Back to Journals » Clinical Ophthalmology » Volume 10
Pachychoroid neovasculopathy in extramacular choroidal neovascularization
Authors Gupta M, Rusu I, Seidman C, Orlin A, D'Amico D , Kiss S
Received 26 January 2016
Accepted for publication 7 April 2016
Published 12 July 2016 Volume 2016:10 Pages 1275—1282
DOI https://doi.org/10.2147/OPTH.S105080
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Mrinali Patel Gupta, Irene Rusu, Carly Seidman, Anton Orlin, Donald J D’Amico, Szilard Kiss
Department of Ophthalmology, Weill Cornell Medicine, New York-Presbyterian Hospital, New York, NY, USA
Purpose: To review a series of extramacular choroidal neovascular membranes (CNVMs) in the context of their choroidal features, as determined by optical coherence tomography (OCT).
Methods: Patients with extramacular CNVMs were identified from a tertiary care center through a review of records. The charts and cases were reviewed using multimodal imaging including fundus photography, OCT, fluorescein angiography (FA), and indocyanine angiography (ICG).
Results: Of six patients with extramacular CNVMs evaluated in this series, four patients (66.7%) exhibited pachychoroidopathy on OCT imaging under or adjacent to the extramacular CNVM. All four of these patients also exhibited pachychoroidopathy in the macular OCT distant from the CNVM.
Conclusion: Pachychoroidopathy is implicated in some cases of extramacular CNVMs. This represents the first report, to our knowledge, of pachychoroidopathy in extramacular CNVM.
Keywords: choroidal neovascularization, pachychoroidopathy, pachychoroid neovasculopathy, peripheral disciform lesions, extramacular choroidal neovascularization, polypoidal choroidal vasculopathy
Introduction
“Pachychoroidopathy” is a recently coined term to describe the shared choroidal features of thickened choroid and dilated outer choroidal vessels that link a spectrum of retinal conditions including pigmentary change, central serous chorioretinopathy (CSCR), some cases of type 1 (sub-retinal pigment epithelium [RPE]) choroidal neovascularization (CNV), and polypoidal choroidal vasculopathy (PCV).1–3 Although controversy remains regarding pachychoroidopathy, recent studies suggest that the genetics and pathogenesis of pachychoroidopathy, as well as response to therapies, may be distinct from that seen in related conditions such as age-related macular degeneration (AMD). Previously, pachychoroidopathy-related type 1 CNV, termed “pachychoroid neovasculopathy,” has been described in patients with choroidal neovascular membranes (CNVMs) localized to the central macula. To evaluate the role of pachychoroidopathy in extramacular CNVMs, also known as peripheral disciform lesions, we retrospectively reviewed a series of cases of extramacular CNVMs in the context of their associated choroidal findings.
Methods
We retrospectively analyzed a nonconsecutive case series of six patients with extramacular CNVMs. All patients were examined by the Retina Service of the Department of Ophthalmology at Weill Cornell Medicine, New York, NY, USA, with slit lamp biomicroscopy, indirect ophthalmoscopy, color fundus photography (Optos™ Panoramic 200A; Optos PLC, Dunfermline, UK), and enhanced-depth imaging optical coherence tomography (EDI-OCT; Heidelberg Spectralis; Heidelberg Engineering, Inc, Vista, CA, USA). EDI-OCT was performed through the macula in all cases, as well as through the CNVM lesion itself whenever possible. Fluorescein angiography (FA) and indocyanine green angiography (ICG) were also reviewed, when available. The study period was January 2015 to December 2015. This study was approved by the Institutional Review Board of Weill Cornell Medicine and was performed in a Health Care Portability and Accountability Act compliant manner. No informed consent was obtained as this was a retrospective case review study.
Results
The six cases reported had an average age of 74.8 years (range 56 to 87 years). Five were female and one was male. Average follow-up was 20 months (range 2 to 35 months). The clinical and choroidal features of the six cases are summarized in Table 1.
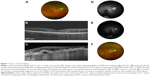
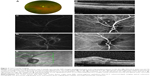
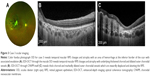
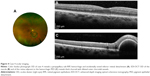
Of the six cases reviewed, four (66.7%; cases 1–4) exhibited pachychoroidopathy (Figures 1–4). These patients were all females ranging in age from 56 to 84 years. Two of these patients presented with photopsia (cases 1 and 3). All four patients exhibited an extramacular CNVM, with macular EDI-OCT revealing thick choroid with dilated outer choroidal vessels. EDI-OCT obtained through the CNVM itself (cases 1–3) revealed Type 1 CNVM overlying thick choroid with dilated outer choroidal vessels which were inwardly displaced and abutting the RPE. EDI-OCT was not possible through the large hemorrhagic pigment epithelial detachment (PED) in case 4, but OCT in the retina adjacent to this lesion similarly revealed thick choroid and dilated outer choroidal vessels. FA was performed in each case and revealed leakage consistent with CNVM in three patients (cases 1–3); case 4 exhibited blockage by the large sub-RPE hemorrhage. ICG was performed in only one case (case 2) and revealed polypoidal neovascular lesions in the area of extramacular CNVM, as well as a few small polypoid lesions in the fellow eye (Figure 2C and D). Two patients (cases 1 and 3) were treated with intravitreal anti-vascular endothelial growth factor (VEGF) injections due to increased exudation or symptomatic CNVM. Case 1 noted no significant response to anti-VEGF therapy nor of her photopsia, while case 3 exhibited stable exudation but resolution of photopsia after therapy. All four cases maintained stable visual acuity at last follow-up.
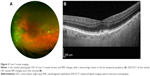
Case 1 is a representative case of extramacular pachychoroid neovasculopathy. This patient is a 79 year old Caucasian female who presented with symptoms of photopsia OD (oculus dexter [right eye]). Visual acuity (VA) was 20/15. There were rare macular RPE changes and subtle choroidal folds consistent with increased choroidal thickness, as well as a superonasal peripapillary CNVM with associated exudation OD (Figure 1A). EDI-OCT of the macula revealed thick choroid with subtle choroidal folds overlying dilated outer choroidal vessels OD (Figure 1B). EDI-OCT through the superonasal exudative lesion OD revealed thickened choroid and dilated outer choroidal vessels with overlying RPE disturbance and type 1 neovascularization (Figure 1C). The dilated choroidal vessels were inwardly displaced and abutted the RPE. Ultrawide-field FA revealed leakage from an occult choroidal neovascular membrane (Figure 1D and E). An ICG was not performed. The lesion was observed, but increased exudation and symptoms were noted 11 months later, prompting treatment with intravitreal ranibizumab (Lucentis®; Hoffman-La Roche Ltd., Basel, Switzerland) 0.5 mg OD and subsequently, aflibercept 2 mg (EYLEA, Regeneron Pharmaceuticals, Inc., Tarrytown, NY, USA) twice, with no significant improvement. At the most recent follow-up, 35 months after initial presentation, exudation was noted to have further increased (Figure 1F), though the macula remains spared and VA is 20/20. The patient declined further intervention such as anti-VEGF therapy or photodynamic therapy.
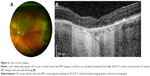
Two of the six cases (cases 5–6) exhibited extramacular CNVM without pachychoroidopathy (Figures 5 and 6). Both were male patients in their 80s who presented with macular drusen and RPE changes and incidentally noted extramacular CNVM with hemorrhage in the far temporal periphery. EDI-OCT through the macula revealed RPE changes and markedly thinned choroid. The lesions were too peripheral to perform EDI-OCT through the CNVM itself.
Discussion
Studies have recently described “pachychoroidopathy”, as a spectrum of conditions (including pigmentary changes, CSCR, some cases of type 1 neovascularization, and polypoidal choroidal vasculopathy) that share common features of thickened choroid and dilated outer choroidal vessels.1–3 On the milder side of this spectrum is pachychoroid pigment epitheliopathy (PPE), in which choroidal thickening and dilated outer choroidal vessels are associated with overlying RPE disturbances. PPE may be a forme fruste of CSCR, sharing the underlying choroidal pathology but lacking the classic macular subretinal fluid or gravitational tracks of CSCR.3 In some patients with PPE, longstanding RPE changes and possibly RPE detachment can lead to disruption of Bruch’s membrane, leading to ingrowth of sub-RPE choroidal neovascular membranes, resulting in Type 1 CNV. These neovascular membranes overlie areas of thickened choroid with dilated outer choroidal vessels and have been termed “pachychoroid neovasculopathy.”1 Over time these neovascular membranes can evolve into branching vascular networks with polypoid lesions seen in PCV. Prior studies have demonstrated associations between CSCR and Type 1 neovascularization, longstanding Type 1 neovascularization and PCV4–7 and CSCR and PCV.8–12 The newly conceived pachychoroidopathy suggests that a pathologic choroidal process characterized by dilated outer choroidal vessels and thick choroid is the underlying common denominator.
Thus far, pachychoroid neovasculopathy has been reported in patients with CNVMs in the central macula.1,3 There are no reports of pachychoroid neovasculopathy in cases with extramacular CNVMs. To evaluate whether pachychoroidopathy may be implicated in extramacular CNVMs, we retrospectively evaluated choroidal features in the central macula and, when possible, under the CNVMs, in a series of six extramacular CNVM cases evaluated at Weill Cornell Medical College. This series is the first, to our knowledge, to examine these peripheral CNVMs in the context of their choroidal findings.
In this small retrospective case series, four of six cases of extramacular CNVMs exhibited pachychoroidopathy – ie, thickened choroids and dilated outer choroidal vessels under or adjacent to the CNVM. This represents the first report of pachychoroid neovasculopathy outside of the central macula. Another feature of pachychoroid neovasculopathy is inward displacement of the dilated outer choroidal vessels below the lesions, such that they are abutting the RPE. This was noted in all four cases. Two patients with pachychoroidopathy presented with symptoms of photopsia. Whether this symptomatology is related to the underlying condition is unclear. In all four cases demonstrating pachychoroidopathy under or adjacent to the extramacular CNVM, the macular OCT also revealed pachychoroidopathy. This suggests that even in cases where the extramacular CNVM itself is too peripheral for OCT imaging, choroidal features visible in the macula itself may support a diagnosis of pachychoroid neovasculopathy. This finding also begs the question of whether presence of such an extramacular CNVM in the setting of pachychoroidopathy in the macula as well suggests an underlying risk for future pigment epitheliopathy or CNVM risk in the macula itself. Further studies with more patients and more long-term follow-up are necessary.
Both cases of extramacular CNVMs without pachychoroid features also had age-related macular degeneration, and their macular choroids exhibited marked thinning, as is common in age-related macular degeneration. Interestingly, the extramacular CNVMs in both of these cases were also far more peripheral than those noted in the four cases with pachychoroidopathy.
Extramacular CNVMs (also known as peripheral disciform lesions, extramacular disciform, or peripheral exudative hemorrhagic chorioretinopathy) comprise a broad diagnostic category. It is now well known that many of these extramacular CNVMs are PCV lesions,13 although large studies evaluating extramacular CNVMs have demonstrated both the absence and presence of PCV-like polyps.13–15 Since PCV is implicated in some extramacular CNVMs and also falls within the pachychoroid spectrum, the pachychoroidopathy noted in cases 1–4 in this series may reflect the known relationship of PCV to extramacular CNVMs. Indeed, in the current study, only one patient received ICG angiography (case 2), and that patient exhibited polypoidal changes consistent with PCV. ICG was not performed or was unable to be performed due to the far peripheral location of the CNVMs in the other cases. The lack of ICG for the other cases is a major limitation of this study, as it is therefore unclear whether there were any cases of extramacular pachychoroidopathy in the absence of PCV features. If pachychoroidopathy were demonstrated in the absence of polyps on ICG in these lesions, pachychoroidopathy may offer an etiology for lesions previously considered idiopathic due to absence of polyps. Prior reports have demonstrated macular pachychoroid neovasculopathy in the absence of PCV.1,3 Further studies of pachychoroid extramacular CNVMs with more extensive ICG evaluation are necessary.
In addition to providing a unifying theme for several related conditions, as well as potentially offering a diagnosis for lesions previously thought to be idiopathic, the conception of pachychoroidopathy may have diagnostic and therapeutic implications. A recent genetic study evaluating eleven AMD susceptibility genes, including complement factor H and ARMS2 rs10490924 found that patients with pachychoroid neovasculopathy exhibited markedly less susceptibility than those with AMD.16 This suggests that a distinct pathogenesis may be implicated in these pachychoroid-driven diseases. Consistent with this finding, we noted that both cases of extramacular CNVM without pachychoroid features in the current study exhibited underlying AMD. Similarly, it is well known that several pachychoroid diseases, including chronic CSCR and PCV, may respond less to anti-VEGF agents and better to photodynamic therapy, than AMD. Thus, the distinction between neovascularization related to or unrelated to pachychoroidopathy may have important implications for therapeutics. Consistent with this, one patient in this series (case 1) with pachychoroid neovasculopathy was treated with anti-VEGF agents with no significant response in exam or symptoms; photodynamic therapy was offered, but the patient deferred.
This study had several limitations. The number of reported cases is small. ICG was not performed or was unable to be performed (due to the far peripheral location of the lesions) in most of the cases evaluated; wide-field FA was used instead. As discussed above, ICG imaging to confirm absence or presence of polypoidal lesions would be instructive. In its absence, it is not possible to determine whether the pachychoroidopathy noted in these extramacular CNVMs reflects the known relation of these lesions to PCV or if there exists cases of extramacular pachychoroid neovasculopathy in the absence of PCV. Finally, the far peripheral location of the extramacular CNVMs in two cases, both of which were felt not to exhibit pachychoroidopathy, prevented the abilitiy to perform OCT through the lesion itself. In both of these cases, choroidal features in the macula were used as a surrogate and revealed thin choroid not consistent with pachychoroidopathy. If the pathology in these extramacular CNVMs is a focal choroidopathy localized to the region of the CNVM itself, using macular choroidal findings to inform the diagnosis of peripheral CNVMs may not be appropriate. However, we noted in this series that in all four cases where sub-CNVM OCTs were able to be performed (cases 1–4), the choroidal findings in the macula mirrored those in near the lesion itself.
Disclosure
The authors report no conflicts of interest in this work.
References
Pang CE, Freund KB. Pachychoroid neovasculopathy. Retina. 2014;35(1):1–9. | ||
Warrow DJ, Hoang QV, Freund KB. Pachychoroid pigment epitheliopathy. Retina. 2013;33(8):1659–1672. | ||
Dansingani KK, Balaratnasingam C, Naysan J, Freund KB. En face imaging of pachychoroid spectrum disorders with swept-source optical coherence tomography. Retina. 2016;36(3):499–516. | ||
Khan S, Engelbert M, Imamura Y, Freund KB. Polypoidal choroidal vasculopathy: simultaneous indocyanine green angiography and eye-tracked spectral domain optical coherence tomography findings. Retina. 2012;32(6):1057–1068. | ||
Tsujikawa A, Ojima Y, Yamashiro K, et al. Development of polypoidal lesions in age-related macular degeneration. Eye. 2011;25(4):481–488. | ||
Tamura H, Tsujikawa A, Otani A, et al. Polypoidal choroidal vasculopathy appearing as classic choroidal neovascularization on fluorescein angiography. Br J Ophthalmol. 2007;91(9):1152–1159. | ||
Freund KB, Zweifel SA, Engelbert M. Do we need a new classification for choroidal neovascularization in age-related macular degeneration? Retina. 2010;30(9):1333–1349. | ||
Sasahara M, Tsujikawa A, Musashi K, et al. Polypoidal choroidal vasculopathy with choroidal vascular hyperpermeability. Am J Ophthalmol. 2006;142(4):601–607. | ||
Ahuja RM, Downes SM, Stanga PE, Koh AH, Vigerling JR, Bird AC. Polypoidal choroidal vasculopathy and central serous chorioretinopathy. Ophthalmology. 2001;108(6):1009–1010. | ||
Yannuzzi LA, Freund KB, Goldbaum M, et al. Polypoidal choroidal vasculopathy masquerading as central serous chorioretinopathy. Ophthalmology. 2000;107(4):767–777. | ||
Ueta T, Obata R, Inoue Y, et al. Background comparison of typical age-related macular degeneration and polypoidal choroidal vasculopathy in Japanese patients. Ophthalmology. 2009;116(12): 2400–2406. | ||
Koizumi H, Yamagishi T, Yamazaki T, Kinoshita S. Relationship between clinical characteristics of polypoidal choroidal vasculopathy and choroidal vascular hyperpermeability. Am J Ophthalmol. 2013;155(2):305–313. | ||
Mantel I, Shalenbourg A, Zografos L. Peripheral exudative hemorrhagic chorioretinopathy: polypoidal choroidal vasculopathy and hemodynamic modifications. Am J Ophthalmol. 2012;153(5):910–922. | ||
Mantel I, Uffer S, Zografos L. Peripheral exudative hemorrhagic chorioretinopathy: a clinical, angiographic, and histologic study. Am J Ophthalmol. 2009;148(6):932–938. | ||
Goldman DR, Freund KB, McCannel CA, Sarraf D. Peripheral polypoidal choroidal vasculopathy as a cause of peripheral exudative hemorrhagic chorioretinopathy: a report of 10 cases. Retina. 2013;33(1): 48–55. | ||
Miyake M, Ooto S, Yamashiro K, et al. Pachychoroid neovasculopathy and age-related macular degeneration. Scientific Reports. 2015;5: 1–11. |
 © 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2016 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.