Back to Journals » OncoTargets and Therapy » Volume 13
miR-424-3p Contributes to the Malignant Progression and Chemoresistance of Gastric Cancer
Authors Li Y, Liu H, Cui Y, Chen H, Cui X, Shao J, Su F, He X
Received 7 September 2020
Accepted for publication 9 November 2020
Published 26 November 2020 Volume 2020:13 Pages 12201—12211
DOI https://doi.org/10.2147/OTT.S280717
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Nicola Silvestris
Yongyuan Li,1,2,* Hongjie Liu,3,* Yu Cui,1 Hekai Chen,1 Xuejun Cui,1 Jianping Shao,1 Feng Su,1 Xianghui He2
1Department of General Surgery, The Fifth Central Hospital, Tianjin 300450, People’s Republic of China; 2Department of General Surgery, Tianjin Medical University General Hospital, Tianjin 300052, People’s Republic of China; 3Department of Radiology, The Fifth Central Hospital, Tianjin 300450, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Xianghui He
Department of General Surgery, Tianjin Medical University General Hospital, Tianjin 300052, People’s Republic of China
Email [email protected]
Background: Gastric cancer (GC) is one of the most common and lethal malignancies worldwide. Therefore, a better understanding of the mechanism of its malignant progression and chemoresistance will be helpful for the treatment of patients with GC.
Methods: The gene expression profiles downloaded from GEO database and the TargetScan Human were used to identify the key regulation model based on miRNA by bioinformatics analyses. The regulation of miRNA to target was clarified by luciferase assay, qPCR, and Western blotting. Then, the in vitro and in vivo experiments were further conducted by overexpression or knockdown of miRNA and/or target to examine the regulation effects and clarify the mechanism.
Results: In the present study, miR-424-3p was identified to be differentially expressed among normal gastric, GC, and chemoresistant GC tissues. Target analysis results indicated that ABCC2, a chemoresistance-related gene, was a regulated target of miR-424-3p. The in vitro and in vivo experiment results further demonstrated that miR-424-3p relied on ABCC2-induced chemoresistance to promote GC proliferation and metastasis.
Conclusion: Overall, this study revealed that miR-424-3p contributed to the malignant progression and chemoresistance of GC. Thus, miR-424-3p could be a potential target for the treatment of GC.
Keywords: gastric cancer, miR-424-3p, chemoresistance, malignant progression
Introduction
Gastric cancer (GC) is a very heterogeneous tumor with a quite complex genotype. The drug resistance mechanism of GC is quite complex due to the microenvironment.1,2 Chemotherapy plays an important role in GC treatment, especially in the treatment of patients with advanced GC, and can often prolong the survival of patients by inhibiting the spread and metastasis.3 However, drug resistance in chemotherapy has always been a difficult problem in clinical practice and is also an important cause of treatment failure and patient deaths.4 The mechanism of chemotherapy resistance is complex, which is mostly related to the increase of drug efflux of cancer cells mediated by ABC transporter protein, the abnormality of cell apoptosis mechanism, and the change of some enzyme activity in cancer cells, reducing the sensitivity of cancer cells to chemotherapy drugs.5–7 Given that chemotherapy resistance is a key factor that affects the prognosis of advanced GC, the mechanism of drug resistance must be further studied.
Cisplatin (DDP) is a common platinum drug used in the treatment of gastric, colorectal, and pancreatic cancers. When DDP enters the cell, it binds to nucleophiles (mainly DNA but also RNA and proteins).8 As a DNA crosslinking agent, DDP can target DNA. Platinum atoms covalently bind to guanine (G) on DNA strands to form intra- and inter-strand crosslinks that interfere with DNA replication and transcription.9 However, intrinsic or acquired resistance to DDP can still counteract its killing effect. Therefore, elucidating the mechanism of DDP resistance and determining effective and targeted strategies to reverse resistance are necessary.
MicroRNAs (miRNAs) are non-coding RNAs that can regulate the expression level of target genes after transcription and participate in the occurrence and development of tumors as oncogenes or tumor suppressor genes.10 In malignant metastatic tumors, the expression of miRNAs is generally downregulated, which increases the expression and function of chemokines, receptors, and other proteins related to tumor cell metastasis and invasion and promotes the occurrence and development of tumors.11,12
High-throughput gene chips and new generation of sequencing technology provide conditions for exploring the molecular typing of cancer, which is helpful to search for biomarkers with excellent prediction effect and perform research on the clinical individualized treatment of GC.13,14 The results of this study confirmed the important role of miR-424-3p in mediating the DDP resistance of GC cells. These results not only elucidate the molecular mechanism of tumor resistance to chemotherapy to some extent but also reveal that miR-424-3p can be used as a tumor resistance marker to guide clinical medication, which has important clinical application value.
Materials and Methods
Omics Analysis
The miRNA data in normal, GC, and chemoresistant GC tissues of GSE3007015 used in this study were downloaded from the GEO database. Among which, 34 healthy volunteers (normal), 90 pre-treatment gastric cancer samples (GC), and 8 post-treatment samples (chemoresistant GC) were included. The differentially expressed miRNA of miR-424-3p was used for further analysis. TargetScan, miRDB, and miRWalk databases were used to analyze the target mRNAs of miR-424-3p, and the intersected mRNAs predicted by the three databases were considered to be the targets of miR-424-3p.
Cell Culture and Transfection
The human gastric mucosal cell GES-1, human GC cell line SGC-7901, and chemoresistant GC cell line SGC-7901/DDP were obtained from the American Type Culture Collection. These cells were cultured in RPMI-1640 medium (Hyclone, USA) with 10% fetal bovine serum (Hyclone, USA) at 37°C in 5% CO2 atmosphere. The 1 μg/mL of DDP (J&K, China) was added to the corresponding cell group. The plasmids of pGL3-ABCC2-wt, pGL3-ABCC2-mut, pcDNA3.1-ABCC2, shRNA-ABCC2, miR-424-3p mimics, miR-424-3p inhibitor, and control vectors were obtained from GeneCopoeia (Guangzhou, China), Obio technology (Shanghai, China), and some of them were constructed by ourselves. The plasmids were transfected into cells by using transfection reagents (Roche, Switzerland).
qPCR
The total RNA in cells was isolated with TRlzol reagent (Invitrogen, USA). Reverse transcription was performed using the Quantscript RT Kit (Tiangen, China). An SYBR RT-PCR Kit (Tiangen, China) was used for transcript quantification with specific primers. The expression levels were quantified using the 2−ΔΔCT method, with β-actin as the internal control. The reverse primer of RT-PCR was provided by the Quantscript RT Kit. The forward primer sequences of miR-424-3p and ABCC2 were as follows: miR-424-3p: 5′- CAGCAGCAAUUCAUGUUUUGAA −3′, ABCC2: 5′-TGAAAAACAGAATGGGACCGA −3′. The reverse primer of qPCR was provided in the SYBR RT-PCR Kit.
Luciferase Reporter Assay
The luciferase reporter plasmids of pGL3-ABCC2-wt and pGL3-ABCC2-mut contained the 3′-UTR genes of “5′- UAUAAAAUGUACGUUUUA −3′” and “5′- UAUAAAAUGUCCCAACAA −3′” separately. After the transfection of the reporter gene plasmids and the miR-424-3p mimics into the tumor cells of SGC-7901 and SGC-7901/DDP, the cells were cultured for another 48 h. Luciferase activities were detected using the Dual-Luciferase Assay System (Promega) and measured using the Luminoskan Ascent Reader System (Thermo Scientific, USA).
Western Blot Analysis
The total proteins in the cultured cells or xenograft tumors were isolated using the RIPA lysate buffer (KeyGen, China). Western blot analysis was performed using the primary antibodies ABCC2 and GAPDH (Abcam, UN), followed by secondary antibody (Affinity, USA). Blots were detected using the enhanced chemiluminescence detection kit (Millipore, USA). Densitometric analysis was performed using the ImageJ software. Each experiment was repeated in triplicate, and the mean values (mean ± s.d.) were presented.
Cell Proliferation
The different treated cells were seeded into a 24-well plate at 5 × 103 cells per well. The cells were dispersed in trypsin and resuspended in phosphate buffer every 24 h for 4 days. Then, they were counted using a light microscope (Olympus, Japan). Each experiment was repeated in three duplicates, and the mean values (mean ± s.d.) were presented.
Matrigel Invasion Assay
The different treated cells were seeded into the Transwell cell culture inserts (Corning, USA) coated with Matrigel (BD, USA). The invasion was allowed for 48 h. The passed cells were fixed in 4% paraformaldehyde, stained with crystal violet solution, and then counted using a light microscope (Nikon, Japan). Each experiment was repeated in triplicate, and the mean values (mean ± s.d.) were presented.
Wound Healing Assay
The different treated cells were seeded into 24-well culture plates at a density of 5 × 105 cells/well. When the tumor cells adhered to the plate, a 200 µL pipette tip was used to scratch the wound and incubated in serum-free medium for 48 h. Wound healings were observed under a light microscope (Nikon, Japan). Each experiment was repeated in triplicate, and the mean values (mean ± s.d.) were presented.
Animal Studies
Fifteen BALB/c nu/nu mice (aged 5–6 weeks) were randomly divided into five groups. The different treated SGC-7901/DDP cells were subcutaneously injected into the flank of every mouse at a density of 5 × 106 cells/mouse. When the xenograft tumors grew to grain size after 8 days, the tumor size was measured every 2 days for another 18 days. The mice were orally treated with 5 mg/kg/day DDP every 2 days after the tumor cells were injected. On the last day, all the mice were sacrificed, and xenografts and lung tissues were collected. Lung tissues were used for histologic examination to measure the extent of metastasis.
Hematoxylin and Eosin (H&E) Staining
The lung tissues from mice were fixed with 4% paraformaldehyde, embedded in paraffin, cut into 4-μm-thick slices, and then placed on slides. The slides were deparaffinized with xylene and rehydrated with decreasing ethanol concentrations. The slides were then stained with H&E. The extent of metastasis in the lung was analyzed using a light microscope (Olympus, Japan).
Statistical Analysis
All data were presented as means ± s.d. After testing for normality and equal variance across the groups, intergroup differences were assessed using Student’s t-tests analysis. All experiments were repeated at least three times. P < 0.05 was considered statistically significant.
Results
Selection of Candidate miRNA in Regulating GC Chemoresistance
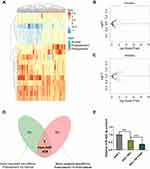
The miRNA expression profile data downloaded from the GEO database were used for screening the candidate miRNA. The miRNA expression profiles among normal gastric, GC, and chemoresistant GC tissues were quite different (Figure 1A). The volcano plots further described the differentially expressed genes (DEGs) between GC and normal gastric tissues (Figure 1B), or chemoresistant GC and wild GC tissues (Figure 1C). Using Venn analysis, we identified that the expression of has-miR-424 was gradually decreased with the malignant progression of GC (Figure 1D). To further analyze the expression trends, we selected three cell lines of normal gastric cell, wild type, and chemoresistant gastric cell to detect the background expression levels of miRNA-424. The qRT-PCR results showed that the miR-424-3p content was gradually remarkably decreased (Figure 1E).
ABCC2 is Negatively Regulated by miR-424-3p by Binding to the Conserved Motifs in the 3′-UTR Regions
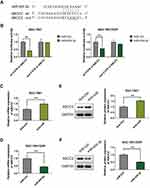
To further understand the molecular mechanism of miR-424-3p in regulating the malignant progression and chemoresistance of GC, we screened the potential targets of miR-424-3p by using the TargetScan, miRDB, and miRWalk databases (Table S1). ABCC2 is considered as a putative target mRNA of miR-424-3p. Thus, we constructed the wild-type and mutated ABCC2 luciferase reporter vectors (Figure 2A). We co-transfected the luciferase reporter vector along with miR-424-3p in SGC-7901 or SGC-7901/DDP cells, and the luciferase activity detection results showed a considerable reduction in the ABCC2 reporter in both cells, whereas the mutated ABCC2 reporter had no effect on the regulation of miR-424-3p (Figure 2B). When miR-424-3p inhibitor was added in SGC-7901 cells, the mRNA content of ABCC2 was significantly increased compared with the control group (Figure 2C). The SGC-7901/DDP cells were transfected with miR-424-3p mimics, and the mRNA content of ABCC2 was significantly inhibited by miR-424-3p (Figure 2D). Western blot analysis results further demonstrated that miR-424-3p inhibitor significantly upregulated the protein expression of ABCC2 (Figure 2E), and the miR-424-3p mimics significantly downregulated its expression (Figure 2F).
miR-424-3p Regulates Cell Proliferation, Invasion, and Migration in GC
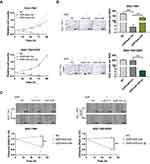
Given that miR-424-3p may play an important role in the malignant progression and chemoresistance in GC, we then explored the effect of miR-424-3p on GC cell behavior. The SGC-7901 and SGC-7901/DDP cells were separately treated with miR-424-3p inhibitor or miR-424-3p mimics incubated with DDP. The proliferation results showed that the downregulation of miR-424-3p could increase the resistance of SGC-7901 to DDP toxicity, whereas the upregulation of miR-424-3p caused the inhibition of proliferation to SGC-7901/DDP (Figure 3A). Adding DDP could significantly inhibit the invasion ability of SGC-7901, and miR-424-3p inhibitor could offset the toxic effect. When miR-424-3p mimics were transfected into SGC-7901/DDP cells, the invasion ability significantly decreased the tolerance to DDP (Figure 3B). Similar to the effects on cell invasion, miR-424-3p also exhibited significant differences in wound healing speed in the transfected cells in these two cell models. Thus, the miR-424-3p inhibitor could increase the migration ability even with the addition of DDP, whereas miR-424-3p mimics almost completely caused SGC-7901/DDP cells to lose the migration ability under the DDP environment (Figure 3C).
miR-424-3p Relies on ABCC2 to Promote Chemoresistance and Further Malignant Progression
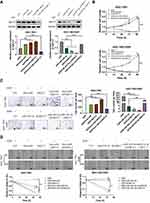
Considering the regulation of miR-424-3p on ABCC2, we further investigated the effect of miR-424-3p/ABCC2 on GC chemoresistance, proliferation, invasion, and migration in vitro by using the downregulated and upregulated cell models in SGCC-7901 and SGC-7901/DDP, respectively. Western blot analysis results showed the significant upregulation of ABCC2 by adding miR-424-3p inhibitor or the overexpression of ABCC2, whereas the transfection of miR-424-3p mimics or the knockdown of ABCC2 significantly decreased ABCC2 content (Figure 4A). The proliferation ability significantly increased when miR-424-3p inhibitor and ABCC2 were upregulated, either alone or both. However, the proliferation ability of SGC-7901 cells significantly decreased when ABCC2 was knocked down even with the addition of the miR-424-3p inhibitor. The proliferation ability was almost as high as the control group when miR-424-3p and ABCC2 were both upregulated in SGC-7901/DDP cells but significantly decreased when miR-424-3p mimics, shABCC2 plasmid, or both were transfected (Figure 4B). The Matrigel invasion assay results showed significant differences in transfected cell counts in the transfected cells between these two cell models (Figure 4C). Wound healing assay showed that the migration speed significantly increased when miR-424-3p inhibitor and/or ABCC2 was upregulated, whereas transfection of miR-424-3p and/or ABCC2 decreased wound healing. The wound healing speed decreased to the control level when ABCC2 was knocked down and miR-424-3p inhibitor was added in SGC-7901cells. Migration was significantly enhanced when the expression of ABCC2 and miR-424-3p in SGC-7901/DDP cells was upregulated than when miR-424-3p, shABCC2 plasmid, or both were transfected (Figure 4D).
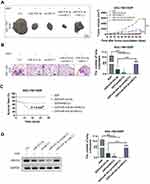
The in vivo SGC-7901/DDP xenograft model experiments were then conducted using the BALB/c nu/nu mice. When miR-424-3p mimics and shABCC2 were individually or both upregulated, tumor growth and lung metastasis were significantly decreased. When ABCC2 was upregulated even though the miR-424-3p content increased, the tumor proliferation and lung metastasis abilities were significantly restored (Figure 5A and B). We analyzed the survival rate of all mice. After the overexpression of miR-424-3p and ABCC2, the mortality increased. By contrast, the overexpression of miR-424-3p, shABCC2, or both protected the mice from death from xenograft tumors (Figure 5C). Consistent with these results, the ABCC2 content detection results showed a significant decrease of ABCC2 when miR-424-3p, shABCC2, or both were upregulated. Upregulating miR-424-3p and ABCC2 significantly increased the protein content of ABCC2 compared with the group individually transfected with miR-424-3p mimics (Figure 5D).
Discussion
GC is one of the most common malignant tumors, and the incidence of GC ranks the first among all types of tumors in China.16 Early GC is mostly asymptomatic or only shows mild symptoms. When the clinical symptoms are obvious, GC is already advanced. Chemotherapy is one of the main methods in the treatment of advanced GC by Western medicine.17 However, many patients develop drug resistance after chemotherapy, leading to treatment failure or even death.
Although many factors leading to drug resistance have been clarified, the detailed mechanism must be further elucidated. Many non-coding miRNAs have been studied, and their expression is dysregulated in many diseases and cancers. Dysregulated miRNAs affect the characteristics of most cancers.18 Therefore, a comprehensive understanding of how miRNAs affect cancer-related biological processes is of great reference value for the diagnosis, treatment, and prognosis of cancer. miR-424-3p is a member of the miR-16 family, and its genes are located on chromosome Xq26.3, which is closely related to the formation and development of various tumors.19,20 In the present study, the results showed that the expression of miR-424-3p gradually decreased as the malignant progression and chemoresistance of GC. miR-424-3p was reported to mediate the chemoresistance by targeting YAP1, galectin-3, or PI3K pathway in tumors like lung cancer, ovarian cancer, and prostate cancer,21–23 but how miR-424-3p regulate the chemoresistance in GC requires further clarification. Further analysis revealed that miR-424-3p relied on ABCC2, a chemoresistance-related receptor protein,24 to regulate the chemoresistance, proliferation, invasion, and migration of GC cells both in vitro and in vivo (Figure 6). Although some research had demonstrated that ABCC2 mediated the chemoresistance to cisplatin in gastric cancer,25 but how ABCC2 was regulated in GC cisplatin resistance was unclear. Therefore, the clarification of the regulation of miR-424-3p to ABCC2 in GC will benefit the diagnosis and prognosis of GC.
 |
Figure 6 Proposed regulatory mechanism of miR-424-3p during GC chemoresistance and malignant progression. |
Chemotherapy is the standard treatment for non-radical advanced GC. However, the mechanism of cisplatin in drug resistance of esophageal cancer and GC, mainly involving the transcriptional regulation of some important miRNA, has rarely been studied. This study reveals the molecular mechanism of cisplatin resistance, which is necessary to avoid and improve this phenomenon and optimize the treatment regimen. The drug resistance mechanism of GC is very complex, involving multiple signaling cell pathways, and multiple intersections exist between many signaling pathways.26 Therefore, current studies are not comprehensive enough to reflect the partial mechanism of cisplatin in the resistance process of GC. Besides, miR-424-3p might have multi-targets in regulating chemoresistance, but my work only clarified one target, and further experimental verification is necessary. If the mechanism of cisplatin resistance in the digestive system can be revealed comprehensively, the clinical application and therapeutic effect of cisplatin on GC can be greatly improved, benefitting many patients.
In summary, the mechanism of drug resistance in GC can be explained to some extent through this study. The in vitro and in vivo experimental results both confirmed that miR-424-3p plays an important role in the drug resistance of GC. The upregulation of miR-424-3p plays an active role in reversing the multidrug resistance of chemotherapy. Therefore, miR-424-3p may be a therapeutic target for GC chemoresistance to enhance the efficacy of chemotherapy to GC.
Data Sharing Statement
The datasets used and/or analyzed during the present study are available from the corresponding author upon reasonable request.
Ethics Approval
The guidelines for experimental animal welfare are GB/T 35892-2018. Animal experiments were approved by the Animal Ethics Committee of Tianjin Medical University with the approval number of 20180913.
Acknowledgments
The study was supported by the Science and Technology Project of Health and Family Planning Commission of Tianjin Binhai New District (grant no. 2018BWKZ004) and the Medical Research Project of the Fifth Central Hospital of Tianjin (grant no. wzx202001).
Disclosure
The authors declare no conflicts of interest.
References
1. Heindl A, Nawaz S, Yuan Y. Mapping spatial heterogeneity in the tumor microenvironment: a new era for digital pathology. Lab Invest. 2015;95(4):377–384. doi:10.1038/labinvest.2014.155
2. Marin JJ, Al-Abdulla R, Lozano E, et al. Mechanisms of resistance to chemotherapy in gastric cancer. Anticancer Agents Med Chem. 2016;16(3):318–334. doi:10.2174/1871520615666150803125121
3. Wagner AD, Syn NL, Moehler M, et al. Chemotherapy for advanced gastric cancer. Cochrane Database Syst Rev. 2017;8:CD004064. doi:10.1002/14651858.CD004064.pub4
4. Huang J, Zhao Y, Xu Y, et al. Comparative effectiveness and safety between oxaliplatin-based and cisplatin-based therapy in advanced gastric cancer: a meta-analysis of randomized controlled trials. Oncotarget. 2016;7(23):34824–34831. doi:10.18632/oncotarget.9189
5. Shi WJ, Gao JB. Molecular mechanisms of chemoresistance in gastric cancer. World J Gastrointest Oncol. 2016;8(9):673–681. doi:10.4251/wjgo.v8.i9.673
6. Begicevic RR, Falasca M. ABC transporters in cancer stem cells: beyond chemoresistance. Int j Mol Sci. 2017;18:11. doi:10.3390/ijms18112362
7. Hombach-Klonisch S, Mehrpour M, Shojaei S, et al. Glioblastoma and chemoresistance to alkylating agents: involvement of apoptosis, autophagy, and unfolded protein response. Pharmacol Ther. 2018;184:13–41. doi:10.1016/j.pharmthera.2017.10.017
8. Chu G. Cellular responses to cisplatin. The roles of DNA-binding proteins and DNA repair. J Biol Chem. 1994;269(2):787–790.
9. Woynarowski JM, Faivre S, Herzig MC, et al. Oxaliplatin-induced damage of cellular DNA. Mol Pharmacol. 2000;58(5):920–927. doi:10.1124/mol.58.5.920
10. Taft RJ, Pang KC, Mercer TR, Dinger M, Mattick JS. Non-coding RNAs: regulators of disease. J Pathol. 2010;220(2):126–139. doi:10.1002/path.2638
11. Riquelme I, Letelier P, Riffo-Campos AL, Brebi P, Roa JC. Emerging role of miRNAs in the drug resistance of gastric cancer. Int J Mol Sci. 2016;17(3):424. doi:10.3390/ijms17030424
12. Chen QN, Wei CC, Wang ZX, Sun M. Long non-coding RNAs in anti-cancer drug resistance. Oncotarget. 2017;8(1):1925–1936. doi:10.18632/oncotarget.12461
13. Seo J, Shin JY, Leijten J, et al. High-throughput approaches for screening and analysis of cell behaviors. Biomaterials. 2018;153:85–101. doi:10.1016/j.biomaterials.2017.06.022
14. Zhang Q, Qin Y, Zhao J, et al. Thymidine phosphorylase promotes malignant progression in hepatocellular carcinoma through pentose Warburg effect. Cell Death Dis. 2019;10(2):43. doi:10.1038/s41419-018-1282-6
15. Kim CH, Kim HK, Rettig RL, et al. miRNA signature associated with outcome of gastric cancer patients following chemotherapy. BMC Med Genomics. 2011;4:79. doi:10.1186/1755-8794-4-79
16. Bray F, Ferlay J, Soerjomataram I, Siegel RL, Torre LA, Jemal A. Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin. 2018. doi:10.3322/caac.21492
17. Song Z, Wu Y, Yang J, Yang D, Fang X. Progress in the treatment of advanced gastric cancer. Tumour Biol. 2017;39(7):1010428317714626. doi:10.1177/1010428317714626
18. Ji W, Sun B, Su C. Targeting MicroRNAs in cancer gene therapy. Genes (Basel). 2017;8(1). doi:10.3390/genes8010021
19. Diaz G, Melis M, Tice A, et al. Identification of microRNAs specifically expressed in hepatitis C virus-associated hepatocellular carcinoma. Int J Cancer. 2013;133(4):816–824. doi:10.1002/ijc.28075
20. Azzoni C, Bottarelli L, Pizzi S, D’Adda T, Rindi G, Bordi C. Xq25 and Xq26 identify the common minimal deletion region in malignant gastroenteropancreatic endocrine carcinomas. Virchows Arch. 2006;448(2):119–126. doi:10.1007/s00428-005-0058-4
21. Zhang M, Zeng J, Zhao Z, Liu Z. Loss of MiR-424-3p, not miR-424-5p, confers chemoresistance through targeting YAP1 in non-small cell lung cancer. Mol Carcinog. 2017;56(3):821–832. doi:10.1002/mc.22536
22. Bieg D, Sypniewski D, Nowak E, Bednarek I. MiR-424-3p suppresses galectin-3 expression and sensitizes ovarian cancer cells to cisplatin. Arch Gynecol Obstet. 2019;299(4):1077–1087. doi:10.1007/s00404-018-4999-7
23. Lu C, Wang H, Chen S, Yang R, Li H, Zhang G. Baicalein inhibits cell growth and increases cisplatin sensitivity of A549 and H460 cells via miR-424-3p and targeting PTEN/PI3K/Akt pathway. J Cell Mol Med. 2018;22(4):2478–2487. doi:10.1111/jcmm.13556
24. Han B, Gao G, Wu W, et al. Association of ABCC2 polymorphisms with platinum-based chemotherapy response and severe toxicity in non-small cell lung cancer patients. Lung Cancer. 2011;72(2):238–243. doi:10.1016/j.lungcan.2010.09.001
25. Materna V, Stege A, Surowiak P, Priebsch A, Lage H. RNA interference-triggered reversal of ABCC2-dependent cisplatin resistance in human cancer cells. Biochem Biophys Res Commun. 2006;348(1):153–157. doi:10.1016/j.bbrc.2006.07.022
26. McCubrey JA, Abrams SL, Fitzgerald TL, et al. Roles of signaling pathways in drug resistance, cancer initiating cells and cancer progression and metastasis. Adv Biol Regul. 2015;57:75–101. doi:10.1016/j.jbior.2014.09.016
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.