Back to Archived Journals » Neuroscience and Neuroeconomics » Volume 5
Primary progressive aphasia: conceptual evolution and challenges
Received 19 December 2015
Accepted for publication 26 February 2016
Published 29 April 2016 Volume 2016:5 Pages 9—18
DOI https://doi.org/10.2147/NAN.S102848
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor SH Annabel Chen
Cristian E Leyton, Kirrie J Ballard
Faculty of Health Sciences, The University of Sydney, Lidcombe, NSW, Australia
Abstract: Since the modern description of primary progressive aphasia (PPA) more than 30 years ago, the interest in neurodegenerative conditions that selectively target the language network has grown exponentially. Fueled by advances in neuroimaging and biomarkers, progress in the field has brought new insights into clinical categorization, neural correlates of language, and pathological mechanisms of progression in PPA. Of relevance, the inception of logopenic progressive aphasia as an atypical presentation of Alzheimer's disease and the formalization of the international diagnostic criteria and classification of PPA represent milestones in the field. Paradoxically, those advances have also brought controversy and challenges. The application of the current classification in cases with mixed or very mild language deficits is still challenging, while the accurate pathological prediction at the individual level remains elusive. In addition, it is more evident now that nonlanguage deficits, including other cognitive and motor deficits, can appear early on and potentially assist in the differential diagnosis. From a historical perspective, this review addresses the conceptual evolution of PPA and the contribution that clinical refinements, cognitive neuropsychology, and pathology have made to the field.
Keywords: primary progressive aphasia, nonfluent variant, logopenic variant, frontotemporal lobar degeneration, frontotemporal dementia, semantic dementia, Alzheimer's disease
Introduction
The term primary progressive aphasia (PPA) refers to a progressive neurodegenerative disorder that manifests initially as a seemingly isolated insidious loss of the ability to comprehend language, retrieve and form words, and/or formulate sentences. Since its modern inception more than 3 decades ago,1 our knowledge on clinical manifestations, molecular pathology, and genetics of this syndrome has grown exponentially. Paradoxically, the increasing knowledge has also brought controversy and challenges, some of which will be addressed in this brief review. We will also outline the historical evolution of PPA and discuss uncertain areas and future directions in the field.
Historical outlook and conceptual developments in PPA
The dawn of the concept of PPA was marked over a century ago when Pick et al2,3 described a series of cases with pronounced language impairment (ie, aphasia) due to nonspecific neuropathology. Contrasting with the prevailing idea of diffuse brain atrophy as the main correlate for cognitive impairment, Pick et al, in 18922 were the first to intuit the existence of circumscribed forms of “senile dementia”. Accordingly, the most prominent clinical manifestation at onset results from relatively focal brain atrophy. At the beginning of the 20th century, Alzheimer4 described Auguste, who also presented with progressive aphasia and behavior changes; however, unlike Pick’s description, this patient displayed severely impaired memory, and more importantly, a distinctive neuropathology typified by widely distributed amyloid plaques and neurofibrillary tangles.4,5 During the first half of the past century, successive clinical and pathological series6–9 confirmed the notion that Pick’s clinical description corresponded to a separate clinical–pathological entity lacking the distinctive histological features previously described by Alzheimer. Those series nevertheless emphasized personality changes and social maladjustments in which loss of cultural or ethical standards were regarded as predominant features. Despite focusing on behavioral changes, those first clinical descriptions were highly precise and defined aphasic profiles that differed from those with typical Alzheimer’s disease (AD).10 A notable example is provided by a clinicopathological report of a 59-year-old woman who, in addition to being paranoid, displayed notorious word-finding difficulties and circumlocutory language. Her language examination revealed marked anomia and misspelling, but preservation of word repetition ability and no difficulties in articulatory agility. Her autopsy revealed left-sided atrophy of the anterior temporal lobe with nonspecific neuronal loss.11 All these features astonishingly coincide with the modern description of the semantic variant of PPA that was to emerge almost 50 years later.12
Although emphasis on behavioral symptoms prevailed for over 50 years, the concept of language-based progressive disorder was kindled by Mesulam.1 In the 1980s, Mesulam1 reported a series of six cases with progressive aphasia as the initial and sole manifestation of disease, where the aphasia was not explained by focal neurological disorders such as stroke or brain tumors. One case underwent brain biopsy, showing nonspecific neuronal loss but absence of Alzheimer’s pathology or vascular changes, suggesting that this entity was pathologically and clinically separate from AD. Mesulam13 proposed a definition of this presentation, still widely accepted, in which aphasia is the most salient deficit for at least the first 2 years after the onset of initial symptoms and has a major impact on communication abilities. In addition, it was argued that aphasia should have a gradual progression not attributable to stroke or other pathological conditions, but attributable to neurodegeneration of the perisylvian region of the left hemisphere.13
Although initially regarded as a unitary entity, the increasing number of reports demonstrated that the term PPA was being applied to a wide spectrum of cases that could be roughly dichotomized as fluent or nonfluent aphasia,14,15 largely mirroring classic descriptions of aphasic cases due to stroke.16 However, aphasic syndromes induced by neurodegeneration are not determined by the anatomy of vascular supply. Rather, they result from a complex interplay between the slow destruction of neural populations and compensatory reorganizations of synaptic circuitry.17 Because linguistic profiles in PPA are not stable, but evolve as pathology spreads, the analysis of language deficits in PPA has turned out to be complex. In addition, classical aphasic syndromes, based mainly on clinicoanatomical correlations established in acute cerebrovascular lesions, may not necessarily account for the whole spectrum of linguistic deficits in PPA.17 Despite this complexity, concepts that emerged from cognitive neuropsychology have provided a theoretical framework that enables us to organize the progressive linguistic deficits of PPA into coherent neurocognitive syndromes.
Undeniably, cases with progressive fluent aphasia profited the most few years before Mesulam’s seminal description when, in 1975, Warrington18 suggested that seemingly unrelated deficits, “amnesic aphasia” and associative agnosia, were explained by a breakdown of a common cognitive system, namely, disintegration of semantic memory. In 1989, the label semantic dementia was introduced by Snowden et al19 to reflect both the semantic deficit and the progressive nature of this disorder. Soon after the syndrome was comprehensively characterized by Hodges et al,12 who defined its core features and drew attention to the consistent anterior temporal lobe atrophy and association with non-AD pathology.
The nonfluent PPA cases, on the other hand, display a wide range of disturbances, which can include phonological errors, oversimplification of linguistic structures and/or frank grammatical errors in spontaneous speech, effortful and halting speech, distorted articulation, and prosodic changes.14,20 In contrast to fluent cases, the myriad of “nonfluent” language manifestations can hardly be conceptualized as a result of damage to a single core cognitive system. Instead, reflecting the multidimensional quality of language fluency, specific aspects of language and speech output have been emphasized. While some authorities focused on the breakdown of syntactic (grammatical) components of speech as a key language deficit,13,15 others drew their attention to the impaired capacity of planning or programming movements for speech, which results in apraxia of speech.21,22 The discrepancy among experts not only reflects the heterogeneity of nonsemantic patients, but it also reveals the complexity of key mechanisms that give rise to nonfluency. As such, it was clear that pooling nonsemantic cases under the rubric of nonfluency represented an oversimplification of the reality.
Advances in neuroimaging and biomarkers also made it evident that the underlying pathology of PPA was heterogeneous, comprising not only pathologies of the spectrum of frontotemporal lobar degeneration (FTLD) as initially described, but also Alzheimer pathology.23,24 The recognition of AD as the cause of pathology in up to a third of PPA cases has been arguably one of the most important and controversial discoveries. It not only confirmed the diversity of AD manifestations – in this instance salient language deficits instead of impaired day-to-day memory – but it also illustrated how elusive the identification of this pathology can be. Notwithstanding, the identification of PPA cases with AD was improved with the clinical and imaging characterization of a third variant, now formally known as logopenic progressive aphasia.25 These cases, most of whom had been previously forced into the “nonfluent” category, display an intermediate aphasic syndrome characterized by word-finding difficulties with hesitations that interrupt the flow of conversation, anomia, and marked impairment in sentence repetition. Unlike other nonfluent cases, logopenic cases have been reported as having neither impaired motor aspects of speech nor impaired grammatical processing, whereas they present with anomia, like semantic dementia, but in the context of preserved semantic knowledge. As the variants of PPA began to take form, with advances in behavioral, neuroimaging, and pathology descriptions, the community realized the need for an international consensus on diagnostic criteria.
The inception of the international consensus criteria
In spite of the advances in PPA descriptions and the formal definition of the two aphasic presentations in FTLD,26 independent research groups emphasized partial aspects of these conditions, and varied terminology was being used to refer to a single deficit, raising confusion in clinicians and hindering research communication and international collaboration. The absence of a common framework motivated the formalization of international consensus criteria for the diagnosis and classification of PPA, which provided operational definitions of language and speech deficits and classified PPA into three clinical variants.27 In this approach, the variants, namely, semantic (sv-PPA), nonfluent/agrammatic (nfv-PPA), and logopenic (lv-PPA), are defined based on the presence or absence of core language and speech deficits. Cases with sv-PPA display marked anomia and difficulties in recognizing not only words, but also objects, people, and tunes, which are all attributed to degradation of semantic representations. By contrast, cases with nfv-PPA show preservation of semantic knowledge but morphosyntactic deficits including omission of grammatical function words (eg, a, the, she, is, to) and degradation of syntactic rules and structures leading to agrammatism and oversimplification of language output. Alternatively, nfv-PPA can present with effortful speech, loss of prosody (ie, control of relative timing and intonational aspects of speech), and articulatory errors, all of which result from disruption of motor planning or speech execution, that is, a sensorimotor speech disorder rather than, or alongside, an aphasia. Unlike other variants, lv-PPA cases display relative preservation of semantic representations and motor aspects of speech production, but instead show marked word-finding difficulties, anomia, and striking difficulties in sentence repetition.
Evidence from neuroimaging studies implicates distinct left hemispheric brain regions as responsible for the core language deficits in each variant. On the basis of that, the criteria include imaging findings to support features for each variant. Cases with sv-PPA display changes of structure, metabolism, or perfusion in the anterior part of the temporal lobes, nfv-PPA in the left inferior frontal gyrus, insula, premotor, and/or supplementary motor areas, and in lv-PPA, atrophy is focused on the left temporoparietal junction.
Of relevance, the proposed criteria also relate each variant with a specific pathology. The sv-PPA is strongly associated with microscopic inclusions of transactive response DNA-binding protein of 43 kDa (TDP-43), the nfv-PPA with tau inclusions, and a large proportion of lv-PPA cases with Alzheimer’s pathology.28–30 Despite these seemingly clear-cut associations, a number of clinical and pathological series demonstrate that some cases show unexpected pathological associations and not all PPA cases can be classifiable into one of the three variants. This raises issues about the biological validity and applicability of this tripartite approach.31 Although different solutions have been proposed to overcome this issue, the optimal approach is still under debate. Whereas some groups pose the subdivision into new subvariants so as to better refine each PPA syndrome and thus improve diagnostic accuracy and pathological prediction,32 others disregard the existence of lv-PPA and restrict the classification into only two variants.31 These opposite views remain unsolved and open the old taxonomic dispute between “lumpers” and “splitters”.
Is PPA a unitary syndrome or an artificial conjunction of distinctive entities?
Despite the formalization of the three clinical variants, there is no general agreement on how many independent aphasic syndromes form the spectrum of possible PPA presentations. One stream of opinions emphasizes the clinical integrity of PPA, whereby each clinical PPA presentation constitutes phenotypic variation of a single disease process. This view is consistent with the notion that neurodegenerative diseases tend to target specific populations of functionally related neurons that comprise large-scale brain networks.33 Briefly, this view claims that although PPA variants have a distinctive profile of language deficits and specific pathological associations, the primary target of neurodegeneration is the language and/or motor speech network. In this view, phenotypical diversity must be understood as a result of the partial and variable destruction of selective components of the network.34,35 As neurodegeneration spreads throughout the network, the distinctive profiles of language deficits blur and global language dysfunction emerges, akin to the global aphasia described for vascular etiology,16 with the presence of features from multiple subtypes. Mirroring language deterioration, longitudinal studies have in fact demonstrated that brain atrophy, albeit initially circumscribed, spreads throughout the left-sided language network as the disease progresses.36–38
The lack of a clear-cut syndrome definition occurring in advanced cases has been one of the main difficulties for establishing reliable clinicopathological associations. Although dual pathology can explain some overlapping PPA syndromes,39 in most instances unclassifiable cases that are due to mixed language deficits, and thus more advanced, have AD pathology,40 consistent with the eventual pervasive nature of this pathology. In accordance with this suggestion, lv-PPA, which is strongly associated with Alzheimer’s pathology, tends to deteriorate more rapidly than other PPA variants,41 exhibits more widespread pathological burden than cases with other types of pathology or cases with typical AD presentation,42 and progresses with more extended changes in white and gray matter over time than other PPA variants.43,44 Longitudinal studies in the other variants, in contrast, have demonstrated that sv-PPA presents the slowest rate of progression and semantic disintegration remains the most salient deficit and declines in a fairly stereotyped manner.41,45,46 Similarly, expressive language deficits in nfv-PPA remains the most salient clinical problem, and before other linguistic deficits become prominent, extrapyramidal deficits often emerge.47,48 The widespread and heterogeneous clinical involvement in lv-PPA has been the main motivation to suggest that this variant should be excluded from the spectrum of PPA presentations. On the basis of a data-driven approach, one systematic analysis of linguistic deficits in PPA demonstrated that while nfv-PPA and sv-PPA conform to discrete linguistic syndromes, lv-PPA showed an insufficiently distinctive clinical pattern to be regarded as an independent clinical syndrome.31 Other studies have argued that lv-PPA is heterogeneous, and several endophenotypes with slightly different patterns of atrophy distribution, disease progression, and likelihood of AD can be distinguished.43,49 Despite the diversity of clinical presentations, those studies revealed that the vast majority fall within the “typical” logopenic syndrome and have evidence of AD, whereas those without evidence of Alzheimer pathology often develop impaired movement, such as extrapyramidal motor features, that warrant an alternative diagnosis such as progressive supranuclear palsy.43
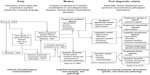
In contrast to the argument for a unitary PPA syndrome, the “splitter” perspective seeks to refine clinical syndromes as finely as possible so that clusters of patients with similar behavioral profiles can be accurately identified. This approach was first posited by Kertesz et al,50 who distinguished six possible clinical presentations of PPA: anomic, logopenic, aphemic, nonfluent aphasia with definite agrammatism, semantic aphasia, and mute. Not so different from Kertesz’s classifications, the group at the Mayo Clinic subsequently proposed a classification system with six clinical variants, based on a comprehensive clinical speech and language assessment and neuroimaging analysis in a large cohort.32 In contrast to other classification systems, this group first divides cases with predominantly movement-based speech alterations, the so-called primary progressive apraxia of speech,51 from those cases that evince predominantly linguistic involvement indicative of an aphasia. Therefore, the previously single entity of nfv-PPA is separated into two variants: progressive agrammatic aphasia and progressive apraxia of speech. This group’s descriptions of sv-PPA and lv-PPA resemble those of the international diagnostic criteria. However, they consider unclassifiable cases and cases with pure anomia as separate variants.32,51 Although the authors demonstrated clinical–neuroanatomical coherence in each variant, and a clinicopathological series with refined syndrome characterization revealed some comparable associations,52 it is not clear if this cross-sectional taxonomy remains stable in a long-term follow-up. Longitudinal studies tracking deficits and atrophy changes over years as well as pathological confirmation may confirm the clinical applicability and biological validity of this proposal against others. Figure 1 summarizes the conceptual evolution of PPA, starting with the first descriptions of cases with a progressive cognitive disorder, followed by the modern inception of PPA, to current classification proposals.
Contributions of genetic advances
The proportion of PPA cases with significant family history of dementia or related disorders ranges considerably depending upon their clinical presentation.53–56 While no more than a fifth of sv-PPA cases have family history of dementia or amyotrophic lateral sclerosis (ALS), up to a third of nfv-PPA cases have significant family history.55,57 As lv-PPA has been recently recognized, few studies have directly addressed genetic factors, but the Apo ε 4 polymorphism is not as relevant here as it is for cases with typical AD.58,59 The finding that most PPA familial cases show an autosomal dominant pattern of inheritance has prompted the search for specific gene mutations. Almost 20 years ago, the first mutation mapped to 17q21 chromosome was a gene that encodes the microtubule-associated protein tau (MAPT).60–62 Soon after it was recognized that this mutation was present in less than a half of cases and that neuropathology in many cases displayed no tau inclusions.63,64 This finding fueled the search for other mutations that were found almost a decade later with the identification of progranulin (GRN) mutation, also mapped on chromosome 17q21.65,66 Although mutations in chromosome 17 explain more than a third of familial cases,57 a substantial number, and especially those with family history of ALS, remained unexplained. It was not until the identification of a novel repeat expansion of the GGGGCC hexanucleotide in the chromosome 9 open reading frame 72 (C9orf72) that a high proportion of cases with familial FTLD (12%) or familial ALS (22.5%) could be explained.67,68
In spite of the recent advances in genetics, a notable difficulty in the field has been the poor correspondence between specific genotypes and aphasic phenotypes, which are largely derived from the description of sporadic cases. Nonlanguage symptoms are often present in genetic cases and have proven useful for relating some gene mutations to specific clinical phenotypes. For example, behavioral changes and parkinsonism alongside language deficits are the main clinical manifestations in cases with MAPT mutations.69 Although the aphasic phenotype in these cases is usually nonfluent, a fluent presentation similar to sv-PPA has also been described. 70–72 The clinical phenotype associated with GRN mutations is even more diverse than the one associated with MAPT mutations. However, like MAPT mutations, behavioral changes are commonly encountered and often accompanied with extrapyramidal features.73,74 Aphasia may also be present in cases with GRN mutations and can take a number of forms.75–77 The lv-PPA pattern seems to be the most common,78,79 with cases often exhibiting phonological disintegration, lexical retrieval problems, anomia with a variable degree of single-word comprehension deficits and reduction in phonological working memory resources, and no evidence of apraxia of speech.75,77,80
In cases with C9orf72 hexanucleotide expansion, like other mutations, the main clinical phenotype is behavioral change, often associated with psychotic symptoms. ALS may or may not co-occur. However, the clinical phenotypical spectrum of this expansion is rapidly growing.81 Although C9orf72 expansion is now recognized as the main cause of familial cases with behavioral FTLD, language deficits have also been described in most series82–84 – for an exception, see Boeve et al.85 The most common language presentation is nfv-PPA, whereas sv-PPA is rarely, if ever, associated with this expansion. Finally, other extremely rare gene mutations can initially manifest as aphasia, such as valosin-containing protein gene, which causes inclusion body myopathy associated with Paget’s disease of bone and FTLD.86 In these cases, the language disorder is usually accompanied by other cognitive or muscle disorder and so may not strictly be classified as PPA.87
Associated symptoms
Another emerging issue in the field of PPA, as more sensitive assessment tools are developed, is the increasing awareness that some cases do indeed present with nonlinguistic impairments in the early stages of the disease, including deficits in motor and other cognitive domains. Although accompanying impairments are overshadowed by language deficits and cause no major functional impact on patients, their detection can potentially assist in the differential diagnosis of PPA upon initial presentation to the clinic.88 For instance, the distinction between nfv-PPA and lv-PPA can be complicated by the presence of similar appearing linguistic deficits, or alternatively, by the presence of minor alterations of expressive language that are difficult to typify.89 In these situations, differential diagnosis can be facilitated by detection of nonverbal impairments. Specifically, some nfv-PPA cases exhibit emotion processing disturbances affecting detection of negative emotions,90 while many lv-PPA cases show subtle impairment in nonverbal episodic memory,90 orientation,91 and executive function.92
Similarly, the presence of specific motor signs like limb myoclonic jerks, albeit rare, can be highly specific to Alzheimer pathology combined with Lewy body inclusions. In contrast, the emergence of extrapyramidal signs (eg, bradykinesia and rigidity), more often seen in nfv-PPA than in lv-PPA,93 prompts consideration of non-Alzheimer pathologies.43 Notably, virtually all cases with apraxia of speech develop bradykinesia at some point in the disease progression.94 Denoting their common association with tau pathologies, a proportion of cases initially classified as nfv-PPA are later diagnosed with either progressive supranuclear palsy or corticobasal degeneration.95 These commonalities, comprising clinical features and pathological changes, have fueled controversy over the nosological identity of nfv-PPA. While some researchers advocate for an integrative approach whereby all these possible clinical presentations are referred to as a “Pick’s complex”,96 others emphasize the usefulness of specific clinical markers and anatomical signatures to better define each clinical entity.97 The presence of nonlanguage deficits can also have direct clinical implications for differential diagnosis. The presence of personality changes and face recognition deficits (prosopagnosia) are often encountered in sv-PPA. These changes correlate with gray matter loss in the right temporal lobe, which is involved in nonverbal processing including theory of mind.98,99 Around a third of sv-PPA cases display predominant right anterior temporal lobe atrophy, accompanied by behavioral changes and prosopagnosia; however, given their disproportionate behavioral changes over language deficits, these cases are not formally included in the category of sv-PPA. Evidence from a longitudinal cohort, however, demonstrates that those cases develop marked language deficits, demonstrating that irrespective of the initial clinical presentation, all sv-PPA cases evolve into a similar syndrome at the neural and behavioral level.45 This convergent clinical progression shows not only the common nosology in both sv-PPA presentations, but it also suggests the relevance of observing the clinical trajectory to refining diagnosis. Of clinical importance, unlike other variants, almost all cases with sv-PPA develop some degree of behavioral symptoms such as agitation and delusions that can become disruptive and require pharmacological intervention.100 This fact prompts clinicians to monitor patients on a regular basis to allow early identification of nonlinguistic changes and advising of caregivers on mitigation of disruptive behaviors and prognosis.
Future directions
One of the challenges in the field is the identification of the fundamental neurocognitive mechanisms and the neuro-correlates that underpin each linguistic syndrome. Sv-PPA represents a formidable achievement on this, as the integration of descriptions from neurocognitive, linguistic, neuroanatomical, and pathological studies made possible the delineation of a robust clinicopathological entity.46 This description would have been impossible without advances in cognitive neuro-psychology that provided the theoretical framework to integrate seemingly unrelated cognitive manifestations under a unitary cognitive system.101 In addition, the capacity of associating core deficits with discrete brain regions has contributed to reveal language–brain relationships and to identify a putative anatomical signature in each variant. In the aforementioned example, progressive loss of semantic representations is mostly associated with bilateral thinning in temporal poles, regions that play a crucial role in semantic processing.
The anatomical basis for concomitant motor speech disorders in cases with nfv-PPA, however, remains controversial, with multiple imaging studies demonstrating the relevance of cortical regions other than Broca’s area. While some highlight the anterior left insula,102 others suggest a role for the superior lateral premotor cortex, bilateral supplementary motor area,51,103,104 and basal ganglia.105 Although the clinical identification of a single neurocognitive process that underpins apraxia of speech remains not entirely defined, behavioral reaction time and neuroimaging analyses suggest that impaired specification of temporal articulatory goals for sequences of speech sounds104,106 possibly is due to weak connectivity between right and left premotor regions, thereby preventing high fidelity integration of feedback and feedforward motor commands.107
Another attempt in identifying coherent clinical–neuroanatomical–pathological markers in PPA is posited by phonological errors or phoneme misplacement in otherwise well-articulated words. This deficit is encountered in lv-PPA cases with presumed AD and has been proposed as a putative clinical marker of lv-PPA.105 Interestingly, this deficit is associated with left superior temporal gyrus atrophy, a region involved in phonological processing that then can potentially be the anatomical signature of lv-PPA.108 Taken together, this converging clinical and anatomical evidence points to phonologic disintegration as the main neurocognitive system affected in lv-PPA, which could explain the co-occurrence of phonologic errors and the reduced phonologic short-term memory that causes impairment of sentence repetition.109
Although, in comparison with the behavioral presentation of FTLD, PPA cases show less frequent family history of dementia and a lower proportion of cases with identified genetic mutations, still this area of research is developing and facing some challenges. It is not clear to what extent the international classification can account for the clinical phenotype arising from these mutations and genotype-language phenotype associations are not yet fully established.
Patients and relatives eagerly await treatments that can halt or delay the progression of these conditions. Refinements in clinical diagnosis and biomarkers are of paramount importance to trial effective drugs targeted to specific pathologies. In particular, PPA cases, given their clinical diversity and pathological heterogeneity, pose a serious challenge to these ambitions. Nevertheless, an increasing area of interest in the field has been the development of behavioral therapies aimed to ameliorate or improve language deficits. Aside from drugs targeting specific pathologies, behavioral interventions following different approaches have been attempted in PPA.110 To date, there are very few studies of low-level evidence investigating behavioral intervention for the speech and language impairments in PPA. All have appropriately applied treatments previously designed to target specific impairments observed in stroke-related aphasia, such as word-finding difficulty or sentence construction and discourse problems.111,112 These preliminary studies are providing promising directions for larger scale trials, especially in the period of the disease when language symptoms predominate and cognition is relatively intact. More information for professionals on treatments and support to patients and relatives can be found in web pages (http://www.ppaconnection.org, http://www.theaftd.org/life-with-ftd/support-for-caregivers/caregiver-support-groups).
Finally, careful scientific investigations are discovering cognitive and linguistic susceptibility factors that modulate the clinical expression of common conditions such as AD. For instance, the antecedent of learning disability has been found more often in cases with PPA.113,114
Concluding remarks
The wide phenotypical diversity in PPA offers a natural paradigm to investigate the complexity of the speech and language systems and the neural networks underpinning these uniquely human abilities. By developing our understanding of these systems and how they break down, we will be better able to detect and differentiate impairments early in disease progression, develop systematic hypotheses about type and distribution of pathology, and link patients with emerging pharmaceutical and neurobehavioral clinical trials to preserve function, independence, and societal participation further into the disease’s course.
Acknowledgments
A DVC University of Sydney Postdoctoral Fellowship (Project ID: 162153 to CEL) and an Australian Research Council Future Fellowship (FT120100355 to KJB).
Disclosure
The authors report no conflicts of interest in this work.
References
Mesulam MM. Slowly progressive aphasia without generalized dementia. Ann Neurol. 1982;11(6):592–598. | |
Pick A, Girling DM, Berrios GE. On the relationship between senile cerebral atrophy and aphasia. Hist Psychiatr. 1994;5(20):542–547. | |
Pick A, Girling DM, Berrios GE. On the symptomatology of left-sided temporal lobe atrophy. Hist Psychiatr. 1997;8(29):149–159. | |
Alzheimer A. Über eigenartige Krankheitsfälle des späteren Alters. [On certain peculiar diseases of old age]. Hist Psychiatr. 1991;2(5):74–101. German. | |
Maurer K, Volk S, Gerbaldo H. Auguste D and Alzheimer’s disease. Lancet. 1997;349(9064):1546–1549. | |
Ferraro A, Jervis GA. Pick’s disease: clinicopathologic study with report of two cases. Arch Neurol Psychiatry. 1936;36(4):739–767. | |
Lowenberg K. Pick’s disease: a clinicopathologic contribution. Arch Neurol Psychiatry. 1936;36(4):768–789. | |
Davison C. Circumscribed cortical atrophy in the presenile psychoses – Pick’s disease: a clinicopathologic study. Am J Psychiatry. 1938;94(4):801–818. | |
Nichols IC, Weigner WC. Pick’s disease – a specific type of dementia. Brain. 1938;61(3):237–249. | |
Kahn E, Thompson LJ. Concerning Pick’s disease. Am J Psychiatry. 1934;90(5):937–946. | |
Malamud N, Boyd DA Jr. Pick’s disease with atrophy of the temporal lobes: a clinicopathologic study. Arch Neurol Psychiatry. 1940; 43(2):210–222. | |
Hodges JR, Patterson K, Oxbury S, Funnell E. Semantic dementia. Progressive fluent aphasia with temporal lobe atrophy. Brain. 1992;115(Pt 6):1783–1806. | |
Mesulam MM. Primary progressive aphasia. Ann Neurol. 2001;49(4):425–432. | |
Hodges JR, Patterson K. Nonfluent progressive aphasia and semantic dementia: a comparative neuropsychological study. J Int Neuropsychol Soc. 1996;2(6):511–524. | |
Grossman M, Mickanin J, Onishi K, et al. Progressive nonfluent aphasia: language, cognitive, and PET measures contrasted with probable Alzheimer’s disease. J Cogn Neurosci. 1996;8(2):135–154. | |
Goodglass H, Kaplan E. The Assessment of Aphasia and Related Disorders. 2nd ed. Philadelphia, PA: Lea and Febiger; 1983. | |
Sonty SP, Mesulam MM, Thompson CK, et al. Primary progressive aphasia: PPA and the language network. Ann Neurol. 2003;53(1):35–49. | |
Warrington EK. The selective impairment of semantic memory. Q J Exp Psychol. 1975;27(4):635–657. | |
Snowden JS, Goulding PJ, Neary D. Semantic dementia: a form of circumscribed cerebral atrophy. Behav Neurol. 1989;2:167–182. | |
Turner RS, Kenyon LC, Trojanowski JQ, Gonatas N, Grossman M. Clinical, neuroimaging, and pathologic features of progressive nonfluent aphasia. Ann Neurol. 1996;39(2):166–173. | |
Duffy JR. Apraxia of speech in degenerative neurologic disease. Aphasiology. 2006;20(6):511–527. | |
Ogar J, Slama H, Dronkers N, Amici S, Gorno-Tempini ML. Apraxia of speech: an overview. Neurocase. 2005;11(6):427–432. | |
Tyrrell PJ, Warrington EK, Frackowiak RS, Rossor MN. Heterogeneity in progressive aphasia due to focal cortical atrophy. A clinical and PET study. Brain. 1990;113(Pt 5):1321–1336. | |
Knibb JA, Xuereb JH, Patterson K, Hodges JR. Clinical and pathological characterization of progressive aphasia. Ann Neurol. 2006; 59(1):156–165. | |
Gorno-Tempini ML, Dronkers NF, Rankin KP, et al. Cognition and anatomy in three variants of primary progressive aphasia. Ann Neurol. 2004;55(3):335–346. | |
Neary D, Snowden JS, Gustafson L, et al. Frontotemporal lobar degeneration: a consensus on clinical diagnostic criteria. Neurology. 1998;51(6):1546–1554. | |
Gorno-Tempini ML, Hillis AE, Weintraub S, et al. Classification of primary progressive aphasia and its variants. Neurology. 2011; 76(11):1006–1014. | |
Chare L, Hodges JR, Leyton CE, et al. New criteria for frontotemporal dementia syndromes: clinical and pathological diagnostic implications. J Neurol Neurosurg Psychiatry. 2014;85(8):865–870. | |
Harris JM, Gall C, Thompson JC, et al. Classification and pathology of primary progressive aphasia. Neurology. 2013;81(21):1832–1839. | |
Leyton CE, Villemagne VL, Savage S, et al. Subtypes of progressive aphasia: application of the international consensus criteria and validation using β-amyloid imaging. Brain. 2011;134(10):3030–3043. | |
Sajjadi SA, Patterson K, Arnold RJ, Watson PC, Nestor PJ. Primary progressive aphasia: a tale of two syndromes and the rest. Neurology. 2012;78(21):1670–1677. | |
Botha H, Duffy JR, Whitwell JL, et al. Classification and clinicoradiologic features of primary progressive aphasia (PPA) and apraxia of speech. Cortex. 2015;69:220–236. | |
Palop JJ, Chin J, Mucke L. A network dysfunction perspective on neurodegenerative diseases. Nature. 2006;443(7113):768–773. | |
Mesulam M. Primary progressive aphasia pathology. Ann Neurol. 2008;63(1):124–125. | |
Mesulam MM. Primary progressive aphasia – a language-based dementia. N Engl J Med. 2003;349(16):1535–1542. | |
Heim S, Pieperhoff P, Grande M, et al. Longitudinal changes in brains of patients with fluent primary progressive aphasia. Brain Lang. 2014;131:11–19. | |
Rogalski E, Cobia D, Harrison TM, Wieneke C, Weintraub S, Mesulam MM. Progression of language decline and cortical atrophy in subtypes of primary progressive aphasia. Neurology. 2011;76(21):1804–1810. | |
Leyton C, Britton A, Hodges J, Halliday G, Kril J. Distinctive pathological mechanism involved in primary progressive aphasias. Neurobiol Aging. 2016;38:82–92. | |
Flanagan EP, Duffy JR, Whitwell JL, Vemuri P, Dickson DW, Josephs KA. Mixed tau and TDP-43 pathology in a patient with unclassifiable primary progressive aphasia. Neurocase. 2016;22(1):55–59. | |
Mesulam MM, Weintraub S, Rogalski EJ, Wieneke C, Geula C, Bigio EH. Asymmetry and heterogeneity of Alzheimer’s and frontotemporal pathology in primary progressive aphasia. Brain. 2014;137(Pt 4):1176–1192. | |
Leyton CE, Hsieh S, Mioshi E, Hodges JR. Cognitive decline in logopenic aphasia: more than losing words. Neurology. 2013;80(10):897–903. | |
Gefen T, Gasho K, Rademaker A, et al. Clinically concordant variations of Alzheimer pathology in aphasic versus amnestic dementia. Brain. 2012;135(5):1554–1565. | |
Leyton CE, Hodges JR, McLean CA, Kril JJ, Piguet O, Ballard KJ. Is the logopenic-variant of primary progressive aphasia a unitary disorder? Cortex. 2015;67(0):122–133. | |
Tu S, Leyton CE, Hodges JR, Piguet O, Hornberger M. Divergent longitudinal propagation of white matter degradation in logopenic and semantic variants of primary progressive aphasia. J Alzheimers Dis. 2015;49(3):853–861. | |
Kumfor F, Landin-Romero R, Devenney E, et al. On the right side? A longitudinal study of left- versus right-lateralized semantic dementia. Brain. 2016;139(Pt 3):986–998. | |
Hodges JR, Mitchell J, Dawson K, et al. Semantic dementia: demography, familial factors and survival in a consecutive series of 100 cases. Brain. 2010;133(Pt 1):300–306. | |
Josephs KA, Whitwell JL, Duffy JR, et al. Progressive aphasia secondary to Alzheimer disease vs FTLD pathology. Neurology. 2008;70(1):25–34. | |
Kertesz A, Blair M, McMonagle P, Munoz DG. The diagnosis and course of frontotemporal dementia. Alzheimer Dis Assoc Disord. 2007;21(2):155–163. | |
Machulda MM, Whitwell JL, Duffy JR, et al. Identification of an atypical variant of logopenic progressive aphasia. Brain Lang. 2013;127(2):139–144. | |
Kertesz A, Davidson W, McCabe P, Takagi K, Munoz D. Primary progressive aphasia: diagnosis, varieties, evolution. J Int Neuropsychol Soc. 2003;9(5):710–719. | |
Josephs KA, Duffy JR, Strand EA, et al. Characterizing a neuro-degenerative syndrome: primary progressive apraxia of speech. Brain. 2012;135(5):1522–1536. | |
Deramecourt V, Lebert F, Debachy B, et al. Prediction of pathology in primary progressive language and speech disorders. Neurology. 2010;74(1):42–49. | |
Chow TW, Miller BL, Hayashi VN, Geschwind DH. Inheritance of frontotemporal dementia. Arch Neurol. 1999;56(7):817–822. | |
Rosso SM, Kaat LD, Baks T, et al. Frontotemporal dementia in The Netherlands: patient characteristics and prevalence estimates from a population-based study. Brain. 2003;126(9):2016–2022. | |
Goldman JS, Farmer JM, Wood EM, et al. Comparison of family histories in FTLD subtypes and related tauopathies. Neurology. 2005;65(11):1817–1819. | |
Flanagan EP, Baker MC, Perkerson RB, et al. Dominant frontotemporal dementia mutations in 140 cases of primary progressive aphasia and speech apraxia. Dement Geriatr Cogn Disord. 2015;39(5–6):281–286. | |
Rohrer JD, Guerreiro R, Vandrovcova J, et al. The heritability and genetics of frontotemporal lobar degeneration. Neurology. 2009;73(18):1451–1456. | |
Rogalski EJ, Rademaker A, Harrison TM, et al. ApoE E4 is a susceptibility factor in amnestic but not aphasic dementias. Alzheimer Dis Assoc Disord. 2011;25(2):159–163. | |
Wolk DA, Dickerson BC. Apolipoprotein E (APOE) genotype has dissociable effects on memory and attentional-executive network function in Alzheimer’s disease. Proc Natl Acad Sci U S A. 2010;107(22):10256–10261. | |
Poorkaj P, Bird TD, Wijsman E, et al. Tau is a candidate gene for chromosome 17 frontotemporal dementia. Ann Neurol. 1998;43(6):815–825. | |
Hutton M, Lendon CL, Rizzu P, et al. Association of missense and 5′-splice-site mutations in tau with the inherited dementia FTDP-17. Nature. 1998;393(6686):702–705. | |
Spillantini MG, Murrell JR, Goedert M, Farlow MR, Klug A, Ghetti B. Mutation in the tau gene in familial multiple system tauopathy with presenile dementia. Proc Natl Acad Sci USA. 1998;95(13):7737–7741. | |
Rosso SM, Kamphorst W, de Graaf B, et al. Familial frontotemporal dementia with ubiquitin-positive inclusions is linked to chromosome 17q21-22. Brain. 2001;124(10):1948–1957. | |
Kertesz A, Kawarai T, Rogaeva E, et al. Familial frontotemporal dementia with ubiquitin-positive, tau-negative inclusions. Neurology. 2000;54(4):818–827. | |
Baker M, Mackenzie IR, Pickering-Brown SM, et al. Mutations in progranulin cause tau-negative frontotemporal dementia linked to chromosome 17. Nature. 2006;442(7105):916–919. | |
Cruts M, Gijselinck I, van der Zee J, et al. Null mutations in progranulin cause ubiquitin-positive frontotemporal dementia linked to chromosome 17q21. Nature. 2006;442(7105):920–924. | |
DeJesus-Hernandez M, Mackenzie IR, Boeve BF, et al. Expanded GGGGCC hexanucleotide repeat in noncoding region of C9ORF72 causes chromosome 9p-linked FTD and ALS. Neuron. 2011;72(2):245–256. | |
Renton AE, Majounie E, Waite A, et al. A hexanucleotide repeat expansion in C9ORF72 is the cause of chromosome 9p21-linked ALS-FTD. Neuron. 2011;72(2):257–268. | |
van Swieten J, Spillantini MG. Hereditary frontotemporal dementia caused by Tau gene mutations. Brain Pathol. 2007;17(1):63–73. | |
Bessi V, Bagnoli S, Nacmias B, Tedde A, Sorbi S, Bracco L. Semantic dementia associated with mutation V363I in the tau gene. J Neurol Sci. 2010;296(1–2):112–114. | |
Seelaar H, Kamphorst W, Rosso SM, et al. Distinct genetic forms of frontotemporal dementia. Neurology. 2008;71(16):1220–1226. | |
Ishizuka T, Nakamura M, Ichiba M, Sano A. Familial semantic dementia with P301L mutation in the Tau gene. Dement Geriatr Cogn Disord. 2011;31(5):334–340. | |
Yu CE, Bird TD, Bekris LM, et al. The spectrum of mutations in progranulin: a collaborative study screening 545 cases of neuro-degeneration. Arch Neurol. 2010;67(2):161–170. | |
Chen-Plotkin AS, Martinez-Lage M, Sleiman PM, et al. Genetic and clinical features of progranulin-associated frontotemporal lobar degeneration. Arch Neurol. 2011;68(4):488–497. | |
Rohrer JD, Crutch SJ, Warrington EK, Warren JD. Progranulin-associated primary progressive aphasia: a distinct phenotype? Neuropsychologia. 2010;48(1):288–297. | |
Mesulam M, Johnson N, Krefft TA, et al. Progranulin mutations in primary progressive aphasia: the PPA1 and PPA3 families. Arch Neurol. 2007;64(1):43–47. | |
Snowden JS, Pickering-Brown SM, Mackenzie IR, et al. Progranulin gene mutations associated with frontotemporal dementia and progressive non-fluent aphasia. Brain. 2006;129(Pt 11):3091–3102. | |
Davion S, Johnson N, Weintraub S, et al. Clinicopathologic correlation in PGRN mutations. Neurology. 2007;69(11):1113–1121. | |
Le Ber I, Camuzat A, Hannequin D, et al. Phenotype variability in progranulin mutation carriers: a clinical, neuropsychological, imaging and genetic study. Brain. 2008;131(Pt 3):732–746. | |
Pickering-Brown SM, Rollinson S, Du Plessis D, et al. Frequency and clinical characteristics of progranulin mutation carriers in the Manchester frontotemporal lobar degeneration cohort: comparison with patients with MAPT and no known mutations. Brain. 2008;131(Pt 3):721–731. | |
Devenney E, Hornberger M, Irish M, et al. Frontotemporal dementia associated with the C9ORF72 mutation: a unique clinical profile. JAMA Neurol. 2014;71(3):331–339. | |
Simon-Sanchez J, Dopper EG, Cohn-Hokke PE, et al. The clinical and pathological phenotype of C9ORF72 hexanucleotide repeat expansions. Brain. 2012;135(Pt 3):723–735. | |
Hsiung GY, DeJesus-Hernandez M, Feldman HH, et al. Clinical and pathological features of familial frontotemporal dementia caused by C9ORF72 mutation on chromosome 9p. Brain. 2012;135(Pt 3):709–722. | |
Mahoney CJ, Beck J, Rohrer JD, et al. Frontotemporal dementia with the C9ORF72 hexanucleotide repeat expansion: clinical, neuroanatomical and neuropathological features. Brain. 2012;135(3):736–750. | |
Boeve BF, Boylan KB, Graff-Radford NR, et al. Characterization of frontotemporal dementia and/or amyotrophic lateral sclerosis associated with the GGGGCC repeat expansion in C9ORF72. Brain. 2012; 135(Pt 3):765–783. | |
Watts GD, Wymer J, Kovach MJ, et al. Inclusion body myopathy associated with Paget disease of bone and frontotemporal dementia is caused by mutant valosin-containing protein. Nat Genet. 2004;36(4):377–381. | |
Kovach MJ, Waggoner B, Leal SM, et al. Clinical delineation and localization to chromosome 9p13.3-p12 of a unique dominant disorder in four families: hereditary inclusion body myopathy, paget disease of bone, and frontotemporal dementia. Mol Genet Metab. 2001;74(4):458–475. | |
Kumfor F, Piguet O. Disturbance of emotion processing in fronto-temporal dementia: a synthesis of cognitive and neuroimaging findings. Neuropsychol Rev. 2012;22(3):280–297. | |
Croot K, Ballard K, Leyton CE, Hodges JR. Apraxia of speech and phonological errors in the diagnosis of nonfluent/agrammatic and logopenic variants of primary progressive aphasia. J Speech Lang Hear Res. 2012;55(5):S1562–S1572. | |
Piguet O, Leyton CE, Gleeson LD, Hoon C, Hodges JR. Memory and emotion processing performance contributes to the diagnosis of non-semantic primary progressive aphasia syndromes. J Alzheimers Dis. 2015;44(2):541–547. | |
Flanagan EC, Tu S, Ahmed S, Hodges JR, Hornberger M. Memory and orientation in the logopenic and nonfluent subtypes of primary progressive aphasia. J Alzheimers Dis. 2014;40(1):33–36. | |
Butts AM, Machulda MM, Duffy JR, Strand EA, Whitwell JL, Josephs KA. Neuropsychological profiles differ among the three variants of primary progressive aphasia. J Int Neuropsychol Soc. 2015;21(6):429–435. | |
Graff-Radford J, Duffy JR, Strand EA, Josephs KA. Parkinsonian motor features distinguish the agrammatic from logopenic variant of primary progressive aphasia. Parkinsonism Relat Disord. 2012; 18(7):890–892. | |
Josephs KA, Duffy JR, Strand EA, et al. The evolution of primary progressive apraxia of speech. Brain. 2014;137(Pt 10):2783–2795. | |
Kertesz A, McMonagle P, Blair M, Davidson W, Munoz DG. The evolution and pathology of frontotemporal dementia. Brain. 2005; 128(Pt 9):1996–2005. | |
Kertesz A. Pick complex: an integrative approach to frontotemporal dementia: primary progressive aphasia, corticobasal degeneration, and progressive supranuclear palsy. Neurologist. 2003;9(6):311–317. | |
Josephs KA, Duffy JR. Apraxia of speech and nonfluent aphasia: a new clinical marker for corticobasal degeneration and progressive supranuclear palsy. Curr Opin Neurol. 2008;21(6):688–692. | |
Mion M, Patterson K, Acosta-Cabronero J, et al. What the left and right anterior fusiform gyri tell us about semantic memory. Brain. 2010;133(11):3256–3268. | |
Irish M, Hodges JR, Piguet O. Right anterior temporal lobe dysfunction underlies theory of mind impairments in semantic dementia. Brain. 2014;137(Pt 4):1241–1253. | |
Gomez-Tortosa E, Rigual R, Prieto-Jurczynska C, et al. Behavioral evolution of progressive semantic aphasia in comparison with nonfluent aphasia. Dement Geriatr Cogn Disord. 2015;41(1–2):1–8. | |
Patterson K, Nestor PJ, Rogers TT. Where do you know what you know? The representation of semantic knowledge in the human brain. Nat Rev Neurosci. 2007;8(12):976–987. | |
Nestor PJ, Graham NL, Fryer TD, Williams GB, Patterson K, Hodges JR. Progressive non-fluent aphasia is associated with hypometabolism centred on the left anterior insula. Brain. 2003;126(Pt 11):2406–2418. | |
Josephs KA, Duffy JR, Strand EA, et al. Syndromes dominated by apraxia of speech show distinct characteristics from agrammatic PPA. Neurology. 2013;81(4):337–345. | |
Ballard KJ, Savage S, Leyton CE, Vogel AP, Hornberger M, Hodges JR. Logopenic and nonfluent variants of primary progressive aphasia are differentiated by acoustic measures of speech production. PLoS One. 2014;9(2):e89864. | |
Gorno-Tempini ML, Murray RC, Rankin KP, Weiner MW, Miller BL. Clinical, cognitive and anatomical evolution from nonfluent progressive aphasia to corticobasal syndrome: a case report. Neurocase. 2004;10(6):426–436. | |
Maas E, Robin DA, Wright DL, Ballard KJ. Motor programming in apraxia of speech. Brain Lang. 2008;106(2):107–118. | |
New AB, Robin DA, Parkinson AL, et al. Altered resting-state network connectivity in stroke patients with and without apraxia of speech. Neuroimage Clin. 2015;8:429–439. | |
Leyton CE, Ballard KJ, Piguet O, Hodges JR. Phonologic errors as a clinical marker of the logopenic variant of PPA. Neurology. 2014;82:1636–1642. | |
Leyton CE, Hodges JR. Towards a clearer definition of logopenic progressive aphasia. Curr Neurol Neurosci Rep. 2013;13(11):396. | |
Savage SA, Ballard KJ, Piguet O, Hodges JR. Bringing words back to mind – improving word production in semantic dementia. Cortex. 2013;49(7):1823–1832. | |
Nickels L, Croot K. Progressive language impairments: intervention and management. Aphasiology. 2009;23(2):123–124. | |
Savage SA, Piguet O, Hodges JR. Cognitive intervention in semantic dementia: maintaining words over time. Alzheimer Dis Assoc Disord. 2015;29(1):55–62. | |
Rogalski E, Weintraub S, Mesulam MM. Are there susceptibility factors for primary progressive aphasia? Brain Lang. 2013;127(2):135–138. | |
Miller ZA, Mandelli ML, Rankin KP, et al. Handedness and language learning disability differentially distribute in progressive aphasia variants. Brain. 2013;136(Pt 11):3461–3473. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.