Back to Journals » Clinical Interventions in Aging » Volume 16
Postoperative Delirium is Not Associated with Long-Term Decline in Activities of Daily Living or Mortality After Laryngectomy
Authors Wang Y, Liu W, Chen K, Shen X
Received 27 January 2021
Accepted for publication 23 April 2021
Published 17 May 2021 Volume 2021:16 Pages 823—831
DOI https://doi.org/10.2147/CIA.S303800
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 5
Editor who approved publication: Dr Zhi-Ying Wu
Yiru Wang,* Weiwei Liu,* Kaizheng Chen, Xia Shen
Department of Anesthesiology, Eye & ENT Hospital, Fudan University, Shanghai, 200031, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Xia Shen
Department of Anesthesiology, Eye & ENT Hospital, Fudan University, 83 Fenyang Road, Shanghai, 200031, People’s Republic of China
Tel +8621-643771334
Fax +8621-64373416
Email [email protected]
Purpose: To determine the relationships between postoperative delirium (POD) and postoperative activities of daily living (ADL) and mortality in patients undergoing laryngectomy. We hypothesized that POD would reduce postoperative ADL and increase postoperative mortality.
Patients and Methods: The prospective study included older participants (age ≥ 65 y) undergoing total laryngectomy, partial laryngectomy, total laryngectomy plus neck dissection, or partial laryngectomy plus neck dissection under general anesthesia. The diagnosis of delirium was based on the Confusion Assessment Method algorithm, which was administered on postoperative days 1 through 6. ADL were evaluated using the Chinese version of the Index of ADL scale. Follow-up assessments of ADL and mortality were conducted 24 months after surgery.
Results: Of 127 participants (aged 70.3 ± 4.1 y), 19 (15.0%) developed POD. POD was not associated with a decrease in ADL after laryngectomy (p=0.599) nor with an increase in postoperative mortality [3/19 (15.8%) vs 12/108 (11.1%), p=0.560, Log rank test]. However, longer surgery duration was significantly associated with worse overall survival (OR, 3.262; 95% CI, 1.261– 9.169, p=0.025).
Conclusion: POD was not associated with long-term ADL or mortality after laryngectomy. Prolonged surgery was the only factor associated with a higher postoperative mortality rate.
Keywords: laryngeal cancer, postoperative delirium, activities of daily living, outcome
Introduction
Postoperative delirium (POD) is a frequent postoperative complication in elderly patients, which can increase the risk of other postoperative complications, prolong hospital stay, reduce postoperative survival, and increase medical costs.1–4 Although it is commonly believed that POD is a transient and reversible cognitive disorder, increasing evidence suggests that POD may lead to poor long-term outcomes.3,5,6
Studies have explored the relationship between POD and activities of daily living (ADL).7,8 Marcantonio et al7 reported that POD could lead to poor ADL 1 month after surgery, but this association disappeared by 6 months postoperatively. Another study showed that POD was associated with persistent impaired postoperative ADL.9 However, a systematic review concluded that the existence of a causal relationship between delirium and postoperative mortality remains controversial.10 Furthermore, a number of studies have reported clear associations between POD and an increased risk of death,11,12 while other studies have noted that this relationship disappears after adjusting for confounding factors.13,14 Thus, the relationships between POD and postoperative ADL and between POD and postoperative mortality remain to be established.
We therefore conducted a prospective study to investigate the effects of POD on postoperative ADL and mortality in patients undergoing laryngectomy. We postulated that POD would lead to a decline in postoperative ADL, as well as an increase in postoperative mortality.
Patients and Methods
Study Population
This protocol was approved by the institutional review board of the Shanghai Eye, Ear, Nose, and Throat Hospital, which is affiliated with Fudan University in Shanghai, China (number: 2017029). And this study was conducted in accordance with the Declaration of Helsinki. All patients signed the informed consent before being enrolled in the study. Qualified participants were screened and enrolled exclusively at this hospital from April 2018 to December 2018. Follow-up assessments were performed 24 months after surgery. We selected patients who met the following criteria: (1) aged 65 y or older, (2) Chinese Mandarin as the native language, (3) scheduled to undergo laryngectomy, and (4) sufficient verbal communication and writing skills to provide informed consent. Eligible surgery included partial laryngectomy and total laryngectomy. The exclusion criteria were as follows: (1) unwillingness to participate in the study; (2) pre-existing neurologic disease, such as Parkinson’s disease or Alzheimer’s disease; (3) history of mental disorders; or (4) preoperative ADL assessment or POD assessments not completed.
Preoperative Interview
Patients were assessed the day before surgery. The assessments included a review of the patient’s medical chart and an interview with the patient. Data of the patients were collected, including age, sex, American Society of Anesthesiologists (ASA) classification, years of education, presence of hypertension, diabetes mellitus, cerebrovascular disease. Cognitive status was measured by using the mini-mental state examination (MMSE).15 The Cumulative Illness Rating Scale (CIRS)16 was used to evaluate each patient. Baseline ADL status was assessed by using the Chinese version of the activities of daily living scale,17 which included a physical self-maintenance scale and instrumental activities of daily living scale. There are 14 items with the total score of ADL scale ranges from 14 to 56. Specifically, the physical self-maintenance scale is used to assess the fundamental skills typically needed to manage basic physical needs and consists of the following six tasks: transferring/ambulating, eating, dressing, grooming/personal hygiene, bathing, and toileting/continence; the instrumental activities of daily living scale is used to assess more complex activities related to independent living and contains the following eight tasks: taking public transportation, preparing food, housekeeping, taking medications, doing laundry, shopping, making phone calls, and managing finances. For each item, the scoring is determined by a 4-point coding system: 1, can do it myself; 2, have some difficulty doing but can still do it by myself; 3, need help to do it; 4, cannot do it at all. The patients with ADL scale scores more than 22 points were defined as having impairment in ADL.18
Anesthesia and Surgery
All patients were scheduled to undergo laryngectomy and followed a standardized perioperative management strategy (including anesthesia and postoperative pain management) based on routine clinical practice at our institution. The patient’s anesthesia records were reviewed for able to obtaining the data of anesthesia types, type of surgery, duration of surgery, tumor stage, hospital stay length, and presence of intraoperative hypotension. Prolonged surgery was defined as duration of surgery ≥3 h. Intraoperative hypotension was defined as blood pressure less than 70% of baseline and lasting for 30 mins or more.
Postoperative Delirium Assessment
POD was assessed once daily from 4:00 pm to 6:00 pm on days 1 through 6 after surgery. Diagnosis of POD was determined according to the Confusion Assessment Method (CAM) diagnostic algorithm,19 a common diagnostic method for identifying the presence of delirium. The algorithm consists of four clinical criteria: (1) acute onset and fluctuating course, (2) inattention, (3) disorganized thinking, and (4) altered level of consciousness. The diagnosis of delirium requires the presence of both the first and second criteria, as well as either the third or fourth criteria. The Chinese-language CAM has been shown to have good reliability and validity among the Chinese elderly population.20 Patients who met the above diagnostic criteria at any time from postoperative days 1 to 6 were designated as having POD.
Follow-Up Assessments
Follow-up interviews were conducted 24 months after surgery. The interviews were performed through telephone calls by staff who were unaware of the patients’ POD diagnosis. The Chinese version of the Index of ADL scale21 was used to assess ADL before and after surgery. Information regarding deaths was obtained by querying family members and reviewing electronic medical records. The CAM assessment for POD was performed on only the first 6 postoperative days, not at the follow-up interview.
Statistical Analysis
The Kolmogorov–Smirnov test was used to verify that all variables exhibited a normal distribution. Between-group differences were compared using Student’s t-test for continuous variables (mean ± standard deviation) or chi-square test for categorical variables (number [%]). The overall mortality rate was estimated using Kaplan–Meier analysis, and differences between groups were compared using the Log rank test. Cox regression analysis was performed to determine the association between POD and overall survival. Factors significantly associated with POD in univariable analysis were included as covariates in the Cox survival analysis model. Because burden of comorbidities and duration of surgery have been demonstrated to affect postoperative short-term and long-term survival rates, the presence of comorbidities and duration of surgery were also included as a covariate in the model. All analyses were performed using SPSS version 20.0 or Prism 6 software, with p<0.05 set as the significance level.
Results
Baseline Characteristics and Rate of Postoperative Delirium
The flow chart in Figure 1 shows disposition of the 142 potential patients, including the number included and excluded. A total of 15 patients were excluded because they declined to participate or did not complete all of the POD assessments. The final study population included 127 patients, aged 70.3 ± 4.1 y. They were all male. All patients underwent laryngectomy under general anesthesia, including total laryngectomy (n=30), partial laryngectomy (n=52), total laryngectomy plus neck dissection (n=29), and partial laryngectomy plus neck dissection (n=16). Patient characteristics are shown in Table 1.
 |
Table 1 Baseline Characteristics of Participants |
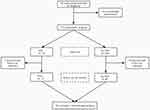 |
Figure 1 Flow chart. This chart shows the patient enrollment, excluded patients, and participants available for analysis. Abbreviation: POD, postoperative delirium. |
Of the 127 patients, 19 (15.0%) developed POD. The POD type was hyperactive in 4 cases (21.1%) and hypoactive in 15 cases (78.9%). There were no significant differences in age, education level, MMSE, CIRs, type of surgery, hospital stay length, or duration of surgery between patients with POD and those without POD. Patients who developed POD had a higher ASA classification (p=0.032) and higher tumor stage (p=0.007). More patients in POD group experienced intraoperative hypotension (p=0.022) (Table 1).
Association Between Postoperative Delirium and Long-Term Outcomes
During the study, 20 patients (15.7%) were lost to follow-up and did not complete the follow-up interview. The rate of POD and other baseline characteristics did not differ significantly between the 107 patients who continued the study and the 20 who were lost to follow-up (Table 2). Another 15 participants (11.8%) died during the follow-up period, which was confirmed by contacting family members and reviewing electronic medical records. Consequently, 92 participants completed the follow-up telephone assessments and were included in the ADL analysis (Figure 1).
 |
Table 2 Demographic and Clinical Characteristics Between Participants Who Continue the Study and Those Who Withdraw from the Study |
When considering all patients, ADL scores at 24 months after surgery were similar between patients who developed POD and those who did not develop POD (98.6 ± 1.4 vs 96.0 ± 2.0, p=0.599). The lack of difference in ADL between patients with or without POD was also observed during subgroup analysis based on the type of surgery (all p >0.05) (Table 3).
 |
Table 3 Comparison of Activities of Daily Living Between Participants with and without Postoperative Delirium |
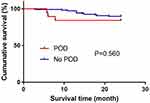
We used Kaplan–Meier analysis and Log rank test to compare mortality in the first 24 months after surgery between patients with or without POD. The mortality rate at 24 months postoperatively was not significantly different between patients with or without POD [3/19 (15.8%) vs 12/108 (11.1%), p=0.560, Log rank test] (Figure 2). Univariable and multivariable analyses of overall survival were performed using Cox regression models. POD was not associated with 24-month survival (OR=0.946, 95% CI, 0.226–3.970, p=0.940). However, increased length of surgery was associated with a higher risk of mortality (OR =3.262, 95% CI, 1.261–9.169, p=0.025) (Table 4).
 |
Table 4 Risk Factors Affecting Postoperative Survival Rate |
Discussion
This study demonstrated that for patients undergoing laryngectomy, ADL at 24 months after surgery and mortality within 24 months postoperatively were not significantly associated with the presence of POD. However, postoperative survival was associated with the duration of surgery.
Previous studies reported POD incidence rates ranging from 11.5% to 17%,22,23 The 15.0% incidence found in the present study is consistent with these previous results. Many studies reported age as a risk factor for POD;23–25 however, we observed no significant relationship between age and POD. A total of 15 older patients were excluded because they declined to participate or did not complete the POD assessments. Had these patients been included, age may have been a risk factor for POD in our study. In our study, advanced tumor stage was a risk factor for POD in elderly patients, which is consistent with the findings of previous studies.26,27 Patient frailty increases as tumor progresses, which may place patients at higher risk for developing POD. Similar to the findings in our previous study,28 we found that advanced ASA classification and intraoperative hypotension were risk factors for POD.
Previous investigations have reported associations between POD and decreased ADL in the first 1 to 3 months after hip surgery.1,7,29 Recently, Shi et al found that patients with POD experienced a greater decline in ADL and exhibited higher mortality within 24 to 36 months after major orthopedic surgery.30 Contrary to these results, we found no association between POD and ADL decline or increased cumulative mortality at 24 months after laryngectomy.
ADL are commonly used to assess quality of life of patients after surgery and are an important aspect of postoperative surgical evaluation.17,18 Patients who develop POD have been shown to have worse recovery within 6 months postoperatively than those who do not develop POD.7,8,11,29 Shi et al found that long-term ADL were impaired after surgery in elderly patients with POD.30 The difference between these results and our finding of no association between POD and long-term ADL may be attributed to differences in study populations and methodologies, including differences in type of surgery (hip or proximal femoral nail surgery vs laryngectomy), baseline ADL score (15 to 22 vs 99), age (79 to 83 y vs mean of 70.3 y), and time of follow-up interview (24 to 36 months vs 24 months).
Our finding of no association between POD and mortality also differs from the results of previous studies. Most studies have suggested that POD is associated with increased mortality at 6 months,11 12 months,12 24 months,30 and 5 years31 postoperatively. However, we did identify prolonged surgery duration as a risk factor for increased postoperative death, which is consistent with the findings of previous studies.25,32 This association may be attributed to prolonged surgery reflecting more complicated procedures and more advanced tumors. This finding suggests that strategies to prevent POD should be considered in patients undergoing longer surgery.
Limitations
The present study has some limitations. First, the sample size was relatively small: only 107 and 92 patients were included in the final analysis of mortality and ADL, respectively, which may have affected the statistical analysis results. Second, because patients were required to sign an informed consent form, individuals who refused to participate or who were unable to sign the form were excluded from the study. Thus, this may have eliminated some patients with a higher risk of POD and thus underestimated the true rates of ADL impairment and death. Third, only the CAM instrument was applied to screen POD in the current study. There is a need to use more validated and structured instruments for delirium assessment.33,34 As well, once daily delirium assessment in this study is also a limitation due to the fluctuating nature of this syndrome. Finally, in contrast with other surgery (eg, hip and proximal femoral nail surgery), which may directly impair ADL, laryngectomy has little effect on ADL. Therefore, the ADL assessment scale used in this study may not be the most appropriate tool for patients undergoing laryngectomy. In addition, POD may associate with postoperative long-term adverse cardiac events35 which we did not investigate in the current study.
Conclusion
In conclusion, the current study showed that POD in patients undergoing laryngectomy was not associated with long-term postoperative decline in ADL or overall survival. Prolonged surgery, however, was associated with lower overall survival postoperatively.
Author Contributions
Xia Shen: study concept and design; critical revision of the manuscript for important intellectual content; study supervision; final approval of the version to be published; and agreement to be accountable for all aspects of the work. Yiru Wang: study concept and design; acquisition, analysis, and interpretation of data; drafting and revision of the manuscript; final approval of the version to be published; and agreement to be accountable for all aspects of the work. Weiwei Liu: study concept and design; acquisition, analysis, and interpretation of data; administrative, technical, and material support; drafting and revision of the manuscript; final approval of the version to be published; and agreement to be accountable for all aspects of the work. Kaizheng Chen: acquisition, analysis, and interpretation of data; administrative, technical, and material support; drafting of the manuscript; final approval of the version to be published; and agreement to be accountable for all aspects of the work. All authors contributed to data analysis, drafting or revising the article, have agreed on the journal to which the article will be submitted, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Funding
This work was supported by the hospital double priority project A, SYA202010.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Jankowski CJ, Trenerry MR, Cook DJ, et al. Cognitive and functional predictors and sequelae of postoperative delirium in elderly patients undergoing elective joint arthroplasty. Anesth Analg. 2011;112:1186–1193. doi:10.1213/ANE.0b013e318211501b
2. Neufeld KJ, Leoutsakos JS, Sieber FE, et al. Outcomes of early delirium diagnosis after general anesthesia in the elderly. Anesth Analg. 2013;117:471–478. doi:10.1213/ANE.0b013e3182973650
3. Maldonado JR. Neuropathogenesis of delirium: review of current etiologic theories and common pathways. Am J Geriatric Psychiatry. 2013;21:1190–1222.
4. Inouye SK, Westendorp RG, Saczynski JS. Delirium in elderly people. Lancet. 2014;383:911–922. doi:10.1016/S0140-6736(13)60688-1
5. Falsini G, Grotti S, Porto I, et al. Long-term prognostic value of delirium in elderly patients with acute cardiac diseases admitted to two cardiac intensive care units: a prospective study (DELIRIUM CORDIS). Eur Heart J Acute Cardiovasc Care. 2018;7:661–670. doi:10.1177/2048872617695235
6. Dasgupta M, Brymer C. Prognosis of delirium in hospitalized elderly: worse than we thought. Int J Geriatr Psychiatry. 2014;29:497–505. doi:10.1002/gps.4032
7. Marcantonio ER, Flacker JM, Michaels M, Resnick NM. Delirium is independently associated with poor functional recovery after hip fracture. J Am Geriatr Soc. 2000;48:618–624. doi:10.1111/j.1532-5415.2000.tb04718.x
8. Marcantonio E, Ta T, Duthie E, Resnick NM. Delirium severity and psychomotor types: their relationship with outcomes after hip fracture repair. J Am Geriatr Soc. 2002;50:850–857.
9. Hshieh TT, Saczynski J, Gou RY, et al. Trajectory of functional recovery after postoperative delirium in elective surgery. Ann Surg. 2017;265:647–653. doi:10.1097/SLA.0000000000001952
10. Hamilton GM, Wheeler K, Di Michele J, Lalu MM, McIsaac DI. A systematic review and meta-analysis examining the impact of incident postoperative delirium on mortality. Anesthesiology. 2017;127:78–88. doi:10.1097/ALN.0000000000001660
11. Mosk CA, Mus M, Vroemen JP, et al. Dementia and delirium, the outcomes in elderly hip fracture patients. Clin Interv Aging. 2017;12:421–430. doi:10.2147/CIA.S115945
12. Dubljanin-Raspopović E, Markovic DL, Marinković J, Grajić M, Tomanovic VS, Bumbaširević M. Use of early indicators in rehabilitation process to predict one-year mortality in elderly hip fracture patients. Hip Int. 2012;22:661–667. doi:10.5301/HIP.2012.10142
13. Gottschalk A, Hubbs J, Vikani AR, Gottschalk LB, Sieber FE. The impact of incident postoperative delirium on survival of elderly patients after surgery for hip fracture repair. Anesth Analg. 2015;121:1336–1343. doi:10.1213/ANE.0000000000000576
14. Furlaneto ME, Garcez-Leme LE. Impact of delirium on mortality and cognitive and functional performance among elderly people with femoral fractures. Clinics (Sao Paulo). 2007;62:545–552. doi:10.1590/S1807-59322007000500003
15. Folstein MF, Folstein SE, McHugh PR. “Mini-mental state”. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res. 1975;12:189–198. doi:10.1016/0022-3956(75)90026-6
16. Miller MD, Paradis CF, Houck PR, et al. Rating chronic medical illness burden in geropsychiatric practice and research: application of the cumulative illness rating scale. Psychiatry Res. 1992;41:237–248. doi:10.1016/0165-1781(92)90005-N
17. Chen P, Yu ES, Zhang M, Liu WT, Hill R, Katzman R. ADL dependence and medical conditions in Chinese older persons: a population-based survey in Shanghai, China. J Am Geriatr Soc. 1995;43:378–383.
18. Lawton MP, Brody EM. Assessment of older people: self-maintaining and instrumental activities of daily living. Gerontologist. 1969;9:179–186.
19. Inouye SK, van Dyck CH, Alessi CA, Balkin S, Siegal AP, Horwitz RI. Clarifying confusion: the confusion assessment method. A new method for detection of delirium. Ann Intern Med. 1990;113:941–948. doi:10.7326/0003-4819-113-12-941
20. Leung J, Leung V, Leung CM, Pan PC. Clinical utility and validation of two instruments (the Confusion Assessment Method Algorithm and the Chinese version of Nursing Delirium Screening Scale) to detect delirium in geriatric inpatients. Gen Hosp Psychiatry. 2008;30:171–176. doi:10.1016/j.genhosppsych.2007.12.007
21. Katz S, Downs TD, Cash HR, Grotz RC. Progress in development of the index of ADL. Gerontologist. 1970;10:20–30. doi:10.1093/geront/10.1_Part_1.20
22. Shah S, Weed HG, He X, Agrawal A, Ozer E, Schuller DE. Alcohol-related predictors of delirium after major head and neck cancer surgery. Arch Otolaryngol Head Neck Surg. 2012;138:266–271. doi:10.1001/archoto.2011.1456
23. Zhu Y, Wang G, Liu S, et al. Risk factors for postoperative delirium in patients undergoing major head and neck cancer surgery: a meta-analysis. Jpn J Clin Oncol. 2017;47:505–511. doi:10.1093/jjco/hyx029
24. Aldecoa C, Bettelli G, Bilotta F, et al. European Society of Anaesthesiology evidence-based and consensus-based guideline on postoperative delirium. Eur J Anaesth. 2017;34:192–214.
25. Densky J, Eskander A, Kang S, et al. Risk factors associated with postoperative delirium in patients undergoing head and neck free flap reconstruction. JAMA Otolaryngol Head Neck Surg. 2019;145:216–221. doi:10.1001/jamaoto.2018.3820
26. Honda S, Furukawa K, Nishiwaki N, et al. Risk factors for postoperative delirium after gastrectomy in gastric cancer patients. World J Surg. 2018;42:3669–3675. doi:10.1007/s00268-018-4682-y
27. Yamagata K, Onizawa K, Yusa H, Wakatsuki T, Yanagawa T, Yoshida H. Risk factors for postoperative delirium in patients undergoing head and neck cancer surgery. Int J Oral Maxillofac Surg. 2005;34:33–36. doi:10.1016/j.ijom.2004.03.005
28. Wang Y, Yu H, Qiao H, Li C, Chen K, Shen X. Risk factors and incidence of postoperative delirium in patients undergoing laryngectomy. Otolaryngol Head Neck Surg. 2019;161:807–813. doi:10.1177/0194599819864304
29. Rudolph JL, Inouye SK, Jones RN, et al. Delirium: an independent predictor of functional decline after cardiac surgery. J Am Geriatr Soc. 2010;58:643–649. doi:10.1111/j.1532-5415.2010.02762.x
30. Shi Z, Mei X, Li C, et al. Postoperative delirium is associated with long-term decline in activities of daily living. Anesthesiology. 2019;131:492–500. doi:10.1097/ALN.0000000000002849
31. Lundstrã¶m M, Edlund A, Bucht G, Karlsson S, Gustafson Y. Dementia after delirium in patients with femoral neck fractures. J Am Geriatr Soc. 2003;51(7):1002–1006. doi:10.1046/j.1365-2389.2003.51315.x
32. Fernandez-Zamora MD, Gordillo-Brenes A, Banderas-Bravo E, et al. Prolonged mechanical ventilation as a predictor of mortality after cardiac surgery. Respir Care. 2018;63:550–557. doi:10.4187/respcare.04915
33. Marra A, Kotfis K, Hosie A, et al. Delirium monitoring: yes or no? That is the question. Am J Crit Care. 2019;28:127–135. doi:10.4037/ajcc2019874
34. Marra A, Boehm LM, Kotfis K, Pun BT. Monitoring for delirium in critically ill adults. Delirium. 2020;13–25.
35. Ogawa M, Izawa KP, Satomi-Kobayashi S, et al. Impact of delirium on postoperative frailty and long term cardiovascular events after cardiac surgery. PLoS One. 2017;12:e190359. doi:10.1371/journal.pone.0190359
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.