Back to Journals » Clinical Ophthalmology » Volume 14
Long-Term Ranibizumab Treatment in Neovascular Age-Related Macular Degeneration: A Belgian Subanalysis from the Global Real-World LUMINOUSTM Study
Authors Leys AM, Ramboer E , Favreau M, Denhaerynck K , MacDonald K , Abraham I, Brié H
Received 16 December 2019
Accepted for publication 29 April 2020
Published 2 June 2020 Volume 2020:14 Pages 1473—1481
DOI https://doi.org/10.2147/OPTH.S242547
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Scott Fraser
Anita M Leys,1,2 Eva Ramboer,3 Mérédis Favreau,3 Kris Denhaerynck,4,5 Karen MacDonald,4 Ivo Abraham,4,6– 8 Heidi Brié3
1Department of Ophthalmology, Universitair Ziekenhuis Gasthuisberg, KULeuven, Leuven, Belgium; 2Oogartsen, Alken, Belgium; 3Novartis Pharma, Vilvoorde, Belgium; 4Matrix45, Tucson, AZ, USA; 5Department of Public Health, University of Basel, Basel, Switzerland; 6Center for Health Outcomes and Pharmacoeconomic Research, University of Arizona, Tucson, AZ, USA; 7Department of Pharmacy Practice and Science, College of Pharmacy, University of Arizona, Tucson, AZ, USA; 8Department of Family and Community Medicine, College of Medicine – Tucson, University of Arizona, Tucson, AZ, USA
Correspondence: Heidi Brié
N.V. Novartis Pharma S.A., Medialaan 40, Vilvoorde B-1800, Belgium
Tel +3222461774
Email [email protected]
Purpose: To evaluate long-term, real-world treatment patterns and outcomes of ranibizumab 0.5 mg for neovascular age-related macular degeneration (nAMD) in a Belgian cohort.
Patients and Methods: This Belgian (BE) cohort of the 5-year global observational LUMINOUS study included 229 patients with nAMD. Outcomes included visual acuity (VA), central retinal thickness (CRT) and safety.
Results: The mean age was 79.5± 7.7 years. The majority of patients (67.7%) were female and all patients were Caucasian. Most patients previously received ranibizumab with only 17.5% of patients being treatment-naïve. The injection frequency declined over time irrespective of prior treatment status (p< 0.0001), with treatment-naïve eyes receiving a mean of 4.2± 2.9 yearly injections and prior-ranibizumab eyes 3.6± 2.7. Regression analysis confirmed first-year VA increases for treatment-naïve eyes (p=0.002) followed by a slight decrease of − 1.8 letters per year. For prior-ranibizumab eyes, the visual changes over 1 year were statistically non-significant (p=0.90) but declined slightly after year one (p< 0.0001). Anatomically, the CRT of treatment-naïve eyes decreased over time from baseline (p< 0.0001), whereas the CRT of prior-ranibizumab eyes remained stable (p=0.43). No new safety findings were identified.
Conclusion: LUMINOUS-BE reconfirms the well-characterized benefit-risk profile of ranibizumab for nAMD treatment. The observed low injection frequency reflects a need for more rigorous treatment in real-world settings.
Clinical Trial Registration: NCT01318941.
Keywords: ranibizumab, effectiveness, safety, treatment patterns, neovascular age-related macular degeneration, Belgium
Introduction
Age-related macular degeneration (AMD) is the leading cause of blindness in patients over the age of 50 in developed countries.1–7 The neovascular form of the disease (nAMD) is characterized by the abnormal growth of choroidal blood vessels beneath the macula that disrupts the anatomy and function of the neurosensory retina and causes severe and irreversible loss of vision.8–10
Ranibizumab (Lucentis®, Novartis, Basel, Switzerland and Genentech Inc., South San Francisco, CA, USA), a recombinant, humanized monoclonal antibody fragment that neutralizes all active forms of vascular endothelial growth factor A (VEGF-A), has been approved as intravitreal therapy for several retinal diseases, including nAMD (approved in 2006 in the US and in 2007 in Europe). While the efficacy and safety profile of ranibizumab use in nAMD is well established based on clinical trial evidence,9–12 most evaluations of the longer-term (≥2 years) effectiveness and safety of ranibizumab in routine clinical practice have been limited-sample studies in one or a few countries.13–19 In addition, treatment patterns of ranibizumab have not been extensively investigated in a real-world setting.
In order to provide an answer to these remaining questions, the LUMINOUSTM study, a 5-year, global, multicenter, observational, open-label study that evaluated real-world ranibizumab use and associated outcomes in diverse populations, settings, and clinical practices for any approved indication included in the local product label, was conducted. Being the largest prospective observational trial in the medical retina field, this study recruited 30,138 patients from 488 sites in 42 countries.20
We have previously reported on the 2-year13 and 6-year14 outcomes of treatment with ranibizumab for nAMD as observed in routine clinical practice in Belgium. Here, we assessed treatment patterns and associated outcomes in patients with nAMD of the Belgian (BE) cohort from the global LUMINOUS study, thus adding to the evidence base of real-world effectiveness and safety of ranibizumab use in Belgium.
Materials and Methods
Design, Sample and Setting
This analysis includes the Belgian nAMD subsample of the global, prospective, multicenter, observational, non-interventional, open-label, single-arm LUMINOUS study (NCT01318941). This 5-year study (March 2011-April 2016) recruited 30,138 consenting adults patients (≥18 years), enrolled by the local investigators at the participating outpatient clinics. Patients were previously treated with, currently treated with, or initiating treatment with ranibizumab for all approved indications per the local product label.20
The global sample included 22,717 patients with nAMD. The LUMINOUS methodology has been detailed elsewhere.20 We summarize below key elements relevant to the LUMINOUS-BE analysis.
Being an observational study, all data were recorded as available from routine clinical practice on a clinical visit schedule determined by the treating physician. Patients not seen at least once per year were discontinued from the study. The overall duration of the study was 5 years, with a minimum of 1-year follow-up period per patient.
The primary eye with nAMD was the unit of observation and analyses were stratified by prior treatment status. Excluded were patients receiving systemic or ocular anti-VEGF therapy other than ranibizumab in the 90 or 30 days prior to enrollment, respectively, or participating in other investigational studies.
Variables and Measurement
Baseline data included socio-demographics, (non-)ocular medical history, prior (non-)ocular treatments, best-corrected visual acuity (VA), central retinal thickness (CRT), and start date and dose of ranibizumab therapy. The lesion characteristics were identified by the investigator and captured at start of study. Follow-up data included the administration date of ranibizumab, concomitant (non-)ocular treatments, (serious) adverse events (SAE/AE), reasons for discontinuation, VA, and CRT. The number of ranibizumab 0.5 mg injections was calculated per completed year of follow-up. Safety evaluations comprised the monitoring and assessment of occurrence, relationship, and severity of (non-)ocular AEs.
Effectiveness parameters used for long-term evaluation were: 1) change in best-corrected VA since baseline, expressed in (approximate) Early Treatment Diabetic Retinopathy Study (ETDRS) letters, and 2) change in CRT since baseline, expressed in µm. VA change was also categorized as gains of ≥15, 10–14, or 5–9 letters and VA status as the proportion of eyes with VA of ≥73 letters.
Statistical Analysis
Patient demographics, medical history, ocular disease history, prior treatments, and other baseline characteristics were presented using standard descriptive statistics under consideration of applicable levels of measurement.
We applied linear mixed regression analysis, employing random intercepts to separate out within-center from between-center and within-patient from between-patient variability. Evaluation of changes over time among the prior treatment subgroups was achieved by entering an interaction of subgroup and time variables and specifying contrasts for specific hypotheses testing. The level of statistical significance was set at 0.05. All statistical analyses were performed using SAS® v.9.4 (SAS Institute Inc., Cary, NC, USA).
Compliance
LUMINOUS was designed, implemented, and reported in accordance with the Guidelines for Good Pharmacoepidemiology Practices issued by the International Society for Pharmacoepidemiology, with any applicable national guidelines, and with the ethical principles laid down in the Declaration of Helsinki. Approval was obtained from an Ethics Committee or Institutional Review Board at each participating center and all patients or their legal proxy gave written informed consent.
Results
Sample Composition & Baseline Ocular Characteristics
Thirteen Belgian centers enrolled 229 patients with nAMD, with a mean age of 79.5±7.7 years (Table 1). The majority of patients (67.7%) were female, and all patients were Caucasian.
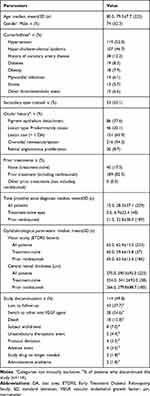 |
Table 1 Patient Demographic and Clinical Characteristics at Study Entry, Study Discontinuation (N=229) |
Mean follow-up time was 30.5±17.0 months, with half the patients discontinuing the study early (n=114; 49.8%) at an average of 13.6±13.4 months. Sample sizes at 1, 2, 3 and 4 years were 186 (81.2%), 139 (60.7%), 100 (43.7%) and 48 (21.0%), respectively. Primary reasons for premature study stop were loss to follow up (37.7%) or switch to another anti-VEGF agent (24.6%) (Table 1). The most frequent non-ocular comorbidities were hypertension (n=119, 52.0%) and hypercholesterolemia/hyperlipidemia (n=107, 46.7%). With regard to the lesion characteristics, as captured at start of study by the investigators, about 20% (n=46) of patients had a lesion of the predominantly classic type and 86 (37.6%) patients had a pigment epithelium detachment. In total, 40 (17.5%) patients were treatment-naïve and the remaining 189 (82.5%) had been previously treated with ranibizumab (prior-ranibizumab).
At baseline, the mean VA was higher in patients treated previously with ranibizumab (63.5±13.6 letters) compared with treatment-naïve patients (59.6±15.8 letters). The mean baseline CRT, on the other hand, was lower in patients treated previously with ranibizumab (279.8±88.7 µm) compared with treatment-naïve patients (341.2±92.0 µm).
Treatment Patterns
The mean number of yearly visits was 7.9±2.8 for treatment-naïve and 7.5±2.9 for prior-ranibizumab patients (Table 2).
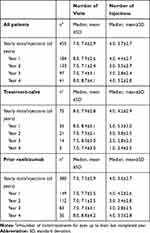 |
Table 2 Number of Visits and Number of Ranibizumab Injections (N=229) |
Regarding the mean number of yearly injections, treatment-naïve eyes received 4.2±2.9 yearly injections and eyes previously treated with ranibizumab 3.6±2.7, with an injection frequency declining over time irrespective of prior treatment status (p<0.0001). With the decline in frequency, an increase in time intervals between injections was observed (Table S1).
Besides unstable VA, the most common reason for re-treatment was optical coherence tomography abnormalities at 62.3% and 63.9% of re-treatments in treatment-naïve and prior-ranibizumab cohorts, respectively (Table S2).
Visual Acuity
Quarterly changes in letters read compared to baseline for treatment-naïve and prior-ranibizumab eyes are presented in Figure 1 (see Table S3 for point estimates). For treatment-naïve eyes, regression analysis confirmed first-year increases with annual VA change estimates of β=3.9 (95% CI: 1.5, 6.3; p=0.002; Table S4). After the first year, VA decreased slightly by −1.8 letters per year (β= −1.8; 95% CI: −2.9, −0.7; p=0.001). For prior-ranibizumab-treated eyes, changes over 1 year were statistically non-significant at 0.03±11.7 (β=−0.1; 95% CI: −1.2, 1.1; p=0.90). After 1 year, VA declined slightly in prior-ranibizumab eyes (β= −1.7; 95% CI: −2.2, −1.2; p<0.0001).
Across years 1 through 4, between 33.3% and 53.3% of treatment-naïve eyes and between 30.4% and 36.3% of prior-ranibizumab eyes attained ≥73 letters read (Table S5). Gains of at least 5 letters (ie, sum of eyes with ≥5, ≥10, and ≥15 letters gained) ranged from 47.6% to 66.7% for treatment-naïve and from 32.9% to 39.5% for prior-ranibizumab over all 4 years.
Central Retinal Thickness
Quarterly changes in CRT compared to baseline for treatment-naïve and prior-ranibizumab eyes are depicted in Figure 2 (see Table S3 for point estimates). Regression analysis (Table S4) showed that the CRT of treatment-naïve eyes decreased over time at a rate of −14.0 µm per year from baseline (95% CI: −18.6, −9.4; p<0.0001), whereas prior-ranibizumab eyes remained stable (β=−0.8, 95% CI: −2.7, 1.1, p=0.43).
Safety
Ocular AEs were reported in 64 (27.9%) patients (treatment-naïve: 22 [55.0%], prior-ranibizumab: 42 [22.2%]) (Table S6). Non-ocular AEs were reported in 100 (43.7%) patients (treatment-naïve: 17 [42.5%], prior-ranibizumab: 83 [43.9%]) (Table S6). Ocular adverse events suspected to be treatment-related (ranibizumab and/or ocular injection) were reported for 14 (6.1%) patients (treatment-naïve: 5 [12.5%], prior-ranibizumab: 9 [4.8%]), the most common of which were conjunctival haemorrhage, endophthalmitis, and eye pain (Table S7). Five (2.6%) prior-ranibizumab patients experienced seven non-ocular AEs suspected to be related to ranibizumab and/or ocular injection (Table S7). Eleven (4.8%) patients had ocular SAEs, leading to discontinuation of ranibizumab for 3 patients (1.3%); however, only two (0.9%) were suspected to be treatment related. Sixty (26.2%) patients experienced non-ocular SAEs, six (2.6%) of which were suspected to be treatment related but did not result in treatment discontinuation. An additional four patients had ocular and two had non-ocular AEs (all non-serious) leading to discontinuation. There were 18 deaths (7.9%) during the study period, none of which were suspected to be treatment-related.
Discussion
This analysis of the Belgian patients with nAMD in the real-world LUMINOUS study consisted of 229 treatment-naïve or prior-ranibizumab-treated patients with an average follow-up of 2.5 years.
The outcomes for the treatment-naïve eyes were largely consistent with data from previous longer-term real-world studies of ranibizumab,13–19 including two Belgian studies reporting on 2-year and 6-year outcomes.13,14 Although variability was detected in the VA and CRT values, overall, a generally well-preserved mean VA was observed, with an initial gain that was gradually lost over time (−1.8 letters/year). Anatomically, a sustained decrease in mean CRT was recorded to study end. This discrepancy in long-term visual and anatomic results is consistent with prior findings.14,18,21 Similarly, the prior-ranibizumab eyes showed a slight decline (−1.7 letters/year) in VA from year 1 onwards, but stable CRT throughout the study period. Reasonably, though pre-ranibizumab VA and CRT parameters were not available for the previously ranibizumab-treated eyes, (many of) these eyes had probably already achieved a therapeutic benefit by the start of the LUMINOUS study and entered the study with stable disease.
Of note, the VA and CRT outcomes observed in this study were associated with a rather low mean number of yearly injections and a steadily declining injection frequency over time. Several studies have reported a relationship between anti-VEGF treatment frequency and VA outcomes.13,18,19,22–25 For instance, in SEVEN-UP,25 a multicenter, non-interventional cohort study of 65 patients originally treated with ranibizumab in the ANCHOR and MARINA trials and the HORIZON extension, showed that better visual outcomes were obtained among intensively treated patients, suggesting an association with injection frequency. One retrospective study18 evaluating an as-needed ranibizumab regimen over 5 years also found a positive association between number of injections and improvements in VA, suggesting the benefit of regular treatment beyond the initial phase. The retrospective AURA study19 demonstrated that more frequent visits (ie, monitoring) and injections (ie, re-treatments) were associated with maintenance of VA gains.
The PRN dosing schedule with treatment guidance by VA and/or optical coherence tomography was the regimen of choice in Belgium during the LUMINOUS study. In individualized, reactive, as-needed anti-VEGF regimens, monitoring frequency and re-treatment criteria impact effectiveness.12,26-28 Being a chronic, progressive disease, nAMD requires sustained monitoring and treatment for many years.15,16,25 However, (re-)treatment inertia may be responsible for irreversible VA deterioration;29 thus, PRN regimens should include monthly monitoring in order to treat any recurrence as soon as possible prior to lasting VA damage. A recent secondary analysis of the Comparison of Age-Related Macular Degeneration Treatment Trial, a randomized clinical trial, has shown that visit adherence contributes to visual acuity outcomes.30 In the current analysis, the mean number of yearly visits was 7.6±2.9, which is not as strict as the monthly monitoring in clinical trials and reflects the contingencies of real-life situations, such as practical feasibility and patients’ willingness and ability to comply. Indeed, in the setting of routine clinical practice, where patients are not followed as intensively as in clinical trials nor treated in accordance with a study protocol, the undertreatment may be accompanied by multiple recurrences of pronounced exudation, potentially damaging photoreceptors and thus leading to vision loss.29,31 This may explain the functional deterioration noticed in this Belgian analysis despite morphologic response to therapy.
Since nAMD patients often require anti-VEGF treatment for many years, evaluation of the long-term ocular and non-ocular safety is necessary. Overall, the ocular and non-ocular AEs observed in the Belgian nAMD sample of the LUMINOUS study were consistent with the types of AEs observed in prior controlled studies and consistent with the well-established safety profile of ranibizumab. No new safety findings were identified.
Limitations of this LUMINOUS-BE analysis are similar to those of the parent global LUMINOUS study. First, due to convenience sampling, selection bias cannot be excluded. Furthermore, as this was a study on real-world ranibizumab practice patterns and outcomes, all patients were treated with ranibizumab and there was no comparison group of untreated patients or patients treated only with other therapies. Lastly, as described in other long-term real-world studies,16,32,33 the study discontinuation rate was significant in the current analysis with half of the patients stopping the study prematurely. Although the data reflect the long-term patient journey in real-life practice, the dropout rate in combination with the rather small sample size may affect the reliability of the effectiveness results, primarily beyond the first year. In analogy with the 2-year Belgian HELIOS study,13 lost-to-follow-up was the main cause for patient drop-out in the current analysis. Recently a study highlighted the significant visual acuity decline observed after a period of being lost to follow-up.34 Factors related to poor follow-up adherence have been identified in previous studies and include among others older age, greater distance to hospital, and lower baseline vision.16,32,35 Though loss of patients from regular follow-up in the long-term is inevitable, these findings highlight the importance of identifying patients at risk and exploring measures to improve proper therapy adherence in order to avoid the deleterious effects caused by a gap in care.
Notwithstanding these limitations and bearing in mind the natural evolution of the disease, the current Belgian sample of the LUMINOUS reconfirms the well-characterized benefit-risk profile of ranibizumab for treatment of nAMD in a real-world clinical setting and adds to the growing body of evidence of the long-term real-world effectiveness and safety of ranibizumab. The observed low injection frequency reflects a need for more rigorous treatment in real-world settings. As such, the real-world evidence from this study may help guide Belgian clinicians in optimizing the frequency of ranibizumab injections in the management of nAMD and counseling patients undergoing long-term anti-VEGF therapy in clinical practice.
Conclusions
LUMINOUS-BE reports long-term real-world ranibizumab treatment patterns and clinical outcomes in nAMD patients that supports the well-characterized benefit-risk profile of ranibizumab. A PRN dosing schedule prevailed in Belgium at the time and a pattern of relative under-treatment was observed, consistent with other real-world studies utilizing this approach.
Abbreviations
AE, adverse event; CRT, central retinal thickness; ETDRS, Early Treatment Diabetic Retinopathy Study; nAMD, neovascular (wet) age-related macular degeneration; SAE, serious adverse event; VA, visual acuity; VEGF, vascular endothelial growth factor.
Data Sharing
This data for this cohort analysis is part of a global real-world observational study, not a clinical trial. As such, the authors do not intend to share the cohort data but leave the decision regarding data sharing to the parent study authors.
Ethics Approval and Informed Consent
LUMINOUS was designed, implemented, and reported in accordance with the Guidelines for Good Pharmacoepidemiology Practices issued by the International Society for Pharmacoepidemiology, with any applicable national guidelines, and with the ethical principles laid down in the Declaration of Helsinki. Approval was obtained from an Ethics Committee or Institutional Review Board at each participating center and all patients or their legal proxy gave written informed consent. The committee approving the study in participating Belgian centers was the Commissie Medische Ethiek of the Universitaire Ziekenhuizen KULeuven 2011, S52749.
Acknowledgments
The authors thank all Belgian centers that participated in the LUMINOUS study for their data acquisition and/or research execution.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
Heidi Brié, Eva Ramboer and Mérédis Favreau are employees of Novartis Pharma. Kris Denhaerynck, Karen MacDonald, and Ivo Abraham are associated with Matrix45, with Karen MacDonald and Ivo Abraham holding equity in Matrix45, which was hired by Novartis Pharma to develop study protocols, conduct statistical analyses and develop study reports and manuscripts for other ophthalmology projects outside the submitted work. By company policy, Matrix45 associates are prohibited from owning equity in sponsor organizations (except through mutual funds or other independently administered investment instruments) or contracting independently with sponsor organizations. Matrix45 provides similar services to those described in this paper to other companies on a non-exclusivity basis. The authors report no other conflicts of interest in this work.
References
1. Friedman DS, O’Colmain BJ, Munzo B, et al. Prevalence of age-related macular degeneration in the United States. Arch Ophthalmol. 2004;122:564–572.
2. Evans J, Wormald R. Is the incidence of registrable age-related macular degeneration increasing? Br J Ophthalmol. 1996;80:9–14. doi:10.1136/bjo.80.1.9
3. Bressler NM. Age-related macular degeneration is the leading cause of blindness. JAMA. 2004;291:1900–1901. doi:10.1001/jama.291.15.1900
4. Resnikoff S, Pascolini D, Etya’ale D, et al. Global data on visual impairment in the year 2002. Bull World Health Organ. 2004;82:844–851. doi:10.1590/S0042-96862004001100009
5. Augood C, Fletcher A, Bentham G, et al. Methods for a population-based study of the prevalence of and risk factors for age-related maculopathy and macular degeneration in elderly European populations: the EUREYE study. Ophthalmic Epidemiol. 2004;11:117–129. doi:10.1076/opep.11.2.117.28160
6. Ferris FL, Fine SL, Hyman L. Age-related macular degeneration and blindness due to neovascular maculopathy. Arch Ophthalmol. 1984;102:1640–1642. doi:10.1001/archopht.1984.01040031330019
7. Klein R, Klein B, Linton KL. Prevalence of age-related maculopathy: the Beaver Dam Eye Study. Ophthalmology. 1992;99:933–943. doi:10.1016/S0161-6420(92)31871-8
8. Brown DM, Kaiser PK, Michels M, et al. Ranibizumab versus verteporfin for neovascular age-related macular degeneration. N Engl J Med. 2006;355(14):1432–1444. doi:10.1056/NEJMoa062655
9. Brown DM, Michels M, Kaiser PK, Heier JS, Sy JP, Ianchulev T. Ranibizumab versus verteporfin photodynamic therapy for neovascular age-related macular degeneration: two-year results of the ANCHOR study. Ophthalmology. 2009;116(1):57–65.e55. doi:10.1016/j.ophtha.2008.10.018
10. Rosenfeld PJ, Brown DM, Heier JS, et al. Ranibizumab for neovascular age-related macular degeneration. N Engl J Med. 2006;355(14):1419–1431. doi:10.1056/NEJMoa054481
11. Abraham P, Yue H, Wilson L. Randomized,double-masked,sham-controlled trial of ranibizumab for neovascular age-related macular degeneration: PIER study year 2. Am J Ophthalmol. 2010;150(3):315–324. e1. doi:10.1016/j.ajo.2010.04.011
12. Lalwani GA, Rosenfeld PJ, Fung AE, et al. A variable-dosing regimen with intravitreal ranibizumab for neovascular age-related macular degeneration: year 2 of the PrONTO Study. Am J Ophthalmol. 2009;148(1):43–58. e1. doi:10.1016/j.ajo.2009.01.024
13. Rakic JM, Leys A, Brié H, et al. Real-world variability in ranibizumab treatment and associated clinical, quality of life, and safety outcomes over 24 months in patients with neovascular age-related macular degeneration: the HELIOS study. Clin Ophthalmol. 2013;7:1849–1858. doi:10.2147/OPTH.S49385
14. Jacob J, Brié H, Leys A, et al. Six-year outcomes in neovascular age-related macular degeneration with ranibizumab. Int J Ophthalmol. 2017;10(1):81–90. doi:10.18240/ijo.2017.01.14
15. Kruger Falk M, Kemp H, Sorensen TL. Four-year treatment results of neovascular age-related macular degeneration with ranibizumab and causes for discontinuation of treatment. Am J Ophthalmol. 2013;155(1):89–95.e83. doi:10.1016/j.ajo.2012.06.031
16. Pushpoth S, Sykakis E, Merchant K, Browning AC, Gupta R, Talks SJ. Measuring the benefit of 4 years of intravitreal ranibizumab treatment for neovascular age-related macular degeneration. Br J Ophthalmol. 2012;96(12):1469–1473. doi:10.1136/bjophthalmol-2012-302167
17. Rasmussen A, Bloch SB, Fuchs J, et al. A 4-year longitudinal study of 555 patients treated with ranibizumab for neovascular age-related macular degeneration. Ophthalmology. 2013;120(12):2630–2636. doi:10.1016/j.ophtha.2013.05.018
18. Zhu M, Chew JK, Broadhead GK, et al. Intravitreal Ranibizumab for neovascular Age-related macular degeneration in clinical practice: five-year treatment outcomes. Graefes Arch Clin Exp Ophthalmol. 2015;253(8):1217–1225. doi:10.1007/s00417-014-2799-8
19. Holz FG, Tadayoni R, Beatty S, et al. Multi-country real-life experience of anti-vascular endothelial growth factor therapy for wet age-related macular degeneration. Br J Ophthalmol. 2015;99(2):220–226. doi:10.1136/bjophthalmol-2014-305327
20. Holz FG, Figueroa MS, Bandello F, et al. Ranibizumab treatment in treatment-naïve neovascular age-related macular degeneration: results from LUMINOUS, a global real-world study. Retina. 2019:1. doi:10.1097/IAE.0000000000002670.
21. Pedrosa AC, Reis-Silva A, Pinheiro-Costa J, et al. Treatment of neovascular age-related macular degeneration with anti-VEGF agents: retrospective analysis of 5-year outcomes. Clin Ophthalmol. 2016;10:541–546. doi:10.2147/OPTH.S90913
22. Kim LN, Mehta H, Barthelmes D, Nguyen V, Gillies MC. Meta analysis of real-world outcomes of intravitreal ranibizumab for the treatment of neovascular age-related macular degeneration. Retina. 2016;36(8):1418–1431. doi:10.1097/IAE.0000000000001142
23. Peden MC, Suner IJ, Hammer ME, Grizzard WS. Long-term outcomes in eyes receiving fixed-interval dosing of anti-vascular endothelial growth factor agents for wet age-related macular degeneration. Ophthalmology. 2015;122(4):803–808. doi:10.1016/j.ophtha.2014.11.018
24. Qin VL, Young J, Silva FQ, Conti FF, Singh RP. Outcomes of patients with exudative age-related macular degeneration treated with antivascular endothelial growth factor therapy for three or more years: a review of current outcomes. Retina. 2018;38(8):1500–1508. doi:10.1097/IAE.0000000000001753
25. Rofagha S, Bhisitkul RB, Boyer DS, Sadda SR, Zhang K. Seven-year outcomes in ranibizumab-treated patients in ANCHOR, MARINA, and HORIZON: a multicenter cohort study (SEVEN-UP). Ophthalmology. 2013;120(11):2292–2299. doi:10.1016/j.ophtha.2013.03.046
26. Boyer DS, Heier JS, Brown DM, Francom SF, Ianchulev T, Rubio RG. A Phase IIIb study to evaluate the safety of ranibizumab in subjects with neovascular age-related macular degeneration. Ophthalmology. 2009;116(9):1731–1739. doi:10.1016/j.ophtha.2009.05.024
27. Ho AC, Busbee BG, Regillo CD, et al. Twenty-four-month efficacy and safety of 0.5 mg or 2.0 mg ranibizumab in patients with subfoveal neovascular age-related macular degeneration. Ophthalmology. 2014;121(11):2181–2192. doi:10.1016/j.ophtha.2014.05.009
28. Martin DF, Maguire MG, Fine SL, et al. Ranibizumab and bevacizumab for treatment of neovascular age-related macular degeneration: two-year results. Ophthalmology. 2012;119(7):1388–1398. doi:10.1016/j.ophtha.2012.03.053
29. Muether PS, Hoerster R, Hermann MM, Kirchhof B, Fauser S. Long-term effects of ranibizumab treatment delay in neovascular age-related macular degeneration. Graefes Arch Clin Exp Ophthalmol. 2013;251(2):453–458. doi:10.1007/s00417-012-2038-0
30. Ramakrishnan MS, Yu Y, VanderBeek BL. Association of visit adherence and visual acuity in patients with neovascular age-related macular degeneration: secondary analysis of the Comparison of Age-Related Macular Degeneration Treatment Trial [published online February 6, 2020]. JAMA Ophthalmol. 2020;138(3):237–242. doi:10.1001/jamaophthalmol.2019.4577
31. Adrean SD, Chaili S, Ramkumar H, Pirouz A, Grant S. Consistent long-term therapy of neovascular age-related macular degeneration managed by 50 or more anti-VEGF injections using a Treat-Extend-Stop Protocol. Ophthalmology. 2018;125(7):1047–1053. doi:10.1016/j.ophtha.2018.01.012
32. Boulanger-Scemama E, Querques G, About F, et al. Ranibizumab for exudative age-related macular degeneration: a five year study of adherence to follow-up in a real-life setting. J Fr Ophthalmol. 2015;38(7):620–627. doi:10.1016/j.jfo.2014.11.015
33. Gillies MC, Campain A, Barthelmes D, et al. Long-term outcomes of treatment of neovascular age-related macular degeneration: data from an observational study. Ophthalmology. 2015;122(9):1837–1845. doi:10.1016/j.ophtha.2015.05.010
34. Soares RR, Mellen P, Garrigan H, et al. Outcomes of eyes lost to follow-up with neovascular age-related macular degeneration receiving intravitreal anti-vascular endothelial growth factor. Ophthalmol Retina. 2020;4(2):134–140. doi:10.1016/j.oret.2019.07.010
35. Obeid A, Gao X, Ali FS, et al. Loss to follow-up among patients with neovascular age-related macular degeneration who received intravitreal anti-vascular endothelial growth factor injections. JAMA Ophthalmol. 2018;136(11):1251–1259. doi:10.1001/jamaophthalmol.2018.3578
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.






