Amadori S, et al. Diagnosis and management of acute myeloid leukemia in adults: recommendations from an international expert panel, on behalf of the European LeukemiaNet. Blood. 2010;115(3):453–474. Epub 2009/11/03. doi:10.1182/blood-2009-07-235358
3. Dohner H, Weisdorf DJ, Bloomfield CD. Acute myeloid leukemia. N Engl J Med. 2015;373(12):1136–1152. Epub 2015/09/17. doi:10.1056/NEJMra1406184
4. Yang X, Wang J. Precision therapy for acute myeloid leukemia. J Hematol Oncol. 2018;11(1):3. Epub 2018/01/06. doi:10.1186/s13045-017-0543-7
5. DiNardo CD, Pratz KW, Letai A, et al. Safety and preliminary efficacy of venetoclax with decitabine or azacitidine in elderly patients with previously untreated acute myeloid leukaemia: a non-randomised, open-label, phase 1b study. Lancet Oncol. 2018;19(2):216–228. doi:10.1016/S1470-2045(18)30010-X
6. Mei M, Aldoss I, Marcucci G, Pullarkat V. Hypomethylating agents in combination with venetoclax for acute myeloid leukemia: update on clinical trial data and practical considerations for use. Am J Hematol. 2019;94(3):358–362. doi:10.1002/ajh.25369
7. Song Y, Magenau J, Li Y, et al. FLT3 mutational status is an independent risk factor for adverse outcomes after allogeneic transplantation in AML. Bone Marrow Transplant. 2016;51(4):511–520. Epub 2015/ 07/21. doi:10.1038/bmt.2015.170
8. Dohner H, Estey E, Grimwade D, et al. Diagnosis and management of AML in adults: 2017 ELN recommendations from an international expert panel. Blood. 2017;129(4):424–447. Epub 2016/11/30. doi:10.1182/blood-2016-08-733196
9. Ouchida AT, Li Y, Geng J, et al. Synergistic effect of a novel autophagy inhibitor and Quizartinib enhances cancer cell death. Cell Death Dis. 2018;9(2):138. Epub 2018/01/28. doi:10.1038/s41419-017-0170-9
10. Zorn JA, Wang Q, Fujimura E, Barros T, Kuriyan J. Crystal structure of the FLT3 kinase domain bound to the inhibitor Quizartinib (AC220). PLoS One. 2015;10(4):e0121177. Epub 2015/04/04. doi:10.1371/journal.pone.0121177
11. Larrue C, Saland E, Boutzen H, et al. Proteasome inhibitors induce FLT3-ITD degradation through autophagy in AML cells. Blood. 2016;127(7):882–892. Epub 2015/08/20. doi:10.1182/blood-2015-05-646497
12. Kapoor S, Natarajan K, Baldwin PR, et al. Concurrent inhibition of pim and FLT3 kinases enhances apoptosis of FLT3-ITD acute myeloid leukemia cells through increased Mcl-1 proteasomal degradation. Clin Cancer Res. 2018;24(1):234–247. Epub 2017/ 10/28. doi:10.1158/1078-0432.ccr-17-1629
13. Fleischmann M, Schnetzke U, Schrenk KG, et al. Outcome of FLT3-ITD-positive acute myeloid leukemia: impact of allogeneic stem cell transplantation and tyrosine kinase inhibitor treatment. J Cancer Res Clin Oncol. 2017;143(2):337–345. doi:10.1007/s00432-016-2290-5
14. Sandmaier BM, Khaled S, Oran B, Gammon G, Trone D, Frankfurt O. Results of a phase 1 study of quizartinib as maintenance therapy in subjects with acute myeloid leukemia in remission following allogeneic hematopoietic stem cell transplant. Am J Hematol. 2018;93(2):222–231. doi:10.1002/ajh.24959
15. Carow CE, Kim E, Hawkins AL, et al. Localization of the human stem cell tyrosine kinase-1 gene (FLT3) to 13q12–>q13. Cytogenet Cell Genet. 1995;70(3–4):255–257. doi:10.1159/000134046
16. Vandergeer P, Hunter T, Lindberg RA. Receptor protein-tyrosine kinases and their signal-transduction pathways. Annu Rev Cell Biol. 1994;10:251–337. doi:10.1146/annurev.cellbio.10.1.251
17. Rosnet O, Buhring HJ, de Lapeyriere O, et al. Expression and signal transduction of the FLT3 tyrosine kinase receptor. Acta Haematol. 1996;95(3–4):218–223. doi:10.1159/000203881
18. Wander SA, Levis MJ, Fathi AT. The evolving role of FLT3 inhibitors in acute myeloid leukemia: quizartinib and beyond. Ther Adv Hematol. 2014;5(3):65–77. doi:10.1177/2040620714532123
19. Small D, Levenstein M, Kim E, et al. Stk-1, the human homolog of Flk-2/Flt-3, is selectively expressed in Cd34(+) human bone-marrow cells and is involved in the proliferation of early progenitor stem-cells. Proc Natl Acad Sci USA. 1994;91(2):459–463. doi:10.1073/pnas.91.2.459
20. Gu JY, Gu X. Natural history and functional divergence of protein tyrosine kinases. Gene. 2003;317(1–2):49–57. doi:10.1016/S0378-1119(03)00696-6
21. Levis M, Small D. FLT3: iTDoes matter in leukemia. Leukemia. 2003;17(9):1738–1752. doi:10.1038/sj.leu.2403099
22. Kiyoi H, Ohno R, Ueda R, Saito H, Naoe T. Mechanism of constitutive activation of FLT3 with internal tandem duplication in the juxtamembrane domain. Oncogene. 2002;21(16):2555–2563. doi:10.1038/sj/onc/1205332
23. Kiyoi H, Towatari M, Yokota S, et al. Internal tandem duplication of the FLT3 gene is a novel modality of elongation mutation which causes constitutive activation of the product. Leukemia. 1998;12(9):1333–1337. doi:10.1038/sj.leu.2401130
24. Griffith J, Black J, Faerman C, et al. The structural basis for autoinhibition of FLT3 by the juxtamembrane domain. Mol Cell. 2004;13(2):169–178. doi:10.1016/S1097-2765(03)00505-7
25. Hay N, Sonenberg N. Upstream and downstream of mTOR. Gene Dev. 2004;18(16):1926–1945. doi:10.1101/gad.1212704
26. Roux PP, Blenis J. ERK and p38 MAPK-activated protein kinases: a family of protein kinases with diverse biological functions. Microbiol Mol Biol Rev. 2004;68(2):320–344. doi:10.1128/MMBR.68.2.320-344.2004
27. Bar-Natan M, Nelson EA, Xiang M, Frank DA. STAT signaling in the pathogenesis and treatment of myeloid malignancies. JAKSTAT. 2012;1(2):55–64. doi:10.4161/jkst.20006
28. Hassanein M, Almahayni MH, Ahmed SO, Gaballa S, El Fakih R. FLT3 inhibitors for treating acute myeloid leukemia. Clin Lymphoma Myeloma Leuk. 2016;16(10):543–549. doi:10.1016/j.clml.2016.06.002
29. Schnittger S, Schoch C, Dugas M, et al. Analysis of FLT3 length mutations in 1003 patients with acute myeloid leukemia: correlation to cytogenetics, FAB subtype, and prognosis in the AMLCG study and usefulness as a marker for the detection of minimal residual disease. Blood. 2002;100(1):59–66. doi:10.1182/blood.V100.1.59
30. Swords R, Freeman C, Giles F. Targeting the FMS-like tyrosine kinase 3 in acute myeloid leukemia. Leukemia. 2012;26(10):2176–2185. doi:10.1038/leu.2012.114
31. Kindler T, Lipka DB, Fischer T. FLT3 as a therapeutic target in AML: still challenging after all these years. Blood. 2010;116(24):5089–5102. doi:10.1182/blood-2010-04-261867
32. Stockard B, Guingab J, Garrett T, Pounds S, Rubnitz JE, Lamba J. Global and targeted metabolic profiling identifies metabolic markers for FLT3-ITD in pediatric AML patients. Blood. 2017;130. PubMed PMID:WOS:000432419705282.
33. Small D. FLT3: biology and molecular targeting to improve outcome in AML. Pediatr Blood Cancer. 2017;64:S2–S.
34. Adamia S, Nemeth J, Bhatt S, et al. FLT3 Splice Variant (FLT3Va) as a potential immunotherapeutic target in patients with Acute Myeloid Leukemia (AML). Blood. 2016;128(22). doi:10.1182/blood-2016-06-724161
35. Dany M, Gencer S, Nganga R, et al. Targeting FLT3-ITD signaling mediates ceramide-dependent mitophagy and attenuates drug resistance in AML. Blood. 2016;128(15):1944–1958. doi:10.1182/blood-2016-04-708750
36. Kazi JU, Chougule RA, Li TF, et al. Tyrosine 842 in the activation loop is required for full transformation by the oncogenic mutant FLT3-ITD. Cell Mol Life Sci. 2017;74(14):2679–2688. doi:10.1007/s00018-017-2494-0
37. Matthews W, Jordan CT, Gw W, Pardoll D, Lemischka IR. A receptor tyrosine kinase specific to hematopoietic stem and progenitor cell-enriched populations. Cell. 1991;65(7):1143–1152.
38. Ostronoff F, Estey E. The role of quizartinib in the treatment of acute myeloid leukemia. Expert Opin Investig Drugs. 2013;22(12):1659–1669. doi:10.1517/13543784.2013.842973
39. Grunwald MR, Levis MJ. FLT3 inhibitors for acute myeloid leukemia: a review of their efficacy and mechanisms of resistance. Int J Hematol. 2013;97(6):683–694. doi:10.1007/s12185-013-1334-8
40. Chao Q, Sprankle KG, Grotzfeld RM, et al. Identification of N-(5-tert-Butyl-isoxazol-3-yl)-N ‘-{4-[7-(2-morpholin-4-yl-ethoxy)imidazo[2,1-b][1,3]benzothiazol-2-yl]phenyl}urea Dihydrochloride (AC220), a uniquely potent, selective, and efficacious FMS-Like Tyrosine Kinase-3 (FLT3) inhibitor. J Med Chem. 2009;52(23):7808–7816. doi:10.1021/jm9007533
41. Hills RK, Gammon G, Trone D, Burnett AK. Quizartinib significantly improves overall survival in FLT3-ITD positive AML patients relapsed after stem cell transplantation or after failure of salvage chemotherapy: a comparison with historical AML database (UK NCRI data). Blood. 2015;126(23). PubMed PMID: WOS:000368020102069.
42. Papadopoulos KP, Ben-Ami E, Patnaik A, Trone D, Li JK, Demetri GD. Safety and tolerability of quizartinib, a FLT3 inhibitor, in advanced solid tumors: a phase 1 dose-escalation trial. BMC Cancer. 2018;18(1):790. doi:10.1186/s12885-018-4242-8
43. Cortes JE, Kantarjian H, Foran JM, et al. Phase I study of quizartinib administered daily to patients with relapsed or refractory acute myeloid leukemia irrespective of FMS-like tyrosine kinase 3-internal tandem duplication status. J Clin Oncol. 2013;31(29):
44. Zarrinkar PP, Gunawardane RN, Cramer MD, et al. AC220 is a uniquely potent and selective inhibitor of FLT3 for the treatment of acute myeloid leukemia (AML). Blood. 2009;114(14):2984–2992. doi:10.1182/blood-2009-05-222034
45. Smith CC, Wang Q, Chin CS, et al. Validation of ITD mutations in FLT3 as a therapeutic target in human acute myeloid leukaemia. Nature. 2012;485(7397):260–U153. doi:10.1038/nature11016
46. Levis MJ, Cortes JE, Gammon GM, Trone D, Kang DW, Li JK. Laboratory and clinical investigations to identify the optimal dosing strategy for quizartinib (AC220) monotherapy in FLT3-Itd-positive (+) relapsed/refractory (R/R) Acute Myeloid Leukemia (AML). Blood. 2016;128(22). doi:10.1182/blood-2016-06-724161
47. Altman JK, Foran JM, Pratz KW, Trone D, Cortes JE, Tallman MS. Phase 1 study of quizartinib in combination with induction and consolidation chemotherapy in patients with newly diagnosed acute myeloid leukemia. Am J Hematol. 2018;93(2):213–221. doi:10.1002/ajh.24974
48. Swaminathan M, Kantarjian HM, Daver N, et al. The combination of quizartinib with azacitidine or low dose cytarabine is highly active in patients (Pts) with FLT3-ITD mutated myeloid leukemias: interim report of a phase I/II trial. Blood. 2017;130. PubMed PMID:WOS:000432419401370.
49. Sanga M, James J, Marini J, Gammon G, Hale C, Li JK. An open-label, single-dose, phase 1 study of the absorption, metabolism and excretion of quizartinib, a highly selective and potent FLT3 tyrosine kinase inhibitor, in healthy male subjects, for the treatment of acute myeloid leukemia. Xenobiotica. 2017;47(10):856–869. doi:10.1080/00498254.2016.1217100
50. Cortes J, Perl AE, Dohner H, et al. Quizartinib, an FLT3 inhibitor, as monotherapy in patients with relapsed or refractory acute myeloid leukaemia: an open-label, multicentre, single-arm, phase 2 trial. Lancet Oncol. 2018;19(7):889–903. doi:10.1016/S1470-2045(18)30240-7
51. Cortes JE, Tallman MS, Schiller GJ, et al. Phase 2b study of 2 dosing regimens of quizartinib monotherapy in FLT3-ITD-mutated, relapsed or refractory AML. Blood. 2018;132(6):598–607. doi:10.1182/blood-2018-01-821629
52. Stone RM, Mandrekar SJ, Sanford BL, et al. Midostaurin plus chemotherapy for acute myeloid leukemia with a FLT3 mutation. N Engl J Med. 2017;377(5):454–464. doi:10.1056/NEJMoa1614359
53. Martin MT, Jeschke G, Perl AE, Carroll M, Figueroa ME. Differentiation response to quizartinib, a potent 2nd generation FLT3 inhibitor, in relapsed FLT3-mutant AML patients correlates with specific DNA methylation signature prior to therapy. Blood. 2017;130. PubMed PMID:WOS:000432419401370.
54. Khaled S, Ganguly S, Perl AE, et al. Concordance between bone marrow and peripheral blood samples for assessment of FLT3 Internal Tandem Duplication (ITD) mutations: data from patients screened for participation in quantum-R, a global, randomized, open-label, phase 3 study examining the effect of quizartinib monotherapy vs salvage chemotherapy on overall survival in patients with FLT3 – ITD – mutated AML who are refractory to or have relapsed after first-line therapy. Blood. 2017;130. PubMed PMID:WOS:000432419403248.
55. Schlenk R, Dombret H, Amadori S, et al. QuANTUM-first: phase 3, double-blind, placebo-controlled study of quizartinib in combination with induction and consolidation chemotherapy, and as maintenance therapy in patients (pts) with newly diagnosed (NDx) FLT3-ITD acute myeloid leukemia (AML). Ann Oncol. 2017;28. doi:10.1093/annonc/mdx075
56. Smith CC, Paguirigan A, Jeschke GR, et al. Heterogeneous resistance to quizartinib in acute myeloid leukemia revealed by single-cell analysis. Blood. 2017;130(1):48–58. doi:10.1182/blood-2016-04-711820
57. Stone RM, DeAngelo DJ, Klimek V, et al. Patients with acute myeloid leukemia and an activating mutation in FLT3 respond to a small-molecule FLT3 tyrosine kinase inhibitor, PKC412. Blood. 2005;105(1):54–60. doi:10.1182/blood-2004-03-0891
58. Hirade T, Abe M, Onishi C, Taketani T, Yamaguchi S, Fukuda S. Internal tandem duplication of FLT3 deregulates proliferation and differentiation and confers resistance to the FLT3 inhibitor AC220 by up-regulating RUNX1 expression in hematopoietic cells. Int J Hematol. 2016;103(1):95–106. doi:10.1007/s12185-015-1908-8
59. Hou PP, Wu C, Wang YC, et al. A genome-wide CRISPR screen identifies genes critical for resistance to FLT3 inhibitor AC220. Cancer Res. 2017;77(16):4402–4413. doi:10.1158/0008-5472.Can-16-1627
60. Traer E, Martinez J, Javidi-Sharifi N, Agarwal A, Dunlap J, English I, et al. FGF2 from marrow microenvironment promotes resistance to FLT3 inhibitors in acute myeloid leukemia. Cancer Res. 2016;76(22):6471–6482. doi:10.1158/0008-5472.Can-15-3569
61. Abe M, Pelus LM, Singh P, et al. Internal tandem duplication in FLT3 attenuates proliferation and regulates resistance to the FLT3 inhibitor AC220 by modulating p21Cdkn1a and Pbx1 in hematopoietic cells. PLoS One. 2016;11(7):e0158290. doi:10.1371/journal.pone.0158290
62. Friedman R. The molecular mechanism behind resistance of the kinase FLT3 to the inhibitor quizartinib. Proteins. 2017;85(11):2143–2152. doi:10.1002/prot.25368
63. Verma S, Singh A, Kumari A, et al. Insight into the inhibitor discrimination by FLT3 F691L. Chem Biol Drug Des. 2018;91(5):1056–1064. doi:10.1111/cbdd.13169
64. Levis M. Quizartinib for the treatment of FLT3/ITD acute myeloid leukemia. Future Oncol. 2014;10(9):1571–1579. doi:10.2217/Fon.14.105
65. Suarasan S, Simon T, Boca S, Tomuleasa C, Astilean S. Gelatin-coated gold nanoparticles as carriers of FLT3 inhibitors for acute myeloid leukemia treatment. Chem Biol Drug Des. 2016;87(6):927–935. doi:10.1111/cbdd.12725
66. Li GX, Wang L, Yaghmour B, Ramsingh G, Yaghmour G. The role of FLT3 inhibitors as maintenance therapy following hematopoietic stem cell transplant. Leuk Res Rep. 2018;10:26–36. doi:10.1016/j.lrr.2018.06.003
67. Cortes J Quizartinib significantly prolongs overall survival in pa‐ tients with FLT3‐internal tandem duplication–mutated (mut) re‐ lapsed/refractory aml in the phase 3, randomized, controlled quantum‐r trial. EHA Learning Center. Abstract LB2600; 2018. Available from: .
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.