Back to Journals » International Journal of Nanomedicine » Volume 15
Nanoparticles of Lovastatin: Design, Optimization and in vivo Evaluation
Authors Gaber DA
Received 4 December 2019
Accepted for publication 18 April 2020
Published 17 June 2020 Volume 2020:15 Pages 4225—4236
DOI https://doi.org/10.2147/IJN.S241120
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Anderson Oliveira Lobo
Dalia A Gaber1,2
1Department of Quality Control & Quality Assurance, Holding Company for Biological Products and Vaccines, Cairo, Egypt; 2Department of Pharmaceutics, College of Pharmacy, Qassim University, Buraidah, Saudi Arabia
Correspondence: Dalia A Gaber Tel +20 1013379892
Fax +20 2 224154781
Email [email protected]
Introduction: The aim of the study was to optimize the processing factors of precipitation–ultrasonication technique to prepare nano-sized particles of Lovastatin (LA) for enhancing its solubility, dissolution rate and in vivo bioavailability.
Methods: LA nanoparticles (LANs) were prepared using precipitation–ultrasonication technique under different processing factors. LANs were characterized in terms of particle size, zeta potential and in vitro release. Stability studies at 4°C, 25°C and 40°C were conducted for optimum formulation. In addition, the in vivo bioavailability of the optimum formula was studied in comparison to a marketed product in white master rats.
Results: The optimized LAN formula (LAN15) had particle size (190± 15), polydispersity index (0.626± 0.11) and a zeta potential (− 25± 1.9 mV). The dissolution study of the nanosuspensions showed significant enhancement compared with pure drug. After 50 min, only 20.12± 1.85% of LA was dissolved while 99.1± 1.09% of LA was released from LAN15. Stability studies verified that nanosuspensions at 4°C and 25°C showed higher stability with no particle growth compared to the samples studied at 40°C. In vivo studies conducted in rats verified that there was 1.45-fold enhancement of Cmax of LAN15 as compared to marketed tablets.
Conclusion: Nanoparticle prepared by ultrasonication-assisted precipitation method is a promising formula for enhancing the solubility and hence the bioavailability of Lovastatin.
Keywords: hyperlipidemia, HPMC, nano size, factors, antisolvent, bioavailability
Introduction
Many studies reported that poor aqueous solubility and hence low bioavailability of drugs belong to class II & IV in Biopharmaceutical Classification System (BCS) is a great challenge for scientists.1,2 Nanosuspension is one of the most successful methods to enhance the water solubility of the drugs. Recently, the conventional methods for preparing nanosize particles face many limitations due to a large amount of solvents used and solvent residual in the pharmaceutical product.3,4 Many researchers reported the use of antisolvent precipitation technique as a successful method to prepare drug-loaded nanosize/micronize particles.5 Antisolvent-precipitation technique is a simple, mild and cheap method for the production of nanosized suspension.6,7 It involves the dissolution of the drug in the solvent phase, followed by introducing the drug solution in an antisolvent phase, which leads to the precipitation of nano-size particles.8,9 The usage of ultrasonication combined with precipitation improves particle-size reduction, decreases particle size distribution and therefore enhances product stability.10,11 Adami et al and Bartos et al have been reported that processing conditions playing an important role in the characters of the developed nanosuspensions; including type and concentration of polymers, type of surfactants, sonication energy, horn length, depth of immersion, in addition to temperature.12,13 Water-soluble polymers are widely used for improving solubility and stability of drug formulations.14 Water-soluble polymers usually dissolve, disperse or swell in water and, thus, alter the physical properties of aqueous systems by emulsification, thickening, gellation, or stabilization.15 Water-soluble polymers are generally divided into two types according to its source (a) Natural polymers, eg, Guar gum, Cellulose ethers, Carrageenan, Dextran, Chitosan derivatives, Pectin and Xanthan gum (b) Synthetic polymers, eg, Polyethylene glycol (PEG), Polyvinyl pyrrolidone (PVP), Polyvinyl alcohol (PVA), Polyacrylic acid (PAA), Polyacrylamide and Polyoxazoline and Polyphosphazenes.15,16 LA, chemical structure shown in Figure 1 is a poorly water-soluble drug and classified as class II according to BCS.3,10 LA belongs to statins and considered as one of the most effective cholesterol-lowering drugs.17 LA works by blocking cholesterol biosynthesis through inhibition of 3-hydroxy-3-methylglutaryl-CoA (HMG-CoA) reductase enzyme.10,18 In addition, LA showed the ability to diminish the level of low-density lipoprotein (LDL), while the high-density lipoprotein level remains unaffected. Many reports showed that LA has reduced the mortality in coronary heart disease.3,19,20 Although the oral route for LA is the most common route of use, it usually shows low oral bioavailability due to its poor solubility.21 Many oral formulations, such as microbeads, microspheres and solid dispersions nanoparticles of LA were evaluated for its ability to improve LA solubility and hence its bioavailability.3,19-22 The study aimed to determine and evaluate the optimized processing factors for preparing nanosize particles of LA; specifically the type and concentration of the polymer used as a stabilizer (ie three polymers were evaluated at three levels) and the duration of ultrasonication. Besides, the in vitro solubility of optimum LAN formulations was studied. Finally, in vivo pharmacokinetic parameters were verified for the selected optimized formulation in comparison to marketed tablets as a reference.
 |
Figure 1 Chemical structure of Lovastatin. |
Materials and Methods
Materials
Lovastatin (LA) and Atorvastatin (Mash for Pharmaceutical Industries, Egypt). Reference tablets; Cholilysis® 10 mg tablets (El-Obour pharmaceutical company, Cairo, Egypt). Hydroxy propyl methyl cellulose K 15M (HPMC K15M) and poly vinyl pyrrolidone K-30 (PVP K-30) (El Kahera Pharmaceuticals, Cairo, Egypt), N-carboxymethylchitosan (N-CMC) (Hubei Kang Baotai Fine Chemical Co., Ltd., China). Tween 80 (Buchs, Switzerland). Ethanol and acetonitrile were HPLC grade. Other chemicals were of analytical grade and were used as obtained.
Method
Formulation of LA Nanosuspensions (LAN)
LAN formulations were designed by precipitation ultrasonication technique. Briefly, 10 mg of LA was dissolved in 2 mL of ethanol as organic solvents. Sequences of aqueous media with 0.1% of Tween and different concentrations (0.25%, 0.5% and 1%) of one of the following polymers PVP K-30/HPMC K15M/N-CMC were prepared and cooled at 10°C (Table 1). Both aqueous and non-aqueous media were passed through a 0.4 μm filter. The drug solution was injected through a syringe into a polymer solution. Drug-loaded polymer solution was stirred at 1000 rpm for 5 min followed by ultrasonication of the suspension for 15, 30 or 60 min at 300 W ultrasonic energy, at 3-s pauses. LAN suspensions were then centrifuged at 4000 rpm for 10 min. The sediment was freeze-dried. Lyophilized preparations were kept in a desiccator until further investigation.
 |
Table 1 Formulation Code, Polymer Type and Concentration, Sonication Time, PDI, ZP and %EE of LAN Formulations |
Characterization of LAN Formulations
Analysis of Particle Size and Zeta Potential
For defining the particle size and zeta potential of LANs; dynamic laser light scattering (Zetasizer Ver. 5.11 Malvern) was used. All LAN formulations were suspended in distilled water for measurement.
Determination of Drug Encapsulation Percentage
The content of LA in nanoparticles formulae was determined as mentioned in the method published by Mehrdad.23 Reversed-phase C18 column (particle size 5 m m; 250 X 4.6 mm) was used for HPLC separation using a mixture of 0.05 M phosphate buffer (pH 7) and acetonitrile (44.5: 55.5, v/v) as mobile phase with UV detection at 238 nm. Atorvastatin was used as internal standard (IS), the analysis was conducted under room temperature conditions. The drug encapsulation percentage was calculated based on the amount of drug in LANs and the actual amount of LA used for the preparation of LANs.
Fourier Transform Infrared (FTIR) Spectroscopic Analysis
Defining the possible interaction between LA and polymers in nanoparticles was showed. FTIR studies were conducted to verify the possible interaction using FTIR spectrophotometer (Shimadzu 1800, Japan). Samples powder was blended with Potassium bromide powder and pellets were made by press.
Differential Scanning Calorimetry
Thermal behavior of LA and selected LAN formulations were studied using differential scanning calorimetry (DSC) (Mettler Toledo, Switzerland). In aluminum pans, 5 mg samples were heated at a scanning rate of 10°C/min at 40–200°C under a nitrogen flow of 50 mL/min.
Saturation Solubility Study
Saturation solubility was done as mentioned by Haroon.24 Briefly, 1.5 mL of LANs was packed into centrifugation tubes and centrifuged at 14,500 rpm for 1 h. The supernatant will be filtered through 0.2 μm filters and LA content was determined using HPLC. Also, the saturation solubility of LA in distilled water and in the polymer solution (w/v) was determined to evaluate the impact of nanosuspension entrapment on LA solubility.
In vitro Release Study
In vitro release study of pure LA and LA from selected LANs were performed. Dissolution studies were accomplished using USP apparatus type II with 500 mL dissolution medium (deionized water) at 37°C and 50 rpm for 60 min. At predetermined time intervals, 5 mL aliquots were withdrawn, filtered, and assayed for LA content using UV spectrophotometer at 238 nm. An equivalent volume of fresh medium was added to the dissolution medium after each sampling to keep it in a constant volume through the test. Each sample was tested triplicate (n = 3).25
Stability Study
A stability study was conducted to study the drug loss and particle aggregation upon storage. The stability of the selected formula of LANs was assessed by storing samples for 3 months at 4°C, 25°C, and 40°C. At constant time intervals (10, 15, 30, 45, 60, 75, and 90 days), drug content was evaluated by the method described in the previous section and nanoparticle size was recorded using the Zetasizer technique.
In vivo Pharmacokinetic Study in Wistar Rats
This in vivo study was conducted with approval number L/A65 from the ethical committee of Research &Development department of Biological product and vaccines institution followed to Cairo University. The experiment was conducted in accordance with the reported principles of animal care reported by The European center for the validation of alternative methods (Diehl et al, 2001).26 In vivo pharmacokinetic study was conducted on 18 male Wistar rats weighing 220–250 gm. Rats were divided into three groups (six rats in each group) with free access to water and food before and during the experiment. Rats in the first group were received a weighted amount of optimized formula of LAN suspended in distilled water (10 mg LA/mL), via oral gavage. Tablets of the marketed product (Cholilysis®,10 mg) were cursed and the weight of tablet with an equivalent amount of LA was suspended in distilled water and given to rats in the second group. One mL of normal saline was given to rats in the third group as a control. Blood samples (0.5 mL) were withdrawn from the eye at 0.5, 1, 2, 3, 4, 6, 8 and 12 h after dosing in heparinized tubes. The collected blood samples were centrifuged (Hettich Zentrifugen, Germany) at 4000 RPM for 10 min and were stored in the freezer at −20°C until further work. The LA concentration in plasma samples was assayed according to Mehrdad23 method after validation for selectivity, linearity, precision, accuracy and stability shortly before the start of the study.
Calculation of LA Concentration in Plasma and Statistical Analysis
All presented pharmacokinetic parameters were calculated from the plasma concentrations versus time curve.LA plasma concentrations are presented as the mean ± standard deviation. Cmax, tmax, and AUC were reported as measured. The relative bioavailability (F) with Cholilysis®, 10 mg was calculated using the following equation:
(1)
Statistical Estimation of the Results
All statistical differences in data were calculated by SPSS Statistics 17 (Armonk, NY, USA) using one-way ANOVA with extended LSD post hoc test for the determined pharmacokinetic parameters, and P value <0.05 was considered significant.
Result and Discussion
In the following study, LANs were prepared through anti-solvent precipitation–ultrasonication process which could be described as a simple and cost-effective technique. The effects of process parameters specifically; polymer type, polymer concentration and sonication time on physical parameters, drug loading and in vitro releases were studied. The study involved the use of the following polymers HPMC K15M, PVP K-30 and N-CMC at three levels 0.25%, 0.5% and 1%. In addition, the ultrasonication time was varied between15, 30 and 60 min. All other processing factors were retained unvaried during the investigation.
Particle Size, Polydispersity Index and Zeta Potential
The particle size (PZ) and the polydispersity index (PI) of the formed LANs were defined immediately after preparation by Zetasizer Ver. 5.11 Malven.
The mean PZ and PI of LANs are shown in Table 1 and Figure 2. LANs particle size range was between 650±34 and 150 ± 28 for LAN1 and LAN27, respectively. LAN27 was the smallest nanoparticles with particle size 150±28 nm and PDI 0.141±0.02. The results showed that there was an inverse relationship between polymer concentration and particle size that it was obvious that, the smallest size among HPMC LANs formulae were LAN3, LAN6 and LAN9 with particle size 287± 15 (PI = 0.305±0.014), 254±21 (PI= 0.356±0.015) and 250 ± 15 nm (PI=0.301±0.013) respectively. The same observation was recorded for the other two polymers (PVP K30 & N-CMC). The same observations could be interpreted as; the growth of the crystals was minimized by the adsorption of stabilizing polymer on its surface. A higher concentration of the polymer will lead to better coverage of the crystal surface to provide sufficient force of repulsion between the nanoparticles.27 Our finding showed that N-CMC at concentration 1% showed the highest ability to stabilize LANs with the smallest crystals. Regarding the reduction in crystal size, polymers could be arranged in the following order N-CMC LANs >PVP K-30 LANs > HPMC K15M LANs. Khan et al also reported in their investigation that the different types of drugs with different crystal surfaces will need different types and concentrations of polymers to achieve stability.28 Furthermore, sonication time revealed a significant effect on crystal growth, that ultrasonication is a kind of annealing that helps in stabilizing nanosuspension by decreasing its energy.29 It was reported that ultrasonication was able to reduce the surface free energy by converting the less ordered solid state to the more order form and enhancing the adsorption of the stabilizer polymer over the particles.8 Our study revealed a reduction in the particle size as sonication time increased from 15 min to 30 min but further increase in sonication time to 60 min showed non-significant decrease in particle size which may be due to the smallest size has been achieved at 30 min and no longer reduction in size could be attained under the experimental conditions. Other studies showed that the smallest particle size of carvedilol nanosuspensions observed after15 min which could be interpreted on the base of the difference in drug type and experiment conditions.30 The surface charge of LANs was measured by zeta potential. The zeta potential is the measure of charge on the surface nanoparticle and it expresses particle stability. It is an important distinctive of nanoparticles which defines the physical stability of the formulation. Results showed that nanoparticles have surface charge and hence accepted stability. Zeta potential of LANs formulae was ranged between −20±0.57 and −27±1.2 mV, showed that all formulations were with accepted stability.
 |
Figure 2 Mean particle size of LANs formulations under different processing conditions. (A) LAN1-LAN9, (B) LAN10-LAN18, and (C) LAN19-LAN27. |
Percentage Encapsulation (%EE) of LA in LANs
Results revealed accepted encapsulation efficiency higher than 95.1% for all LANs formulations as shown in Table 1. This indicates the efficiency of the technique in designing nanoparticles with high drug loading. Non-significant differences in encapsulation efficiency were observed between different formulations at p level <0.5. Minimum variations in drug encapsulation between LANs formulae could be due to the variation in type and concentration of polymer and differences in sonication time.
Differential Scanning Calorimetry (DSC)analysis
LANs were characterized by DSC analysis, to realize the nature of the drug in nanoparticles and to detect any change in crystal state or possible interaction between LA and polymers. Thermograms obtained for pure LA, HPMC K15M, PVP K30, N-CMC and optimized formulation of each polymer under optimum condition are shown in Figure 3. The DSC of LA showed a sharp endothermic peak at 171.881°C which equivalent to its melting point. Thermograms of the optimized formulations did not demonstrate any considerable shift in the endothermic peak with a small reduction in intensity compared to pure LA due to precipitation and addition of other materials.
 |
Figure 3 DSC thermogram of LA, HPMC K15M, LAN6, PVP K30, LAN15, N CMC and LAN24. |
Fourier Transform Infrared (FTIR) Spectroscopic Analysis
Figure 4 shows the FTIR spectrum of pure LA and above-stated excipients and optimized formulations. LA showed a peak at 1275 cm−1 and 1050 cm−1 which is due to lactone and ester C-O-C bending vibration stretching and another peak at 2930 cm−1 due to the presence of methyl and methylene C-H stretching. Other additional peaks were observed with an optimized formulation which could be due to the presence of polymers. Spectrums revealed that incorporation of LA into the nanoparticles did not alternate the nature of its functional groups. Thus, it confirms the structure of the drug.
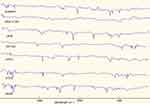 |
Figure 4 FTIR spectrums of LA, HPMC K15M, LAN6, PVP K30, LAN15, N CMC and LAN24. |
Saturation Solubility
The solubility of LA was expressed in water and stabilizer solution with concentrations (0.25%, 0.5% and 1%), also the solubility of selected LANs formula in water was analyzed. The poor solubility of LA in water was enhanced significantly (P<0.05) in the stabilizer solution. Further enhancement of solubility was observed by the formulation of nanoparticles of LA. The solubility of LA in water was 0.4±0.109 μg/mL. The solubility of LA in stabilizer solutions at different levels was varied between 0.5±0.089 and 1.1±0.204 in 0.25% N-CMC and 1% PVP K30, respectively. The solubility of LAN in water was enhanced significantly. LAN15 showed the highest solubility enhancement; that it reported 4.6±0.25 (11.5) times improving in saturation solubility in comparison to pure LA and 4.18 times improving in comparison to LA in the stabilizer solution as represented in Figure 5. Water-soluble Poly vinyl pyrrolidone derivatives have been used conveniently to enhance the bioavailability of numerous drugs with low aqueous solubility like indomethacin, tolbutamide, and nifedipine.31 According to our study N CMC showed the lowest ability to enhance the solubility of LA compared with HPMC K15M and PVP K30, which could be interpreted on the base of the structure of the LA and N CMC.32–34
In vitro Dissolution Study
Based on particle size, encapsulation, and saturation solubility results; LANs formulations prepared with 1% stabilizer and 30-min sonication time were studied for in vitro dissolution study. Dissolution profiles of pure LA, LAN6, LAN15, and LAN24 are presented in Figure 6. A significant improvement in the dissolution rate of LA from nanoparticles in comparison to pure drug. In the first 10 min, 24.5±4.5%, 35.26±3.5% and 15.25± 3.3% of LA were released from LAN6, LAN15, and LAN24, respectively, compared to 5.17±0.85% of pure LA. After 50 min only 20.12±1.85% of LA was dissolved while 85.25±3.8%, 99.1±1.09% and 80.54±3.1% of LA were released from LAN6, LAN15, and LAN 24, respectively. Many studies reported the enhancement of the solubility of poor water-soluble drugs by using solubilizing agents, such as the soluble methylcellulose derivatives, soluble PVP grades and soluble form of chitosan polymers. Acetaminophen in tablets formulated with 4% PVP released the drug more rapidly than tablets formulated with gelatin or hydroxypropyl cellulose.35 Reverse relationship between dissolution and particle size was proved by other studies, which discussed the relation between particle size and the solubility of the drug.27,35,36
 |
Figure 6 Comparative in vitro dissolution profiles of pure LA, LAN6, LAN15 and LAN24. |
Stability Study
The stability of LANs at different storage conditions is an important issue, to evaluate the impact of temperature on the possibility of particle size growth and/or drug degradation upon storage. LANs 6 and LANs 15 prepared at optimized formulation conditions were studied for its stability at temperatures 4°C, 25°C, and 40°C. The selected formulations were analyzed for physical appearance, drug content and particle size growth at intervals 10, 15, 30, 45, 60, 75, and 90 days. No physical changes in the color, texture, and appearance of any formula were observed all over the test duration. Figure 7 shows the results of stability tests, it reported that neither significant crystal growth nor drug loss was observed for both formulations at 4°C with stable nanosuspension over 90 days. A negligible increase in particle size was observed at 25°C; that 276± 6.9nm and198±5.5 was recorded for LAN6 and LAN15, respectively, with non-significant loss in drug content in both formulations (Figure 7A and B). However, an obvious growth in particle size more than a 75 nm increase in particle size for LAN6 and more than 61 nm increase in particle size for LAN15 occurred at 40°C at the end of 3 months as shown in Figure 7C. The results could be interpreted on the base that; at a higher temperature, the growth of the size of the nanoparticles is due to Ostwald ripening.37
 |
Figure 7 Stability of LAN6 & LAN15 in terms of particle size, drug loading at (A) 4°C (B) 25°C, and (C) 40°C. Abbreviations: PZ, particle size; %EE, percentage entrapment efficiency. |
In vivo Bioavailability Study
LAN15 showed accepted results in PZ, solubility, in vitro release and stability studies for that it was selected for further investigation for in vivo bioavailability study. Plasma concentrations of LA after oral administration of LAN15 and commercial tablets showed that LAN15 enhanced the absorption of LA compared with commercial tablets. Maximum plasma concentrations of LA were 2.41±0.3 and 1.66± 0.36 µg/mL for LAN15 and commercial tablets, respectively (Table 2 and Figure 8). There was a 1.45-fold enhancement of Cmax of LAN15 as compared to commercial tablets. The area under the plasma concentration–time curve (AUC) of LA after oral administration of Cholyasis® was 20.61±1.20 μg/mL h. The AUC of LA after LAN15 oral administration was 22.56 ± 2.3 μg/mL h. The time to reach the maximum plasma concentration (Tmax), of LA in the LAN15 showed no significant (3±0.12 h) variations compared to those of the commercial tablets. The superior bioavailability of LA after oral administration of LAN could be interpreted on the base of faster absorption of LAN. This could be explained as the enhancement in its saturation solubility due to the large surface area.38,39 Nanocrystals of Aceclofenac, Artemether and Glimbride showed higher solubility, dissolution rate and ultimately faster rate of absorption compared with pure drugs.24,40,41
 |
Table 2 Pharmacokinetic Parameters of LA Following an Oral Administration of LAN15 and Marketed Tablets in Rats |
 |
Figure 8 LA plasma concentration (mean ± SE) time profiles in rats after oral administrations of LAN15 and commercial tablets (Cholilysis®10mg). |
Conclusion
Improving the therapeutic efficacy of LA was achieved by precipitation–ultrasonication technique. Precipitation–ultrasonication was operated under different processing conditions for producing stabilized nanoparticles of LA. The optimized condition was found at 1% (w/v) PVP K30 with 30-min ultrasonication and input 300 W, with 3-s pauses. The in vitro dissolution study of LA was improved distinctly by employing this method. Optimum LAN formula showed a marked enhancement in the bioavailability of LA compared to commercial tablets. The study proved that nanoparticles formulated under optimum conditions can enhance the therapeutic activity of Lovastatin.
Acknowledgments
Researcher would like to thank the Deanship of Scientific Research, Qassim University for funding publication of this project. Author also appreciates the help of the animal house department and QC lab.
Disclosure
The author reports no conflicts of interest in this work.
References
1. Sabzevari A, Adibkia K, Hashemi H, et al. Polymeric triamcinolone acetonide nanoparticles as a new alternative in the treatment of uveitis: in vitro and in vivo studies. Eur J Pharm Biopharm. 2013;84(1):63–71. doi:10.1016/j.ejpb.2012.12.010
2. Charman WN. Lipids, lipophilic drugs, and oral drug delivery-some emerging concepts. J Pharm Sci. 2000;89(8):967–978. doi:10.1002/1520-6017(200008)89:8<967:AID-JPS1>3.0.CO;2-R
3. Neuvonen PJ, Backman JT, Niemi M. Pharmacokinetic comparison of the potential over-the-counter statins simvastatin, lovastatin, fluvastatin and pravastatin. Clin Pharmacokinet. 2008;47(7):463–474. doi:10.2165/00003088-200847070-00003
4. De Castro ML, Priego-Capote F. Ultrasound-assisted crystallization (sonocrystallization). Ultrason Sonochem. 2007;14(6):717–724. doi:10.1016/j.ultsonch.2006.12.004
5. Pereira VJ, Matos RL, Cardoso SG, et al. A new approach to select solvents and operating conditions for supercritical antisolvent precipitation processes by using solubility parameter and group contribution methods. J Supercrit Fluids. 2013;81:128–146. doi:10.1016/j.supflu.2013.05.010
6. Merisko-Liversidge EM, Liversidge GG. Drug nanoparticles: formulating poorly water-soluble compounds. Toxicol Pathol. 2008;36(1):43–48. doi:10.1177/0192623307310946
7. Merisko-Liversidge E, Liversidge GG, Cooper ER. Nanosizing: a formulation approach for poorly-water-soluble compounds. Eur Pharm Sci. 2003;18(2):113–120. doi:10.1016/S0928-0987(02)00251-8
8. Matteucci ME, Hotze MA, Johnston KP, Williams RO. Drug nanoparticles by antisolvent precipitation: mixing energy versus surfactant stabilization. Langmuir. 2006;22(21):8951–8959.
9. Meyer MC. Bioavailability and bioequivalence of drugs. In: Swarbik J, editor. Encyclopedia of Pharmaceutical Technology.
10. Patel M, Tekade A, Gattani S, Surana S. Solubility enhancement of lovastatin by modified locust bean gum using solid dispersion techniques. AAPS PharmSciTech. 2008;9(4):1262–1269. doi:10.1208/s12249-008-9171-4
11. Suresh G, Manjunath K, Venkateswarlu V, Satyanarayana V. Preparation, characterization, and in vitro and in vivo evaluation of lovastatin solid lipid nanoparticles. AAPS PharmSciTech. 2007;8:162–170. doi:10.1208/pt0801024
12. Bartos C, Ambrus R, Sipos P, et al. Study of sodium hyaluronate-based intranasal formulations containing micro-or nanosized meloxicam particles. Int J Pharm. 2015;491(1–2):198–207. doi:10.1016/j.ijpharm.2015.06.046
13. Adami R, Osseo LS, Huopalahti R, Reverchon E. Supercritical AntiSolventmicronization of PVA by semi-continuous and batch processing. J Supercrit Fluids. 2007;42(2):288–298. doi:10.1016/j.supflu.2007.04.002
14. Zhang X, Xia Q, Gu N. Preparation of all-trans retinoic acid nanosuspensions using a modified precipitation method. Drug Dev Ind Pharm. 2006;32(7):857–863. doi:10.1080/03639040500534184
15. Wu TY, Guo N, Teh CY, Hay JX. Advances in Ultrasound Technology for Environmental Remediation. Heidelberg: Springer; 2012.
16. Bhakay A, Rahman M, Dave R, Bilgili E. Bioavailability enhancement of poorly water-soluble drugs via nanocomposites: formulation processing aspects and challenges. Pharmaceutics. 2018;10(3):86. doi:10.3390/pharmaceutics10030086
17. Li Z, Seeram NP, Lee R, et al. Plasma clearance of lovastatin versus Chinese red yeast rice in healthy volunteers. J. Altern. Complement. Med. 2005;11(6):1031–1038. doi:10.1089/acm.2005.11.1031
18. Chen CH, Uang YS, Wang ST, Yang JC, Lin CJ. Interaction between red yeast rice and CYP450 enzymes/P-glycoprotein and its implication for the clinical pharmacokinetics of lovastatin. Evid Based Complement Alternat Med. 2012;1:1–10.
19. Qigang G, Wei C, Xianming H. Development of lovastatin-loaded poly(lactic acid) microspheres for sustained oral delivery: in vitro and ex vivo evaluation. Drug Des Devel Ther. 2015;9:791–879. doi:10.2147/DDDT.S76676
20. Vikas AS, Vipin K, Mahesh K. Dissolution enhancement of drugs part II: effect of carriers. Int J Health Res. 2009;2(2):207–223.
21. Slater EE, MacDonald JS. Mechanism of action and biological profile of HMG Co A reductase inhibitors: a new therapeutic alternative. Drugs. 1998;36(3):72–82. doi:10.2165/00003495-198800363-00016
22. Hajjaj H, Niederberger P, Duboc P. Lovastatin biosynthesis by Aspergillus terreus in a chemically defined medium. Appl Environ Microbiol. 2001;67(6):2596–2602. doi:10.1128/AEM.67.6.2596-2602.2001
23. Mehrdad H, Najmeh Z, Mohammad SH. A simple and sensitive HPLC-UV method for quantitation of lovastatin in human plasma: application to a bioequivalence study. Biol Pharm Bull. 2009;32(9):1600–1603. doi:10.1248/bpb.32.1600
24. Rahim H, Sadiq A, Khan S, et al. Fabrication and characterization of glimepiride nanosuspension by ultrasonication-assisted precipitation for improvement of oral bioavailability and in vitro α-glucosidase inhibition. Int J Nanomed. 2019;14:6287–6296. doi:10.2147/IJN.S210548
25. Rakesh P, Madhabhai P. Preparation, characterization, and dissolution behavior of a solid dispersion of simvastatin with polyethylene glycol 4000 and polyvinylpyrrolidone K30. J Dispers Sci Technol. 2008;29(2):193–204. doi:10.1080/01932690701706946
26. Diehl KH, Hull R, Morton D, Pfister R. A good practice guide to the administration of substances and removal of blood, including routes and volumes. J Appl Toxicol. 2001;21:15–23. doi:10.1002/jat.727
27. Rabinow BE. Nanosuspensions in drug delivery. Nat Rev Drug Discov. 2004;3(9):785–796. doi:10.1038/nrd1494
28. Khan S, Matas M, Plakkot S, Anwar J. Nanocrystal recovery by use of carrier particles. Cryst Growth Des. 2014;14:1003–1009. doi:10.1021/cg401432m
29. Alshweiat A, Katona G, Csóka I, Ambrus R. Design and characterization of loratadine nanosuspension prepared by ultrasonic-assisted precipitation. Eur J Pharm Sci. 2018;122:94–104. doi:10.1016/j.ejps.2018.06.010
30. Xinggang Y, Weisan P. Fabrication of carvedilol nanosuspensions through the anti-solvent precipitation–ultrasonication method for the improvement of dissolution rate and oral bioavality. AAPS Pharm SciTech. 2012;13(1):295–304. doi:10.1208/s12249-011-9750-7
31. Jijun F, Lishuang X, Xiaoli W, et al. Nimodipine (NM) tablets with high dissolution containing NM solid dispersions prepared by hot-melt extrusion. Drug Dev. Ind. Pharm. 2011;37(8):934–944. doi:10.3109/03639045.2010.550301
32. Cai B, Zhong T, Chen P, et al. Preparation, characterization and in vitro release study of drug-loaded sodium carboxymethylcellulose/chitosan composite sponge. PLoS One. 2018;13(10):62–75. doi:10.1371/journal.pone.0206275
33. Wu YB, Yu SH, Mi FL. Preparation and characterization on mechanical and antibacterial properties of chitosan/cellulose blends. Carbohydr Polym. 2004;57(4):435–440. doi:10.1016/j.carbpol.2004.05.013
34. Jayakumar R, Menon D, Manzoor K, Nair S, Tamura H. Biomedical applications of chitin and chitosan based nanomaterials—a short review. Carbohydr Polym. 2010;82(2):227–232. doi:10.1016/j.carbpol.2010.04.074
35. Patel TB, Patel LD. Formulation and development strategies for drugs insoluble in gastric fluid. Int Res J Pharm. 2012;3(1):106–113.
36. Matteucci ME. Drug nanoparticles by antisolvent precipitation: mixing energy versus surfactant stabilization. Langmuir. 2006;22(21):8951–8959.
37. Deng JL, Liu F. Understanding the structure and stability of paclitaxel nanocrystals. Int J Pharm. 2010;390(2):242–249. doi:10.1016/j.ijpharm.2010.02.013
38. Junghanns J, Müller RH. Nanocrystal technology, drug delivery and clinical applications. Int J Nanomedicine. 2008;3(3):295–309. doi:10.2147/ijn.s595
39. Hintz RJ, Johnson KC. The effect of particle size distribution on dissolution rate and oral absorption. Int J Pharma. 1989;51(1):9–17. doi:10.1016/0378-5173(89)90069-0
40. Shah SMH, Ullah F, Khan S, et al. Smart nanocrystals of artemether: fabrication, characterization, and comparative in vitro and in vivo antimalarial evaluation. Drug Des Devel Ther. 2016;10:3837–3850. doi:10.2147/DDDT.S114962
41. Haroon R, Abdul Sadiq SK, Khan MA, et al. Aceclofenac nanocrystals with enhanced in vitro, in vivo performance: formulation optimization, characterization, analgesic and acute toxicity studies. Drug Des Devel Ther. 2017;11:2443–2452. doi:10.2147/DDDT.S140626
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

