Back to Journals » Clinical Ophthalmology » Volume 14
Literature Review of Surgical Treatment in Idiopathic Full-Thickness Macular Hole
Authors Ittarat M , Somkijrungroj T, Chansangpetch S , Pongsachareonnont P
Received 15 May 2020
Accepted for publication 13 July 2020
Published 30 July 2020 Volume 2020:14 Pages 2171—2183
DOI https://doi.org/10.2147/OPTH.S262877
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Mantapond Ittarat,1,2 Thanapong Somkijrungroj,2,3 Sunee Chansangpetch,2,4 Pear Pongsachareonnont2,3
1Surin Hospital and Surin Medical Education Center, Department of Ophthalmology, Suranaree University of Technology, Surin, Thailand; 2Department of Ophthalmology, Faculty of Medicine, Chulalongkorn University and King Chulalongkorn Memorial Hospital, Thai Red Cross Society, Bangkok, Thailand; 3Vitreoretinal Research Unit, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand; 4Glaucoma Research Unit, Faculty of Medicine, Chulalongkorn University, Bangkok, Thailand
Correspondence: Pear Pongsachareonnont Department of Ophthalmology, Faculty of Medicine 1873 Rama IV Road, Patumwan, Bangkok 10330, Thailand
Tel +66-2256-4142
Fax +66-2-252-8290
Email [email protected]
Purpose: To summarize current surgical techniques for treating primary macular holes (MHs).
Methods: We reviewed publications detailing surgical approaches to primary MHs, briefly described their protocols, and outlined their results.
Results: Currently, the technique for primary MH repair is pars plana vitrectomy, removing the posterior cortical vitreous, stripping the epiretinal membranes, and ending with intraocular gas tamponade. The evident benefit of peeling off the internal limiting membrane (ILM) was clearly shown for MHs at stages 2 to 4 by achieving an anatomical closure rate of > 90%, even in large MH up to 650 μm. Newer MH surgical techniques include modification of ILM flap techniques, placing an autologous scaffolding of tissue within the hole, and cell therapy has shown to increase the closure rate of large and chronic macular holes, resulting in modest functional improvement in complicated MHs.
Conclusion: Since the turn of the century, the success rate of modern macular surgery has increased, even for large and chronic MHs. There seems to be no limit to novel concepts in MH surgery, which range from anatomical closure to those proposing natural restoration of visual function via stem cell therapy.
Keywords: macular hole, macular hole surgery, stem cell therapy, internal limiting membrane peeling
Introduction
The idiopathic macular hole (MH) was first described by Johnson and Gass in 1988.1 The full-thickness macular hole (or just “macular hole”) is defined as an anatomical defect in the fovea that interrupts all neuroretinal layers. The pathogenesis of MH arises from the remaining vitreous cortex in the macular area after the vitreous has separated. The vitreoretinal interface force plays an important role in the development of MH. The dynamic forces of the vitreous fluid concentrate on the macular layers, causing swelling of the middle and outer macular region, with elevation and retraction of inner retinal layers. As the swelling increased, the hole became enlarged.2–4 The idiopathic MHs account for most of the MHs (85%). Other secondary causes are blunt trauma, high myopia, macular schisis, macular telangiectasia type 2, wet age-related macular degeneration with intravitreal injections of anti-VEGF, and surgical trauma.5 The MH predominantly affects women >65 years of age and is more common in myopic eyes.6 The prevalence of MH in the general population is around 3.3/1000 people.7 MH is usually unilateral, although bilateral MHs have been reported at a rate of 10–15%.8,9 There are two main classification systems for MH. The first classification described by Gass is based on the clinical observations on the evolution of MH.1 The recent classification has been proposed by The International Vitreomacular Traction Study (IVTS) Group. This scheme encompasses the presence of vitreomacular adhesion (VMA), vitreomacular traction (VMT) in conjunction with the characteristics of the MH.5 Table 1 shows the summary of both classifications. Small MHs close spontaneously in 2.7–8.6% of patients.1,2 Overall progression from a small to a large MH occurs in 74% of patients within 2 years of the initial diagnosis.1,2
 |
Table 1 Classification in Idiopathic Macular Holes |
Most MHs are surgical cases. Currently, the only medication that can be used as an alternative to MH surgery is ocriplasmin (OCP). OCP breaks down the vitreoretinal interface by activating matrix metalloproteinase-2. This medication is approved for the treatment of symptomatic vitreomacular adhesion (VMA) which includes VMA with MH of <400 µm. The MIVI-TRUST clinical trial reported significantly better closure of the MH in 40.6% vs.10.6%, favoring the OCP-treated group. Although the success of MH repair using OCP is evident in small MHs with VMA, some adverse effects due to vitreolytic effect are associated with OCP.10 The other types of MH, particularly Gass stage 2 and higher, are usually indicated for surgical correction.11,12 The purpose of this articles is to review the current surgical techniques and outcomes in idiopathic MH surgery.
Core Principles of Macular Hole Surgery
In 1990, Kelly and Wendel first reported successful closure (58%) of MHs in 52 eyes that underwent pars plana vitrectomy, stripping of the epiretinal membrane (ERM), intraocular gas tamponade and postoperative face down position.13 The benefit of vitrectomy and ERM removal for MHs is that it basically relieves VMT at the hole edge (from both anteroposterior and tangential forces) and induces retinal glial tissue to bridge and close the hole. Similar to the results of two large randomized controlled trials (RCTs), which described the use of vitrectomy for treating full-thickness stage 3 or 4 MHs (VMHS study)14 and the use of surgery for treating idiopathic full-thickness MHs (MMHS study),12 This clearly showed the benefit of surgical management of MH. VMHS reported a 69% anatomical closure rate in the vitrectomy group compared with 4% in the controls. MMHS reported an anatomical closure rate of 80.6% in the surgery group compared with 11.5% in the controls. All patients in these two RCTs showed improved visual acuity.
In 2015, The Cochrane Database of Systemic Reviews presented data from a comparison of vitrectomy versus observation in MH eyes. The study emphasized that vitrectomy improved the anatomical closure of MH (76% in the vitrectomy group, 11% in the observation group) and also improved visual acuity by 1.5 Snellen lines after 6–12 months of follow-up. The Cochrane report also concluded that vitrectomy benefited those with stages 2–4 MH. When present, ERM around the hole should be peeled off. A study from Chen et al showed a higher anatomic hole closure rate of 67% in the ERM peeled eyes compared to 35% of the non-peeled eyes, and MH reopening was significantly associated with excessive ERM growth.15 Based on this evidence, vitrectomy, posterior hyaloid removal, and may include ERM peeling with gas tamponade has become a central component of the surgical treatment for MH.16
Microincision Vitrectomy Surgery (MIVS)
Following the micro-incision vitrectomy surgery (MIVS) era, the theoretical advantages of less invasive surgery could lower the rate of postoperative inflammation and cystoid macular edema, which is believed to be a potential cause of MH reopening. Nevertheless, the current evidence has not proved an advantage of MIVS in decreasing the rate of MH reopening. A retrospective study by Abbey et al showed that MH reopening occurs in 3.3% of patients after primary, small-gauge vitrectomy repair, and the anatomical results are similar to those reported before the smaller-vitrectomy era,17,18 In addition, a study from Krishnan et al found that visual acuity improvement and closure rate outcome were comparable between 20-gauge and 23-gauge phacovitrectomy for MH repair. However, the MIVS offers a benefit of having less operative time with lower incidence of retinal break and short-term elevated intraocular pressure (IOP) than the 20 gauge MH repair.19
Gas Choice
Gas tamponade helps keep the hole closed by bridging the hole edge more closely, thereby preventing fluid from the vitreous cavity from flowing through the hole. Lai et al reported using silicone oil (SO) tamponade compared with gas C3F8. The anatomical closures were 65% and 91%, respectively, with the visual results poorer in the eyes with the SO tamponade. As the filled SO eyes must undergo a second operation to remove the SO from the retina, this method is rarely used for primary MH surgery. In 2008, Kim et al compared the use of SF6 for MH closure compared with C3F8 on 79 eyes with an MH. The result has shown a (34/38) 90% closure rate for SF6 and (37/41) 91% for C3F8,20 which is similar to the prospective RCT results reported by Briand et al, with anatomical closure in 93.3% for SF6 and 92.9% for C3F8.21 Similar results were reported using air tamponade. That retrospective study found an anatomical closure rate for air of 92% and for SF6 90%.22 Based on the present data, the use of an air or short-acting gas tamponade such as SF6 was ideal for MH surgery.23
Postoperative Prone Posturing
Although postoperative prone posturing intensifies the buoyancy force exerted to the posterior pole, which theoretically contributes to the success of MH surgery, the duration of the positioning and its benefit are still under debated. Recent publications indicate that long-lasting posturing is not necessary for MH closure after surgery. Yamashita et al evaluated the need for the face-down posture. They reported results from 107 eyes with an MH that were divided into two groups, one with pro re nata posturing and the other with no posturing compared with control eyes, which undertook the traditional 7 days of posturing. The results showed no differences in closure rates. MH surgery achieved high closure rates of 95–97% in all groups.24 Zhang et al reported a prospective RCT of 80 eyes with small- to medium-size MHs that were repaired using ILM peeling and gas tamponade, with and without face-down posturing. They found no differences in the MH closure rates or delayed MH closure. The authors concluded that face-down posturing is not necessary for medium-size MH.25 Similarly, a recent report by Cochrane reviewed three RCTs and found that two of them reported a benefit of face-down positioning only for large MHs. There were no significant effects on the successful closure of small- to medium-size MHs.26 Recently, an RCT by Pasu et al reported 185 eyes with large MHs comparing facedown positioning and face-forward positioning outcomes. The results do not guarantee that facedown positioning after surgery is more likely to close the MH than face-forward positioning, and they are not statistically significant (P=0.08) with an 85.6% closure rate in the face-forward position group and 95.5% closure rate in the facedown position group.27
Concepts Using in Macular Hole Surgery
Internal Limiting Membrane (ILM) Peeling and Flap Techniques
Internal Limiting Membrane Peeling
The ILM peeling technique was first described in 1997 by Eckardt et al.28 The rationale for ILM peeling is the removal of residual adherent vitreous cortex remnants, thereby increasing retinal compliance. Moreover, ILM serves as a scaffold for cellular proliferation, and its removal could decrease the associated fibrocellular proliferation that disallows MH reopening. A pragmatic RCT (n=141) by Lois et al also reported improvement after 1 month of follow-up, with an 84% closure rate of MHs in eyes that underwent ILM peeling compared with 48% of eyes that did not. There were also fewer reoperations (12% vs. 48%, respectively).29 In 2013, the Cochrane Database of Systemic Reviews concluded that, among the RCTs reviewed, there was sufficient evidence to support the beneficial effects of ILM peeling for stages 2–4 idiopathic MHs to improve the primary anatomical hole closure rate, although there was no clear benefit for small MH holes.30 There was also no strong evidence of a difference in best-corrected visual acuity (BCVA) regarding whether to perform ILM peeling in a study with long-term follow-up (6 months postoperatively).31 Foveal sparing ILM peeling is another variation, base on the concept of Muller cells is important for maintaining foveal architecture and reduce the trauma on Muller cells at the foveal area. Foveal sparing ILM peeling shown a resulted in a high closure rate and better postoperative visual acuity.32
Adjuvant dyes, or chromovitrectomy, play an important role in MH surgery because they enhance the visualization of preretinal membranes and/or ILM, thus allowing more precise peeling and limiting the risk of iatrogenic mechanical trauma to the retina. Intraoperative dyes are particularly important for ILM peeling. There are a few dyes to stain the ERM and ILM: indocyanine green (ICG), brilliant blue (BB), and trypan blue (TB). It is known that ICG has a selective affinity for the ILM. Because of its osmolarity, concentration, and presence of iodine, ICG may be toxic to the retina.33 BB also has a selective affinity for ILM with an iso-osmolar solution of 0.25 mg/mL.34 In contrast, TB poorly stains the ILM but also the ERM.35 Shukla et al compared brilliant blue G (BBG), TB, and ICG for use during ILM peeling in patients undergoing MH surgery. The results showed that, among the three dyes, BBG provided the greatest performance in intraoperative facilitation, easy preparation and removal, and excellent ILM staining. It was also friendlier to the retina, containing no toxic iodine, giving it a potential advantage over TB and ICG.36
Internal Limiting Membrane Inverted Flap
The inverted flap technique is developed based on an ILM that Müller cell fragments, which resides in the ILM, can produce cytokines to induce proliferation of gliosis tissue. The inverted flap acts as a scaffold, stimulating glial tissue proliferation on the surface and growing into the hole and retina. The ILM flap thus serves as a barrier, preventing fluid from the vitreous from entering the hole. Creating this microenvironment encourages photoreceptors to move into the correct position. These techniques were first intended to treat large MH.37,38 Fifty large MHs in eyes that had undergone the Michalewska technique showed improved rates of anatomical closure and function. There was a 98% anatomical closure rate, compared with 88% with a standard technique (not inverted ILM peeling). MH closure type II (flat, open) appeared in 2% compared with 19% with the standard technique.39 A Variety of ILM flap techniques have been proposed and have shown good results, such as temporal ILM inverted, the cabbage leaf technique, folded inverted flaps [Figure 1], pedicle ILM transposition flap, and the free flap technique. However, there is still controversy about which technique gives the best outcome. The authors suggest that in cases where ILM is present at the MH, temporal inverted flap or cabbage leaf flap should be employed to leave the hinge attached and prevent the loss of the ILM flap. In cases with no ILM around the macular area, a free ILM flap has been shown to yield a favorable anatomical result. In a large MH, there might be a need to insert the ILM flap into the MH to prevent the free-floating of the ILM flap in the vitreous cavity.38,40,41
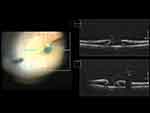 |
Figure 1 Multi-layers of ILM in macular hole during vitrectomy surgery with modified ILM flap technique. |
Autologous Transplantation of Internal Limiting Membrane
Morizane et al determined the using autologous transplantation of ILM for refractory MH. Ten eyes from either the complicated MH or idiopathic MH that failed to achieve closure after the primary surgery was included in the study. The ILM-free flap was peeled off in diameter as the MH size from area of residual ILM. The free flap of ILM was taped by placing low molecular weight viscoelastic material for stabilizing. The result has shown 90% closure rate with significant better postoperative BCVA.42 Pires et al adapted autologous ILM translocation techniques in 12 refractory MH eyes with previous pars plana vitrectomy (PPV) and ILM peeled. The study has shown anatomical closure rate of 91% with significant improvement in BCVA.43
Implantation of a Scaffold for Glial Cell Proliferation
Autologous Lens Capsule Flap Transplantation
The use of autologous lens capsule flap technique was first reported by Chen et al.44 The technique increased the anatomical closure rate in 20 persistent MH eyes which ILM peeled may not available or may not candidate to do ILM adapted techniques. The lens capsule is a natural basement membrane that can be obtained from either anterior capsule or posterior capsule. The concept of application of the lens capsule flap is similar to the ILM-free flap method. This surgical technique combined cataract and MH surgery. The lens capsule flap was gravitationally dropped into the MH followed by air–fluid exchange. Ten anterior capsule flaps and 10 posterior capsule flaps were used in the study. The results showed improved closure rates: 100% and 50% for the anterior and posterior capsule flaps, respectively. At the 4-month follow-up, the mean BCVA had mildly improved.44
Human Amniotic Membrane
Human amniotic membrane (hAM) demonstrated excellent growth support properties for RPE cells and induce RPE cell proliferation and differentiation.45 In vivo transplantation of hAM plug has been used successfully for repairing choroidal hole.46 Rizzo et al reported excellent outcomes using hAM in 8 recurrent MH and 6 retinal detachment.47 Caporossi et al reported the efficacy of hAM as a scaffold in recurrent MHs in pathologic myopia. Sticky chorion layer was facing down the (RPE) under the neuroretina inside the MH.48 Of 16 eyes, the MH was closed in 15 eyes and visual improvement was evident in all patients.
Autologous Neurosensory Retinal Free Flap
Autologous neurosensory retinal-free flap is one of the modified techniques for treating refractory cases especially in highly myopic MH of which thin ILM precludes safe and adequate peeling. The hypothesis is that neurosensory retina, similar to the ILM, can work as a scaffold and help in sealing the hole by forming a macular plug. Grewal et al using autologous neurosensory retinal-free flap also in treating a refractory myopic MHs also showed the successful MH closure.49
Relieving Macular Hole Stiffness and Increasing Retinal Compliance
Tapping the Hole Edges
Tapping the edges of the MH techniques was proposed by Kumar et al in 2013. By observing the macular morphology using OCT, Kusuhara et al found an MH (height/base) index of ≥0.5 with a significantly higher postoperative BCVA after MH repair.50 The MH index represents anteroposterior and tangential traction. Applying this observation, the authors hypothesized that increasing the MH index by tapping the edges of the MH using silicone-tipped drainage could improve closure. The anatomical success rate of this technique in 28 eyes was 89.3%, with visual acuity improving from 20/145 to 20/54 postoperatively.51
Temporal Arcade Retinotomy
This technique, by Charles et al, aimed to release the tangential traction and increase retinal compliance around the MH. The study was performed in six eyes. Closure was achieved in 5 eyes (83%), and visual function improved in 50%, highlighting the drawback of traumatic RPE damage.52
Macular Hole Hydrodissection
This technique aimed to lyse these adhesions between the retina and RPE by passing fluid into the MH using a reflux mode of vitrectomy directed at the area of the MH. Reducing the intrinsic retinal stiffness resulted in the retina becoming more compliant. The technique was first presented by Felfeli et al to increase the closure rate for large and chronic MHs.53 Their results showed completed type 1 anatomical closure in 87.2% and vision improvement in 94.9% of 39 eyes with either a persistent or chronic large MH. In addition, 79.5% of the eyes achieved a BCVA gain of more than two lines.53
Induction Retinal Detachment
Szigiato et al described an induction of macular detachment technique for treating persistent and recurrent MH (N=10). By injection of balanced salt solution into subretina in multiple quadrants, the tighten adhesion of the retina was relieved and allowed the hole edged reapproximate and close. The result showed the closure rate of 90% with modest visual improvement at 6 months of follow-up.54
Promoting Chorioretinal Adhesion
Autologous blood plug can help maintain the ILM flap in place. Moreover, various autologous blood products can act a slow-release fibrin matrix which contains several growth factors and cytokines which are believed to promote the healing process.55 The use of autologous whole blood, autologous serum, autologous platelet concentration, and thrombin has been described for facilitating hole closure.56–59 Paques et al, in an RCT, compared the use of autologous platelet concentrate versus no adjuvant use. They prepared 0.1 mL of the concentrate just before the operation from 16 mL of venous blood mixed with anticoagulant citrate dextrose A. The MH closure rates were 98% and 82%, respectively, with no significant BCVA improvement.57 In 2017, Chakrabarti et al modified the techniques by creating macular plug or autologous gluconated blood clumps, which were composed of 5% glucose and autologous whole blood, to enhance the closure rate. In all, 26 eyes with an MH underwent PPV with an inverted ILM flap adjunct using autologous gluconated blood clamps, the results have shown a higher closure rate (100%) with BCVA improvement (20/200 to 20/63) without the use of gas tamponade.56
The laser application has also been tried. Cho et al reported the use of argon green wavelength laser at the center of the macula to stimulate cytokines, which would promote the formation of a glial plug to close the hole. The results from their RCT that included 29 eyes with a large MH, comparing laser adjuvant after vitrectomy with peeling of ILM and control eyes (without laser) showed MH closure rates of 94.4% vs. 76.9%, respectively. At 3 months postoperatively, the BCVA had significantly improved (p<0.05). Even with the presence of a scotoma, there were only insignificant changes in the visual field.60,61
Promoting Neuroregeneration and Neural Function Recovery
Cell therapy represents a novel alternative option to obtain regeneration of damaged retinal, aiming to improve functional outcome in MH surgery. Transplantation of retinal cells has been considered as a possible treatment of MHs.62 The most recent concept makes use of mesenchymal stem cells (MSCs) and MSC-derived exosomes (MSC-Exos) to promote healing in large and refractory MHs. The MSCs were isolated from human umbilical cord tissue, and their exosomes were created from sequential ultracentrifugation of supernatants of cultured MSCs. It is well known that MSCs and MSC-Exos can prevent retinal damage by inhibiting apoptosis, causing an inflammatory response, and promoting neurodegeneration and recovery of neural function. These techniques are applied by dropping MSCs and MSC-Exos into the MH after PPV with ILM peeling. At the 6-month follow-up, the MHs in six of seven eyes had closed, and the BCVA had improved in five eyes. The drawback of these techniques was the formation of a fibrotic membrane and severe inflammation. However, the risks and benefits of the techniques are still uncertain because of the small sample sizes. Well-designed, larger clinical trials will clarify the potential of these techniques.62,63
Macular Hole Closure
MH closure occurs most often within 7 days after the surgery.2 Based on OCT criteria, Kang et al categorized MH closure into two types. Type 1 closure was when the MH closed without a foveal neurosensory retinal defect. Type 2 closure was with a foveal neurosensory retinal defect (bare RPE). The results showed that type I closure was strongly associated with better postoperative visual acuity as more residual neurosensory retina indicates a better outcome. In contrast, type 2 closure was associated with MH recurrence, which indicates an unsuccessful repair.64 According to the IVTS, closure of small- and medium-size MHs has a high probability of anatomical success after vitrectomy. The primary anatomical closure rate has been reported at 90–95% with ILM peeling and around 75% without ILM peeling. Large, chronic or persistent MHs and those complicated with retinal detachment (RD) remain a challenge for vitreoretinal surgeons.5
It should be noted that visual acuity outcomes are not always satisfactory even with anatomical success. Michalewska et al found that a foveal photoreceptor defect and the thickness of the outer retinal layer are highly specific predictors of the postoperative BCVA.39 OCT imaging shows that the ellipsoid zone represents one of the aspects of photoreceptor integrity. Chang et al emphasized that the postoperative BCVA was correlated with a restored external limiting membrane and ellipsoid zone line.65 Oh et al reported that a poor postoperative BCVA correlated with a postoperative large-diameter ellipsoid zone defect (p=0.010).66 Thus, the factors that influence BCVA depend on foveal photoreceptors and may not correlate with anatomical closure.
Application of Novel Concepts in Challenging Cases
Large Macular Hole
MH with a diameter of 400 µm or greater has unsatisfactory surgical outcomes, even with the ILM peeling.14,67 Ch’ng et al reported an application of ILM peeling and gas tamponade in the large MH repair, and the study claimed more than 90% success for MH between 400 and 649 µm but only 76% for those between 650 and 1416 µm. This study concluded that the standard MH surgical repair gained very high success rate of up to 650 µm.68 Various techniques in combination with ILM peelings such as ILM flaps or retinal expansion techniques have been reported to improve the success rates.
The inverted ILM flap technique, which was proposed by Michalewska et al,20 ideally leaves a piece of ILM that attaches to the edge of the MH and then inverts to cover the MH. Gu et al reported a systematic review of inverted ILM flap techniques for large MHs. The results clearly supported the use of inverted ILM flap techniques as an effective procedure for large MHs, which provides an anatomical closure rate of up to 95% and significantly improved the BCVA in 75%.69 Studied in large MH, Rizzo et al reported 78.6% success of the standard ILM peeling technique compared to 95.6% of the ILM flap technique.70 Moreover, the ILM flap technique also improved the outcomes in large and myopic MH. The inverted flap technique had a higher success rate of 88.4% in the myopic subgroup compared to 38.9% of the standard ILM peeling.70
In 2015, Michalewska, again, developed a modified (temporal) inverted ILM flap technique that inverted only the temporal side to cover the large MH. The aim was to minimize trauma to the ILM caused by the peeling. The results showed successful MH closure in 93% of 44 eyes, which was not different from the closure rate with the original inverted ILM flap.38
Another inverted ILM flap-related technique is a folded inverted ILM flap which was proposed by Andrew et al. The technique was that applying the viscoelastic cap helped maintain the ILM flap on the MH. The 24 eyes that underwent this technique have shown anatomical improvement with a 100% closure rate and improved BCVA.40
Recently, Ghassemi F et al compared the 3 different techniques of inverted ILM flap dealing with large MHs, 24 eyes with hemicircular ILM peel with temporally hinged inverted flap, 23 eyes with circular ILM peel with temporally hinged inverted flap and 25 eyes with circular ILM peel with superior inverted flap. The closure rate is as high as 87.5–100% in inverted flap techniques and not statistically significant in 3 different techniques (P=0.115). All eyes improved in BCVA.71
Other surgical concepts such as tapping the hole edges and temporal macular arcuate retinotomy have also been used in large MHs; however, the results are less satisfactory compared to those with ILM-related techniques. Table 2 summarizes the reported techniques and outcomes of large MHs.38–40,51,52,56,63,68,70-72
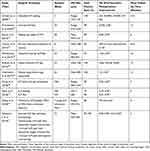 |
Table 2 Reported Techniques and Outcomes in Large Macular Holes |
Persistent/Recurrent Macular Hole
Failure of primary MH surgery or persistent MH is the most common complication of MH repairing, accounting for 10–12%.73 Besides an inadequate tamponade and poor compliance to face down position, the failure of primary surgery is thought to be related with the persistence of vitreomacular traction, either from an inadequate removal of the ILM during prior surgeries or a regeneration of the ERM.28 Repeating the vitrectomy, enlargement of the peeled ILM area, autologous serum usage, and their combinations have shown to increase the closure rate.73–76
Information from OCT imaging indicated that chronic MH often has a square-edged shape, resulting in underlying RPE adhesions. Felfeli et al presented an MH hydrodissection technique. The technique involves injecting fluid into the hole to break the adhesion, thus, allowing the hole edge to become less stiff and easy to close. Their group reported the outcomes of this technique in MH stages 3 and 4 that were either persistent or chronic or large. The complete closure was achieved in 87.2%. The vision improved 94.9% and 79.5% gain of vision ≥ 2 lines.53
Many modified techniques to release the tractional force such as radial retinal incision, induction of macular detachment techniques, and other ILM-manipulated techniques, such as ILM insertion and ILM-free flap, in conjunction with utilizing autologous adhesive substances seem to have the promising closure rate in persistent MH.42,54,77 Moreover, techniques aiming to promote glial cell proliferation have been shown to improve the surgical outcomes.78,79 Table 3 summarizes the reported techniques and outcomes of persistent/recurrent MHs.42–44,48,49,53,54,73-77 The schematic diagram of resuming choice of surgical methods for idiopathic macular hole: perspective, Figure 2.
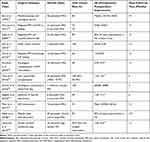 |
Table 3 Reported Techniques and Outcomes in Persistent/Recurrent Macular Holes |
Ocular Changes Following Macular Hole Surgery
Morphological Changes of Macular Hole Eyes Treated Surgically
The MH closure is due to the proliferation of glial cells and sealed holes. Glial cell proliferation occurred on the fourth day after the gas tamponade, and the hole had been closed on the seventh day by the glial tissue.80 OCT is a useful tool to evaluate the healing process of foveal defects in MH surgery. Caprani et al have described the restoration of outer retinal layers and its relevant visual acuity after MH surgery using SD-OCT morphological imaging. The study showed that half of the patients had an inner segment/outer segment junction (IS-OS) band on OCT image at 3 months after surgery, and 91% of patients who underwent surgery showed progressive re-compositing of the inner segment/outer segment layer at the 6th month of follow-up, which was related to an improvement in the BCVA. The IS-OS band and cone outer segment tips (COST) line on OCT images in the early postoperative period may reflect the structural and functional recovery of photoreceptors in MH surgery. However, not all patients in this study showed a correspondence between anatomical and functional success. Some patients in this study showed hyperreflective lesions instead of the re-compositing of outer retina structures and low recovery of the BCVA.81 ILM peeling evidentially improved the anatomical closure rate of MH, but the peeling itself is reported to cause mechanical trauma. Several studies reported retinal microhemorrhages and the appearance of dark striae on autofluorescence imaging in areas of peeling that corresponded with nerve fiber layer swelling. Such swelling disappears within 1 month following by the formation of small dimples and irregularity of the retinal nerve fiber layer (RNFL). The dimples of RNFL, detected by OCT, are called the dissociated optic nerve fiber layer (DONFL). Visual acuity is the same with or without the DONEL. Anatomical defect dimples are asymptomatic paracentral scotomas,82–84 Kim et al studied the correlation of the foveal avascular zone (FAZ) and the postoperative visual acuity in eyes with MH using OCT angiography. Their study showed that the MH eyes with surgery had a smaller FAZ in both the superficial and deep capillary plexi than their fellow eyes. Also, small FAZs correlated better with the postoperative BCVA, especially FAZs in a deep capillary plexus. The association may be explained by the fact that eyes with a smaller FAZ may have more neural tissues in the MH, leading to better central visual function.85 Although Teng et al observed a choriocapillary circulation in idiopathic MH eyes and MH eyes that underwent surgery, their results showed that idiopathic MH eyes have a smaller choriocapillary flow area and lower parafoveal vessel density than their fellow eyes and healthy eyes. After vitrectomy, choriocapillary flow area and density dramatically increase, but there is no significant correlation with visual acuity.86
Conclusions
A majority of idiopathic MH classifications are based on macular size and OCT characteristics, both of which determine long-term visual outcomes and closure rates. Spontaneous MH closure is presented in small MH, initial observation can be used in clinical practice. For simple idiopathic MHs like primary small-medium-sized MH, PPV to remove surface tension over the holes in combination with short-acting gas tamponade are usually sufficient to achieve successful outcomes, with more than 90% success rate and satisfied improving visual recovery. In a more challenging condition like large-sized MHs, ILM flap technology should be considered to increase the closure rate. With the current advances in modified surgical techniques and advances in microsurgical instruments have allowed improving outcomes. Managements of recurrent or persistent MHs are more complicated. Several surgical techniques have been proposed to improve the success rate of this complex entity, however there is not enough evidence from which to draw a firm conclusion regarding the best surgical option.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Johnson RN, Gass JD. Idiopathic macular holes. Observations, stages of formation, and implications for surgical intervention. Ophthalmology. 1988;95(7):917–924. doi:10.1016/S0161-6420(88)33075-7
2. Ezra E. Idiopathic full thickness macular hole: natural history and pathogenesis. Br J Ophthalmol. 2001;85(1):102–108. doi:10.1136/bjo.85.1.102
3. Azzolini C. Macular hole: from diagnosis to therapy. J Ophthalmol. 2020;2020:1473763. doi:10.1155/2020/1473763
4. Tornambe PE. Macular hole genesis: the hydration theory. Retina. 2003;23(3):421–424. doi:10.1097/00006982-200306000-00028
5. Duker JS, Kaiser PK, Binder S, et al. The International Vitreomacular Traction Study Group classification of vitreomacular adhesion, traction, and macular hole. Ophthalmology. 2013;120(12):2611–2619. doi:10.1016/j.ophtha.2013.07.042
6. Ali FS, Stein JD, Blachley TS, Ackley S, Stewart JM. Incidence of and risk factors for developing idiopathic macular hole among a diverse group of patients throughout the United States. JAMA Ophthalmol. 2017;135(4):299–305. doi:10.1001/jamaophthalmol.2016.5870
7. Rahmani B, Tielsch JM, Katz J, et al. The cause-specific prevalence of visual impairment in an urban population. The Baltimore Eye Survey. Ophthalmology. 1996;103(11):1721–1726. doi:10.1016/S0161-6420(96)30435-1
8. McCannel CA, Ensminger JL, Diehl NN, Hodge DN. Population-based incidence of macular holes. Ophthalmology. 2009;116(7):1366–1369. doi:10.1016/j.ophtha.2009.01.052
9. Sen P, Bhargava A, Vijaya L, George R. Prevalence of idiopathic macular hole in adult rural and urban south Indian population. Clin Experiment Ophthalmol. 2008;36(3):257–260. doi:10.1111/j.1442-9071.2008.01715.x
10. Stalmans P, Benz MS, Gandorfer A, et al. Enzymatic vitreolysis with ocriplasmin for vitreomacular traction and macular holes. N Engl J Med. 2012;367(7):606–615. doi:10.1056/NEJMoa1110823
11. Yu Y, Liang X, Wang Z, Wang J, Liu W. Clinical and morphological comparisons of idiopathic macular holes between stage 3 and stage 4. Graefes Arch Clin Exp Ophthalmol. 2018;256(12):2327–2333. doi:10.1007/s00417-018-4158-7
12. Ezra E, Gregor ZJ. Surgery for idiopathic full-thickness macular hole: two-year results of a randomized clinical trial comparing natural history, vitrectomy, and vitrectomy plus autologous serum: Morfields Macular Hole Study Group Report no. 1. Arch Ophthalmol. 2004;122(2):224–236. doi:10.1001/archopht.122.2.224
13. Kelly NE, Wendel RT. Vitreous surgery for idiopathic macular holes. Results of a pilot study. Arch Ophthalmol. 1991;109(5):654–659. doi:10.1001/archopht.1991.01080050068031
14. Freeman WR, Azen SP, Kim JW, El-Haig W, Mishell DR
15. Cheng L, Azen SP, El-Bradey MH, et al. Effects of preoperative and postoperative epiretinal membranes on macular hole closure and visual restoration. Ophthalmology. 2002;109(8):1514–1520. doi:10.1016/S0161-6420(02)01093-X
16. Parravano M, Giansanti F, Eandi CM, Yap YC, Rizzo S, Virgili G. Vitrectomy for idiopathic macular hole. Cochrane Database Syst Rev. 2015;5:Cd009080.
17. Abbey AM, Van Laere L, Shah AR, Hassan TS. Recurrent macular holes in the era of small-gauge vitrectomy: a review of incidence, risk factors, and Outcomes. Retina. 2017;37(5):921–924. doi:10.1097/IAE.0000000000001252
18. Park SS, Marcus DM, Duker JS, et al. Posterior segment complications after vitrectomy for macular hole. Ophthalmology. 1995;102(5):775–781. doi:10.1016/S0161-6420(95)30956-6
19. Krishnan R, Tossounis C, Fung Yang Y. 20-gauge and 23-gauge phacovitrectomy for idiopathic macular holes: comparison of complications and long-term outcomes. Eye. 2013;27(1):72–77. doi:10.1038/eye.2012.227
20. Kim SS, Smiddy WE, Feuer WJ, Shi W. Outcomes of sulfur hexafluoride (SF6) versus perfluoropropane (C3F8) gas tamponade for macular hole surgery. Retina. 2008;28(10):1408–1415. doi:10.1097/IAE.0b013e3181885009
21. Briand S, Chalifoux E, Tourville E, et al. Prospective randomized trial: outcomes of SF(6) versus C(3)F(8) in macular hole surgery. Can J Ophthalmol. 2015;50(2):95–100. doi:10.1016/j.jcjo.2014.12.006
22. Hasegawa Y, Hata Y, Mochizuki Y, et al. Equivalent tamponade by room air as compared with SF(6) after macular hole surgery. Graefes Arch Clin Exp Ophthalmol. 2009;247(11):1455–1459. doi:10.1007/s00417-009-1120-8
23. Sano M, Inoue M, Itoh Y, et al. Duration of prone positioning after macular hole surgery determined by swept-source optical coherence tomography. Retina. 2017;37(8):1483–1491. doi:10.1097/IAE.0000000000001394
24. Yamashita T, Sakamoto T, Yamashita T, et al. Individualized, spectral domain-optical coherence tomography-guided facedown posturing after macular hole surgery: minimizing treatment burden and maximizing outcome. Retina. 2014;34(7):1367–1375. doi:10.1097/IAE.0000000000000087
25. Zhang Y, Chen X, Hong L, et al. Facedown positioning after vitrectomy will not facilitate macular hole closure based on swept-source optical coherence tomography imaging in gas-filled eyes: a Prospective, Randomized Comparative Interventional Study. Retina. 2019;39(12):2353–2359.
26. Solebo AL, Lange CA, Bunce C, Bainbridge JW. Face-down positioning or posturing after macular hole surgery. Cochrane Database Syst Rev. 2011;12:Cd008228.
27. Pasu S, Bell L, Zenasni Z, et al. Facedown positioning following surgery for large full-thickness macular hole: a multicenter randomized clinical trial. JAMA Ophthalmol. 2020;138(7):725. doi:10.1001/jamaophthalmol.2020.0987
28. Eckardt C, Eckardt U, Groos S, Luciano L, Reale E. Removal of the internal limiting membrane in macular holes. Clinical and morphological findings. Ophthalmologe. 1997;94(8):545–551. doi:10.1007/s003470050156
29. Lois N, Burr J, Norrie J, et al. Internal limiting membrane peeling versus no peeling for idiopathic full-thickness macular hole: a pragmatic randomized controlled trial. Invest Ophthalmol Vis Sci. 2011;52(3):1586–1592. doi:10.1167/iovs.10-6287
30. Spiteri Cornish K, Lois N, Scott N, et al. Vitrectomy with internal limiting membrane (ILM) peeling versus vitrectomy with no peeling for idiopathic full-thickness macular hole (FTMH). Cochrane Database Syst Rev. 2013;6:Cd009306.
31. Spiteri Cornish K, Lois N, Scott NW, et al. Vitrectomy with internal limiting membrane peeling versus no peeling for idiopathic full-thickness macular hole. Ophthalmology. 2014;121(3):649–655. doi:10.1016/j.ophtha.2013.10.020
32. Murphy DC, Fostier W, Rees J, Steel DH. Foveal sparing internal limiting membrane peeling for idiopathic macular holes: effects on anatomical restoration of the fovea and visual function. Retina. 2019. doi:10.1097/IAE.0000000000002724
33. Engelbrecht NE, Freeman J, Sternberg P
34. Enaida H, Hisatomi T, Hata Y, et al. Brilliant blue G selectively stains the internal limiting membrane/brilliant blue G-assisted membrane peeling. Retina. 2006;26(6):631–636. doi:10.1097/01.iae.0000236469.71443.aa
35. Lesnik Oberstein SY, de Smet MD. Use of heavy trypan blue in macular hole surgery. Eye. 2010;24(7):1177–1181. doi:10.1038/eye.2010.3
36. Shukla D, Kalliath J, Neelakantan N, Naresh KB, Ramasamy K. A comparison of brilliant blue G, trypan blue, and indocyanine green dyes to assist internal limiting membrane peeling during macular hole surgery. Retina. 2011;31(10):2021–2025. doi:10.1097/IAE.0b013e318213618c
37. Hu Z, Lin H, Liang Q, Wu R. Comparing the inverted internal limiting membrane flap with autologous blood technique to internal limiting membrane insertion for the repair of refractory macular hole Int Ophthalmol. 2020;40(1):141–149.
38. Michalewska Z, Michalewski J, Dulczewska-Cichecka K, Adelman RA, Nawrocki J. Temporal inverted internal limiting membrane flap technique versus classic inverted internal limiting membrane flap technique: a comparative Study. Retina. 2015;35(9):1844–1850. doi:10.1097/IAE.0000000000000555
39. Michalewska Z, Michalewski J, Adelman RA, Nawrocki J. Inverted internal limiting membrane flap technique for large macular holes. Ophthalmology. 2010;117(10):2018–2025. doi:10.1016/j.ophtha.2010.02.011
40. Andrew N, Chan WO, Tan M, Ebneter A, Gilhotra JS. Modification of the inverted internal limiting membrane flap technique for the treatment of chronic and large macular holes. Retina. 2016;36(4):834–837. doi:10.1097/IAE.0000000000000931
41. Xu Q, Luan J. Internal limiting membrane flap technique in macular hole surgery. Int J Ophthalmol. 2020;13(5):822–831. doi:10.18240/ijo.2020.05.19
42. Morizane Y, Shiraga F, Kimura S, et al. Autologous transplantation of the internal limiting membrane for refractory macular holes. Am J Ophthalmol. 2014;157(4):861–9.e1. doi:10.1016/j.ajo.2013.12.028
43. Pires J, Nadal J, Gomes NL. Internal limiting membrane translocation for refractory macular holes. Br J Ophthalmol. 2017;101(3):377–382. doi:10.1136/bjophthalmol-2015-308299
44. Chen SN, Yang CM. Lens capsular flap transplantation in the management of refractory macular hole from multiple etiologies. Retina. 2016;36(1):163–170. doi:10.1097/IAE.0000000000000674
45. Ohno-Matsui K, Ichinose S, Nakahama K, et al. The effects of amniotic membrane on retinal pigment epithelial cell differentiation. Mol Vis. 2005;11:1–10.
46. Zhu D, Jin X, Zhou J. Transplantation of amniotic membrane for choroidal hole to treat suprachoroidal silicone oil migration. Acta Ophthalmol. 2017;95(6):e522–e3. doi:10.1111/aos.13516
47. Rizzo S, Caporossi T, Tartaro R, et al. A human amniotic membrane plug to promote retinal breaks repair and recurrent macular hole closure. Retina. 2019;39(Suppl 1):S95–S103. doi:10.1097/IAE.0000000000002320
48. Caporossi T, Pacini B, De Angelis L, Barca F, Peiretti E, Rizzo S. Human amniotic membrane to close recurrent, high myopic macular holes in pathologic myopia with axial length of >/=30 mm. Retina. 2019. doi:10.1097/IAE.0000000000002699
49. Grewal DS, Mahmoud TH. Autologous neurosensory retinal free flap for closure of refractory myopic macular holes. JAMA Ophthalmol. 2016;134(2):229–230. doi:10.1001/jamaophthalmol.2015.5237
50. Kusuhara S, Teraoka Escano MF, Fujii S, et al. Prediction of postoperative visual outcome based on hole configuration by optical coherence tomography in eyes with idiopathic macular holes. Am J Ophthalmol. 2004;138(5):709–716. doi:10.1016/j.ajo.2004.04.063
51. Kumar A, Tinwala SI, Gogia V, Sehra SV. Tapping of macular hole edges: the outcomes of a novel technique for large macular holes. Asia Pac J Ophthalmol (Phila). 2013;2(5):305–309. doi:10.1097/APO.0b013e31829a1919
52. Charles S, Randolph JC, Neekhra A, Salisbury CD, Littlejohn N, Calzada JI. Arcuate retinotomy for the repair of large macular holes. Ophthalmic Surg Lasers Imaging Retina. 2013;44(1):69–72. doi:10.3928/23258160-20121221-15
53. Felfeli T, Mandelcorn ED. Macular hole hydrodissection: surgical technique for the treatment of persistent, chronic, and large macular holes. Retina. 2019;39(4):743–752.
54. Szigiato AA, Gilani F, Walsh MK, Mandelcorn ED, Muni RH. Induction of macular detachment for the treatment of persistent or recurrent idiopathic macular holes. Retina. 2016;36(9):1694–1698. doi:10.1097/IAE.0000000000000977
55. Choukroun J, Diss A, Simonpieri A, et al. Platelet-rich fibrin (PRF): a second-generation platelet concentrate. Part IV: clinical effects on tissue healing. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2006;101(3):e56–e60. doi:10.1016/j.tripleo.2005.07.011
56. Chakrabarti M, Benjamin P, Chakrabarti K, Chakrabarti A. Closing macular holes with “macular plug” without gas tamponade and postoperative posturing. Retina. 2017;37(3):451–459. doi:10.1097/IAE.0000000000001206
57. Paques M, Chastang C, Mathis A, et al. Effect of autologous platelet concentrate in surgery for idiopathic macular hole: results of a multicenter, double-masked, randomized trial. Platelets in Macular Hole Surgery Group. Ophthalmology. 1999;106(5):932–938. doi:10.1016/S0161-6420(99)00512-6
58. Olsen TW, Sternberg P
59. Liggett PE, Skolik DS, Horio B, Saito Y, Alfaro V, Mieler W. Human autologous serum for the treatment of full-thickness macular holes. A preliminary study. Ophthalmology. 1995;102(7):1071–1076. doi:10.1016/S0161-6420(95)30909-8
60. Cho HY, Kim YT, Kang SW. Laser photocoagulation as adjuvant therapy to surgery for large macular holes. Korean J Ophthalmol. 2006;20(2):93–98. doi:10.3341/kjo.2006.20.2.93
61. Ikuno Y, Kamei M, Saito Y, Ohji M, Tano Y. Photocoagulation and fluid-gas exchange to treat persistent macular holes after prior vitrectomy. A Pilot Study. Ophthalmology. 1998;105(8):1411–1418.
62. Nuzzi R, Tridico F. Perspectives of autologous mesenchymal stem-cell transplantation in macular hole surgery: a review of current findings. J Ophthalmol. 2019;2019:3162478. doi:10.1155/2019/3162478
63. Zhang X, Liu J, Yu B, Ma F, Ren X, Li X. Effects of mesenchymal stem cells and their exosomes on the healing of large and refractory macular holes. Graefes Arch Clin Exp Ophthalmol. 2018. doi:10.1007/s00417-018-4097-3
64. Kang SW. Types of macular hole closure and their clinical implications. Br J Ophthalmol. 2003;87(8):1015–1019. doi:10.1136/bjo.87.8.1015
65. Chang YC, Lin WN, Chen KJ, et al. Correlation between the dynamic postoperative visual outcome and the restoration of foveal microstructures after macular hole surgery. Am J Ophthalmol. 2015;160(1):100–6.e1. doi:10.1016/j.ajo.2015.03.019
66. Oh J, Smiddy WE, Flynn HW
67. Gupta B, Laidlaw DA, Williamson TH, Shah SP, Wong R, Wren S. Predicting visual success in macular hole surgery. Br J Ophthalmol. 2009;93(11):1488–1491. doi:10.1136/bjo.2008.153189
68. Ch’ng SW, Patton N, Ahmed M, et al. The Manchester Large Macular Hole Study: is it time to reclassify large macular holes? Am J Ophthalmol. 2018;195:36–42. doi:10.1016/j.ajo.2018.07.027
69. Gu C, Qiu Q. Inverted internal limiting membrane flap technique for large macular holes: a systematic review and single-arm meta-analysis. Graefes Arch Clin Exp Ophthalmol. 2018;256(6):1041–1049.
70. Rizzo S, Tartaro R, Barca F, Caporossi T, Bacherini D, Giansanti F. Internal limiting membrane peeling versus inverted flap technique for treatment of full-thickness macular holes: a comparative study in a large series of patients. Retina. 2018;38(Suppl 1):S73–s8. doi:10.1097/IAE.0000000000001985
71. Ghassemi F, Khojasteh H, Khodabande A, et al. Comparison of three different techniques of inverted internal limiting membrane flap in treatment of large idiopathic full-thickness macular hole. Clin Ophthalmol. 2019;13:2599–2606. doi:10.2147/OPTH.S236169
72. Al Sabti K, Kumar N, Azad RV. Extended internal limiting membrane peeling in the management of unusually large macular holes. Ophthalmic Surg Lasers Imaging. 2009;40(2):185–187. doi:10.3928/15428877-20090301-03
73. D’Souza MJ, Chaudhary V, Devenyi R, Kertes PJ, Lam WC. Re-operation of idiopathic full-thickness macular holes after initial surgery with internal limiting membrane peel. Br J Ophthalmol. 2011;95(11):1564–1567. doi:10.1136/bjo.2010.195826
74. Che X, He F, Lu L, et al. Evaluation of secondary surgery to enlarge the peeling of the internal limiting membrane following the failed surgery of idiopathic macular holes. Exp Ther Med. 2014;7(3):742–746. doi:10.3892/etm.2014.1477
75. Ezra E. Membranectomy and autologous serum for the retreatment of full-thickness macular holes. Arch Ophthalmol. 1997;115(10):1276–1280. doi:10.1001/archopht.1997.01100160446010
76. Rizzo S, Genovesi-Ebert F, Vento A, Cresti F, Miniaci S, Romagnoli MC. Heavy silicone oil (Densiron-68) for the treatment of persistent macular holes: densiron-68 endotamponade for persistent macular holes. Graefes Arch Clin Exp Ophthalmol. 2009;247(11):1471–1476. doi:10.1007/s00417-009-1131-5
77. Reis R, Ferreira N, Meireles A. Management of stage IV macular holes: when standard surgery fails. Case Rep Ophthalmol. 2012;3(2):240–250. doi:10.1159/000342007
78. Lai CC, Chen YP, Wang NK, et al. Vitrectomy with internal limiting membrane repositioning and autologous blood for macular hole retinal detachment in highly myopic eyes. Ophthalmology. 2015;122(9):1889–1898. doi:10.1016/j.ophtha.2015.05.040
79. Chen S-N, Yang C-M. Inverted internal limiting membrane insertion for macular hole–associated retinal detachment in high myopia. Am J Ophthalmol. 2016;162(99–106.e1). doi:10.1016/j.ajo.2015.11.013
80. Yamana T, Kita M, Ozaki S, Negi A, Honda Y. The process of closure of experimental retinal holes in rabbit eyes. Graefes Arch Clin Exp Ophthalmol. 2000;238(1):81–87. doi:10.1007/s004170050014
81. Caprani SM, Donati S, Bartalena L, et al. Macular hole surgery: the healing process of outer retinal layers to visual acuity recovery. Eur J Ophthalmol. 2017;27(2):235–239. doi:10.5301/ejo.5000905
82. Mitamura Y, Suzuki T, Kinoshita T, Miyano N, Tashimo A, Ohtsuka K. Optical coherence tomographic findings of dissociated optic nerve fiber layer appearance. Am J Ophthalmol. 2004;137(6):1155–1156. doi:10.1016/j.ajo.2004.01.052
83. Ito Y, Terasaki H, Takahashi A, Yamakoshi T, Kondo M, Nakamura M. Dissociated optic nerve fiber layer appearance after internal limiting membrane peeling for idiopathic macular holes. Ophthalmology. 2005;112(8):1415–1420. doi:10.1016/j.ophtha.2005.02.023
84. Steel DH, Dinah C, Habib M, White K. ILM peeling technique influences the degree of a dissociated optic nerve fibre layer appearance after macular hole surgery. Graefes Arch Clin Exp Ophthalmol. 2015;253(5):691–698. doi:10.1007/s00417-014-2734-z
85. Kim YJ, Jo J, Lee JY, Yoon YH, Kim JG. Macular capillary plexuses after macular hole surgery: an optical coherence tomography angiography study. Br J Ophthalmol. 2018;102(7):966–970. doi:10.1136/bjophthalmol-2017-311132
86. Teng Y, Yu M, Wang Y, Liu X, You Q, Liu W. OCT angiography quantifying choriocapillary circulation in idiopathic macular hole before and after surgery. Graefes Arch Clin Exp Ophthalmol. 2017;255(5):893–902. doi:10.1007/s00417-017-3586-0
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

