Back to Journals » Patient Preference and Adherence » Volume 16
Polypharmacy, Medication-Related Burden and Antiretroviral Therapy Adherence in People Living with HIV Aged 50 and Above: A Cross-Sectional Study in Hunan, China
Authors Zheng C, Meng J, Xiao X, Xie Y, Zhao D ![]() , Wang H
, Wang H ![]()
Received 3 October 2021
Accepted for publication 17 December 2021
Published 7 January 2022 Volume 2022:16 Pages 41—49
DOI https://doi.org/10.2147/PPA.S340621
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Naifeng Liu
Chunyuan Zheng, Jingjing Meng, Xueling Xiao, Ying Xie, Di Zhao, Honghong Wang
Xiangya Nursing School, Central South University, Changsha, Hunan, People’s Republic of China
Correspondence: Honghong Wang
Xiangya Nursing School, Central South University, 172 Tongzipo Road, Changsha, Hunan, People’s Republic of China
Tel +86-731-82650270
Fax +86-731-88710136
Email [email protected]
Purpose: People living with HIV (PLWHIV) are susceptible to non-communicable diseases (NCDs) because of aging and infections. This means that the number of non-HIV medications increases, along with issues of polypharmacy and medication-related burden. The purpose of this study was to identify the current situation of polypharmacy and medication-related burden among PLWHIV aged 50 and above, as well as the relation between medication-related burden and antiretroviral therapy (ART) adherence.
Patients and Methods: A cross-sectional study was conducted with 185 participants recruited from two HIV clinics in Yuelu District Center for Disease Control (CDC) and Changsha First Hospital in Hunan, China. Participants filled questionnaires about comorbidities, polypharmacy, medication-related burden, ART adherence and sociodemographic characteristics.
Results: Among the participants, 40% were receiving polypharmacy, and PLWHIV, who were female (β = 5.946; 95% CI = 1.354, 10.541), had a lower monthly income (β = − 4.777; 95% CI = − 6.923, − 2.632), and took more drugs (β = 2.200; 95% CI = 1.167, 3.233) were more likely to report a higher level of medication-related burden. The score of ART adherence was negatively associated with medication-related burden (rs = − 0.250 p = 0.001).
Conclusion: The findings suggest that more attention should be paid to the issues of polypharmacy and targeted interventions should be developed to reduce medication-related burden among older PLWHIV.
Keywords: AIDS, aging, comorbidity, potential drug–drug interaction, medication burden, medication adherence
Introduction
With the scaling-up of antiretroviral therapy (ART), human immunodeficiency virus (HIV) has transformed from a fatal disease to a chronic one. People living with HIV (PLWHIV) have a near-normal life expectancy.1 By the end of 2020, the number of PLWHIV aged 50 and above reached 8,100,000 globally.2 It is estimated that, by 2030, 73% of PLWHIV will be elderly (aged 50 and above).3 Similarly, in China, the number of PLWHIV aged 50 and above rose from 20% in 2011 to 44% in 2020.4
PLWHIV are susceptible to comorbidity owing to significant immune remodeling with aging, and HIV infection has a major impact on this process.5 A modeling study has projected that about 84% of PLWHIV will have at least one non-communicable disease (NCD) and 28% will have at least three comorbidities in the next decade.3 Comorbidities will inevitably lead to polypharmacy, which is defined as taking five or more medications at one time.6 In different regions, the prevalence of polypharmacy among older PLWHIV ranges from 15% to 55%.7,8 Because of age-related physiological changes and organ hypofunction, the polypharmacy issue among older PLWHIV becomes complicated with the subsequent risk of potential drug–drug interactions (PDDIs). A cross-sectional study9 conducted in Spain with PLWHIV aged 65 and above reported that 93% were taking polypharmacy and 65% showed at least one PDDI. In China, PDDIs were found in 20% of older PLWHIV taking polypharmacy.10
A medication-related burden appears along with polypharmacy and PDDIs. It is associated with various kinds of drugs, a high frequency of taking drugs, complex treatment schemes, increased toxic and side effects, and high drug or treatment costs. A cross-sectional study11 in Kuwait showed that the vast majority of patients from specialized geriatric clinics reported suffering different degrees of medication-related burden and that there is a significant trend toward a heavier perceived burden among aged patients.
The taking of antiretroviral drugs (ARVs) correctly as prescribed is known to be the key factor in the success of treatment, as well as an important step in the HIV care continuum.12 It has been reported that the higher the medication-related burden the lower the level of medication adherence among geriatric patients.11 It therefore becomes reasonable to speculate that a medication-related burden may be negatively associated with ART adherence and accordingly to explore medication-related burden among PLWHIV aged 50 and above.
Several studies have focused on polypharmacy among elderly patients, whereas few studies have been conducted among the population of older PLWHIV in China.10,13 Owing to the chronic and persistent activation of the immune system, PLWHIV suffer from an accelerated aging and an increased prevalence of non-HIV-associated comorbidities compared to general geriatric patients.14 Although medication-related burden has been measured among elderly chronic disease patients in the community, knowledge regarding the status of the medication-related burden specifically among older PLWHIV is lacking. Therefore, we aimed to determine the current situation of polypharmacy and medication-related burden in PLWHIV aged 50 and above in Hunan province, China. The findings from this study could provide useful evidence for reducing medication-related burden among elderly PLWHIV.
Materials and Methods
Study Design and Setting
This was a cross-sectional study conducted in Changsha, the capital of Hunan province, China. By the end of October 2019, it was reported that the total number of PLWHIV in the province was 38,597.15 The research was conducted in two HIV clinics in Yuelu District Center for Disease Control (CDC) and Changsha First Hospital. PLWHIV visit the clinic to receive serological tests for treatment evaluation and ART medications every 3 to 6 months.
Sampling and Recruitment Strategies
A consecutive sample method was used to recruit PLWHIV older than 50 years who went to Yuelu District CDC and Changsha First Hospital for health services from September 2020 to January 2021. Based on a review of existing literature,11 we estimated the standard deviation of the medication burden mean score was 14.9. We used a statistical power of 95% and an alpha of 0.05, the final sample size was estimated to be 185, allowing for a 20% rate of invalid questionnaires.16 The inclusion criteria were: (a) being diagnosed with HIV, (b) being 50 years or older, (c) currently receiving ART treatment. PLWHIV were excluded from the study if they had cognitive or audiovisual impairment that prevented them from correctly understanding and filling out the questionnaire.
Study Variables and Measurement
Medication-related burden was assessed using the Chinese version of LMQ-3 (C-LMQ-3), which was originally developed and validated by Krska.17 The results of cross-cultural adaptation of C-LMQ-3 demonstrated adequate content and construct validity. The Cronbach’s α of C-LMQ-3 for elderly patients with chronic diseases was 0.855, and the result of test–retest also indicated good reliability.17 There are 8 domains and 39 items in this tool. Domains include practical difficulties (6 items), lack of effectiveness (5 items), cost-related burden (3 items), communication/relationships with health professionals (5 items), concerns about medicine use (7 items), side-effect burden (4 items), interference with day-to-day life (6 items), and autonomy/control (3 items). From strongly agree to strongly disagree, each item scored at a Likert 5-point scale. A score of 3 indicates a neutral attitude. Negatively worded statements were reverse coded for calculation of the score. The score of all items in each domain was added up, giving a total score ranging from 39 to 195. The higher the total score the heavier the medication-related burden. The degree of burden was categorized as: minimal (39–105), moderate (106–121), and high (122–195).18
We used a simple composite, 3-item measure of self-reported ART adherence, the Center for Adherence Support Evaluation (CASE) Adherence Index,19 which contains 3 multiple choices: (1) the overall situation of being unable to take ART medication on time (scored from 4-never to 1-all of the time); (2) the average number of days per week on which at least one dose of ART medication was missed (scored from 1-everyday to 6-never); (3) the last time at least one dose of ART medication was missed (scored from 1-within the past week to 6-never). Depending on the choices, an overall score ranging from 3 to 16 is obtained. The higher the score, the better the ART adherence. A score of 11 or more is generally considered as good adherence to take ART medication, and a score of less than 10 indicates “poor adherence”. The Liverpool Drug Database (https://www.hiv-druginteractions.org) was utilized to assess PDDIs. PDDIs were classified into four grades. A red flag suggests “do not co-administer”; an amber flag suggests “potential interaction”; a yellow flag suggests “potential weak interaction”; and a green flag suggests “no interaction expected.”
The sociodemographic characteristics included sex, age, place of residence, education, marital status, and income. Disease-related information was assessed on comorbidities and current use of all kinds of drugs.
Data Collection
Three trained data collectors distributed questionnaires and collected answers from participants who filled in the form themselves or by interview after obtaining verbal informed consent. We prepared a quiet room for the data collection to ensure participants’ privacy. Each interview took approximately 20 min (range = 15–25 min). Each participant received a gift valued at 20 Yuan (US$3.13) to reward them for their time and commitment.
Ethical Considerations
This study was conducted in accordance with the Declaration of Helsinki. Considering that the participants were all elderly patients, informed consent without a signature was adopted in order to minimize the burden on them. Each participant was informed about the procedures, objectives, and possible benefits/risks of the study. The questionnaire was initiated only after informed consent had been confirmed. Potential participants had the right to refuse to participate or to withdraw at any time. This study and informed consent was approved by the institutional review board (IRB) of Xiangya Nursing School of Central South University.
Statistical Analysis
We used EpiData 3.1 for data entry and Statistical Package for the Social Sciences (SPSS) 18.0 for data analysis. The distributions of continuous variables were examined by descriptive analysis and are presented as mean and standard deviation. Frequency and percentage were used to present categorical variables. An independent-sample t-test, nonparametric test, and Spearman correlation analysis were utilized to explore the independent correlation variables of medication-related burden among PLWHIV aged 50 and above. Significant correlation variables were eventually included in the analysis of multiple linear regression. The correlation between ART adherence and medication-related burden was also analyzed using Spearman correlation analysis.
Results
Demographic Characteristics
The mean age of participants was 59 years (SD = 7.5, range 50–84 years). The participants were predominantly men (n = 137, 73.5%), married (n = 145, 78.4%), and living in urban areas (n = 121, 65.4%). In terms of income, approximately 60.6% of the participants had a monthly income of less than 3000 yuan. Demographic characteristics are summarized in Table 1.
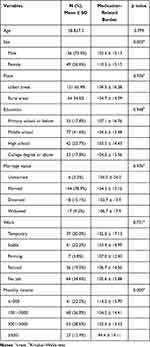 |
Table 1 Sociodemographic and Disease-Related Characteristics for People Live with HIV Aged 50 and Above (N=185) |
Comorbidities, Polypharmacy, and Potential Drug-Drug Interactions
Overall, 57.3% (106/185) of this sample had at least one comorbidity with HIV. NCDs were the most common comorbidities, including hypertension (27.0%), hyperlipidemia (17.3%), and diabetes mellitus (9.7%). Fifteen (8.1%) participants had co-infections, including tuberculosis (TB) (5.4%), hepatitis B (1.1%), hepatitis C (0.5%), and syphilis (1.1%).
The participants reported taking an average of 4.3 (SD = 1.9) kinds of drugs per day, and approximately 40% (74/185) had polypharmacy. Cardiovascular and hypoglycemic drugs were the predominant combination drugs. The top three medications that participants took were metformin (8.1%), atorvastatin (6.5%), and amlodipine (5.4%). Health care medication (21%) such as protein powder and vitamin tablets were also common in this sample (Figure 1).
 |
Figure 1 Specific classification of polypharmacy. |
A total of 45 PDDIs, including 37 amber flags, 7 yellow flags, and 1 red flag, were identified among 36 participants. The prevalence of PDDIs in participants with polypharmacy (52.8%) was significantly higher than in participants without polypharmacy (6.1%) (x2 = 26.580, p < 0.001). PDDIs occurred predominantly between antihypertensives and ARVs, accounting for 33.3% of the PDDIs. ART regimens containing Efavirenz (EFV) were most likely to manifest PDDIs, accounting for 71.1% PDDIs. PDDIs between specific medications are shown in Table 2.
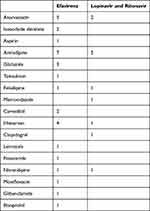 |
Table 2 Distribution of Potential Drug-Drug Interactions (PDDI) Among Specific Medications |
Medication-Related Burden and Associated Factors
The total scores for medication-related burden were normally distributed, with a mean score of 104.7 (95% CI = 102.4, 106.9) and a range of 63–154. Further analysis showed that the mean scores for medication-related burden among participants with and without polypharmacy were 109.8 (SD = 16.3) in moderate degree and 101.24 (SD = 14.0) in minimal degree, respectively, and the difference was significant (t = −3.678, p = 0.000). More than half of participants receiving polypharmacy (44/74) had a degree of burden that was moderate to high. As for domain analysis (Table 3), domains that with 4–5 scores accounted for the largest proportion were autonomy/control (94.6%), Concerns about medicine use (43.2%).
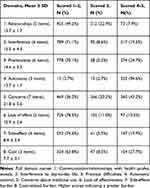 |
Table 3 Domain Analysis of Medication-Related Burden |
The results of univariate analysis (Table 1) showed that older PLWHIV who were female (t = −3.138, p = 0.002) and receiving polypharmacy (t = 2.430, p = 0.026) were more likely to report a higher level of medication-related burden. The nonparametric test showed participants who had a lower income were more likely to perceive their burden as being heavier (x2 = 22.176, p = 0.000). Further, the results from Spearman correlation analysis showed that the number of comorbidities (rs = 0.286, p = 0.000) and the number of drugs (rs = 0.218, p = 0.003) were both significantly and positively correlated with medication-related burden.
Multiple linear regression analysis showed that several variables were significantly associated with the overall score for medication-related burden. PLWHIV who were female (β = 5.946; 95% CI = 1.354, 10.541), had a lower monthly income (β = −4.777; 95% CI = −6.923, −2.632), and took more drugs (β = 2.200; 95% CI = 1.167, 3.233) were more likely to report a higher level of medication-related burden (Table 4).
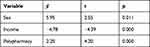 |
Table 4 Multivariable Analysis of Factors Associated with Medication-Related Burden |
ART Adherence and Its Relationship with Medication-Related Burden
Overall, the mean score of ART adherence among 185 participants was 14.8 (SD = 2.4, range 4–27). Approximately 94.6% (n = 175) of older PLWHIV had a score above 11, which means that most of the participants had good ART adherence. Based on the results of Spearman correlation analysis, the score for ART adherence was negatively associated with the overall score for medication-related burden (rs = −0.250, p = 0.001), with poor adherence being significantly associated with heavy medication-related burden. Meanwhile, it was also indicated that poor ART adherence was particularly associated with heavy burdens in following domains: practical difficulties (rs = −0.334, p = 0.000), communication/relationships with health professionals (rs = −0.267 p = 0.000), interference in day-to-day life (rs = −0.172 p = 0.019), and lack of effectiveness (rs = −0.213, p = 0.004).
Discussion
From a clinical point of view,20 HIV infection leads to an accelerated aging process, which raises the prevalence of NCDs. Despite effective ART, HIV viral replication could still cause chronic inflammation and an immune response. Moreover, the toxicity of ARVs is likely to contribute to bone, heart, and kidney diseases21 as well as neurodegenerative disorders.22 In the context of an aging cohort of PLWHIV, it is necessary to fully assess comorbidities, allocate resources appropriately, and make targeted interventions.23
Owing to the high prevalence of comorbidities, older PLWHIV are prescribed more medications for treatment compared with general geriatric patients, therefore placing them at a higher risk of polypharmacy and PDDIs.24 In addition, patients tend to visit different medical facilities for health services. When there is insufficient medical consultation and communication, patients may take medications prescribed by more than one clinician at the same time. Some patients also buy health care products over the counter. The result of mixing ARVs and these co-medications is that PDDIs are common and the metabolism, absorption, or elimination of medication through multiple pathways can be affected, sometimes to the extent that the medications lose their efficacy and the treatment of diseases can be compromised. Moreover, it has been proven that polypharmacy and PDDIs are associated with adverse health outcomes, including cognitive impairment, hospitalization, falls, and even mortality.25,26 Interestingly, the rate of PDDIs is relatively lower than that found in a previous study in the UK and Ireland, which was 57.3%.27 This may be partly because Chinese traditional medicine is an important part of Chinese culture and accordingly some patients tend to take Chinese herbs when they feel unwell. Owing to the lack of herbal medicine information in the Liverpool database, we were not able to analyze PDDIs between Chinese herbs and ARVs. This indicates a need to assess PDDIs for those patients using Chinese herbs through clinical manifestations and laboratory tests.
As expected, we found older PLWHIV who took polypharmacy reported a higher level of medication-related burden than those who did not. Indeed, most participants taking polypharmacy reported having a moderate to high level of burden. The level of medication-related burden in this sample was relatively heavy and quite close to that found in a previous study in China using the same tool for general elderly patients with chronic diseases and polypharmacy.28 However, the mean age of the sample in Wang et al’s study was 10 years older than this study. In other words, HIV infection may raise the medication-related burden for PLWHIV aged 50 and above to the same level as general geriatric patients aged 60 and above, which is an issue that deserves more attention and investigation. It is recommended that nurses start screening for medication-related burden among PLWHIV aged 50, as we did for general geriatric patients.
Autonomy/control, concerns about medicine use were the main drivers of medication-related burden. Lack of autonomy/control to vary ART regimens contributed to medication-related burden in most participants (94.6%), which was consistent with study in New Zealand.29 Adhering to ART strictly proved difficult and stressful for some patients.30 It’s challenging for aged PLWHIV to remember the time and quantity of their various medications and establish a proper schedule for taking them. Because PLWHIV have to be on ART for life, patients are much concerned about toxicities and side effects caused by long-term medication.31 In addition to encountering PDDIs, they lack drug-related information and consequently also worry about interactions between drugs and food.
The multiple linear regression analysis in the present study revealed that gender, income, and polypharmacy were closely related to the medication-related burden among older PLWHIV. Women tended to show moderate degree of medication-related burden while men with only minimal degree, which is in agreement with previous studies reporting that women tended to show higher levels of both medication-related burden and treatment burden compared with men.32,33 This difference may be linked to women’s homemaker and caregiver roles: women are playing a more important role in caring for sick family members and taking on household management duties. When women are sick, they are not able to perform these roles well, therefore women tend to perceive a greater burden related to medical treatment and more emotional distress than men.34
The cost-related burden is an important part of the medication-related burden. Although low-income patients can receive free ARVs from the China AIDS Care Program, there remain a significant number of medications that are not covered by health insurance in China. A certain degree of regionalization exists in China’s basic medical insurance system, which is also impacted by many factors such as institutional settings and economic foundations.35 Besides, worries about rising medical costs that could result from deterioration of their condition in future further increase the medication-related burden on older PLWHIV. Accordingly, the government and relevant departments should facilitate the reform of medical insurance to expand the coverage of reimbursement for chronic disease-related medications. In addition, hospitals and communities should promote the implementation of innovative outpatient chronic disease management and family doctor contract services to reduce the burden on older PLWHIV.36
A higher number of co-medications was also associated in the present study with a higher medication-related burden. This may because the more medications patients take every day, the more energy, time, money, and emotion they need to spend on medication management, including the selection, purchase, preservation, and use of drugs, observing precautions, and dealing with a possible taboo on drugs.37 Limited mobility, declining memory, and blurred vision, which are common among elderly patients, can make managing medication more difficult and complex. For older PLWHIV, nurses should assist patients with scheduling medications in a way that fits into their daily routine, such as taking medications that require an empty stomach at the same time and reducing the times for taking drugs as much as possible.
Our findings showed that medication-related burden being a significant barrier to ART adherence. Defaulting from ART leads to detrimental consequences, including treatment failure, development of viral resistance and higher risks of disease progression. Studies in the literatures reported that adherence decreased in elderly patients taking more medications38 and higher medication use was also significantly associated with non-adherence.39 Previous researches indicated that health care provider engagement and communication is highly associated with better adherence,40,41 patients had experienced poor treatment by clinical staff tend to show higher ART non-adherence.42 Therefore, it is recommended that clinicians strengthen communication with older PLWHIV, so that patients can better understand possible side effects and how to deal with them. While emphasizing the correct use of medications, we should also give priority to a single-pill combination regimen to reduce practical difficulties in taking drugs.
Our research had several limitations. First, it was based on self-reported data without verifying medical records. Older PLWHIV may not have had accurate recall of the name and quantity of drugs they were taking. Second, the Liverpool database does not have information on Chinese traditional medicines or drugs made from herbal ingredients, so the prevalence of PDDI in this study may be underestimated. Third, as our participants were recruited only from two HIV clinics in Changsha, Hunan province, the results may not be generalizable to other parts of China. Further studies should be based on medical records to guarantee the accuracy and comprehensiveness of the collected information. The PDDIs of Chinese herbs should be assessed through clinical manifestations and laboratory tests. In future, we should pay more attention to prescriptions for older PLWHIV, avoiding PDDIs as far as possible.
Conclusion
The results of our study showed that nearly half of older PLWHIV took polypharmacy, and more than half encountered PDDIs. PLWHIV who were female, had a lower income, and took more drugs were more likely to report a higher level of medication-related burden, which was significantly associated with poor ART adherence. The findings suggest that the medication issues among aged PLWHIV should be emphasized in HIV clinical settings. Clinicians and nurses should conduct thorough evaluations and be keenly aware of PDDIs when prescribing, giving priority to combination pills and long-acting drugs. Nurses could also help older PLWHIV schedule medications that pose fewer practical difficulties to further improve ART adherence.
Acknowledgments
No funding was received. We appreciate all participants for their kindly contribution to this study.
Disclosure
The authors report no real or perceived vested interests related to this article that could be construed as a conflict of interest.
References
1. Trickey A, May MT, Vehreschild J-J, et al. Survival of HIV-positive patients starting antiretroviral therapy between 1996 and 2013: a collaborative analysis of cohort studies. Lancet HIV. 2017;4(8):e349–e356. doi:10.1016/S2352-3018(17)30066-8
2. UNAIDS. AIDSinfo | UNAIDS Global data on HIV epidemiology and response; 2021.
3. Smit M, Brinkman K, Geerlings S, et al. Future challenges for clinical care of an ageing population infected with HIV: a modelling study. Lancet Infect Dis. 2015;15(7):810–818. doi:10.1016/S1473-3099(15)00056-0
4. Qiao YC, Xu Y, Jiang DX, et al. Epidemiological analyses of regional and age differences of HIV/AIDS prevalence in China, 2004–2016. Int J Infect Dis. 2019;81:215–220. doi:10.1016/j.ijid.2019.02.016
5. Leng SX, Margolick JB. Aging, sex, inflammation, frailty, and CMV and HIV infections. Cell Immunol. 2020;348:104024. doi:10.1016/j.cellimm.2019.104024
6. Masnoon N, Shakib S, Kalisch-Ellett L, Caughey GE. What is polypharmacy? A systematic review of definitions. BMC Geriatr. 2017;17(1):230. doi:10.1186/s12877-017-0621-2
7. Freedman SF, Johnston C, Faragon JJ, Siegler EL, Del CT. Older HIV-infected adults. Complex patients (III): polypharmacy. Eur Geriatr Med. 2019;10(2):199–211. doi:10.1007/s41999-018-0139-y
8. Ssonko M, Stanaway F, Mayanja HK, et al. Polypharmacy among HIV positive older adults on anti-retroviral therapy attending an urban clinic in Uganda. BMC Geriatr. 2018;18(1):125. doi:10.1186/s12877-018-0817-0
9. Bastida C, Grau A, Márquez M, et al. Polypharmacy and potential drug-drug interactions in an HIV-infected elderly population. Farm Hosp. 2017;41(5):618–624. doi:10.7399/fh.10778
10. Chen R, Chen J, Tang Q, et al. Use of comedications and potential drug-drug interactions in people living with HIV in China. J Infect Chemother. 2020;26(7):722–728. doi:10.1016/j.jiac.2020.04.003
11. Awad A, Alhadab A, Albassam A. Medication-related burden and medication adherence among geriatric patients in Kuwait: a cross-sectional study. Front Pharmacol. 2020;11:1296. doi:10.3389/fphar.2020.01296
12. Hogg RS. Understanding the HIV care continuum. Lancet HIV. 2018;5(6):e269–e270. doi:10.1016/S2352-3018(18)30102-4
13. Su BB, Ma JX, Song W, Yuan J, Dong XY, Wan J. Analysis of comorbidity and polypharmacy in middle-aged and elderly patients. Natl Med J China. 2020;100(25):1983–1987.
14. Jiménez Z, Sánchez-Conde M, Brañas F. HIV infection as a cause of accelerated aging and frailty. Rev Esp Geriatr Gerontol. 2018;53(2):105–110. doi:10.1016/j.regg.2017.04.007
15. Dan L. World AIDS day was staged by Hunan Government; 2019.
16. Sun Q. Medical statistics. B, Renwei Building, No.19 panjiayuan Nanli, Chaoyang District, Beijing: People’s Medical Publishing House; 2014.
17. Katusiime B, Corlett SA, Krska J. Development and validation of a revised instrument to measure burden of long-term medicines use: the Living with Medicines Questionnaire version 3. Patient Relat Outcome Meas. 2018;9:155–168. doi:10.2147/PROM.S151143
18. Wang Y. Cross-Cultural Adaptation and Application of Chinese Version of the Living with Medicines Questionnaire in Elderly Patients with Chronic Diseases [master]. Zhengzhou University; 2020.
19. Mannheimer SB, Mukherjee R, Hirschhorn LR, et al. The CASE adherence index: a novel method for measuring adherence to antiretroviral therapy. Aids Care. 2006;18(7):853–861. doi:10.1080/09540120500465160
20. Morowatisharifabad MA, Movahed E, Farokhzadian J, et al. Antiretroviral therapy adherence based on information, motivation, and behavioral skills model and its association with depression among HIV-positive patients: health promotion strategy towards the 909090 target. J Educ Health Promot. 2019;8:192. doi:10.4103/jehp.jehp_42_19
21. Guaraldi G, Milic J, Mussini C. Aging with HIV. Curr HIV/AIDS Rep. 2019;16(6):475–481. doi:10.1007/s11904-019-00464-3
22. Bertrand L, Velichkovska M, Toborek M. Cerebral vascular toxicity of antiretroviral therapy. J Neuroimmune Pharmacol. 2021;16(1):74–89. doi:10.1007/s11481-019-09858-x
23. Bulsara SM, Wainberg ML, Rogers K, McAloon J, Grove R, Newton-John T. The role of comorbidity on retention in HIV care. Aids Behav. 2021;25(5):1532–1541. doi:10.1007/s10461-020-02992-1
24. Harmon JL, McGee KS. Addressing polypharmacy in older adults living with HIV. J Assoc Nurses AIDS Care. 2019;30(1):73–79. doi:10.1097/JNC.0000000000000028
25. Womack JA, Murphy TE, Rentsch CT, et al. Polypharmacy, hazardous alcohol and illicit substance use, and serious falls among PLWH and uninfected comparators. J Acquir Immune Defic Syndr. 2019;82(3):305–313. doi:10.1097/QAI.0000000000002130
26. Niikawa H, Okamura T, Ito K, et al. Association between polypharmacy and cognitive impairment in an elderly Japanese population residing in an urban community. Geriatr Gerontol Int. 2017;17(9):1286–1293. doi:10.1111/ggi.12862
27. Halloran MO, Boyle C, Kehoe B, et al. Polypharmacy and drug-drug interactions in older and younger people living with HIV: the POPPY study. Antivir Ther. 2019;24(3):193–201. doi:10.3851/IMP3293
28. Wang Y, Li X, Jia D, et al. Exploring polypharmacy burden among elderly patients with chronic diseases in Chinese community: a cross-sectional study. BMC Geriatr. 2021;21(1):308. doi:10.1186/s12877-021-02247-1
29. Tordoff JM, Brenkley C, Krska J, Smith A. Exploring medicines burden among adults in New Zealand: a cross-sectional survey. Patient Prefer Adherence. 2019;13:2171–2184. doi:10.2147/PPA.S231202
30. Demain S, Gonçalves AC, Areia C, et al. Living with, managing and minimising treatment burden in long term conditions: a systematic review of qualitative research. PLoS One. 2015;10(5):e125457. doi:10.1371/journal.pone.0125457
31. Wang Y, Wang F, Wu T, et al. polypharmacy and related factors in elderly patients with functional dyspepsia. Chin J Health Stat. 2021;38(03):432–435.
32. Eton DT, Ramalho DOD, Egginton JS, et al. Building a measurement framework of burden of treatment in complex patients with chronic conditions: a qualitative study. Patient Relat Outcome Meas. 2012;3:39–49. doi:10.2147/PROM.S34681
33. Zidan A, Awaisu A, El-Hajj MS, Al-Abdulla SA, Figueroa D, Kheir KN. Medication-related burden among patients with chronic disease conditions: perspectives of patients attending non-communicable disease clinics in a primary healthcare setting in Qatar. Pharmacy. 2018;6(3). doi:10.3390/pharmacy6030085
34. Haugstvedt A, Wentzel-Larsen T, Rokne B, Graue M. Perceived family burden and emotional distress: similarities and differences between mothers and fathers of children with type 1 diabetes in a population-based study. Pediatr Diabetes. 2011;12(2):107–114. doi:10.1111/j.1399-5448.2010.00661.x
35. Zou XZ. Discussion on chronic diseases management from perspective of medical insurance. Med Soc. 2018;31(02):42–44.
36. Ye H, Wen J, Zheng J. Analysis of chronic disease long prescription in Shanghai based on the stakeholders theory. Chin Hosp. 2016;20(04):52–54.
37. Krska J, Corlett SA, Katusiime B. Complexity of medicine regimens and patient perception of medicine burden. Pharmacy. 2019;7(1). doi:10.3390/pharmacy7010018
38. Chapman RH, Petrilla AA, Benner JS, Schwartz JS, Tang SS. Predictors of adherence to concomitant antihypertensive and lipid-lowering medications in older adults: a retrospective, cohort study. Drugs Aging. 2008;25(10):885–892. doi:10.2165/00002512-200825100-00008
39. Gray SL, Mahoney JE, Blough DK. Medication adherence in elderly patients receiving home health services following hospital discharge. Ann Pharmacother. 2001;35(5):539–545. doi:10.1345/aph.10295
40. Zolnierek KB, Dimatteo MR. Physician communication and patient adherence to treatment: a meta-analysis. Med Care. 2009;47(8):826–834. doi:10.1097/MLR.0b013e31819a5acc
41. Edmonds KA, Aspiras OG, Rose JP, et al. Cross-sectional evaluation of perceived health care provider engagement, self-efficacy, and ART adherence in people living with HIV/AIDS. Aids Care. 2021;33(2):154–158. doi:10.1080/09540121.2019.1703889
42. Becker N, Poudel KC, Cordeiro LS, Sayer AG, Sibiya TE, Sibeko LN. A quantitative analysis of food insecurity and other barriers associated with ART nonadherence among women in rural communities of Eswatini. PLoS One. 2021;16(8):e256277. doi:10.1371/journal.pone.0256277
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
