Back to Journals » Orthopedic Research and Reviews » Volume 11
Pilon Fractures: Challenges and Solutions
Authors Saad BN ![]() , Yingling JM, Liporace FA, Yoon RS
, Yingling JM, Liporace FA, Yoon RS ![]()
Received 31 May 2019
Accepted for publication 28 August 2019
Published 24 September 2019 Volume 2019:11 Pages 149—157
DOI https://doi.org/10.2147/ORR.S170956
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Clark Hung
Video abstract presented by Richard S Yoon
Views: 892
Bishoy N Saad, John M Yingling, Frank A Liporace, Richard S Yoon
Division of Orthopaedic Trauma and Complex Adult Reconstruction, Department of Orthopaedic Surgery, Jersey City Medical Center - RWJBarnabas Health, Jersey City, NJ, USA
Correspondence: Richard S Yoon
Division of Orthopaedic Trauma and Complex Adult Reconstruction, Department of Orthopaedic Surgery, Jersey City Medical Center – RWJBarnabas Health, 377 Jersey Ave, Suite 280A, Jersey City, NJ 07302, USA
Tel +1 201 716 5850
Fax +1 201 915 2424
Email [email protected]
Abstract: Pilon fractures include a wide range of complexity. The timing and type of definitive fixation is dictated by the soft tissue injury and energy imparted to the fracture. One should have a low threshold for staged protocols and delayed definitive fixation to avoid complications. Proper radiographs and advanced imaging should be obtained for an exacting diagnosis and preoperative planning. Diligent management of the soft tissue and anatomic restoration of the articular surface, length, rotation, and axial alignment with stable fixation to the diaphysis should be obtained once feasible. Intramedullary implants with percutaneous articular fixation for simple or extra-articular patterns provide good results with little soft tissue insult in the zone of injury. Minimally invasive plate osteosynthesis techniques can help mitigate some concerns with soft tissue compromise while obtaining good articular alignment. Locking or conventional plating with lag screw fixation is used for complex articular injuries with or without fibular fixation. External fixators are generally used for temporizing measures but can be utilized as definitive fixation when indicated. There is a role for acute fusion in severely comminuted, osteoporotic, or arthritic fractures in patients with poor healing potential. This article outlines the diagnostic workup and treatment of these vexing injuries with solutions to challenges that arise.
Keywords: pilon fracture, plafond fracture, intra-articular ankle fractures, distal tibia fracture, AO/OTA 43A-C
Introduction
First described by French radiologist Destot in 1911, pilon fractures are defined as injuries that involve the articular weight-bearing surface of the distal tibia. The term “pilon” is derived from the French language, meaning pestle, resembling a pharmacist’s pestle when paralleled to the distal tibial metaphysis. Later termed “plafond” meaning “ceiling” in the French language, equating the distal tibial articular surface as the ceiling of the ankle joint. These injuries compile <1% of all lower extremity fractures and achieving good clinical outcomes is both challenging and complex.1 Compared to the fractures originally described and treated by Rüedi and Allgöwer, pilon fractures globally represent higher-energy mechanisms that often involve substantial articular impaction and severe soft tissue injury due to an axial load rather than the relatively low energy rotational mechanism originally studied.2–7 The importance of addressing all components of the skeletal trauma cannot be overstated. Even after successful treatment of these injuries, complications in the postoperative period, such as infection, wound dehiscence, non-union, malunion, and post-traumatic osteoarthritis are difficult to avoid without proper technique.6 Thus, this review offers an update to surgical management and treatment of pilon fractures with special considerations taken during the decision-making process.
Mechanism of Injury and Classification Systems
Rüedi and Allgöwer were one of the first to describe pilon fractures. Their classification was derived from the evaluation of rotational injuries sustained following skiing accidents.8,9 Three different fracture types based on comminution and displacement of the articular surface were proposed. Type I are intra-articular fractures without displacement, type II are displaced fractures without comminution, and type III are displaced fractures with impaction and comminution (Table 1).
 |
Table 1 Classification Systems |
While rotational pilon fractures still occur, the vast majority are the result of higher-energy mechanisms such as falls from a great height and motor vehicle accidents. The fracture pattern and soft tissue injury is dictated by the positioning of the foot at the time of injury. Typically, the talus is driven into the plafond during a high-energy axial load. When the foot is plantar-flexed at the time of injury, forces are directed into the posterior portion of the articular surface leading to impaction and posterior talar displacement. The opposite is true when the foot is dorsiflexed, the energy is transmitted through the anterior region. Neutral foot positioning results in a purely vertical vector engaging the entire articular surface, resulting in both anterior and posterior column fractures with variable varus and valgus angulation. When the force is predominantly midline or medial to the ankle, the fracture will result in a varus deformity. Likewise, when exerted lateral to the center of the ankle, valgus configuration results. Evaluation of the fibula can provide further information on the stability of the injury. For example, an intact fibula can necessitate medial column instability and varus deformity while the opposite is true when the fibula is involved.5,10,11
The Arbeitsgemeinschaft für Osteosynthesefragen/Orthopedic Trauma Association (AO/OTA) offers a more comprehensive classification system dividing up pilon fractures into Types A, B, and C with subsequent subtypes (Table 1). Type A are extra-articular fractures, Type B are partial articular involving a single column, and Type C are complete articular fractures, all with subtypes differentiated on fracture pattern, amount of comminution, and presence or location of impacted articular fragments. Likely due to the nature and variability of the multitude of possible fracture patterns, this classification is very inclusive and descriptive but shows inconsistent interobserver reliability.12–15
As a result, DeCoster et al classified patients based on the severity of injury regarding the articular surface, the entire fracture pattern, and the quality of the reduction after operative fixation. Ninety-four percent of orthopedic surgeons agreed on ranking the severity of the articular surface injury, 89% on fracture pattern and reduction of the articular surface, and 88% on the quality of the overall reduction of the injury.16 Therefore, despite disagreement on the classification of pilon fractures found among orthopedic surgeons, an interobserver agreement can be found based on evaluating the severity of injury and quality of the reduction.
Initial Evaluation and Treatment
A thorough history and physical exam upon initial presentation can aid the clinician in dictating treatment. Comorbidities, such as diabetes and smoking, tend to increase the threat of overall complications and need for revision surgery by 3.8 and 5 times, respectively.17–20 Smokers have an increased risk of wound complications due to microvascular pathology.21 Multidisciplinary care of these often polytrauma patients is important, as up to 57% have associated multisystem injuries.3,4,22–25 Initial imaging includes anteroposterior, mortise, and lateral radiographs of the ankle. Full-length tibia and fibula images further help evaluate possible extension of fracture lines into the tibial shaft, coexisting proximal fractures, or prior implants in the extremity.
The incidence of open pilon fractures ranges from 12% to 56%.3,24,25 Treatment consists of appropriate antibiotics given within 66 mins and tetanus vaccination as needed. Fracture fragments that are tenting the skin require immediate reduction to limit damage to the local circulation and minimize the risk of conversion into an open injury. Evaluating the severity of soft tissue edema plays a critical role in determining timing of definitive fixation of these complex injuries and often photographs should be taken before splinting to compare with subsequent exams. Early definitive internal fixation in the setting of severe soft tissue swelling is associated with poorer outcomes and increased complications, such as infections and wound dehiscence.11,26,27 The presence of fracture blisters can provide insight into the amount of soft tissue injury the patient has sustained. While their presence may not necessarily require a delay in definitive fixation, their location may limit the surgical approaches that can be utilized. Hemorrhagic blisters should be kept intact if possible as their rupture confers communication to the subdermal tissue. Surgical fixation should be postponed until re-epithelization of the region is achieved.28,29
A staged protocol involving initial external fixation followed by delayed definitive treatment has shown favorable results.5,10,28,30,31 Metaphyseal spikes are often present, can tent the skin, and obstruct the blood supply leading to necrosis and eventual open injury and are usually difficult to reduce. To combat this issue, posterior splint application or supplementation with metatarsal pins attached to the main ankle-spanning frame can help maintain a plantigrade foot and combat this issue.5,10,23,25,32,33 Proximal Schanz pins are placed well outside the zone of injury to prevent overlap of definitive fixation, if possible. Either a transcalcaneal or talar neck pin can be placed, taking care to avoid neurovascular structures.34 Use caution with placement of the talar pin as communication with the ankle joint or definitive incision can lead to unwanted infection. Other proposed techniques involve early limited open reduction and internal fixation (ORIF) of metadiaphyseal spikes and/or fibular fractures to provide further protection of the soft tissue and enhance the stability of the external fixator. This technique risks limiting future incisions if placed in a position that violates a desired approach. Furthermore, fixing segments in place prior to addressing the entire injury prevents their mobility during reduction, and is generally discouraged.30,31,35 The main goal of these methods is to provide an environment for the soft tissue to recover while restoring length, alignment, and rotation of the limb. The peak inflammatory response is usually reached by day 5 and resolution of edema thereafter is assessed by the skin’s ability to wrinkle. Strict adherence to ice and elevation acutely can aid in reducing edema in preparation for definitive surgery. Open injuries with soft tissue defects or tenuous closures benefit from negative pressure wound therapy and should be closely monitored with changes every 3–4 days.
Preoperative Planning
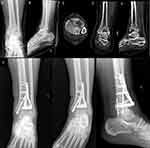
Preoperative planning begins with a thorough evaluation of the patient’s co-morbidities, functional and social status. Factors such as sex, lower socioeconomic status, laborers, and work-related injuries portend poorer outcomes. Next, a thorough evaluation of the imaging obtained to define the diagnosis and develop a treatment approach. Traction radiographs can provide a simple adjunct to injury films in a patient too unstable for advanced imaging. General restoration of the length, rotation, and axial alignment may help delineate the true fracture pattern, fragments, and range of reduction. Computed tomography (CT) provides a more detailed evaluation of the articular segments and most would agree is imperative for surgical planning. Advantages of obtaining a CT scan after external fixation or preliminary reduction and immobilization include an accurate illustration of the fracture pattern, mobility of the fragments, limit radiation exposure and cost but also as this new information may change the approach compared to a CT done prior to preliminary stabilization (Figure 1A–E).36,37 The most common fracture pattern usually splits the articular surface into three variable yet predictable fragments: the medial fragment consisting of the medial malleolus and adjacent weight-bearing segment, the anterolateral or Chaput fragment, and the posterolateral or Volkman fragment usually with their ligamentous attachments intact.38 The location of where these fracture lines exit the cortex, position of articular segments, and if those fragments lie in continuity with the intact tibial shaft dictate the location of implant placement and subsequently the surgical approach(es) used. In addition to the boney injury, it is important to identify the soft tissue components, usually with a “soft tissue window” on CT, to detect interposition of vital structures or evidence of prior surgery/injury that may dictate changes in the operative plan. There is a limited role for MRI in the acute setting of pilon fractures.
With these considerations in mind, concomitant injuries, such as spine or abdominal injuries may prevent the patient from lying prone for posterior fixation and soft tissue injury may dictate a staged approach to allow for healing or flap coverage.
Generally, an incision should overlay where the majority of implants will be placed for ease of instrument use and limit superficial soft tissue insult. The deep interval is more readily mobilized than the skin to accommodate implant placement and often multiple deep interval windows may be required through a single skin incision. A “work horse” surgical incision can be chosen depending on where one can visualize cortical alignment for a “read” during the reconstruction process or the area with the most comminuted articular fragments allowing direct visualization for reduction to the more stable fragments.5 Traditionally, anteromedial and posterolateral approaches are used to maximize exposure and the ability to evaluate the majority of articular fragments.5,8,9,39–43 When additional incisions are required, adequate spacing between them is important to avoid skin necrosis and wound complications.5,18,39 Previous teachings were a minimum of a 7-cm skin bridge needed between incisions, however low soft tissue complication rates in pilon fractures were observed in patients that had an average of 5.9 cm.39 Though likely of secondary importance to proper reduction and implant placement, be mindful of the length of the incision as skin receives its blood supply from overlapping angiosomes that may be insulted from the injury or other incisions.
The anteromedial approach is used for OTA 43B and C fractures and allows access for medial and anterior hardware placement especially when the posterolateral (Volkman) is the constant fragment.4,40,44,45 An incision is made 5 cm proximal to the ankle joint line, 1–2 fingerbreadths lateral to the tibial crest to maintain full thickness skin coverage over the near subcutaneous anteromedial tibia, and extended distally using a 60–80° curve 1 cm past the medial malleolus or along the tibialis anterior (TA) tendon toward the talonavicular joint.44,46,47 Care is taken to avoid violating the TA tendon sheath due to the fact that injury to it would limit soft tissue graft options that can be used in the event of wound complications.48 Limitation of this approach is access to the anterolateral (Tillaux-Chaput) fragment that can be more readily addressed with Böhler’s anterolateral approach.41,49
For the anterolateral Böhler’s incision, with the foot in neutral dorsiflexion, an incision is started 5 cm proximal to the tibiotalar joint and extended distally in line with the fourth metatarsal. Careful dissection is carried out in the subcutaneous tissue to identify and protect the superficial peroneal nerve branches. Furthermore, the approach can be extended to visualize the talar dome, neck, lateral talonavicular, subtalar, and calcaneocuboid joints without an increase in wound complications or difficulty in closure.41 Exposure to the anteromedial and anterolateral fragments simultaneously can be obtained with the direct anterior approach with minimal soft tissue dissection via a linear incision centered over the ankle avoiding the neurovascular bundle and being cognitive of its relation above and below the joint line.
The posterolateral approach is used to visualize the posterior central and posterolateral distal tibia and fibula. The incision is made halfway between the posterior border of the lateral malleolus and the lateral border of the Achilles tendon with caution taken to identify and protect the sural nerve. The nerve usually crosses the lateral border of the Achilles about 9.8 cm from its insertion or about four fingerbreadths and travels retromaleolar in the distal extent. A deep interval between peroneus longus and flexor hallucis longus is formed to visualize the posterior tibia and fibula. The fibula fracture can be addressed through the same deep interval medial or lateral to the peroneus muscles within the same incision. Though not observed in our experience, caution should be utilized when using this approach, as there have been reports of higher complication rates that include nonunion, wound issues, and suboptimal clinical outcomes when complete fixation is performed through one surgical approach.50 These issues may be mitigated with thorough skin prep, strict hemostasis, longer incisions, and strict protection postoperatively due to its depended location.
The incision for the posteromedial approach is made along the posterior tibialis tendon (PTT) posterior to the medial malleolus and an interval is created between PTT and flexor digitorum longus (FDL). Care is taken when placing a retractor anterior to FDL and traction is limited in this region to avoid injury to the posterior tibial artery and tibial nerve. Posteromedial approach can be utilized when addressing tendon or neurovascular bundle entrapment.42 Due to the minimal skin bridge available between both posterior approaches, consideration should be made and the area in need of direct manipulation should be chosen. If further exposure is needed, a small window for placement of a reduction aid can be used but with great caution.
Surgical Techniques
Surgical indications for operative fixation of pilon fractures include open injuries, 2 mm of articular displacement, talar subluxation, or malalignment greater than 5 degrees.8,9,36 Following AO principles, surgical fixation should provide an anatomically reduced and stable construct, be conducted with gentle soft tissue handling, and allow for early rehabilitation and mobilization.1,2,9,51 General sequence in treating these fractures includes reestablishing length and general axial alignment through fixation of the lateral column, restoration of the articular surface, filling of metaphyseal defects, and reattachment to the diaphysis.8,9
Fibular reduction functions to prevent valgus deformity of the ankle and aides in reduction of the tibial plafond. By restoring the overall limb length, the ligamentotaxis effect via the anterior inferior tibiofibular ligament and posterior inferior tibiofibular ligament allows indirect reduction of the anterolateral and posterolateral fragments, respectively. One-third tubular plates with penetration of six cortices on either side combined with lag screws perpendicular to the fracture site are sufficient for fixation. Over lengthening and malreduction can lead to varus deformity of the distal tibia and excessive loading of the lateral articular surface.47 The mortise view of the ankle is used to confirm the anatomical reduction between the distal end of the fibula, lateral tibial metaphysis, and talus.52 The fibula may not always have to be fixed. If the fibula cannot be restored to its anatomical position or does not aid in tibia reduction, it can be addressed after the pilon component or left to heal without surgical intervention. Recent literature has shown that there is no difference in final alignment when comparing fibular fractures with versus without fixation in nonrotational pilon injuries.53 Some studies show patients with ORIF of the fibula had higher nonunion rates, occasionally required plate removal and had an associated increased incidence of superficial infections.53–58
Three main fracture fragments, medial malleolus, Chaput, and Volkmann are commonly formed as a result of the fracture lines created in pilon injuries (Figure 1C).38 Again, the variability and personality of these fragments is dictated by the position of the foot and load applied, bone quality, and presence of arthritis. In use of a 2-incision approach, the posterolateral incision provides the surgeon with the ability to convert a complex pattern, OTA C-type, into one treated in a simpler manner, B-type. The posterolateral articular fragment is traditionally the more constant piece and can be the source of initial stability and preliminary fixation especially if it remains in continuity with the tibial shaft.45 In a severely comminuted scenario, the posterolateral column should be restored with preliminary reduction and fixation using a locking unicortical construct through a posterior incision in a staged fashion. This simplifies subsequent fixation from an anterior approach that is reconstructing the articular segments from a posterior to anterior direction building to that stable portion.35,43,44,46 Distraction through an AO distractor or external fixator can be utilized to obtain length, alignment, and indirect reduction by means of ligamentotaxis.45 The use of a medial talar pin can induce a distraction, plantar flexion, and valgus force. Conversely, a lateral calcaneal pin can induce a distraction, dorsiflexion, and varus force. Preliminary reduction is obtained with the combination of elevators, osteotomes, and pointed reduction clamps then preliminarily fixed with Kirschner wires (K-wires) or biologic fixation pins. In the event of small irreconstructable articular fragments, the impacted articular segment should not be disrupted but manipulated as a whole by, using the talus as a template. One technique used is levering a wide osteotome well above subchondral bone and incorporating a portion of spongy metaphyseal bone, to aid in dissipating focal point pressures, and dis-impacting the portion as one piece. By direct and indirect visualization under fluoroscopy, the reduction is evaluated for restoration of the articular surface with standard ankle views as well as oblique views to evaluate the anteromedial and lateral corners for reduction. Keep in mind the inherent 3–5 degree anterior tilt of the distal tibia articular surface when using fluoroscopy especially on the lateral view. Upon confirmation, K-wires are replaced with definitive screw fixation, and the metaphyseal defect is then filled with auto- or allograft substitutes ideally with osteoconductive, osteoinductive, and osteogenic properties.5,59 If not preliminarily reduced beforehand, the metaphyseal-diaphyseal dissociation is then addressed to realign the anatomical axis of the tibia. Columnar restoration and stability should be obtained with the construct after anatomic articular reduction and fixation. Medial column stability is mandated in varus deformities, conversely lateral column for valgus deformities, posterior column for plantar flexion, and anterior column for dorsiflexion injuries.60 Proper contouring of the plates is important to avoid residual displacement during plate fixation although this is irrelevant in the minimally invasive plate osteosynthesis (MIPO) technique.61,62
The quality of the soft tissue in the region can limit the options of multiple plate fixation. To minimize further soft tissue injury caused by surgical dissection, minimally invasive techniques such as MIPO and intramedullary nailing (IMN) have been popularized. Spatial frame application is also a useful skill in a surgeon’s armamentarium and can be utilized by those experienced in its principles and facile with the technique. Utilizing the MIPO technique, the extraosseous blood supply of the medial distal tibia is less compromised when compared to open plating.63 Challenges with this technique include plate tendency to drift posteriorly in the sagittal plane upon submuscular placement. Applying a K-wire in the posterior third of the tibia on the lateral view at one half of the plate length can aid in aligning the plate centrally.64 Though not always warranted, locking plates have demonstrated reliable treatment for patients with osteoporosis or severe comminution and provide further stability against rotational forces.46 IMN has been shown to have a role when addressing both extra-articular (AO/OTA-43A1) and simple intra-articular (AO/OTA-43C1/C2) fracture patterns (Figure 2). After addressing simple articular fractures with independent screw fixation, IMN placement restores the metaphyseal-diaphyseal dissociation and restores the overall alignment of the distal tibia reliably without insult to the surrounding soft tissue in the zone of injury.65 In the setting of severe non-reconstructable comminution, osteopenia, and arthritis in a patient with poor healing potential, there is a role for acutely fusing the tibiotalar joint. Denuding the cartilage of the talus and fusing the joint using a compression plate or screw construct, tibiotalar intramedullary device, or a combination with addition of bone graft has proven to be successful.
Summary
Pilon fractures include a wide range of complexity. The timing and type of definitive fixation is dictated by the soft tissue injury and energy imparted to the fracture. One should have a low threshold for staged protocols and delayed definitive fixation. Proper radiographs and advanced imaging should be obtained for an exacting diagnosis and preoperative planning. Diligent management of the soft tissue and anatomic restoration of the articular surface, length, rotation and axial alignment with stable fixation to the diaphysis should be obtained once feasible. Intramedullary implants with percutaneous articular fixation for simple or extra-articular patterns provide good results with little soft tissue insult in the zone of injury. MIPO techniques can help mitigate some concerns with soft tissue compromise while obtaining good articular alignment. Locking or conventional plating with lag screw fixation is used for complex articular injuries with or without fibular fixation. External fixators are generally used for temporizing measures but can be utilized as definitive fixation when indicated. There is a role for acute fusion in severely comminuted, osteoporotic, or arthritic fractures in patients with poor healing potential.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Bourne RB. Pylon fractures of the distal tibia. Clin Orthop Relat Res. 1989;240:42–46.
2. Bourne RB, Rorabeck CH, Macnab J. Intra-articular fractures of the distal tibia: the pilon fracture. J Trauma. 1983;23(7):591–596. doi:10.1097/00005373-198307000-00008
3. Grose A, Gardner MJ, Hettrich C, et al. Open reduction and internal fixation of tibial pilon fractures using a lateral approach. J Orthop Trauma. 2007;21(8):530–537. doi:10.1097/BOT.0b013e318145a227
4. Helfet DL, Koval K, Pappas J, Sanders RW, DiPasquale T. Intraarticular “pilon” fracture of the tibia. Clin Orthop Relat Res. 1994;298:221–228.
5. Sirkin M, Sanders R, DiPasquale T, Herscovici D. A staged protocol for soft tissue management in the treatment of complex pilon fractures. J Orthop Trauma. 1999;13(2):78–84.
6. Thordarson DB. Complications after treatment of tibial pilon fractures: prevention and management strategies. J Am Acad Orthop Surg. 2000;8(4):253–265.
7. Egol KA, Wolinsky P, Koval KJ. Open reduction and internal fixation of tibial pilon fractures. Foot Ankle Clin. 2000;5(4):873–885.
8. Rüedi T, Matter P, Allgöwer M. [Intra-articular fractures of the distal tibial end]. Helv Chir Acta. 1968;35(5):556–582.
9. Rüedi TP, Allgöwer M. The operative treatment of intra-articular fractures of the lower end of the tibia. Clin Orthop Relat Res. 1979;138:105–110.
10. Teeny SM, Wiss DA. Open reduction and internal fixation of tibial plafond fractures. Variables contributing to poor results and complications. Clin Orthop Relat Res. 1993;292:108–117. doi:10.1097/00003086-199307000-00013
11. McFerran MA, Smith SW, Boulas HJ, Schwartz HS. Complications encountered in the treatment of pilon fractures. J Orthop Trauma. 1992;6(2):195–200.
12. Dirschl DR, Adams GL. A critical assessment of factors influencing reliability in the classification of fractures, using fractures of the tibial plafond as a model. J Orthop Trauma. 1997;11(7):471–476.
13. Martin JS, Marsh JL, Bonar SK, DeCoster TA, Found EM, Brandser EA. Assessment of the AO/ASIF fracture classification for the distal tibia. J Orthop Trauma. 1997;11(7):477–483.
14. Ramappa M, Bajwa A, Singh A, Mackenney P, Hui A, Port A. Interobserver and intraobserver variations in tibial pilon fracture classification systems. Foot (Edinb). 2010;20(2–3):61–63.
15. Swiontkowski MF, Sands AK, Agel J, Diab M, Schwappach JR, Kreder HJ. Interobserver variation in the AO/OTA fracture classification system for pilon fractures: is there a problem? J Orthop Trauma. 1997;11(7):467–470.
16. DeCoster TA, Willis MC, Marsh JL, et al. Rank order analysis of tibial plafond fractures: does injury or reduction predict outcome? Foot Ankle Int. 1999;20(1):44–49.
17. Ovadia DN, Beals RK. Fractures of the tibial plafond. J Bone Joint Surg Am. 1986;68(4):543–551.
18. White TO, Guy P, Cooke CJ, et al. The results of early primary open reduction and internal fixation for treatment of OTA 43.C-type tibial pilon fractures: a cohort study. J Orthop Trauma. 2010;24(12):757–763.
19. Mehta SK, Breitbart EA, Berberian WS, Liporace FA, Lin SS. Bone and wound healing in the diabetic patient. Foot Ankle Clin. 2010;15(3):411–437.
20. Wukich DK, Joseph A, Ryan M, Ramirez C, Irrgang JJ. Outcomes of ankle fractures in patients with uncomplicated versus complicated diabetes. Foot Ankle Int. 2011;32(2):120–130.
21. Mills E, Eyawo O, Lockhart I, Kelly S, Wu P, Ebbert JO. Smoking cessation reduces postoperative complications: a systematic review and meta-analysis. Am J Med. 2011;124(2):144–154.e148. doi:10.1016/j.amjmed.2010.09.013
22. Bacon S, Smith WR, Morgan SJ, et al. A retrospective analysis of comminuted intra-articular fractures of the tibial plafond: open reduction and internal fixation versus external Ilizarov fixation. Injury. 2008;39(2):196–202.
23. Tornetta P, Weiner L, Bergman M, et al. Pilon fractures: treatment with combined internal and external fixation. J Orthop Trauma. 1993;7(6):489–496.
24. Pollak AN, McCarthy ML, Bess RS, Agel J, Swiontkowski MF. Outcomes after treatment of high-energy tibial plafond fractures. J Bone Joint Surg Am. 2003;85-A(10):1893–1900. doi:10.2106/00004623-200310000-00005
25. Bone L, Stegemann P, McNamara K, Seibel R. External fixation of severely comminuted and open tibial pilon fractures. Clin Orthop Relat Res. 1993;292:101–107. doi:10.1097/00003086-199307000-00012
26. Tscherne H, Gotzen L. Fractures with Soft Tissue Injuries. Berlin Heidelberg: Springer-Verlag; 1984.
27. Tscherne H, Schatzker J. Major Fractures of the Pilon, the Talus, and the Calcaneus: Current Concepts of Treatment. Berlin Heidelberg: Springer-Verlag; 1993.
28. Wyrsch B, McFerran MA, McAndrew M, et al. Operative treatment of fractures of the tibial plafond. A randomized, prospective study. J Bone Joint Surg Am. 1996;78(11):1646–1657. doi:10.2106/00004623-199611000-00003
29. Giordano CP, Koval KJ. Treatment of fracture blisters: a prospective study of 53 cases. J Orthop Trauma. 1995;9(2):171–176.
30. Liporace FA, Mehta S, Rhorer AS, Yoon RS, Reilly MC. Staged treatment and associated complications of pilon fractures. Instr Course Lect. 2012;61:53–70.
31. Liporace FA, Yoon RS. Decisions and staging leading to definitive open management of pilon fractures: where have we come from and where are we now? J Orthop Trauma. 2012;26(8):488–498. doi:10.1097/BOT.0b013e31822fbdbe
32. Barbieri R, Schenk R, Koval K, Aurori K, Aurori B. Hybrid external fixation in the treatment of tibial plafond fractures. Clin Orthop Relat Res. 1996;332:16–22. doi:10.1097/00003086-199611000-00004
33. Marsh JL, Nepola JV, Wuest TK, Osteen D, Cox K, Oppenheim W. Unilateral external fixation until healing with the dynamic axial fixator for severe open tibial fractures. J Orthop Trauma. 1991;5(3):341–348.
34. Casey D, McConnell T, Parekh S, Tornetta P
35. Dunbar RP, Barei DP, Kubiak EN, Nork SE, Henley MB. Early limited internal fixation of diaphyseal extensions in select pilon fractures: upgrading AO/OTA type C fractures to AO/OTA type B. J Orthop Trauma. 2008;22(6):426–429. doi:10.1097/BOT.0b013e31817e49b8
36. Watson JT, Moed BR, Karges DE, Cramer KE. Pilon fractures: treatment protocol based on severity of soft tissue injury. Clin Orthop Related Res. 2000;375:78–90. doi:10.1097/00003086-200006000-00010
37. Tornetta P
38. Cole PA, Mehrle RK, Bhandari M, Zlowodzki M. The pilon map: fracture lines and comminution zones in OTA/AO type 43C3 pilon fractures. J Orthop Trauma. 2013;27(7):e152–e156. doi:10.1097/BOT.0b013e318288a7e9
39. Howard JL, Agel J, Barei DP, Benirschke SK, Nork SE. A prospective study evaluating incision placement and wound healing for tibial plafond fractures. J Orthop Trauma. 2008;22(5):299–305. discussion 305–306. doi:10.1097/BOT.0b013e318172c811
40. Müller ME, Allgöwer M, Allgower M, Schneider R, Willenegger H. Manual of internal fixation: techniques recommended by the AO-ASIF group. Springer Science & Business Media; 1991.
41. Herscovici D
42. Kao KF, Huang PJ, Chen YW, Cheng YM, Lin SY, Ko SH. Postero-medio-anterior approach of the ankle for the pilon fracture. Injury. 2000;31(2):71–74. doi:10.1016/S0020-1383(99)00202-8
43. Konrath GA, Hopkins G. Posterolateral approach for tibial pilon fractures: a report of two cases. J Orthop Trauma. 1999;13(8):586–589.
44. Schatzker J, Tile M. The rationale of operative fracture care. In: Schatzker J, Tile M, editors. The Rationale of Operative Fracture Care.
45. Mast JW, Spiegel PG, Pappas JN. Fractures of the tibial pilon. Clin Orthop Relat Res. 1988;230:68–82.
46. Browner BD. Skeletal trauma: basic science, management, and reconstruction. Elsevier Health Sciences; 2009.
47. Borrelli J, Catalano L. Open reduction and internal fixation of pilon fractures. J Orthop Trauma. 1999;13(8):573–582.
48. Gould JS. Reconstruction of soft tissue injuries of the Foot and Ankle with microsurgical techniques. ORTHOPEDICS. 1987;10(1):151–157.
49. Assal M, Ray A, Stern R. The extensile approach for the operative treatment of high-energy pilon fractures: surgical technique and soft-tissue healing. J Orthop Trauma. 2007;21(3):198–206. doi:10.1097/BOT.0b013e3180316780
50. Bhattacharyya T, Crichlow R, Gobezie R, Kim E, Vrahas MS. Complications associated with the posterolateral approach for pilon fractures. J Orthop Trauma. 2006;20(2):104–107. doi:10.1097/01.bot.0000201084.48037.5d
51. Etter C, Ganz R. Long-term results of tibial plafond fractures treated with open reduction and internal fixation. Arch Orthop Trauma Surg. 1991;110(6):277–283.
52. Hedström M, Ahl T, Dalén N. Early postoperative ankle exercise. A study of postoperative lateral malleolar fractures. Clin Orthop Relat Res. 1994;300:193–196.
53. Kurylo JC, Datta N, Iskander KN, Tornetta P. Does the fibula need to be fixed in complex pilon fractures? J Orthop Trauma. 2015;29(9):424–427. doi:10.1097/BOT.0000000000000304
54. Brown BD, Steinert JN, Stelzer JW, Yoon RS, Langford JR, Koval KJ. Increased risk for complications following removal of hardware in patients with liver disease, pilon or pelvic fractures: a regression analysis. Injury. 2017;48(12):2705–2708. doi:10.1016/j.injury.2017.09.030
55. Torino D, Mehta S. Fibular fixation in distal tibia fractures: reduction aid or nonunion generator? J Orthop Trauma. 2016;30(Suppl 4):S22–s25. doi:10.1097/BOT.0000000000000695
56. Vallier HA, Cureton BA, Patterson BM. Randomized, prospective comparison of plate versus intramedullary nail fixation for distal tibia shaft fractures. J Orthop Trauma. 2011;25(12):736–741. doi:10.1097/BOT.0b013e318213f709
57. Zelle BA, Bhandari M, Espiritu M, Koval KJ, Zlowodzki M. Treatment of distal tibia fractures without articular involvement: a systematic review of 1125 fractures. J Orthop Trauma. 2006;20(1):76–79.
58. Avilucea FR, Triantafillou K, Whiting PS, Perez EA, Mir HR. Suprapatellar intramedullary nail technique lowers rate of malalignment of distal tibia fractures. J Orthop Trauma. 2016;30(10):557–560. doi:10.1097/BOT.0000000000000631
59. Patterson MJ, Cole JD. Two-staged delayed open reduction and internal fixation of severe pilon fractures. J Orthop Trauma. 1999;13(2):85–91.
60. Busel GA, Watson JT, Israel H. Evaluation of fibular fracture type vs location of tibial fixation of pilon fractures. Foot Ankle Int. 2017;38(6):650–655. doi:10.1177/1071100717695348
61. Heim U. The Pilon Tibial Fracture: Classification, Surgical Techniques, Results. Saunders; 1995.
62. Vidovic D, Matejcic A, Ivica M, Jurisic D, Elabjer E, Bakota B. Minimally-invasive plate osteosynthesis in distal tibial fractures: results and complications. Injury. 2015;46(Suppl 6):S96–S99. doi:10.1016/j.injury.2015.10.067
63. Borrelli J
64. Liporace FA, Yoon RS. An adjunct to percutaneous plate insertion to obtain optimal sagittal plane alignment in the treatment of pilon fractures. J Foot Ankle Surg. 2012;51(2):275–277. doi:10.1053/j.jfas.2011.11.008
65. Marcus MS, Yoon RS, Langford J, et al. Is there a role for intramedullary nails in the treatment of simple pilon fractures? Rationale and preliminary results. Injury. 2013;44(8):1107–1111. doi:10.1016/j.injury.2013.02.014
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.