Back to Journals » Clinical Interventions in Aging » Volume 16
Prevalence and Risk Factors of Osteoporosis in Chinese Postmenopausal Women Awaiting Total Knee Arthroplasty
Authors Tao Y, Tang S, Huang X, Wang H, Zhou A, Zhang J
Received 17 December 2020
Accepted for publication 10 February 2021
Published 26 February 2021 Volume 2021:16 Pages 379—387
DOI https://doi.org/10.2147/CIA.S297947
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Zhi-Ying Wu
Yuzhang Tao,1 Siying Tang,2 Xiao Huang,1 Hongwei Wang,1 Aiguo Zhou,1 Jian Zhang1
1Department of Orthopaedics, The First Affiliated Hospital of Chongqing Medical University, Chongqing, 400016, People’s Republic of China; 2Department of Clinical Nutrition, The First Affiliated Hospital of Chongqing Medical University, Chongqing, 400016, People’s Republic of China
Correspondence: Jian Zhang
Department of Orthopaedics, The First Affiliated Hospital of Chongqing Medical University, Chongqing, 400016, People’s Republic of China
Email [email protected]
Background: Total knee arthroplasty (TKA) complications associated with low bone quality are challenging for orthopaedic surgeons to treat, but little is known about bone quality in Chinese postmenopausal women awaiting TKA. This study investigated the incidence of osteoporosis (OP) and explored the preoperative risk factors for OP in this population.
Methods: We retrospectively reviewed the data of Chinese postmenopausal women who were indicated for TKA between May 2017 and June 2020. The bone mineral density (BMD) of the hip and lumbar spine and multiple preoperative parameters were collected and analyzed. Binary logistic regression analysis was performed to identify independent risk factors for OP in this population.
Results: A total of 204 postmenopausal women with advanced knee OA were included in the study (age: 69.7± 8.5 years; body mass index [BMI]: 25.5± 4.0 kg/m2). The OP prevalence among all participants was 59.8%, and the patients aged 60– 80 years had a significantly lower BMD than did the age/ethnicity-adjusted population. An age ≥ 60 years, a BMI< 25, and the presence of a varus knee deformity were independent risk factors for preoperative OP in the postmenopausal women awaiting TKA.
Conclusion: The prevalence of OP in Chinese postmenopausal women awaiting TKA is higher than that in the age/ethnicity-adjusted normal population. An age ≥ 60 years, a BMI< 25, and the presence of a varus knee deformity are independent risk factors that can be used to predict preoperative OP in this population.
Keywords: osteoporosis, postmenopausal women, total knee arthroplasty, Chinese, bone mineral density
Introduction
Total knee arthroplasty (TKA) has advanced significantly since it was developed. It ameliorates pain and improves the function of the knee in millions of patients suffering from knee osteoarthritis (OA) and greatly improves their quality of life.1 However, with a steadily increasing surgery volume, multiple TKA-related complications are occurring, creating an enormous challenge for orthopaedic surgeons.2 Decreased bone quality has been shown to increase the incidence of various TKA complications, such as periprosthetic fracture, osteolysis, and implant loosening/malposition.3,4 Osteoporosis (OP) is regarded as the most common cause of low bone quality. Elderly/postmenopausal women comprise approximately 70–90% of TKA candidates;5,6 moreover, this population is at high risk of OP development.7–9 Anti-OP treatment before TKA has been shown to reduce the chance of TKA complications.10 Therefore, for better outcomes in postmenopausal women awaiting TKA, it is necessary to evaluate and manage OP preoperatively.
Osteoporosis and osteoarthritis are two related diseases with different pathogeneses.11 The exact interactive mechanism between them is complex and has not been well elucidated. Some studies have shown a positive correlation between the severity of OA and the level of bone mineral density (BMD) and that OA is a protective factor against OP,12–14 while several researchers have instead suggested that OP exists in a considerable number of patients with advanced OA.15,16 Dual-energy X-ray absorptiometry (DXA) scans of at least two bone sites are recommended by the International Society for Clinical Densitometry (ISCD) to diagnose osteoporosis based on the T-score. However, some studies have shown that the BMD region of interest (ROI) may be affected by orthopaedic diseases, thus resulting in the BMD not being correlated with OP and inconsistent diagnoses between different sites.17–19 For women with advanced knee OA awaiting TKA, there is a lack of relevant evidence to determine which site can be used to appropriately evaluate OP in this population. Due to population aging, the number of Chinese postmenopausal women indicated for TKA is increasing, but little is known about the prevalence and independent risk factors for OP in this population.
More information on the preoperative bone status characteristics of Chinese postmenopausal women awaiting TKA may help surgeons select interventions more prudently and efficiently. The purposes of this study were to (1) investigate the prevalence of OP in Chinese postmenopausal women awaiting TKA, (2) determine the influence of the DXA examination site on OP detection and diagnostic discordance, and (3) identify preoperative risk factors for OP in this population to build an OP screening strategy.
Patients and Methods
Study Population
This retrospective, descriptive study was approved by the ethics committee of our hospital. All patient data were from one tertiary medical institute and treated with confidentiality. From May 2017 to June 2020, all patients indicated for TKA were routinely screened for OP using DXA 1 day before surgery. The data for these consecutive TKA candidates were searched in the electronic medical record system. The inclusion criteria were (1) postmenopausal women, (2) patients diagnosed with unilateral or bilateral advanced primary knee osteoarthritis who were scheduled for TKA, (3) patients who underwent standing anteroposterior/lateral X-ray scans of the affected knee and full-length lower limb radiography scans, (4) patients with a complete preoperative examination data of routine blood and serum biochemistry tests, and (5) patients who underwent left hip and lumbar spine DXA examinations preoperatively. The exclusion criteria were as follows: (1) patients diagnosed with secondary knee OA or OA-like diseases, such as septic arthritis, rheumatoid arthritis, gout, etc; (2) patients with a previous history of TKA; (3) patients who underwent lumbar spine or hip internal fixation/implantation or had severe spine OA, which may affect BMD measurements; (4) patients who previously had fractures affecting the lumbar spine or lower extremities; and (5) patients who were undergoing standardized anti-OP therapy.
DXA and BMD Analysis
All DXA examinations were conducted and analyzed by experienced and qualified operators. The areal BMDs (g/cm2) of the lumbar spine (L1-L4, LS), proximal femur (PF), and femoral neck (FN) were obtained by a Discovery A scanner (Hologic Inc., Marlborough, MA, USA). The World Health Organization (WHO) classifications for osteopenia and OP were used for each bone site: normal (T-score greater than −1.0), osteopenia (T-score between −1.0 and 2.5), and osteoporosis (T-score below −2.5).20 The white female peak BMD in the Discovery A built-in reference database was used for the T-score calculation. In accordance with the ISCD protocol,21 the lowest T-score among multiple sites was considered the decisive T-score for a patient-level OP diagnosis. Discordance of the OP diagnosis between two sites was determined in a patient when the T-score of one site was indicative of OP and the T-score of another site was not. Hologic BMD data from the study by Zhang et al were used to compare the data from the population in this study with those of an ethnicity/age/sex-adjusted normal population.22
Preoperative Data Collection
Age, body mass index (BMI), comorbidities, medication use, and previous medical history were included in the demographic information. The laboratory test results obtained upon hospitalization for every participant were collected, which included the hemoglobin level (g/L), lymphocyte count (109/L), prealbumin level (mg/L), total protein level (g/L), albumin level (g/L), serum calcium level (mmol/L), serum creatinine level (mmol/L), and estimated glomerular filtration rate (eGFR, mL/min/1.73 m2). The OA grade of the affected knee was determined with the Kellgren-Lawrence (K-L) system. Bilateral OA was recorded when both knees of one patient were graded greater than K-L I according to the full-length lower limb radiograph. The knee with more severe symptoms and worse K-L grade was deemed the study knee for the patients with bilateral OA. The hip-knee-ankle (HKA) angle on the full-length lower limb radiograph (the angle formed by the mechanical femoral axis and mechanical tibial axis) was used to assess the coronal knee deformity: varus (HKA<177°), normal (177°≤HKA≤183°) and valgus (HKA>183°).23 Knee contracture was determined when the study knee could not be fully extended actively or passively. Patellofemoral OA was defined when the study knee had a K-L grade greater than I on the lateral radiograph of the knee. Knee attrition, a severe deformity, was defined as bone loss in the medial or lateral knee compartment.24
Statistical Analysis
All data were analyzed with SPSS software (version 26.0; IBM, Chicago, IL). The Shapiro–Wilk test was used to assess the normality of the continuous variables. The variables were compared between groups using the independent t-test when the data were normally distributed. For the data with skewed distributions, the Mann–Whitney U-test was used for comparisons. The differences between categorical variables were assessed with the Pearson chi-square test. Binary logistic regression was conducted to identify the independent risk factors (odds ratio [OR] with 95% confidence interval [CI]) associated with OP (dependent variable) in postmenopausal women awaiting TKA, and the forward stepwise method was used to enter variables with a P-value<0.1, while variables with a P-value<0.05 remained in the model (independent variables: age, BMI, symptom duration, incidence of the bilateral knee OA, presence of a varus knee deformity, presence of a valgus knee deformity). P-values of less than 0.05 were considered statistically significant.
Results
After selection, a total of 204 postmenopausal women were included in this study. These women were mainly (79.42%) aged between 60–80 years, and 88.2% of them suffered from bilateral knee OA. The median symptom duration was eight years, and the mean ± standard deviation of age and BMI were 69.7±8.5 years and 25.5±4.0 kg/m2. All the participants’ study knees had at least K-L III grade OA, and 63.7% of all OA cases were considered severe (K-L IV). Only 4.9% of patients were classified as normal, whereas 59.8% of all women were categorized as having osteoporosis (Table 1). To further determine the age-related characteristics of OP distribution, age stratification was performed (Figure 1). There was a significantly lower incidence of OP (18.2%) and a higher incidence of normal case (13.6%) in the postmenopausal women aged <60 years than in the patients aged ≥60 years. In contrast, 63.1%, 67.9% and 60.0% of patients aged 60–70, 70–80 and ≥80 years were diagnosed with OP, respectively.
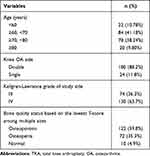 |
Table 1 Demographics and Characteristics of Women Awaiting TKA |
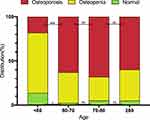 |
Figure 1 Distribution of bone quality status of different age groups. *P<0.05, ***P<0.001. Abbreviation: ns, no significance. |
OP prevalence based on the DXA examination site is shown in Figure 2. There was an increase in OP incidence of PF and FN with patient aging, whereas the OP incidence of LS decreased after age 80. Compared with the OP prevalence at multiple sites, which is used as the gold standard for patient-level OP diagnosis proposed by ISCD, the OP incidence of LS showed no significant differences among all age groups, while the OP incidence rates in the PF and FN were significantly lower between the ages 60 and 80 years.
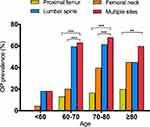 |
Figure 2 Osteoporosis prevalence based on different DXA examination sites. **P<0.01, ***P<0.001. Abbreviation: OP, osteoporosis. |
The discordance in OP diagnoses between different DXA exam sites is demonstrated in Table 2. When the T-score of the LS was indicative of OP, 56.76 and 76.58% of the T-scores for the FN and PF were not suggestive of the same diagnosis. Although there was less discordance between sites when the T-scores of the FN and PF were positive for OP, the absolute number of T-scores of these two sites positive for OP was much smaller than that of LS (58 and 28 vs 111).
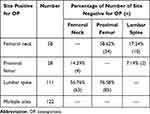 |
Table 2 The Exact Number of Different Sites Tested Positive for OP and Their Diagnostic Discordance |
The FN (Figure 3A) and LS (Figure 3B) BMDs for postmenopausal women of all age groups awaiting TKA were compared to those of an age/ethnicity/site-adjusted reference population of normal Chinese individuals. Both the FN and LS BMDs from the patients aged 60–80 years in this study were remarkably lower than those of the reference population. The descending trend with aging in the FN BMD was consistent between the two populations (Figure 3A), but the decreasing tendency in the LS BMD reached a plateau at the age of 60–70 years for both groups (Figure 3B).
According to the T-scores at multiple sites, the patients were classified into groups with OP or without OP, and then, the preoperative parameters were compared between the two groups (Table 3). The age (P=0.023) and the percentage of patients with varus knee deformities (P=0.025) were higher, and the BMI was lower (P=0.035) in the OP group, while the blood parameters and symptom duration showed no significant differences between groups. Binary logistic regression analysis (Table 4) revealed that an age ≥60 (OR=7.76, P<0.001), a BMI<25 (OR=1.85, P=0.048), and the presence of a knee varus deformity (OR=2.10, P=0.020) were independent risk factors associated with OP in postmenopausal women awaiting TKA.
 |
Table 3 Comparison Between Non-OP and OP Women Awaiting TKA |
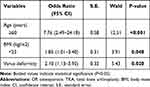 |
Table 4 Binary Logistic Regression Analysis for the Determination of Independent OP Risk Factors in Postmenopausal Women Awaiting TKA |
Discussion
As the demand for total knee arthroplasty has increased to an unprecedented extent in China, perioperative complications associated with low bone quality are receiving more attention. The majority of TKA candidates are postmenopausal women, who are prone to poorer bone health and short of proper preoperative anti-osteoporosis management.25,26 As the bone quality status of postmenopausal women awaiting TKA in China has been insufficiently studied, this study was mainly performed to investigate the prevalence and risk factors for preoperative OP in this population. We found that a significant proportion (59.8%) of women had evidence of OP, and 35.3% of patients had osteopenia. OP detection for several DXA sites and the discordance between them showed that the LS was a reliable BMD site for OP diagnosis in this population. Age, BMI, and the presence of varus knee deformity were found to be independent risk factors for predicting OP before TKA.
Several studies have reported the incidence of OP before TKA. In the non-Asian population, 9.6–33% of TKA candidates have been found to suffer from OP, regardless of the patient’s sex,16,27–30 and 35% of women awaiting TKA or total hip arthroplasty have been found to have OP.15 In contrast, two Korean studies have reported OP incidence rates of 40.1 and 53.4% among women indicated for TKA.26,31 The prevalence of OP in the Chinese women awaiting TKA in our study was higher (59.8%) than that in women of other ethnicities, especially when the patients were aged ≥60 years (60–68%). We speculate the bone health of Chinese women awaiting TKA is lower because of the ethnic BMD variance caused by genetics, physical activity levels, diet, and lifestyle factors, as Zhang et al showed that Chinese individuals have lower systematic BMD values than do non-Hispanic White, Japanese and Korean individuals.22
In addition to the ethnic differences, lower FN and LS BMDs were found in the women aged 60–80 years awaiting TKA than in the ethnicity/age-adjusted population (Figure 3A and B). The OP incidence of normal Chinese women aged ≥50 years ranges from 24.6% to 31.2%,22,32,33 which is also much lower than that reported in our study. The difference may indicate a positive correlation between knee OA and OP. Im et al found that a higher degree of knee OA was associated with a lower BMD.34 A low level of physical activity related to pain caused by advanced knee OA may lead to disuse osteoporosis. Although some investigators have shown an inverse relationship between knee OA and OP,35,36 the study subjects were mostly Caucasian, who have significantly higher BMI values and different lifestyles than do their Chinese counterparts, and mild or moderate knee OA (KL-I/II) cases were often included in their studies, which may affect the results. The interesting phenomenon that the LS BMD of the included patients and the reference population increased after age 80 (Figure 3B) was likely caused by the natural degenerative OA change in the lumbar spine with aging.
Discordance in OP diagnoses between different DXA skeletal sites is common, and five etiologic types (physiologic, pathophysiologic, anatomic, artifactual, and technical) have been proposed.19 Over 50% of OP diagnostic discordance has been found between the LS and FN in the normal Chinese population,32 which is consistent with the findings of our study (Table 2). A large-scale study by Moayyeri et al showed that lower BMD for LS was more prevalent than hip in community-based individuals,37 and they proposed that the higher velocity of bone loss at trabecular bones (typical of LS) than cortical bones (typical of FN/PF) in the postmenopausal state could be the main reason for OP diagnostic discordance. In our study, the OP prevalence based on LS in all age groups was not significantly different from that based on multiple sites, while the OP prevalence based on FN was much smaller (Figure 2), suggesting the LS alone might be used as a reliable DXA exam site for OP diagnosis in Chinese postmenopausal women awaiting TKA.
Several risk factors, including age, sex, and BMI, are associated with OP in the normal Chinese population,38 but OP predictors specific for Chinese postmenopausal women awaiting TKA have rarely been investigated. Our study showed that the presence of a varus knee deformity was an independent risk factor for OP in this population (Tables 3 and 4), while other preoperative parameters were of little predictive value. From an anatomical perspective, an increased degree of knee varus is correlated with a larger femoral neck-shaft angle, which has been shown to be related to lower hip stresses.39,40 The lower hip BMD possibly caused by the decreased hip stresses may partly explain our finding of the varus knee deformity as an independent OP risk factor. Moreover, Chang et al demonstrated that the degree of varus knee malalignment is significantly associated with the severity of pain and functional decline in advanced knee OA,41 suggesting the positive relationship between varus knee and OP, to some extent, might be correlated with the decreased physical activity caused by knee function loss in TKA candidates.
The blood nutritional markers measured showed no significant differences between groups in this study, although nutritional supplementation has been shown to correlate with a higher BMD.42 This result may suggest that nutritional status plays a limited role in developing OP in this population, while the estrogen depletion caused by menopause and aging could be the major determinant of OP development.43 Future studies are needed to determine the exact role of various blood parameters, including bone turnover markers and vitamin D, in the pathophysiology of OP in patients awaiting TKA.
Patients indicated for TKA are usually given inadequate attention for OP screening.29,44 Moreover, subjects undergoing TKA may experience significant bone loss in the first 1 to 3 years postoperatively.45,46 Given the high prevalence of preoperative OP in the subjects of our study, neglected postmenopausal women awaiting TKA may be more likely to suffer from OP-related complications. However, preoperative anti-OP treatment has been shown to lower the risk of revision and preserve periprosthetic BMD after TKA.10,47,48 Therefore, we propose that postmenopausal women aged ≥60 years awaiting TKA who have a BMI<25 and varus knee deformity are recommended for OP screening preoperatively.
Although the COVID-19 pandemic may have influenced TKA services,49,50 all elective TKA surgeries were canceled from February to March 2020 (the most severe period of the epidemic in China) in our hospital, and DXA protocol remained the same for all TKA candidates from April to June 2020. Therefore, we believe the pandemic has had a limited impact on the results of this study.
There are some limitations of our study. First, this is a retrospective study. Although the subjects were continuously included, the number of patients in each age group could not be matched, which may introduce selection bias. Second, some functional parameters of the knee, such as the WOMAC (The Western Ontario and McMaster Universities Osteoarthritis Index) score, were not accessible for some participants. Therefore, information about symptom-related differences between groups is not available. Third, data on bone turnover markers, vitamin D and calcium intake were not all available for the included subjects, making the analysis of these parameters between groups unfeasible. Finally, the generalizability of the results is limited because of the moderate sample size of this single-center study.
Conclusion
In summary, for Chinese postmenopausal women awaiting TKA, the prevalence of OP is higher than that in age/ethnicity-adjusted normal populations. The lumbar spine may serve as a reliable DXA exam site for OP diagnosis, while an age ≥60 years, a BMI<25, and the presence of varus knee deformity are independent risk factors that can be used to predict preoperative OP in this population.
Data Sharing Statement
The data are available upon reasonable request.
Ethical Approval
This study was approved by the ethics committee of the First Affiliated Hospital of Chongqing Medical University (No. 2020-642). Written informed consent was not needed due to the retrospective nature of this study. All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1975 Helsinki declaration and its later amendments or comparable ethical standards.
Funding
This study was supported by the Medical Research Project from the Health and Family Planning Commission in Chongqing [grant numbers 2017ZDXM006]; the General Project of Technology Innovation and Application Development from the Chongqing Science and Technology Bureau [grant numbers cstc2019jscx-msxmX0245].
Disclosure
The authors report no conflicts of interest in this work.
References
1. Cram P, Lu X, Kates SL, Singh JA, Li Y, Wolf BR. Total knee arthroplasty volume,utilization, and outcomes among medicare beneficiaries, 1991–2010. JAMA. 2012;308:1227–1236. doi:10.1001/2012.jama.11153
2. Healy WL, Della Valle CJ, Iorio R, et al. Complications of total knee arthroplasty: standardized list and definitions of the knee society knee. Clin Orthop Relat Res. 2013;471(1):215–220. doi:10.1007/s11999-012-2489-y
3. Russell LA. Osteoporosis and orthopedic surgery: effect of bone health on total joint arthroplasty outcome. Curr Rheumatol Rep. 2013;15(11):371. doi:10.1007/s11926-013-0371-x
4. Lee DH, Padhy D, Lee SH, Nha KW, Park JH, Han SB. Osteoporosis affects component positioning in computer navigation-assisted total knee arthroplasty. Knee. 2012;19(3):203–207. doi:10.1016/j.knee.2011.02.010
5. Waddell J, Johnson K, Hein W, Raabe J, FitzGerald G, Turibio F. Orthopaedic practice in total hip arthroplasty and total knee arthroplasty: results from the Global Orthopaedic Registry (GLORY). Am J Orthop (Belle Mead NJ). 2010;39(9 Suppl):5–13.
6. Yang B, Yu JK, Gong X, et al. Sex, age, and annual incidence of primary total knee arthroplasty: a university affiliated hospital survey of 3118 chinese patients. Chin Med J (Engl). 2012;125(22):3952–3955. doi:10.3760/cma.j.issn.0366-6999.2012.22.007
7. Black DM, Rosen CJ. Clinical practice. postmenopausal osteoporosis. N Engl J Med. 2016;374(3):254–262. doi:10.1056/NEJMcp1513724
8. Yan G, Huang Y, Cao H, Wu J, Jiang N, Cao X. Association of breastfeeding and postmenopausal osteoporosis in Chinese women: a community-based retrospective study. BMC Womens Health. 2019;19(1):1–7. doi:10.1186/s12905-019-0808-0
9. Yu F, Xia W. The epidemiology of osteoporosis, associated fragility fractures, and management gap in China. Arch Osteoporos. 2019;14:1. doi:10.1007/s11657-018-0549-y
10. Shi M, Chen L, Xin Z, Wang Y, Wang W, Yan S. Bisphosphonates for the preservation of periprosthetic bone mineral density after total joint arthroplasty: a meta-analysis of 25 randomized controlled trials. Osteoporos Int. 2018;29(7):1525–1537. doi:10.1007/s00198-018-4488-7
11. Geusens PP, Van Den Bergh JP. Osteoporosis and osteoarthritis: shared mechanisms and epidemiology. Curr Opin Rheumatol. 2016;28(2):97–103. doi:10.1097/BOR.0000000000000256
12. Hart DJ, Mootoosamy I, Doyle DV, Spector TD. The relationship between osteoarthritis and osteoporosis in the general population: the Chingford study. Ann Rheum Dis. 1994;53(3):158–162. doi:10.1136/ard.53.3.158
13. Kim YH, Lee JS, Park JH. Association between bone mineral density and knee osteoarthritis in Koreans: the Fourth and Fifth Korea National Health and Nutrition Examination Surveys. Osteoarthr Cartil. 2018;26(11):1511–1517. doi:10.1016/j.joca.2018.07.008
14. Dequeker J, Aerssens J, Luyten FP. Osteoarthritis and osteoporosis: clinical and research evidence of inverse relationship. Aging Clin Exp Res. 2003;15(5):426–439. doi:10.1007/BF03327364
15. Lingard EA, Mitchell SY, Francis RM, et al. The prevalence of osteoporosis in patients with severe hip and knee osteoarthritis awaiting joint arthroplasty. Age Ageing. 2010;39(2):234–239. doi:10.1093/ageing/afp222
16. Sadigursky D, Barretto Junior LA, Vieira Lobão DM, Fernandes Carneiro RJ, Colavolpe PO. Osteoporosis in Brazilian patients awaiting knee arthroplasty. Acta Ortop Bras. 2017;25(3):74–77. doi:10.1590/1413-785220172503167325
17. Blake GM, Fogelman I. The role of DXA bone density scans in the diagnosis and treatment of osteoporosis. Postgrad Med J. 2007;83(982):509–517. doi:10.1136/pgmj.2007.057505
18. Gupta A, Upadhyaya S, Patel A, et al. DEXA sensitivity analysis in patients with adult spinal deformity. Spine J. 2020;20(2):174–180. doi:10.1016/j.spinee.2019.08.011
19. Woodson G. Dual X-ray absorptiometry T-score concordance and discordance between hip and spine measurement sites. J Clin Densitom. 2000;3(4):319–324. doi:10.1385/JCD:3:4:319
20. Kanis JA, Melton III LJ, Christiansen C, Johnston CC, Khaltaev N. The diagnosis of osteoporosis. J Bone Miner Res. 1994;9(8):1137–1141. doi:10.1002/jbmr.5650090802
21. Lewiecki EM, Kendler DL, Kiebzak GM, et al. Special report on the official positions of the International Society for Clinical Densitometry. Osteoporos Int. 2004;15(10):779–784. doi:10.1007/s00198-004-1677-3
22. Zhang ZQ, Ho SC, Chen ZQ, Zhang CX, Chen YM. Reference values of bone mineral density and prevalence of osteoporosis in Chinese adults. Osteoporos Int. 2014;25(2):497–507. doi:10.1007/s00198-013-2418-2
23. Bellemans J, Colyn W, Vandenneucker H, Victor J. The Chitranjan Ranawat Award: is neutral mechanical alignment normal for all patients?: The concept of constitutional varus. Clin Orthop Relat Res. 2012;470(1):45–53. doi:10.1007/s11999-011-1936-5
24. Dieppe PA, Reichenbach S, Williams S, Gregg P, Watt I, Jüni P. Assessing bone loss on radiographs of the knee in osteoarthritis: a cross‐sectional study. Arthritis Rheum. 2005;52(11):3536–3541. doi:10.1002/art.21418
25. Chen P, Li Z, Hu Y. Prevalence of osteoporosis in China: a meta-analysis and systematic review. BMC Public Health. 2016;16(1):1–11. doi:10.1186/s12889-016-3712-7
26. Ha CW, Park YB. Underestimation and undertreatment of osteoporosis in patients awaiting primary total knee arthroplasty. Arch Orthop Trauma Surg. 2020;140(8):1109–1114. doi:10.1007/s00402-020-03462-y
27. Linde KN, Puhakka KB, Langdahl BL, et al. Bone mineral density is lower in patients with severe knee osteoarthritis and attrition. Calcif Tissue Int. 2017;101(6):593–601. doi:10.1007/s00223-017-0315-y
28. Bernatz JT, Krueger DC, Squire MW, Illgen RL, Binkley NC, Anderson PA. Unrecognized osteoporosis is common in patients with a well-functioning total knee arthroplasty. J Arthroplasty. 2019;34(10):2347–2350. doi:10.1016/j.arth.2019.05.041
29. Bernatz JT, Brooks AE, Squire MW, Illgen RI, Binkley NC, Anderson PA. Osteoporosis is common and undertreated prior to total joint arthroplasty. J Arthroplasty. 2019;34(7):1347–1353. doi:10.1016/j.arth.2019.03.044
30. Labuda A, Papaioannou A, Pritchard J, Kennedy C, DeBeer J, Adachi JD. Prevalence of osteoporosis in osteoarthritic patients undergoing total hip or total knee arthroplasty. Arch Phys Med Rehabil. 2008;89(12):2373–2374. doi:10.1016/j.apmr.2008.06.007
31. Chang CB, Kim TK, Kang YG, Seong SC, Kang SB. Prevalence of osteoporosis in female patients with advanced knee osteoarthritis undergoing total knee arthroplasty. J Korean Med Sci. 2014;29(10):1425–1431. doi:10.3346/jkms.2014.29.10.1425
32. Lu YC, Lin YC, Lin YK, et al. Prevalence of osteoporosis and low bone mass in older chinese population based on bone mineral density at multiple skeletal sites. Sci Rep. 2016;6(April):1–9. doi:10.1038/srep25206
33. Zhu H, Fang J, Luo X, et al. A survey of bone mineral density of healthy Han adults in China. Osteoporos Int. 2010;21(5):765–772. doi:10.1007/s00198-009-1010-2
34. Im G-I, Kwon O-J, Kim CH. The relationship between osteoarthritis of the knee and bone mineral density of proximal femur: a cross-sectional study from a Korean population in women. Clin Orthop Surg. 2014;6(4):420–425. doi:10.4055/cios.2014.6.4.420
35. Hannan MT, Anderson JJ, Zhang Y, Levy D, Felson DT. Bone mineral density and knee osteoarthritis in elderly men and women. The Framingham Study. Arthritis Rheum. 1993;36(12):1671–1680. doi:10.1002/art.1780361205
36. Lethbridge-Cejku M, Tobin JD, Scott WW, et al. Axial and hip bone mineral density and radiographic changes of osteoarthritis of the knee: data from the Baltimore Longitudinal Study of Aging. J Rheumatol. 1996;23(11):1943–1947.
37. Moayyeri A, Soltani A, Tabari NK, Sadatsafavi M, Hossein-neghad A, Larijani B. Discordance in diagnosis of osteoporosis using spine and hip bone densitometry. BMC Endocr Disord. 2005;5:1–6. doi:10.1186/1472-6823-5-3
38. Cui R, Zhou L, Li Z, Li Q, Qi Z, Zhang J. Assessment risk of osteoporosis in Chinese people: relationship among body mass index, serum lipid profiles, blood glucose, and bone mineral density. Clin Interv Aging. 2016;11:887–895. doi:10.2147/CIA.S103845
39. Coskun Benlidayi I, Guzel R, Basaran S, Aksungur EH, Seydaoglu G. Is coxa valga a predictor for the severity of knee osteoarthritis? A cross-sectional study. Surg Radiol Anat. 2015;37(4):369–376. doi:10.1007/s00276-014-1359-6
40. Ng KCG, Mantovani G, Lamontagne M, Labrosse MR, Beaulé PE. Increased hip stresses resulting from a cam deformity and decreased femoral neck-shaft angle during level walking. Clin Orthop Relat Res. 2017;475(4):998–1008. doi:10.1007/s11999-016-5038-2
41. Chang CB, Koh IJ, Seo ES, Kang YG, Seong SC, Kim TK. The radiographic predictors of symptom severity in advanced knee osteoarthritis with varus deformity. Knee. 2011;18(6):456–460. doi:10.1016/j.knee.2010.08.010
42. Shams-White MM, Chung M, Du M, et al. Dietary protein and bone health: a systematic review and meta-analysis from the National Osteoporosis Foundation. Am J Clin Nutr. 2017;105(6):1528–1543. doi:10.3945/ajcn.116.145110
43. Tarantino U, Iolascon G, Cianferotti L, et al. Clinical guidelines for the prevention and treatment of osteoporosis: summary statements and recommendations from the Italian Society for Orthopaedics and Traumatology. J Orthop Traumatol. 2017;18(1):3–36. doi:10.1007/s10195-017-0474-7
44. Gillespie CW, Morin PE. Trends and disparities in osteoporosis screening among women in the United States, 2008–2014. Am J Med. 2017;130(3):306–316. doi:10.1016/j.amjmed.2016.10.018
45. Beaupre LA, Rezansoff A, Clark M, Jen H, Lambert RG, Majumdar S. Bone mineral density changes in the hip and spine of men and women 1-year after primary cemented total knee arthroplasty: prospective cohort study. J Arthroplasty. 2015;30(12):2185–2189. doi:10.1016/j.arth.2015.06.026
46. Gundry M, Hopkins S, Knapp KA. Review on bone mineral density loss in total knee replacements leading to increased fracture risk. Clin Rev Bone Miner Metab. 2017;15(4):162–174. doi:10.1007/s12018-017-9238-4
47. Namba RS, Inacio MCS, Cheetham TC, Dell RM, Paxton EW, Khatod MX. Lower total knee arthroplasty revision risk associated with bisphosphonate use, even in patients with normal bone density. J Arthroplasty. 2016;31(2):537–541. doi:10.1016/j.arth.2015.09.005
48. Shi M, Chen L, Wu H, et al. Effect of bisphosphonates on periprosthetic bone loss after total knee arthroplasty: a meta-analysis of randomized controlled trials. BMC Musculoskelet Disord. 2018;19(1):1–8. doi:10.1186/s12891-018-2101-z
49. Mitura K. The impact of COVID-19 pandemic on critical care and surgical services availability. Crit Care Innov. 2020;3(2):43–50.
50. Zheng MH, Boni L, Fingerhut A. Minimally invasive surgery and the novel coronavirus outbreak: lessons learned in China and Italy. Ann Surg. 2020;272(1):20–21. doi:10.1097/SLA.0000000000003924
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

