Back to Journals » OncoTargets and Therapy » Volume 12
Low Expression of ASK1-Interacting Protein-1 Is Significantly Correlated with Tumor Angiogenesis and Poor Survival in Patients with Early Stage Non-Small Cell Lung Cancer
Authors Chen C , Geng Q, Sun D, Hu W, Zhong C, Fan L, Song X
Received 8 July 2019
Accepted for publication 25 September 2019
Published 10 December 2019 Volume 2019:12 Pages 10739—10747
DOI https://doi.org/10.2147/OTT.S222332
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Sanjeev K. Srivastava
Chengyu Chen,1 Qun Geng,2 Dongfeng Sun,1 Wensi Hu,1 Chenxi Zhong,3 Limin Fan,3 Xiaoming Song1
1Department of Thoracic Surgery, The First Affiliated Hospital of Shandong First Medical University, Jinan, People’s Republic of China; 2Department of Ultrasound Diagnosis and Treatment, Shandong Provincial Hospital, Shandong University, Jinan, People’s Republic of China; 3Department of Thoracic Surgery, Shanghai Chest Hospital, Shanghai JiaoTong University, Shanghai, People’s Republic of China
Correspondence: Dongfeng Sun
Department of Thoracic Surgery, The First Affiliated Hospital of Shandong First Medical University, Jinan 250014, People’s Republic of China
Tel +86 13589032106
Email [email protected]
Objective: To investigate the expression of tumor suppressor protein ASK1-interacting protein-1 (AIP1) in cancer tissues of patients with early-stage non-small cell lung cancer (NSCLC) and its correlation with tumor progression, tumor angiogenesis and prognosis.
Methods: A total of 136 patients with stage I NSCLC who underwent radical resection of lung cancer in Qianfoshan Hospital of Shandong Province from January 2011 to December 2011 were enrolled. Immunohistochemistry was used to detect AIP1 protein in tumor tissues. Vascular endothelial CD34 immunohistochemical staining was used to count intratumoral microvessel density (MVD). SPSS 19.0 software was used to analyze the relationship between AIP1 protein expression and clinicopathological features, tumor angiogenesis and prognosis.
Results: Low expression of AIP1 was more common in tumor tissues with high MVD, and patients with low expression of AIP1 were more likely to have tumor recurrence. Multivariate analysis showed that low expression of AIP1 had predictive value for overall survival, disease-free survival, and disease-specific survival.
Conclusion: Downregulation of AIP1 protein expression is associated with lung cancer progression, tumor angiogenesis and poor prognosis. Consequently, AIP1 may prove to be an important predictor of recovery from lung cancer and could become a new therapeutic target for lung cancer treatment.
Keywords: NSCLC, ASK1-interacting protein-1, angiogenesis, prognosis
Introduction
Lung cancer currently has the highest incidence and mortality of any cancer in China.1 In recent years, with the application of high-resolution computed tomography (CT), the detection of early lung cancer has gradually increased.2–4 However, in clinical work it has been found that different patients have very different prognoses after surgery or/and corresponding treatment, even if the pathological type and staging are the same,5–7 so the current clinical application of the staging criteria does not fully or accurately reflect the prognosis of lung cancer patients, and is also not conducive to individualized treatment of the disease.8 As a result, it has been found that high-risk factors of lung cancer recurrence can guide the subsequent individualized treatment of lung cancer and thus become a useful supplement to the current stage of lung cancer and improve patient prognosis.
In recent years, with developments in molecular biology, some newly discovered molecular indicators have been applied to detect tumors, predict prognosis, and judge tumor progression and response to treatment.9–11 AIP1, also known as disabled homolog 2 interacting protein (DAB2IP), is a new member of the Ras GTPase activating protein (Ras-GAP) family, which acts to inhibit Ras-dependent mitosis.12 In addition, as a signal adapter, AIP1 inhibits tumor production through the TNFα/NF-κB, WNT/β-catenin, PI3K/AKT, and androgen receptor pathways.13 Recent studies have shown that AIP1 is significantly associated with tumor angiogenesis.14–17 Many types of tumors have low expression of AIP1,18–21 including lung cancer.22 AIP1 protein deficiency in mice with knockout of the AIP1 gene greatly enhances epithelial cell migration and angiogenesis.23 Tumor angiogenesis is an early event in lung cancer. Tumor angiogenesis occurs early in the onset of cancer and is a necessary condition for deterioration and metastasis of malignant tumors; consequently, it is an important factor in tumor treatment resistance.24,25 As an angiogenesis inhibitor, the AIP1 protein has attracted more and more attention in inhibiting tumor angiogenesis.21,23,26 However, to the best of our knowledge, the relationship between AIP1 protein and angiogenesis has not been elucidated in non-small cell lung cancer (NSCLC). The potential significance of AIP1 protein as an independent prognostic factor in NSCLC has not been systematically studied. Therefore, we designed this experiment to evaluate the expression level of AIP1 protein in tumor tissues of patients with early NSCLC, to explore its relationship with clinicopathological features, tumor angiogenesis and prognosis, and to determine its independent predictive effect on the long-term prognosis of cancer patients.
Patients and Methods
A total of 136 patients treated between January and December 2011 in Qianfoshan Hospital of Shandong Province were enrolled in this study, consisting of 93 males and 43 females, aged 40–75 years. Inclusion criteria were: preoperative PET-CT assessment of regional lymph nodes and distant organ metastasis, complete tumor resection (lobectomy), and regional lymph node dissection; postoperative pathology without regional lymph node metastasis, T stage T1–T2a (International Union Against Cancer (UICC) 8th Edition TNM staging of lung cancer); pathological type was non-small cell lung cancer; no preoperative or postoperative adjuvant therapy was performed before tumor recurrence. Exclusion criteria were: loss to follow-up after discharge; death due to perioperative complications. Tissue samples from patients with NSCLC and adjacent histologically normal tissue samples were acquired from these patients. This study was approved by the Ethics Committee of Qianfoshan Hospital of Shandong Province and has been performed in accordance with the ethical standards as laid down in the 1964 Declaration of Helsinki and its later amendments. The written informed consent of each patient was obtained. The clinicopathological features of all 136 patients are listed in Table 1.
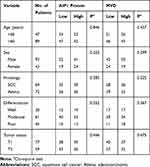 |
Table 1 Correlation of Clinicopathologic Variables with AIP1 Protein and MVD |
Immunohistochemical Staining of AIP1 and CD34
NSCLC tissues were fixed overnight in 10% neutral-buffered formalin and embedded in paraffin; then tissues were cut into 3 μm slices and stained with hematoxylin and eosin (HE). Paraffin sections were immunostained using microwave-based antigen retrieval techniques. AIP1 antibody (ab87811; Santa Cruz Biotechnology, Santa Cruz, CA, USA) and CD34 (sc-19621; Santa Cruz Biotechnology) used in this study were processed in slices using the Envision+ DAB kit (Dako, Glostrup, Denmark) according to the manufacturer’s instructions. A human kidney cancer sample known to express the AIP1 protein was used as a positive control, and the sections were incubated with phosphate-buffered saline (PBS) instead of the primary antibody as a negative control.
Analysis of AIP1 Protein Expression and MDV
The staining intensity of AIP1 and the proportion of stained cells were measured using a semi-quantitative method. Ten fields of view were observed at 400× magnification, with 100 tumors or alveolar epithelial cells counted per field of view. The proportions of positive cells were scored as follows: <5% positive cells was awarded 0 points; 5–25% was 1 point; 25–50% was 2 points; 50–75% was 3 points; >75% was 4 points. The staining intensity scores were as follows: unstained was 0 points; light yellow was 1 point; yellowish-brown was 2 points; and dark brown was 3points. The final score was the sum of the positive cell score and the stain intensity score, and was further graded as follows: (-), 0–1; (+), 2–3; (++), 4–6; and (+++), 8–12. A final score of ≥4 points defines the high expression of AIP1.
The number of microvessels in the tumor was measured by counting CD34 positive cells.27,28 Positive CD34 staining was defined as clear brown or dark brown particles in the cytoplasm and/or cell membrane that may include stained microvessels, individual endothelial cells or cell clumps. Separation or multiple closely arranged endothelial cell clusters, if they had a distinct boundary with adjacent tumor cells and surrounding connective tissue, regardless of the lumen of the vessel, were counted as microvessels.29 Referring to the Chalkley counting method,30 the two pathologists first observed the entire section at low magnification without knowing the patient information, and found three “hot spots,” that is, areas where positively stained blood vessels were highly concentrated. The number of microvessels was then counted under the high power field of view (HPF). Blood vessels with a lumen diameter larger than that of red blood cells were excluded or blood vessels of smooth muscle observed in the blood vessel wall. The average number of microvessels in the five fields of view was taken as the MVD of the sample. If the difference between the two pathologists exceeded 10%, then a recalculation was required.
Patient Follow-Up
Patients were seen for follow-up visits every 3 months within 2 years after discharge, and every 6 months from 2 years until death, tumor recurrence or metastasis or the end of the study, whichever was soonest. The follow-up program included physical examination, blood analysis, computed tomography (CT) scans, and ultrasound examinations. Recurrence or metastasis was determined based on clinical, radiological, or histological examinations. The location and timing of tumor recurrence and metastasis were recorded. The follow-up was completed in December 2016 with a median follow-up of 42 months (range, 5–72 months).
Statistical Analysis
SPSS, version 19.0 software (IBM SPSS Statistics for Windows, Armonk, NY, USA) was used for all statistical analyses. The chi-square test was used to analyze the correlation between AIP1 protein, MVD and various clinical features and prognostic factors. The Spearman rank correlation method was used to assess the correlation between AIP1 and MVD. Survival curves were estimated by the Kaplan–Meier (KM) method. Multivariate Cox regression analysis was used to identify significant independent prognostic factors. A P value <0.05 was considered to be significantly different.
Results
Relationship Between AIP1 Protein Expression and Clinicopathological Factors in Patients with NSCLC
Immunohistochemical staining showed that AIP1 protein was expressed in normal cells and in tumor cell membranes and cytoplasm (Figure 1), and the expression of AIP1 protein in NSCLC tissues was significantly lower than that in normal tissues (Figure 1A–C). An independent sample t-test showed the expression of AIP1 in normal tissue and NSCLC tissue had a significant difference (Figure 4, P<0.0001). The staining intensity of AIP1 was different in NSCLC tissues from different patients. Based on the criteria defined above, we detected 71 cases of low expression of AIP1 among all 136 patients. To understand the role of AIP1 in NSCLC, we investigated the association between AIP1 expression and clinicopathological features, including age, gender, pathological type, degree of differentiation, and T stage. The results showed no obvious correlation between AIP1 expression and these pathological features (P > 0.05).
MVD in NSCLC and Its Correlation with Clinicopathological Factors of NSCLC
In this study, CD34 immunohistochemical staining was used to assess MVD in tumor tissues. In positively stained endothelial cells, diffuse staining for CD34 was observed in the cytoplasm and membrane (Figure 1D–F). All NSCLC specimens had an average MVD of 28/HPF with a range from 12 to 57/HPF. We divided the patients into a high-MVD group (≥28) and a low-MVD group (<28) with the average MVD28/HPF as the cutoff value. The data showed no significant correlation between MVD and clinicopathological factors (P > 0.05).
AIP1 and MVD Relationship
We next studied the relationship between AIP1 expression and MVD and found that they were significantly correlated (P <0.0001, Spearman), with AIP1 low expression being more common in high-MVD tumor tissues (Figure 3).
Correlation Between AIP1, MVD and Tumor Recurrence
Of the 136 patients, 36 had tumor recurrence (26.5%); of these, 14 patients had local recurrence, 15 patients had distant metastases, and seven patients had local recurrence with distant metastases. Specifically, in 71 cases with low expression of AIP1, 27 cases (38.0%) had tumor recurrence, while 9 (13.8%) of 65 cases with normal expression of AIP1 had tumor recurrence. Twenty-five (36.2%) of the 69 high-MVD cases relapsed, while only 11 (16.4%) of the 67 patients with low MVD relapsed. Further, KM analysis showed that AIP1 low expression, high MVD and lower 5-year disease-free survival (DFS) were associated (P = 0.001, P = 0.004, Table 2). In addition, the multivariate analysis confirmed that low expression of AIP1 protein continued to maintain its predictive value for DFS (P = 0.025, Table 2).
 |
Table 2 Univariate and Multivariate Analyses of Prognostic Variables |
Univariate and Multivariate Survival Analysis
Of the 136 patients, 45 died within 5 years after surgery; 36 patients died of causes associated with NSCLC tumors, and 7 patients died for other reasons. According to survival analysis, the overall and DFS rates for 5 years were 66.9% and 73.5%, respectively. The predictive effect of AIP1 protein and MVD on OS and DFS was found by univariate survival analysis (log-rank test, Table 2, Figure 2). Patients with low AIP1 expression (52.3% vs. 79.7%, P = 0.000) and high MVD (57.2% vs. 75.8%, P = 0.007) had lower 5-year OS (Figure 2). Moreover, the analysis also showed that patients with low expression of AIP1 protein (59.2% vs. 85.7%, P = 0.000) and high MVD (61.2% vs. 83.0%, P = 0.003) had lower 5-year disease-specific survival (DSS).
 |
Figure 3 Cross-correlation analyses revealed strong relationships between the low expressions of AIP1 and high MVD in NSCLC. |
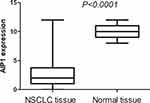 |
Figure 4 Independent sample t-test showed the expression of AIP1 in normal tissue and NSCLC tissue had a significant difference. |
To investigate the interference between AIP1 protein and MVD, we further investigated the difference in survival between low MVD and high MVD in the same AIP1 protein expression state. The results showed that there was no significant difference in survival rate between the different MVD groups in patients with the same AIP1 protein expression (Table 3, P > 0.05).
 |
Table 3 Survival Differences Stratified by Low MVD and High MVD in the AIP1 Low Expression and AIP1 Normal Expression Subgroups |
Multivariate COX regression analysis showed that the prognostic predictive effect of MVD in univariate analysis disappeared, while low expression of AIP1 protein as an independent predictor remained for OS, DSS and DFS (P = 0.005, 0.020, and 0.025, Table 2).
Discussion
Our results showed that low expression of AIP1 protein was common in early NSCLC tissues and was significantly associated with intratumoral microangiogenic activity. Low expression of AIP1 is positively correlated with high MVD, suggesting that AIP1 protein may slow tumor progression and metastasis by inhibiting tumor angiogenesis, and low expression of AIP may lead to increased tumor microangiogenesis. Some scholars have found that methylation of the AIP1 encoding gene in lung, breast, gastrointestinal, renal, and prostate tumors, which leads to inactivation of the gene, results in decreased AIP1 protein levels and is associated with tumor progression and therapeutic resistance.22,31–33,36 Many researchers believe that angiogenesis is a prerequisite for solid tumor growth and metastasis; tumor growth rate and patient prognosis are related to the rate of microangiogenesis in the tumor.34,37 Tumor blood vessels provide a material basis for the rapid division and growth of tumor cells. At the same time, due to the structural and functional defects of the neonatal tumor blood vessel, tumor cells are more likely to migrate through blood vessels, thereby aggravating local invasion and distant metastasis.21 Consequently, the AIP1 protein and its coding gene may be potential therapeutic targets for anti-angiogenic therapy in NSCLC patients. However, tumor angiogenesis is an extremely complex process involving multiple steps and multiple diffusion factors produced by tumor cells. To date, the exact molecular mechanism by which AIP1 protein inhibits the angiogenic potential of tumor cells and the formation of new tumor microvessels is far from clear, and further clarification of molecular levels is needed.
So far, there have been only two clinical studies on the expression of AIP1 in lung cancer. Yano et al found that methylation of the AIP1 protein-encoding gene is frequently found in lung cancer patients and leads to inactivation of the coding gene and is associated with later disease stages.22 Yang et al found that mutations in the AIP1 protein-encoding gene lead to an increased risk of lung cancer and early age of onset, especially in men.35 To the best of our knowledge, our study is the first to evaluate AIP1 protein expression in surgically resected early NSCLC patients and is the first to investigate the prognostic relationship between AIP1 protein and angiogenesis in patients with NSCLC.
In our study, high MVD subgroup showed longer OS, DFS, and DSS than low MVD in the AIP1 low expression group, although the difference was not statistically significant. The possible reason was that tumor progression and metastasis involved many other factors besides microvessel density, such as tumor microvascular function, vascular endothelial cell activation, tumor infiltration of lymphatic vessels, etc., and further research is needed.
In our study, low expression of AIP1 and high MVD were significantly associated withthe higher risk of tumor recurrence and low DSS. KM analysis showed that low expression of AIP1 protein and high MVD were significantly associated with lower 5-year OS and DSS, suggesting that AIP1 protein and MVD may be potential prognostic predictors in early NSCLC patients. Multivariate analysis showed that relative to MVD, low expression of AIP1 protein maintained its prognostic value and was an independent prognostic predictor for OS, DFS, and DSS. Therefore, the evaluation of the AIP1 protein expression level can effectively improve the risk stratification of the conventional staging system in early NSCLC patients, and prophylactic treatment for high-risk patients can improve patient outcomes.
All patients in this study underwent complete tumor resection and regional lymph node dissection, and did not receive radiochemotherapy before or after surgery unless tumor recurrence was found. In addition, in order to reduce statistical bias, relatively rare large cell carcinomas, mixed cancers, etc., were not included in the study, thereby improving comparative efficiency, reducing statistical bias, and making our results more objective.
In conclusion, our results suggested that low expression of AIP1 protein is common in early NSCLC and was significantly associated with tumor angiogenesis and recurrence. In addition, low expression of AIP1 protein had a significant impact on survival and is an independent predictor of OS, DFS, DSS. These findings suggested that AIP1 protein may have clinical potential, not only as a promising predictor of prognosis but also as a new target for anti-angiogenic therapy in NSCLC patients.
In future, further research is needed to determine the mechanism by which AIP1 promotes tumor microangiogenesis at the molecular level. Molecular targeting agents targeting AIP1 may become new anti-angiogenic drugs for the treatment of NSCLC in the future. In addition, the possible link between AIP1 protein and intensive therapy needs further prospective studies. Because the low expression of AIP1 protein may be associated with high risk of recurrence and poor prognosis, it could be given to high-risk patients together with intensive post-operative adjuvant therapy or combined anti-angioproliferative therapy, thereby improving the prognosis of such patients. These studies may provide important information to optimize personalized treatment for early NSCLC patients.
As a new prognostic predictor and a potential therapeutic target, AIP1 can be used as an adjunct to the lung cancer staging system and help to provide better treatment for patients with lung cancer.
Acknowledgements
We thank the International Science Editing for editing this manuscript. This work was supported by the Science and Technology Development Plan of Jinan (201907061).
Disclosure
The authors declare that they have no conflicts of interest.
References
1. Chen W, Zheng R, Baade PD, et al. Cancer statistics in China, 2015. CA Cancer J Clin. 2016;66:115–132. doi:10.3322/caac.21338
2. Zhang L, Li M, Wu N, et al. Time trends in epidemiologic characteristics and imaging features of lung adenocarcinoma: a population study of 21,113 cases in China[J]. PLoS ONE. 2015;10(8):1–13.
3. Palma DA, Warner A, Louie AV, et al. Thoracic radiotherapy for extensive stage small-cell lung cancer: a meta-analysis[J]. Clin Lung Cancer. 2016;17(4):239–244. doi:10.1016/j.cllc.2015.09.007
4. Black WC, Chiles C, Church TR, et al. Lung cancer incidence and mortality with extended follow-up in the National Lung Screening Trial National Lung Screening Trial Writing Team [J]. J Thor Oncol. 2019. doi:10.1016/j.jtho.2019.05.044
5. Kris MG, Gaspar LE, Chaft JE, et al. Adjuvant systemic therapy and adjuvant radiation therapy for stage I to IIIA completely resected non-small-cell lung cancers: American Society of Clinical Oncology/Cancer Care Ontario Clinical Practice Guideline Update[J]. J Clin Oncol. 2017:JCO2017724401. doi:10.1200/JCO.2017.72.4401.
6. Fibla JJ, Molins L, Quero F, et al. Perioperative outcome of lung cancer surgery in women: results from a Spanish nationwide prospective cohort study[J]. J Thorac Dis. 2019;11(4):1475–1484. doi:10.21037/jtd.2019.03.30
7. Dubaere E, Goffaux M, Wanet M, et al. Long term outcome after 48 Gy stereotactic ablative body radiotherapy for peripheral stage I non-small cell lung cancer[J]. BMC Cancer. 2019;19(1):639. doi:10.1186/s12885-019-5863-2
8. Yu Y. Molecular classification of non-small-cell lung cancer: diagnosis, individualized treatment, and prognosis[J]. Front Med. 2013;7(2):157–171. doi:10.1007/s11684-013-0272-4
9. Jin M, Ren J, Luo M, et al. Long noncoding RNA JPX correlates with poor prognosis and tumor progression in non-small cell lung cancer by interacting with miR-145-5p and CCND2[J]. Carcinogenesis. 2019. doi:10.1093/carcin/bgz125
10. Chi Y, Luo Q, Song Y, et al. Circular RNA circPIP5K1A promotes non-small cell lung cancer proliferation and metastasis through miR-600/HIF-1α regulation[J]. J Cell Biochem. 2019;120:19019–19030. doi:10.1002/jcb.29225
11. Yang R, Liu N, Chen L, et al. LSH interacts with and stabilizes GINS4 transcript that promotes tumourigenesis in non-small cell lung cancer[J]. J Exp Clin Cancer Res. 2019;38(1):280. doi:10.1186/s13046-019-1276-y
12. Guicciardi ME. AIP1: a new player in TNF signaling[J]. J Clin Invest. 2003;111(12):1813–1815. doi:10.1172/JCI18911
13. Bellazzo A, Di Minin G. Block one, unleash a hundred. Mechanisms of DAB2IP inactivation in cancer. Cell Death Differ. 2017;24:15–25. doi:10.1038/cdd.2016.134
14. Xie D, Gore C, Liu J, et al. Role of DAB2IP in modulating epithelial-to-mesenchymal transition and prostate cancer metastasis[J]. Proc Natl Acad Sci U S A. 2010;107(6):2485–2490. doi:10.1073/pnas.0908133107
15. Malapelle U. Emerging angiogenesis inhibitors for non-small cell lung cancer[J]. Expert Opin Emerg Drugs. 2019;1–11. doi:10.1080/14728214.2019.1619696
16. Wang T, Xing Y, Meng Q, et al. Mammalian Eps15 homology domain 1 potentiates angiogenesis of non-small cell lung cancer by regulating β2AR signaling[J]. J Exp Clin Cancer Res. 2019;38(1):174. doi:10.1186/s13046-019-1162-7
17. Cheng XK, Lin WR, Jiang H, et al. MicroRNA-129-5p inhibits invasiveness and metastasis of lung cancer cells and tumor angiogenesis via targeting VEGF[J]. Eur Rev Med Pharmacol Sci. 2019;23(7):2827–2837. doi:10.26355/eurrev_201904_17559
18. Qin W, Xiong Y, Chen J, et al. DC-CIK cells derived from ovarian cancer patient menstrual blood activate the TNFR1-ASK1-AIP1 pathway to kill autologous ovarian cancer stem cells[J]. J Cell Mol Med. 2018;22(7):3364–3376. doi:10.1111/jcmm.13611
19. Lee JH, Kim JE, Kim BG, et al. STAT3-induced WDR1 overexpression promotes breast cancer cell migration[J]. Cell Signal. 2016;28(11):1753–1760. doi:10.1016/j.cellsig.2016.08.006
20. Liu L, Xu C, Hsieh JT, et al. DAB2IP in cancer[J]. Oncotarget. 2016;7(4):3766–3776. doi:10.18632/oncotarget.6501
21. Ji W, Li Y, He Y, et al. AIP1 Expression in tumor niche suppresses tumor progression and metastasis[J]. Cancer Res. 2015;75(17):3492–3504. doi:10.1158/0008-5472.CAN-15-0088
22. Yano M, Toyooka S, Tsukuda K, et al. Aberrant promoter methylation of human DAB2 interactive protein (hDAB2IP) gene in lung cancers[J]. Int J Cancer. 2005;113(1):59–66. doi:10.1002/ijc.20531
23. Zhang H, He Y, Dai S, et al. AIP1 functions as an endogenous inhibitor of VEGFR2-mediated signaling and inflammatory angiogenesis in mice[J]. J Clin Invest. 2008;118(12):3904–3916. doi:10.1172/JCI36168
24. Ceci C, Lacal PM, Tentori L, et al. Experimental evidence of the antitumor, antimetastatic and antiangiogenic activity of ellagic acid[J]. Nutrients. 2018;10:11. doi:10.3390/nu10111756
25. Agustoni F, Suda K, Yu H, et al. EGFR-directed monoclonal antibodies in combination with chemotherapy for treatment of non-small-cell lung cancer: an updated review of clinical trials and new perspectives in biomarkers analysis[J]. Cancer Treat Rev. 2018;72(12):15–27. doi:10.1016/j.ctrv.2018.08.002
26. Zhou HJ, Chen X, Huang Q, et al. AIP1 mediates vascular endothelial cell growth factor receptor-3-dependent angiogenic and lymphangiogenic responses[J]. Arterioscler Thromb Vasc Biol. 2014;34(3):603–615. doi:10.1161/ATVBAHA.113.303053
27. Chabowski M, Nowak A, Grzegrzolka J, et al. Comparison of microvessel density using nestin and CD34 in colorectal cancer[J]. Anticancer Res. 2018;38(7):3889–3895. doi:10.21873/anticanres.12673
28. Pammar C, Nayak RS, Kotrashetti VS. Comparison of microvessel density using CD34 and CD105 in oral submucous fibrosis and its correlation with clinicopathological features: an immunohistochemical study[J]. J Cancer Res Ther. 2018;14(5):983–988. doi:10.4103/0973-1482.181186
29. Yuan A, Yu CJ, Shun CT, et al. Total cyclooxygenase-2 mRNA levels correlate with vascular endothelial growth factor mRNA levels, tumor angiogenesis and prognosis in non-small cell lung cancer patients. Int J Cancer. 2005;115:545–555. doi:10.1002/ijc.20898
30. Vermeulen PB, Gasparini G, Fox SB, et al. Second international consensus on the ethodology and criteria of evaluation of angiogenesis quantification in solid human tumours. Eur J Cancer. 2002;38(12):1564–1579. doi:10.1016/S0959-8049(02)00094-1
31. Dote H, Toyooka S, Tsukuda K, et al. Aberrant promoter methylation in human DAB2 interactive protein (hDAB2IP) gene in breast cancer. Clin Cancer Res. 2004;10(6):2082–2089. doi:10.1158/1078-0432.CCR-03-0236
32. Dote H, Toyooka S, Tsukuda K, et al. Aberrant promoter methylation in human DAB2 interactive protein (hDAB2IP) gene in gastrointestinal tumour. Br J Cancer. 2005;92(6):1117–1125. doi:10.1038/sj.bjc.6602458
33. Yang C, He H, Zhang T, et al. Decreased DAB2IP gene expression, which could be induced by fractionated irradiation, is associated with resistance to γ-rays and α-particles in prostate cancer cells[J]. Mol Med Rep. 2016;14(1):567–573. doi:10.3892/mmr.2016.5281
34. Li B, Xu WW, Han L, et al. MicroRNA-377 suppresses initiation and progression of esophageal cancer by inhibiting CD133 and VEGF. Oncogene. 2017;36(28):3986–4000.
35. Yang L, Li Y, Ling X, et al. A common genetic variant (97906C>A) of DAB2IP/AIP1 is associated with an increased risk and early onset of lung cancer in Chinese males[J]. PLoS One. 2011;6(10):e26944. doi:DOI:10.1371/journal.pone.0026944
36. Wang ZR, Wei JH, Zhou JC, et al. Validation of DAB2IP methylation and its relative significance in predicting outcome in renal cell carcinoma[J]. Oncotarget. 2016;7(21):31508–31519. doi:10.18632/oncotarget.8971
37. Zhu J, Geyan W, Qingyuan L, et al. Overexpression of suprabasin is associated with proliferation and tumorigenicity of esophageal squamous cell carcinoma. Sci Rep. 2016;6:21549.
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


