Back to Journals » Neuropsychiatric Disease and Treatment » Volume 15
Psychache and Suicidal History in Patients with Obsessive-Compulsive Disorder
Authors Demirkol ME , Namlı Z , Eriş Davul Ö, Karaytuğ MO , Tamam L , Yılmaz H
Received 13 November 2019
Accepted for publication 12 December 2019
Published 24 December 2019 Volume 2019:15 Pages 3531—3539
DOI https://doi.org/10.2147/NDT.S237369
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Roger Pinder
Mehmet Emin Demirkol,1 Zeynep Namlı,1 Özge Eriş Davul,2 Mahmut Onur Karaytuğ,3 Lut Tamam,1 Hamdi Yılmaz1
1Deparment of Psychiatry, Çukurova University School of Medicine, Adana, Turkey; 2Department of Psychiatry, Hatay State Hospital, Hatay, Turkey; 3Department of Psychiatry, Dr Ekrem Tok Hospital for Mental and Nervous Disease, Adana, Turkey
Correspondence: Lut Tamam; Mehmet Emin Demirkol
Department of Psychiatry, Çukurova University School of Medicine, Adana, Turkey
Tel + 90 533 6306006; +90 535 5849684
Fax +90 322 3386204
Email [email protected]; [email protected]
Purpose: Suicide is an important cause of death in patients diagnosed with obsessive-compulsive disorder (OCD) as well as other psychiatric disorders. Early determining of risk factors provides an opportunity for intervention. The mediating effect of psychological pain (also known as psychache) on suicide has been shown in various disorders but has not been investigated in patients with OCD. In this study, we aimed to show the relationship between psychological pain and other clinical variables and suicide in OCD patients.
Patients and methods: This cross-sectional study consisted of 67 patients diagnosed with OCD according to DSM-5 criteria with no comorbid psychiatric diagnosis who applied to the psychiatric outpatient clinic of Çukurova University Faculty of Medicine and 63 healthy controls. Among the OCD patients, 12 had previous suicide attempts. In addition to the sociodemographic data form, participants filled out the Yale-Brown Obsessive Compulsive Scale (YBOCS), the Psychache Scale (PS), the Beck Scale for Suicidal Ideation (BSIS), and the Hamilton Depression Scale (HDS).
Results: OCD group’s median obsession, compulsion, and the total scores of YBOCS, and the mean PS scores were higher than the control group. There was no difference between the sociodemographic variables of OCD patients with and without previous suicide attempts such as age, gender, years of education, place of residence, marital, and occupational status. The median scores of obsession, avoidance, global severity, and indecisiveness subdimensions of YBOCS, the mean BSIS and PS scores, the rates of current aggressive, current contamination, and the past religious obsessions were higher in the suicidal group. There were moderately significant relationships in the same direction between the PS, BSIS, and total YBOCS scores. Multivariate regression analysis demonstrated that only the PS scores predicted previous suicide attempts.
Conclusion: Our results demonstrated that current aggressive, current contamination, past religious obsessions, and the higher psychological pain are related to previous suicide attempts in OCD patients. Our regression analysis supports Shneidman’s hypothesis: there would be no suicide without psychache. Relieving psychache in OCD patients may reduce suicide attempts even if there is no diagnosis of comorbid depression.
Keywords: obsessive compulsive disorder, suicide, psychological pain, psychache
Introduction
Obsessive-compulsive disorder (OCD) is characterized by a chronic course, reduced functionality, generally partial response to existing treatment methods, and causing disability.1 OCD’s prevalence is approximately 2% in the United States.2 The negative consequences of OCD, such as decreased quality of life, and frequent psychiatric comorbidities, have often been focused on, but the relationship between OCD and suicide has not been adequately addressed.3
Suicide is a major public health problem in all communities, characterized by processes that can range from thinking of death, desire to die, or not to find life worth living to the planning, undertaking and completing the attempt.4 Psychiatric disorders are important risk factors for suicide. Suicide-related studies have often focused on mood disorders, psychotic disorders, substance use disorders, and personality disorders.5 Previous studies reported that the history of suicide attempts was 3–4%, and the completed suicide rates were lower than 1% in patients with OCD.6,7 However, recent studies have shown that there are higher risks of suicide attempts and death as a result of suicide in OCD patients than healthy individuals.8
Suicide risk factors in patients with OCD were, until recently, an often neglected area where there was not enough data.1,5 Research has shown that comorbid mood disorders have mediating effects on suicide in OCD.9 A significant relationship was found between being single, family history of suicide attempts, childhood trauma, comorbidity of posttraumatic stress disorder, low socioeconomic level, and lack of religious activities and suicidal thoughts and attempts.1,5,10
Studies on the relationship between obsessions and compulsions to suicidal behavior have not yielded a common result. Previous studies revealed that sexual, aggressive,11–13 symmetry/order,1 and religious obsessions and compulsions5 were related to suicidal thoughts and suicide attempts. Although Dhyani et al14 stated that patients with OCD usually attempt suicide by poisoning, there is no common opinion on the method of suicide.
Psychological pain (also known as psychache) is the process of mental suffering, a state of emotional unease caused by negative emotions such as shame, grief, anger, and despair that arise as a result of the hindrance of the individual’s basic needs.15,16 Shneidman17 concluded that there would be no suicide without psychological pain as a result of his review of suicide notes. Studies about Shneidman’s model stated that psychological pain provides the relationship between depression and suicidal ideation and lifelong suicide attempts, and that psychological pain has a catalyst effect on suicide risk factors.18,19 The effect of psychological pain on suicidality has been shown in different groups like students,20 prisoners,21 homeless,18 and depressed patients.22 The researchers revealed the effect of psychological pain on suicide in patients with depressive disorder,23 bipolar disorder,24 and schizophrenia25 in the Turkish population.
Although Brown et al3 reported the similarity of obsession-related stress to psychological pain recently, to the best of our knowledge, there is no study about psychache in patients with OCD. Determining risk factors for suicide in patients with OCD will provide an opportunity for early intervention and help to prevent possible deaths. Based on the Rudd’s Fluid Vulnerability theory of suicide, it can be concluded that chronic pain caused by OCD may be a risk factor for suicide, similar to psychological pain.26 In this study, we aimed to determine the relationship between psychological pain, previous suicide attempts and obsessions, compulsions, and sociodemographic variables in patients with OCD.
Materials and Methods
Sample
Cukurova University Faculty of Medicine (CUSM) Non-Interventional Clinical Research Ethics Committee approved the study. All participants signed an informed consent form before the interviews. The study was conducted in accordance with the Declaration of Helsinki. The first author conducted psychiatric interviews based on diagnostic criteria of the Diagnostic and Statistical Manual of Mental Disorders-5 (DSM-5).27 Eighty-two patients who were treated in outpatient clinics of the Department of Psychiatry of CUSM formed the OCD group. The control group consisted of 74 healthy volunteers who were compatible with the patients in terms of variables such as age, gender, marital status, and educational level. All participants were older than 18 and literate. Exclusion criteria were comorbid mental retardation, cognitive impairment, and psychotic disorders. We also excluded 15 patients from the OCD group and 11 subjects from the control group who were diagnosed with depression according to DSM-527 or had a total score of 7 or above on the Hamilton Depression Scale (HDS)28 considering the confounding effects of depression on suicide. The final analysis included 67 patients with OCD and 63 healthy controls.
Power Analysis
With a moderate effect size (Cohen’s d = 0.50), 0.80 power, and 0.05 error (p = 0.05), we calculated the sample size for the study to be 128 with the G Power program (version 3.1).29 Accordingly, we concluded that a sample consisting of 130 individuals has adequate power.
Procedure
In addition to the sociodemographic data form, the participants filled out the Beck Scale for Suicidal Ideation (BSIS), the Hamilton Depression Rating Scale (HDS), the Yale-Brown Obsessive Compulsive Scale (YBOCS), and the Psychache Scale (PS). Approximately 60–90 mins were given to each patient for a clinical interview and filling out the scales. The interviewer (first author) explained the points that the participants did not understand.
Measures
The Beck Scale for Suicidal Ideation (BSIS)
It is a five-section scale developed to evaluate the severity of suicidal ideation. The total score is obtained from the arithmetic sum of the scores from sub-sections. The highest score is 38, and high scores indicate the seriousness of suicidal ideation.30 In the Turkish validity and reliability study, Cronbach’s alpha value was 0.84.31
The Hamilton Depression Scale (HDS)
HDS is developed to assess the severity of depressive symptoms. This 17-item scale is filled by the clinician.28 Scores between 0–7 indicate no depression.32 In the Turkish validity and reliability study, Cronbach’s alpha value was 0.75.33
The Yale-Brown Obsessive Compulsive Scale (YBOCS)
It is a semi-structured scale consisting of 19 items that evaluate the types and severity of obsessive-compulsive symptoms. The items are rated from 0 to 4 on this Likert-type scale. The total score is obtained by calculating only the first ten items (except items 1b and 6b). High scores indicate increased disorder severity. The first five questions are related to obsessive symptoms, and the next five are related to compulsions. Symptoms are evaluated regarding how much they occupy the person’s time, prevent normal functioning, induce distress, are actively resisted, and can be controlled by the patient. Items 11–16 evaluate the insight, avoidance, indecisiveness, pathological responsibility, pathological slowness, and pathological doubting, respectively. Items 17 and 18 are scored on the interviewer’s comment on disorder severity and global improvement. Item 19 evaluates the reliability of the scores. The symptom checklist next to the scale helps to determine the types of obsessions and compulsions as current and past.34 In the Turkish validity and reliability study, and the Cronbach’s alpha value was 0.81 in the internal consistency.35
The Psychache Scale (PS)
The PS is based on Shneidman’s definition of chronic, nonspecific psychological pain resulting from failure to meet vital psychological needs. It is a self-report scale consisting of 13 questions. The first nine items evaluate the frequency of psychache (eg, item 5: my pain makes my life seem dark), and the next four evaluate its intensity (eg, item 12: my pain is making me fall apart). The answers to the five-point Likert-type questions range from “never” to “always” or from “strongly agree” to “strongly disagree.” High scores indicate that the intensity and the frequency of psychological pain increases.36 PS has been shown to distinguish depressive patients with and without previous suicide attempts, successfully. In the Turkish validity and reliability study, the Cronbach’s alpha value was 0.98.23
Statistical Analysis
We showed descriptive statistics as mean ± standard deviation or as median and interquartile ranges according to the distribution of data. We summarized categorical variables as number and percentage and compared between the groups using the Fisher Exact or chi-square tests. We compared continuous variables with the independent samples t-test when data were normally distributed, and the Mann Whitney U-test otherwise. The Spearman’s rho correlation coefficient was used to assess the relationship between the scale scores when the data were not normally distributed. We used univariate and multivariate logistic regression models to investigate the risk factors affecting suicide attempts (dependent variable), and results were given as 95% confidence interval (CI) with odds ratio (OR). We used the Jamovi (Version 1.0.7) and JASP (Version 0.11.1) programs for statistical analysis and considered a value of p < 0.05 statistically significant.
Results
Table 1 compares the sociodemographic characteristics of OCD and control groups. Age, sex, years of education, place of residence, marital, and occupational status showed similar distribution by groups (p> 0.05 for each).
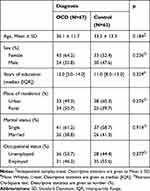 |
Table 1 Sociodemographic Characteristics of Groups |
Table 2 compares the scale scores between the groups. The total obsession and compulsion scores and the median total score of the YBOCS of the OCD group were significantly higher than the control group (p <0.001). The median scores of insight, avoidance, indecisiveness, pathological responsibility, pathological slowness, pathological doubting, global severity, global improvement, and reliability sub-dimensions of YBOCS were significantly higher in the OCD group (p <0.05 for each). We also found that the mean total scores of HDS and PS of the OCD group were significantly higher (p <0.001 for each).
 |
Table 2 Comparison of Scale Scores by Groups |
Table 3 compares sociodemographic characteristics and the BSIS, HDS, YBOCS, and PS scores of OCD patients according to the presence of suicide attempts. The sociodemographic characteristics of OCD patients were similar according to the presence of suicide attempts (p> 0.05 for each). The total obsession and YBOCS total scores of the OCD patients who had a history of attempted suicide were significantly higher (p = 0.007 and p = 0.028, respectively). The avoidance, indecisiveness, and global severity scores of OCD patients who had a history of attempted suicide were significantly higher (p = 0.009, p = 0.038 and p = 0.021, respectively). Finally, the BSIS and PS scores of OCD patients who had suicide attempts were also significantly higher (p <0.001 for each).
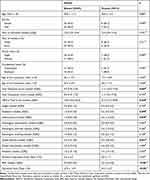 |
Table 3 Sociodemographic Characteristics and Scale Scores of OCD Patients According to the Presence of Suicide Attempts |
Table 4 compares obsession and compulsion types (current and the past) according to the presence of suicide attempts in patients with OCD. The rates of current aggressive, current contamination, and past religious obsessions of OCD patients who had a history of attempted suicide higher (p <0.001, p = 0.020 and p = 0.024, respectively).
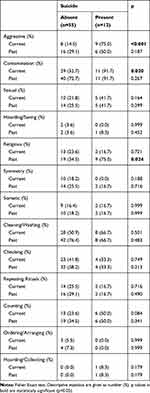 |
Table 4 Comparison of Obsession and Compulsion Types of OCD Patients According to the Presence of Suicide Attempts |
Table 5 shows the correlations between the scales. There were moderately significant correlations between BSIS and PS, total obsession, compulsion scores, and YBOCS total scores of OCD patients (p <0.05 for each) in the same direction. There were also moderately significant correlations between PS scores and total obsession, compulsion, and total scores of YBOCS in the same direction (p <0.05 for each).
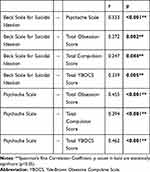 |
Table 5 The Relationship Between BSIS, YBOCS and PS Scores of OCD Patients |
In Table 6, we investigated the risk factors for suicide attempts with univariate and multiple logistic regression models. The univariate logistic regression model revealed that the effect of current aggressive, contamination, and past religious obsessions, the BSIS, and PS scores, avoidance, indecisiveness, and global severity subdimensions of the YBOCS were significant on suicide attempts (p <0.05 for each). The multivariate logistic regression analysis showed that only the PS score was predicting previous suicide attempts significantly (p = 0.043).
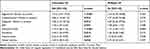 |
Table 6 Univariate and Multiple Logistic Regression Analysis of Factors Affecting Suicide Attempts |
Discussion
According to the World Health Organization (WHO), about 800 000 people die due to suicide every year,37 and suicide is a preventable cause of death. Therefore, suicidal ideation and attempts have an important place in OCD, as in other psychiatric disorders. The most important outcome of this study is determining the relationship between suicide and psychological pain in patients with OCD.
One of the most important theories put forward to prevent suicide and determine its predictors is the psychache theory.38 Psychache was investigated in many suicide-related studies after Shneidman’s17 pioneering definition. Verrocchio et al39 considered psychache as an important risk factor for suicide independent of the diagnosis of mental disorders. The mediating effect of psychache was demonstrated between perfectionism and suicidal ideations,40 between general distress and suicidal ideations,19 and between childhood traumas and suicidal ideations.41 Montemarano et al42 conducted a 4-year follow-up study that supported Shneidman’s model and pointed out that other factors were increasing the risk for suicide only when they were associated with psychache. In the Turkish population, previous studies revealed that the average PS score of patients with major depressive disorder was 43.98 ± 11.43,23 45.88 ± 10.44 of patients with bipolar disorder24 and 37.6 ± 14.28 of patients with schizophrenia.25 We found the mean score of PS as 37.6 ± 15.3 in the OCD and 23.6 ± 7.1 in the control group. The PS scores of the patients with OCD who had previous suicide attempts were significantly higher than those who had not (54.3 ± 6.7 and 33.9 ± 14.2, respectively). Besides, there was a significant positive correlation between YBOCS, BSIS, and PS. These data suggest that the severity of psychache and suicidal thoughts may increase as the severity of the OCD increases. Although the OCD patients included in our study were not diagnosed with comorbid depression, the association of psychological pain with suicide attempts supports the hypothesis that psychache is independent of the diagnosis.39 Our results also suggest that relieving psychache in patients with OCD may help to reduce suicide risk.
The results of the studies on the relationship between OCD symptoms and suicide risk differ. Repeating and trust seeking compulsions,9 symmetry/order obsessions and compulsions,1 and sexual/religious obsessions5 have been reported to be more frequent in patients with OCD who had previous suicide attempts and suicidal ideation. We found current aggressive, sexual obsessions, and past religious obsessions to be more frequent in OCD patients with previous suicide attempts. Kamath et al9 have found higher YBOCS obsession subscale scores in patients with OCD who had suicidal ideation and previous suicide attempts. Brown et al3 have determined a one-way relationship between OCD symptoms and suicidal ideation in a 6-year follow-up study. According to Brown et al,3 as the severity of OCD symptoms increased, the severity of suicidal ideation increased, but suicidal ideation did not affect OCD symptoms over the years. We found higher scores in avoidance, indecisiveness, global severity, and total obsession subdimensions of YBOCS, and also higher BSIS, PS, and total YBOCS scores in OCD patients with a history of previous suicide attempts. Hollander et al43 reported suicide behaviors that did not result in death in approximately 15% of OCD patients. In subsequent studies, Kamath et al9 reported past suicidal ideation in 59% of patients with OCD, current suicidal ideation in 28%, and suicide attempt history in 27%.44 These rates are three times higher than healthy individuals and are similar to other mental disorders such as bipolar disorder, schizophrenia, major depressive disorder, alcohol use disorder, and personality disorders.44 In a multicenter study, the rate of suicide attempts was 14.6% in OCD patients.45 We found lifetime suicide attempts to be 17.9% in OCD patients. We also found suicidal thoughts and lifetime suicide attempts to be significantly higher in the OCD group than the controls. Other comorbid mental disorders, especially mood disorders,9 personality disorders, and behavioral disorders affect the risk of suicide in OCD.43,46 Considering the confounding effects on suicide, we did not include patients with comorbid mental disorders in our study. Suicide attempts rates would be expected to be higher if patients diagnosed with comorbid mental disorders, particularly major depression, were included in the study.
Family history of suicide attempts, being single, and low socioeconomic status are sociodemographic variables related to suicide in patients with OCD.1,5 We did not find any significant relationship between sociodemographic variables and previous suicide attempts. There were also no relationships between the previous suicide attempts and the age of first symptoms and treatment. These data suggest that psychological pain rather than sociodemographic variables may be more important in the relationship between OCD and suicidality.
Our study has some strengths and limitations. We questioned whether patients had attempted suicide lifelong but did not classify suicide attempts as past and current. We also did not investigate the method and the severity of suicide attempts. Investigating a possible relationship between the level of psychological pain and the severity of suicide attempts in patients with OCD may be of interest for future studies. Follow-up studies may show more clearly the change in the level of psychological pain during the course OCD and whether it affects suicidal ideation. Only the inclusion of patients admitted to the psychiatry clinics of a tertiary clinic may limit the generalization of our results. Finally, the fact that we did not question hopelessness, which is an important risk factor for suicide, can be considered as another limitation of our study. The most important strength of our study is the direct evaluation of the relationship between psychological pain and suicide in OCD and the first demonstration of this relationship.
Conclusion
In conclusion, it is crucial to relieve the obsessions and compulsions because the severity of OCD can trigger suicidal ideation, but not only typical symptoms, but also attention to clinical variables such as psychological pain and tolerance to psychological pain will help to prevent suicide attempts and possible deaths in patients with OCD.
Disclosure
The authors reportno conflicts of interest in this work
References
1. Alonso P, Segalàs C, Real E, et al. Suicide in patients treated for obsessive – compulsive disorder: a prospective follow-up study. J Affect Disord. 2010;124(3):300–308. doi:10.1016/j.jad.2009.12.001
2. Ruscio AM, Stein DJ, Chiu WT, Kessler RC. The epidemiology of obsessive-compulsive disorder in the National Comorbidity Survey Replication. Mol Psychiatry. 2010;15(1):53–63. doi:10.1038/mp.2008.94
3. Brown LA, Wakschal E, Russman-Block S, et al. Directionality of change in obsessive compulsive disorder (OCD) and suicidal ideation over six years in a naturalistic clinical sample. J Affect Disord. 2019;245:841–847. doi:10.1016/j.jad.2018.11.006
4. Karakus G, Tamam L. Sleep and suicide relationship in patients with obsessive-compulsive disorder. Anatol J Psychiatry. 2018;19(1):37–44.
5. Torres AR, Ramos-Cerqueira AT, Ferrão YA, Fontenelle LF, Miguel EC. Suicidality in obsessive-compulsive disorder: prevalence and relation to symptom dimensions and comorbid conditions. J Clin Psychiatry. 2011;72(1):17–26. doi:10.4088/JCP.09m05651blu
6. Koran LM, Thienemann ML, Davenport R. Quality of life for patients with obsessive-compulsive disorder. Am J Psychiatry. 1996;153(6):783–788.
7. Khan A, Leventhal RM, Khan S, Brown WA. Suicide risk in patients with anxiety disorders: a meta-analysis of the FDA database. J Affect Disord. 2002;68(2–3):183–190. doi:10.1016/S0165-0327(01)00354-8
8. de la Cruz LF, Rydell M, Runeson B, et al. Suicide in obsessive–compulsive disorder: a population-based study of 36 788 Swedish patients. Mol Psychiatry. 2017;22(11):1626. doi:10.1038/mp.2016.115
9. Kamath P, Reddy YC, Kandavel T. Suicidal behavior in obsessive-compulsive disorder. J Clin Psychiatry. 2007;68(11):1741–1750. doi:10.4088/JCP.v68n1114
10. Khosravani V, Kamali Z, Ardakani RJ, Ardestani MS. The relation of childhood trauma to suicide ideation in patients suffering from obsessive-compulsive disorder with lifetime suicide attempts. Psychiatry Res. 2017;255:139–145. doi:10.1016/j.psychres.2017.05.032
11. Ching THW, Williams M, Siev J. Violent obsessions are associated with suicidality in an OCD analog sample of college students. Cogn Behav Ther. 2017;46(2):129–140. doi:10.1080/16506073.2016.1228084
12. Dell’Osso L, Casu G, Carlini M, Conversano C, Gremigni P, Carmassi C. Sexual obsessions and suicidal behaviors in patients with mood disorders, panic disorder and schizophrenia. Ann Gen Psychiatry. 2012;11(1):27. doi:10.1186/1744-859X-11-27
13. Velloso P, Piccinato C, Ferrao Y, et al. The suicidality continuum in a large sample of obsessive–compulsive disorder (OCD) patients. Eur Psychiatry. 2016;38:1–7. doi:10.1016/j.eurpsy.2016.05.003
14. Dhyani M, Trivedi JK, Nischal A, Sinha PK, Verma S. Suicidal behaviour of Indian patients with obsessive compulsive disorder. Indian J Psychiatry. 2013;55(2):161. doi:10.4103/0019-5545.111455
15. Orbach I, Mikulincer M, Gilboa-Schechtman E, Sirota P. Mental pain and its relationship to suicidality and life meaning. Suicide Life-Threatening Behav. 2003;33(3):231–241. doi:10.1521/suli.33.3.231.23213
16. Shneidman ES. The psychological pain assessment scale. Suicide Life-Threatening Behav. 1999;29(4):287–294. doi:10.1111/j.1943-278X.1999.tb00524.x
17. Shneidman ES. Commentary: suicide as psychache. J Nerv Ment Dis. 1993;181(3):145–147. doi:10.1097/00005053-199303000-00001
18. Patterson AA, Holden RR. Psychache and suicide ideation among men who are homeless: a test of Shneidman’s model. Suicide Life-Threatening Behav. 2012;42(2):147–156. doi:10.1111/j.1943-278X.2011.00078.x
19. Campos RC, Gomes M, Holden RR, Piteira M, Rainha A. Does psychache mediate the relationship between general distress and suicide ideation? Death Stud. 2017;41(4):241–245. doi:10.1080/07481187.2016.1251510
20. Troister T, Holden RR. A two-year prospective study of psychache and its relationship to suicidality among high-risk undergraduates. J Clin Psychol. 2012;68(9):1019–1027. doi:10.1002/jclp.21869
21. Pereira EJ, Kroner DG, Holden RR, Flamenbaum R. Testing Shneidman’s model of suicidality in incarcerated offenders and in undergraduates. Pers Individ Dif. 2010;49(8):912–917. doi:10.1016/j.paid.2010.07.029
22. Mee S, Bunney BG, Bunney WE, Hetrick W, Potkin SG, Reist C. Assessment of psychological pain in major depressive episodes. J Psychiatr Res. 2011;45(11):1504–1510. doi:10.1016/j.jpsychires.2011.06.011
23. Demirkol ME, Güleç H, Çakmak S, et al. Reliability and validity study of the Turkish version of the Psychache Scale. Anatol J Psychiatry. 2018;19(1):14–20. doi:10.5455/apd.292935
24. Demirkol ME, Güleç H, Tamam L, et al. Reliability and validity of Mee-Bunney Psychological Pain Assessment Scale Turkish version. Curr Psychol. 2019:1–8. doi:10.1007/s12144-019-00400-z
25. Demirkol ME, Tamam L, Namli Z, Karaytug MO, Ugur K. Association of psychache and alexithymia with suicide in patients with schizophrenia. J Nerv Ment Dis. 2019;207(8):668–674. doi:10.1097/NMD.0000000000001023
26. Rudd MD. Fluid vulnerability theory: a cognitive approach to understanding the process of acute and chronic suicide risk. In: Ellis TE, editor. Cognition and Suicide. Washington: American Psychological Association; 2006;355–368.
27. American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders.
28. Williams JBW. A structured interview guide for the Hamilton Depression Rating Scale. Arch Gen Psychiatry. 1988;45(8):742–747. doi:10.1001/archpsyc.1988.01800320058007
29. Faul F, Erdfelder E, Buchner A, Lang AG. Statistical power analyses using G Power 3.1: tests for correlation and regression analyses. Behav Res Methods. 2009;41(4):1149–1160. doi:10.3758/BRM.41.4.1149
30. Beck AT, Kovacs M, Weissman A. Assessment of suicidal intention: the Scale for Suicide Ideation. J Consult Clin Psychol. 1979;47(2):343. doi:10.1037/0022-006X.47.2.343
31. Ozcelik HS, Ozdel K, Bulut SD, Orsel S. The reliability and validity of the Turkish version of the Beck Scale for Suicide Ideation (Turkish BSSI). Bull Clin Psychopharmacol. 2015;25(2):141–150. doi:10.5455/bcp.20141214105009
32. Zimmerman M, Martinez JH, Young D, Chelminski I, Dalrymple K. Severity classification on the Hamilton depression rating scale. J Affect Disord. 2013;150(2):384–388. doi:10.1016/j.jad.2013.04.028
33. Akdemir A, Örsel S, Dağ İ, Türkçapar H, İşcan N, Özbay H. Hamilton Depresyon Derecelendirme Ölçeği (HDDÖ)’nin geçerliği, güvenirliği ve klinikte kullanımı. Psikiyatr Psikol Psikofarmakol (3P) Derg. 1996;4(4):251–259.
34. Goodman WK, Price LH, Rasmussen SA, et al. The Yale-Brown Obsessive Compulsive Scale: II. Validity. Arch Gen Psychiatry. 1989;46(11):1012–1016. doi:10.1001/archpsyc.1989.01810110054008
35. Karamustafalıoğlu O, Üçışık AM, Ulusoy M, Erkmen H. Yale-Brown Obsesyon Kompulsiyon Derecelendirme Ölçeği’nin Türkçe’de geçerlik ve güvenirlik çalışması. Ulusal Psikiyatri Kongresi Özet Kitabi. 1993;29.
36. Holden RR, Mehta K, Cunningham EJ, McLeod LD. Development and preliminary validation of a scale of psychache. Can J Behav Sci. 2001;33(4):224. doi:10.1037/h0087144
37. World Health Organization. National Suicide Prevention Strategies: Progress, Examples and Indicators. Geneva: WHO; 2018. Available from: https://www.who.int/mental_health/suicide-prevention/national_strategies_2019/en/.
38. Zou Y, Li H, Shi C, Lin Y, Zhou H, Zhang J. Efficacy of psychological pain theory–based cognitive therapy in suicidal patients with major depressive disorder: a pilot study. Psychiatry Res. 2017;249:23–29. doi:10.1016/j.psychres.2016.12.046
39. Verrocchio MC, Carrozzino D, Marchetti D, Andreasson K, Fulcheri M, Bech P. Mental pain and suicide: a systematic review of the literature. Front Psychiatry. 2016;20(7):108. doi:10.3389/fpsyt.2016.00108
40. Flamenbaum R, Holden RR. Psychache as a mediator in the relationship between perfectionism and suicidality. J Couns Psychol. 2007;54(1):51–61. doi:10.1037/0022-0167.54.1.51
41. Zarrati I, Bermas H, Sabet M. The relationship between childhood trauma and suicide ideation: mediating role of mental pain. Ann Mil Heal Sci Res. 2019;1–7. doi:10.5812/amh.89266
42. Montemarano V, Troister T, Lambert CE, Holden RR. A four-year longitudinal study examining psychache and suicide ideation in elevated-risk undergraduates: a test of Shneidman’s model of suicidal behavior. J Clin Psychol. 2018;1–13. doi:10.1002/jclp.22639
43. Hollander E, Greenwald S, Neville D, Johnson J, Hornig CD, Weissman MM. Uncomplicated and comorbid obsessive-compulsive disorder in an epidemiologic sample. CNS Spectr. 1998;3(S1):10–18. doi:10.1017/S1092852900007148
44. Balci V, Sevincok L. Suicidal ideation in patients with obsessive–compulsive disorder. Psychiatry Res. 2010;175(1–2):104–108. doi:10.1016/j.psychres.2009.03.012
45. Dell’Osso B, Benatti B, Arici C, et al. Prevalence of suicide attempt and clinical characteristics of suicide attempters with obsessive-compulsive disorder: a report from the International College of Obsessive-Compulsive Spectrum Disorders (ICOCS). CNS Spectr. 2018;23(1):59–66. doi:10.1017/S1092852917000177
46. Apter A, Horesh N, Gothelf D, et al. Depression and suicidal behavior in adolescent inpatients with obsessive compulsive disorder. J Affect Disord. 2003;75(2):181–189. doi:10.1016/S0165-0327(02)00038-1
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
