Back to Journals » Therapeutics and Clinical Risk Management » Volume 16
Lateral Position versus Prone Position for Cervical Laminoplasty: A Retrospective Comparative Study
Authors Du L, Gao Y, Gao K, Yang G, Gao S
Received 12 October 2019
Accepted for publication 6 February 2020
Published 21 February 2020 Volume 2020:16 Pages 133—140
DOI https://doi.org/10.2147/TCRM.S227799
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Deyun Wang
Lin Du, 1, 2 Yanzheng Gao, 1 Kun Gao, 1 Guang Yang, 1 Shanjun Gao 2
1Department of Spine Surgery, Henan Provincial People’s Hospital, People’s Hospital of Zhengzhou University, Zhengzhou City, Henan Province, People’s Republic of China; 2Microbiome Laboratory, Henan Provincial People’s Hospital, People’s Hospital of Zhengzhou University, Zhengzhou City, Henan Province, People’s Republic of China
Correspondence: Yanzheng Gao; Kun Gao
Department of Spine Surgery, Henan Provincial People’s Hospital, People’s Hospital of Zhengzhou University, 7 Weiwu Road, Zhengzhou City, Henan Province 450000, People’s Republic of China
Tel +86 13783505855;
+86 13838372271
Fax +86 0371 65964376
Email [email protected]; [email protected]
Purpose: To examine the safety of lateral decubitus positions for cervical laminoplasty.
Patients and Methods: A retrospective comparative study was conducted on the safety between the lateral and prone positions in cervical laminoplasty. After screening, 466 patients who underwent cervical laminoplasty at a single medical center were enrolled and categorized into the lateral (n=229) and prone (n=237) groups. Data on positioning time, surgical time, blood loss, complication rates, and surgical outcomes were collected and compared between the two groups. The patients were further divided into underweight, normal weight, overweight, and obesity subgroups according to their body mass index, and the collected data were compared between the lateral and prone groups.
Results: The lateral group had a lower incidence of facial pressure ulcers (2.18%) than the prone group (11.39%). However, positioning time, surgical time, blood loss, and surgical outcomes were not significantly different between the two groups. In the subgroup analysis, no significant difference in positioning time, operative time, and blood loss was observed in the underweight, normal weight, and overweight patients between the two groups, but in the obesity subgroup, the lateral group had a significantly shorter positioning time (15.23± 6.44 vs 21.63± 9.43 min, P=0.045) and operative time (140.16± 40.48 vs 178.62± 51.82 min, P=0.037) and lesser blood loss (285.31± 171.75 vs 430.46± 189.84 mL, P=0.044) than the prone group.
Conclusion: The lateral position is as safe as the prone position for cervical laminoplasty, but it has advantages over the prone position for patients with obesity.
Keywords: lateral position, prone position, laminoplasty, cervical myelopathy
Introduction
The position of the patient is important for facilitated access, clear exposure, and ensuring spinal alignment and stability in cervical procedures. In laminoplasty, the choice of surgical position was considered to be dependent on the surgeon’s preference, research regarding this is lacking.1 As a general rule, laminoplasty is performed with the patient in the prone position. Performing posterior cervical surgery in the prone position was established since the very early stage of spinal surgery, and it has continuously improved with the introduction of mattress or frames for head, neck, chest, and belly support and for face protection.2,3 Although the prone position is regarded as a regular position in spinal surgery, some position-related complications, such as facial pressure ulcers and post-operative visual loss, have been reported. In addition, it will be cumbersome to ensure the safety of obese patients, especially those with a pot belly in the prone position.
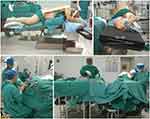
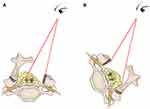
The lateral decubitus position is generally used in spine surgery for transthoracic or thoracoabdominal lateral vertebral column access, although its usage in posterior cervical spine surgery is seldom reported.4–7 In recent years, we have begun to use the lateral position in cervical laminoplasty in our hospital, we found that the lateral position has some advantages over the prone position. The lateral position facilitates surgical field drainage and intraspinal inspection (Figures 1 and 2). In addition, the complex preparatory work to ensure the abdominal hangover of obese patients is simpler in the lateral position than in the prone position.
Although laminoplasty can be performed in either the prone or the lateral position, comparisons of these two positions are lacking in the literature. The purpose of this study was to determine the role and safety of the lateral position for cervical laminoplasty through a retrospective comparison with those of the prone position.
Methods
Patients
Between May 2011 and June 2018, 535 patients underwent cervical laminoplasty for multilevel cervical compression. Laminoplasty was indicated in the treatment of cervical myelopathy due to ossified posterior longitudinal ligament (OPLL) and multilevel cervical spondylosis myelopathy (CSM) involving three or more segments. Only the patients who underwent decompression at levels C3-C6 or C3-C7 and those with a microplate to stabilize the lamina were included in this study (n=497). We excluded patients with impaired cardiorespiratory function (n=10), those receiving treatment with beta-blockers (n=19), and those with coagulation abnormality (n=2). The included patients (n=466) were divided into the lateral decubitus (lateral group, n=229) and prone position (prone group, n=237) groups.
Then, the body mass index (BMI) was calculated based on the patients’ weight and height. The patients were categorized into the underweight (BMI<18.5 kg/m2); normal weight (18.5≤BMI<24.0 kg/m2), overweight (24.0≤BMI<28.0 kg/m2), and obesity (BMI≥28.0 kg/m2) subgroups according to the criteria of weight for adults (Chinese Public Health Standards, No: WS/T 428–2013). In this way, we identified 6 underweight, 175 normal weight, 35 overweight, and 13 obese patients in the lateral group, whereas, in the prone group, there were 8 underweight, 184 normal weight, 30 overweight, and 15 obese patients. The demographic data of the two groups are listed in Table 1. Given that the aim of this study was to review existing practices and owing to the retrospective nature of this study, written consent from the involved patients were not obtained. Patient data confidentiality was maintained, and that this study was conducted in accordance with the Declaration of Helsinki. The study was approved by the Ethics Committee of Henan Provincial People’s Hospital.
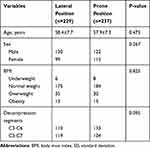 |
Table 1 Baseline Characteristics of the Study Patients |
Patients’ Position
In the prone group, after tracheal intubation was performed, the patient was cautiously turned in the prone position on the operating table with two longitudinal bolsters already in place to ensure free abdominal movements. The horseshoe silica gel head rest was placed under the face with the neck in a neutral position. Forehead and chin were well padded, and the eyes were ensured to have no extrinsic pressure.
In the lateral decubitus position, after endotracheal intubation, the patient was turned in the lateral position and secured with a longitudinal bolster and a position bracket placed ventrally. A small square pillow was placed under the head to maintain the cervical spine alignment, and medical tape was used to fix the head on the operating table. All bony prominences were well padded, and the anterior abdomen was kept hanging free. The operating table is tilted forward by 10–15° to facilitate field inspection and surgical operation (Figure 1). The choice of the right versus left lateral position was based on the side with predominant symptoms. The symptomatic side was selected as the open side of the lamina and the upside of the patient. The surgeon stands behind the patient, while the first assistant stands on the same side of the surgeon.
Data Collection
The medical records were retrospectively analyzed. In the anesthesia note, four time points were recorded, which include the start and end times of the operation and the time of tracheal intubation and extubation. Based on these time points, we defined the positioning time as the period from accomplishment of the tracheal intubation to the start time of the operation. Moreover, the surgical time was defined as the period between the start and end times of the operation as recorded in the anesthesia note. The operation procedure and blood loss were recorded in the surgical record sheet. All of the complications directly related to patient positioning were recorded in the surgical nursing recording sheet, including pressure ulcers, ocular complications, and peripheral nerve paralysis. Given that the recording of these four medical documents is highly patterned and these documents are strictly regulated by laws and regulations, we believe that the data collection in this manner was unbiased and highly reliable.
For the surgical outcome comparison, we followed up 30 patients who were operated in the recent years (referred herein as the latest patients) in both groups via telephone and evaluated them using the Japanese Orthopedic Association (JOA) score and visual analog scale (VAS).8,9 Using the pre-operative JOA and VAS scores documented in the medical records, the recovery rate of the JOA score and axial pain symptom recovery were compared between the two groups.
Statistical Analysis
The IBM SPSS Statistics software package (IBM Corporation, version 22, Chicago, Illinois, USA) was utilized for statistical analyses. All continuous variables were demonstrated as mean ± standard deviation (X±SD) and all categorical variables as frequencies and percentages. For comparisons of continuous variables between groups, we used the independent sample t test, if the assumptions of equal variance and the Gaussian distribution were met. Otherwise, a nonparametric Mann–Whitney test was used. For the comparison of categorical variables, the Fisher’s exact or chi-square test was used as appropriate. P values<0.05 based on a 2-sided hypothesis test were considered significant.
Results
Demographic Results
In this study, 466 patients met the inclusion criteria. The lateral group consisted of 229 patients (130 men, 99 women) with a mean age of 58.4±7.7 years. The prone group comprised 237 patients (122 men, 115 women) with a mean age of 57.9±7.3 years. No statistically significant differences were found in the baseline demographics between the lateral and prone groups in terms of age (P=0.473), sex (P=0.267), BMI (P=0.825), and operative segments (P=0.095) (Table 1).
Direct Comparison
The incidence of facial pressure ulcers was 2.18% (5/229 patients) and 11.39% (27/237 patients) in the lateral and prone groups, respectively, showing significant difference. No other position-related complications, such as ocular complication and peripheral nerve paralysis were found in both groups. There was no significant difference in the positioning time, operative time, blood loss, and incidence of other complications between the two groups (Table 2).
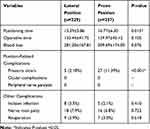 |
Table 2 Direct Comparison of the Characteristics and Surgical Outcomes of the Patients |
Surgical outcomes were compared among the latest 30 patients in both groups. There were no statistically significant differences in the recovery rate of JOA (P=0.103) and VAS scores (P=0.684) between the two groups (Table 3).
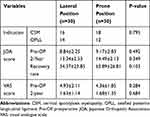 |
Table 3 Surgical Outcomes of the Latest 30 Patients |
Stratified Analysis
The included patients were stratified according to BMI, and further divided into the underweight, normal weight, overweight, and obesity subgroups. For the obesity subgroup, the lateral group had significantly shorter positioning and operative times and lesser blood loss than the prone group. However, in the underweight, normal weight, and overweight subgroups, no significant difference in these indicators was found between the lateral and prone groups (Table 4).
 |
Table 4 Outcomes of the Stratified Analysis |
Discussion
Cervical myelopathy is compression of the cervical spinal cord leading to pathognomonic neurological symptoms and physical exam findings. Compression can be secondary to degenerative changes, a herniated disk, trauma, tumor, bleeding, infection, or ossification diseases such as ossified posterior longitudinal ligament or ossified yellow ligament. Surgery is the only effective treatment option for advanced degenerative cervical myelopathy. Decompression may be achieved via either an anterior or posterior approach.10 They are both well-established techniques that are used to achieve optimal clinical results with each approach having its own pros and cons. Also, there is lack of agreement between non-instrumented laminectomy, laminectomy and fusion and laminoplasty in case of posterior approach. The diagnosis and treatment of degenerative cervical myelopathy (DCM) has been continuously evolving over the past 5 decades.11 Laminoplasty still a useful posterior-based technique most frequently used in a lordotic spine that has compression at multi-levels, a congenitally stenotic canal, or a fused anterior column.12
The choice of surgical position is important in cervical laminoplasty, but scientific studies regarding this are lacking. In this study, we examined the safety of lateral decubitus position for cervical laminoplasty by comparing it with the traditional prone position. Our findings revealed that the lateral position is as safe as the prone position for cervical laminoplasty. It is easier to place the obese patients in the lateral position to ensure free abdominal movements.
In general, the prone position is used in cervical laminoplasty, which is a classic procedure for posterior cervical spinal cord decompression. Much efforts had been made to improve the safety of the prone position.13 In the earlier period of this study, we used the prone position routinely for laminoplasty surgery. However, we found it to be cumbersome and unreliable for ensuring the safety for certain patient groups, specifically obese patients with protruding bellies who require longer positioning time to ensure free abdominal movements. However, for these patients, even with meticulous positioning and despite ensuring that the bolster had adequate height and length, the bolsters still move away from each other under the body weight during operation. Anesthetic and position-related venous back pressure producing excessive hemorrhage may complicate the surgery and may further lengthen the operative time.2
The primary advantage of the lateral position is that it simplifies the procedure of patient’s position placement. In the lateral position, the patient is placed in a side-lying position on the operative table, with two longitudinal bolsters used to maintain the lateral position, rather than to support the patient’s weight as in the prone position. This method can be easily implemented to ensure free abdominal movements. Turning over the patients is not required as in the prone position; thus, the lateral position can be accomplished with little effort from the nurse and surgeon. The simplicity of the lateral position was tested in this study. As shown in our results, for obese patients, the positioning time was significantly shorter in the lateral group than in the prone group. Moreover, in the lateral position, the inferior vena cava was subjected to minimal body weight, venous plexus reflux was unobstructed, and it resulted in lesser blood loss and shorter operative time.
Many position-related complications have been reported for the prone position, with facial pressure ulcer being its well-known complication, which is most likely to occur at the forehead and chin.14,15 These sites have little muscle mass; thus, within the time period required for laminoplasty, pressure ulcers may likely form because of the high interface pressure and local blood supply shortage. In this study, the incidence of pressure ulcers was 11.39%, while in the lateral position, the incidence of pressure ulcers was only 2.18% in the lateral positions. Ocular complications have been reported to be related to patient malpositioning and prolonged pressure on the eye. Especially, post-operative visual loss following posterior spine surgery is rare but catastrophic. The overall incidence of blindness after spine surgery was estimated to be one case per 100 spine surgeons annually.16,17 Although we did not have any cases of vision complications in both groups, it is clear that the lateral position decreased the possibility of extrinsic pressure over the eyeball.
There are several other advantages of the lateral position. Firstly, the lateral position provides a relatively blood-less surgical field by promoting gravity drainage of blood and cerebral spinal fluid (CSF). The blood could run out of the wound rather than collect in the depths of the cavity. Next, when the surgeon looks down from the open side of the lamina, it will be easy to inspect the spinal canal and detach the adhesion under direct vision, which potentially decreases the opportunity of iatrogenic neural injury (Figure 2). Then, in the lateral position, the access to the airway is maintained at all times; thus, any tube problem may be corrected quickly. However, in the prone position, it is difficult to access the airway, which is difficult for proper airway management. Finally, the surgeon is more relaxed in the operation when the patient is in the lateral position. That is, in the lateral position, the surgeon may sit and can look at the surgical field with his or her cervical spine in the neutral position; thus, the surgeon does not easily get tired (Figure 1C). However, in the prone position, the surgeon always stands during the procedure, and needs to lower his head to properly visualize the surgical field, which may likely cause occupational hazard to the surgeon’s cervical spine.
For the comparison of the surgical outcomes of this study, we followed up the JOA and VAS scores of 30 latest patients in the lateral and prone groups. As expected, the differences in surgical position did not result in differences in surgical outcomes.
There are relative disadvantages of the lateral position. Firstly, performing cervical traction is difficult in lateral position. So, for patients with cervical deformity need correction and fixation, lateral position is inapplicable. Secondly, the surgeon should familiar with operative techniques for the lateral position. There will be a short learning curve for the surgeons accustomed to operating in the lateral position. Thirdly, in the lateral position, both the surgeon and his assistant stand at the back side of the patient, rather than at bilateral side of the patient in the prone position. Occasionally, this results in the assistant being inconvenient to observe the surgical field. Fourthly, intraoperative ultrasound is a useful tool in spine surgery, while the lateral approach might limit the quality of intraoperative ultrasound due to the difficulty to fill the surgical site with saline solution.18
One of the limitations of this study was its retrospective design. The comfort and workload of the operating team member is interesting for research, but it is impossible to evaluate these objectively in a retrospective manner. This problem can be solved by means of well-designed questionnaires for the operating room team to fill out. We noticed significant predictors of outcome following surgery for degenerative cervical myelopathy have been reported.19 It will be meaningful to address the question of significant predictors of outcome following cervical decompression with lateral position. Future studies that compare the lateral position with the prone position in a prospective, randomized, and controlled manner are warranted.
Conclusion
Our data showed that the lateral position is as safe as the prone position for cervical laminoplasty. It is easier to position obese patients in lateral position and to ensure free abdominal movements in this position. It seems reasonable to recommend the performance of laminoplasty in the lateral position for obese patients.
Acknowledgments
This work was partly supported by the 2016 Henan Science and Technology Research Project (grant number: 162102310018); the 2018 National and Provincial Co-Construction Project of Henan Provincial Medical Science and Technology Research (grant number: SBGJ2018076); and Henan Provincial Zhongyuan Thousand Talents Plan.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Petraglia AL, Srinivasan V, Coriddi M, et al. Cervical laminoplasty as a management option for patients with cervical spondylotic myelopathy: a series of 40 patients. Neurosurgery. 2010;67:272–277. doi:10.1227/01.NEU.0000371981.83022.B1
2. Anderton JM. The prone position for the surgical patient: a historical review of the principles and hazards. Br J Anaesth. 1991;67:452–463. doi:10.1093/bja/67.4.452
3. Dharmavaram S, Jellish WS, Nockels RP, et al. Effect of prone positioning systems on hemodynamic and cardiac function during lumbar spine surgery: an echocardiographic study. Spine (Phila Pa 1976). 2006;31:1388–1393. doi:10.1097/01.brs.0000218485.96713.44
4. Marchi L, Pimenta L, Oliveira L, et al. Distance between great vessels and the lumbar spine: MRI study for anterior longitudinal ligament release through a lateral approach. J Neurol Surg a Cent Eur Neurosurg. 2017;78:144–153. doi:10.1055/s-0036-1592144
5. Oikawa Y, Eguchi Y, Watanabe A, et al. Anatomical evaluation of lumbar nerves using diffusion tensor imaging and implications of lateral decubitus for lateral transpsoas approach. Eur Spine J. 2017;26:2804–2810. doi:10.1007/s00586-017-5082-y
6. Ziino C, Konopka JA, Ajiboye RM, et al. Single position versus lateral-then-prone positioning for lateral interbody fusion and pedicle screw fixation. J Spine Surg. 2018;4:717–724. doi:10.21037/jss
7. Lalonde NM, Villemure I, Pannetier R, et al. Biomechanical modeling of the lateral decubitus posture during corrective scoliosis surgery. Clin Biomech (Bristol, Avon). 2010;25:510–516. doi:10.1016/j.clinbiomech.2010.03.009
8. Japanese Orthopedic Association. Scoring system for cervical myelopathy. J Jpn Orthop Assoc. 1994;68:490–503.
9. Hirabayashi K, Miyakawa J, Satomi K, et al. Operative results and postoperative progression of ossification among patients with ossification of cervical posterior longitudinal ligament. Spine. 1981;6:354–364. doi:10.1097/00007632-198107000-00005
10. Kato S, Ganau M, Fehlings MG. Surgical decision-making in degenerative cervical myelopathy – anterior versus posterior approach. J Clin Neurosci. 2018;58:7–12. doi:10.1016/j.jocn.2018.08.046
11. Ganau M, Holly LT, Mizuno J, et al. Future directions and new technologies for the management of degenerative cervical myelopathy. Neurosurg Clin N Am. 2018;29:185–193. doi:10.1016/j.nec.2017.09.006
12. Rao RD, Currier BL, Albert TJ, et al. Degenerative cervical spondylosis: clinical syndromes, pathogenesis, and management.J. Bone Joint Surg Am. 2007;89:1360–1378. doi:10.2106/00004623-200706000-00026
13. Edgcombe H, Carter K, Yarrow S. Anaesthesia in the prone position. Br J Anaesth. 2008;100:165–183. doi:10.1093/bja/aem380
14. Grisell M, Place H. Face tissue pressure in prone positioning: a comparison of three face pillows while in the prone position for spinal surgery. Spine. 2007;7:84S–85S. doi:10.1016/j.spinee.2007.07.209
15. Jain V, Bithal PK, Rath GP. Pressure sore on malar prominences by horseshoe headrest in prone position. Anaesth Intensive Care. 2007;35:304–305.
16. Myers MA, Hamilton SR, Bogosian AJ, et al. Visual loss as a complication of spine surgery. A review of 37 cases. Spine (Phila Pa 1976). 1997;22:1325–1329. doi:10.1097/00007632-199706150-00009
17. Heitz JW, Audu PB. Asymmetric postoperative visual loss after spine surgery in the lateral decubitus position. Br J Anaesth. 2008;101:380–382. doi:10.1093/bja/aen163
18. Ganau M, Syrmos N, Martin AR, et al. Intraoperative ultrasound in spine surgery: history, current applications, future developments. Quant Imaging Med Surg. 2018;8:261–267. doi:10.21037/qims.2018.04.02
19. Tetreault L, Palubiski LM, Kryshtalskyj M, et al. Significant predictors of outcome following surgery for the treatment of degenerative cervical myelopathy: a systematic review of the literature. Neurosurg Clin N Am. 2018;29:115–127. doi:10.1016/j.nec.2017.09.020
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.