Back to Journals » Clinical Ophthalmology » Volume 13
Quality of life after refractive surgery: ReLEx SMILE vs Femto-LASIK
Authors Klokova OA, Sakhnov SN , Geydenrikh MS , Damashauskas RO
Received 15 April 2018
Accepted for publication 18 September 2018
Published 26 March 2019 Volume 2019:13 Pages 561—570
DOI https://doi.org/10.2147/OPTH.S170277
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Scott Fraser
Olga Aleksandrovna Klokova, Sergey Nikolaevich Sakhnov, Maria Sergeevna Geydenrikh, Roman Olegovich Damashauskas
Krasnodar Branch of Fyodorov Eye Microsurgery, Federal State Institution, Krasnodar, Russia
Purpose: The safety and effectiveness of complex myopic astigmatism correction using ReLEx SMILE or Femto-LASIK techniques have been well established. The purpose of the current study is to compare quality of life (QoL) outcomes following ReLEx SMILE or Femto-LASIK procedures in parallel with functional vision and anatomic outcomes of treated eyes.
Patients and methods: This prospective, consecutive series included 118 patients, 18–43 years of age, out of which 56 underwent ReLEx SMILE and 62 underwent Femto-LASIK surgery for correction of myopic astigmatism. All patients underwent standard comprehensive ophthalmic examinations, and additionally, completed The Quality of Life Impact of Refractive Correction Questionnaire to determine the impact the vision-correction treatment had on their QoL.
Results: In both treatment groups, the postoperative refractive outcomes were comparable, with visual acuity improvements for both groups noted the day following surgery. After laser correction of complex myopic astigmatism using Femto-LASIK and ReLEx SMILE methods, the overall QoL indicators are statistically significant (P<0.01) exceeding preoperative values 1 month after the operation and reaching the maximum values by the end of the observation period (P<0.0001).
Conclusion: The results of the study suggest that patients require some time to adapt to their new visual function and its impact on their daily living, delaying detectable improvements in QoL. Moreover, these results may suggest a higher satisfaction trend and long-term QoL in patients undergoing ReLEx SMILE in comparison to Femto-LASIK. Long-term results from the study demonstrated high patient satisfaction with both methods.
Keywords: ReLEx SMILE, Femto-LASIK, quality of life, QoL questionnaire, refractive surgery
Introduction
There are several recognized corneal refractive surgery platforms and techniques to correct myopia, hyperopia, or astigmatism by changing the curvature of the cornea. The evaluation of efficacy and safety of ophthalmic treatments or procedures are conventionally subdivided into objective and subjective assessment categories. Key treatment evaluation indicators include the quantitative outcomes of visual acuity testing (corrected and uncorrected), keratometry, refractometry, contrast sensitivity, corneal high-order aberrations, nerve fiber regeneration, centration of the treatment zone, and corneal biomechanical properties.1–4 Often, patient satisfaction is more subjective and determined by a qualitative comparison of the vision experienced postoperatively, balanced with their preoperative expectations. As the predictability of refractive correction and visual outcomes improve, patient satisfaction and managing patient expectations become key in the context of modern ophthalmology.5 Simply correcting the refractive error is no longer the only consideration, and patients, particularly those within the working-age population, expect that the procedure will positively influence their quality of life (QoL).
Numerous studies have been published comparing two state-of-the-art vision correction techniques used for correcting complex myopic astigmatism, the ReLEx SMILE and the Femto-LASIK.6–11 The safety, predictability, and effectiveness of complex myopic astigmatism correction, using ReLEx SMILE or Femto-LASIK techniques, have been well established. The majority of these studies focus on the objective measures for evaluation, yet often neglect the subjective experience or QoL outcomes of the patient.12–21 Few publications compare QoL following ReLEx SMILE technique, and a paucity of the literature exists for any comparative measures.13,22,23
QoL combines various aspects, which include physical condition, functional capabilities, psychological state, general condition, and social interaction.24–26 Various QoL questionnaires have been used to evaluate patients’ satisfaction with their life conditions, their work, education, home environment, and even political beliefs in relation to their visual status.
A survey developed and validated by Pesudovs et al, the Quality of Life Impact of Refractive Correction (QIRC) Questionnaire, was specifically developed for patients with refractive error corrected by spectacles, contact lenses, and refractive surgery.27–29 [Our team was granted copyright permission to reproduce the QIRC Questionnaire and the questionnaire items in this paper.]
The purpose of the current study is to compare questionnaire-based QoL of patients following complex myopic astigmatism correction with ReLEx SMILE or Femto-LASIK procedures in parallel with functional vision and anatomic outcomes of treated eyes.
Patients and methods
This prospective, single-center, consecutive series included 118 patients, age 18–43 years. Fifty-six patients received ReLEx SMILE and 62 patients received Femto-LASIK surgery for correction of myopic astigmatism. Procedures were performed from March 2015 to May 2017 by two equally experienced refractive surgeons. The research was conducted at the Krasnodar Branch of Fyodorov Eye Microsurgery Federal State Institution in Krasnodar, Russia. Patients were not included in the series if they had other serious ocular disorders; neurologic and systemic diseases; myopic correction >8.5 D; corrected vision acuity <0.1 log MAR (poorer than 20/25 Snellen equivalent); “dry eye” syndrome; epitheliopathy; or previous inflammatory corneal diseases.
This study adhered to the tenets of the Declaration of Helsinki. Each patient included in the study provided written informed consent for the procedure and collection of data. This study was approved by the Ethics Committee in the Body of Scientific Medical Board of the Krasnodar Branch of Fyodorov Eye Microsurgery Federal State Institution, Russia.
Patients underwent femtosecond vision correction using ReLEx SMILE and Femto-LASIK techniques and laser system VisuMax™ (Carl Zeiss Meditec AG, Jena, Germany) with pulse frequency comprising 500 kHz and laser system EX 500 (Novartis/ALCON/WaveLight, Germany) for complex myopic astigmatism correction. The surgeries were carried out by two equally experienced clinical surgeons using general techniques. The femtosecond laser flaps were obtained using the following settings: thickness 100.72±5.43 μm (from 90 to 110 μm), diameter 8.52±0.32 mm (from 7.9 to 8.8 mm), with a superior hingle in all eyes. The average central optical ablation zone was 6.24±0.42 mm (from 6.0 to 7.0 mm).
Small-incision lenticule extraction (ReLEx SMILE) surgeries were performed using the technology described by Sekundo et al.30 The intended thickness of the upper tissue arcade (the cap) was 120 mm, with an intended diameter of 7.5 mm, whereas the average diameter of the refractive lenticule was 6.37±0.44 mm (from 6.0 to 7.0 mm). A single-side cut of 90° with a circumferential length of 3.0–4.5 mm was made in the superior position. Following the cutting procedure, the refractive lenticule was dissected and separated through the side-cut and manually removed.
All patients underwent standard comprehensive ophthalmic examinations, preoperatively and at regular postoperative intervals, including assessment of best-corrected visual acuity (BCVA), manifest and cycloplegic refraction, intraocular pressure assessment by tonometry, corneal topography by Pentacam (Oculus, Germany), determination of endothelial cell count, and dilated examination of ocular fundus with Goldmann lens.
In addition to the traditional clinical assessments, patients completed the 20 items in The QIRC Questionnaire28,29 to determine the impact the vision-correction treatment had on their QoL. Questionnaires were completed preoperatively, and at 1, 3, and 6 months postoperatively. Each question has five possible responses, ranging from “none at all”, “a little bit”, to “a moderate amount”, “a lot”, or “so much that I can’t do this activity”.29
The questionnaire weighs questions and individual responses with a score that can range from 14.39 to 88.21, with higher scores correlating with a more favorable outcome. Questions from 1–7 have a range 24.07–65.11 scores, questions 8–13 has a range 28.59–66.62, questions 14–20 has a range 14.39–88.21 scores. Patients were followed for a minimum of 6 months.
Statistical analysis
Statistical processing and graphical presentation of the results were carried out using the software MS Excel 2016 (Microsoft, USA) and Statistica version 10.0 (StatSoft Inc., Tulsa, OK, USA). The data obtained are presented as the mean and SD (M±SD). For comparison of two independent groups, Student’s unpaired t-criterion was applied, and for comparison of dependent ones, the Student’s t-test was applied. The critical level of significance of the null statistical hypothesis in accordance with the criteria accepted in biomedical research was taken as 0.05.
Results
The baseline characteristics and demographics of the study cohort are shown in Table 1. Preoperatively and within the postoperative period, no complications or adverse events were observed in any patient. Table 2 includes the uncorrected visual acuity (UCVA) for both groups within different observation periods. In the vast majority of cases, within the first 2 weeks after the refractive procedure, the UCVA was equivalent to the preoperative BCVA.
  | Table 1 Characteristics of patients in study groups |
In both groups, compatible refractive values were reached (Figures 1 and 2). Thus, as a result of applying ReLEx SMILE technique, the refractive value of ±0.5 D was achieved in 93.8% of cases and ±1.0 D in 100% of cases. Within the first days postoperatively, an insignificant hypermetropic refractive shift was noted, which stabilized within 1 month, and the achieved planned emmetropia remained sustainable during the full observation period. In the Femto-LASIK group, the planned refractive value of ±0.5 D was achieved in 94.2% of cases and ±1.0 D in 100% of cases.
  | Figure 1 Predictability of the reached average spherical equivalent in ReLEx SMILE group 6 months after the surgery (n=112). |
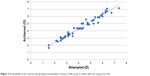  | Figure 2 Predictability of the reached average spherical equivalent in Femto-LASIK group 6 months after the surgery (n=124). |
A comparative analysis the answers of patients in the study groups to the questions of the QIRC questionnaire indicated that prior to surgery, patients in the ReLEx SMILE group were more dissatisfied with the quality of sight, dependence on spectacle correction, as demonstrated by their answers to question 11 (P<0.01), questions 5–6 (P<0.01) and question 7 (P<0.05). Analyzing the answers of patients in the study groups to questions in the postoperative period, we noted a positive dynamics in the evaluation of quality of life during the observation period in both groups (Table 3). Patients of both study groups noted that it became easier to drive a car (P<0.01), and less feeling fatigue or strain in the eyes (P=0.0004 and P=0.002, respectively). Patients in the ReLEx SMILE group 6 months after the correction were more satisfied with visual quality compared to patients in the Femto-LASIK group, which is particularly reflected in the answers to question 4 after 6 months (P=0.0003).
Six months after the surgery, more than 90% of respondents were satisfied with the visual acuity and quality of vision achieved. Notably, difficulties while driving a car at night were experienced in the ReLEx SMILE group by only two persons (3.6%) and in the Femto-LASIK group by four persons (6.4%).
The QIRC provided an evaluation of patient’s anxiety, the less anxious a patient is, the higher the score. An analysis of the answers to the questionnaire questions 8–10 and 13 characterizing the patients’ concern about their eye protection from ultraviolet radiation and possible financial losses, showed that before the operation the level of anxiety in the groups was the same (P=0.23) (Table 3). So in questions 8–9 concerning the cost of the initial and additional refractive surgery, an overwhelming number of respondents answered “Not at all” and “A little bit”. The answers to question 10 showed the same level (P>0.05) depending on glasses and contact lenses used. After refractive surgery, the respondents did not need an additional correction, and in this connection they did not answer question 7. It is worth noting that patients of the ReLEx SMILE group are to a lesser extent (P<0.0001) concerned with medical complications of laser correction (question 12). This result can be explained by the technologic advantages of ReLEx SMILE. At the same time, patients after the ReLEx SMILE during the early postoperative period (1 month) were more concerned (P<0.01) about the quality of vision compared with the Femto-LASIK group (question 11). This trend correlates with the dynamics of the recovery of the UCVA (Table 2). As for the respondents in the Femto-LASIK group, there is a decrease in the level of anxiety about possible medical complications from month to month (P=0.001, P=0.0002 and P<0.0001).
An analysis of Femto-LASIK group’s answers to the “emotional well being” block questions (14–20) revealed the following: it was dominated by people who were unhappy with their appearance (P<0.0001) (question 14). In the SMILE group, there were people who were self-confident, feeling attractive, and apparently they went for vision correction more likely to improve their vision, increase convenience in everyday life, and not because of low self-esteem. Despite their great self-confidence, patients from the SMILE group were initially more dissatisfied with being unable to deal with the cases they would like (question 19) (P=0.003) and had a stronger desire to try something new (question 20) (P=0.02). After refractive surgery, the self-esteem of Femto-LASIK patients increased and remained high for all 6 months (P<0.0001). They began to receive compliments more often (P=0.03). As for the SMILE group, its participants noted that they became more self-confident and more happy 1 month after the operation (P<0.0001).
It is important to note that in general, the patients of the SMILE group (P<0.01) and the Femto-LASIK group (P<0.01) felt statistically significantly more comfortable compared to preoperative data, starting from the first month. Given all the data received, the answers to the 20-item QIRC Questionnaire (Table 3), it can be concluded that the groups “Femto-LASIK” and “SMILE” were initially comparable in terms of QoL (P>0.05). After laser correction of complex myopic astigmatism using Femto-LASIK and ReLEx SMILE methods, the overall QoL indicators are statistically significant (P<0.01) exceeding preoperative data (Figure 3).
Change of average score representing the patients’ answers to the questions of the QIRC questionnaire in study groups over the follow up after the operation is reaching the maximum values by the end of the observation period (P<0.001) (Figure 3).
Discussion
This study has demonstrated that although patients in both treatment groups achieved desired refractive correction following surgery, there is a paucity in the literature regarding QoL measures following refractive correction surgery, particularly following ReLex SMILE. The US Food and Drug Administration (FDA) collaborated with the National Eye Institute and the Department of Defense to develop an online questionnaire, Patient-Reported Outcomes with LASIK (PROWL) survey, to assess functional limitations and patient satisfaction after LASIK surgery.31 They found that patient-rated satisfaction at 3 and 6 months was greater than 90%, with 1%–2% of patients reporting dissatisfaction after surgery.
Notably, the authors report that the questionnaire may be relevant for the assessment of visual symptoms in clinical trials, including for FDA approval, and it might not be practical for use by surgeons to assess individual patient outcomes. Additionally, it did not address the more qualitative aspects of QoL, such as anxiety and happiness, as we have in the current study.
A study from Lesueur et al investigated predictors of QoL related to PRK, LASIK, and phakic IOL refractive procedures.32 They found that those patients with higher degrees of myopia had significant improvements in self-esteem and coping as compared to other patients. They found that quality of vision was directly correlated with improvement of QoL, satisfaction scores, and BCVA preoperatively and postoperatively in all patients, but interestingly no correlation was noted between visual acuity and patient satisfaction.
Katzen published a paper in 2002 related to the anxiety of patients undergoing laser refractive surgery, noting that as refractive surgery has rapidly evolved and the quest to obtain faster visual recovery, fewer complications, and early stability continues, there is little in the literature that addresses the anxiety experienced by most refractive surgical patients.33 Unfortunately in the 16 years since that publication, minimal steps have been taken to further study the anxiety and management of anxiety or fears in refractive surgery patients.
As a result of laser correction, the study group patients gave us comparable visual results, as no complications occurred in either group and refractive results were within ±1.0 D for all eyes. Contrary to our expectations, despite technologic advantages of ReLEx SMILE technique, general anxiety level did not differ in both groups. It should be noted that 1 month after surgery, patients of both groups under study experienced a significantly higher level (P<0.01) of anxiety than in the long-term postoperative period (6 months). In our opinion, this determines the need for psychological support from the surgeon during this period. It is worth noting positive dynamics in both groups within a month after the operation in the fall of anxiety level due to vision (P<0.0001).
All the patients equally felt certain fears, especially in the first months after surgery: the fear to lose the reached vision acuity, the fear of possible complications and financial losses. This observation provides some explanation regarding fears or stress that a patient may experience that the physician can be aware of and offer assistance or advice. We found more interesting facts in the course of analyzing the answers to the “emotional well being” block questions (14–20). A significant variation of answers to certain questions draws attention.
The authors speculate whether the different physical qualities of the procedures themselves may influence the differences in QoL results and timing of results. ReLEx SMILE and Femto-LASIK procedures have variable degrees of trauma to the tissue, ocular shape transformation due to surgery, and corneal drought. Other contributing factors may be related to the time duration of surgery, recovery time needed, and postoperative management protocol. All of these factors are planned to be investigated in future studies.
Evaluation and measurement of the patients’ QoL based on the questionnaire represents important additional information and conclusions related to patient satisfaction and expectations that cannot be determined from visual acuity and refractive status alone. QoL assessment provides evaluation of the emotional condition of patients and may allow for an individual approach to the patient management in pre- and postoperative periods.
Conclusion
This study focused on addressing patients’ satisfaction and QoL following vision-correcting ReLEx SMILE and Femto-LASIK surgeries. In addition to traditional objective measurements of visual acuity and ophthalmic examination, the patient experience was evaluated using a QoL questionnaire. Results of the study confirm a positive visual acuity outcome after treatment regardless of the surgical technique implemented. Improvements in QoL can be appreciated as early as the first day following surgery.
However, it is apparent that patients usually need some time to adapt to the new vision conditions and how these changes impact their daily lives as maximum QoL improvement was not achieved until later in the observation period. Long-term results from the study demonstrated high patient satisfaction with both methods. However, our findings revealed a higher satisfaction trend in QoL in those who received the ReLEx SMILE refractive correction.
As patient satisfaction is key in vision-correcting surgery, the addition of QoL assessment to traditional ophthalmic assessments offers a more detailed evaluation of patient outcomes. We recommend that QoL be included as best practice in the postoperative period to assess the results after corrective surgery.
Author contributions
All authors contributed toward data analysis, drafting and revising the paper, gave approval for the final version to be published and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Klokova OA, Piskunov AV, Khashaova SR. Qualitative evaluation of the results of ReLex surgeries (SMILE technique) based on contrast sensitivity. J Mod Tech Ophthalmol. 2014;3:149–152. | ||
Agca A, Cankaya KI, Yilmaz I, et al. Fellow eye comparison of nerve fiber regeneration after SMILE and femtosecond laser-assisted LASIK: a confocal microscopy study. J Refract Surg. 2015;31(9):594–598. | ||
Blum M, Kunert K, Schröder M, Sekundo W. Femtosecond lenticule extraction for the correction of myopia: preliminary 6-month results. Graefes Arch Clin Exp Ophthalmol. 2010;248(7):1019–1027. | ||
Reinstein DZ, Carp GI, Archer TJ, Gobbe M. Outcomes of small incision lenticule extraction (SMILE) in low myopia. J Refract Surg. 2014;30(12):812–818. | ||
Schmidt GW, Yoon M, McGwin G, Lee PP, McLeod SD. Evaluation of the relationship between ablation diameter, pupil size, and visual function with vision-specific quality-of-life measures after laser in situ keratomileusis. Arch Ophthalmol. 2007;125(8):1037–1042. | ||
Wu W, Wang Y. The correlation analysis between corneal biomechanical properties and the surgically induced corneal high-order aberrations after small incision lenticule extraction and femtosecond laser in situ keratomileusis. J Ophthalmol. 2015;2015:758196. | ||
Ali MA, Kobashi H, Kamiya K, et al. Comparison of astigmatic correction after femtosecond lenticule extraction and wavefront-guided LASIK for myopic astigmatism. J Refract Surg. 2014;30(12):806–811. | ||
Teus MA, Garcia-Gonzalez M, Lin F, Yang Y. Comparison of the visual results after small incision lenticule extraction and femtosecond laserassisted LASIK for myopia. J Refract Surg. 2014;30(9):582. | ||
Chan TC, Ng AL, Cheng GP, et al. Vector analysis of astigmatic correction after small-incision lenticule extraction and femtosecond-assisted LASIK for low to moderate myopic astigmatism. Br J Ophthalmol. 2016;100(4):553–559. | ||
Chen X, Wang Y, Zhang J, Yang SN, Li X, Zhang L. Comparison ofocular higher-order aberrations after SMILE and wavefront-guided femtosecond LASIK for myopia. BMC Ophthalmol. 2017;17(1):42. | ||
Ye MJ, Liu CY, Liao RF, Gu ZY, Zhao BY, Liao Y. SMILE and wavefront-guided LASIK out-compete other refractive surgeries in ameliorating the induction of high-order aberrations in anterior corneal surface. J Ophthalmol. 2016;2016:8702162. | ||
Zhang J, Zheng L, Zhao X, Xu Y, Chen S. Corneal biomechanics after small-incision lenticule extraction versus Q-value-guided femtosecond laser-assisted in situ keratomileusis. J Curr Ophthalmol. 2016;28(4): 181–187. | ||
Shchuko AG, Pisarevskaya OV, Bukina VV, Iureva TN. Femtosecond technology of myopia correction. Fyodorov J Ophthalmic Surg. 2014;2:33–38. | ||
Ang M, Tan D, Mehta JS. Small incision lenticule extraction (SMILE) versus laser in-situ keratomileusis (LASIK): study protocol for a randomized, non-inferiority trial. Trials. 2012;13:75. | ||
Sekundo W, Kunert K, Russmann C, et al. First efficacy and safety study of femtosecond lenticule extraction for the correction of myopia: six-month results. J Cataract Refract Surg. 2008;34(9):1513–1520. | ||
Blum M, Flach A, Kunert KS, Sekundo W. Five-year results of refractive lenticule extraction. J Cataract Refract Surg. 2014;40(9):1425–1429. | ||
Reinstein DZ, Archer TJ, Gobbe M. Small incision lenticule extraction (SMILE) history, fundamentals of a new refractive surgery technique and clinical outcomes. Eye Vis. 2014;1(1):3. | ||
Reinstein DZ, Gobbe M, Gobbe L, Archer TJ, Carp GI. Optical zone centration accuracy using corneal fixation-based SMILE compared to eye tracker-based femtosecond laser-assisted LASIK for myopia. J Refract Surg. 2015;31(9):586–592. | ||
Ivarsen A, Asp S, Hjortdal J. Safety and complications of more than 1500 small-incision lenticule extraction procedures. Ophthalmology. 2014;121(4):822–828. | ||
Lee JK, Chuck RS, Park CY. Femtosecond laser refractive surgery: small-incision lenticule extraction vs. femtosecond laser-assisted LASIK. Curr Opin Ophthalmol. 2015;26(4):260–264. | ||
Shah R, Shah S. Effect of scanning patterns on the results of femtosecond laser lenticule extraction refractive surgery. J Cataract Refract Surg. 2011;37(9):1636–1647. | ||
Vestergaard A, Ivarsen AR, Asp S, Hjortdal JØ. Small-incision lenticule extraction for moderate to high myopia: predictability, safety, and patient satisfaction. J Cataract Refract Surg. 2012;38(11):2003–2010. | ||
Ang M, Ho H, Fenwick E, et al. Vision-related quality of life and visual outcomes after small-incision lenticule extraction and laser in situ keratomileusis. J Cataract Refract Surg. 2015;41(10):2136–2144. | ||
Batalina LV [webpage on the Internet]. Clinical and Functional Study of the Dynamics of the State of the Organ of Vision after Carrying Out LASIK in Myopia [PhD thesis]. Available from: http://medical-diss.com/medicina/kliniko-funktsionalnoe-issledovanie-dinamiki-sostoyaniyaorgana-zreniya-posle-provedeniya-lasik-pri-miopii. Accessed on November 7, 2018. | ||
Ovechkin IG, Pozharitskiy MD. Application of methodical approaches of restorative medicine to the assessment of excimer laser vision correction efficacy. J Restor Med Rehabil. 2010;2:64–66. Russian. | ||
Trubilin VN, Shchukin SY. Sub”yektivnyye rezul’taty eksimernoy lazernoy korrektsii miopii [Subjective results of excimer laser correction of myopia]. Oftal´mologya. 2012;9(3):4–8. Russian. | ||
Lamoureux EL, Pallant JF, Pesudovs K, Hassell JB, Keeffe JE. The Impact of Vision Impairment Questionnaire: an evaluation of its measurement properties using Rasch analysis. Invest Ophthalmol Vis Sci. 2006;47(11):4732–4741. | ||
Pesudovs K, Burr JM, Harley C, Elliott DB. The development, assessment, and selection of questionnaires. Optom Vis Sci. 2007;84(8):663–674. | ||
Pesudovs K, Garamendi E, Elliott DB. The Quality of Life Impact of Refractive Correction (QIRC) Questionnaire: development and validation. Optom Vis Sci. 2004;81(10):769–777. | ||
Sekundo W, Kunert KS, Blum M. Small incision corneal refractive surgery using the small incision lenticule extraction (SMILE) procedure for the correction of myopia and myopic. Br J Ophthalmol. 2011;95(3):335–339. | ||
Sugar A, Hood CT, Mian SI. Patient-reported outcomes following LASIK: quality of life in the PROWL studies. JAMA. 2017;317(2):204–205. | ||
Lesueur L, Munoz-Sastre MT, Mullet E, Dabadie B, Arné JL. Predictors of quality of life in refractive surgery. J Fr Ophtalmol. 2003;26(7):699–709. | ||
Katzen J. Management of anxiety in the refractive surgery patient. Insight. 2002;27(4):103108–107109. |
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.



