Back to Journals » Clinical Interventions in Aging » Volume 16
Physical Activity Patterns, Psychosocial Well-Being and Coping Strategies Among Older Persons with Cognitive Frailty of the “WE-RISE” Trial Throughout the COVID-19 Movement Control Order
Authors Murukesu RR, Singh DKA , Shahar S, Subramaniam P
Received 6 November 2020
Accepted for publication 26 January 2021
Published 4 March 2021 Volume 2021:16 Pages 415—429
DOI https://doi.org/10.2147/CIA.S290851
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Prof. Dr. Nandu Goswami
Video abstract of "WE-RISE” trial during the COVID-19 pandemic [ID 290851].
Views: 630
Resshaya Roobini Murukesu,1 Devinder Kaur Ajit Singh,1 Suzana Shahar,2 Ponnusamy Subramaniam3
1Physiotherapy Programme, Centre for Healthy Ageing and Wellness, Faculty of Health Sciences, Universiti Kebangsaan Malaysia, Kuala Lumpur, Malaysia; 2Dietetic Programme and Centre for Healthy Ageing and Wellness, Faculty of Health Sciences, Universiti Kebangsaan Malaysia, Kuala Lumpur, Malaysia; 3Health Psychology Programme and Centre for Healthy Ageing and Wellness, Faculty of Health Sciences, Universiti Kebangsaan Malaysia, Kuala Lumpur, Malaysia
Correspondence: Devinder Kaur Ajit Singh
Centre for Healthy Ageing and Wellness, Faculty of Health Sciences, Universiti Kebangsaan Malaysia, Jalan Raja Muda Abdul Aziz, Kuala Lumpur, 50300, Malaysia
Tel/Fax +603 92897352
Email [email protected]
Purpose: Older persons have been identified as a vulnerable population with respect to the novel coronavirus outbreak, COVID-19. Aiming to “flatten the curve” a strict Movement Control Order (MCO) was implemented in Malaysia. Older adults with cognitive frailty are prone to physical, cognitive and psychosocial decline. This study aims to compare physical activity patterns, psychological wellbeing and coping strategies of older persons with cognitive frailty in the “WE-RISE” trial (intervention versus control) throughout this period.
Materials and Methods: This study was conducted as a sub-analysis of the ongoing “WE-RISE” randomized controlled trial. This study included 42 community-dwelling older adults, aged 60 years and above, with cognitive frailty, stratified into intervention (n=21) and control (n=21) groups who are receiving a multi-domain intervention and usual care, respectively, within the Klang Valley, Malaysia. Phone call interviews were conducted during the MCO period. Physical activity patterns were assessed using International Physical Activity Questionnaire (IPAQ) and Functional Activities Questionnaire (FAQ). Psychological wellbeing was assessed using Flourishing Scale (FS) and General Health Questionnaire (GHQ-12), while the Brief Coping Orientation to Problems Experienced (COPE) assessed coping strategies. Data were analysed descriptively and with independent samples t-test.
Results: The WE-RISE intervention group had significantly higher levels of estimated resting energy expenditure (MET) for “walking activity” (I:μ=1723.1± 780.7;C:μ=537.4± 581.9)(p< 0.001), “moderate activity” (I:μ=1422.8± 1215.1;C:μ=405.7± 746.9)(p=0.002) and “total physical activity” (I: μ=3625.9± 3399.3;C:μ=994.6± 1193.9)(p=0.002). The intervention group was also significantly more independent in functional activities (μ=1.76± 1.73) as compared to the control group (μ=5.57± 8.31) (p< 0.05). Moreover, significant higher self-perception of living a meaningful life and feeling respected (p< 0.05) was demonstrated in regard to psychological well-being in the intervention group. Regarding coping strategies, the intervention group relied significantly on the domains of religion (I:μ=6.43± 0.99;C:μ=6.09± 1.09)(p< 0.05) and planning (I:μ=4.81± 0.75; C:μ=4.04± 1.28)(p< 0.05) whilst the control group relied on humour (C:μ=3.14± 1.19; I:μ=2.38± 0.74)(p< 0.05).
Conclusion: Participants of the WE-RISE intervention group were more physically active, functionally independent and had higher self-perceived social-psychological prosperity regarding living a meaningful life and feeling respected; whilst both groups relied on positive coping strategies during the MCO. These results indicate that it is vital to ensure older persons with cognitive frailty remain physically active and preserve their psychosocial wellbeing to be more resilient in preventing further decline during a crisis such as the COVID-19 pandemic.
Keywords: COVID-19, public health, cognitive frailty, physical activity, psychological well-being, geriatric health introduction
The highly infectious, novel coronavirus disease (COVID-19) was declared a global pandemic by the World Health Organization (WHO) in March 2020 as a result of its rapid spread across the globe, including Malaysia.1 Described as a respiratory illness emulating viral pneumonia, the transmission of the COVID-19 virus occurs through the transfer of respiratory droplets among infected individuals or contact with contaminated objects and surfaces. The most common symptoms of infection include fever, dry cough and fatigue.1,2
Following the vast spread of the disease, COVID-19 was labelled a “public health emergency of international concern”; forcing affected countries into a nationwide “lock down” to limit and prevent the spread of the disease.3,4 Malaysia implemented a strict Movement Control Order (MCO) from the 18th of March to the 3rd of May 2020 aimed to “break the chain of infection” which enforced all citizens to remain at home with the exception of obtaining essentials.5 Individuals who did not adhere to the MCO regulations were held accountable under the Malaysian Laws of Prevention and Control of Infectious Diseases Act 1988.6 The MCO was followed by a Conditional Movement Control Oder (CMCO). Malaysia was in the Recovery Movement Control Oder (RMCO) phase which begun in August 2020 and was expected to last till the 31st of December 2020.7 Unfortunately, as of October 2020, Malaysia has entered the third wave of the COVID-19 pandemic, causing “red zone” areas (including the Klang Valley) to revert to the CMCO ruling.7
The general population is vulnerable to the COVID-19.8 However, evidence has established that older persons who are immunocompromised, with pre-existing diseases (diabetes, hypertension, cardiovascular disease and cerebrovascular disease) are more predisposed to infection.1,9 The vulnerability of older persons leads to critical illnesses, admission to intensive care unit (ICU) and higher mortality rates.8 In Europe, 95% of fatalities due to COVID-19 were among those aged 60 years and above and is causing ‘hidden deaths’ across the continent.10 The majority of the deceased had at least one underlying chronic condition.10 However, in the United States, 8 out of 10 deaths due to COVID-19 infections have been in older persons aged 65 years and above.11 In the Malaysian context, the Ministry of Health’s mortality review established that the age-group with the highest COVID-19 deaths is between 61 and 70 years (32.2%) followed secondly by the 71 to 80 age-group (19.2%); hence, older persons aged 60 years and older are a “high-risk group”.12
Older persons are known to be typically less active than the younger population and are more at risk of poor health outcomes.13 The routine activities of daily living of older persons have been abruptly halted due to the requirement of “physical distancing” and staying at home throughout the MCO period. Given the vulnerability of the older population to COVID-19, it is highly likely that they will have to continue adhering to these strict precautionary protocols and restrictions until a vaccine is authorized for distribution.3 As a consequence of physical isolation, older persons may be subjected to sedentary behavior due to a decline in physical activity.13 The MCO has led to restrain and the inability to carry out regular daily tasks such as outdoor daily chores, halted participation in community activities and social gatherings, as well as engagement in formal exercises such as community-based group exercises, daily walks, usual exercise regimes and more. Physical and social isolations have also highly compromised the mental wellbeing of older adults.14
Malaysia is en route to attaining the status of an aged nation by the year 2030 as older persons increase in population as well as life expectancy, resulting in increased susceptibility to morbidity and disability.15,16 Cognitive frailty is a geriatric syndrome characterized by the simultaneous presence of cognitive impairment and physical frailty without the presence of dementia.17 Physical frailty is a multi-faceted, age-related syndrome caused by multiple physiological dysfunctions and is characterized by weakness, slowness, shrinking, exhaustion and diminished physical function.18 Cognitive impairment is a noticeable and measurable deterioration of cognitive function.19 Risk factors of cognitive impairment include polypharmacy, chronic illness (hypertension, diabetes mellitus, heart disease, brain disease), metabolic disorders, depression, infections and smoking.20 The presence of cognitive impairment within older persons with frailty has been found to occur without the presence of evident brain disease.20 Physical frailty is a predictor of cognitive impairment and vice-versa, hence its coalition as cognitive frailty.20
Physical frailty was found to be highly prevalent at 56.6% among Malaysian older persons residing in institutions and has been strongly associated with cognitive decline.21 Within the community-dwelling population, cognitive frailty has been reported to be prevalent at 2.2%.22 Among the significant predictors of this potentially debilitating condition are depression, decline in functional mobility, physical frailty and increasing age.23 It has been suggested that both constructs are potentially reversible should it be detected at the early stages of development such as pre-frailty or mild cognitive impairment.17,20 In an effort to specifically address the clinical manifestations of cognitive frailty and potential reversibility, a multi-domain intervention (The WE-RISE intervention) was conducted prior to the pandemic in senior citizen activity centers among community-dwelling older persons with this condition.24
Physical inactivity and poor mental health have been labelled as ‘adverse effects’ of physical and social isolation measures in combatting the spread of COVID-19.13,25 Frailty has been identified as a predictor of poor prognosis amongst older persons with COVID-19.26 “Inflammaging” is the concept referring to the dysregulation of inflammatory mediators within the ageing body resulting in a persistent low-intensity inflammation which is often the cause for age-related disorders, including frailty.10 This leads to the inability to fight against infections such as COVID-19 due to the pro-inflammatory state, resulting in the risk of severe disease complications.26 A decline in physical function may lead to further severity of frailty status. Where cognitive function and psychosocial impact are a concern, the pandemic has been associated with the worsening of neuropsychiatric symptoms, sleep disorders, high levels of anxiety and lower self-perceived psychological wellbeing attributed to the drastic change in lifestyle and fear of infection itself among older persons with or without cognitive impairment.27 The lack or absence of social contact, social support and inadequate social network has been postulated to accelerate neurological ageing and increase the risk of dementia development among older persons.14
Older persons with cognitive frailty are already prone to functional disability and decline in cognitive function.17 Hence, there is a possibility that the strictly imposed “stay at home” restrictions may have had an impact upon their physical and psychosocial wellbeing. There is inadequate evidence highlighting the effect of isolation specifically among the population with cognitive frailty. The aim of this current study was to compare physical activity patterns, psychosocial wellbeing and coping strategies among older persons with cognitive frailty in the ongoing WE-RISE trial (intervention versus control) throughout the MCO due to the COVID-19 outbreak.
Materials and Methods
This cross-sectional study is a sub-analysis conducted among Malaysian older persons with cognitive frailty, aged 60 years and above who are participants in an ongoing randomized controlled trial, the “WE-RISE Trial”. Participants of this 6-month trial consisted of two matched community-dwelling older persons groups whereby the Intervention group received the WE-RISE intervention encompassing multi-component exercise regimen, cognitive stimulation, dietary counselling and psychosocial support; whereas the Control group continued active usual care from their respective activity centers.
The operational definition of cognitive frailty in the WE-RISE trial is as defined by the International Consensus Group at the International Academy on Nutrition and Aging (I.A.N.A) and the International Association of Gerontology and Geriatrics (I.A.G.G).17 It is understood as the co-existence of physical frailty based on that developed in the Cardiovascular Health Study and mild cognitive impairment (MCI) defined as objective evidence in one or more cognitive domains and preserved independence in functional abilities (Clinical Dementia Rating Scale (CDR) score of 0.5).17 The classification of the cognitive frailty groups in the WE-RISE Trial is as outlined in Table 1 .17 Figure 1 summarizes the trial flow and further detailed information on the WE-RISE trial has been described in the protocol paper.24
 |
Table 1 Operational Definition and Classification of Cognitive Frailty Groups. |
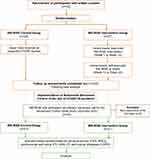 |
Figure 1 Study trial flow diagram. |
Study Population
The participants of the WE-RISE trial are registered members of the Activity Centers for Older Persons; known locally as “Pusat Aktiviti Warga Emas” (PAWE) within the Klang Valley.28 The participants were contacted via a phone call between April to May 2020, during the MCO period and the duration of the interview was between 45 and 60 minutes long. Verbal consent was obtained for voluntary participation in this study with the assurance of anonymity.
Sociodemographic Data, Clinical Characteristics and Self-Rated Satisfaction of Life
Sociodemographic data obtained included gender, age, ethnicity, education level, marital status, status of employment, average household income and smoking history. Medical history included history of falls, surgery and hypercholesterolemia as well as a robust list of co-morbidities adapted from the Self-Administered Comorbidity Questionnaire (SCQ).29 Comorbidity was determined with the simultaneous presence of two or more chronic diseases.30 Depression was evaluated using the validated Malay version of the Geriatric Depression Scale (M-GDS–14) with a cut-off point of 5/6 to indicate clinically significant depression.31 Satisfaction with current life and access to health services during the MCO was self-reported based binary responses (yes/no) to the questions “Are you satisfied with your current state of living?” and “Are currently obtaining the health services that you require?”.
Physical Activity Pattern
The Functional Activities Questionnaire (FAQ) evaluates the level of independence of older persons when carrying out activities of daily living. The 10-items screened for are ability to handle finances, taxes and important documents, shopping for essentials, playing games or hobbies, making a hot drink, preparing a meal, awareness of current events, attention to media (television, books, magazine), remembering vital dates or events and travelling. Scoring of the questionnaire ranges from 0 to 30 with a cut-off point at 9 (dependency in at least three activities); implying the possibility of impaired functioning.32
International Physical Activity Questionnaire (IPAQ) short form was used as a surveillance of physical activity levels within a population. The quantification of physical activity uses the metabolic equivalent of task (MET) values as follows: walking = 3.3 METs, moderate activity = 4.0 METs and vigorous activity = 8.0 METs. Final scores are calculated in MET-minutes per week (MET-min week −1) using the formula: minutes of activity/day × days/week × MET value for each activity category. Total MET-min week −1 is a sum of all three categories. The activity of “sitting” in the IPAQ is used as a measure of time spent doing sedentary activities per week and is not included as a part of the physical activity scores. The “sitting” component is reported in median values and interquartile ranges as outlined in the IPAQ guideline.33,34
Psychological Wellbeing and Coping Strategies
The Brief-Coping Orientation to Problems Experienced (COPE) scale assessed coping strategies of older persons in this study resorted to during the MCO. The scale comprises 28 items, with a 4-point Likert scale ranging from “I haven’t been doing this at all” to “I have been doing this a lot”. The 14 domains of coping strategies are active coping, use of emotional support, use of instrumental support, positive reframing, planning, acceptance, self-distraction, denial, substance abuse, behavioral disengagement, venting, self-blame, humor and religion. There is no overall total score, only total scores for each of the 14 domains which range between 2 and 8 points. Higher scores indicate a higher dependency on the particular domain as a coping mechanism.35,36
The Flourishing Scale (FS) is an assessment of “social-psychological prosperity” in terms of subjective well-being. The 8-item questionnaire consists of recognized psychological needs for human functioning, namely, purposefulness, social relationships, competence, optimism, self-respect, self-acceptance, contributing to others’ wellbeing and engagement in activities. Each item is scored between 1 (strongly disagree) to 7 (strongly agree), and total score ranges between 8 and 56. Higher scores indicate that the respondent perceives themselves to be on the more positive spectrum and have healthier psychological well-being.37
The General Health Questionnaire (GHQ-12) is a measure of overall psychological distress. The 12-items items include psychological factors such as sleep disturbance, stress, inability to overcome problems and feeling happy or depressed. Each item assesses the level of psychological well-being ever since the commencement of MCO using a 4-point scale ranging from “more than usual” to “much less than usual”. For the purpose of this study the scoring method selected was 0-0-1-1 instead of the Likert scale scoring of 0-1-2-3; aimed at eliminating bias. Total score ranges from 0 to 12, whereby higher scores indicate higher levels of psychological distress.38
Statistical Analysis
Sociodemographic data and clinical characteristics of the participants were descriptively analyzed, stratified by the intervention and control groups. Physical activity patterns, psychological wellbeing and coping strategies were analyzed using independent samples t-test with the participant groups (intervention/control) as the dependent variable. Significance level was set at p<0.05 and data were analyzed using the Statistical Package for Social Sciences (SPSS) software, version 23.0.
Results
A total of 42 participants (Intervention=21; Control=21) were successfully contacted and agreed to participate in the present study, summing the response rate at 76.4%. The participants in this study were not infected with the COVID-19 virus upon interview and were in strict adherence to the imposed MCO. The sociodemographic and clinical characteristics of the participants are as outlined in Table 2. Participants were mostly females (88.1%) with a mean age of 69.3±6.0 years. Ethnically, participants comprised Malay (69.0%), Chinese (9.5%) and Indian (21.4%) which are the predominant ethnicities in Malaysia. Mean body mass index (BMI) of the participants is 27.3±4.6 kg/m2 which is within the “normal” range for older persons.39 In terms of clinical characteristics, the three most prevalent chronic diseases among the participants were hypertension (66.7%), hypercholesterolemia (69.0%) and diabetes mellitus (47.6%). Interestingly, 9.5% of the participants, all of whom were from the control group reported to experiencing back pain during the MCO (p<0.05). Participants were generally satisfied with their current lives and had no unmet health needs throughout this period.
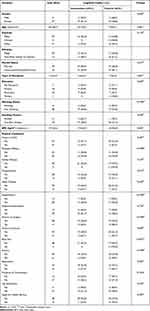 |
Table 2 Sociodemographic, Clinical Characteristics, Life Satisfaction and Need for Health Needs of the WE-RISE Participants During the MCO |
The IPAQ scores of the participants are outlined in Table 3. During the MCO, participants in the intervention group scored significantly higher MET-min per week for the “walking” category as they walked at home, around the neighborhood or to obtain essentials as recreation, exercise or leisure (p<0.001). Likewise, the intervention group also participated more in “moderate” activities which encompass cycling, carrying light weights, gardening or exercises requiring moderate physical effort (p<0.05). Participants in the control group were found to spend longer minutes per week engaging in passive activities in sitting or lying down positions. The total IPAQ scores imply that the control group was more sedentary during the MCO as they had lower MET-min per week as compared to the intervention group (p<0.05). The independence levels of the participants during the MCO are as described in Table 4. In terms of the specific activities, the control group required assistance or were dependent on carrying out skilled tasks, making a hot beverage, preparing meals, keeping updated with current events, paying attention and remembering important information (p<0.05) as compared to the intervention group. This is reflected in the total FAQ scores which are significantly higher in the control group than the intervention group (p<0.05).
 |
Table 3 IPAQ Scores of the WE-RISE Participants During the MCO |
 |
Table 4 FAQ Scores of the WE-RISE Participants During the MCO |
Overall scores of the FS indicate that both groups experienced similar levels of social-psychological prosperity throughout the MCO (Table 5). However, when each item of the scale was individually analyzed, the intervention group had significantly higher scores in terms of purposefulness and feeling respected (P<0.05) as compared to the control group. The GHQ-12 scores of the participants in this study imply that both groups did not experience concerning levels of psychological distress during the MCO period (Table 6). When stratified by items of the GHQ-12, the psychological distress that the participants experienced most was loss of sleep and the least was feeling worthless. Coping strategies employed by the participants during the MCO period are as described in Table 7. Both groups relied the most on the domain of “religion” as a coping strategy though it was significantly higher among the intervention group (p<0.05). Likewise, the intervention group relied significantly more on the domain of “planning” (p<0.05). Contrastingly, the control group sought the “humor” domain as a coping mechanism more significantly than the intervention group (p<0.05).
 |
Table 5 Social-Psychological Prosperity Scores of the WE-RISE Participants During the MCO |
 |
Table 6 Psychological Distress Experienced by the WE-RISE Participants During the MCO |
 |
Table 7 Coping Strategies Sought by the WE-RISE Participants During the MCO Based on the Brief COPE Scale |
Discussion
This study describes the physical activity patterns, psychosocial well-being status and coping strategies of older persons with cognitive frailty of the ongoing WE-RISE trial during the government imposed MCO period (March to May 2020) in Malaysia due to the COVID-19 pandemic. The drastic but necessary precautionary effort was noted to be effective in “breaking the chain of infection”.5 Nonetheless, this extended period of quarantine has challenged the resilience of the ageing population in terms of economic well-being, social exclusion, mental health, physical inactivity and vulnerability to adverse health outcomes.40,41
Sociodemographically, there is no disparity between the intervention and control groups as the samples were pair-matched prior to the commencement of the WE-RISE trial. Clinically there were no changes in the presence of chronic illnesses from the time of baseline screening, but older persons from the control group (9.5%) reported experiencing “back pain” at the time of the phone call interviews which they previously had not been diagnosed with prior to the MCO. The home quarantine restrictions have been reported to increase the likelihood of older persons engaging in prolonged periods of sedentary behavior.13,42 Sedentary behavior during the MCO may explain the sudden onset of back pain as it has been significantly associated with multiple detrimental health outcomes which include chronic back pain among older persons.43
The importance of physical activity and its role in extending functional independence, preserving cognitive reserves and promoting quality of life within the ageing population are well established.44 Physical activity guidelines for older persons which encompass endurance, resistance, flexibility and balance exercises have been outlined.45 Nevertheless, older persons still remain the least physically active population as they have not been meeting these recommendations, even during ‘pre-COVID-19ʹ times.3,44,46 A further exacerbated reduction in physical activity and increase in dormancy among older persons can be inferred, given the strict “Stay at Home” ruling imposed by the government. A cross-sectional study by Yamada et al (2020) studying the effects of the COVID-19 pandemic on community-dwelling older persons reported a significant decrease in time spent engaging in physical activity among those who were frail.47 In the present study, this phenomenon can be observed amongst the participants of the control group who spent more time (expressed in MET-min week−1) partaking in sedentary activities (in sitting, reclined or lying postures) as compared to engaging in light (walking) or moderate physical activities. Physical exercise is a vital component of cognitive frailty management.17 Continuous disengagement from physical activity may result in further degradation in functionality and disability in time.47
The results of this study have shown that older persons who are engaging in the WE-RISE intervention were more physically active during the MCO period. The WE-RISE intervention includes a guided 3-month home program (WE-RISE at Home) which may have enabled the participants to carry out multi-component exercise training safely and effectively on their own.24 It can be hypothesized that given their exposure to the intervention and awareness of the importance of maintaining an active lifestyle, these participants may have been more motivated to execute some form of physical activity in the comforts of their own homes during the MCO. Regarding the functional independence of the participants in our study, both groups have considerably adequate levels of functional independence. The total scores of the FAQ were way below the cut-off value (>9); implying that they may not be completely dependent but require some assistance in carrying out certain functional tasks. However, the control group required more assistance than the intervention group for tasks that involved executive function, attention and memory which could be attributed to their pre-existing deficits in cognitive functioning.48
Physical inactivity could consequently lead to a compromise in immunity among older persons hence increasing exposure to infection by way of exacerbating existing age-related pathologies.49 The severity of COVID-19 infection is not just caused by the virus itself but also heavily relies on the immune response of the host.49 Lower physical activity levels are associated with immunosenescence; understood as a decline in the immune system parallel to increasing age. This in turn results in a risk of chronic diseases, frailty, mortality, reduced efficacy in response to vaccine and decline in cognitive function.49 This could imply that engaging in regular exercise and physical activity could suppress or delay the risks and age-related adverse outcomes with a stronger immune system.
The COVID-19 vaccine is on the cusp of dissemination around the world. Seeing as the ageing population with frailty has been the most heavily impacted by the pandemic, it can be assumed that older persons would most likely be prioritized for vaccination.50 The developed COVID-19 vaccines are new and its efficacy amongst the older population has yet to be determined. Older persons with frailty and those with comorbidities have been excluded in the majority of the vaccine study trials, despite being the most vulnerable to infection.50 Taking immunosenescence into consideration, theoretically the vaccines may be less effective in older persons as a result of inadequate antibody levels.50 With the uncertainty of how the immune system may response to the vaccine, there is a possibility of increasing overall risk to adverse outcomes especially among the already predisposed older persons with frailty.50 Therefore, preventing physical inactivity and boosting the body’s immunity via engagement in regular exercise and functional activities could possibly mitigate these potential adverse outcomes.
In relation to psychosocial well-being, both groups expressed relatively favorable overall levels of self-perceived success. Contrastingly when analyzed by each domain of the scale, intervention group participants seem to have a higher sense of self-worth in the sense that they reported leading a purposeful and meaningful life and that they are respected by other people. The WE-RISE intervention incorporated the element of psychosocial support as evidence has advocated its incorporation for the promotion of adherence to physical activity and stimulation of cognitive function.24,51 A two-way relationship has been established whereby older persons with higher levels of psychological well-being have been associated with higher physical activity levels.41 Likewise, active engagement in physical activity resulted in the improvement of mental and emotional well-being among older persons;52 corroborating with the findings in this present study.
Coping is understood as a self-protective mechanism that is used to help in the management of potential psychological stress when experiencing a stressful circumstance.53 In this study, “religion”, “acceptance” and “positive reframing” were the top three coping strategies recruited which fall under “approach coping”, while “self-blame”, “denial” and “substance abused” which fall under “avoidant coping” were the least popular choices. When compared between both groups, older persons from the intervention group relied more on the coping strategy of “planning” (approach coping) than their control group counterparts. Approach coping strategies are a more valuable method of responding to adverse circumstances. It reflects the ability to adapt and react to situations with better emotional composure and taking control of the situation appropriately.53 Whereas resorting to avoidance coping strategies may result in emotional numbness, disruptive behaviors and non-productive outcomes.53
Heavy reliance and belief in the religion of the participants is in congruence with existing evidence that asserts religion as a vital coping strategy among older persons.54 Among the ageing population, religion and spirituality have been strongly associated with positive psychological well-being as it provides support, sense of belonging, purpose in life and aids in ameliorating distress; especially in the face of adversity.54 Humor was significantly more tapped into by the control group during the MCO. From a psychological standpoint, humor and laughter are significantly helpful coping mechanisms that bring about positive mental outcomes and when dealing with unexpected calamities, such as a global pandemic.55 With these findings, it can be deduced that the participants in this study (both control and intervention groups) pursued positive coping strategies to get by the challenging MCO circumstances.
The mental and psychological vulnerability faced by older persons worldwide during the pandemic can be considered “social frailty”. Social frailty is an understudied frailty phenotype that requires more understanding as its relevance is unquestionable in the times of social isolation brought forth by the pandemic.56 Older persons without dementia were found to experience high stress levels, anxiety, depression and peri-traumatic stress during COVID-19 related isolation. Whereas older adults with mild cognitive impairment and dementia faced agitation, apathy, depression, irritability, restlessness and sleep difficulty, which improved with social engagement (such as video calls with family members).14 The participants in the present study did not experience symptoms associated with the COVID-19 virus and were not diagnosed with the disease during the period of data collection. However, existing literature has reported that older persons express symptoms of delirium and agitation upon acute infection of the COVID-19 virus.14 The direct and indirect effects of the COVID-19 infection upon brain function and psychiatric well-being require further research. If the infection triggers damage to neural tissue, it could result in cognitive decline and psychological dysfunction and will require early attention to halt or delay its progression.14
It has been suggested that with the continuation of quarantine and physical isolation, the general older population are predisposed to mental health disturbances, functional disability and frailty.57 The already predisposed older population with cognitive frailty is at greater risk of further physical and cognitive functional decline as well as an overwhelming psychological burden. Malaysians have expressed positive attitudes towards battling COVID-19 and recognize the importance of quarantine and adhering to the standard operating procedures in order to “flatten the curve”.58 Nevertheless, a symbiosis between ‘pre-COVID-19ʹ and current times must be met. The WHO has encouraged maintaining social activities virtually and engage in regular physical activity at home as alternatives to maintaining regular daily activities during this pandemic.59
To our knowledge, there is yet to be a study describing the physical activity patterns and psychosocial well-being of older persons with cognitive frailty during the nationwide MCO brought forth by the COVID-19 crisis. Observing these physical and psychosocial domains provides insight into their overall well-being during the pandemic. Addressing the limitations of this study, data analyzed for this present study were self-reported and there is a possibility of the participants providing responses that they perceive to be socially desirable. In addition, an analysis of the variables stratified by gender was not executed due to the imbalance of male and female participants in this study. There is evidence supporting that men are less forthcoming when participating in health promotion programs, as experienced in the WE-RISE trial participant recruitment.60 However, all samples were pair-matched during randomization and there were no significant differences between the groups despite the small number of male participants. The sample size of this study is relatively small and employs a univariate analysis; however, these findings can be used as a platform for larger and more explorative future research undertakings. In addition, the WE-RISE intervention was developed with the aim of reversing cognitive frailty. The difference in physical activity patterns could potentially indicate that some reversal or improvement of frailty symptoms have taken place in this ongoing trial as the results of the trial have yet to be analyzed. There is a need for larger studies investigating the effects of other existing potential factors such as genetic and nutritional variables on cognitive status and physical activity patterns (independently or interactively) among older adults with cognitive frailty. As a recommendation, home-based intervention packages that address the components of physical, psychosocial and mental well-being among older persons should be disseminated. In the light of this global crisis, it is important to create awareness that physical and social isolation is not a deterrent to maintaining normalcy in terms of physical and psychological well-being.
Considering the existing association between frailty, cognitive impairment, immunosenescence and susceptibility to infection and other inflammatory diseases, it can be assumed that older persons with cognitive frailty are at higher risk of COVID-19 infection with higher severity, poorer prognosis and are less likely to respond to vaccination.10 This study hopes to highlight the importance of targeted research and treatment development with respect to the older persons with frailty and comorbidities as they are the population that requires it the most. Frailty screenings are important amongst the older population because chronological ageing does not necessarily equate to the physiological differences brought upon by biological ageing.26 The potential reversal of cognitive frailty in its early stages (pre-frailty and mild cognitive impairment) emphasizes the importance of early assessment as it may improve prognosis with prompt management.20,26 Further understanding of COVID-19 and its impact upon the multi-facets of frailty and cognitive impairment is required for strategic and efficient management by public health sectors. Age-specific, client-tailored management of COVID-19 may prevent infection, hospitalization due to complications and reduce fatalities. Preservation of physical and cognitive function, delaying the age-related degradation of both constructs and the potential reversibility of cognitive frailty among older persons is vital and may improve the efficacy of immunization and provide long-lasting protection from the COVID-19 virus.
Conclusion
To conclude, our study observed that older persons with cognitive frailty from the intervention group who were engaged in the WE-RISE community-based multi-domain intervention were more physically active, functionally independent and had higher self-perceived social-psychological prosperity regarding living a meaningful life and feeling respected; while both control and intervention groups sought positive coping strategies during the MCO. Ensuring that older persons remain physically active with the preservation of psycho-social well-being is fundamental during these unprecedented times to promote resilience, prolong functional independence, prevent further deterioration of physical and cognitive reserves and to be prepared for immunization.
Ethics
The studies involving human participants were reviewed and approved by the Research Ethics Committee of Universiti Kebangsaan Malaysia (UKM PPI/111/8/JEP-2018-558) and the Department of Social Welfare Malaysia (MyResearch Reference: JKMM 100/12/5/2: 2018/405). The authors affirmed that informed consent was obtained from the participants involved with assurance of anonymity. This study was conducted in accordance with the Declaration of Helsinki.
Acknowledgments
We would like to extend our gratitude and appreciation to the WE-RISE participants who participated in this study during this trying period for not only the nation but also the world. We thank the Department of Social Welfare Malaysia and “Pusat Aktiviti Warga Emas” (PAWE) for their continuous support. We would also like to thank Prof Dr Michael Fenech, Distinguished Professor, Faculty of Health Sciences, UKM, for reviewing and proofreading this manuscript.
Funding
This study is funded by Universiti Kebangsaan Malaysia (DCP-2017-002/1; DCP-2017-002/2) and Long-term Research Grant Scheme (LRGS) provided by the Ministry of Education Malaysia (LRGS/BU/2012/UKM-UKM/K/01).
Disclosure
The authors report no conflicts of interest in this work.
References
1. Cucinotta D, Vanelli M. WHO declares COVID-19 a pandemic. Acta Biomed. 2020;91(1):157–160. doi:10.23750/abm.v91i1.9397
2. Shah AUM, Safri SNA, Thevadas R, et al. COVID-19 outbreak in Malaysia: actions taken by the Malaysian government. Int J Infect Dis. 2020;97:108–116. doi:10.1016/j.ijid.2020.05.093
3. Said CM, Batchelor F, Duque G. Physical activity and exercise for older people during and after the coronavirus disease 2019 pandemic: a path to recovery. J Am Med Dir Assoc. 2020;21(7):977–979. doi:10.1016/j.jamda.2020.06.001
4. World Health Organization. Public health emergency of international concern (PHEIC). 2020. Available from: https://www.who.int/blueprint/priority-diseases/key-action/Global_Research_Forum_FINAL_VERSION_for_web_14_feb_2020.pdf.
5. Prime Minister’s Office of Malaysia. Perutusan Khas COVID-19 (18Mac 2020) – stay at home. 2020. Available from: https://www.pmo.gov.my/2020/03/perutusan-khas-covid-19-18-mac-2020/.
6. Ministry of Health Malaysia. . COVID-19: Akta pencegahan dan pengawalan penyakit berjangkit 1988. 2020. Available from: http://covid-19.moh.gov.my/faqsop/akta-342.
7. National Security Council. COVID-19: movement control order. 2020. Available from: https://www.mkn.gov.my/web/ms/covid-19/.
8. Liu K, Chen Y, Lin R, Han K. Clinical features of COVID-19 in elderly patients: a comparison with young and middle-aged patients. J Infect. 2020;80:e14–e18. doi:10.1016/j.jinf.2020.03.005
9. Huang C, Wang Y, Li X, et al. Clinical features of patients infected with 2019 novel coronavirus in Wuhan, China. Lancet. 2020;395(10223):497–506. doi:10.1016/S0140-6736(20)30183-5
10. Palermo S. Covid-19 pandemic: maximizing future vaccination treatments considering aging and frailty. Front Med. 2020;7:1–11. doi:10.3389/fmed.2020.558835
11. Centers for Disease Control and Prevention. Coronavirus disease: older adults. 2020. Available from: https://www.cdc.gov/coronavirus/2019-ncov/need-extra-precautions/older-adults.html.
12. Ministry of Health Malaysia. Press statement: updates on the coronavirus disease 2019 (COVID-19) situation in Malaysia. 2020. Available from: http://covid-19.moh.gov.my/terkini/052020/situasi-terkini-03-mei-2020/103%20Kenyataan%20Akhbar%20KPK%20COVID-19%20(3%20Mei%202020)%20-%20EN.pdf.
13. Roschel H, Artioli GG, Gualano B. Risk of increased physical inactivity during COVID-19 outbreak in older people: a call for actions. J Am Geriatr Soc. 2020;68(6):1126–1128. doi:10.1111/jgs.16550
14. Manca R, De Marco M, Venneri A. The impact of COVID-19 infection and enforced prolonged social isolation on neuropsychiatric symptoms in older adults with and without dementia: a review. Front Psychiatry. 2020;11. doi:10.3389/fpsyt.2020.585540
15. Masud J, Tengku Aizan H, Sharifah AH. Measuring poverty among elderly Malaysians. AJPS. 2015;1(1):73–81.
16. Crimmins EM. Lifespan and healthspan: past, present, and promise. Gerontologist. 2015;55(6):901–911. doi:10.1093/geront/gnv130
17. Kelaiditi E, Cesari M, Canevelli M, et al. Cognitive frailty: rational and definition from an (I.A.N.A./I.A.G.G.) international consensus group. Astrophys J. 2012;756(1):59.
18. Fried LP, Tangen CM, Walston J, et al. Frailty in older adults: evidence for a phenotype. J Gerontol Ser a Biol Sci Med Sci. 2001;56(3):M146–M157. doi:10.1093/gerona/56.3.M146
19. Petersen RC, Caracciolo B, Brayne C, Gauthier S, Jelic V, Fratiglioni L. Mild cognitive impairment: a concept in evolution. J Intern Med. 2014;275(3):214–228. doi:10.1111/joim.12190
20. Morley JE, Morris JC, Berg-weger M, et al. Brain health: the importance of recognizing cognitive impairment. J Am Med Dir Assoc. 2016;16(9):731–739. doi:10.1016/j.jamda.2015.06.017
21. Murukesu M, Singh S, Subramaniam S, et al. Prevalence of frailty and its association with cognitive status and functional fitness among ambulating older adults residing in institutions within west coast of Peninsular Malaysia. Int J Environ Res Public Health. 2019;16(23):1–13. doi:10.3390/ijerph16234716
22. Rivan NFM, Shahar S, Rajab NF, et al. Cognitive frailty among Malaysian older adults: baseline findings from the LRGS TUA cohort study. Clin Interv Aging. 2019;14:1343–1352. doi:10.2147/CIA.S211027
23. Rivan NFM, Shahar S, Rajab NF, et al. Incidence and predictors of cognitive frailty among older adults: a community-based longitudinal study. Int J Environ Res Public Health. 2020;17(5):1–17. doi:10.3390/ijerph17051547
24. Murukesu RR, Kaur D, Singh A, Shahar S. A multi-domain intervention protocol for the potential reversal of cognitive frailty: “WE-RISE” randomized controlled trial. Front Public Heal. 2020;8(471):1–11.
25. Mukhtar S. Psychological impact of COVID-19 on older adults. Curr Med Res Pract. 2020;10:201–202.
26. Ma Y, Hou L, Yang X, et al. The association between frailty and severe disease among COVID-19 patients aged over 60 years in China: a prospective cohort study. BMC Med. 2020;18(1):1–8. doi:10.1186/s12916-020-01761-0
27. Forte G, Favieri F, Tambelli R, Casagrande M. The enemy which sealed the world: effects of COVID-19 diffusion on the psychological state of the Italian population. J Clin Med. 2020;9(6):1802. doi:10.3390/jcm9061802
28. Department of Social Welfare. Activity center for older person. 2016. Available from: http://www.jkm.gov.my/jkm/index.php?r=portal/left&id=aC90Vy81SVhKTEZDcVoxRE5JRzNRZz09.
29. Sangha O, Stucki G, Liang MH, Fossel AH, Katz JN. The self-administered comorbidity questionnaire: a new method to assess comorbidity for clinical and health services research. Arthritis Rheum. 2003;49(2):156–163. doi:10.1002/art.10993
30. Valderas JM, Starfi B, Sibbald B, Salisbury C, Roland M. Defining comorbidity: implications for understanding health and health services. Ann Fam Med. 2009;7(4):357–363. doi:10.1370/afm.983
31. Teh EE, Ismail HC. Validation of Malay version of geriatric depression scale among elderly inpatients. Priory. 2005.
32. Pfeffer RI, Kurosaki TT, Harrah CH, Chance JM, Filos S. Measurement of functional activities in older adults in the community. J Gerontol. 1982;37(3):323–329.
33. International Physical Activity Questionnaire (IPAQ). IPAQ scoring protocol: guidelines for data processing and analysis of the international physical activity questionnaire (IPAQ) – short and long forms. 2005. Available from: http://www.ipaq.ki.se/scoring.pdf.
34. Chu AHY, Moy FM. Reliability and validity of the Malay international physical activity questionnaire (IPAQ-M) among a Malay population in Malaysia. Asia-Pacific J Public Heal. 2015;27(2):1–9.
35. Carver CS. You want to measure coping but your protocol’s too long: consider the brief COPE. Int J Behav Med. 1997;4(1):92–100. doi:10.1207/s15327558ijbm0401_6
36. Yusoff N, Low WY, Yip CH. Reliability and validity of the Malay version of Brief COPE Scale: a study on Malaysian women treated with adjuvant chemotherapy for breast cancer. MJP. 2009;18(1).
37. Diener E, Wirtz D, Tov W, et al. New well-being measures: short scales to assess flourishing and positive and negative feelings. Soc Indic Res. 2010;97(2):143–156. doi:10.1007/s11205-009-9493-y
38. Zulkefly NS, Baharudin R. Using the 12-item general health questionnaire (GHQ-12) to assess the psychological health of Malaysian college students. Glob J Health Sci. 2010;2(1):73–80. doi:10.5539/gjhs.v2n1p73
39. Winter JE, MacInnis RJ, Wattanapenpaiboon N, Nowson CA. BMI and all-cause mortality in older adults: a meta-analysis. Am J Clin Nutr. 2014;99(4):875–890. doi:10.3945/ajcn.113.068122
40. United Nations. Policy brief: the impact of COVID-19 on older persons. 2020. Available from: https://unsdg.un.org/sites/default/files/2020-05/Policy-Brief-The-Impact-of-COVID-19-on-Older-Persons.pdf.
41. Goethals L, Barth N, Guyot J, et al. Impact of home quarantine on physical activity among older adults living at home during the COVID-19 pandemic: qualitative interview study. J Med Internet Res. 2020;22(5):1–5.
42. Ricci F, Izzicupo P, Moscucci F, et al. Recommendations for physical inactivity and sedentary behavior during the coronavirus disease (COVID-19) pandemic. Front Public Heal. 2020;8(471):8–11.
43. Vancampfort D, Stubbs B, Koyanagi A. Physical chronic conditions, multimorbidity and sedentary behavior amongst middle-aged and older adults in six low- and middle-income countries. Int J Behav Nutr Phys Act. 2017;14(1):1–13. doi:10.1186/s12966-016-0456-9
44. Sun F, Norman IJ, While AE. Physical activity in older people- a systematic review. BMC Public Health. 2013;13(449):1–17. doi:10.1186/1471-2458-13-449
45. Chodzko-Zajko WJ, Proctor DN, Fiatarone Singh MA, et al. American college of sports medicine position stand. Exercise and physical activity for older adults. Med Sci Sports Exerc. 2009;41(7):1510–1530. doi:10.1249/MSS.0b013e3181a0c95c
46. Singh DKA, Rahman NNAA, Rajaratnam BS, Yi TC, Shahar S. Validity and reliability of physical activity scale for elderly in Malay language (PASE-M). Malaysian J Public Heal Med. 2018;1:116–123.
47. Yamada M, Kimura Y, Ishiyama D, et al. Effect of the COVID-19 epidemic on physical activity in community-dwelling older adults in Japan: a cross-sectional online survey. J Nutr Heal Aging. 2020;2020:1–3.
48. Sachdev PS, Blacker D, Blazer DG, et al. Classifying neurocognitive disorders: the DSM-5 approach. Nat Rev Neurol. 2014;10(11):634–642. doi:10.1038/nrneurol.2014.181
49. Damiot A, Pinto AJ, Turner JE, Gualano B. Immunological implications of physical inactivity among older adults during the COVID-19 pandemic. Gerontology. 2020;66(5):431–438. doi:10.1159/000509216
50. Soiza RL, Scicluna C, Thomson EC. Efficacy and safety of COVID-19 vaccines in older people. Age Ageing. 2020;1–5.
51. Frost R, Belk C, Jovicic A, et al. Health promotion interventions for community-dwelling older people with mild or pre-frailty: a systematic review and meta-analysis. BMC Geriatr. 2017;17(1):1–13. doi:10.1186/s12877-017-0547-8
52. Delle Fave A, Bassi M, Boccaletti ES, et al. Promoting well-being in old age: the psychological benefits of two training programs of adapted physical activity. Front Psychol. 2018;9:1–13. doi:10.3389/fpsyg.2018.00828
53. Roth S, Cohen LJ. Approach, avoidance, and coping with stress. Am Psychol. 1986;41(7):813–819. doi:10.1037/0003-066X.41.7.813
54. Vitorino LM, Low G, Vianna LAC. Linking spiritual and religious coping with the quality of life of community-dwelling older adults and nursing home residents. Gerontol Geriatr Med. 2016;2:1–9. doi:10.1177/2333721416658140
55. Berk RA. The greatest veneration: humor as a coping strategy for the challenges of aging. Soc Work Ment Health. 2015;13(1):30–47. doi:10.1080/15332985.2014.890152
56. Lozupone M, La Montagna M, Di Gioia I, et al. Social frailty in the COVID-19 pandemic era. Front Psychiatry. 2020;11:1–8. doi:10.3389/fpsyt.2020.577113
57. Chen LK. Older adults and COVID-19 pandemic: resilience matters. Arch Gero. 2020;89:104124.
58. Azlan AA, Hamzah MR, Sern TJ, Ayub SH, Mohamad E. Public knowledge, attitudes and practices towards COVID-19: a cross-sectional study in Malaysia. PLoS One. 2020;15(5):1–15. doi:10.1371/journal.pone.0233668
59. World Health Organization. Mental health and psychosocial considerations during the COVID-2019 outbreak. 2020. Available at: https://www.who.int/docs/default-source/coronaviruse/mental-health-considerations.pdf.
60. Ryan J, Lopian L, Le B, et al. It’s not raining men: a mixed-methods study investigating methods of improving male recruitment to health behaviour research. BMC Public Health. 2019;19(1):1–9. doi:10.1186/s12889-019-7087-4
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
