Back to Journals » International Journal of General Medicine » Volume 13
Prevalence of Anemia Among Jazan University Students
Authors Hamali HA , Mobarki AA, Saboor M , Alfeel A, Madkhali AM, Akhter MS , Dobie G
Received 17 August 2020
Accepted for publication 9 September 2020
Published 5 October 2020 Volume 2020:13 Pages 765—770
DOI https://doi.org/10.2147/IJGM.S275702
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Hassan A Hamali, Abdullah A Mobarki, Muhammad Saboor, Aymen Alfeel, Aymen M Madkhali, Mohammad S Akhter, Gasim Dobie
Department of Medical Laboratory Technology, Faculty of Applied Medical Sciences, Jazan University, Gizan, Saudi Arabia
Correspondence: Hassan A Hamali
Department of Medical Laboratory Technology, Faculty of Applied Medical Sciences, Jazan University, P.O. Box 1906, Gizan 45142, Saudi Arabia
Tel +966581155585
Email [email protected]
Purpose: Anemia is one of the most common disorders affecting the population in both low-income and developing countries. This study aimed to determine the prevalence of anemia and iron deficiency in apparently normal male and female students of Jazan University, Saudi Arabia.
Material and Methods: This cross-sectional study was conducted at the Faculty of Applied Medical Sciences, Jazan University, Gizan, Saudi Arabia. One hundred thirty-four (85 males and 49 females) healthy students with no outward signs of illness were recruited. A specific questionnaire related to sociodemographic and health characteristics was designed and validated. The collected samples were analyzed for complete blood count, serum iron, and serum ferritin.
Results: In the male group, 81 participants (95.3%) were nonanemic with normal hemoglobin (14.99 ± 1.11g/dl), whereas only 4 males were anemic (hemoglobin < 13.0 g/dl). On the other hand, anemia was more prevalent in female students, as 67.35% had hemoglobin values less than 12.0 g/dl. In addition, 26.54% of the anemic females had low serum iron and serum ferritin, indicating iron-deficiency anemia. Although the majority of male participants had normal hemoglobin levels, 37.6% of them had low mean cell volume (MCV), low mean cell hemoglobin (MCH), low mean cell hemoglobin concentration (MCHC), and high red blood cell (RBC) counts, suggesting thalassemia.
Conclusion: Anemia, in particular iron-deficiency anemia, was found to be highly prevalent in females, whereas more than one-third of the male participants might be carriers of alpha or beta thalassemia. Additionally, low dietary iron intake and irregular meal consumption could be two of the possible causes of anemia in the study population. Conducting this study on a large scale of male and female students from different faculties of Jazan University will provide in-depth details about the prevalence and types of anemia among them.
Keywords: anemia, iron deficiency, students, Jazan University
Introduction
Anemia is one of the most common human ailments.1 It is estimated that around one-third of the world’s population suffers from anemia.2 It is also reported that in 50% of cases, anemia is due to iron deficiency. In the Middle East, the prevalence of iron deficiency is similar to that in developing countries, ranging from 25% to 35%, compared with 5–8% in developed countries.3 Several factors contribute to the development of iron deficiency (ID) and iron-deficiency anemia (IDA). Any blood loss amounts to loss of iron from the body, which may lead to ID. Limited absorption of iron from the gut is another factor which predisposes a person to ID. Women during their reproductive period are prone to additional iron loss through menstruation, pregnancy, and lactation.4 Milk, though a poor source of iron, has enough iron to predispose lactating mothers to developing IDA. During the period of rapid somatic growth, children are also at risk of developing IDA if their increased iron demand during this period is not met.5
Anemia is common in Saudi Arabia. Several studies have been conducted in urban areas of the country, especially in children, young females, and women of childbearing age.6–9 However, there is no data regarding the prevalence of anemia and ID in young males and females in the Jazan Area. This study aimed to determine the prevalence of anemia and ID in male and female students of Jazan University, Saudi Arabia.
Materials and Methods
Study Design
This cross-sectional study was conducted at the Faculty of Applied Medical Sciences, Jazan University, Gizan, Saudi Arabia. One hundred thirty-four (85 males and 49 females) healthy students with no outward signs of disease were recruited. A specific questionnaire was developed to inquire about sociodemographic and health characteristics (age, weight, height, marital status, menstrual cycle, the use of oral contraceptives, personal and family history of disease, type and intake of food). Body mass index (BMI) was calculated as previously described.10
Ethical Approval
The current study was approved by the Scientific Research Ethics Committee, Jazan University and was conducted in accordance with the Declaration of Helsinki.
Sample Size and Sample Collection
Sample size was calculated with G*Power 3.1.9.4 calculator power analysis with two sided exact one sample proportion case. The prevalence of anemia among female students reported by Al Hasnad et al11 as 64%. The desired sample size at 5% level of significance, 80% power and the design effect of 0.112 is 134.
After informed written consent was obtained, venous blood was collected from all study participants into (i) a plain tube for serum iron and serum ferritin analysis and (ii) an Ethylenediaminetetraacetic acid (EDTA) anticoagulant tube for a complete blood count (CBC).
Complete Blood Count
A Sysmex XN–1000 Hematology Analyzer (Japan) was used to determine the CBC including red blood cells (RBC, x1012/L), hemoglobin (Hb, g/dL), hematocrit (Hct, %), mean cell volume (MCV, fL), mean cell hemoglobin (MCH, pg), mean cell hemoglobin concentration (MCHC, g/dL), and red blood cell distribution width (RDW-CV and SD). A chemiluminescence Immunoassay system (China) using Maglumi 600 was used for the determination of serum ferritin. Serum iron was tested with a HumaStar 200 (Germany) chemistry analyzer.
Statistical Analysis
Statistical analysis of the data was performed using GraphPad Prism software, version 8.0 for Windows (GraphPad Software Inc., San Diego, CA, USA). Unless otherwise stated, results are presented as mean ± standard deviation (SD). Independent unpaired Student’s t‑tests were used for analysis of hematological parameters, serum iron, and ferritin. The chi‑squared test was used for the correlation of nonparametric data, including demographic data analysis. For each test, differences were considered statistically significant if P < 0.05.
Results
Demographic and health characteristic data on the male and female participants in the current study are presented in Tables 1 and 2. Table 3 presents the mean values of red cell parameters, serum iron, and serum ferritin in the male and female groups. In the male group, the mean Hb of 81 males was 14.99 ± 1.11 g/dl (mean ± SD), representing 95.3% of the male participant population with normal Hb, while 4 males had a mean Hb of 12.69 ± 0.18 g/dl (mean ± SD) and were considered anemic, representing 4.7% (Figure 1A). In the female group, 16 females had normal Hb (>12.0 g/dl) representing 32.65%; on the other hand, 67.35% (n = 33) of the females were anemic (<12.0 g/dl) (Figure 1B).
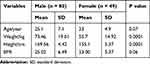 |
Table 1 Characteristic and Demographic Data of the Study Participants |
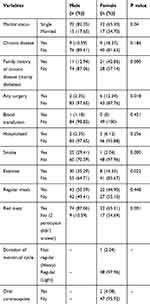 |
Table 2 Health Characteristics and Lifestyle of the Participants |
 |
Table 3 Red Blood Cell Parameters, Serum Iron and Serum Ferritin, of the Study Participants |
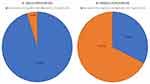 |
Figure 1 Percentage of anemia in the study population. Left (A) Percentage of anemia in the male population. Right (B) Percentage of anemia in the female population. |
In addition, Hb, Hct, MCV, MCH, MCHC, and ferritin were reduced in the anemic female population compared with the normal group, whereas, RDW was significantly higher in anemic females (18.77 ± 3.15 vs. 16.59 ± 1.99; P = 0.0006) (Table 3). The anemic male group also had low values of Hct, MCV, MCH, MCHC, serum iron, and ferritin compared with the normal male group, as shown in Table 3. However, only the red cell count, Hb, and RDW-CV showed statistically significant differences in the male group. In terms of severity, out of 33 anemic females, 78.8% (n = 26) were mildly anemic (Hb <12.0 g/dl), 15.1% (n = 5) were moderately anemic (Hb <10.0 g/dl), and 6.1% (n = 2) had severe anemia (Hb <8.0 g/dl).
Hematological data were further categorized based on the MCV parameter, and the normal male and female populations fell into two groups. In the male group, 31 subjects had low MCV as compared with the rest (n = 50), ie, 84.94 ± 5.36 vs. 74.48 ± 6.32; P < 0.0001 (Table 4). Additionally, RBC counts and RDW were found to be high in this group (n = 31; with low MCV) compared with the normal MCV group (5.50 ± 0.45 vs. 6.21 ± 0.61; P < 0.0001 and 16.00 ± 1.21 vs. 18.35 ± 2.21; P < 0.0001, respectively). MCH, MCHC, and ferritin were significantly lower in males with low MCV as compared with normal males with normal MCV. In females with normal Hb values, similar observations were noted, with MCV and MCH reaching significant differences (Table 4). In anemic females, three further subdivisions were made based upon MCV, i.e. >80 fl (n = 7), 70–80 fl (n = 13), and <70 fl (n = 13), as shown in Table 5. Lower MCV in a significant number of females correlates well with moderate anemia in this group. A review of the laboratory results and study questionnaire showed that 49.41% of males and 55.10% of females did not take regular meals. Moreover, 10.59% of males and 34.69% of females in the study population disclosed no red meat consumption. Chi-square test results correlating red meat and iron intake are shown in Table 6. A significant correlation of dietary iron intake with MCV and serum ferritin was observed, whereas other parameters failed to show a significant correlation with iron intake.
 |
Table 4 Mean cell Volume (MCV) of Males and Females with Normal Hb Levels |
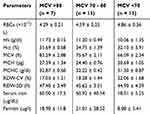 |
Table 5 Categorization of Anemic Females Based on Their MCV (n = 33) |
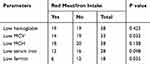 |
Table 6 Correlation of Red Meat/Iron Intake with Red Cell and Iron Profile Parameters |
Discussion
Anemia is a public health burden in Saudi Arabia: the prevalence of anemia in women of childbearing age is around 30.2%, as reported by the WHO11 and up to 37% of women in Riyadh, as reported by AlQuaiz et al.12 Moreover, anemia is a health burden in the Gulf countries, where 30% of women aged 17–24 years13 and 12.9% of males and 17.6% of females aged 11–19 years suffer from anemia.14
As the majority of previous studies conducted in the country were related to female participants, both children and women of childbearing age, this study was conducted to determine the frequency of anemia in both male and female students of Jazan University. The findings of this study showed that 95.3% (n = 81) of male students had normal Hb, while only 4.7% (n = 4) had anemia. Conversely, in the female group, 67.65% of participants had a low Hb concentration. A local study showed a prevalence of anemia ranging from 30.2% to 40%.10
IDA is the most common cause of anemia among all types of anemia affecting people in developed as well as developing countries and considered as the most prevalent micronutrient deficiency in the world.15 In the current study, anemic females showed a wide range of serum iron and ferritin levels 50.31 ± 32.07 and 15.99 ± 20.15, respectively. When the anemic group was categorized further based upon the MCV, it was found that there were three groups as shown in Table 5. Those in group 3 (n = 13) with MCV less than 70 fl, markedly low levels of serum iron and ferritin were observed. These females were considered to have IDA, while in the group with MCV 70–80 fl, mildly low serum iron and ferritin were observed, and these females were considered as iron deficient (n = 13). Hence, it may be concluded that out of 49 females, 26.54% had ID, while 26.54% had IDA. These findings are consistent with other studies conducted in the same group of females in Saudi Arabia, i.e. (35.3%),16 38.3%,17 and 41.6%.18 However, they are discordant with other literature reports of the lowest prevalence of IDA in students of Tabuk University, i.e. 12.5%.19 Another study showed that out of 64% of anemic female university students in Madina, 81% had IDA.20 It is estimated that 40.5% of girls between 16 and 18 years of age suffer from IDA in the Arab region.21 In the current study, ID could be partly attributed to irregular meals and a lack of red meat intake (heme iron) by the female group. In addition, 34.70% of female participants were married; hence, the overall low level of iron could be explained by their increased iron requirements due to pregnancy and lactation. It should be noted that 49.41% of males and 55.10% of females mentioned that they did not take regular meals, while 10.59% of males and 34.69% of females disclosed no red meat consumption. These factors could contribute to the development of anemia and ID in the long run. A review of the CBC report showed that both normal male and female groups had significant variation in their parameters, as shown in Table 4. The division was established on the basis of red cell count and MCV. In both groups, those who had a MCV less than 80 fl with normal Hb had a significantly high red cell count, while low red cell indices were observed. These features are consistent with thalassemia (beta or alpha).22,23 It should also be kept in mind that alpha and beta thalassemia are prevalent in this area.24,25 As Hb electrophoresis was not carried out in this study, the authors could not make a definitive diagnosis of the thalassemia trait.
Conclusion
Form the above results, anemia, in particular IDA, was found to be highly prevalent in females, whereas more than one-third of male participants might be carriers for alpha or beta thalassemia. Conducting this study on a large scale of male and female students from different faculties of Jazan University will provide in-depth details about the prevalence and type of anemia among them. Consequently, well-organized nutritional and educational programs shall be considered by the university to improve the health of the enrolled students.
Funding
This work was supported by the MRC initiative (MRC-004) by the Deanship of Scientific Research, Jazan University.
Disclosure
The authors declare no conflicts of interest in this work.
References
1. de Benoist B, McLean E, Egli I, Cogswell M. Worldwide prevalence of anaemia 1993–2005: WHO global database on anaemia. In: de Benoist B, McLean E, Egli I, Cogswell M, editors. WHO Global Database on Anaemia. 2008.Geneva, Switzerland. World Health Organization;1–40.
2. Kassebaum NJ, Jasrasaria R, Naghavi M, et al. A systematic analysis of global anemia burden from 1990 to 2010. Blood. 2014;123(5):615–624. doi:10.1182/blood-2013-06-508325
3. Stoltzfus RJ. Iron deficiency: global prevalence and consequences. Food Nutr Bull. 2003;24(4Suppl):S99–S103. doi:10.1177/15648265030244S206
4. Camaschella C, Longo DL. Iron-deficiency anemia. N Eng J Med. 2015;372(19):1834–1843. doi:10.1056/NEJMra1401038
5. Camaschella C. Iron metabolism and its disorders; iron deficiency. Blood. 2019;133(1):30–39. doi:10.1182/blood-2018-05-815944
6. Alquaiz AJM, Khoja TAM, Alsharif A, et al. Prevalence and correlates of anaemia in adolescents in Riyadh city, Kingdom of Saudi Arabia. Public Health Nutr. 2015;18(17):3192–3200. doi:10.1017/S1368980015001214
7. El-Hazmi MAF, Warsy AS. Normal reference values for hematological parameters, red cell indices, Hb A2 and Hb F from early childhood through adolescence in Saudis. Ann Saudi Med. 2001;21(3–4):165–169. doi:10.5144/0256-4947.2001.165
8. Hanafi MI, Abdallah AR, Zaky A. Study of hemoglobin level and body mass index among preparatory year female students at Taibah University, Kingdom of Saudi Arabia. J Taibah Univ Med Sci. 2013;8(3):160–166.
9. Abalkhail B, Shawky S. Prevalence of daily breakfast intake, iron deficiency anaemia and awareness of being anaemic among Saudi school students. Int J Food Sci Nutr. 2002;53(6):519–528.
10. Alquaiz AM, Gad Mohamed A, Khoja TAM, et al. Prevalence of anemia and associated factors in child bearing age women in Riyadh, Saudi Arabia. J Nutr Metab. 2013;636585.
11. Al Hassand N. The prevalence of iron deficiency anemia in a Saudi University female students. J Microsc Ultrastruct. 2015;3(1):25–28. doi:10.1016/j.jmau.2014.11.003
12. Report WHO. World Prevalence of Anemia 1993–2005. WHO Global Data Base on Anemia. WHO Global data base anemia; 2013.
13. Al-Quaiz JM. Iron deficiency anemia: a study of risk factors. Saudi Med J. 2001;22(6):490–496.
14. Jackson TR, Al-Mousa Z. Iron deficiency is a more important cause of anemia than hemoglobinopathies in Kuwaiti adolescent girls. J Nutr. 2000;130:1212–1216. doi:10.1093/jn/130.5.1212
15. Al-Sharbatti SS, Al-Ward NJ, Al-Timimi DJ. Anemia among adolescents. Saudi Med J. 2003;24(2):189–194.
16. Soleimani N, Abbaszadeh N. Relationship between anaemia, caused from the iron deficiency, and academic achievement among third grade high school female students. Procedia Soc Behav Sci. 2011;29:1877–1884. doi:10.1016/j.sbspro.2011.11.437
17. Al-Jamea L, Woodman A, Elnagi EA, et al. Prevalence of iron-deficiency anemia and its associated risk factors in female undergraduate students at Prince Sultan Military College of Health Sciences. J Appl Hematol. 2019;10(4):126–133. doi:10.4103/joah.joah_44_19
18. AlSheikh M. Prevalence and risk factors of iron-deficiency anemia in Saudi female medical students. Saudi J Health Sci. 2018;7(3):148–152. doi:10.4103/sjhs.sjhs_79_18
19. Alswailem A, Alahmed S, Alshehri M. The prevalence of iron deficiency anemia and its associated risk factors among a sample of females in Riyadh, Saudi Arabia. Egypt J Hosp Med. 2018;72(6):462.
20. Alzaheb RA, Al-Amer O. The prevalence of iron deficiency anemia and its associated risk factors among a sample of female university students in Tabuk, Saudi Arabia. Clin Med Insights Womens Health. 2017;10:1179562X17745088.
21. Musaiger AO. Iron deficiency anaemia among children and pregnant women in the Arab Gulf countries: the need for action. Nutr Health. 2002;16(3):161–171. doi:10.1177/026010600201600302
22. Jamnok J, Sanchaisuriya K, Chaitriphop C, et al. A new indicator derived from reticulocyte hemoglobin content for screening iron deficiency in an area prevalent for thalassemia. Lab Med. 2020;lmz099.
23. Narchi H, Basak RB. Comparison of erythrocyte indices to differentiate between iron deficiency and alpha-thalassaemias in children with microcytosis and/or hypochromia. East Mediterr Health J. 2010;16(9):966–971. doi:10.26719/2010.16.9.966
24. Hamali HA, Saboor M. Undiagnosed hemoglobinopathies: a potential threat to the premarital screening program. Pak J Med Sci. 2019;35(6):1611–1615. doi:10.12669/pjms.35.6.976
25. Saboor M, Mobarki A, Hamali H, Abdullah S, Mashi A, Hobani Y. Frequency and genotyping of alpha thalassemia in individuals undergoing premarital screening. J Pak Med Assoc. 2020. Available from: https://www.ejmanager.com/mnstemps/33/33-1564064972.pdf?t=1595956536.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
