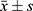Back to Journals » International Journal of Chronic Obstructive Pulmonary Disease » Volume 16
Nursing Outcomes and Risk Factors of Patients with Chronic Obstructive Pulmonary Disease After Discharge
Authors Chai YH , Yang H, Huang GP, Wu T, Dong Y
Received 25 May 2021
Accepted for publication 27 September 2021
Published 21 October 2021 Volume 2021:16 Pages 2911—2916
DOI https://doi.org/10.2147/COPD.S321375
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Richard Russell
Yun-Hua Chai,1 Hui Yang,2 Gai-Ping Huang,1 Ting Wu,1 Yan Dong3
1Department of Geriatrics, First Hospital of Shanxi Medical University, Taiyuan City, Shanxi Province, People’s Republic of China; 2Nursing College of Shanxi Medical University, Jinzhong City, Shanxi Province, People’s Republic of China; 3Department of Respiratory and Critical Illness, First Hospital of Shanxi Medical University, Taiyuan City, Shanxi Province, People’s Republic of China
Correspondence: Yun-Hua Chai
Department of Geriatrics, First Hospital of Shanxi Medical University, No. 85 Jiefang South Road, Taiyuan City, Shanxi Province, 030001, People’s Republic of China
Tel +86 15203405557
Email [email protected]
Background: Chronic obstructive pulmonary disease (COPD) is a physical and mental disease, and there is currently no cure, so the health guidance of COPD patients after discharge from hospital is crucial. The purpose of this study is to investigate the nursing outcomes and risk factors for patients with COPD discharged from hospital.
Methods: In this study, a total of 200 patients with COPD who were stable and ready to be discharged from two tertiary hospitals in Taiyuan were surveyed by the Nursing Outcome Evaluation Form for COPD patients, and the relevant risk factors of these patients were analysed.
Results: The results of this study showed that patients with COPD who were to be discharged from hospital had low scores in the perceived health domain (1.9708 ± 0.70525) and psychosocial health domain (1.5267 ± 0.68289), while the scores in the rest of the domains were above the medium level. The main factors affecting the two domains of the nursing outcome were degree of education, dietary habits, complications (perceived health domain), drinking, marital status, medical insurance and smoking (psychosocial health domain) (p < 0.05).
Conclusion: Clinical nurses should pay attention to the perceived and psychosocial health domains when educating COPD patients who are to be discharged from hospital, and should primarily focus on the risk factors of smoking and drinking status, degree of education, dietary habits, complications, marital status and medical insurance.
Keywords: chronic obstructive pulmonary disease, COPD, discharge, core nursing outcomes, risk factors
Introduction
Chronic obstructive pulmonary disease (COPD) is a disease that seriously affects the physical and mental health and daily life of older patients because of its protracted and recurrent characteristics.1–4 There is currently no cure for this disease. The purpose of clinical treatment is to control symptoms, reduce the number of attacks and prevent complications. Therefore, the health guidance of COPD patients after discharge from hospital is essential.
At present, the influencing factors on the quality of life of COPD patients according to their importance are age, duration of bed rest, exercise, daily smoking and patients’ family relationships.5–7 However, there is a lack of continuous follow-up of nursing outcomes in the health domain of COPD patients and specific quantification of patients’ quality of life. The Nursing Outcomes Classification (NOC)8 is a system for objectively measuring the outcomes of nursing interventions and was developed to help nurses and other health professionals assess and quantify the status of patients, caregivers, families or communities by measuring changes in patient status. The NOC is important to the development of the nursing discipline as one of the standardised nursing languages. The application of a standardised nursing language is helpful for nursing development in China, and helps to reflect the value of clinical nurses and contributes to the development of a nursing discipline.9
Our group previously developed a Nursing Outcome Evaluation Index System for Patients with Chronic Obstructive Pulmonary Disease based on a literature review, semi-structured interviews, the modified Delphi method and the pre-survey method.10 In this study, it was applied to the analysis of nursing outcomes and the risk factors of discharged patients with COPD, providing a basis for the development of personalised discharge planning models and health education and the promotion of patient rehabilitation.
Materials and Methods
Study Design
In this study, general information of the participants was collected, and a convenience sampling was used in which five investigators administered a questionnaire to eligible subjects on the day of the patient’s discharge with the consent of the patients themselves or their caregivers. An analysis of nursing outcomes and risk factors of discharged patients with COPD was performed.
Subjects
In this study, convenience sampling was used to select patients with COPD admitted to two tertiary care hospitals in Taiyuan from December 2017 to December 2018 and were ready to be discharged from hospital in stable condition as the primary study subjects. The study conforms to the World Medical Association Declaration of Helsinki and has been approved by the Ethics Committee of First Hospital of Shanxi Medical University, and all patients signed informed consent.
Inclusion criteria: 1. meeting the diagnostic criteria of COPD; 2. clear consciousness, able to write and read correctly, without communication disorders; 3. confirmed diagnosis and willing to participate in the survey; 4. ready to be discharged in stable condition.
Exclusion criteria: 1. discharged to a nursing home; 2. continued to receive further follow-up treatment in an outpatient clinic after discharge; 3. COPD combined with other mental and psychological diseases; 4. incomplete case data.
Data Collection Method
The data collected in this study mainly included: ① general data, including gender, age, marital status, education level, occupation, smoking status, health insurance status, alcohol consumption, monthly income, comorbidities and dietary habits; ② the Nursing Outcome Evaluation Form for COPD patients, which was developed based on the Nursing Outcome Evaluation Index System for COPD patients previously studied by our research group.10 This evaluation system consisted of six domains, including 14 items in the functional health domain, 12 items in the physical health domain, 12 items in the psychosocial health domain, 16 items in the health knowledge and behaviour domain, 13 items in the perceived health domain and 13 items in the family health domain, with a total of 80 items. Each item contained a title, a set of indicators related to the item description and a 5-point Likert scale that can be objectively measured (4 = always, 3 = often, 2 = about half the time, 1 = occasionally and 0 = never) with a cut-off value of 2.5 for all domains. Among them, the lower the score of the physical health domain, the better the health status, while the higher the score in the remaining domains, the better the health status and perception effect. Cronbach’s alpha showed the questionnaire to reach acceptable reliability, α = 0.81. The respondents themselves generally filled out the questionnaires, and the investigators dictated to those with dysgraphia or dyslexia. A total of 210 questionnaires were distributed in this survey, and 200 valid questionnaires were returned, with an effective recovery rate of 95.24%, and investigators filled out 15 of the questionnaires.
Statistical Analysis
In this study, SPSS (version 22.0, IBM Corp.) statistical software was used for data processing. Measurement data were expressed as mean ± standard deviation (X ± s). Enumeration data were presented as a percentage (%). The t-test was used for comparison between two groups that obeyed a normal distribution; the non-parametric test was used for comparison between groups that did not follow a normal distribution. Enumeration data were analysed by the chi-square test. For categorical variables (categories were >2), dummy variables needed to be set, and the risk factors were analysed by multiple linear regression analysis. P-values <0.05 indicated that the difference was statistically significant.
Results
General Information
A total of 200 COPD patients were selected in this study, including 168 males and 32 females aged 22–88 years. There were 24 patients aged <60 years, 114 aged between 60 and 70 years and 62 aged >70 years. The classification of gender, marital status, education level, occupation, smoking status, health insurance status, alcohol consumption, monthly income, comorbidities and dietary habits are shown in Table 1.
 |
Table 1 The Classification of Main Influencing Factors |
Level of Nursing Outcomes for COPD Patients
The scores of the perceived health domain (1.9708 ± 0.70525) and the psychosocial health domain (1.5267 ± 0.68289) were low for the nursing outcomes of discharged COPD patients, while the scores of the remaining domains, including functional health, physical health, health knowledge and behaviour and family’s health domains were moderate to high, as shown in Table 2.
 |
Table 2 Scores of Nursing Outcomes of COPD Patients Discharged from Hospital ( |
Analysis of Influencing Factors of Nursing Outcomes of COPD Patients Discharged from Hospital
Univariate analysis was performed by grouping patients by gender, age, marital status and occupation to investigate whether there were differences in the scores of all dimensions of nursing outcomes in different groups. The results of this study showed that smoking status, gender, occupation, health insurance status, education level, alcohol consumption, monthly income, comorbidities, dietary habits and marital status affected all dimensions of nursing outcomes. Multiple linear regression analysis was performed using the study subjects’ nursing outcomes as the dependent variable and the 10 factors mentioned above as independent variables. The main factors affecting the two domains of the nursing outcome were degree of education, smoking, dietary habits, complications (perceived health domain), drinking, marital status, medical insurance and smoking (psychosocial health domain) (p < 0.05). The results are shown in Tables 1 and 3.
 |
Table 3 Multiple Linear Regression Analysis Results of Influencing Factors for Nursing Outcomes of 200 Discharged Patients with Chronic Obstructive Pulmonary Disease |
Discussion
The Nursing Outcome Evaluation Form for discharged COPD patients is a reasonable assessment tool to continuously track the patients’ health status and provide continuous nursing in the home and community, while the Quality of Life Scale is a tool to identify the degree of disorders and determine the prognosis of rehabilitated patients in order to develop rehabilitation programs and evaluate treatment outcomes. The nursing outcome classification covers the entire category of nursing practice and can evaluate the status of patients and their caregivers in all aspects of hospital, family and community, and the quantification of indicators facilitate the use of health service personnel.11 Studies have shown that patients are carefully cared for during hospitalisation by the medical staff, while it is difficult to effectively continue these care activities after discharge.12 The development and application of a nursing outcome classification system can better guide nursing practice to provide nursing outcomes for patients with the same disease, which requires comprehensive selection based on the patient’s condition, medical diagnosis or nursing problems, physical and mental status and treatment outcomes. At the same time, the rehabilitation status and rehabilitation degree of different patients are quantitatively evaluated using indicators and metrics. The nursing outcome is used as an important tool and is a way to evaluate the quality of nursing services and the effect of nursing measures. As the clinical nurse has the highest contact with patients, it is necessary for them to have critical scientific thinking and rich clinical experience to provide individualised nursing outcomes for patients with COPD. In this study, the Nursing Outcome Evaluation Form for COPD Patients was used to evaluate the effectiveness of its implementation in the health status of discharged COPD patients. According to the measurement of nursing outcome scores and analysis of their influencing factors, a discharge planning model form could be established and implemented for COPD patients at the time of discharge.
The results of this study showed that the nursing outcome scores of the functional and physical health domains were above moderate levels for discharged COPD patients. The reason for this was that the physiological indicators of COPD patients, including cough, expectoration symptoms and saturation, were restored to a healthy level at discharge and met the discharge indications. However, the psychosocial and perceived health domains scores were low, and these domains need to be continuously strengthened. In particular, the lowest score was obtained in the psychosocial health domain because COPD is complicated by chronic respiratory failure, spontaneous pneumothorax and chronic pulmonary heart disease,13–16 which leads to altered health status, a heavy economic burden and an anxious and stressful mental state. The score of the perceived health domain was also low because perception refers to the beliefs patients use to interpret the signals received by their organs, while the main feature of COPD is airflow limitation. These patients mainly feel shortness of breath and dyspnoea, and nurses need to instruct them to perform respiratory function exercises, such as abdominal and lip retraction breathing. It is suggested that nurses should carry out individualised guidance and intervention in health behaviours and habits for caregivers in conducting health education, and the improvement of continuous nursing skills of caregivers depends on the standardised training of nurses. As one of the high-quality and low-cost medical strategies to reduce the rehospitalisation rate of chronic diseases, continuous nursing has been shown to improve the quality of life of COPD patients.17–20
In addition, the results of this study suggested that multiple factors affected the nursing outcomes of discharged patients with COPD, and the level of nursing outcomes varies among discharged COPD patients with different demographic signs and comorbidities. The main factors affecting the two domains of the nursing outcome were degree of education, complications (perceived health domain), dietary habits, drinking, marital status, medical insurance and smoking (psychosocial health domain). Patients who pay out-of-pocket have a higher financial burden, and their health status is less optimistic because of it. Alcohol consumption can reduce airway ciliary clearance and cause minor airway stenosis, which induces the occurrence of COPD. Thus, alcohol consumption is a risk factor for nursing outcomes. Unreasonable dietary habits are also one of the risk factors of COPD. The reason is that reasonable dietary habits can maintain and improve lung function and delay the progression of COPD. Therefore, dietary habits should be appropriate for COPD patients, and the intake of nutrients should be diversified. Marital status mainly affects the psychosocial health domain of COPD patients. Patients with spouses can receive financial and spiritual support from family caregivers, and high-quality care from spouses can maintain a high level of health. Smokers with COPD had a lower health status and awareness than non-smokers. Nurses spend less time on health education for discharged COPD patients with higher education levels, as these patients pay more attention to health knowledge and behaviour, perceived disease and family support. The more comorbidities, the worse the physical and mental health of COPD patients. Nurses should pay more attention to the physical and mental status of COPD patients with two or more complications, closely observe their conditions and mentality changes, identify the risk factors according to the scores of the nursing outcome and timely give psychological and pacifying guidance.
It is suggested that nurses strengthen discharge education in terms of occupation, monthly income, medical insurance, alcohol consumption, dietary habits, marital status, gender, smoking status, education level and comorbidities. They should also have a continuous follow-up to extend nursing to communities and families, taking advantage of the hospital’s health resources to provide ongoing services for patients and ensure they receive continued care and strengthen the establishment and seamless hospital-community-family ternary linkage nursing model.
This study still has the following shortcomings. First, the sample size included in this study was small, and further studies are still needed to increase the sample size. Second, there was no uniform standard for individualised education programs for COPD patients, which remains to be further studied and explored.
In conclusion, clinical nurses should pay attention to the perceived and psychosocial health domains when educating COPD patients who are to be discharged from hospital, and should mainly focus on the risk factors of smoking and drinking, degree of education, dietary habits, complications, marital status and medical insurance. The constructed Nursing Outcome Evaluation Form for discharged COPD patients was applied to clinical practice in this study. The clinical nurse leaders or nurses could implement the model based on the standardised nursing language, which could improve the awareness and compliance of patients, change their unhealthy lifestyle, finally improve their quality of life and delay the progression of the disease.
Ethical Statement
This study was conducted in accordance with the Declaration of Helsinki and approved by the ethics committee of First hospital of Shanxi Medical University. All participants had signed the informed consent.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Duffy SP, Criner GJ. Chronic obstructive pulmonary disease. Med Clinics North Am. 2019;103(3):296–302. doi:10.1016/j.mcna.2018.12.005
2. Barstow C, Forbes D. Respiratory conditions: chronic obstructive pulmonary disease. FP Essent. 2019;486:26–32.
3. Guo C, Xiang G, Xie L, et al. Effects of Tai Chi training on the physical and mental health status in patients with chronic obstructive pulmonary disease: a systematic review and meta-analysis. J Thorac Dis. 2020;12(3):504–521.
4. Duan JX, Cheng W, Zeng YQ, et al. Characteristics of patients with chronic obstructive pulmonary disease exposed to different environmental risk factors: a large cross-sectional study. Int J COPD. 2020;15:2857–2867. doi:10.2147/COPD.S267114
5. Welling A. Evaluation of lower limb muscle strength and function in individuals with chronic obstructive pulmonary disease. Int J Current Advan Res. 2020;7(7):14043–14046.
6. Guo C, Xiang G, Xie L, et al. Effects of Tai Chi training on the physical and mental health status in patients with chronic obstructive pulmonary disease: a systematic review and meta-analysis. J Thorac Dis. 2020;12(3):504–521.
7. Arslan Y, Cal N, Doan D, An A, Sar O. The awareness of chronic obstructive pulmonary disease among smokers admitting to pulmonary medicine outpatient clinic: single center experience. Gulhane Med J. 2021;63(1):59–67. doi:10.4274/gulhane.galenos.2021.1517
8. Wu Yuan JY. Classification of Nursing Outcomes. Beijing: Peking University Medical Press; 2006.
9. Barnett M. Nursing management of chronic obstructive pulmonary disease. Br J Nurs. 2013;17(21):1314–1318.
10. Yang H, Chai YH. Establishment and Evaluation of Nursing Outcome Evaluation Index System for COPD Patients Based on Nursing Outcome Classification. Taiyuan: Shanxi Medical University; 2015.
11. Cavalcante MD, Larocca LM, Chaves MM, Cubas MR, Macedo Piosiadlo LC, Azevedo Mazza C. Nursing terminology as a work process instrument of nurses in collective health. Rev Esc Enferm USP. 2016;50(4):610. doi:10.1590/S0080-623420160000500010
12. Yan XM, Sun W, Han Y, Su JP. Application of multidisciplinary cooperative continuous nursing oriented by nursing outcome in postoperative patients with esophageal cancer after radical operation. Chin Nurs Res. 2018;32(10):1612–1615.
13. Nakawah MO, Hawkins C, Barbandi F. Asthma, chronic obstructive pulmonary disease (COPD), and the overlap syndrome. J Am Board Fam Med. 2013;26:470–477. doi:10.3122/jabfm.2013.04.120256
14. Ota H, Kawai H, Matsuo T. Treatment outcomes of pneumothorax with chronic obstructive pulmonary disease. Asian Cardiovasc Thorac Ann. 2014;22(4):448–454. doi:10.1177/0218492313505230
15. Fettal N, Taleb A. Pneumothorax secondary to chronic obstructive pulmonary disease. Eur J Anaesthesiol. 2012;23(7):621–623.
16. Zhang Y, Jiang G, Chen C, Ding J, Zhu Y, Xu Z. Surgical management of secondary spontaneous pneumothorax in elderly patients with chronic obstructive pulmonary disease: retrospective study of 107 cases. Thorac Cardiovasc Surg. 2009;57(6):347–352. doi:10.1055/s-0029-1185767
17. Aboumatar H, Naqibuddin M, Chung S, et al. Better Respiratory Education and Treatment Help Empower (BREATHE) study: methodology and baseline characteristics of a randomized controlled trial testing a transitional care program to improve patient-centered care delivery among chronic obstructive pulmonary disease patients. Contemp Clin Trials. 2017;62(1):159–167.
18. Weina J, Yanhua L, Jian W, Shao Y. Therapeutic effects of statins drugs use and continuous nursing on patients with chronic obstructive pulmonary disease and the influence of life quality. Pak J Pharm Sci. 2018;31(3(Special)):11184–11794.
19. Yuan HJ. Research progress of continuing nursing care to improve the quality of life of patients with chronic obstructive pulmonary disease. Nurs Sci. 2017;06(3):81–85. doi:10.12677/NS.2017.63016
20. Barnett M. Nursing management of chronic obstructive pulmonary disease. Br J Nurs. 2013;17(21):1314–1318.
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.