Back to Journals » Journal of Healthcare Leadership » Volume 16
Leading Quality and Safety on the Frontline – A Case Study of Department Leaders in Nursing Homes
Authors Magerøy MR , Braut GS, Macrae C, Clay-Williams R, Braithwaite J, Wiig S
Received 9 December 2023
Accepted for publication 30 March 2024
Published 23 April 2024 Volume 2024:16 Pages 193—208
DOI https://doi.org/10.2147/JHL.S454109
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Professor Zhanming Liang
Malin Rosell Magerøy,1 Geir Sverre Braut,2,3 Carl Macrae,1,4 Robyn Clay-Williams,5 Jeffrey Braithwaite,5 Siri Wiig1
1SHARE- Centre for Resilience in Healthcare, Faculty of Health Science, University of Stavanger, Stavanger, Norway; 2Department of Research, Stavanger University Hospital, Stavanger, Norway; 3Department of Social Science, Western Norway University of Applied Sciences, Sogndal, Norway; 4Centre for Health, Innovation, Leadership and Learning, Nottingham University Business School, Nottingham, UK; 5Australian Institute of Health Innovation. Faculty of Medicine, Health and Human Sciences, Macquarie University, Sydney, New South Wales, Australia
Correspondence: Malin Rosell Magerøy, SHARE- Centre for Resilience in Healthcare, Faculty of Health Science, University of Stavanger, Stavanger, Norway, Tel +47 47385445, Email [email protected]
Purpose: The role of healthcare leaders is becoming increasingly complex, and carries great responsibility for patients, employees, and the quality of service delivery. This study explored the barriers and enablers that department leaders in nursing homes encounter when managing the dual responsibilities in Health, Safety and Environment (HSE) and Quality and Patient Safety (QPS).
Methodology: Case study design with data collected through semi structured interviews with 16 department leaders in five Norwegian municipalities. We analyzed the data using qualitative content analysis.
Results: Data analysis resulted in four themes explaining what department leaders in nursing homes experience as barriers and enablers when handling the dual responsibility of HSE and QPS: Temporal capacity: The importance of having enough time to create a health-promoting work environment that ensures patient safety. Relational capacity: Relationships have an impact on work process and outcomes. Professional competence: Competence affects patient safety and leadership strategies. Organizational structure: Organizational frameworks influence how the dual responsibilities are handled.
Conclusion: Evidence from this study showed that external contextual factors (eg, legislations and finances) and internal factors (eg, relationships and expectations) are experienced as barriers and enablers when department leaders are enacting the dual responsibility of HSE and QPS. Of these, relationships were found to be the most significant contributor.
Keywords: leadership, patient safety, quality, human factors, staff safety
Introduction
Healthcare leaders have an important role in managing and handling the dual responsibilities of Health, Safety and Environment (HSE) and Quality and Patient Safety (QPS). HSE regulation ensures health, safety, and welfare of employees, while QPS includes patient safety, quality of service delivery, clinical effectiveness, and patient experience.1–3 In Norway, different legislations regulate the responsibilities of HSE and QPS,4–6 but research and practical experience show that it is necessary to understand HSE and QPS in a holistic way, as they can affect each other and generate conflicts of interests.1,7–10 Factors, such as organizational, cultural, and psychosocial conditions have a role in QPS and HSE, but there is no clear understanding of leaders` perspectives, and the strategies they enact, regarding this duality.1,7,11 Leadership competence and efficiency are associated with challenges regarding QPS.3,12 Leadership in healthcare can influence employee- and patient outcomes, and different leadership approaches and styles can produce variation in outcomes.13–15 Leadership can have significant effect on patient safety culture and work engagement, and hierarchic leadership levels and organizational factors can affect leadership approaches and outcome for HSE and QPS.14,16,17 This study seeks to explore department leaders` roles across their dual responsibilities for HSE and QPS. Department leaders have the same position as frontline leaders in the organization, and a frontline leader is defined as a member of the organizations leadership team with direct supervisory responsibility over employees who deliver the organization`s services.18
There are several theoretical approaches to understand leadership in healthcare,14,19 and the Leader-Member-Exchange (LMX) theory is one of them.20 LMX theory is a relationship-based, dyadic theory of leadership that suggests that leaders develop different and unique relationships with each of their employees, and that quality of leader-member relationships moves on a continuum from low to high.20–22 In low quality relationships the exchange is limited to the employment contract, while high quality relationships are based on mutual liking, respect, and influence. LMX theory suggests that leaders can develop high-quality relationships with employees that are related to positive outcomes such as higher organizational commitment, job satisfaction, empowerment, social support and lower role conflict, and thus affect safety culture for both patients and staff.20,23,24
The System Engineering Initiative for Patient Safety (SEIPS) model can be used as a framework when exploring the dual leadership responsibility for HSE and QPS. The SEIPS model of work systems and patient safety focuses on system design, and its impact on process and outcome.25 There are five components to a work system within the SEIPS model: person, task, tool/instrument, physical environment, organizational conditions.25,26 The components interact with and influence each other, which could result in different outcomes related to patients, staff, and organization. Patient outcomes include patient safety or quality of care, while organizational or staff outcomes emphasize employee health and safety, job satisfaction, job stress, burnout, and turnover.25,26 The SEIPS model shows how all parts of an organization can affect and depend on each other and illustrates how changes in one part of the organization can influence the outcome in another.
The current knowledge base on leadership and QPS has been growing in hospital settings over the last two decades, but there is a need to increase the knowledge base about nursing homes and homecare services.2,27,28 Research on understanding of leaders` practical handling of the dual responsibility of QPS and HSE in this context is particularly lacking. This knowledge gap is addressed in the current study. By applying the SEIPS model and LMX theory for mapping and understanding how leaders in nursing homes perform their responsibility for both patients and staff, the study contributes to reducing the knowledge gap on how front-line leaders handle the dual responsibility of HSE and QPS in their everyday work.
The Norwegian Healthcare Context
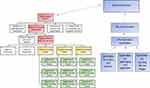
The responsibility for healthcare in Norway is divided between regional health authorities and the municipalities. Municipalities are responsible for nursing homes, home care, doctor on call schemes and general practitioners (GP), and are regulated by the Act on Municipalities and County Municipality.29 Nursing homes in Norway are financed by the municipality, through political grants, and by resident copayment. The chairmanship model is the most common for organization of Norwegian municipalities (see Figure 1). In this model the political committees have overall control and management of the municipality. The municipal council is the highest political authority and makes decisions on behalf of the municipality, and according to the chairmanship model leaders in healthcare follow the political decisions regarding priorities and financial allotments. Systematic work targeting QPS improvements is a leadership responsibility at all levels and is regulated in legislation: the Regulations on management and quality improvements in the health and care service, the Health and Care Services Act and also anchored in the National action plan for patient safety and quality improvement.6,30,31 To ensure employee health and safety, HSE work is articulated in Regulations on systematic health, environment and safety work in companies and The working environment act.4,6
Aim and Research Questions
The aim of this study was to explore the barriers and enablers that department leaders in nursing homes encounter when managing the dual responsibility of HSE and QPS. The following research questions guided the study:
- What do frontline leaders experience as the enablers and barriers in managing the dual responsibility of HSE and QPS?
- How do frontline leaders experience and manage the practical consequences of, and interactions between HSE and QPS?
Material and Methods
Design
This study is a part of a single embedded case study, conducted in accordance with Yin`s description of case study research.32 A case study is a method that investigates a contemporary phenomenon in-depth in a real-world context, and the approach is suitable when seeking to understand a complex social phenomenon.32 The case for this study is defined as the two perspectives of safety: HSE and QPS in a Norwegian nursing home context, and how they are organized, controlled, and followed up, and the possible tensions between them from a leadership perspective. The main study consists of three levels of the healthcare system, which includes: politicians and top-level leaders in health and care services in the municipalities (municipal director, director of health and welfare, and head of health and care service), head of nursing homes (mid-level leaders), and department leaders in nursing homes (frontline leaders). This study explored department leaders experiences in five Norwegian municipalities (see Figure 1).
Sample and Recruitment
The municipalities were recruited through recommendations from the Norwegian Association of Local and Regional Authorities, of which all Norwegian municipalities and county councils are members. The recommended municipalities were contacted with an invitation to participate in this study, together with an attached information letter. The municipalities were purposively selected to provide a diverse sample based on size and location (urban/rural). When the municipalities agreed to participate, and the included nursing homes were selected, the heads of these nursing homes recruited the participating department leaders (see Table 1 for the characteristics of the participating municipalities).
 |
Table 1 Characteristics of Municipalities and Data Collection |
Data Collection
We conducted individual-semi structured interviews with 16 department leaders (n =16) in 14 nursing homes. The participants had different levels of leadership experience and leadership education, varying from being newly employed without a leader background and formal leader training, to being experienced and with some form of leadership training, either internal courses or education at university level. Most participants in this study had 5–10 years of leadership experience, and extensive practice in the healthcare system. All interviews were conducted physically in the respective nursing homes from March to June 2022. The interviews were conducted by the first author and were based on an interview guide. We used the SEIPS model and LMX- theory as a framework when the research questions and interview guide were formulated, and in the discussion of the results,20,25 and topics were related to what department leaders in nursing homes experience as barriers and enablers when managing the dual responsibility of HSE and QPS, how they experience the practical consequences of sick leave, and the available system and support they had (or needed) to manage the dual responsibility. Each interview lasted approximately one hour. All interviews were audio recorded and transcribed verbatim by the first author.
Data Analysis
The data was uploaded into NVivo and analyzed according to Graneheim and Lundman`s33 approach to qualitative content analysis. The unit of analysis (the transcribed interviews) was divided into meaning units, condensed, coded, and sorted into subcategories, categories, and themes.33,34 See Tables 2 and 3 for examples of the analysis process for theme 2. The lead researcher was responsible for the analysis with input from the research team who read transcripts and discussed development of codes, subcategories, categories, and themes throughout the analysis period. We used NVivo to analyze the lower levels (extracting meaning units, coding, and creating subcategories), while the higher abstraction levels (categories and themes) were analyzed manually. During the analysis process potential themes emerged, and the lead researcher constructed a mind map to understand underlying meanings (latent content). The analysis was discussed in meetings between the researchers and finally agreed upon by all authors.
 |
Table 2 Examples of the Content Analysis Process Theme 2. Relational Capacity |
 |
Table 3 Examples of Content Analysis theme 2. Relational Capacity |
Results
The higher abstract levels of analyses resulted in nine categories, that were poled into four common themes. All categories fit into the four themes on the various enablers and barriers experienced by department leaders when managing the work with HSE and QPS. Developing of the themes were discussed and agreed upon by all authors. The themes were: temporal capacity, relational capacity, professional competence, and organizational structure. Themes are presented in detail, alongside illustrative citations from the participants in the following text.
T1: Temporal Capacity
For all leaders, having enough time was essential to build a health-promoting environment that cared for the employees and ensured QPS. Having time to be a leader, time to organize good care quality, and time to follow up sick leave were reported to be factors of greatest importance.
“Time. It is all about time. We get more and more tasks, and that means that we must lower priority on other things. Both HSE and QPS are important, but when you don’t have time to focus on these things, the quality won’t be good. In many situations you cannot handling HSE or QPS without affecting the other, and that is challenging”. (leader, municipality 2)
Operational pressures: The leaders described a busy working day with many tasks, lack of time and resources, as well as the need to always be available. For many participants, the distinction between work and personal leisure had disappeared. They described a feeling of never doing enough, feeling guilty for not having enough time for their employees, and not being able to exercise leadership the way they wanted; all could adversely affect HSE and QPS, leaders said. They experienced great pressure and explained that being a frontline leader is hard work, implying always considering everyone’s interests, and often fielding complaints from employees, patients, higher leadership levels and other stakeholders. The leaders had a genuine desire for creating a good working environment and safe nursing homes with high quality care for the patients. To achieve this, leaders saw the need to be present at the ward, attend handover reports between shifts and always keep their office door open. Employees at nursing homes work shifts, and the leaders found it challenging to be present for those who only worked nightshifts. Everyday life could make it challenging to handle requirements connected to HSE and QPS and daily operations took much of the time that could otherwise be used to follow up employees and engage in development work. Basic staffing was too low to deliver services of desired quality level, leaders said, and they therefore focused on how to lower the standard to “good enough” and “acceptable”. They were rethinking the standard of the care and accepted that if patients had their primary needs met and received the necessary medical care, it would have to be good enough.
“We had to change from showering the patients once a week to every 14th day. We thought that this would save us a lot of time and have the least impact on quality”. (leader, municipality 1)
Comprehensive responsibility: The dual responsibility of HSE and QPS was a familiar concept for the leaders. All participants knew they were responsible for both HSE and QPS, but experienced it as an enormous undertaking, and not everyone had an overview over what they were responsible for. Leaders experienced the dual responsibility as a dilemma, having different laws regulating HSE and QPS, constantly making priorities and assessing what was more important. Political decisions and expectations from society made it challenging for the leaders to enact their responsibilities. Having tight finances that made them unable to keep to their budgets was demotivating and stressful, and leaders recognized that there were not enough resources and time to look after both staff and patients in a satisfactory manner. Even if there were conflicting interests, leaders were clear that HSE and QPS should be integrated and handled holistically.
“When we talk about the dual responsibility, there are various pieces of legislation that regulate patient safety and HSE. In addition, you have politicians who make decisions, and then it is me as the leader who must handle all these requirements. We also have an economy that is not sufficient and a budget that we are unable to keep…., yes, that’s the way it is. At the same time, it is connected and would be difficult to separate. There is something about having responsibility for both parts to be able to see the bigger picture….”. (leader, municipality 2)
What was perceived as most challenging, was balancing the employees` entitlement to a safe working environment with restrictions against use of coercion when patients were acting out. Weighing patients` and next of kin wishes of not using aids versus protecting employees against strain injuries was also a frequently reported problem. Having a dual responsibility with conflicting interests was an everyday challenge and a huge responsibility. Several leaders described this situation as stressful, with constant frustration for both patients and staff, who felt bad about not having the mandate, competence, and time to solve these issues in a satisfactory manner. Several leaders reported considering leaving their roles and exiting the sector as they experienced the gap between resources and demands as unbridgeable, and the challenges of constantly having to prioritize between competing needs as so challenging it adversely affected their health.
“This is why I have resigned and found another job. I get very stressed because I am not able to look after the employees working environment the way I want, and the way I have learned that I should. I have thought about this a lot…. this is not good for my health, it has made me sick”. (leader, municipality 5)
None of the participants had direction from their superiors on how to prioritize in the event of conflicting interests, and when asked, participants were divided in their answers. They experienced having to assess it on a case-by-case basis. All recipients were unanimous that work environment and quality of service delivery were connected. If the employees felt safe, being part of a good competent team and were empowered, they would perform better and provide care of higher quality. They also saw a clear connection between work environment and sick leave, and leaders experienced that great work pressure, physical and psychological stress injuries and poor workplace culture were the cause of high sickness absence of staff in nursing homes.
T2: Relational Capacity
Relationships between the participants and superiors, colleagues, employees, patients, next of kin, and other stakeholders were crucial for work process and outcome for patients and staff.
Interaction: According to participants, being a frontline leader in nursing homes demands collaboration. Interactions with healthcare institutions such as hospitals and municipalities within the county were necessary and important to deliver good quality care. The small municipalities, especially, benefited from collaboration in meeting the requirements from authorities to handle HSE and QPS, and leaders experienced that having good relationships improved collaboration. According to the participants, patients in nursing homes are more demanding now and in need of more advanced care compared to only a few years ago.
“When patients come to us, relatives have had them at home for a long time and are often tired and despondent. They often have a bad conscience for leaving their spouse in a nursing home, and they take their frustrations out on us. We are being criticized for the clothes we have put on the patient, questioned why they are not eating enough…. There is a lot of despair here”. (Leader, municipality 2)
Department leaders depended on collaboration with other department leaders when solving complex and demanding issues regarding HSE and QPS. However, for leaders in small municipalities this was not always an option as they often worked alone. Leaders in small municipalities had to establish relationships with leaders in other areas of expertise such as schools, social services, or in neighboring municipalities. Having a team of colleagues to lean on was felt to be a great support for the frontline leaders, and they highlighted the importance of having a good relationship with their superior. Having their superior`s support when decisions were made, understanding the dilemmas they were facing, and their everyday work life was important and made challenges easier to handle, participants reported.
Relationships between participants and the employees were crucial when tasks became demanding. Good relations could buffer stress, frustration, and conflicts, and leaders also recognized that employees were willing to work more and perform better if they had a fundamentally good relationship based on mutual respect and trust. If the relationships were good, it was easier for employees to be open, have a good dialogue and be honest about their limitations and any health issues that affected their ability to work. Finding good solutions for both parties would be more likely, leaders said. The leaders also acknowledged that relationships also could have a negative effect, especially related to sick leave follow-up and opportunities for adapted work tasks.
“I must be honest and say that the relationships are important. Employees who have repeated absences and call in sick before the work weekend….then I must honestly say that I struggle….It is frustrating, and I feel irritated because it affects the other employees and the patients. I know that I must focus on being a good leader in these cases…it is easier to reach out for someone who’s always present and performing, than those who takes advantage of the system”. (leader, municipality 1)
Engagement: Having engaged employees who were proud of the care they provided and their workplace, was important to create good relations with other stakeholders. Having variety and diversity in the workforce was perceived as a strength but could also lead to challenges, according to the leaders. Nursing homes are traditionally a female-dominated workplace, but some of the nursing homes in this study had male care personnel. Leaders saw this as a strength, since men added another dimension to the work environment, male patients, and relatives. Ethnicity and cultural background were important issues in relation to QPS and HSE for the leaders in this study. They appreciated diversity and the broader interpretation this could bring, but it also created challenges, especially related to language. Language barriers made communication challenging, and the leaders feared that it could affect QPS. Familiarity with the Norwegian culture and religion, especially during the holidays was an advantage and contributed to create good relations with patients and next of kin. Cultural traditions, relationships and time were used to explain the frequency of reporting adverse events. Leaders focused on the importance of reporting, so that it could be used in the improvement work, but they experienced that employees dreaded reporting adverse events as it was perceived to be unpleasant and could destroy relationships with colleagues.
T3: Professional Competence
Competence: Competence of leaders and employees was a core factor when leaders elaborated on what kind of factors that influenced working on HSE and QPS. All leaders had received mandatory HSE- courses when first employed, but they recognized the need for more education to keep updated. The need for competence and qualifications had increased over the years and the leaders highlighted the connection between healthcare workers competence and QPS. Recruiting qualified personnel was challenging for all participants, and in the small municipalities it had become noticeably more difficult in recent years. Leaders experienced that the media contributed to maintaining the recruitment challenges by referring to the working conditions of healthcare personnel in a negative way.
“It has become more difficult to recruit. There are fewer and fewer residents in the municipality, so there is less recruitment potential. We see it in the number of applicants for summer jobs…we have always had many students as summer workers, but now there is barely enough to manage…. I also don’t think the media is helping to turn elderly care or the nursing profession into something positive. It is difficult”. (leader, municipality 4)
The results showed a hierarchy within elderly care and nursing homes, where working in short-term wards and rehabilitation had the highest status, while dementia wards had the lowest rank and was therefore least desirable. According to the participants, educational institutions highlight hospitals as the best learning arena where students and newly graduated nurses could develop the most.
Recipients of the health care service: Patients in nursing homes are a diverse group, but they all have a great need for care, and the disease(s) are often complex and advanced. All leaders saw an increase in the need of care in recent years and described it as a dramatic change. Due to the severity of their disease, the patients were considered more demanding, particularly related to cognitive and mental disorders. Some patients were seen as a risk for staff, and healthcare workers needed to have expertise in the risk factors in their work environment, and how to handle them. Results showed examples of employees fearing patients, doubting their competence and ability to resist the strain over time. Especially patients with an aggressive behavior were demanding for the staff. Increasing competence, training for situations, and focusing on debrief was some of the important measures for employees to manage the situations. Being present as a leader and supporting the employees was prioritized for the participants.
“Many employees are a bit afraid to go to work, due to some unpredictable patients with an aggressive behavior….we probably must reorganize, maybe create a group of employees who feel safe working this way and let them have the main responsibility for these patients”. (leader, municipality 4)
Quality and safety in service delivery: Leaders in this study were concerned with QPS but believed that they delivered high quality services despite the challenges in resources and competence. QPS is aspects of work they would try not to compromise, and they argued that routines, dedicated employees, organization of work tasks, welfare technology, and available aids were factors that influenced the QPS outcome. The concept of quality was considered in different ways by the leaders, but they all described quality as a subjective experience that could be difficult to measure. Quality was linked to the standard of care provision, the work environment for staff and patient safety. Although measuring could be difficult, leaders experienced it as important to have some sort of standards to compare themselves with.
“When I think of quality, I think of how we collaborate, how we develop, how we practice our profession in relation to patients and relatives, and how we reflect together. For me, quality means delivering services that are not only at a minimum, but services that you can be proud of”. (leader, municipality 1)
Patient safety was easier to conceptualize, as the participants agreed that it was about keeping patients safe, prevent injuries, and have good systems and routines when errors occurs so that they were able to detect, response, and prevent adverse events. Leaders were constantly focusing on improving QPS by building competence amongst staff. Leaders encouraged employees to report deviations and were concerned that everyone should be competent in what to report, knowing the reporting system, and knowing that deviations were hand according to routines. According to the leaders, getting these reports is the only way to improve our work, change routines, and getting an overview of where the errors occur. Medication errors, patients acting out, and falls were the areas with most error reports. Problems in the working environment were rarely reported. To meet future needs and demands, nursing home leaders acknowledged that they had to be willing to change the way they organized their staff, developed competence, and solved tasks. Leaders of short-term departments experienced their personnel to be used to handle rapid changes, thus were more robust in relation to new challenges. Economics played an important role in what opportunities the leaders had to meet present and future needs. Hiring substitutes, sending employees to courses to maintain and develop competence, providing qualified care, and plan for future needs were not included in their current budget, and leaders experienced that the decision makers did not understand the challenges.
“We are under cost-saving measures all the time. That means I can’t employ more people, while at the same time the complexity of the tasks increases. I don’t have the money to hire substitutes, so in the event of sick leave we must manage without. To save money and not hiring substitutes, I have often worked at the ward myself, but then I am not able to do my original tasks. The only thing I am measured on and must report upwards in the system is finances, and that I am able to keep the budget”. (leader, municipality 5)
T4: Organizational Structure
Structure: To manage the dual responsibility of HSE and QPS, leaders pointed out the need for understanding systems, knowing the regulations, having experienced colleagues to discuss with, and a supportive leader. All nursing homes in this study used Complio as their quality system, and leaders were satisfied with the opportunities this system provided. Complio is an electronic system where documents are stored. It is used to save regulations, guidelines, and procedures, and for reporting deviations, such as adverse events. Some of the nursing homes had systems for reporting deviations up the management line and reviewed them weekly, while others had more spontaneous ways of working. The latter particularly applied to the small municipalities. All leaders highlighted the importance of support from the Human Resources (HR) department and being part of a leadership team. Documentation and thorough handovers between healthcare organizations and shifts were crucial to maintain QPS. Leaders acknowledged that it was challenging to secure information in an institution where staff worked shifts, often in part-time positions, and where language barriers among employees were common. To effectively utilize resources and reduce the number of handovers and substitutes, all nursing homes were looking at how the rotation schemes were organized and position sizes for the personnel. Increasing job sizes was a priority for all, as they believed that would solve some of the challenges related to having enough qualified personnel, buffering for sick leave, and fewer handovers. One way of organizing this was by introducing long shifts.
“We have introduced long shifts; 3-5 days at work for 14 hours per shift, followed by a longer period off. The department benefits from having the same person working both dayshift and evening-shift, the quality will be better then. When we introduced long shifts, it resulted in us only having qualified staff at work, and we have the same staffing whether it is Sunday or Monday, day, or evening. I can’t remember the last time I only had qualified staff at work. Now there are fewer errors, and the employees have a sense of ownership in their work. Both patients and next of kin are extremely satisfied”. (leader, municipality 1)
Introducing technology to monitor patient welfare could improve both HSE and QPS, participants said. By using individually adapted sensors where you can enter specific data, eg, how far from the bed the patient can walk, how long they can stay in the bathroom etc. before the alarm goes off, leaders experienced they could prevent several patient injuries and increase patient safety. They presumed that welfare technology was a good aid for the employees, giving them better overview and control.
Organization: The size of the municipality influenced how work with HSE and QPS was organized. Leaders who had been working in both large and small municipalities, described the work process as more cumbersome in large municipalities, involving more levels and decision makers. Size and number of patients and employees varied in the various nursing homes and departments in this study, from those with a single leader to those where the leader was part of a leadership team. How staff were organized also varied but, to meet future needs, several had reorganized and used staff working across departments and tasks.
“We are organized differently to other nursing homes in the municipality. We have nurses as a separate team, not belonging to de various departments, and it is the assistant nurses who run the departments. This is a pilot project initiated from higher management level as an attempt to use the right skills in the right place. In addition, an effect of this organization will be that it contributes to higher competence among assistant nurses, and the nurses are freed to do tasks only for which they are certified”. (leader, municipality 2)
The nursing homes in this study had different systems for, and ways of organizing, HSE and QPS. Some nursing homes had plans and procedures that applied to all departments, while others made plans by department without common guidelines. Some of the leaders had full control over the plans that were available and knew what was expected of them, while others were not aware of what plans and guidelines they had. Deviations and safety inspections were described as regular tasks by all leaders in this study, and they experienced these as important for safety and improvement work. Covid-19 was offered as a common reason why HSE and QPS work had not been updated or conducted according to plan.
Discussion
This study examined how department leaders in nursing homes manage the dual responsibility of HSE and QPS, and what they experienced as barriers and enablers in this task. Time, relationships, competence, and organizational structure were identified as the four themes that affect experience and outcome for HSE and QPS, and our findings show the complexity in this work (see Figure 2).
 |
Figure 2 The four themes of how department leaders in nursing homes manage the dual responsibility of HSE and QPS, the barriers and enablers, using a human factors perspective. |
Human factors, and the SEIPS model, refer to environmental, organizational and job factors, and human and individual characteristics, which influence behavior at work in a way that can affect health and safety. Using this perspective when analyzing the challenges of the dual responsibility of HSE and QPS provides a system orientation to understanding the work system, processes, and outcomes by enacting leadership roles in a nursing home context.35–37 The LMX-theory provides an enriched, relational understanding of leaders` actions, attitudes, and opportunities when handling dilemmas linked to the dual responsibility of HSE and QPS.20,38,39 This is discussed in what follows along with documentation on the future implications for research and practice.
Time and Competence
Participants in this study were unanimous that they experienced discrepancy between the resources they had available and the expectations and demands they had to meet. Resources were defined as time, sufficient and qualified staffing, and a budget that made it possible to run the department effectively. Legislations, finances, and expectations from stakeholders caused continuous trade-offs for leaders in this study when handling the dual responsibility of HSE and QPS. Employees` statutory rights to a safe working environment was often in conflict with legislation preventing use of coercion. When patients acted out, leaders experienced this to be demanding when handling the dual responsibility of HSE and QPS.4,31,40,41 The Efficiency-Thoroughness-Trade-Off principle (ETTO) posits that leaders are making constant adjustments between demands and resources that affect efficiency and thoroughness, and an imbalance could lead to errors and adverse events.42 Achieving an ETTO- balance is an essential leadership responsibility when maintaining QPS and HSE.43,44 Leaders in this study described their role as demanding, since they had to comply with instructions and decisions from mid-level leaders, top-level leaders, and politicians while at the same time translating the needs of employees, patients and next of kin into sustainable, high quality healthcare45 (See Figure 3). This is also in line with other models describing how systems affect safety and is a dynamic process.46
 |
Figure 3 Frontline leaders position in the municipalities, with responsibilities, considerations and influencing factors in a human factors perspective. |
Leadership is about coping with change,47 and our study showed that the ability to change is essential to deliver good quality care and maintain health and safety for both patients and staff. It is a leadership responsibility to ensure that the organization is adapted to the environment,19,47 and reform processes in the Norwegian healthcare system have resulted in frequent reorganizations. Together with future challenges and expectations this requires constant adaptations and commitment from the department leaders in nursing homes. To motivate and inspire change, leaders aim to be agile and flexible, with a propensity to adjust to pressure, events and circumstances,47,48 which requires competence and time. Training in HSE is mandatory for leaders in Norway, while there are no legal requirements for competence in QPS,4 and leaders in our study experienced it as challenging to separate HSE and QPS as they often influenced each other. In our study competence and time were seen as facilitators, and lack of them was perceived as a barrier when handling the dual responsibility of HSE and QPS. Healthcare leaders are often professionals who have taken on a leadership role, sometimes with limited leadership qualifications,16,48–50 In our study, all participants had a health-related bachelor’s degree, and extended experience from clinical practice, but varying degrees of managerial expertise and education. Having a clinical background provided them with a unique position as they know their area well, can translate decision-makers` strategy into everyday life and act as sense-givers to the staff.45,48,51 Local expertise can provide a broader understanding of barriers and facilitators in the work system.35 In our study the department leaders possessed local expertise on the opportunities and challenges in their department, whereas decisions from policymakers and nursing home leaders often applied to all nursing homes or all departments in the specific nursing home regardless of local needs and resources. This explains how organizational factors within the department, and external factors such as political decisions, legislation, and the economic situation in the municipality and nursing home have consequences for the work system (department), and the people performing the tasks (department leader).52–54 Handling frequent changes to meet future challenges and needs in healthcare, such as changed disease patterns, aging populations, technological advancements, and political reforms, places great demands on healthcare organizations and professionals’ capacity to implement change.55,56 This requires leaders to be present, to be qualified, and to allocate time to translate political and managerial decisions into sensemaking and sensegiving activities.47,48 In this study, leaders found that being a good and present leader sometimes involved trade-offs to manage the daily tasks and challenges. This indicates that department leaders in nursing homes must have the local expertise and know the appropriate trade-offs to balance tensions and manage QPS and HSE. There is a need for future studies investigating the role of local expertise when frontline leaders maneuver in a landscape of conflicting demands, needs and resources. There is also a need to investigate the difference in mandatory courses where the Norwegian legislation requires HSE training and the QPS legislation does not.
Relations and Organizational Structure
Leadership is associated with HSE and QPS outcome,13,15 and LMX theory suggests that leaders can develop high-quality relationships with employees and thus affect safety culture.20,24 LMX views the dyadic relationship quality as the key to understanding how leadership affects members, teams, and organizations. It assumes that leaders influence their employees through the quality of the relationships they develop with them.21,22 Leaders in our study clearly stated that relations had a significant impact on their work with HSE and QPS and they tried to establish good relations and effective collaboration with all stakeholders. Leaders indicated that having positive relationships with patients and relatives, where information was shared, improved QPS. This concurs with Nilsen et al (2019), who found it is important to support work on positive patient/provider relationship to maintain high quality and safety for both patients and staff.55 The LMX theory assumes that the dyadic relationship between leader and employee develops continuously over time, and that development is affected by the leader’s delegation of tasks and the employee’s performance.38,39,57 In this study leaders acknowledged that the relations they had with the employees affected not only the work environment, but also the opportunities for arranged work tasks and sick leave follow up. The participants strived to treat all employees equally and fairly but experienced that that was not always possible Previous research pinpoints that leadership should be individualized and supportive in order to encourage development, resolve conflicts, buffer stress and strengthen staff and patient safety.7 Low quality relationships may lead to more work-related stress and less social support from the leader which in turn can lead to burnout. Burnout is associated with lower patient satisfaction and reduced health outcomes and could thus affect both HSE and QPS.7,58 This shows how relationships can have an impact on both work systems (organization) and individuals (leaders and employees) and thus affect the process and outcomes of HSE and QPS. Our study indicates that relations are an additional and crucial process component when using a human systems approach such as the SEIPS model.35,37
Frequent changes influence employees` health and well-being, and poorly implemented and communicated change processes can cause workforce stress and uncertainty, and thus affect HSE and consequently reduce QPS.9,55 Successful change-processes are a leadership responsibility, and in healthcare, sensemaking-sensegiving is a challenging task due to constant adjustments and the need for quick decisions based on the current situation.47,48 The healthcare system in Norway is constantly reorganizing to meet demands with available resources, and leaders in this study experienced not having enough time to facilitate good change processes, and that they traded off facilitating and implementing changes thoroughly to maintain daily activities. Sensemaking processes are essential to understand employees` responses to change and trading them off could therefore affect HSE and QPS outcome.55,59 Moreover, studies indicate that relations between employees and frontline leaders have an important role in employees` participation in patient safety efforts, and there is a positive association of high quality relationships between leaders and employees in reporting-structure and culture.60 In our study, reporting deviations and adverse events was important to the leaders, and they focused on improving the reporting culture. Few deviations were reported regarding the working environment, and the leaders assumed this to be grounded in relations. They experienced that employees would not readily reveal each other’s mistakes, but when employees` had a good relationship with their leaders, they would be more likely to report more sensitive incidents. This demonstrates how relations influence improvement work, and thus the outcome for HSE and QPS. According to Hofmann et al (2003), frontline leaders, and the safety climates they create in their work group, can have significant impacts on the safety performance of their staff,61 Consequently, leaders should strive to create good relationships with their employees, so that all aspects of safety are maintained. This is in line with LMX theory. This study shows that the SEIPS model can be used to understand how individual behavior affected by relations in the work system can affect the process, and thus the outcome for HSE and QPS. Changing the way of thinking, from safety silos that see patient safety and employee safety as separate entities, to an integrated whole, would provide a more holistic view of HSE and QPS.9,35–37,58
Conclusion
This study shows that both external contextual factors (eg, legislations and finances) and internal factors (eg, relations and expectations) influence what department leaders in nursing homes experience as barriers and enablers when handling the dual responsibility of HSE and QPS. The department leaders acknowledge that time, relationships, competence, and organizational structure influence their experience when enacting their responsibility for both versions of safety. This study indicates that relationships are important for leaders to maintain QPS and HSE. Adding the process of relations to the human factors SEIPS model (see Figure 2), has potential to improve our understanding of how the safety silos can be integrated and give a more holistic view of HSE and QPS.
Strengths and Limitations
This study is the first to explore department leaders in nursing homes experiences of the dual responsibility of HSE and QPS. The strength of this study is that it contributes new insight regarding enablers and barriers when handling this duality. The enablers and barriers explored here are not exhaustive, but they provide an insight that may be transferrable to other similar contexts.32 The study has some limitations. The participating department leaders were recruited by head of nursing homes, with some risk of selection bias or unintended potential experience of pressure to participate in the study. This was mitigated by information letters to all informants prior to the interview, and by the interviewer elaborating on the possibility to withdraw at any time and that the participation was voluntary and withdrawing would have no negative consequences. When using a semi structured interview guide, it is possible that participants may be prompted to answer in a certain way.62 To minimize that risk, we informed participants that we were interested in their experiences, and that no answer was right or wrong. This study consisted of 16 participants, and having a higher sample of department leaders and municipalities could have provided other elements to the results.
Abbreviations
HSE, Health, Safety and Environment; QPS, Quality and Patient Safety; SEIPS, Systems Engineering Initiative for Patient Safety; LMX, Leader-Member-Exchange.
Data Sharing Statement
The data material is available on request from the corresponding author.
Acknowledgments
The authors wish to thank all participants for sharing their valuable knowledge and experience.
Ethics Approval and Informed Consent
All methods were carried out in accordance with relevant guidelines and regulations. Ethical approval and all protocols were approved through Sikt- Norwegian Agency for Shared Services in Education and Research (formerly known as the Norwegian Centre for Research Data (NSD)) ref. nr: 886397. Sikt provides the ethics approval, information security and privacy services, as part of the HK-dir (Norwegian Directorate for Higher Education and Skills). The study followed the Helsinki Declaration. All participants gave their written informed consent included publication of anonymized responses before participating in the study. They were informed that participation was voluntary and that they could withdraw from the study at any time. The authors confirm that all methods were performed in accordance with regulations and guidelines.
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
This project is funded by the University of Stavanger.
Disclosure
CM acts as the National Professional Advisor for Patient Safety at the Care Quality Commission, England. The authors declare no other conflicts of interests in this work.
References
1. Ose SO, Busch HJ. HMS i offentlig sektor: Forebygging av sykefravær og tidlig avgang fra arbeidslivet [HSE in the public sector: prevention of sickness absence and early departure from working life].
2. Aase I, Ree E, Johannessen T, et al. Talking about quality: how ‘quality’ is conceptualized in nursing homes and homecare. BMC Health Serv Res. 2021;21(1):104. doi:10.1186/s12913-021-06104-0
3. Doyle C, Lennox L, Bell D. A systematic review of evidence on the links between patient experience and clinical safety and effectiveness. BMJ Open. 2013;3(1):e001570. doi:10.1136/bmjopen-2012-001570
4. Ministry of Labor and Inclusion. Lov om arbeidsmiljø arbeidstid og stillingsvern m.v [Act relating to the working environment, working hours and employment protection, etc]; 2005. Available from: https://lovdata.no/dokument/NL/lov/2005-06-17-62.
5. Forskrift om systematisk helse. miljø- og sikkerhetsarbeid i virksomheter [Regulations relating to Systematic Health, Environment and Safety Activities in Enterprises]; 1996. Available from: https://lovdata.no/forskrift/1996-12-06-1127).
6. Ministry of Health and Welfare. Forskrift om ledelse og kvalitetsforbedring i helse- og omsorgstjenesten [Regulations on management and quality improvement in the health and care service]; 2017. Available from: https://lovdata.no/dokument/SF/forskrift/2016-10-28-1250.
7. Eklof M, Torner M, Pousette A. Organizational and social-psychological conditions in healthcare and their importance for patient and staff safety. A critical incident study among doctors and nurses. Safety Science. 2014;70:211–221. doi:10.1016/j.ssci.2014.06.007
8. Magerøy MR, Braut GS, Macrae C, Wiig S. Healthcare leaders’ and elected politicians’ approach to support-systems and requirements for complying with quality and safety regulation in nursing homes – a case study. BMC Health Serv Res. 2023;23(1):1–880. doi:10.1186/s12913-023-09906-6
9. Jones A, Neal A, Bailey S, Cooper A. When work harms: how better understanding of avoidable employee harm can improve employee safety, patient safety and healthcare quality. BMJ Leader. 2023. doi:10.1136/leader-2023-000849
10. Magerøy MR, Macrae C, Braut GS, Wiig S. Managing patient safety and staff safety in nursing homes: exploring how leaders of nursing homes negotiate their dual responsibilities-a case study. Front Health Serv. 2024;4:1275743. doi:10.3389/frhs.2024.1275743
11. Aase K, Høyland S, Olsen E, Wiig S, Nilsen ST. Patient safety challenges in a case study hospital – of relevance for transfusion processes? Transfus Apher Sci. 2008;39(2):167–172. doi:10.1016/j.transci.2008.06.003
12. Wiig S, Ree E, Johannessen T, et al. Improving quality and safety in nursing homes and home care: the study protocol of a mixed-methods research design to implement a leadership intervention. BMJ Open. 2018;8(3):e020933–e020933. doi:10.1136/bmjopen-2017-020933
13. Sfantou DF, Laliotis A, Patelarou AE, Sifaki-Pistolla D, Matalliotakis M, Patelarou E. Importance of leadership style towards quality of care measures in healthcare settings: a systematic review. Healthcare. 2017;5(4):73. doi:10.3390/healthcare5040073
14. Ree E, Wiig S. Linking transformational leadership, patient safety culture and work engagement in home care services. Nurs Open. 2020;7(1):256–264. doi:10.1002/nop2.386
15. Ree E, Wiig S. Employees’ perceptions of patient safety culture in Norwegian nursing homes and home care services. BMC Health Serv Res. 2019;19(1):607. doi:10.1186/s12913-019-4456-8
16. Birken S, Clary A, Tabriz AA, et al. Middle managers’ role in implementing evidence-based practices in healthcare: a systematic review. Implement Sci. 2018;13(1):149. doi:10.1186/s13012-018-0843-5
17. Furunes T. Leadership in Healthcare. In: Løvseth LT, dLA H, editors. Integrating the Organization of Health Services, Worker Wellbeing and Quality of Care. Springer; 2020:135–157.
18. Longenecker CO, Longenecker PD. Why hospital improvement efforts fail: a view from the front line. J Healthc Manag. 2014;59(2):147–157. doi:10.1097/00115514-201403000-00010
19. Hennestad BW, Revang Ø. Endringsledelse og ledelsesendring: Fra plan til praksis [Change management and management change: from plan to practice].
20. Graen GB, Uhl-Bien M. Relationship-based approach to leadership: development of leader-member exchange (LMX) theory of leadership over 25 years: applying a multi-level multi-domain perspective. Leadersh Q. 1995;6(2):219–247. doi:10.3389/frhs.2024.1275743
21. Erdogan B, Bauer TN. Leader–member exchange theory. In: Wright JD, editor. International Encyclopedia of the Social & Behavioral Sciences.
22. Bauer TN, Erdogan B. Leader-member exchange (LMX) theory: An introduction and overview. In: Bauer TN, Erdogan B, editors. The Oxford Handbook of Leader-Member Exchange. Oxford University Press; 2015:3–9.
23. Furunes T, Mykletun RJ, Einarsen S, Glasø L. Do low-quality leader-member relationships matter for subordinates? Evidence from three samples on the validity of the Norwegian LMX scale. Nordic j Working Life Stud. 2015;5(2):71. doi:10.19154/njwls.v5i2.4794
24. Trinchero E, Farr-Wharton B, Brunetto Y. A social exchange perspective for achieving safety culture in healthcare organizations. Int j Public Sec Manag. 2019;32(2):142–156. doi:10.1108/IJPSM-06-2017-0168
25. Carayon P, Schoofs Hundt A, Karsh BT, et al. Work system design for patient safety: the SEIPS model. Qual Saf Health Care. 2006;15(suppl 1):i50–i58. doi:10.1136/qshc.2005.015842
26. Carayon P, Wooldridge A, Hoonakker P, Hundt AS, Kelly MM. SEIPS 3.0: Human-centered design of the patient journey for patient safety. Appl Ergon. 2020;84:103033. doi:10.1016/j.apergo.2019.103033
27. Parand A, Dopson S, Renz A, Vincent C. The role of hospital managers in quality and patient safety: a systematic review. BMJ Open. 2014;4(9):e005055–e005055. doi:10.1136/bmjopen-2014-005055
28. Wiig S, Aase K, von Plessen C, et al. Talking about quality: exploring how ‘quality’ is conceptualized in European hospitals and healthcare systems. BMC Health Serv Res. 2014;14(1):478. doi:10.1186/1472-6963-14-478
29. Ministry of Local Government and Districts. Lov om kommuner og fylkeskommuner [Act relating to municipalities and county authorities (The Local Government Act)]; 2018. Available from: https://lovdata.no/dokument/NL/lov/2018-06-22-83.
30. Helsedirektoratet. Nasjonal handlingsplan for pasientsikkerhet og kvalitetsforbedring 2019-2023 [National action plan for patient safety and quality improvement]; 2019. Available from: https://www.helsedirektoratet.no/veiledere/ledelse-og-kvalitetsforbedring-i-helse-og-omsorgstjenesten/Nasjonal%20handlingsplan%20for%20pasientsikkerhet%20og%20kvalitetsforbedring%202019-2023.pdf/_/attachment/inline/79c83e08-c6ef-4adc-a29a-4de1fc1fc0ef:94a7c49bf505dd36d59d9bf3de16769bad6c32d5/Nasjonal%20handlingsplan%20for%20pasientsikkerhet%20og%20kvalitetsforbedring%202019-2023.pdf.
31. Ministry of Health and Welfare. Lov om kommunale helse- og omsorgstjenester m.m [Act relating to municipal health and care services etc]; 2011. Available from: https://lovdata.no/dokument/NL/lov/2011-06-24-30.
32. Yin RK. Case Study Research and Applications: Design and Methods.
33. Graneheim UH, Lundman B. Qualitative content analysis in nursing research: concepts, procedures and measures to achieve trustworthiness. Nurse Educ Today. 2004;24(2):105–112. doi:10.1016/j.nedt.2003.10.001
34. Graneheim UH, Lindgren B-M, Lundman B. Methodological challenges in qualitative content analysis: a discussion paper. Nurse Educ Today. 2017;56:29–34. doi:10.1016/j.nedt.2017.06.002
35. Carayon P, Perry S. Human factors and ergonomics systems approach to the COVID-19 healthcare crisis. Oxford. 2021;33:1–3.
36. Dul J, Bruder R, Buckle P, et al. A strategy for human factors/ergonomics: developing the discipline and profession. Ergonomics. 2012;55(4):377–395. doi:10.1080/00140139.2012.661087
37. Carayon P, Wetterneck TB, Rivera-Rodriguez AJ, et al. Human factors systems approach to healthcare quality and patient safety: Systems ergonomics/human factors. Appl Ergon. 2014;45(1):14–25. doi:10.1016/j.apergo.2013.04.023
38. Graen GB. Role making processes within complex organizations. In: Dunnette MD, editor. Handbook in Industrial and Organizational Psychology. Chicago: Rand Mcnally; 1976:1201–1245.
39. Graen GB. Unwritten Rules for Your Career: 15 Secrets for Fast-Track Success. New York: John Wiley; 1989.
40. Ministry of Health and Welfare. Lov om pasient- og brukerrettigheter [Patient and User Rights Act]; 2001. Available from: https://lovdata.no/dokument/NL/lov/1999-07-02-63#:~:text=Pasient%2D%20og%20brukerrettighetsloven%20er%20en,%2C%20transport%2C%20informasjon%20og%20innsyn.
41. Ministry of Health and Welfare. Helsepersonelloven; Lov om helsepersonell m.v [The Health Personnel Act; Act relating to health personnel, etc]; 2001. Available from: https://lovdata.no/dokument/NL/lov/1999-07-02-64.
42. Hollnagel E. The ETTO Principle: Efficiency-Thoroughness Trade-Off: Why Things That Go Right Sometimes Go Wrong.
43. Grant S, Guthrie B. Efficiency and thoroughness trade-offs in high-volume organisational routines: an ethnographic study of prescribing safety in primary care. BMJ Qual Saf. 2018;27(3):199–206. doi:10.1136/bmjqs-2017-006917
44. Glette MK, Wiig S. The role of organizational factors in how efficiency-thoroughness trade-offs potentially affect clinical quality dimensions – a review of the literature. Int J Health Governance. 2021;26:250–265. doi:10.1108/IJHG-12-2020-0134
45. Bradley EH, Taylor LA, Cuellar CJ. Management matters: a leverage point for health systems strengthening in global health. Int J Health Policy Manag. 2015;4(7):411–415. doi:10.15171/ijhpm.2015.101
46. Cook R, Rasmussen J. “Going solid”: a model of system dynamics and consequences for patient safety. Qual Saf Health Care. 2005;14(2):130–134. doi:10.1136/qshc.2003.009530
47. Kotter JP. What Leaders Really Do.
48. Braithwaite J, Churruca K, Hibbert P, Clay-Williams R. At the heart of getting things done in complex healthcare ecosystems: leadership, strategy, sensemaking and sensegiving. In: Chambers N, editor. Research Handbook on Leadership in Healthcare. Edward Elgar Publishing; 2023:775–792.
49. Hartviksen TA, Sjolie BM, Aspfors J, Uhrenfeldt L. Healthcare middle managers’ experiences developing leadership capacity and capability in a public funded learning network. BMC Health Serv Res. 2018;18(1):433. doi:10.1186/s12913-018-3259-7
50. Clay-Williams R, Ludlow K, Testa L, Li Z, Braithwaite J. Medical leadership, a systematic narrative review: do hospitals and healthcare organisations perform better when led by doctors? BMJ Open. 2017;7(9):e014474–e014474. doi:10.1136/bmjopen-2016-014474
51. Grinde E, Nilsen Y, Valebrokk K. Lederne. Balansekunstnerne: Om Lederne og ledelse i 100 år [The managers. The balance artists: about the leaders and management for 100 years]. Dinamo; 2010.
52. Holden RJ, Carayon P, Gurses AP, et al. SEIPS 2.0: a human factors framework for studying and improving the work of healthcare professionals and patients. Ergonomics. 2013;56(11):1669–1686. doi:10.1080/00140139.2013.838643
53. Ree E, Johannessen T, Wiig S. How do contextual factors influence quality and safety work in the Norwegian home care and nursing home settings? A qualitative study about managers’ experiences. BMJ Open. 2019;9(7):e025197–e025197. doi:10.1136/bmjopen-2018-025197
54. Johannessen T, Ree E, Aase I, Bal R, Wiig S. Exploring managers’ response to a quality and safety leadership intervention: findings from a multiple case study in Norwegian nursing homes and homecare services. BMJ Open Quality. 2021;10(3):e001494. doi:10.1136/bmjoq-2021-001494
55. Nilsen P, Schildmeijer K, Ericsson C, Seing I, Birken S. Implementation of change in health care in Sweden: a qualitative study of professionals’ change responses. Implement Sci. 2019;14(1):51. doi:10.1186/s13012-019-0902-6
56. Gadolin C. The logics of healthcare - in quality improvement work; 2017.
57. Ferris GR, Liden RC, Munyon TP, Summers JK, Basik KJ, Buckley MR. Relationships at work: Toward a multidimensional conceptualization of dyadic work relationships. J Manage. 2009;35(6):1379–1403. doi:10.1177/0149206309344741
58. Bodenheimer T, Sinsky C. From triple to quadruple aim: Care of the patient requires care of the provider. Anna Family Med. 2014;12:573–576. doi:10.1370/afm.1713
59. Loretto W, Platt S, Popham F. Workplace change and employee mental health: results from a longitudinal study. British J Manage. 2010;21(2):526–540. doi:10.1111/j.1467-8551.2009.00658.x
60. Jungbauer K-L, Loewenbrück K, Reichmann H, Wendsche J, Wegge J. How does leadership influence incident reporting intention in healthcare? A dual process model of leader–member exchange. German J Human Res Manag. 2018;32(1):27–51. doi:10.1177/2397002217745315
61. Hofmann DA, Morgeson FP, Gerras SJ. Climate as a moderator of the relationship between leader-member exchange and content specific citizenship: safety Climate as an Exemplar. J Appl Psychol. 2003;88(1):170–178. doi:10.1037/0021-9010.88.1.170
62. Hsieh H-F, Shannon SE. Three approaches to qualitative content analysis. Qual Health Res. 2005;15(9):1277–1288. doi:10.1177/1049732305276687
 © 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2024 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.