Back to Journals » Clinical Ophthalmology » Volume 8
Melanocytoma of the ciliary body misdiagnosed as iridodialysis
Received 1 March 2014
Accepted for publication 15 April 2014
Published 29 May 2014 Volume 2014:8 Pages 1051—1053
DOI https://doi.org/10.2147/OPTH.S63328
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Moosang Kim, Seung-Jun Lee
Department of Ophthalmology, School of Medicine, Kangwon National University, Chuncheon, Republic of Korea
Abstract: A 62-year-old female presented to our institution with dimness of vision in her right eye. On examination, her best corrected visual acuity was 20/100 in the right eye. The intraocular pressures were 14 mmHg in both eyes. Slit-lamp examination revealed nuclear sclerotic cataracts bilaterally and iridodialysis in her right eye. Seven days after the first visit, cataract surgery was performed without any complications. One year later, she presented to our institution with acute visual loss and ocular pain in the right eye. Best corrected visual acuity of the right eye was light perception and the intraocular pressure was 44 mmHg. Slit-lamp examination revealed a ciliary body mass with widespread pigment dispersion in the anterior segment. Due to no useful vision and uncontrolled pain, enucleation of the right eye was performed. Histopathologic examination revealed a melanocytoma of the ciliary body.
Keywords: ciliary body, iridodialysis, melanocytoma
Introduction
Although melanocytomas are typically located in the optic nerve head, they can also be found anywhere along the uveal tract, including the iris, choroid, and ciliary body.1–3 Melanocytoma is a variant of melanocytic nevi, and its occurrence in the uveal tract is relatively uncommon. In this paper, we report a case of melanocytoma of the ciliary body misdiagnosed as iridodialysis.
Case report
A 62-year-old female presented to our institution with dimness of vision in the right eye. On examination, her best corrected visual acuity was 20/100 in the right eye and 20/50 in the left eye. Intraocular pressures were 14 mmHg in both eyes. Slit-lamp examination revealed nuclear sclerotic cataracts bilaterally and a small iridodialysis in her right eye. The iridodialysis was within 20 degrees in the 11 o’clock direction, and the iris and its surrounding structures were otherwise unremarkable. However, she had no history of ocular trauma. The pupil was grossly concentric and almost fully dilated after instillation of mydriatics, even though the finding was consistent with the iridodialysis. Fundus examination was unremarkable in both eyes. We considered these findings in the iris as a small asymptomatic dialysis that did not require any specific treatment. The patient wanted surgery for her right eye cataract. Seven days after presentation, the cataract surgery was performed without any complications (Figure 1).
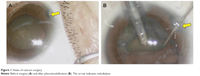  | Figure 1 Views of cataract surgery. |
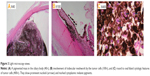
One year later, the patient presented to our institution with acute visual loss and ocular pain in her right eye. Best corrected visual acuity of the right eye was light perception and the intraocular pressure was 44 mmHg. Slit-lamp examination and ultrasonography revealed an iridodialysis of nearly 40 degrees and a ciliary body mass with widespread pigment dispersion in the anterior segment (Figure 2). Due to her lack of useful vision and her uncontrolled pain, enucleation of the right eye was performed. Histopathologic examination revealed small, round to oval shaped cells with cytoplasm containing abundant melanin pigments, consistent with a melanocytoma. Along with the melanocytoma of the ciliary body, focal malignant transformation with an extension of tumor cells and macrophages into both the trabecular meshwork and anterior chamber angle was noted (Figure 3).
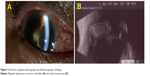  | Figure 2 Anterior segment photograph and ultrasonographic findings. |
Discussion
Melanocytoma of the ciliary body is an uncommon tumor of the uveal tract and is generally regarded as benign; it has the ability to invade local tissues,4 but has never been shown to metastasize.5 Typically it is described at the optic nerve head,1 but is encountered less frequently at the ciliary body,6 and there are rare reports of occurrence in the iris,7 sclera,8 conjunctiva,9 and choroid.10,11
Melanocytoma of the ciliary body is often clinically undetected until it extends into the pupil, anterior chamber, or sclera, since it is hidden by the iris. Seeding of tumor cells on the iris, pigment dispersion from necrosis, elevated intraocular pressure, extrascleral extension, change in refractive error with increasing astigmatism, or cataract from compression are other telltale signs. These findings may be suggestive of a malignant change in the tumor.12–14
Anatomically speaking, iridodialysis is a separation between the iris root and the ciliary body. It is usually caused by blunt or penetrating trauma, or by an iatrogenic complication of intraocular surgery. Since it rarely occurs for reasons other than direct trauma, a thorough search for etiologies that could have caused structural changes in the iris or ciliary body is recommended. In this case, we found that the iridodialysis was widened, with widespread pigment dispersion into the surrounding structures, which had not been detectable at the initial examination.
A spontaneous iridodialysis and ongoing anatomic changes could indicate a neoplasm of an angle structure origin, which is difficult to identify clinically. Early detection of such a neoplasm increases the chance of preserving the eyeball and vision by various methods, including an en bloc resection.15 If a spontaneous iridodialysis with no plausible explanation is encountered, an early and thorough search should be done in the anterior chamber angle, including gonioscopy or anterior segment optical coherence tomography. In summary, melanocytoma of the ciliary body is a rare tumor, is clinically hard to detect, and can invade chamber angle structures and appear as a pigmented mass at the iris root.
Conclusion
This is a case of melanocytoma of the ciliary body misdiagnosed as iridodialysis. A physician should always keep in mind that a careful evaluation of the anterior chamber angle (eg, gonioscopy, anterior segment optical coherence tomography) is the most important step for making an accurate diagnosis.
Disclosure
The authors report no conflicts of interest in this work.
References
Demirci H, Mashayekhi A, Shields CL, Eagle RC Jr, Shields JA. Iris melanocytoma: clinical features and natural course in 47 cases. Am J Ophthalmol. 2005;139(3):468–475. | ||
Brownstein S, Dorey MW, Mathew B, Little JM, Lindley JI. Melanocytoma of the choroid: atypical presentation and review of the literature. Can J Ophthalmol. 2002;37(4):247–252. | ||
Shields JA, Shields CL, Eagle RC Jr. Melanocytoma (hyperpigmented magnocellular nevus) of the uveal tract: the 34th G. Victor Simpson lecture. Retina. 2007;27(6):730–739. | ||
Zimmerman LE. Melanocytes, melanocytic nevi and melanocytomas. Invest Ophthalmol. 1965;4:11–41. | ||
Raichand M, Peyman GA, Juarez CP, Seetner AA, Sugar J, Goldberg MF. Resection of uveal melanocytoma: clinicopathological correlation. Br J Ophthalmol. 1983;67(4):236–243. | ||
Shammas HJ, Minckler DS, Hulquist R, et al. Melanocytoma of the ciliary body. Ann Ophthalmol. 1981;13:1381–1383. | ||
Shields JA, Augsburger JJ, Bernardino V Jr, Eller AW, Kulczycki E. Melanocytoma of the ciliary body and iris. Am J Ophthalmol. 1980; 89(5):632–635. | ||
Lee JS, Smith RE, Minckler DS. Scleral melanocytoma. Ophthalmology. 1982;89(2):178–182. | ||
Verdaguer J, Valenzuela H, Strozzi L. Melanocytoma of the conjunctiva. Arch Ophthalmol. 1974;91(5):363–366. | ||
Shields JA, Font RL. Melanocytoma of the choroid clinically simulating a malignant melanoma. Arch Ophthalmol. 1972;87:396–400. | ||
Jürgens I, Roca G, Sedó S, Pujol O, Berniell JA, Quintana M. Presumed melanocytoma of the macula. Arch Ophthalmol. 1994;112(3): 305–306. | ||
Bhorade AM, Edward DP, Goldstein DA. Ciliary body melanocytoma with anterior segment pigment dispersion and elevated intraocular pressure. J Glaucoma. 1999;8(2):129–133. | ||
Cialdini AP, Sahel JA, Jalkh AE, Weiter JJ, Zakka K, Albert DM. Malignant transformation of an iris melanocytoma. A case report. Graefes Arch Clin Exp Ophthalmol. 1989;227(4):348–354. | ||
Radcliffe NM, Finger PT. Eye cancer related glaucoma: current concepts. Surv Ophthalmol. 2009;54(1):47–73. | ||
Weinstein GW, Quayle WH. An en bloc technique for the resection of anterior uveal tumors. Am J Ophthalmol. 1979;88(3 Pt 1):519–523. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.