Back to Journals » Patient Preference and Adherence » Volume 16
Poor Compliance Causes Acute Rejection in Kidney Transplant Recipients During COVID-19 Pandemic: 2 Cases Report
Authors Ma K , An Y, Lu X, Wu J
Received 25 September 2021
Accepted for publication 16 December 2021
Published 11 January 2022 Volume 2022:16 Pages 61—68
DOI https://doi.org/10.2147/PPA.S337448
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Naifeng Liu
Kuifen Ma,1 Yuanheng An,1 Xiaoyang Lu,1 Jianyong Wu2
1Department of Pharmacy, The First Affiliated Hospital, Zhejiang University School of Medicine, Hangzhou, Zhejiang, People’s Republic of China; 2Kidney Disease Center, The First Affiliated Hospital, College of Medicine, Zhejiang University, Hangzhou, Zhejiang, People’s Republic of China
Correspondence: Jianyong Wu Email [email protected]
Abstract: The COVID-19 pandemic has lasted for more than one year, which caused much trouble to the health management of kidney transplant recipients. Numerous patients cancelled their review appointment or even lost connection with doctors because of the great pressure medical system undergoing, strict travel restrictions, and the worries about COVID-19 infection risk. Herein, we introduce two kidney transplant recipients, a 33-year-old man and a 32-year-old man, who did not take the immunosuppressant drugs and did not go back to the hospital to do the renal function examination as the doctor’s request. When they paid their first return visit several months after the pandemic outbreak, they were both diagnosed with acute rejection and admitted to the hospital. After receiving pulse steroid therapy, they were in remission but failed to reverse the rejection. The level of serum creatinine did not recover to the one before pandemic outbreak. These cases suggest that it is necessary to ensure that kidney transplant recipients follow the doctor’s advice to take drugs and follow-up regularly to examine their renal function over pandemic period. Additionally, typical pulse steroid therapy may not that effective toward these patients.
Keywords: acute rejection, kidney transplantation, health management, COVID-19, compliance
Introduction
Since novel coronavirus disease (COVID-19) pandemic outbreaks began in Wuhan, China, in Dec. 2019, it spread all over the world within a few months. As of 1 November 2021, over 249 million confirmed cases and more than 5 million deaths related to COVID-19 have been reported worldwide.1 The mortality rate of SARS-CoV-2 infection is significantly differs around the world, ranging from 0.3% to 8.4%.2 Although the COVID vaccines have now been developed and distributed to every nation gradually, we need fairly a long time to fully eliminate the disastrous influence this pandemic has made.
Comparing with normal healthy people, kidney transplant recipients who are immunocompromised because of long-term using of immunosuppressant faced much higher infected risk during this pandemic. Some researchers have focused on the balance of immunosuppression and antiinfection, giving suggestions about how to adjust immunosuppressive scheme to improve the overall clinical outcome as far as possible.3,4 The experiences about the treatment of transplant recipients with COVID-19 have been also shared.5,6
However, the incompliance and sharp decline of return visit frequency caused indirectly by the pandemic, which is a huge threat to the health management of kidney transplant recipients, have not yet raised enough concern. Ensuring the patients following the doctor’s advice to take immunosuppressant during the pandemic period is necessary. Accumulating experiences can also help us to improve the outcome of these patients. Thus, we share our experience with two kidney transplant recipients with acute rejection after the pandemic outbreak displaying their clinical course.
The source of the donated kidneys in case 1 was from his father, and case 2 was donated after cardiac death. Both kidneys were donated voluntarily with written informed consent, and that this was conducted in accordance with the Declaration of Istanbul. The study was approved by Clinical research ethics committee of the First Affiliated Hospital Zhejiang University School of Medicine (NO. 2021-667). Individual informed consents for case presentations and publication were obtained from patients.
Case 1
A 33-year-old man was diagnosed as IgA nephropathy and received living-related donor kidney transplantation in Oct. 2014. The maintenance immunosuppressants were prednisone (5mg qd), tacrolimus capsules (1mg bid), mycophenolate mofetil (MMF) (500mg bid), in addition diltiazem hydrochloride tablets (30mg bid) (Figure 1). The level of serum creatinine (sCr) fluctuated between 120 and 130μmol/L in a long period of time after operation (Figure 2). The tacrolimus trough was around 5.0ng/mL (Figure 3).
After the outbreak of COVID-19 pandemic, he has no longer paid return visit to hospital from Jan. 2020 to Aug. 2020. According to the patient’s word, he randomly reduced the dosage and frequency of medication for about 2 months (Feb. 2020 and Mar. 2020) without consulting with doctors. On September 1, 2020, he went back to hospital and had the renal function examination. Laboratory examination reported that his sCr level increased to 187μmol/L and he presented proteinuria (1+). The tacrolimus trough was 5.1ng/mL, showing no abnormity. So, the outpatient doctor rose the dosage of prednisone and MMF. One week after, his renal function did not improve, and he was admitted to hospital on September 7, 2020.
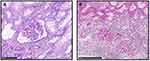
The patient had no obvious symptom when he was hospitalized. On hospital day 2, the laboratory findings showed that the level of sCr and estimated glomerular filtration rate (eGFR using CKD-EPI equation) was 168μmol/L and 35mL/min/1.73m2. C-reactive protein (CRP) was 1.8mg/L and proteinuria improved (±). The tacrolimus trough spiked to 9.1ng/mL because of interaction with dose adjustment of prednisone and MMF. Therefore, we lessened the tacrolimus dose. After that, the trough level steadily declined (Figure 3). Then, he received renal biopsy on hospital day 2. Two days after, pathology report concluded T-cell mediated acute rejection (TCMR) type IA and glomerulonephritis, conforming with pulse steroid therapy indication (Figure 4). Thus, the patient was given high dose of intravenous methylprednisolone for 4 days (500mg qd for 3 days and 240mg qd for 1 day). After the pulse therapy, the level of eGFR rose to 45mL/min/1.73m2, and sCr level fell to 170μmol/L. On hospital day 8, the day after the end of pulse therapy, he was discharged from hospital with stable vital sign and no discomfort. His renal function kept stable after this hospitalization and the sCr level fluctuated between 160 and 170μmol/L (Figure 2).
Case 2
A 32-year-old male kidney transplant recipient, with polyuria, foamy urine, and nocturia, was admitted to our hospital on Sep. 26, 2020. He received kidney transplantation in other transplantation center in Jun, 2013. The source of donor kidney was unknown. He had regular follow-up examination of renal function in our hospital after the operation. The maintenance immunosuppressants were methylprednisolone (8mg qd), tacrolimus (1mg bid), mycophenolate mofetil (MMF) (750mg bid) (Figure 5). The level of sCr stabilized at around 80μmol/L in 7 years after transplantation. However, he did not follow up after the pandemic outbreak for 7 months, from Jan. 2020 to Jul. 2020. The change of his kidney function is not clear during that period. Also, due to the lockdown policy and his busy work, the patient sometimes skipped a dose without the doctor’s advice.
 |
Figure 5 Changes in drug administrations of case 2. Abbreviations: PDN, prednisone; Tac, tacrolimus; MMF, mycophenolate mofetil; MPN, methylprednisolone; TMG, thymoglobulin; D1 1st, the hospital day 1 of first hospitalization; D1 2nd, the hospital day 1 of second hospitalization. Note: The grey grids mean the same as the ones in Figure 1. |
One month before, in Jul. 2020, the patient felt stomachache. Nausea, vomiting, and diarrhea occurred. Therefore, he went to a local hospital and had the examination which reported that the sCr level was as high as 181μmol/L, the 24-hour ration volume of urine protein was 287mg/24h, and level of type II panel reactive antibody (PRA) was 22.5%. He received gamma globulin pulse therapy for 5 days (4 bottles per day) but the sCr level increased continuously. The symptoms mentioned above occurred subsequently. Thus, he came to our hospital to seek further treatment. On Sep.24, 2020, the latest follow-up examination before hospitalization reported that his renal function deteriorated further. His sCr level rose to 236μmol/L, and the level of eGFR was 30mL/min/1.73m2 (Figure 6).
On the hospital day 1, we adjusted his immunosuppressants first. We stopped methylprednisolone, and started prednisone (10mg qd). Tacrolimus dose was increased to 1mg in the morning and 1.5mg in the evening. MMF dose was 750mg in the morning and 500mg in the evening (Figure 5). We expected that this adjustment of immunosuppressants can improve his renal function, but it produced only little effect. Urine volume decreased gradually. So, he received renal biopsy on the hospital day 5. It was suggested orally that the patient had rejection by the surgeon. In consideration of the high level of PRA reported one month ago by that local hospital, we decided to start the pulse steroid therapy. The patient was given intravenous methylprednisolone for 4 days (500mg qd for 3 days and 240mg qd for 1 day). The effect of pulse therapy was significant. Foamy urine and nocturia disappeared. The rise of sCr level was reversed. On the hospital day 13, the day he was discharged from hospital, the sCr level sharply declined from the highest 294μmol/L (appeared on the hospital day 8) to 200μmol/L (Figure 6). We increased the doses of MMF and prednisone again when he was discharged (MMF 750mg bid and prednisone 16mg qd).
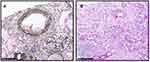
10 days after, the detailed pathology report was finished, which concluded TCMR type II A, tubular atrophy, and renal interstitial fibrosis, and occasionally seen glomerulonephritis and tubal nephritis (Figure 7). After receiving this report, we suggested him that he may need another hospitalization, taking into consideration his relative high level of sCr additionally. The patient accepted our suggestion and was admitted to hospital again on Oct. 16, 2020.
On the hospital day 1, the laboratory finding reported his sCr level was 208μmol/L. The patient was given intravenous thymoglobulin (50mg qd) for 5 days and intravenous methylprednisolone (40mg qd) for 3 days. Also, we adjusted his immunosuppressants’ dosage.
Tacrolimus dose was increased to 1.5mg bid. Prednisone dose was increased on the hospital day 3 from 16mg qd to 20mg qd. After the treatment, he was discharged on the hospital day 6 without any discomfort. After that, follow-up regular examinations reported that his sCr level fluctuated between 180 to 210μmol/L and the eGFR level stabled at around 40mL/min/1.73m2. The change of tacrolimus concentration in the whole process is shown in Figure 8. And the relevant important laboratory index values of the two cases are shown in Table 1.
 |
Table 1 Changes in Laboratory Findings of Both Two Cases |
 |
Figure 8 Changes in tacrolimus trough level of case 2. |
Discussion
Keeping the compliance of drug use is the first principle of health management of kidney transplant recipients. It requires the efforts made by the patients themselves. Also, the doctors need to remind them regularly in a long term.7 These two cases above only reduced the medication or skipped a dose, instead of stopping the medication completely. Some other cohort studies towards solid organ transplant recipients showed a similar conclusion: almost no patients completely discontinued the use immunosuppressants, but other nonadherence behaviors, such as delayed doses or skipping a dose, were very commonly seen in COVID-19 era.8,9 We can find similar phenomena in rheumatic diseases population. According to a survey conducted in America in April 2020, 48% of the total of 530 interviewees cancelled or postponed the appointment with their rheumatologists. Besides, 14% of interviewees changed their daily drug list and dosage regardless of the doctor’s advice. 10% of them could even not obtain the drugs they need totally.10 Another investigation held in Middle East, which had 2163 participants, reported that more than 30% of participants stopped all or some medication because of the fear of infection and the shortage of drugs.11 The nonadherence of immunosuppressant differs from regions. Areas with higher COVID‐19 prevalence may see higher levels of nonadherence and patient concern.12 It is obvious that the drug compliance of countless patients with chronic diseases, not only the kidney transplant recipients, was severely impacted by this pandemic.
Another thing we find is that typical pulse steroid therapy was unable to reverse the renal dysfunction in these two cases. It only stopped the rise of sCr level, but could not restore sCr level to the one before pandemic outbreak. Even if the second patient mentioned above was admitted to hospital twice and received additional immunosuppressive treatment, his outcome was barely acceptable On the other hand, the renal dysfunction can be imperceptible. According to the experience of the first patient, his sCr level has risen by around 60μmol/L, yet he did not develop any symptoms. In summary, the deterioration of renal function can be hard to discover in condition of lack of the return visit during the pandemic period and can result in unreversed renal dysfunction, leading to poor outcome.
To improve the compliance of drug use of kidney transplant recipients in this COVID-19 pandemic, the key point is that making patients keep in touch with their doctors. In early 2020, the kidney transplant program at Columbia University Irving Medical Center implemented a telehealth program that offers virtual visits for ambulatory patients when the in-person visit is unsafe to the most patients.13 Telemedicine may have a huge potent in this area, but its effectiveness still needs a long-term evaluation. Besides, reducing the number of daily doses is another possible way to prevent patients from time nonadherence.8
In this study, we demonstrated two kidney transplant recipient cases with acute rejection caused by poor compliance. They had different immunosuppressant scheme and clinical manifestation. They received pulse steroid therapy both. The second case was in a more aggravating condition than the first case. So, he was admitted to hospital for second time and we gave him additional treatment. In the end, these two cases were discharged with acceptable clinical outcome. Basing on these two cases’ experience, it is meaningful to ensure the connection between doctors and kidney transplant recipients during pandemic period.
Disclosure
The authors report no conflicts of interest for this work.
References
1. WHO. Coronavirus (COVID-19) dashboard. Available from: https://covid19.who.int/.
2. Kordzadeh-Kermani E, Khalili H, Karimzadeh I. Pathogenesis, clinical manifestations and complications of coronavirus disease 2019 (COVID-19). Future Microbiol. 2020;15:1287–1305. doi:10.2217/fmb-2020-0110
3. Tekin S, Özdoğan H, Demir MK, Soultan H, Zafar S. Kidney transplantation and COVID-19: two case reports. Transplant Proc. 2021;53(4):1207–1210. doi:10.1016/j.transproceed.2020.10.051
4. Kute VB, Bhalla AK, Guleria S, et al. Clinical profile and outcome of COVID-19 in 250 kidney transplant recipients: a multicenter cohort study from India. Transplantation. 2021;105(4):851–860. doi:10.1097/TP.0000000000003593
5. Guillen E, Pineiro GJ, Revuelta I, et al. Case report of COVID‐19 in a kidney transplant recipient: does immunosuppression alter the clinical presentation? Am J Transplant. 2020;20:1875–1878. doi:10.1111/ajt.15874
6. Pérez‐Sáez MJ, Blasco M, Redondo‐Pachón D, et al. Use of tocilizumab in kidney transplant recipients with COVID‐19. Am J Transplant. 2020;20:3182–3190. doi:10.1111/ajt.16192
7. Moradi O, Karimzadeh I, Davani-Davari D, Shafiekhani M, Sagheb MM. Pattern and associated factors of adherence to immunosuppressive medications in kidney transplant recipients at a referral center in Iran. Patient Prefer Adherence. 2019;13:729–738. doi:10.2147/PPA.S198967
8. Cheung CY, Chan KM, Tang G, Cheung A, Chak WL. Immunosuppressive medication adherence in kidney transplant recipients during the COVID-19 pandemic: a cross-sectional study in Hong Kong. Transplant Proc. 2021;53(8):2447–2450. doi:10.1016/j.transproceed.2021.08.018
9. Hussain T, Nassetta K, Badawy SM. Adherence to immunosuppression medications among heart transplant recipients: challenges, opportunities, and potential role of digital approaches in the COVID-19 era. J Cardiovasc Dev Dis. 2021;8(6):68. doi:10.3390/jcdd8060068
10. Michaud K, Wipfler K, Shaw Y, et al. Experiences of patients with rheumatic diseases in the United States during early days of the COVID‐19 pandemic. ACR Open Rheumatol. 2020;2:335–343. doi:10.1002/acr2.11148
11. Ziadé N, El Kibbi L, Hmamouchi I, et al. Impact of the COVID‐19 pandemic on patients with chronic rheumatic diseases: a study in 15 Arab countries. Int J Rheum Dis. 2020;23:1550–1557. doi:10.1111/1756-185X.13960
12. Barnes A, Andrews J, Spizzo P, Mountifield R. Medication adherence and complementary therapy usage in inflammatory bowel disease patients during the coronavirus disease 2019 pandemic. JGH Open. 2021;5(5):585–589. doi:10.1002/jgh3.12537
13. Chang J‐H, Diop M, Burgos YL, et al. Telehealth in outpatient management of kidney transplant recipients during COVID‐19 pandemic in New York. Clin Transplant. 2020;34:e14097. doi:10.1111/ctr.14097
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.