Back to Journals » Substance Abuse and Rehabilitation » Volume 5
Nalmefene: a new approach to the treatment of alcohol dependence
Received 28 February 2014
Accepted for publication 19 May 2014
Published 8 August 2014 Volume 2014:5 Pages 87—94
DOI https://doi.org/10.2147/SAR.S45666
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
François Paille, Hervé Martini
Department of Addiction Treatment, University Hospital, Vandœuvre-lès-Nancy, France
Abstract: Reduction of alcohol consumption is not yet a widely accepted treatment objective for alcohol-dependent patients, as abstinence is often considered to be the only possible objective in this situation. However, various studies have demonstrated the value of proposing these two options to such patients. Firstly, reduction of alcohol consumption very significantly reduces the risk of alcohol-related damage, and also modifies the patient's and the doctor's perception of the disease, resulting in improved access to care and better patient adherence with the proposed treatment objective and consequently better clinical results. Recent studies have shown that some medicinal products can help patients reduce their alcohol consumption. One such product, nalmefene, has been granted European marketing authorization and is now being released onto the market in various countries. The ESENSE 1 and 2 studies in alcohol-dependent patients showed that, in combination with BRENDA, a psychosocial intervention focusing on reinforcement of motivation and treatment adherence, nalmefene significantly reduced the number of heavy drinking days and mean daily total alcohol consumption versus placebo. This reduction was more marked in the marketing authorization target population, ie, patients with a high or very high drinking risk level according to World Health Organization criteria. Another original feature of this molecule is that it can be used as needed if the patient perceives a risk of drinking, which is a more flexible approach and more likely to ensure the patient's active involvement in the treatment of his/her disease. This molecule opens up interesting and original therapeutic prospects in the treatment of alcohol dependence.
Keywords: alcohol dependence, reduction, consumption, damage reduction, drug therapy, nalmefene
Letter to the editor has been published
Corrigendum has been published
A second letter to the editor has been received and published for this article
Introduction
Alcohol dependence is a major public health problem in both Europe and the USA, and more generally throughout the world. Despite its high prevalence and its multiple and serious consequences for patients and society, the management of alcohol dependence remains largely inadequate. A study of the use of mental health services in Europe showed that only 8% of patients with alcohol abuse or alcohol dependence were actively treated, while the corresponding figure in the USA was approximately 25%.1–3 Only about 10% of patients in the USA receive the care recommended for alcohol dependence.4
The reasons for this situation are multiple: stigmatization of this disease and the patient’s shame causing them not to seek help; resistance to the idea of total abstinence; often limited motivation as a result of the patient being referred by family members, the court, or an employer; a low level of confidence in the capacity to remain abstinent on the part of patients and in the ability to help on the part of doctors; and finally, delayed management, although early intervention is much less intensive, does not necessarily imply abstinence and can prevent progression to dependence and its complications.5,6
Some authors have proposed a more pragmatic approach to the management of alcohol-dependent patients, whereby reduction of alcohol consumption is part of a more global risk and damage reduction strategy.7,8 Alcohol-dependent patients do not constitute a homogeneous group, because each patient who enters a health care process has different objectives, ranging from abstinence to reduction of consumption. Individuals who are not yet ready or not yet able to commit themselves to total abstinence may seek to reduce the amount they drink per occasion and work toward a goal of abstinence.7 Controlled drinking can be a transient period in the patient’s management trajectory.9
The therapeutic objective is no longer rigidly determined but, in line with the transtheoretical model of behavior change proposed by Prochaska, is adapted to the patient’s current stage of change.10
Although abstinence remains an appropriate objective to be systematically proposed in alcohol-dependent patients, the objective of controlled drinking has been proposed by several countries in the context of clinical practice guidelines and consensus conferences. For example, in the UK, the National Institute for Health and Clinical Excellence suggests that a controlled drinking objective can be proposed when the subject does not wish to be totally abstinent.11 In 2005, The National Institute on Alcohol Abuse revised their clinical guidelines.12 In Australia, this alcohol reduction strategy has also been proposed as an alternative to abstinence for patients presenting low levels of dependence.13
The treatment of alcohol dependence is based on a combination of drug therapy and psychosocial management.14,15 Many approaches have been proposed, and several have demonstrated efficacy in terms of abstinence, such as cognitive behavioral therapy, motivational enhancement, social skills training, and case management.16
Only a few drug treatments are indicated in the treatment of alcohol dependence, ie, oral and long-release injectable naltrexone, acamprosate, disulfiram, and sodium oxybate (only marketed in Austria and Italy in this indication), but their efficacy is limited.17–19 Off-label use of other agents, such as baclofen, is not unusual in France.
To date, all agents approved for the treatment of alcohol dependence are indicated as an aid to maintenance of total abstinence and none are indicated to reduce alcohol consumption. Molecules such as nalmefene and baclofene could broaden the treatment objectives, especially reduction of alcohol consumption, an objective which is more readily accepted by some patients. One of the major challenges for pharmacologic research in the field of alcohol dependence is to find other more effective and better tolerated molecules acting on other neurotransmitter systems and targets.17–20
This review presents the recent scientific data for nalmefene (Selincro®; Lundbeck, Valbi, Denmark), describes the value of this molecule in reducing alcohol consumption in alcohol-dependent patients, and discusses some practical aspects of its use.
Nalmefene
The opioid system is involved in alcohol dependence. Alcohol consumption stimulates endogenous release of opioids, which bind to mu and delta receptors, thereby increasing the release of dopamine in the nucleus accumbens, which induces reward and positive reinforcement effects.21 Antagonists of this system, including naltrexone and nalmefene, are able to reduce alcohol consumption in humans by reducing the positive reward effect of alcohol, as well as its sedative and dysphoric properties. These agents reduce alcohol craving in response to external cues. Naltrexone is already marketed in many countries for the treatment of alcohol dependence.
However, unlike naltrexone, which is a relatively pure mu and delta receptor antagonist, nalmefene has a partial agonist effect on kappa receptors. The first animal studies showed that stimulation of kappa receptors is able to antagonize the acute reward and positive reinforcement effects of drugs by decreasing dopamine in the nucleus accumbens.22,23 It was therefore suggested that nalmefene could be more effective than naltrexone in the treatment of alcohol dependence. In alcohol-dependent rats, peripheral administration of nalmefene appeared to be more effective than naltrexone in decreasing self-administration of alcohol.24 However, the role of the dynorphin (DYN)/kappa receptor (KOR) system in heavy drinking is complex and still poorly elucidated. Recent studies have shown that acute alcohol intake stimulates the release of DYN, the endogenous ligand of KOR, which induces dysphoria and anhedonia in humans and aversive behavior in animals.25,26
Dysphoric and anhedonic properties of an overactive DYN/KOR system could promote the excessive seeking and consumption observed in alcohol-dependent animals.24,27 KOR antagonists selectively reduce the increased alcohol consumption induced by dependence without affecting nondependent animals.24,28,29 Nealy et al also showed that administration of nalmefene into the nucleus accumbens more markedly reduced self-administration of alcohol in dependent rats than in nondependent rats and that this phenomenon was related to KOR.28
The hypothesis proposed to explain this phenomenon is that upregulation of the DYN/KOR system due to neuroadaptation during the pathogenesis of alcohol dependence results in hyperactivity of this system, which is responsible for the development of a negative reinforcement effect of alcohol.25–27 Previous studies have demonstrated increased levels of prodynorphin messenger RNA and DYN levels in the nucleus accumbens, as well as increased expression of KOR messenger RNA.30,31
Under these conditions, a partial agonist like nalmefene could therefore act as a functional antagonist by limiting DYN/KOR hyperactivity, thereby contributing to reduce self-administration phenomena in alcohol-dependent rats.27
From a pharmacokinetic point of view, nalmefene is rapidly absorbed after oral administration. The peak plasma level is reached about 90 minutes after ingestion. Protein binding is low and metabolism is mainly hepatic with renal elimination. The plasma half-life is about 12 hours.
Clinical studies
Efficacy
The first study by Mason et al, published in 1994, was a randomized, double-blind, placebo-controlled trial conducted in a small group of alcohol-dependent patients (n=21) treated for 12 weeks by either nalmefene at a daily dosage of 10 mg (n=7) or 40 mg (n=7), or placebo (n=7). The results indicated a significant decrease in the number of drinking days (P≤0.09) and the number of drinks per drinking day (P≤0.04) in patients treated with nalmefene compared with placebo.32
A second study by the same team was conducted in 105 alcohol-dependent outpatients who were abstinent at the time of inclusion.33 Subjects received nalmefene at a dosage of 20 mg or 80 mg per day or placebo for 12 weeks. A weekly session of cognitive behavioral therapy was also proposed in addition to drug treatment. No significant difference was demonstrated between the two doses of nalmefene, but more patients relapsed with placebo (odds ratio [OR] 2.4; 95% confidence interval [CI] 1.05–5.59).
The third study, by Anton et al, concerned 270 recently abstinent patients randomized to four treatment arms, ie, nalmefene 5 mg, 20 mg, or 40 mg, or placebo.34 Drug treatment was associated with motivational enhancement therapy. With a follow-up of 12 weeks, all patients had decreased their alcohol consumption, but no significant difference was observed between the four arms.
Following the discordant results of these various studies, often conducted using small sample sizes and for short durations (12 weeks), Karhuvaara et al conducted a new, more original multicenter, double-blind, placebo-controlled study in 403 patients, designed to evaluate the capacity of nalmefene to decrease alcohol consumption over 28 weeks.35 In contrast with the usual studies in which treatment is taken regularly every day at a fixed dose, nalmefene was taken “as needed”, ie, the patient took a tablet of nalmefene on the days when he/she perceived an increased risk of drinking and did not take treatment on the other days. The BRENDA psychosocial intervention was proposed in addition to nalmefene. Although alcohol consumption was decreased in both arms, a significantly greater reduction was observed in the nalmefene arm.35
The BRENDA program was developed with this objective in mind and comprises six elements:36,37
- Biopsychosocial evaluation
- Report findings of the evaluation are given to the patient
- Empathy
- Needs collaboratively indentified by the patients and treatment provider
- Direct advice to the patient on how to meet those needs
- Assess reaction of the patient to advice and adjust as necessary for best care.
The first two steps consist of a global evaluation of the patient followed by providing the patient with the findings of this evaluation. These two points correspond to the brief intervention validated by many studies in the field of addiction medicine. BRENDA has been extensively studied and has been demonstrated to be effective in combination with drug therapy.36,37
Understanding of the patient’s situation, or empathy, has also been described as a factor that promotes the therapeutic alliance, as described by Miller in the motivational interview.38 The BRENDA method is therefore largely based on the motivational interview, centered on the patient’s needs and identification of resistance, which tends to decrease treatment adherence and, more broadly, the patient’s adherence with management.
Based on this model, three large-scale international studies evaluated as-needed dosing of nalmefene in order to reduce alcohol consumption in alcohol-dependent patients, assessed in terms of the number of heavy drinking days per month and mean daily total alcohol consumption. These three European multicenter studies39,40,42 constituted the basis for approval of nalmefene for the treatment of alcohol dependence by the European Medicines Agency.
The first multicenter, randomized, double-blind, placebo-controlled study of nalmefene (ESENSE 1, ClinicalTrials.gov identifier NCT00811720) conducted in four countries, ie, Germany, Austria, Finland, and Sweden, was published by Mann et al in 2013.39 This study included 604 alcohol-dependent patients who were randomized to one of two treatment arms, ie, an as needed nalmefene 18 mg (one tablet) arm (n=306) or a placebo arm (n=298). BRENDA psychosocial therapy was also proposed in both arms. The duration of treatment was 24 weeks. Efficacy was assessed in terms of two primary outcomes: modification, between baseline and 6 months, of the number of heavy drinking days per month; and modification of total alcohol consumption. A heavy drinking day was defined as a day during which alcohol consumption was ≥60 g of pure alcohol in men and ≥40 g in women. At 6 months, the authors observed a significant reduction in the number of heavy drinking days in the nalmefene arm. (−2.3 days; 95% CI −3.8, −0.8) compared to the placebo arm Furthermore, on drinking days, patients consumed significantly less alcohol in the nalmefene arm (−11 g/day; 95% CI −16.8, −5.1, Table 1).
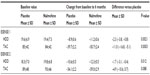  | Table 1 Comparison of the results between nalmefene and placebo on the two primary outcomes of the ESENSE 1 and 2 studies |
The second study (ESENSE 2, ClinicalTrials.gov identifier NCT00812461) was conducted according to a similar methodology in seven other European countries (Spain, France, Portugal, Italy, Belgium, Poland, and the Czech Republic) and included 718 patients, comprising 360 in the placebo arm and 358 in the nalmefene arm.40 Once again, with a follow-up of 6 months, the results demonstrated the superior efficacy of treatment with nalmefene versus placebo with regard to both the number of heavy drinking days (−1.7 day per month; 95% CI −3.1, −0.4; P=0.012) and total alcohol consumption (−4.9g/day; 95% CI −10.6, 0.7; P=0.088, Table 1).
In the ESENSE 1 (n=579), and 2 (n=655) studies, 18%, and 33% of the total population, respectively, considerably reduced their alcohol consumption in the period between screening and randomization. In the subgroup of patients with a high or very high drinking risk level at baseline, 35% experienced improvement due to nonpharmacologic effects in the period between the initial visit (screening) and randomization. At randomization, these patients consumed such a small amount of alcohol that there was little room for further improvement (floor effect). Therefore, the patients who maintained a high or very high drinking risk level at randomization were defined post hoc as the target population.
Analysis of this subgroup of 667 patients (ESENSE 1 and 2 studies) with a high drinking risk level according to World Health Organization criteria (>60 g/day for men, >40 g/day for women, Table 2) showed that nalmefene was more effective than placebo with regard to the two outcomes, but, more importantly, alcohol consumption was more markedly reduced in this subgroup than in the overall population included in the two studies (1,322 patients), ie, an average of 3.2 fewer heavy drinking days (95% CI −4.8, −1.6; P<0.0001) versus 2.0 fewer heavy drinking days (95% CI −3.0, −1.0; P<0.0001) in the total population and −14.3 g of pure alcohol per day (95% CI −20.8, −7.8; P<0.0001) versus −7.6 g/day (95% CI −11.6, −3.5; P<0.0003) in the total population.41,42 A responder analysis of the pooled data from the two studies is provided in Table 3.43
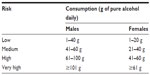  | Table 2 World Health Organization criteria for risk of alcohol consumption on a single drinking day |
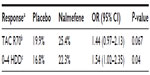  | Table 3 Pooled responder analysis results in patients with a high or very high drinking risk at screening and randomization |
An analysis of secondary outcomes in this population with at least a high drinking risk yielded interesting results. The percentage of patients who lowered their drinking risk to the lowest level according to the World Health Organization criteria (40 g/day of pure alcohol for men and 20 g/day for women) was 43% in the nalmefene arm versus 32% in the placebo arm (P<0.001). A similar difference was observed for patients who lowered their drinking risk by at least two World Health Organization categories (57% with nalmefene versus 42% with placebo; (P<0.001). These studies confirmed the efficacy of nalmefene in reducing alcohol consumption in alcohol-dependent patients treated on an outpatient basis.
Safety
More than 3,000 patients have been exposed to nalmefene in clinical studies. Adverse events were frequently reported in these studies, and were slightly more frequent in the nalmefene arms (81% and 68% in ESENSE 1 and ESENSE 2, respectively) than in the placebo arms (67% and 59% in ESENSE 1 and ESENSE 2, respectively). The most common adverse reactions were nausea, dizziness, insomnia, and headache. However, the majority of these reactions were mild or moderate, associated with initiation of treatment, and of short duration. Confusional state and, rarely, hallucinations and dissociation were reported in the clinical studies. The majority of these reactions were mild or moderate, associated with treatment initiation, and of short duration. A slightly higher percentage of patients discontinued treatment because of adverse events in the nalmefene arms compared with the placebo arms (23% and 6.7% in the nalmefene arms versus 7% and 5.9% in the placebo arms of the ESENSE 1 and 2 studies, respectively). No difference was observed in terms of serious adverse events.39,40
Discussion
Conventionally, the objective of treatment for alcohol dependence is total abstinence and prevention of relapse, while reduction of alcohol consumption is not considered to be a stable objective over time.
The available studies on nalmefene show that this medicinal product is more effective than placebo with regard to reducing the number of heavy drinking days and total alcohol consumption.39,40,42,44
Nalmefene was well tolerated. The most common side effects were nausea, dizziness, insomnia, and headache. The majority of these reactions were mild or moderate and of short duration.
Nalmefene was approved by the European Medicines Agency in February 2013 with the following therapeutic indication:
"Selincro® is indicated for the reduction of alcohol consumption in adult patients with alcohol dependence who have a high drinking risk level, without physical withdrawal symptoms and who do not require immediate detoxification.
Selincro® should only be prescribed in conjunction with continuous psychosocial support focused on treatment adherence and reducing alcohol consumption.
Selincro® should be initiated only in patients who continue to have a high drinking-risk level two weeks after initial assessment…."43
Selincro® must not be used in people who are hypersensitive (allergic) to nalmefene or any of its other ingredients. It must not be used in patients taking opioid medicines, in patients who have current or recent opioid addiction, patients with acute symptoms of opioid withdrawal, or patients in whom recent use of opioids is suspected.
It must also not be used in patients with severe liver or kidney impairment or a recent history of acute alcohol withdrawal syndrome (including hallucinations, seizures, and tremors).
However, prescription of nalmefene in clinical practice raises a number of questions. After the withdrawal period, all treatments currently used to treat alcohol dependence have a single objective, ie, abstinence. However, the results of these treatments remain somewhat disappointing. Few studies have considered reduction of consumption as an effective therapeutic alternative in alcohol-dependent patients. The COMBINE (Combined Pharmacotherapies and Behavioral Interventions for Alcohol Dependence) study demonstrated a reduction in the number of heavy drinking days by combining naltrexone with specific medical management (OR 0.72; 95% CI 0.53–0.98; P=0.02).45 However, new studies have evaluated the efficacy of reduction of consumption in terms of reduction of morbidity and mortality in alcohol-dependent patients only in the last few years.46,47
Recent studies have shown that some agents can help patients reduce their consumption.5,39,40,42,48 Evaluation of new medicinal products designed to achieve this target is potentially very valuable. This approach, better adapted to patients who do not wish (or cannot) remain totally abstinent is able to considerably reduce the damage related to alcohol consumption.49,50 This objective, which is more accessible and better accepted because it more closely corresponds to the patient’s preference, can enable the patient to modify his/her attitude in relation to alcohol dependence.51 This approach would encourage the patient to seek medical attention and would increase the percentage of patients accessing care. Only 30% of patients in the ESENSE 1 study and 40% of those in the ESENSE 2 study had already received previous management for alcohol dependence, which suggests that this type of treatment promotes the patient’s adherence with treatment.39,40 Further, Adamson et al showed that the result of treatment depends on the patient’s initial objective.51 Patients are more likely to achieve their objective that they have chosen themselves as opposed to an objective imposed by the physician. Patients who choose abstinence more often achieve abstinence, while patients who choose reduction of consumption more often achieve this objective. As-needed treatment gives patients a more active role in management of their disease by making them more attentive to the quantity of alcohol consumed and the situations in which they drink. General practitioners, who often feel relatively impotent when the only objective is abstinence, could feel more confident about helping their patients. Reduction of consumption can be either an intermediate objective until the patient understands and accepts the need for abstinence, or, in less severely dependent patients, a realistic long-term objective.8,9
Alcohol-dependent patients do not constitute a homogeneous patient group, but present a diversity of profiles in terms of age, history and severity of heavy drinking, genetic susceptibility, presence or absence of psychiatric comorbidity, and social or family difficulties. The diversity of patient profiles therefore implies the need for personally tailored management for each patient.7,10
The ESENSE 1 and 2 studies showed that significant improvements, usually observed within the first 4 weeks of treatment, were obtained in patients who were already drinking more than 60 g of alcohol per day (for men) or more than 40 g of alcohol per day (for women). In these patients, after 6 months of treatment, the number of heavy drinking days per month with nalmefene decreased from 23 to nine in the first study and from 23 to ten in the second study. Daily alcohol consumption with nalmefene decreased from 102 g to 40 g in the first study and from 114 g to 44 g in the second study. These improvements were better than those observed with placebo by about 2.7–3.7 heavy drinking days a month and about 10–18 g of alcohol per day.39,40
It should be stressed that the efficacy of nalmefene was demonstrated in ESENSE 1 and 2 in a population of alcohol-dependent patients according to the DSM-IV (Diagnostic and Statistical Manual of Mental Disorders, Fourth Edition)52 with a high or very high drinking risk according to World Health Organization criteria. These two studies excluded more severely ill patients with a history of delirium tremens, seizures, major psychiatric illness, or significant liver function test abnormalities. Although abstinence remains the objective of treatment in patients with multiple complications, these patients nevertheless represent a very interesting target population for controlled drinking when abstinence is either refused or impossible for the purposes of harm reduction.
Post hoc analysis of the ESENSE 1 and 2 studies also more clearly defined the population likely to derive the greatest benefit from treatment with nalmefene.42 The ESENSE 2 clearly demonstrated the superior efficacy of treatment in patients who had not modified their consumption between the run-in period and initiation of treatment. This result implies that prescription of nalmefene should be delayed by a period of 2 weeks.39,40,42
In ESENSE 1 and 2, nalmefene was linked to a BRENDA psychosocial intervention designed to achieve motivational reinforcement, management of consumption, and treatment adherence.39,40 Adherence with drug treatment has been extensively studied, especially with naltrexone, and many authors have demonstrated the link between good adherence and abstinence.14,17,53–55 Various methods have been proposed to improve adherence, based on individual decreased intensity (medical) management models or more intensive cognitive behavioral therapy. However, cognitive behavioral therapy requires specifically trained therapists, making it an approach that is poorly accessible to primary care medicine. The objective is therefore to propose a model that reinforces treatment adherence and consequently the chances of success, and can be readily used by primary care providers (eg, general practitioners, nonaddiction specialists, and nurses).
Finally, the role of nalmefene needs to be compared with that of naltrexone. It has been suggested that the difference between these two molecules in terms of their opioid receptor binding profile, especially to KOR, could account for the superior efficacy of nalmefene compared with naltrexone in rats.24 No clinical studies comparing these two products in man are available at the present time.
The safety profiles of these two molecules are fairly similar. Cases of hepatotoxicity have been reported with naltrexone. This type of adverse effect has not been reported with nalmefene, which could constitute an advantage.
Conclusion
Nalmefene appears to be an effective treatment to reduce alcohol consumption in alcohol-dependent patients not wanting to become totally abstinent. It differs from other drug therapies essentially by replacing systematic dosing by “as-needed” dosing adapted to the patient’s clinical situation on a day-to-day basis. Patients therefore take nalmefene when they feel that alcohol consumption is imminent. Nalmefene is well tolerated overall. The main adverse effects are nausea, dizziness, and sleep disturbance, such as insomnia. Drug treatment must be combined with a biopsychosocial approach especially designed to improve adherence with treatment. Further studies are required to define the exact place of nalmefene, compared with drugs at present used in the treatment of alcohol dependence, especially naltrexone.
Disclosure
The authors report no conflicts of interest in this work.
References
Alonso J, Angermeyer MC, Bernert S, et al; ESEMeD/MHEDEA 2000 Investigators, European Study of the Epidemiology of Mental Disorders (ESEMeD) Project. Use of mental health services in Europe: results from the European Study of the Epidemiology of Mental Disorders (ESEMeD) project. Acta Psychiatr Scand Suppl. 2004;420:47–54. | |
Dawson DA, Grant BF, Stinson FS, Chou PS, Huang B, Ruan WJ. Recovery from DSM-IV alcohol dependence: United States, 2001–2002. Addiction. 2005;100(3):281–292. | |
Schuckit MA. Alcohol-use disorders. Lancet. 2009;373(9662):492–501. | |
McGlynn EA, Asch SM, Adams J, et al. The quality of health care delivered to adults in the United States. N Engl J Med. 2003;348(26):2635–2645. | |
Aubin HJ, Daeppen JB. Emerging pharmacotherapies for alcohol dependence: a systematic review focusing on reduction in consumption. Drug Alcohol Depend. 2013;133(1):15–29. | |
Grant BF. Barriers to alcoholism treatment: reasons for not seeking treatment in a general population sample. J Stud Alcohol. 1997;58(4):365–371. | |
Gastfriend DR, Garbutt JC, Pettinati HM, Forman RF. Reduction in heavy drinking as a treatment outcome in alcohol dependence. J Subst Abuse Treat. 2007;33(1):71–80. | |
Van Amsterdam J, van den Brink W. Reduced-risk drinking as a viable treatment goal in problematic alcohol use and alcohol dependence. J Psychopharmacol. 2013;27(11):987–997. | |
Hodgins DC, Leigh G, Milne R, Gerrish R. Drinking goal selection in behavioral self-management treatment of chronic alcoholics. Addict Behav. 1997;22(2):247–255. | |
Prochaska JO. Systems of Psychotherapy: A Transtheoretical Analysis. Homewood, IL, USA: Dorsey Press; 1979. | |
National Institute for Health and Clinical Excellence. Alcohol-use disorders: diagnosis, assessment and management of harmful drinking and alcohol-dependence 2011. Available from: http://www.nice.org.uk/nicemedia/live/13337/53191/53191.pdf. Accessed February 21, 2014. | |
National Institute on Alcohol Abuse and Alcoholism. Helping Patients Who Drink Too Much: A Clinician’s Guide. Bethesda, MD, USA: National Institutes of Health Publications; 2005. | |
Australian Government Department of Health and Ageing. Guidelines for the treatment of alcohol problems, 2009. Available from: http://www.alcohol.gov.au/internet/alcohol/publishing.nsf/Content/877AC32A7ADD8AEECA2576C00007B5C7/$File/evid.pdf. Accessed February 21, 2014. | |
Oslin DW, Lynch KG, Pettinati HM, et al. A placebo-controlled randomized clinical trial of naltrexone in the context of different levels of psychosocial intervention. Alcohol Clin Exp Res. 2008;32(7):1299–1308. | |
Martin GW, Rehm J. The effectiveness of psychosocial modalities in the treatment of alcohol problems in adults: a review of the evidence. Can J Psychiatry. 2012;57(6):350–358. | |
Miller WR, Wilbourne PL. Mesa Grande: a methodological analysis of clinical trials of treatments for alcohol use disorders. Addiction. 2002;97(3):265–277. | |
Garbutt JC. The state of pharmacotherapy for the treatment of alcohol dependence. J Subst Abuse Treat. 2009;36(1):S15–S23. | |
Caputo F, Vignoli T, Grignaschi A, Cibin M, Addolorato G, Bernardi M. Pharmacological management of alcohol dependence: from mono-therapy to pharmacogenetics and beyond. Eur Neuropsychopharmacol. 2014;24(2):181–191. | |
Johnson BA. Update on neuropharmacological treatments for alcoholism: scientific basis and clinical findings. Biochem Pharmacol. 2008;75(1):34–56. | |
Franck J, Jayaram-Lindström N. Pharmacotherapy for alcohol dependence: status of current treatments. Curr Opin Neurobiol. 2013;23(4):692–699. | |
Gianoulakis C. Influence of the endogenous opioid system on high alcohol consumption and genetic predisposition to alcoholism. J Psychiatry Neurosci. 2001;26(4):304–318. | |
Chefer VI, Czyzyk T, Bolan EA, Moron J, Pintar JE, Shippenberg TS. Endogenous kappa-opioid receptor systems regulate mesoaccumbal dopamine dynamics and vulnerability to cocaine. J Neurosci. 2005;25(20):5029–5037. | |
Shippenberg TS, Zapata A, Chefer VI. Dynorphin and the pathophysiology of drug addiction. Pharmacol Ther. 2007;116(2):306–321. | |
Walker BM, Koob GF. Pharmacological evidence for a motivational role of kappa-opioid systems in ethanol dependence. Neuropsychopharmacology. 2008;33(3):643–652. | |
Walker BM, Valdez GR, McLaughlin JP, Bakalkin G. Targeting dynorphin/kappa opioid receptor systems to treat alcohol abuse and dependence. Alcohol. 2012;46(4):359–370. | |
Wee S, Koob GF. The role of the dynorphin-k opioid system in the reinforcing effects of drug of abuse. Psychopharmacology. 2010;210(2):121–135. | |
Kissler JL, Sirohi S, Reis DJ, et al. The one-two punch of alcoholism: role of central amygdala dynorphins/kappa-opioid receptors. Biol Psychiatry. 2014;75(10):774–782. | |
Nealy KA, Smith AW, Davis SM, Smith DG, Walker BM. Ќ-opioid receptors are implicated in the increased potency of intra-accumbens nalmefene in ethanol-dependent rats. Neuropharmacology. 2011;61(1–2):35–42. | |
Walker BM, Zorilla EP, Koob GF. Systemic kappa-opioid receptor antagonism by nor-binaltorphimine reduces dependence-induced excessive alcohol self-administration in rats. Addict Biol. 2011;16(1):116–119. | |
Przewlocka B, Turchan J, Lason W, Przewlocki R. Ethanol withdrawal enhances the prodynorphin system activity in the rat nucleus accumbens. Neurosci Lett. 1997;238(1–2):13–16. | |
D’Addario C, Caputi FF, Rimondini R, et al. Different alcohol exposures induce selective alterations on the expression of dynorphin and nociceptin systems related genes in rat brain. Addict Biol. 2013;18(3):425–433. | |
Mason BJ, Ritvo EC, Morgan RO, et al. A double-blind, placebo-controlled pilot study to evaluate the efficacy and safety of oral nalmefene HCl for alcohol dependence. Alcohol Clin Exp Res. 1994;18(5):1162–1167. | |
Mason BJ, Salvato FR, Williams LD, et al. A double-blind, placebo-controlled study of oral nalmefene for alcohol dependence. Arch Gen Psychiatry. 1999;56(8):719–724. | |
Anton RF, Pettinati H, Zweben A, et al. A multi-site dose ranging study of nalmefene in the treatment of alcohol dependence. J Clin Psychopharmacol. 2004;24(4):421–428. | |
Karhuvaara S, Simojoki K, Virta A, et al. Targeted nalmefene with simple medical management in the treatment of heavy drinkers: a randomized double-blind placebo-controlled multicenter study. Alcohol Clin Exp Res. 2007;31(7):1179–1187. | |
Volpicelli JR, Pettinati HM, McLellan AT, O’Brien CP. Enhanced Medication and Treatment Adherence for Addiction Treatment. The BRENDA Model. New York, NY, USA: Guilford Press; 2001. | |
Starosta AN, Leeman RF, Volpicelli JR. The BRENDA model: integrating psychosocial treatment and pharmacotherapy for the treatment of alcohol use disorders. J Psychiatr Pract. 2006;12(2):80–89. | |
Miller WR. Motivational Interviewing. Preparing People for Change. New York, NY, USA: Guilford Press; 2002. | |
Mann K, Bladström A, Torup L, et al. Extending the treatment options in alcohol dependence: a randomized controlled study of as-needed nalmefene. Biol Psychiatry. 2013;73(8):706–713. | |
Gual A, He Y, Torup L, et al. A randomised, double-blind, placebo-controlled, efficacy study of nalmefene, as-needed use, in patients with alcohol dependence. Eur Neuropsychopharmacol. 2013;23(11):1432–1442. | |
World Health Organization. International Guide for Monitoring Alcohol Consumption and Related Harm. Available from: http://whqlibdoc.who.int/hq/2000/who_msd_msb_00.4.pdf. Accessed Feb 2014. | |
Van den Brink W, Aubin HJ, Bladström A, Torup L, Gual A, Mann K. Efficacy of as-needed nalmefene in alcohol-dependent patients with at least a high drinking risk level: results from a subgroup analysis of two randomized controlled 6-month studies. Alcohol Alcohol. 2013;48(6):570–578. | |
European Medicines Agency. European public assessment report (EPAR) for Selincro. Available from: http://www.ema.europa.eu/ema/index.jsp?curl=pages/medicines/human/medicines/002583/human_med_001620.jsp&mid=WC0b01ac058001d124. Accessed May 20, 2014. | |
Keating GM. Nalmefene: a review of its use in the treatment of alcohol dependence. CNS Drugs. 2013;27(9):761–772. | |
Anton RF, O’Malley SS, Ciraulo DA, et al. Combined pharmacotherapies and behavioral interventions for alcohol dependence: the COMBINE study: a randomized controlled trial. JAMA. 2006; 295(17):2003–2017. | |
Rehm J, Zatonksi W, Taylor B, Anderson P. Epidemiology and alcohol policy in Europe. Addiction. 2011;106 Suppl 1:11–19. | |
Roerecke M, Gual A, Rehm J. Reduction of alcohol consumption and subsequent mortality in alcohol use disorders: systematic review and meta-analyses. J Clin Psychiatry. 2013;74(12):1181–1189. | |
Rösner S, Leucht S, Lehert P, Soyka M. Acamprosate supports abstinence, naltrexone prevents excessive drinking: evidence from a meta-analysis with unreported outcomes. J Psychopharmacol. 2008;22(1):11–23. | |
Marlatt GA, Witkiewitz K. Harm reduction approaches to alcohol use: health promotion, prevention, and treatment. Addict Behav. 2002;27(6):867–886. | |
Marlatt GA, Witkiewitz K. Update on harm-reduction policy and intervention research. Annu Rev Clin Psychol. 2010;6:591–606. | |
Adamson SJ, Heather N, Morton V, Raistrick D. UKATT Research Team. Initial preference for drinking goal in the treatment of alcohol problems: II. Treatment outcomes. Alcohol Alcohol. 2010;45(2):136–142. | |
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. Fourth Edition. Washington, DC: American Psychiatric Association; 1994. | |
Swift R, Oslin DW, Alexander M, Forman R. Adherence monitoring in naltrexone pharmacotherapy trials: a systematic review. J Stud Alcohol Drugs. 2011;72(6):1012–1018. | |
Vuoristo-Myllys S, Lipsanen J, Lahti J, Kalska H, Alho H. Outcome predictors for problem drinkers treated with combined cognitive behavioral therapy and naltrexone. Am J Drug Alcohol Abuse. 2014;40(2):103–110. | |
Zweben A, Pettinati HM, Weiss RD, et al. Relationship between medication adherence and treatment outcomes: the COMBINE study. Alcohol Clin Exp Res. 2008;32(9):1661–1669. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
