Back to Journals » International Journal of Nanomedicine » Volume 17
PDA-Based Drug Delivery Nanosystems: A Potential Approach for Glioma Treatment
Authors Wu H , Wei M, Xu Y, Li Y , Zhai X, Su P, Ma Q, Zhang H
Received 28 June 2022
Accepted for publication 22 August 2022
Published 30 August 2022 Volume 2022:17 Pages 3751—3775
DOI https://doi.org/10.2147/IJN.S378217
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Prof. Dr. Anderson Oliveira Lobo
Hao Wu,1 Min Wei,1 Yu Xu,2 Yuping Li,3 Xue Zhai,4 Peng Su,4 Qiang Ma,3 Hengzhu Zhang3
1Neurosurgery, Graduate School of Dalian Medical University, Dalian, People’s Republic of China; 2Nanotechnology, Jinling Institute of Technology, Nanjing, People’s Republic of China; 3Department of Neurosurgery, Clinical Medical College, Yangzhou University, Yangzhou, People’s Republic of China; 4Department of Advanced Materials, Nanjing University of Posts & Telecommunications, Nanjing, People’s Republic of China
Correspondence: Hengzhu Zhang, 98 Nantong Xi Lu, Yangzhou, Jiangsu Province, People’s Republic of China, Tel +86 18051061558, Fax +86-0514-87373562, Email [email protected]
Abstract: Glioma is characterized by high mortality and low postoperative survival. Despite the availability of various therapeutic approaches and molecular typing, the treatment failure rate and the recurrence rate of glioma remain high. Given the limitations of existing therapeutic tools, nanotechnology has emerged as an alternative treatment option. Nanoparticles, such as polydopamine (PDA)-based nanoparticles, are embodied with reliable biodegradability, efficient drug loading rate, relatively low toxicity, considerable biocompatibility, excellent adhesion properties, precisely targeted delivery, and strong photothermal conversion properties. Therefore, they can further enhance the therapeutic effects in patients with glioma. Moreover, polydopamine contains pyrocatechol, amino and carboxyl groups, active double bonds, catechol, and other reactive groups that can react with biofunctional molecules containing amino, aldehyde, or sulfhydryl groups (main including, self-polymerization, non-covalent self-assembly, π-π stacking, electrostatic attraction interaction, chelation, coating and covalent co-assembly), which form a reversible dynamic covalent Schiff base bond that is extremely sensitive to pH values. Meanwhile, PDA has excellent adhesion capability that can be further functionally modified. Consequently, the aim of this review is to summarize the application of PDA-based NPs in glioma and to acquire insight into the therapeutic effect of the drug-loaded PDA-based nanocarriers (PDA NPs). A wealthy understanding and argument of these sides is anticipated to afford a better approach to develop more reasonable and valid PDA-based cancer nano-drug delivery systems. Finally, we discuss the expectation for the prospective application of PDA in this sphere and some individual viewpoints.
Keywords: glioma, polydopamine, polymeric nanoparticles, photothermal therapy, chemotherapy, synergistic therapy
Introduction
In clinical practice, glioma especially GBM, is known as a malignant tumor originating from glioma cells. This type of tumor has been categorized as a grade IV tumor by the World Health Organization (WHO).1 The global incidence of primary craniocerebral malignancy has been increasing annually. According to the recent data from The Central Brain Tumour Registry of the United States (CBTRUS), the highest proportion and the most common malignancy among the primary malignancies of the central nervous system (CNS) are attributed to glioma, which accounts for 14.9% of all major craniocerebral malignancies and other CNS tumors, and 47.1% of major malignant brain cancers. Glioma is more common in the elderly population than in children and young adults. The data also suggest that glioma accounts for about 3% of all brain tumors and other CNS tumors reported in patients aged 0–19 years. A positive dynamic distribution of prevalence with increasing age was also confirmed, with the highest prevalence in patients aged 75–84 years and a male-to-female prevalence ratio of 1.58:1. However, 5.5% of patients with glioma have a relative survival rate of <5 years,2 In addition, the disease rapidly deteriorates with a survival rate of 12–15 months after diagnosis.3 According to data from the CBTRUS, glioma seriously threatens human health because of its low cure rate and high mortality rate. At present, surgical resection functions as the main treatment modality, however, achieving complete tumor resection is difficult because of its unique anatomical location. Postoperative radiotherapy is the standard strategy for glioma treatment,4 but clinical evidence shows that although active, when standardized and real-time postoperative radiotherapy is initiated, the benefit for patients is not ideal because of various individual conditions. Temozolomide (TMZ), a first-line United States Food and Drug Administration (USFDA)-approved clinical therapeutic for glioma, can be administered orally or intravenouslyTMZ is currently the primary treatment strategy and it cures tumors by inducing apoptosis.5 However, the antitumor effects of TMZ are not ideal due to poor targeting and evident side effects with a higher probability of drug resistance.6 Hence, the annual survival rate for patients 5 years after surgery cannot be improved, seriously affecting their quality of life and becoming a major long-standing concern in clinical practice. Different basic studies and clinical trials have revealed that glioma treatment serves as both a difficult and popular topic. In recent years, various types of nanodrug delivery systems (NDDS’), such as liposomes, nanoparticles (NPs), polymeric micelles, dendrimers, and metal particles, among others, have also been increasingly used for basic research on postoperative glioma chemotherapy and other treatments, with a focus on multifunctional PDA nanoparticles.7–11 The representative NDDS’ are multifunctional drug delivery systems (eg, liposome-modified:ICG-AuNPS@PDA (indocyanine green-gold nanoparticles@polydopamine),12 DiR-DOX-Gd@pCaCO3-PEG (1,1’-dioctadecyl-3,3,3’,3’-tetramethylindotricarbocyanine iodide pH-dissociable calcium carbonate-polydopamine-polyethylene glycol),13 semiconducting polymer nanoparticles PSBTBT@PDANPs (Poly[(4,4′-bis (2- ethylhexyl) dithieno[3,2-b:2′,3′-d]silole)-2,6-diyl-alt-(2,1,3-benzothiadiazole)-4,7-diyl]-polydopamine),14 Gd-PDA-Ce6@Gd-MOF (Gadolinium[Gd]-polydopamine-chlorine6@metal-organic framework),15 PDA@CeO2 (polydopamine@cerium dioxide)),10 in which chemotherapeutic drugs can be loaded into PDA-based nanoparticles, making chemotherapy more effective and less toxic owing to precise targeting of tumor tissues due to the combined photothermal effects of PDA, as well as the therapeutic effects of drugs used to effectively combat cancer cells, which may improve the survival rate and prognosis of patients in the near future.16,17
Methodology
We mainly consulted articles through PubMed Advanced Search Builder.
Input the keyword: drug delivery system, polydopamine nanoparticles and cancer (or glioma/Brain cancer)
Advanced Search: ((drug delivery system) AND (polydopamine)) AND (cancer)/(polydopamine nanoparticles) AND (anticancer)
Publication date: 5 years (mainly)
Preparation and Advantages of PDA in Constructing Drug Delivery Systems
History of Polydopamine
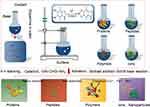
PDA is a novel type of polymer synthesized inspired by adhesion proteins in marine mussels. So, marine mussels are key players in the development of PDA. Marine mussels have a strong adhesion capacity, which can be adsorbed to a variety of solid surfaces in the ocean. Studies have found that the adhesive proteins secreted by mussels can adhere to almost all basal materials.18 Studies into mussel foot filament proteins found that it is rich in a large number of 3.4-di-hydroxyphenylalanine (DOPA) molecules, and that the catechol group contained in DOPA has a strong coordination ability, can form reversible organometallic complexes with metals, and that the catechol group is oxidized to form a quinone, which can react with many groups to form covalent bonds. The formation of multiple covalent and non-covalent interactions between the DOPA molecular structure and the adhered substrate is the fundamental reason for the extremely strong adhesion ability of mussel adhesion proteins.19 Scientists have studied the adhesion of mussels and applied this superior adhesion to adhesion material development. As such, researchers chose the small molecule dopamine (DA) with a catechol and amino group as a precursor to develop a new mussel-based bionic material. Subsequently, in 2007 Messersmith et al obtained PDA via the oxidation and self-polymerization of DA with tris (hydroxymethyl) aminomethane hydrochloric acid (Tris–HCl, pH = 8.5) at room temperature without a catalyst.20 The loaded polymer or metal oxide surface formed a PDA coating with multipurpose functionalized reactive groups capable of subsequent Michael addition reactions or Schiff base reactions and cascade reactions through amino–amino, amino–mercapto, or aldehyde groups for the multidimensional functional loading of desired materials. PDA has excellent advantages in the field of surface modification and has been rapidly developed in recent years.21 Studies have reported that DA oxidation can be modulated by other functional molecules and self-polymerization reactions.22 Furthermore, the coassembly of DA with other functional molecules can be used to prepare microstructures and nanostructures with novel compositions and morphologies, including NPs, semiconductors, and organic conjugated polymer-based nanomaterials.23 Based on its aforementioned properties, the special attributes of PDA determine its value for a wide range of applications.24 (Figure 1).
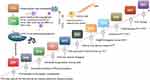 |
Figure 1 The development history of PDA. Abbreviations: PDT, photodynamic therapy; PTA, photothermal antibacterial. |
Preparation of PDA
At present, the preliminary ways of PDA synthesis mainly include electropolymerization, enzyme oxidation, and solution oxidation. Solution oxidation is widely used due to its simple reaction conditions, low cost, and easy preparation. 7.5 Alkaline solution adopts spontaneous oxidation polymerization, and the color of the solution changes from colorless to dark brown.25,26 Due to many reaction sites and acting forces involved in the reaction, the complex structure and molecular mechanism of self-polymerization of PDA has not been fully studied. Currently, the widely accepted theory is that PDA is shaped through two diverse ways: non-covalent self-assembly and covalent polymerization.27 Key factors such as solvent temperature, pH, concentration of oxidant DA, and reaction time affect the morphology of PDA, film thickness, and reaction rate. Therefore, PDA-based NPs with desirable properties can be obtained by changing these conditions.22 For instance, paclitaxel (PTX) has been dissolved in Genexol PM, a polymeric micelle (PM), or human albumin N (nab-PTX).28 The accumulation of chemotherapeutic drugs loaded onto PDA nanocarriers allow for controlled pH-response and sustained drug release in tumor cells while protecting the chemotherapeutic drug from degeneration, metabolism, and renal clearance during transport. Therefore, this approach allows for improved bioavailability by extending its half-life in the blood. The therapeutic properties of PDA-based NPs are mainly determined by their physicochemical properties, with the most considerable properties being the size, shape, surface modifications, and surface charge of drugs. Many studies have shown that NP size is the main factor affecting their distribution in tumors.29–32 The size of PDA-based NPs usually ranges from 10 nm to 200 nm.33 NPs measuring approximately 100 nm are better at targeting tumor. A recent study by Perrault et al reported that particles measuring <20 nm can be rapidly internalized by tumor tissues; however, poor retention/accumulation is a major disadvantage.34 In contrast, NPs measuring >200 nm may lead to NP retention in the spleen and liver, resulting in damage to normal tissues. Similarly, NP shape may affect cellular uptake, half-life, biodistribution and degradation. The maximum NPs that can be used are orbicular; however, oblate particles adhere better to biological substrates, may deliver more drugs, and display superior adhesion to vascular system. PDA-based NPs have excellent adhesion properties and are abundant in various functional groups (eg, amino and hydroxyl groups), which facilitate further chemical modifications and may exert better therapeutic effects. Moreover, cell internalization, biodistribution, and cellular interactions are determined by the surface charge of nanocarriers. Although positively charged NPs are more toxic and lead to increased generation of ROS in the mitochondria, lysosomes, and plasma membrane than neutral or negatively charged particles, they are more likely to be internalized. In the case of biodistribution, neutral nano preparations are highly charged NPs (negative or positive) mainly accumulate in the liver. Their uptake by the reticuloendothelial system and the liver is lower. However, slightly negatively charged NPs accumulate more in tumor tissues, which further increases their efficacy. PDA-based NPs are negatively charged and have enhanced cell internalization, biodistribution, and bioavailability to cross biological barriers. At present, the development and application of PDA-based NDDS’ in GBM treatment are the major focus areas of basic research and preclinical trials. The main advantages of NDDS’ are the highly targeted delivery rate of antitumor drugs, improved drug redistribution in vivo, increased drug solubility, ability to penetrate the blood brain barrier (BBB) and blood brain tumor barrier (BBTB), prolonged drug half-life, improved bioavailability, and reduced toxic side effects in all bodily organs.35 To date, all studies and trials have sought to create maximal antitumor activity against tumor cells and to provide new strategies for clinical treatment. PDA-based NPs can be loaded with clinical chemotherapeutic drugs, such as TMZ, doxorubicin (DOX), and PTX, or modified with nucleic acids, polymers, peptides, polypeptides, and other small molecules to exert more precise and effective therapeutic effects by targeting specific sites.
Advantages of PDA in Constructing Drug Delivery Systems
Improved Cellular Biocompatibility
Biocompatibility if an important consideration for avoiding drug carrier-induced systemic toxicity. PDA-based NPs have better blood compatibility, no obvious hemolysis, no acute toxicity to C6 and U87MG human cell lines, including glioma cells, HeLa cells (a human cervical carcinoma cell line), 4T1 cells (a mouse breast cancer cell line) and HBE cells (a human bronchial epithelial cell line).36 Moreover, mouse cell lines can grow on the surface of PDA coatings, thereby confirming the safety of PDA at the cell level.37,38 The median lethal dose (LD50) is a normal method used to appraise the acute lethality of agents. Studies have shown that the LD50 (intravenous injection) of PDA blank vector was 483.95 mg·kg−1 and the 95% confidence interval was 400.22~ 585.19 mg·kg−1.25 In addition, the same studies have also indicated that PDA blank vectors have no obvious abnormalities and do not induce any obvious signs of hepatic damage when tested against some significant hepatic indicators. Some experiments have also proven that PDA is biodegradable in vivo.39 However, the detailed degradation mechanism and degradation products of PDA in vivo remain unclear and require further detailed systematic study.
Excellent Photothermal Conversion Performance
Photothermal therapy (PTT) is an emerging physicochemical treatment method with high selectivity and minimal invasiveness, in which light energy is converted to thermal energy via near-infrared light irradiation from an external auxiliary light source. The rapidly increasing temperature is used to conquer targeted tumor cells through photothermal effects. The latest recorded photothermal therapeutic strategies are primarily based on precious metal NPs, such as gold, silver, and palladium (Pd) NPs, copper-based NPs, carbon-based nanomaterials and organic polymers. PDA can be used as a photothermal therapeutic agent, without significant damage to the surrounding normal tissues and with reduced side effects. This was originally discovered by Liu et al who prepared stable and well-dispersed PDA-based NPs with an advanced photothermal conversion rate of 40%.19 The dispersion temperature of these PDA-based NPs was rapidly increased by 33.6°C via 808 nm laser irradiation (2 W/cm2) for 5 min at a concentration of 200 μg/mL in almost all 4T1 and HeLa cells. This study demonstrated the superior photothermal effects of PDA. Although the above studies are based on 4T1 and HeLa cells, we speculate that PDA-based NPs may hold significant promise for PTT of GBM. Interestingly, the same study showed that NDs@PDA@ICG can be used in PTT for glioblastoma.40
Strong Adhesiveness and Highly Chemical Reactivity
It is widely believed that the large amount of catechol and amino coexisting in PDA are the main reason for its strong adhesion to almost all inorganic or organic substrates, but the exact adhesion mechanism remains unclear.15,22 PDA nanocarriers can be stably stored in water for several months without agglomeration. Even after being dispersed in a 10% serum solution for 24 h, their ultraviolet absorption shows almost no change, indicating that they have good colloid stability. Therefore, PDA self-polymerization can be used to bond and deposit a thin film on the surface of easily agglomerated matrix nanomaterials (eg, carbon nanotube gold nanoparticles and magnetic nanoparticles) to form a core-shell structure and improve the dispersion of NPs in aqueous solution.41,42 More importantly, mercapto- or amino-capped molecules can be linked to catechol or amino on the surface of PDA through Michael addition or Schiff base reaction to achieve functional modification of PDA.43,44 In addition, the catechol structure unit of PDA can chelate with many metal ions such as Gd3+, Mn2+, and Fe3+. Anti-tumor drugs such as TMZ, DOX, PTX, camptothecin, and curcumin can adsorb on the surface of PDA through π-π stacking with the rich aromatic rings in PDA. Furthermore, drugs can be stably loaded onto these structures under physiological conditions with less drug leakage. Once internalized into tumor cells, drug release is triggered by the acidic conditions of lysosomes, showing the powerful potential of PDA for drug delivery.23
Multiple Drug Release Response Mechanisms
Effective release of chemotherapy drugs at tumor sites is essential for cancer treatment. As a drug delivery carrier material with a variety of stimulation-responsive drug release mechanisms, PDA can respond to exogenous stimulation of NIR and endogenous stimulation of pH and glutathione (GSH). The drug can be stably stored in the nanocarrier in blood circulation, and the intelligent release of the drug can be realized when the nanoparticles are ingested by tumor cells. Although the intracellular pH of healthy tissues and tumor cells is similar, the extracellular pH of tumor cells is lower than that of normal tissues. In normal tissue and blood, the extracellular pH is around 7.4.45 Fast growing tumor cells usually have a high metabolic rate.46 Hypoxia and high glycolysis activity are common features of solid tumors. Acidic metabolites, mainly lactic acid, will accumulate in the outer stroma of tumor cells.47,48 When nanometrics arrive at the tumor tissue, they need to be transported into the cell through the endosome-lysosome pathway, and the pH of the endosome-lysosome is as low as 5.5–6.0 and 4.5–5.0, respectively.49 PDA exhibits amphoteric ionic properties, because PDA contains a large number of amino and phenolic hydroxyl groups, which are positively charged due to the protonation of amino groups at low pH. At high pH, the negative charge due to deprotonation of phenolic groups will have an impact on the adsorption and release of charged drug molecules.50 Therefore, PDA and charge properties of drugs can be used to design nano-delivery systems for releasing drugs in response to the pH of the tumor microenvironment (TME), allowing for drugs to stably exist in their delivery carrier in blood circulation and be released in the acidic TME. For example, at pH 7.4, PDA can load DOX through π-π stacking and under acidic conditions, the amino protonation of PDA and DOX increase the solubility of DOX, thus the drug can be released.51 ROS play an essential role in regulating various physiological functions of living organisms.52 GSH is the most abundant endogenous antioxidant in cells, and excessive GSH can remove ROS with some cytotoxicity.53 The concentration of GSH in tumor tissues is at least 4 times that of normal tissues, so a high concentration of GSH in tumor tissues can be used as a nano carrier to release endogenous stimulators of drugs.54 Some researchers have found that when PDA is incubated with GSH solution, the concentration of GSH gradually decreases with the increase of PDA concentration and increased incubation time. Furthermore, drug release significantly increases when GSH is added into drug-carrying PDA NPs.32 When temperature increases, the non-covalent π-π-mediated interaction between drugs and PDA at aromatic regions is disrupted. Therefore, the photothermal effect of PDA can be used to effectively trigger drug release.55,56
In conclusion, PDA involves plentiful functional groups (such as amine, imine, and catechol). Thus, PDA has the following remarkable characteristics: (1) negative potential and stability; (2) a strong ligand of multivalent metals and adhesion to almost all substrates; (3) high loading ability; (4) easy preparation and easy modification (-SH or -NH2); (5) flexible control; (6) targeted delivery; (7) able to penetrate the BBB and BBTB; (8) amenable to controlled drugs release.
Application of Drug Delivery System Based on PDA in Tumor Targeting
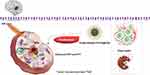
In terms of drug delivery strategies, targeting agents can be divided into three categories: passive targeting, active targeting, and physicochemical targeting agents.57 Although PDA has no direct targeting effect on tumor tissues or cells, it is a key carrier material for transporting diagnostic and therapeutic substances, such as contrast agents and photothermal agents, as well as modifying targeted groups (eg, PDA nanospheres,58 mesoporous polydopamine NPs,59 PDA-coated NPs,60 and PDA nanocapsules.61 A graphical illustration of applications of four common PDA NPs is detailed in Figure 2.
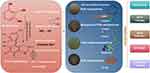 |
Figure 2 Synthesis and main features of PDA. Schematic illustration and applications of four common PDA-based nanoparticles. |
PDA Nanospheres
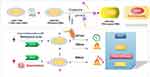
PDA NPs were integrated by neutralization of DA hydrochloride with NaOH in water.53 PDA NPs can be uncoupled into two varieties according to different preparation methods. The first is to prepare blank solid spherical carrier of PDA, and then achieve the purpose of passive or active targeting through drug loading or secondary modification. The second method involves the PDA self-polymerization reaction after mixing the bulk drug or synthetic precursor drug with DA.62–64 In the first preparation method, the bulk drug or ligand modification is carried out on the external surface of PDA NPs. Due to the high content of PDA, the photothermal effect is higher when applied to PTT, but drug loading is restricted by the limited surface area. The second mixed drug delivery method can increase drug loading. In the field of tumor drug delivery, PDA NP surfaces can simultaneously load a metal ion contrast agent, chemotherapy drug, photothermal agent or photosensitizer, coupled with the photothermal conversion ability of PDA. Therefore, PDA NPs have a unique advantage in the field of combination treatment in the integration of diagnosis and treatment compared with other material constructed NPs. Dong et al have exploited PDA-ICG-PEG/DOX (Mn), which can enable imaging-oriented chemotherapy and PTT of tumors.65 Mpeg-sh MPEG-NH2 or other forms of polyethylene glycol (PEG) are often used to chemically modify PDA NPs to increase colloidal stability of nanoparticles and prevent particle aggregation in order to maintain stability and achieve long circulation of nanoparticles in blood and avoid recognition and phagocytosis by the reticuloendothelial system66 (Figure 3).
In addition to the PTT, PDT is an emerging treatment method for tumors, which uses light and has the advantages of fewer side effects and high controllability. It includes three basic components; a photothermal agent, light, and oxygen. The basic principle of this treatment is the reaction between the photosensitizer and oxygen under the action of light to produce ROS to eradicate tumor cells.67 TME and tumor stem cells, which exhibit enhanced proliferation and abnormal angiogenesis in their suitable microenvironment, consume a large amount of oxygen and result in a hypoxic state, which favors the migration, proliferation, and deterioration of tumor cells, leading to photodynamic resistance. He et al used PDA to prepare stable GNR-PDA-based NPs loaded with DOX to achieve the delivery of chemotherapeutic agents and the combined therapeutic effects of PDT and PTT for tumors.68 Cao et al investigated a nanoplatform constructed by assembling Pt nanoparticles and PDA, which improved TME while improving PDT efficacy and the lack of oxygen when combined with PTT.69 PDT can stimulate non-toxic photosensitizers to produce cytotoxic ROS that hit cancer cells, close-down microvasculature, and stimulate the immune system.70 This approach also can reduce the growth of U87MG and, in conjunction with photothermal therapy, increase survival of GBM xenografted mice.71,72 Remaining glioma cells are leading factors of postoperative recurrence. Therefore, a hypoxia-responsive lipid polymer nanoparticle (LN) has been developed for fluorescence-oriented surgery, chemotherapy, PDT, and PTT combined with multitherapy strategies for targeting glioma.73 At present, most PDA NP drugs are loaded by π-π stacking. Zhang et al showed that a pH sensitive polymeric pro-drug was modified on the surface of PDA NPs by amidation chemistry for alliance of chemotherapy with photothermal treatment. Studies of the raw data proved successful preparation of the PDA@PCPT NP (camptothecin-containing polymeric prodrug), which covers 24.7% CPT (mass ratio, with the tumor inhibitory rate of PDA@PCPT + NIR irradiation therapy being 92.8%).74 By combining pH and INR, the drug delivery method is faster than the π-π stacking drug delivery method, which can have a greater therapeutic effect, but the preparation process is more complex, which is why there are few studies on this kind of drug delivery method (Figures 4 and 5).
Mesoporous Polydopamine Nanoparticles (MPDA)
The drug load of PDA NPs itself is not high, especially when it is loaded with multiple drugs at the same time. The drug load of each drug is lower than that of a single drug. Therefore, the application of PDA NPs in multimodal therapy is limited. Mesoporous PDA NPs (MPDA) can be used to overcome this problem. Chen et al reported that the MPDA structure fully utilizes the π-π stacking interactions between PDA structures and the π-electron of TMB molecules.75 By changing the mass ratio of TMB to Pluronic F127, mesoporous NPs with ideal diameters and pore sizes can be prepared compared with PDA NPs. The pores in MPDA significantly increase the surface area of nanoparticles, thus increasing drug loading. Xing et al designed MPDA with DOX as chemotherapy drug.76 In addition, through π-π stacking and hydrophobic interaction, the surface was modified with PEG 1000 vitamin E succinate, a drug efflux inhibitor, to inhibit the multiple drug resistance of tumor cells and enhance the sensitivity of tumor cells to DOX. The drug loading capacity of the nanoparticles was 2000 μg·mg−1. The DOX loading was significantly higher than that of PDA NPs (52–660 μg mg−1), but the photothermal conversion efficiency of the nanoparticles was 12.8% due to the mesoporous structure.75
Polydopamine Nanocapsules, PDAC
PDA nanocapsules (PDACs) are prepared using a template method, which can be either soft or hard. The principle is to disperse the template in 10 mmol·L-1 Tris-HCl buffer (pH = 8.5) dissolved with DA at room temperature under aerobic conditions. The PDA can then be deposited on the surface of the template after a certain period of reaction time by vigorous stirring, and then the template material is selectively dissolved in a solvent.77 The advantage of PDACs lies in their larger surface area compared to PDA NPs, which is conducive to improving drug loading. The hard template method uses solid NPs (CaCO3, SiO2, and polystyrene, among others) as templates to prepare PDACs. The advantages of this approach include improved stability and monodispersity of solid particles, which can better control the shape and size of the final nanoparticles. However, the hard template method requires the use of acid or organic solvent to dissolve the template. This can easily affect the nature of PDA.78,79 Zhuang et al indicated a modified DMDES emulsion template method to acquire 200 nm PDACs, and act as extremely valid theranostic agent for photoacoustic imaging (PAI) and chemo-photothermal collaborative treatment.80 This research demonstrated the great potential of PDACs as a new therapeutic diagnostic agent.
PDA-Coated Nanoparticles
The preparation method of the PDA-coated nanoparticles was as follows: DA in 10 mmol·L−1 Tris-HCl buffer (pH = 8.5) at room temperature under aerobic conditions. A layer of PDA film was formed on the surface of the NPs, which was then dispersed after centrifugation. PDA adheres strongly to almost all types of matrix surfaces, which greatly widens the application range of other carrier materials. The purpose of multimodal diagnostic imaging and combination therapy can be realized by coating the required functional materials. PDA-coated NPs can first encapsulate drugs internally. Next, the targeted ligand modification on the PDA surface can separate drug delivery and chemical modification, which can not only give the active targeting function of NPs, but can also reduce the interference of complex physiological environment on drug properties in blood circulation. This has significant advantages in the construction of complex nano vectors. Du et al showed that the DOX-loaded Mesoporous silica NPs, MSNs (MSNs-DOX@PDA@keratin), can be internalized by tumor cells through endocytosis, having great potential in drug delivery applications.81 PDA is an ideal drug delivery carrier for intelligent drug delivery into tumor cells. Although PDA is not tumor-targeting specific, it can be modified by adapting the surface of PDA with well-known tumor markers such as hyaluronic acid (HA), peptide and folic acid (FA). This increases the interaction of NPs with receptors or specific molecules over-expressed by tumor cells without changing the overall biological distribution of NPs to significantly increase the amount of drug delivered to tumor cells.82 However, some studies have used HA to modify PDAs coated NPs, and found that HA delays drug release, indicating that the chemical modification of the PDA surface may affect interactions between PDA and drugs and their physicochemical properties. Therefore, we should pay attention to the effect of PDA surface modification on NPs when designing future drug delivery systems. Due to the mild reaction conditions of Michael reaction and Schiff base, targets such as antibody polypeptide nucleoacid aptamers, which are unstable in organic solvents or reaction conditions, can be easily attached to PDA surfaces without losing their biological activity.83 Some special physical and chemical methods can also be used to achieve targeted drug delivery, such as using PDA adhesion coating of iron, nickel, cobalt, and other metals and their oxides, as well as other magnetic substances. Further, under the guidance of local magnetic field in vitro NPs are directed to the tumor site, to achieve magnetic targeting, in order to reduce the systemic toxicity of drugs to the body. These include Fe3O4@PDA@HA-MTX (based on magnetic polydopamine (MPDA) coated with hyaluronic acid-methotrexate and Fe3O4 conjugates), BiVO4/Fe3O4@PDA SPs (BiVO4/Fe3O4@polydopamine superparticles).84,85
Above all, PDA is a kind of simple preparation and property of multi-purpose carrier material that can be used to build a nanometer carrier and plays a key role in connecting to a variety of functional groups or molecules by PDA. PDA has great development potential in targeted drug delivery and multi-mode collaborative therapy.
The applications of common PDA-based nanodrug delivery systems (PDA nanospheres, PDA mesoporous nanoparticles, PDA-coated nanoparticles, and PDA nanocapsules) are summarized in Table 1. 58–61,65,86–97
 |
Table 1 Some Examples of Drug-Loaded PDA-Based Nanoparticles |
Based on existing studies, PDA0Based NPs are expected to be key to solving some fundamental problems concerning glioma treatment.
Glioma and PDA Nanocarriers
New strategies, such as PDA NP-based therapeutics, are increasingly being used to treat human tumors, especially with relevance to the therapeutic research of glioma.98 These new strategies are based on the use of nanomaterials with physicochemical properties and the proteins, charges, polypeptides, and other substances they are loaded with, which are beneficial to the development of new therapeutic approaches or the improvement of existing therapeutic strategies.99,100 The properties of standard NPs are presented in Figure 6.
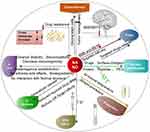 |
Figure 6 Properties of standard nanoparticles. |
Passive and Active Targeting of PDA NPs in Glioma
Rationale for Utilization of Nanomedicines in Glioma Therapy
Passive Targeting
The penetrability of nearby brain vasculature alters during the growth of glioma. In the early phase, the growth of tumor cells depends only on normal brain vessels and the BBB is intact. With tumor progression and permeation, glioma cells intrude the area normal tissues. When a large enough volume (>0.2 mm3) is reached by the tumor cell cluster, a configurational damage will impact the BBB and the BBTB.101 Within this aspect, claudin-1, a protein specifically expressed in the tight junctions of endothelial cells, is down-regulated in vessels surrounding high-grade gliomas, thus increasing the permeability of the BBB.102,103 This “leaky” BBTB is a common characteristic of high-grade gliomas, because metabolic demand is increased. Furthermore, in accordance with the high angiogenic nature of high-grade gliomas, VEGF enhances BBB permeability, by irritative angiogenesis in response to hypoxia.104,105 The “leaky” BBTB can be exploited for drug delivery objectives, by utilizing the alleged enhanced permeability and retention (EPR) effect. Since the pore cut-off size at the BBTB is extremely variable, the size and shape of nanocarriers mainly effects the extent and efficacy of drug delivery. But in reality, vascular leakage is considerably decreased in tumors within the brain microenvironment compared to other regions, and it is influenced by the tumor phase and/or to the tumor model used.106 For example, the key cut-off size of the BBTB for intracranial U87MG xenografts ranges between 7 and 100 nm.107 In spite of the reduced size of vessels, fenestrations may restrain the feasibility of passive targeting strategy to handle brain cancer. Drug-loaded nanocarriers free of targeting ligands indicated hopeful efficiency in orthotopic brain glioma models, hence, permitting a translation to clinical therapy.108
Active Targeting
However, high-grade gliomas promptly infiltrate the surrounding healthy tissue, where the BBB is not modified and the EPR effect cannot be gained.109 In actual fact, unlike in animal tumor models, chemotherapy in human patients is only used as an adjuvant treatment, and it should primarily be addressed towards the eradication of residual tumor cells after surgery or radiotherapy. This cell population includes cells migrating from the tumor into healthy tissue or that reach the tumor from distant sites. Therefore, the most important aspect for chemotherapy is the one surrounding the glioma, the so-called brain adjacent to tumor (BAT), including cells in the invasion stage, that do not still influence the integrity of the BBB. Since BAT should be the primary aim of chemotherapy, the development of formulations easily crossing the intact BBB is fundamental.110 In this circumstance, appropriate active targeting of nanocarriers is needed to achieve the target tissue, by exploiting carrier and/or receptors over-expressed at the BBB. Carrier-mediated transporters (CMTs) are necessary in the transport of basic small molecules into the brain. Receptor-mediated transporters (RMTs) are largely expressed at the BBB, being utilized by large endogenous biomolecules.111 Specific peptide receptors are included in RMT (eg, low-density lipoprotein (LDL) receptor, transferrin (Tf) receptor, lactoferrin (Lf) receptor, insulin receptor, and receptors for insulin-like growth factors (IGF-1 and IGF-2)).112 CMT and RMT ligands have been continually utilized for drug delivery as molecular “Trojan horses” for nanocarriers.113
In conclusion, active and passive methods are two widely used strategies for nanocarrier-based drug targeting.114 There may be two kinds of cellular targets among active targeting pathways: (1) targeting tumor cells mediated by cell surface receptors; and (2) the common target tumor endothelial cells.115 Until now, no nanocarriers with active targeting have been approved by the FDA, and only a few clinical trials are underway. This clinical failure is attributed to the fact that these nanocarriers seep into the tumor vascular system. Inescapably, they have to cross different and considerable obstacles to reach and infiltrate cancer cells.100 The targeted drug delivery is prepared for the release of therapeutics in detailed components or a targeted field of the body based on the EPR effect or the receptor-mediated endocellular transport and for the removal of the drug concentration in nontargeted components.116 Drug-loaded PDA NPs offer exceptional advantages for the passive and active targeting of tumor33 (Figure 7). Passive targeting takes into account the permeability of the tumor vascular system and the improved EPR effect to exert a transport role, which allows the chemotherapeutic drug to attach around the tumor and exert a killing effect after its release.117 Meanwhile, active targeting is achieved by loading functionalization of the surface of PDA NPs loaded with chemotherapeutic agents. The target site provides a selective recognition of different receptors or antigens overexpressed in cancer cells, improving their therapeutic effects by increasing precision and overcoming multidrug resistance. PDA NPs carriers can be internalized by the TME once they come close to the tumor and can perform a continuous release of cancer-killing toxins to achieve the treatment purpose.118 However, in vivo, the EPR effect does not work well; hence, when nanocarriers achieve “long-circulation” in the body, the EPR effect can work perfectly.119 The exploitation of NP decks with a long in vivo cycle half-life has long been one of the primary aims in the sphere of tumor drug transport. Long-circulating NPs may be able to more efficiently concentrate to the tumor through either the passive or active targeting mechanism. The PTDDS primarily transmit drugs to tumor tissues based on the improved EPR effect in tumor tissues instead of normal tissues.120,121
PDA-Based NPs and the BBB and the BBTB
The BBB separates the central nervous system from the systemic circulation.122 As such, the BBB not only stops toxins and pathogens from entering the brain, but also restricts the brain uptake of therapeutic molecules. Whereas, under specific pathological circumstances, the BBB is undermined, permitting immediate interaction between blood components and the diseased area. Alzheimer’s disease, brain tumor and Parkinson’s disease. The prime sides of nanocarriers project as they are associated with infiltration and preservation in the CNS are also prominent.123 In recent years, a number of strategies have been studied to aid drug delivery across the BBB, including infiltrative destruction of the BBB and chemical modification of pro-drugs. Moreover, NP-mediated drug delivery gaining increased interest as a potential and non-invasive system to cure cerebral diseases.124,125 PDA NPs are specifically internalized by specific regions of the BBB and the BBTB under receptor-mediated cellular transcytosis. However, penetrating tumor tissues to target the release of sufficient drug concentrations is a challenge for nanomedicine. The permeability and the retention effects of PDA NPs are low because they are not only highly selective in penetrating the BBB, but are also prevented by the dense brain matrix. Therefore, solely relying on passive targeting is insufficient. Tumors must be actively targeted using molecules (ie, antibodies, proteins, and peptides) on the NP surface that can bind to tumor cell antigens. The structure and the function of the BBB in brain tumor tissues are altered by angiogenesis, which transforms the BBB into the BBTB having a heterogeneous neovascular system with a wide variation in permeability. However, this heterogeneity does not increase the effectiveness of antitumor drugs for glioma treatment. Drugs, enzymes, DNA or RNA molecules, and antioxidant or inorganic molecules encapsulated in NPs are currently used to cross the BBB or BBTB in glioma. NPs are very limited in their ability to cross the BBB without assembling specific ligands or coatings, whereas polymeric PDA NPs show great versatility and penetration. The targets overexpressed in GBM are LRP1, TfR, GLUT, αvβ3 integrin, GFAP, Cx43, EGFR, EGFRvIII, IL-13Ra2, and Fn14, which are commonly targeted molecules in nanomedicine. Gregory (2020) designed GBM-targeted synthetic protein NPs (SPNPs) composed of polymerized human serum albumin and oligo (ethylene glycol) containing the cell-penetrating peptides, iRGD and STAT3 inhibitor (STAT3i), which can effectively cross the BBB. These protein-based nanocarriers can bind to the cell surface receptors overexpressed in the glioma cells and tumor vascular endothelial cells, precisely targeting the tumor cells.126 Other studies suggest that dodecamer peptide (G23)-intelligentized PDA-coated curcumin-loaded zein nanoparticles (CUR-ZpD-G23 NPs) can effectively thread the BBB and deliver curcumin to the glioma cells. NPs have improved the cellular uptake of curcumin by C6 glioma cells compared to free curcumin and indicate strong infiltration into three-dimensional tumor spheroids. The functionalization of the NPs with G23 stimulated the BBB traversing and the tumor spheroid infiltration. Moreover, NPs have been shown to dramatically restrain propagation and transplantation, and induce cell death in the liquid and soft agar models of the C6 glioma cell growth127 (Figure 8).
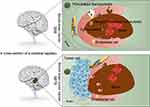 |
Figure 8 Internalization of nanoparticles through the BBB and BBTB. |
TME Targeting of PDA NPs May Be an Area for Future Research
To enhanced glioma therapy, plenty of iatrochemistry have been encapsulated in nanosystems to accelerate their capacity to surmount the BBB and specifically arrive at the cancer cells, diminishing negative effects and boosting drug concentration in the cancer microenvironment. Glioma, especially GBM, is a highly invasive tumor without a clear boundary with the surrounding normal tissues.128 The absence of this boundary is also one of the reasons why glioma is difficult to cure. Glioma invasion mainly involves three processes: (1) adhesion of tumor cells to the extracellular matrix (ECM); (2) ECM degradation; and (3) migration and angiogenesis of tumor cells. In these processes, the TME plays a regulatory role in tumor invasion.129 In the perspective of active tumor targeting, the TME is an important key domain for designing any nanocarrier for effective drug targeting130 (Figure 9). TME-normalizing therapies advance and uniformize the intratumor allocation of nanomedicines. Nonetheless, we believe that TME targeting of PDA NPs may be an area in glioma for future research.131 In brief, the normalizing of TME can enhance the efficacy of targeted nanomedicines that associate cytotoxic agents with immunotherapies.132 Taken together, we believe that PDA will be a promising drug targeted delivery vehicle.
 |
Figure 9 Normalizing the TME to increase the penetration of combination therapies. Targeted, functionalized and/or combination nanomedicines widely distribute throughout tumour lesion. |
Up to now, the part of the content has not been studied about TME targeting of PDA NPs, especially glioma. This could be an area for future research and provide a direction of research for us.
PDA NPs on the AKT/ERK Signaling Pathway
Recent research into nanotoxicology has not centered on the feasible biological toxic effects of nanoparticles, but on the toxic mechanism of nanoparticles. To date, oxidative stress and inflammatory reaction in cells are two of the major views to illuminate the toxicity theory of nanomaterials. Nevertheless, recent studies have shown that the tumor signaling pathway is a potential toxic mechanism. The nine signaling pathways that are the most researched include NF-κB, PI3K/AKT, MAPK, JAK-STAT, TGF-β, Wnt, Notch, Hedgehog, and Hippo pathways.133 Some researchers have indicated that the AKT/ERK signaling pathway plays a considerable role in many cellular responses, including propagation, apoptosis, and autophagy (Figure 10). Zhao X and Qi T et al believed the AKT/ERK signaling pathway is relevant with the prohibitive impact of Au–Ag@PDA NPs (PDA-coated gold-silver alloy nanoparticles) by measuring the phosphorylated forms of AKT and ERK1/2 with Western blot analysis. Furthermore, some studies have suggested that dual functionalized brain-targeting nanoinhibitors can control TMZ-resistant glioma via attenuating EGFR and MET signaling pathways.134 Therefore, diverse NPs have the potential of being extremely advantageous as vectors for therapeutic cargo delivery to GBM cells, which opens new possible methods to treat fatal tumors.135
PDA Improve Adverse Effect
In clinical practice, the chemotherapeutic drugs TMZ and PTX are the most common treatments for glioma.136 However, their severe side effects often lead to reduced patient compliance. To address this limitation, scientists have been investigating novel drug delivery systems to improve the targeted delivery rate, reduce side effects, eliminate the first-pass effect, and improve drug bioavailability. PDA-based NPs are expected to address such shortcomings.23 The controlled release system can identify the lesions and quantitatively release drugs regularly to achieve better therapeutic effect. After normal body awareness, a controlled drug release system can stop drug release to realize the feedback regulation of a controlled release system of control signals not only confined to the body (eg, pH, reduction potential, temperature, ionic strength, enzyme concentration, and pressure difference, as well as external signals, such as thermo-optical electric field, acoustic waves, and magnetic fields).137 Controlled drug release systems usually need to use intelligent materials as drug carriers, sensor processing and execution functions in one, so as to achieve the purpose of intelligent controlled drug release. The controllable drug release system and conventional dosage form ratio can improve drug efficacy and reduce side effects, which has become a rapidly developing research frontier in the field of biomedicine.138 The pH of tumor tissue microenvironment is usually lower than that of normal tissue. This characteristic shows potential advantages in the design and construction of pH-sensitive drugs, while PDA-based catechol in NPs can coordinate with many ions and other groups, which can release chemotherapeutic drugs in acidic conditions with pH response, while almost no drugs are released in alkaline conditions to reduce toxic and side effects and overcome the multiple resistance of chemotherapeutic drugs.139 This extraordinary combination of PDA nanomaterials with autophagy inhibitors could afford a promising tactic for tumor therapy in the immediate future.140
Applications of Polydopamine Nanoparticles in GBM Therapy
Application of PDA-Based NPs in Chemotherapy
Chemical therapy plays an important role in the treatment of GBM. Although the chemotherapeutic agent, TMZ, currently exhibits the best clinical performance in glioblastoma treatment, new therapeutic techniques aimed at improving its efficacy remain an urgent goal, where the emergence of PDA-based NPs can also play a key role in achieving this. Because of the versatility of the modification, PDA, a mussel adhesive protein mimetic that binds to Asn-GlyArg (NGR), has been used to enhance the targeting ability of drug carriers. Zhang, Peng et al used PDA-coated MSNPs as a TMZ vector and NGR as a targeting ligand to synthesize a drug-carrying targeting system (MSN-TMZ-PDA-NGR) for glioma chemotherapy. Their results showed increased accumulation of NGR-MSNPs in C6 cells compared to unmodified MSNPs. Anticancer drugs can cause autophagy in tumor cells, whereas autophagy inhibitors can block this reaction and enhance the TMZ effect of the drugs.141
Application of PDA-Based NPs in Combination Therapy
There are many challenges in treatment of tumors, such as tumor heterogeneity, the BBB. Drug combination therapies have indicated more and more advantages against those challenges. With the assistance of nanocarriers, an increase in efficacy and safety could be acquired using collaborative combinations of diverse therapeutic agents.11 Combination therapy is a method of treating GBM aimed at double or multiple combinations of attack against tumors to obtain satisfactory therapeutic effects. The commonly used combination methods are “chemotherapy + PTT”, “PTT + PDT”, and “radiotherapy + PTT”, which can effectively compensate for the inherent defects of a single treatment, further optimize the treatment and maximize the therapeutic effects. In addition, it can regulate multiple signal transduction pathways of cancer-causing cells. However, the combination therapy characteristics are complex and variable, and the reduction in the dose of therapeutic drugs, overcoming drug resistance and enhancing therapeutic effects remain as the major concerns. In addition, several issues must be carefully addressed, including the design and implementation of experiments, timing, sequence, dose and concentration of drug administration, reduction in side effects, and improvement in bioavailability. Based on the PDA properties, researchers have designed PDA-based NPs with targeted delivery, controlled drug release, reduced side effects, improved bioavailability and decreased drug resistance. Multifunctional drug delivery and combined multimodal therapy strategies are very promising in tumor theranostic applications. Wang, Shaowei et al developed a simple and versatile nanoplatform based on biologically inspired polydopamine capped gold nanorods (Graphene nanoribbon[GNR]-PDA-DOX/MB).142 Methylene blue (MB) and DOX are directly adsorbed on GNR-PDA via electrostatic and/or π-π stacking interactions, forming GNR-PDA-MB and GNR-PDA-DOX nanocomposites, respectively. The GNR-PDA-MB can generate ROS from MB or hyperthermia (from GNR-PDA) with high efficiency under deep-red/NIR laser irradiation, while the GNR-PDA-DOX exhibits light-enhanced drug release under NIR laser irradiation. The combined dual-modal light-mediated therapy, by using GNR-PDA-MB [photodynamic/photothermal therapy (PDT/PTT)] and GNR-PDA-DOX (Chemo/PTT), is carried out and shows remarkable cancer cell killing efficiency in vitro and significant suppression of tumor growth in vivo, which are much more distinct than any single-modal therapeutic strategy. Conventional radiotherapy has a pivotal role in the treatment of glioblastoma; nevertheless, its clinical utility has been limited by radiation resistance. There is emerging evidence that upregulated heat shock protein A5 (HSPA5) in cancer cells maintains or restores the homeostasis of a cellular microenvironment and results in cancer resistance in various treatments. Zhu, Haitao et al describe a bioresponsive nanoplatform that can deliver a HSPA5 inhibitor (pifithrin-μ, PES) and radiosensitizer (gold nanosphere, AuNS), to expand the synergistic photothermal therapy and radiotherapy.143 The therapeutic effects of “chemotherapy + PTT”, “PTT + PDT”, and “radiotherapy + PTT” in GBM are discussed in the subsequent sections.
Chemotherapy + PTT
Multifunctional PDA-based NPs have recently been widely used for basic research on PTT combined with chemotherapy for GBM. This combination therapy takes advantage of the photothermal conversion efficiency of PDA and the accumulation and penetration of chemotherapeutic drug-loaded PDA-based NPs in the tumor tissue to combat and kill cancer cells. PEG is a water-soluble polymer with good biocompatibility. It is preferred by many researchers because PEG-modified PDA-based NPs can be loaded with various chemotherapeutic drugs, such as DOX and cisplatin. Currently, PEG-modified PDA-based NPs are widely used for basic research on GBM. The combination of chemotherapy and PTT has also yielded satisfactory results for GBM treatment (Figure 11).
PTT + PDT
Photothermal therapy and photodynamic therapy are both light-assisted treatments, so if these two phototherapy techniques can be effectively combined, the therapeutic effect may exceed the single treatment method and play a better effect. To date, only a few studies have reported the cases of combined photothermal therapy and photodynamic therapy based on PDA nanomaterials for glioma treatment. Huang, Xiaqin et al adopted a phototherapy-chemotherapy combination strategy based on targeted delivery of the near-infrared photosensitizer indocyanine green (ICG), photothermal conversion agent PDA, and tirapazamine (TPZ), a hypoxia-activated prodrug. Under laser irradiation, ICG consumption of oxygen and aggravated hypoxia in tumor sites can activate TPZ to damage DNA. In parallel, ICG produces reactive oxygen species which work in synergy with PDA to enhance phototherapeutic efficiency. Hybrid CaCO3/TPGS nanoparticles delivering ICG, PDA, and TPZ (ICG-PDA-TPZ NPs[indocyanine green-polydopamine- tirapazamine]) were designed for effective and safe cancer therapy. ICG-PDA-TPZ NPs showed significantly improved cellular uptake and accumulation in tumors. Furthermore, their results demonstrated that ICG-PDA-TPZ NPs showed intensive photodynamic and photothermal effects in vitro and in vivo, which synergized with TPZ in subcutaneous U87 malignant glioma growth and orthotopic B16F10 tumor inhibition, with negligible side effects. Thus, ICG-PDA-TPZ NPs could be an effective strategy for improvement of PDT (Table 2).138
 |
Table 2 The Application of PDA-Based NPs-PTT + PDT |
Radiotherapy + PTT
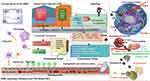
Clinically, radiotherapy (RT) is one of the cornerstones in the current treatment paradigm for GBM.157 However, little has changed in the management of GBM since the establishment of the current protocol in 2005, and the prognosis remains grim. Further, 50–70% of patients with malignant tumors require radiotherapy. GBM is resistant to radiotherapy; hence, a therapeutic modality for enhancing the effects of radiotherapy against tumor cells must be developed. Zhu et al designed and synthesized PES-Au@PDA NPs ((pifithrin-µ, PES-gold nanosphere-polydopamine)) to enhance radiotherapy and PTT of GBM. Their results showed that PES-Au@PDA specifically activates the proapoptotic unfolded protein response (UPR) cascade in vitro and in vivo, thereby significantly improving the efficiencies of both radiotherapy and PTT158 (Figure 12).
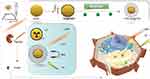 |
Figure 12 Schematic diagram of PES-Au@PDA for the synergistic photothermal treatment. Abbreviations: PES, pifithrin-µ; AuNS, gold nanospherent and radiotherapy of GBM. |
Conclusion
GBM is characterized by diffuse brain infiltration, active local recurrence, low cure rates, limited effectiveness of radiotherapy and some objective limitations of conventional treatment modalities. The main challenges encountered in GBM treatment include poor drug penetration, BBB, tumor barrier, tumor location, cellular infiltration, heterogeneity, and resistance to radiotherapy. Based on these challenges, the PDA applications in GBM treatment in recent years were summarized in this review. PDA-based NPs have good biocompatibility and biodegradability, high adhesion ability, reducibility and photothermal conversion properties, and can modify clinical first-line chemotherapeutic drugs. In other words, they can improve drug penetration and delivery rate, reduce marginal effects, and resistance to radiotherapy, increase control in different pH environments, and enhance antitumor activity. In addition, the combination of PTT and PDT based on PDA can also be used to kill tumor cells. However, the current research is in the experimental stage and has not yet entered the clinical trial stage. Although many studies have made progress and laid a solid foundation for a step-by-step attack on tumors, several problems must be addressed in terms of toxicity, size, composition, and efficiency of drug encapsulation to ensure the clinical application of PDA-based NPs. In addition, a broader understanding of the biological morphology of GBM and a disruption of tumor signaling pathways and possible tumor biomarkers may help in developing new NPs with more definite targeting, which will significantly improve the therapeutic efficacy. In recent years, the discovery of new markers enabled the functionalization of NPs to precisely target tumors. Nanotechnology is a new prospect for GBM treatment, and more comprehensive, effective, refined and individualized strategies are required. Several aspects must first be considered before conducting an in-depth research. Can PDA-based NPs drug loading specifically induce the apoptosis of glioma cells and inhibit cell growth and invasion in the actual clinical stage? Is it possible to investigate the effect of PDA drug loading on the glioma microenvironment in primary human glioma surgical specimens selected from patients with glioma? If the patient enters the clinical stage, what are his/her prognostic evaluation indicators? How can we achieve inflammatory factors (CRP, PCT, IL-6, TNF-α), immune correlation (CD3+, CD4+, CD4+/CD8+, IgG, IL-1), metabolic correlation (BMI, neuropeptide Y, albumin) and photothermal therapy in PDA in actual clinical patients? Does PTT burn the scalp? Even if it does not burn, how can it penetrate the hard skull? After penetrating the skull, how will the dura, pia mater, and arachnoid membrane be penetrated? Can we do PDA photothermal therapy immediately when the tumor is fully exposed during surgery? That is, surgical excision combined with PTT and PDT of intraoperative PDA. We believe that intraoperative tumor resection combined with PDA photothermal and photodynamic therapies and with postoperative PDA loading chemotherapy drugs for treatment, even if clinical trials are not possible, it is important to investigate these questions at least animals, along with the ability to rely on drug-loaded NPs to interfere with tumor signaling pathways and in the identification of new therapeutic targets.
Future Perspective
In recent years, targeting tumor sites and targeted immune cell nanoparticle drug systems have generated much interest among scientists. The tumor antigen is the key to waking up the body’s antitumor immune response and is the key immune therapy. However, although glioma-related antigen has been emphasized in several studies and is a difficulty in the present study, an increasing number of studies are focusing on the tumor with the constant appearance of a new nanometer technology. Many studies have confirmed that multiple signaling pathways play important biological functions in gliomas, including the initiation of malignant progression and other phenotypic gliomas in Hippo/YAP PI3K/AKT/mTOR miRNA WnT/β-catenin Notch, Hedgehog, TGF-β and other signaling pathways and the mechanism of action of the key enzymes. Nanotechnology-assembled YAP1 inhibitors combined with immunotherapy may become an effective target for glioma treatment in the future, while inhibiting PI3K/Akt/mTOR Shh WNT/β-catenin and HIF-1α can reduce the migration ability and drug resistance of tumor cells and improve glioma prognosis. Studies have analyzed the positive feedback regulation mechanism of Notch1 and Sox2, and Notch4 predicted the malignant degree of glioma, which not only can be used in the clinical treatment of glioma stem cells, but can also improve Notch. As an indicator of prognosis, this provides an exploratory attempt for glioma treatment. The combination of nano-loaded chemotherapy drugs, TMZ, and WnT/β-catenin inhibitors, can better improve the postoperative survival of GBM, which may be the target for future glioma treatment. Moreover, miRNA plays an important role in diagnosis and can provide antitumor effects with TMZ through nanoparticle delivery. In addition, nanotechnology can also be used to explore new diagnostic and prognostic biomarkers and highly effective molecular therapeutic targets. Nanodelivery drugs can also be used to block key factor activation pathways in the signaling pathway to limit the further development and progression of tumors. However, some aspects must be further explored. Firstly, tumor cells show obvious heterogeneity by recruiting various types of cells in the tumor microenvironment, and there are relatively few studies on signaling pathways and tumor heterogeneity. Second, although there have been various reported advances in the relationship between signaling pathway involvement and glioma, cross-talk between multiple signaling pathways makes it difficult to identify effective molecular targets for glioma treatment. Lastly and most importantly, tumor signal transduction is not caused by a single factor, but a variety of regulatory mechanisms, and the body’s immune system is very complex; hence, the present research strategy may be an efficient and accurate approach of treating glioma. The application of an organic or inorganic nanometer carrier or outside secret body combined with clinical drug use and adjuvant immunotherapy, such as monoclonal antibody targeting therapy, peptide vaccine, DC vaccine adoptive immunotherapy, and cytokine therapy, may be more efficient. In general, the PDA nanodrug delivery technology combined with immunotherapy has a very broad prospect for antitumor signaling pathways and immune regulation. However, more large-scale cohort studies and related molecular experiments are needed. We are confident that these studies will advance our understanding of glioma and lead to novel glioma treatments.
Acknowledgments
This study was supported by grants from the National Natural Science Foundation of China (No. 82172603) and the Natural Science Foundation of Jiangsu Province (No. BK20190241) and was supported by a grant from the Program《Nanoparticle Drug Carrier System for Glioma》of the Northern Jiangsu People’s Hospital of Jiangsu Province (NO.SBJC21009),《Improvement and clinical application of cervical 7 nerve transposition via cervical posterior approach in the treatment of central upper limb paralysis》of Project 333, The fifth phase of Yangzhou in 2019 (NO.BRA2019026),《The role of Neurod1 in neuronal reprogramming of NG2 cells in the repair of neural function in hemorrhagic stroke》of Yangzhou commission of health china (NO.H2018064).
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Brat DJ, Prayson RA, Ryken TC, Olson JJ. “Diagnosis of malignant glioma: role of neuropathology.”. J Neurooncol. 2008;89(3):287–311. doi:10.1007/s11060-008-9618-1
2. Cioffi G, Waite K, Kruchko C, et al. CBTRUS statistical report: primary brain and other central nervous system tumors diagnosed in the United States in 2013–2017. Neuro-Oncology. 2020;22(12):iv1–iv96. doi:10.1093/neuonc/noaa200
3. Barnholtz-Sloan JS, Ostrom QT, Cote D. “CBTRUS Statistical Report: primary brain and other central nervous system tumors diagnosed in the United States in 2010–2014.”. Neuro-Oncology. 2017;19(suppl_5):v1–v88. doi:10.1093/neuonc/nox158
4. Batash R, Asna N, Schaffer P, Francis N, Schaffer M. “Glioblastoma multiforme, diagnosis and treatment; recent literature review.”. Curr Med Chem. 2017;24(27):3002–3009. doi:10.2174/0929867324666170516123206
5. Alifieris C, Trafalis DT. “Glioblastoma multiforme: pathogenesis and treatment.”. Pharmacol Ther. 2015;152:63–82. doi:10.1016/j.pharmthera.2015.05.005
6. Wang L, Tang S, Yu Y, et al. “Intranasal delivery of temozolomide-conjugated gold nanoparticles functionalized with Anti-EphA3 for glioblastoma targeting.”. Mol Pharm. 2021;18(3):915–927. doi:10.1021/acs.molpharmaceut.0c00911
7. Silva GA. Nanotechnology applications and approaches for neuroregeneration and drug delivery to the central nervous system. Ann N Y Acad Sci. 2010;1199:221–230. doi:10.1111/j.1749-6632.2009.05361.x
8. Saeedi M, Eslamifar M, Khezri K, Dizaj SM. Applications of nanotechnology in drug delivery to the central nervous system. Biomed Pharmacother. 2019;111:666–675. doi:10.1016/j.biopha.2018.12.133
9. Glaser T, Han I, Wu L, Zeng X. Targeted nanotechnology in glioblastoma multiforme. Front Pharmacol. 2017;8:166. doi:10.3389/fphar.2017.00166
10. Guo X, Li Z, Liu S, et al. Studying the effect of PDA@CeO2 nanoparticles with antioxidant activity on the mechanical properties of cells. J Mater Chem B. 2021;9(44):9204–9212. doi:10.1039/d1tb01918j
11. Bolat G, Vural OA, Yaman YT, Abaci S. Polydopamine nanoparticles-assisted impedimetric sensor towards label-free lung cancer cell detection. C Material Biol Appli. 2021;119:111549. doi:10.1016/j.msec.2020.111549
12. Zeng Y, Zhang D, Wu M, et al. Lipid-AuNPs@PDA nanohybrid for MRI/CT imaging and photothermal therapy of hepatocellular carcinoma. ACS Appl Mater Interfaces. 2014;6(16):14266–14277. doi:10.1021/am503583
13. Ma X, Wang C, Dong Z, Hu C, Feng L. Lipid-coated CaCO3-PDA nanoparticles as a versatile nanocarrier to enable pH-responsive dual modal imaging-guided combination cancer therapy. J Mater Chem B. 2022;10(21):4096–4104. doi:10.1039/d2tb00022a
14. Bao B, Tong L, Xu Y, et al. Mussel-inspired functionalization of semiconducting polymer nanoparticles for amplified photoacoustic imaging and photothermal therapy. Nanoscale. 2019;11(31):14727–14733. doi:10.1039/c9nr03490k
15. Pu Y, Zhu Y, Qiao Z, et al. A Gd-doped polydopamine (PDA)-based theranostic nanoplatform as a strong MR/PA dual-modal imaging agent for PTT/PDT synergistic therapy. J Mater Chem B. 2021;9(7):1846–1857. doi:10.1039/d0tb02725a
16. Zhao M, van Straten D, Broekman M, Préat V, Schiffelers RM. Nanocarrier-based drug combination therapy for glioblastoma. Theranostics. 2020;10(3):1355–1372. doi:10.7150/thno.38147
17. Cao H, Jiang B, Yang Y, et al. Cell membrane covered polydopamine nanoparticles with two-photon absorption for precise photothermal therapy of cancer. J Colloid Interface Sci. 2021;604:596–603. doi:10.1016/j.jcis.2021.07.004
18. Waite JH, Tanzer ML. Polyphenolic substance of Mytilus edulis: novel adhesive containing l-dopa and hydroxyproline. Science. 1981;212(4498):1038–1040. doi:10.1126/science.212.4498.1038
19. Lin Q, Gourdon D, Sun C, et al. Adhesion mechanisms of the mussel foot proteins mfp-1 and mfp-3. Proc Natl Acad Sci U S A. 2007;104(10):3782–3786. doi:10.1073/pnas.0607852104
20. Lee H, Dellatore SM, Miller WM, Messersmith PB. Mussel-inspired surface chemistry for multifunctional coatings. Science. 2007;318(5849):426–430. doi:10.1126/science.1147241
21. Li H, Jia Y, Peng H, Li J. Recent developments in dopamine-based materials for cancer diagnosis and therapy. Adv Colloid Interface Sci. 2018;252:1–20. doi:10.1016/j.cis.2018.01.001
22. Batul R, Tamanna T, Khaliq A, Yu A. Recent progress in the biomedical applications of polydopamine nanostructures. Biomaterials Sci. 2017;5(7):1204–1229. doi:10.1039/c7bm00187h
23. Madhurakkat Perikamana SK, Lee J, Lee YB, et al. Materials from mussel-inspired chemistry for cell and tissue engineering applications. Biomacromolecules. 2015;16(9):2541–2555. doi:10.1021/acs.biomac.5b00852
24. Liu M, Zeng G, Wang K, et al. Recent developments in polydopamine: an emerging soft matter for surface modification and biomedical applications. Nanoscale. 2016;8(38):16819–16840. doi:10.1039/c5nr09078d
25. Liu Y, Ai K, Lu L. Polydopamine and its derivative materials: synthesis and promising applications in energy, environmental, and biomedical fields. Chem Rev. 2014;114(9):5057–5115. doi:10.1021/cr400407a
26. Zhang M, Zhang L, Chen Y, Li L, Su Z, Wang C. Precise synthesis of unique polydopamine/mesoporous calcium phosphate hollow Janus nanoparticles for imaging-guided chemo-photothermal synergistic therapy. Chemical Sci. 2017;8(12):8067–8077. doi:10.1039/c7sc03521g
27. Cheng W, Zeng X, Chen H, et al. Versatile polydopamine platforms: synthesis and promising applications for surface modification and advanced nanomedicine. ACS nano. 2019;13(8):8537–8565. doi:10.1021/acsnano.9b04436
28. Gratton SE, Ropp PA, Pohlhaus PD, et al. The effect of particle design on cellular internalization pathways. Proc Natl Acad Sci U S A. 2008;105(33):11613–11618. doi:10.1073/pnas.0801763105
29. Zhang YR, Lin R, Li HJ, He WL, Du JZ, Wang J. Strategies to improve tumor penetration of nanomedicines through nanoparticle design. Nanomed Nanobiotechnol. 2019;11(1):e1519. doi:10.1002/wnan.1519
30. Caster JM, Yu SK, Patel AN, et al. Effect of particle size on the biodistribution, toxicity, and efficacy of drug-loaded polymeric nanoparticles in chemoradiotherapy. Nanomedicine. 2017;13(5):1673–1683. doi:10.1016/j.nano.2017.03.002
31. Jędrzak A, Grześkowiak BF, Golba K, et al. Magnetite nanoparticles and spheres for chemo- and photothermal therapy of hepatocellular carcinoma in vitro. Int J Nanomedicine. 2020;15:7923–7936. doi:10.2147/IJN.S257142
32. Champion JA, Champion JA, Walker A, Mitragotri S. Role of particle size in phagocytosis of polymeric microspheres. Pharm Res. 2008;25(8):1815–1821. doi:10.1007/s11095-008-9562-y
33. Rejman J, Oberle V, Zuhorn IS, et al. Size-dependent internalization of particles via the pathways of clathrin- and caveolae-mediated endocytosis. Biochem J. 2004;377(1):159–169. doi:10.1042/BJ20031253
34. Perrault SD, Walkey C, Jennings T, Fischer HC, Chan WC. Mediating tumor targeting efficiency of nanoparticles through design. Nano Lett. 2009;9(5):1909–1915. doi:10.1021/nl900031y
35. Wang AZ, Langer R, Farokhzad OC. Nanoparticle delivery of cancer drugs. Annu Rev Med. 2012;63:185–198. doi:10.1146/annurev-med-040210-162544
36. Chen Q, Shan X, Shi S, et al. Tumor microenvironment-responsive polydopamine-based core/shell nanoplatform for synergetic theranostics. J Mater Chem B. 2020;8(18):4056–4066. doi:10.1039/d0tb00248h
37. Ho CC, Ding SJ. The pH-controlled nanoparticles size of polydopamine for anti-cancer drug delivery. J Mater Sci Mater Med. 2013;24(10):2381–2390. doi:10.1007/s10856-013-4994-2
38. Ku SH, Ryu J, Hong SK, Lee H, Park CB. General functionalization route for cell adhesion on non-wetting surfaces. Biomaterials. 2010;31(9):2535–2541. doi:10.1016/j.biomaterials.2009.12.020
39. Brieger K, Schiavone S, Miller FJ, Krause KH. Reactive oxygen species: from health to disease. Swiss Med Wkly. 2012;142:w13659. doi:10.4414/smw.2012.13659
40. Li S, Wang H, Young M, Xu F, Cheng G, Cong H. Properties of electropolymerized dopamine and its analogues. Langmuir. 2019;35(5):1119–1125. doi:10.1021/acs.langmuir.8b01444
41. Farokhi M, Mottaghitalab F, Saeb MR, Thomas S. Functionalized theranostic nanocarriers with bio-inspired polydopamine for tumor imaging and chemo-photothermal therapy. J Control Release. 2019;309:203–219. doi:10.1016/j.jconrel.2019.07.036
42. Jiang Q, Pan M, Hu J, et al. Regulation of redox balance using a biocompatible nanoplatform enhances phototherapy efficacy and suppresses tumor metastasis. Chemical Sci. 2020;12(1):148–157. doi:10.1039/d0sc04983b
43. Liu S, Pan J, Liu J, et al. Dynamically PEGylated and borate-coordination-polymer-coated polydopamine nanoparticles for synergetic tumor-targeted, chemo-photothermal combination therapy. Small. 2018;14(13):e1703968. doi:10.1002/smll.201703968
44. Deng Z, Shang B, Peng B. Polydopamine based colloidal materials: synthesis and applications. Chemical Record. 2018;18(4):410–432. doi:10.1002/tcr.201700051
45. Wojtkowiak JW, Verduzco D, Schramm KJ, Gillies RJ. Drug resistance and cellular adaptation to tumor acidic pH microenvironment. Mol Pharm. 2011;8(6):2032–2038. doi:10.1021/mp200292c
46. Anderson NM, Simon MC. The tumor microenvironment. Current Biol. 2020;30(16):R921–R925. doi:10.1016/j.cub.2020.06.081
47. Boedtkjer E, Pedersen SF. The acidic tumor microenvironment as a driver of cancer. Annu Rev Physiol. 2020;82:103–126. doi:10.1146/annurev-physiol-021119-034627
48. Vaupel P, Kallinowski F, Okunieff P. Blood flow, oxygen and nutrient supply, and metabolic microenvironment of human tumors: a review. Cancer Res. 1989;49(23):6449–6465.
49. Mellman I, Fuchs R, Helenius A. Acidification of the endocytic and exocytic pathways. Annu Rev Biochem. 1986;55:663–700. doi:10.1146/annurev.bi.55.070186.003311
50. Yu B, Liu J, Liu S, Zhou F. Pdop layer exhibiting zwitterionicity: a simple electrochemical interface for governing ion permeability. Chem Comm. 2010;46(32):5900–5902. doi:10.1039/c0cc00596g
51. Zheng X, Zhang J, Wang J, Xueqiang Q, Jessica M, Cai K. Polydopamine coatings in confined nanopore space: toward improved retention and release of hydrophilic cargo. J Phys Chem C. 2015;119(43):24512–24521. doi:10.1021/acs.jpcc.5b08558
52. Yang B, Chen Y, Shi J. Reactive oxygen species (ROS)-based nanomedicine. Chem Rev. 2019;119(8):4881–4985. doi:10.1021/acs.chemrev.8b00626
53. Zhong H, Huang PY, Yan P, et al. Versatile nanodrugs containing glutathione and heme oxygenase 1 inhibitors enable suppression of antioxidant defense system in a two-pronged manner for enhanced photodynamic therapy. Adv Healthcare Mater. 2021;10(19):e2100770. doi:10.1002/adhm.202100770
54. Kuppusamy P, Li H, Ilangovan G, et al. Noninvasive imaging of tumor redox status and its modification by tissue glutathione levels. Cancer Res. 2002;62(1):307–312.
55. Yuan Z, Lin C, He Y, et al. Near-infrared light-triggered nitric-oxide-enhanced photodynamic therapy and low-temperature photothermal therapy for biofilm elimination. ACS nano. 2020;14(3):3546–3562. doi:10.1021/acsnano.9b09871
56. Gao G, Jiang YW, Jia HR, Wu FG. Near-infrared light-controllable on-demand antibiotics release using thermo-sensitive hydrogel-based drug reservoir for combating bacterial infection. Biomaterials. 2019;188:83–95. doi:10.1016/j.biomaterials.2018.09.045
57. Van Lehn RC, Sing CE, Chen H, Alexander-Katz A. Multidimensional targeting: using physical and chemical forces in unison. Curr Pharm Biotechnol. 2010;11(4):320–332. doi:10.2174/138920110791233299
58. Wang Z, Chen Y, Zhang H, et al. Mitochondria-targeting polydopamine nanocomposites as chemophotothermal therapeutics for cancer. Bioconjug Chem. 2018;29(7):2415–2425. doi:10.1021/acs.bioconjchem.8b00325
59. Hu X, Lu Y, Shi X, Yao T, Dong C, Shi S. Integrating in situ formation of nanozymes with mesoporous polydopamine for combined chemo, photothermal and hypoxia-overcoming photodynamic therapy. Chem Comm. 2019;55(98):14785–14788. doi:10.1039/c9cc07125c
60. Zhang L, Yang P, Guo R, Sun J, Xie R, Yang W. Multifunctional mesoporous polydopamine with hydrophobic paclitaxel for photoacoustic imaging-guided chemo-photothermal synergistic therapy. Int J Nanomedicine. 2019;14:8647–8663. doi:10.2147/IJN.S218632
61. Zhang T, Jiang Z, Xve T, et al. One-pot synthesis of hollow PDA@DOX nanoparticles for ultrasound imaging and chemo-thermal therapy in breast cancer. Nanoscale. 2019;11(45):21759–21766. doi:10.1039/c9nr05671h
62. Du C, Ding Y, Qian J, Zhang R, Dong CM. Achieving traceless ablation of solid tumors without recurrence by mild photothermal-chemotherapy of triple stimuli-responsive polymer-drug conjugate nanoparticles. J Mater Chem B. 2019;7(3):415–432. doi:10.1039/c8tb02432d
63. Du C, Qian J, Zhou L, Su Y, Zhang R, Dong CM. Biopolymer-drug conjugate nanotheranostics for multimodal imaging-guided synergistic cancer photothermal-chemotherapy. ACS Appl Mater Interfaces. 2017;9(37):31576–31588. doi:10.1021/acsami.7b10163
64. Luiz MT, Delello D, Filippo L, et al. Highlights in targeted nanoparticles as a delivery strategy for glioma treatment. Int J Pharm. 2021;604:120758. doi:10.1016/j.ijpharm.2021.120758
65. Dong Z, Gong H, Gao M, et al. Polydopamine nanoparticles as a versatile molecular loading platform to enable imaging-guided cancer combination therapy. Theranostics. 2016;6(7):1031–1042. doi:10.7150/thno.14431
66. Attia MF, Anton N, Wallyn J, Omran Z, Vandamme TF. An overview of active and passive targeting strategies to improve the nanocarriers efficiency to tumour sites. J Pharm Pharmacol. 2019;71(8):1185–1198. doi:10.1111/jphp.13098
67. Ding F, Gao X, Huang X, et al. Polydopamine-coated nucleic acid nanogel for siRNA-mediated low-temperature photothermal therapy. Biomaterials. 2020;245:119976. doi:10.1016/j.biomaterials.2020.119976
68. Dai Y, Xu C, Sun X, Chen X. Nanoparticle design strategies for enhanced anticancer therapy by exploiting the tumour microenvironment. Chem Soc Rev. 2017;46(12):3830–3852. doi:10.1039/c6cs00592f
69. Cao H, Yang Y, Liang M, et al. Pt@polydopamine nanoparticles as nanozymes for enhanced photodynamic and photothermal therapy. Chem Comm. 2021;57(2):255–258. doi:10.1039/d0cc07355e
70. Gallego L, Ceña V. Nanoparticle-mediated therapeutic compounds delivery to glioblastoma. Expert Opin Drug Deliv. 2020;17(11):1541–1554. doi:10.1080/17425247.2020.1810015
71. Tsai YC, Vijayaraghavan P, Chiang WH, et al. Targeted delivery of functionalized upconversion nanoparticles for externally triggered photothermal/photodynamic therapies of brain glioblastoma. Theranostics. 2018;8(5):1435–1448. doi:10.7150/thno.22482
72. Hirschberg H, Madsen SJ. Cell mediated photothermal therapy of brain tumors. J Neuroimmune Pharmacol. 2017;12(1):99–106. doi:10.1007/s11481-016-9690-9
73. Xu H, Han Y, Zhao G, et al. Hypoxia-responsive lipid-polymer nanoparticle-combined imaging-guided surgery and multitherapy strategies for glioma. ACS Appl Mater Interfaces. 2020;12(47):52319–52328. doi:10.1021/acsami.0c12971
74. Zhang H, Sun Y, Huang R, Cang H, Cai Z, Sun B. pH-sensitive prodrug conjugated polydopamine for NIR-triggered synergistic chemo-photothermal therapy. Eur J Pharm Biopharm. 2018;128:260–271. doi:10.1016/j.ejpb.2018.05.013
75. Chen F, Xing Y, Wang Z, Zheng X, Zhang J, Cai K. Nanoscale polydopamine (PDA) meets π-π interactions: an interface-directed coassembly approach for mesoporous nanoparticles. Langmuirs. 2016;32(46):12119–12128. doi:10.1021/acs.langmuir.6b03294
76. Xing Y, Zhang J, Chen F, Liu J, Cai K. Mesoporous polydopamine nanoparticles with co-delivery function for overcoming multidrug resistance via synergistic chemo-photothermal therapy. Nanoscale. 2017;9(25):8781–8790. doi:10.1039/c7nr01857f
77. El Yakhlifi S, Ball V. Polydopamine as a stable and functional nanomaterial. Colloids Surf B Biointerfaces. 2020;186:110719. doi:10.1016/j.colsurfb.2019.110719
78. Mrówczyński R. Polydopamine-based multifunctional (nano) materials for cancer therapy. ACS Appl Mater Interfaces. 2018;10(9):7541–7561. doi:10.1021/acsami.7b08392
79. Tran HQ, Bhave M, Xu G, Sun C, Yu A. Synthesis of polydopamine hollow capsules via a polydopamine mediated silica water dissolution process and its application for enzyme encapsulation. Front Chem. 2019;7:468. doi:10.3389/fchem.2019.00468
80. Zhuang H, Su H, Bi X, et al. Polydopamine nanocapsule: a theranostic agent for photoacoustic imaging and chemo-photothermal synergistic therapy. ACS Biomater Sci Eng. 2017;3(8):1799–1808. doi:10.1021/acsbiomaterials.7b00260
81. Jinsong D, Wang L, Han X, Dou J, Jiang X, Yuan J. Polydopamine/keratin complexes as gatekeepers of mesoporous silica nanoparticles for pH and GSH dual responsive drug delivery. Mater Lett. 2021;293:129676. doi:10.1016/j.matlet.2021.129676
82. Bertrand N, Wu J, Xu X, Kamaly N, Farokhzad OC. Cancer nanotechnology: the impact of passive and active targeting in the era of modern cancer biology. Adv Drug Deliv Rev. 2014;66:2–25. doi:10.1016/j.addr.2013.11.009
83. Wu M, Zhong C, Zhang Q, et al. pH-responsive delivery vehicle based on RGD-modified polydopamine-paclitaxel-loaded poly (3-hydroxybutyrate-co-3-hydroxyvalerate) nanoparticles for targeted therapy in hepatocellular carcinoma. J Nanobiotechnology. 2021;19(1):39. doi:10.1186/s12951-021-00783-x
84. Li X, Chen Q, Zhou Y, et al. Hyaluronic acid-methotrexate conjugates coated magnetic polydopamine nanoparticles for multimodal imaging-guided multistage targeted chemo-photothermal therapy. Mol Pharm. 2018;15(9):4049–4062. doi:10.1021/acs.molpharmaceut.8b00473
85. Wang Z, Wang G, Kang T, et al. BiVO4/Fe3O4@polydopamine superparticles for tumor multimodal imaging and synergistic therapy. J Nanobiotechnology. 2021;19(1):90. doi:10.1186/s12951-021-00802-x
86. Wang X, Zhang J, Wang Y, et al. Multi-responsive photothermal-chemotherapy with drug-loaded melanin-like nanoparticles for synergetic tumor ablation. Biomaterials. 2016;81:114–124. doi:10.1016/j.biomaterials.2015.11.037
87. Ruan J, Liu H, Chen B, et al. Interfacially engineered ZnxMn1-xS@polydopamine hollow nanospheres for glutathione depleting photothermally enhanced chemodynamic therapy. ACS nano. 2021;15(7):11428–11440. doi:10.1021/acsnano.1c01077
88. Ding M, Miao Z, Zhang F, et al. Catalytic rhodium (Rh)-based (mesoporous polydopamine) MPDA nanoparticles with enhanced phototherapeutic efficiency for overcoming tumor hypoxia. Biomaterials Sci. 2020;8(15):4157–4165. doi:10.1039/d0bm00625d
89. Guan Q, Guo R, Huang S, et al. Mesoporous polydopamine carrying sorafenib and SPIO nanoparticles for MRI-guided ferroptosis cancer therapy. J Control Release. 2020;320:392–403. doi:10.1016/j.jconrel.2020.01.048
90. Tian Y, Younis MR, Tang Y, et al. Dye-loaded mesoporous polydopamine nanoparticles for multimodal tumor theranostics with enhanced immunogenic cell death. J Nanobiotechnology. 2021;19(1):365. doi:10.1186/s12951-021-01109-7
91. Wu Y, Huang Y, Tu C, et al. A mesoporous polydopamine nanoparticle enables highly efficient manganese encapsulation for enhanced MRI-guided photothermal therapy. Nanoscale. 2021;13(13):6439–6446. doi:10.1039/d1nr00957e
92. Cheng FF, Zhang JJ, Xu F, Hu LH, Abdel-Halim ES, Zhu JJ. pH-sensitive polydopamine nanocapsules for cell imaging and drug delivery based on folate receptor targeting. J Biomed Nanotechnol. 2013;9(7):1155–1163. doi:10.1166/jbn.2013.1611
93. Cui J, Yan Y, Such GK, et al. Immobilization and intracellular delivery of an anticancer drug using mussel-inspired polydopamine capsules. Biomacromolecules. 2012;13(8):2225–2228. doi:10.1021/bm300835r
94. Liu Y, Wei C, Lin A, et al. Responsive functionalized MoSe2 nanosystem for highly efficient synergistic therapy of breast cancer. Colloids Surf B Biointerfaces. 2020;189:110820. doi:10.1016/j.colsurfb.2020.110820
95. Lin X, Cao Y, Li J, et al. Folic acid-modified Prussian blue/polydopamine nanoparticles as an MRI agent for use in targeted chemo/photothermal therapy. Biomaterials Sci. 2019;7(7):2996–3006. doi:10.1039/c9bm00276f
96. Xi J, Da L, Yang C, et al. Mn2+-coordinated PDA@DOX/PLGA nanoparticles as a smart theranostic agent for synergistic chemo-photothermal tumor therapy. Int J Nanomedicine. 2017;12:3331–3345. doi:10.2147/IJN.S132270
97. Shao M, Chang C, Liu Z, et al. Polydopamine coated hollow mesoporous silica nanoparticles as pH-sensitive nanocarriers for overcoming multidrug resistance. B Biointerfaces. 2019;183:110427. doi:10.1016/j.colsurfb.2019.110427
98. Thorley AJ, Tetley TD. New perspectives in nanomedicine. Pharmacol Ther. 2013;140(2):176–185. doi:10.1016/j.pharmthera.2013.06.008
99. Wei Q-Y, Xu YM, Lau AT. Recent progress of nanocarrier-based therapy for solid malignancies. Cancers. 2020;28(12):2783. doi:10.3390/cancers12102783
100. Pérez-Herrero E, Alberto F-M. Advanced targeted therapies in cancer: drug nanocarriers, the future of chemotherapy. Eur J Pharm Biopharm. 2015;93:52–79. doi:10.1016/j.ejpb.2015.03.018
101. Groothuis DR. The blood-brain and blood-tumor barriers: a review of strategies for increasing drug delivery. Neuro-Oncology. 2000;2(1):45–59. doi:10.1093/neuonc/2.1.45
102. Liebner S, Fischmann A, Rascher G, et al. Claudin-1 and claudin-5 expression and tight junction morphology are altered in blood vessels of human glioblastoma multiforme. Acta Neuropathol. 2000;100(3):323–331. doi:10.1007/s004010000180
103. Li M, Deng H, Peng H, Wang Q. Functional nanoparticles in targeting glioma diagnosis and therapies. J Nanosci Nanotechnol. 2014;14(1):415–432. doi:10.1166/jnn.2014.8757
104. Argaw AT, Zhang Y, Snyder BJ, et al. IL-1beta regulates blood-brain barrier permeability via reactivation of the hypoxia-angiogenesis program. J Immunol. 2006;177(8):5574–5584. doi:10.4049/jimmunol.177.8.5574
105. Zhang ZG, Zhang L, Jiang Q, et al. VEGF enhances angiogenesis and promotes blood-brain barrier leakage in the ischemic brain. J Clin Invest. 2000;106(7):829–838. doi:10.1172/JCI9369
106. Schlageter KE, Molnar P, Lapin GD, Groothuis DR. Microvessel organization and structure in experimental brain tumors: microvessel populations with distinctive structural and functional properties. Microvasc Res. 1999;58(3):312–328. doi:10.1006/mvre.1999.2188
107. Liu Y, Lu W. Recent advances in brain tumor-targeted nano-drug delivery systems. Expert Opin Drug Deliv. 2012;9(6):671–686. doi:10.1517/17425247.2012.682726
108. Gaoe H, Pang Z, Pan S, et al. Anti-glioma effect and safety of docetaxel-loaded nanoemulsion. Arch Pharm Res. 2012;35(2):333–341. doi:10.1007/s12272-012-0214-8
109. Karim R, Palazzo C, Evrard B, Piel G. Nanocarriers for the treatment of glioblastoma multiforme: current state-of-The-art. J Control Release. 2016;227:23–37. doi:10.1016/j.jconrel.2016.02.026
110. Schiffer D, Annovazzi L, Caldera V, Mellai M. On the origin and growth of gliomas. Anticancer Res. 2010;30(6):1977–1998.
111. Allhenn D, Boushehri MA, Lamprecht A. Drug delivery strategies for the treatment of malignant gliomas. Int J Pharm. 2012;436(1–2):299–310. doi:10.1016/j.ijpharm.2012.06.025
112. Zhang TT, Li W, Meng G, Wang P, Liao W. Strategies for transporting nanoparticles across the blood-brain barrier. Biomaterials Sci. 2016;4(2):219–229. doi:10.1039/c5bm00383k
113. Muntoni E, Martina K, Marini E, et al. Methotrexate-loaded solid lipid nanoparticles: protein functionalization to improve brain biodistribution. Pharmaceutics. 2019;11(2):65. doi:10.3390/pharmaceutics11020065
114. Das RP, Gandhi VV, Singh BG, Kunwar A. Passive and active drug targeting: role of nanocarriers in rational design of anticancer formulations. Curr Pharm Des. 2019;25(28):3034–3056. doi:10.2174/1381612825666190830155319
115. Akhter MH, Rizwanullah M, Ahmad J, et al. “Nanocarriers in advanced drug targeting: setting novel paradigm in cancer therapeutics.”. Artif Cells Nanomed Biotechnol. 2018;46(5):873–884. doi:10.1080/21691401.2017.1366333
116. Akhter MH, Rizwanullah M, Ahmad J, et al. Molecular targets and nanoparticulate systems designed for the improved therapeutic intervention in glioblastoma multiforme. Drug Res. 2021;71(3):122–137. doi:10.1055/a-1296-7870
117. Kang H, Rho S, Stiles WR, et al. Size-dependent EPR effect of polymeric nanoparticles on tumor targeting. Adv Healthcare Mater. 2020;9(1):e1901223. doi:10.1002/adhm.201901223
118. An P, Fan F, Gu D, Gao Z, Hossain A, Sun B. Photothermal-reinforced and glutathione-triggered in Situ cascaded nanocatalytic therapy. J Control Release. 2020;321:734–743. doi:10.1016/j.jconrel.2020.03.007
119. Sun D, Zhou S, Gao W. What went wrong with anticancer nanomedicine design and how to make it right. ACS nano. 2020;14(10):12281–12290. doi:10.1021/acsnano.9b09713
120. Maeda H, Wu J, Sawa T, Matsumura Y, Hori K. Tumor vascular permeability and the EPR effect in macromolecular therapeutics: a review. J Control Release. 2000;65(1–2):271–284. doi:10.1016/s0168-3659(99)00248-5
121. Li J, Zhao J, Tan T, et al. Nanoparticle drug delivery system for glioma and its efficacy improvement strategies: a comprehensive review. Int J Nanomedicine. 2020;15:2563–2582. doi:10.2147/IJN.S243223
122. Zhou Z, Sun T, Jiang C. Recent advances on drug delivery nanocarriers for cerebral disorders. Biomed Mater. 2021;16(2):024104. doi:10.1088/1748-605X/abdc97
123. Umlauf BJ, Shusta EV. Exploiting BBB disruption for the delivery of nanocarriers to the diseased CNS. Curr Opin Biotechnol. 2019;60:146–152. doi:10.1016/j.copbio.2019.01.013
124. Zhou Y, Peng Z, Seven ES, Leblanc RM. Crossing the blood-brain barrier with nanoparticles. J Control Release. 2018;270:290–303. doi:10.1016/j.jconrel.2017.12.015
125. Gao Y, Wang R, Zhao L, Liu A. Natural polymeric nanocarriers in malignant glioma drug delivery and targeting. J Drug Target. 2021;29(9):960–973. doi:10.1080/1061186X.2021.1904250
126. Ortiz R, Cabeza L, Perazzoli G, et al. Nanoformulations for glioblastoma multiforme: a new hope for treatment. Future Med Chem. 2019;11(18):2459–2480. doi:10.4155/fmc-2018-0521
127. Zhang H, Tian X, Zu G, et al. Development of curcumin-loaded zein nanoparticles for transport across the blood-brain barrier and inhibition of glioblastoma cell growth. Biomaterials Sci. 2021;9(21):7092–7103. doi:10.1039/d0bm01536a
128. Chouleur T, Tremblay ML, Bikfalvi A. Mechanisms of invasion in glioblastoma. Curr Opin Oncol. 2020;32(6):631–639. doi:10.1097/CCO.0000000000000679
129. Fabian C, Han M, Bjerkvig R, Niclou SP. Novel facets of glioma invasion. Int Rev Cell Mol Biol. 2021;360:33–64. doi:10.1016/bs.ircmb.2020.08.001
130. Park H, Saravanakumar G, Kim J, Lim J, Kim WJ. Tumor microenvironment sensitive nanocarriers for bioimaging and therapeutics. Adv Healthcare Mater. 2021;10(5):e2000834. doi:10.1002/adhm.202000834
131. Martin JD, Panagi M, Wang C, et al. Dexamethasone increases cisplatin-loaded nanocarrier delivery and efficacy in metastatic breast cancer by normalizing the tumor microenvironment. ACS nano. 2019;13(6):6396–6408. doi:10.1021/acsnano.8b07865
132. Martin JD, Cabral H, Stylianopoulos T, et al. Improving cancer immunotherapy using nanomedicines: progress, opportunities and challenges. Clin Oncol. 2020;17(4):251–266. doi:10.1038/s41571-019-0308-z
133. Li B, Tang M. Research progress of nanoparticle toxicity signaling pathway. Life Sci. 2020;263:118542. doi:10.1016/j.lfs.2020.118542
134. Meng X, Zhao Y, Han B, et al. Dual functionalized brain-targeting nanoinhibitors restrain temozolomide-resistant glioma via attenuating EGFR and MET signaling pathways. Nat Commun. 2020;11(1):594. doi:10.1038/s41467-019-14036-x
135. Játiva P, Ceña V. Use of nanoparticles for glioblastoma treatment: a new approach. Nanomedicine. 2017;12(20):2533–2554. doi:10.2217/nnm-2017-0223
136. Choi S, Yu Y, Grimmer MR, Wahl M, Chang SM, Costello JF. Temozolomide-associated hypermutation in gliomas. Neuro-Oncology. 2018;20(10):1300–1309. doi:10.1093/neuonc/noy016
137. Sasikala AR, GhavamiNejad A, Unnithan AR, et al. A smart magnetic nanoplatform for synergistic anticancer therapy: manoeuvring mussel-inspired functional magnetic nanoparticles for pH responsive anticancer drug delivery and hyperthermia. Nanoscale. 2015;7(43):18119–18128. doi:10.1039/c5nr05844a
138. Huang X, Wu J, He M, et al. Combined cancer chemo-photodynamic and photothermal therapy based on ICG/PDA/TPZ-loaded nanoparticles. Mol Pharm. 2019;16(5):2172–2183. doi:10.1021/acs.molpharmaceut.9b00119
139. Tang XL, Jing F, Lin BL, et al. pH-responsive magnetic mesoporous silica-based nanoplatform for synergistic photodynamic therapy/chemotherapy. ACS Appl Mater Interfaces. 2018;10(17):15001–15011. doi:10.1021/acsami.7b19797
140. Tang JH, Yang L, Chen JX, et al. Bortezomib inhibits growth and sensitizes glioma to temozolomide (TMZ) via down-regulating the FOXM1-Survivin axis. Cancer Commun. 2019;39(1):81. doi:10.1186/s40880-019-0424-2
141. Zhang P, Tang M, Huang Q, et al. Combination of 3-methyladenine therapy and Asn-Gly-Arg (NGR)-modified mesoporous silica nanoparticles loaded with temozolomide for glioma therapy in vitro. Biochem Biophys Res Commun. 2019;509(2):549–556. doi:10.1016/j.bbrc.2018.12.158
142. Wang S, Zhao X, Wang S, Qian J, He S. Biologically inspired polydopamine capped gold nanorods for drug delivery and light-mediated cancer therapy. ACS Appl Mater Interfaces. 2016;8(37):24368–24384. doi:10.1021/acsami.6b05907
143. Wang Z, Wang L, Prabhakar N, et al. CaP coated mesoporous polydopamine nanoparticles with responsive membrane permeation ability for combined photothermal and siRNA therapy. Acta Biomaterial. 2019;86:416–428. doi:10.1016/j.actbio.2019.01.002
144. Ouyang X, Wang X, Kraatz HB, et al. A Trojan horse biomimetic delivery strategy using mesenchymal stem cells for PDT/PTT therapy against lung melanoma metastasis. Biomaterials Sci. 2020;8(4):1160–1170. doi:10.1039/c9bm01401b
145. Li Y, Jiang C, Zhang D, et al. Targeted polydopamine nanoparticles enable photoacoustic imaging guided chemo-photothermal synergistic therapy of tumor. Acta Biomaterial. 2017;47:124–134. doi:10.1016/j.actbio.2016.10.010
146. Hu D, Liu C, Song L, et al. Indocyanine green-loaded polydopamine-iron ions coordination nanoparticles for photoacoustic/magnetic resonance dual-modal imaging-guided cancer photothermal therapy. Nanoscale. 2016;8(39):17150–17158. doi:10.1039/c6nr05502h
147. Hu H, Yang Q, Baroni S, Yang H, Aime S, Steinmetz NF. Polydopamine-decorated tobacco mosaic virus for photoacoustic/magnetic resonance bimodal imaging and photothermal cancer therapy. Nanoscale. 2019;11(19):9760–9768. doi:10.1039/c9nr02065a
148. Li N, Li T, Hu C, Lei X, Zuo Y, Han H. Targeted near-infrared fluorescent turn-on nanoprobe for activatable imaging and effective phototherapy of cancer cells. ACS Appl Mater Interfaces. 2016;8(24):15013–15023. doi:10.1021/acsami.5b02037
149. Sun Y, Chen H, Liu G, Ma L, Wang Z. The controllable growth of ultrathin MnO2 on polydopamine nanospheres as a single nanoplatform for the MRI-guided synergistic therapy of tumors. J Mater Chem B. 2019;7(45):7152–7161. doi:10.1039/c9tb02002k
150. Zhao X, Qi T, Kong C, et al. Photothermal exposure of polydopamine-coated branched Au-Ag nanoparticles induces cell cycle arrest, apoptosis, and autophagy in human bladder cancer cells. Int J Nanomedicine. 2018;13:6413–6428. doi:10.2147/IJN.S174349
151. Zeng J, Shi D, Gu Y, et al. Injectable and near-infrared-responsive hydrogels encapsulating dopamine-stabilized gold nanorods with long photothermal activity controlled for tumor therapy. Biomacromolecules. 2019;20(9):3375–3384. doi:10.1021/acs.biomac.9b00600
152. Huang C, Zhang Z, Guo Q, et al. A dual-model imaging theragnostic system based on mesoporous silica nanoparticles for enhanced cancer phototherapy. Adv Healthcare Mater. 2019;8(19):e1900840. doi:10.1002/adhm.201900840
153. Li X, Jiang M, Zeng S, Liu H. Polydopamine coated multifunctional lanthanide theranostic agent for vascular malformation and tumor vessel imaging beyond 1500 nm and imaging-guided photothermal therapy. Theranostics. 2019;9(13):3866–3878. doi:10.7150/thno.31864
154. Feng J, Yu W, Xu Z, Wang F. An intelligent ZIF-8-gated polydopamine nanoplatform for in vivo cooperatively enhanced combination phototherapy. Chemical Sci. 2020;11(6):1649–1656. doi:10.1039/c9sc06337d
155. Yang JC, Chen Y, Li YH, Yin XB. Magnetic Resonance imaging-guided multi-drug chemotherapy and photothermal synergistic therapy with pH and NIR-stimulation release. ACS Appl Mater Interfaces. 2017;9(27):22278–22288. doi:10.1021/acsami.7b06105
156. Xing Y, Ding T, Wang Z, et al. Temporally controlled photothermal/photodynamic and combined therapy for overcoming multidrug resistance of cancer by polydopamine nanoclustered micelles. ACS Appl Mater Interfaces. 2019;11(15):13945–13953. doi:10.1021/acsami.9b00472
157. Ruiz-Garcia H, Ramirez-Loera C, Malouff TD, Seneviratne DS, Palmer JD, Trifiletti DM. Novel strategies for nanoparticle-based radiosensitization in glioblastoma. Int J Mol Sci. 2021;22(18):9673. doi:10.3390/ijms22189673
158. Zhu H, Cao X, Cai X, et al. Pifithrin-μ incorporated in gold nanoparticle amplifies pro-apoptotic unfolded protein response cascades to potentiate synergistic glioblastoma therapy. Biomaterials. 2020;232:119677. doi:10.1016/j.biomaterials.2019.119677
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.