Back to Journals » Diabetes, Metabolic Syndrome and Obesity » Volume 14
Knowledge, Attitude and Practice Towards Insulin-Self Administration Among Diabetic Patients Attending Bedele Hospital, Southwest Ethiopia, 2019/2020
Authors Fego MW ![]() , Yasin JT, Aga GM
, Yasin JT, Aga GM
Received 27 August 2020
Accepted for publication 31 March 2021
Published 29 April 2021 Volume 2021:14 Pages 1919—1925
DOI https://doi.org/10.2147/DMSO.S279186
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Prof. Dr. Antonio Brunetti
Melese Workneh Fego,1 Jihad Tahir Yasin,2 Gezahegn Mamo Aga2
1Department of Nursing, College of Public Health and Medical Sciences, Mettu University, Mettu, Ethiopia; 2Mettu Health Science College, Mettu, Ethiopia
Correspondence: Melese Workneh Fego
Mettu University, PO Box: 318, Ethiopia
Email [email protected]
Background: Diabetes mellitus is a heterogeneous clinical syndrome secondary to defects in insulin secretion, action, or both. The worldwide fatality and disability rate imposed diabetic patients for insulin self-administration regardless of a scarcity of their knowledge, attitude, and practices. Thus, the study aimed to assess knowledge, attitude, and practice towards insulin-self administration among diabetic patients attending Bedele Hospital, southwest of Ethiopia.
Methods: A facility-based cross-sectional study was conducted by a consecutive sampling technique at Bedele Hospital from 15 December 2019 to 22 January 2020. A pretested structured English version relevant questionnaire translated to local language was administered on 196 subjects. Data were tested for clarity, consistency and analyzed using The Statistical Package for Social Sciences version 23 and summarized using descriptive statistics in the form of tables and figures.
Results: Of 196 subjects, 180 subjects participated in the study giving a response rate of 92%. The study reveals that knowledge, attitude, and practice towards insulin self-administration were 132 (67.3%), 113 (57.6%), and 123 (62.8%), receptively, which implies that good knowledge, a favorable attitude, and good practice to insulin self-administration.
Conclusion: While the patients had good knowledge, good practice, and a favorable attitude to insulin self-administration, it does not match sufficient thus, to achieve a maximum level the hospital should develop several strategies like constant information education communication.
Keywords: attitude, diabetic patients, insulin self-administration, knowledge, practice
Introduction
Diabetes mellitus (DM) is one of the metabolic conditions described by chronic hyperglycemia with disruption of fat, protein, and carbohydrate metabolism caused by a shortage of insulin secretion, action, or both.1 Insulin is a hormone essential for normal carbohydrate, protein, and fat metabolism. People with type 1 DM do not produce a sufficient amount of this hormone to sustain life and rely on exogenous insulin to survive.2 On contrary, persons with type 2 diabetes are not dependent on exogenous insulin for survival. However, over time, many of these individuals will show decreased insulin production, therefore requiring supplemental insulin for suitable blood glucose control, mainly in stress or acute illness time. Diabetic ketoacidosis (DKA) is an acute and unsafe complication and a medical emergency that is more shared in type I diabetes. Worldwide fatality and disability rate’ enforced diabetic patients to Insulin self-administration despite a scarcity of their Knowledge, Attitude, and Practices.1–5 The good knowledge, favorable attitude, and practices of insulin self-administration (ISA) among insulated diabetic patients including taking medication properly, regular exercise, following a diabetic meal plan, and blood glucose test are some of the most crucial components’ glycemic control.2,3
Worldwide, the prevalence of good knowledge and favorable attitudes ISA was ranged nearly from 33.3% to 98.7%, 50.3% to 98% receptively.3 In South Africa, a result reveals that there is Poor knowledge, a negative attitude, and poor practices related to diabetes were observed which uncover morbidity and death.4 Lack of understanding of patients’ characteristics and diabetes-related knowledge, practice, and attitude will lead to a high possibility of unsuitable direction and faulty education program.5–8 Research studies conducted in different parts of the world showed evidence of inadequate knowledge and poor practice level on ISA among DM patients.9
Studies reveal that the knowledge level of diabetic patients on self-care management should be supported.10 Patients or family members must know and follow specific insulin storage guidelines provided by the manufacturers which include how to store and refrigerate insulin vials that not used to avoid loss of potency, how to draw insulin into an insulin syringe, selection and preparation of injection site, and correct injection technique for safe administration.11–14 Repeated practice is enforced for safe administration using exact dose and hygienic techniques. But, diabetic patients are fearful of self-injection and would prefer to delay learning. Thus, nurses should teach them irrespective of voicing the strain or fear of insulin self-administration by the patients.11 Though some diabetes patients inject themselves, most of the steps in the performance of insulin administration were incorrect.12 Diabetic patients who are on insulin need to be knowledgeable regarding the disease and insulin therapy and also they must have the competency and positive attitude towards Self-administration of insulin injection to overcome the barriers of insulin injection and to have good glycemic control.14,15
Various studies have been conducted in various parts of the world towards knowledge, attitude, and practice of diabetes patients towards self-administration of insulin for the enhanced management of the disease.9 Even though many studies were done in Ethiopia, regarding patients’ knowledge, attitude, and practices still know there is a scarcity of data in the study area.
Hence, the current study aimed to assess the level of knowledge, attitude, and practice towards insulin self-administration among diabetic patients attending Bedele Hospital, Southwest of Ethiopia.
Methods
A facility-based cross-sectional study design was conducted on 196 subjects to assess knowledge, attitude, and practice towards insulin self-administration among diabetic patients in Bedele hospital (BH), Bedele Town. The Town is located about 480km southwest of Addis Ababa which is the capital city of Ethiopia. The study was conducted from 15 December 2019 to 22 January 2020. All inpatients’ and outpatients’ diabetics in BH were a source population while all diabetic patients started to use insulin and having follow-ups in BH were the study population. All type I and type II diabetic patients taking insulin treatments was included in the study and severely ill, physically impaired, newly diagnosed, and psychiatric patients and involuntary to participate were excluded during data collection. The sample size was determined by using a single population proportion formula by considering the average expected proportion of poor knowledge, poor practice, and unfavorable attitude 68% extracted from four similar studies,2,6,16,17 5% margin of error, 95% CI and 10% non-response rate and considering correction formula. The sampling technique was all patients meeting the inclusion criteria having follow-up in BH during the study period. The pretest of the data collection tool was done on 5% of the study subjects within five days before actual data collection. Data were collected using a structured questionnaire composed of socio-demographic and clinical characteristics, validated knowledge questions adapted from spoken knowledge in low literacy in diabetes knowledge assessment scale, and attitude and practice questions were adapted from other relevant literature.18,19 To ensure the quality of data the questionnaire has prepared to cover a wide area of interest including socio-demographic characteristics, source of information about Knowledge, Attitude, and practice of insulin self-administration. Two days of training were given for data collectors. The collected data were checked for clarity and analyzed by SPSS version 23 and descriptive statistics were used to summarize the findings. This study was conducted agreeing to comply with the declaration of Helsinki. The ethical clearance with a reference number CBE/26/03/2012 was obtained from the faculty of public health and medical sciences, Mettu University, and submitted to the study hospital. The verbally informed consent process was approved by the Faculty of Public Health and Medical Sciences, Mettu University. Formal informed consent was obtained from study participants, and for diabetes patients under 18 years old verbal informed consent was secured from their parents/legal guardian to join in the study, and set free to withdraw them-selves any time as they want”. All of the participant’s information was kept confidential throughout the study period.
Results
Socio-Demographic Characteristics
A total of 196 subjects were included in the present study of which the majority 112 (57.1%) were male. The majority of the respondents 130 (66.3%) were Oromo, followed by 37 (18.9%) were Amhara. Regarding the educational level, University degree, secondary school, and primary school were 17 (8.7%), 57 (29%), and 36 (18.3%) receptively. The majority 122 (62.2%) were married. Concerning their occupation, government employer accounts 27 (13.8%). Regarding economic status, about 38 (39.7%) were an annual income of less than two thousand Ethiopian birrs (Table 1).
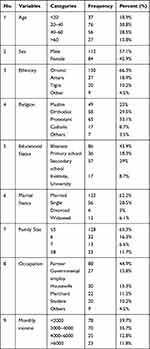 |
Table 1 Socio-Demographic Variables of Diabetic Patients in Bedele Hospital from 15 December 2019 to 22 January 2020, Southwest Ethiopia (n=196) |
Knowledge Towards Insulin Self-Administration
The current study shows that the overall knowledge level of patients towards insulin self-administration was 55% of which 132 (67.3%) had good knowledge and 64 (33.7%) had poor knowledge. More than half 132 (67.3%) of the respondents were knowledgeable about the definition of diabetic Mellitus and 136 (69.3%) participants believe that diabetes mellitus is not curable. The result also shows that 189 (96.4%) participants were believed as being on insulin therapy were controlled their blood glucose level. More than half 290 (96.9%) knows about the benefit of insulin therapy for the prevention of complication related to diabetes mellitus. Among the total respondents, about 128 (65.3%) of the respondents consider that insulin absorption is faster through the abdominal wall or umbilicus than other roots of insulin injection. About 164 (83.6%) know the significance of circling insulin injection sites for faster absorption. About 45 (22.9%) of respondents knew about the proper way for insulin self-administration (Figure 1).
 |
Figure 1 Knowledge of insulin self-administration among diabetic patients in Bedele Hospital, from 15 December 2019 to 22 January 2020, Southwest Ethiopia (n=196). |
Attitude Towards Insulin Self-Administration
According to the present study, the diabetic patients’ attitude towards insulin self-administration was 113 (57.6%) and 83 (42.4%) which implies favorable and unfavorable attitudes, receptively. Out of 196 study subjects, about 118 (60.2%) agreed with the direct relationship between exercise and rate of insulin absorption. Regarding insulin injection and Luke’s water bath, 26 (13.2%) did not agree about the avoidance of insulin injection immediately before and after a hot bath. On the other hand, 71 (33.6%) of the respondent agree with insulin causes weight gain. But, 108 (55.1%) and 126 (64.2%) of the patients disagree with managing insulin treatment takes a lot of time and energy, and insulin injection is pain full, respectively. Also, 147 (75%) of the participants were agreeing with being on insulin leads to family and friends being more concerned about them. Among the total participants129 (65.8%) of the respondents disagree that, needle length should not be a concern in patients who are obese or overweight (Table 2).
 |
Table 2 Attitude of Patients Towards Insulin Self-Administration in Bedele Hospital from 15 December 2019 to 19 January 2020, Southwest Ethiopia (n=196) |
Practice Towards Insulin Self-Administration
The present study exposes that, 123 (62.8%) of the respondents had a good practice of insulin self-administration, while 73 (37.2%) had poor practice. More than half 157 (80.1%) of the participants were washing their hands before insulin self-injection, while 153 (78%) had washing their hands after insulin self-injection. About 70 (35.7%) of the respondents had a practice of cleaning and drying the site of injection before insulin self-administration. Regarding site rotation majorities of the respondents, 121 (61.7%) had established orders from their health caregivers. Regarding the site of injection about 128 (65.3%) of the respondents were injecting insulin around the umbilicus subcutaneously on the abdomen while the others 29 (14.5%) injected on their upper thigh. Among the total participants, 120 (61.2%) followed manufacturer guidelines to prepare the dose of insulin. One hundred and ninety-one (97.4%) of the respondents use the needle for injection more than one time and 186 (95%) of them recap the needle after the completion of the injection. Among them, 178 (90.8%) participants recap by Supporting the syringe in the hand and replacing the cap with a straight motion of the thumb and forefinger, and 17 (8.6%) of them by recapping the needle. About 178 (90.8%) of the respondents removed the air bubble from the insulin syringe before injection (Figure 2).
 |
Figure 2 Practice of insulin self-administration among diabetic patients attending in Bedele hospital from 15 December 2019 to 22 January 2020, Southwest Ethiopia (n=196). |
Discussions
The present study identified the level of knowledge, attitude, and practice towards insulin self-administration among diabetic patients attending Bedele hospital, Bunno Bedele zone, Southwest Ethiopia. The finding reveals that 132 (67.3%), 113 (57.6%), and 123 (62.8%) of the respondents had good knowledge, a favorable attitude, and good practice of insulin self-administration receptively.
Regarding the knowledge level of diabetic patients toward insulin-self administration, 132 (67.3%), the result was higher than a study conducted at Mettu Karl Referral hospital in Ethiopia, Bale in southeast Ethiopia, Mekele hospital in Ethiopia, Ramaiah Hospital in Bengaluru, Jordan, and Northwest University hospital in Gonder (38.4%), (52.5%), (55.3%), (58%), (53.3%), and (60%) receptively.2,6,16,17,20,21 The possible explanation of the difference within the country might be the variability of socio-demographic characteristics of the area, it might also be variances in study design, study period or sample size used when we compare with the study conducted in Ethiopia. It might also be due to the establishment time varies from each hospital that might affect the training duration of diabetic patients. This result was lower than a study conducted in India, Ayder Comprehensive Specialized Hospital in North Ethiopia, and Hawassa Referral Hospital in Southern Ethiopia, (77.3%), (70.4%), and (85.6%), respectively.22–24 The possible explanation of the differences might be due to the lower educational level in the study area compared to India. The differences might also due to poor dedicated time to teach patients by health care providers, and inadequate follow-up of awareness creation about diabetic patients’ self-care activities. The current study reveals that the core sources of information allied to insulin-self administration were health professionals especially nurses and Physicians (100%). This finding was consistent with two studies done in India that showed health professionals were the key source of information, 78% and 68%, respectively.22,25 This directed the need for additional insulin self-administration strategies.
Regarding the attitude of diabetic patients toward insulin-self administration 113 (57.6%) which implies good knowledge, this result was higher than a study conducted at Mettu Karl Referral Hospital, Southwest Ethiopia in 2019, average favorable attitudes towards insulin self-administration (20.7%). The possible explanation of the differences might be variations in data collection methods, investigator, number of patients flows that might be beyond the available number of health professionals which enforce them to week quality health care services that may increase or decrease the patients’ attitudes. But the finding is lower than a study done at Hawassa Referral Hospital, Southern Ethiopia in 2019, Mekele Hospital in 2015 Northern Ethiopia, Gonder university hospital in Northwestern Ethiopia in 2013 (71.1%), (68.0%), and (78%) receptively which implies a favorable attitude toward insulin self-administration.17,20,24 The possible explanation of the variances might be as Bedele hospital is the young or primary hospital that may hinder to provide suitable information education services to diabetic patients to achieve maximum satisfaction and contribute very well to the fluctuation of patients’ attitudes when we compared with the others.
Regarding the practice level of diabetic patients toward insulin-self administration, 123 (62.8%) of participants had a good practice. This finding was higher than a similar study conducted at Hawassa Referral Hospital Southern Ethiopia (54.4.5) of the participants had a good practice towards insulin self-administration and a quantitative study was done at Karnataka State, in India in 2011, (72%) of the subjects had poor practice. It also higher than the study conducted at Harari town in 2011 (60.7%) had poor self-care practices.9,22,26 The possible explanation of the differences might be due to differences in the study period or due to respondents’ partiality and might also be due to differences in socio-demographic variability in Ethiopia and India. It might also due to the high illiteracy flow rate of the study participants, lack of health care access, and/or poor personal habits to attend the hospital; it might also be due to obstacles due to health professionals like scarcity of time due to the scarce human power that enforces hospitals to focus only on acutely ill patients than preventive care.
Conclusions
Diabetes imposes lifelong threats on individuals and their families. This study showed that there were knowledge, attitude, and practice gap among the patients concerning insulin self-administration. The finding reveals that sixty-seven point three percent of the total respondents have good knowledge, a favorable attitude, and sixty-two point eight had a good practice of insulin self-administration.
Recommendation
To raise the knowledge, attitude, and practice level of diabetic patients towards ISA, both governmental and non-governmental organization could invest their collaborative efforts through active immersion to ensure patients are receiving exciting efforts from health care professionals. Bedele hospital should deliver constant health information communication concerning ISA and Mettu University could conduct auxiliary studies by covering factors upsetting ISA among diabetic patients thus, it helps to develop strategies to overcome the root causes.
Acknowledgments
The authors want to pass their thanks to Mettu University and BH for their consent for the study. Secondly, we would like to direct our sincere thanks to Mr. Tsegaye Workneh Fego (MA Candidate) for revising the language and grammar of the manuscript. Finally, we would like to appreciate study members who gave their deserved effort for realizing the work.
Disclosure
The authors declare that there is no competing interests in this work.
References
1. World Health Organization Diabetes Management Directorate of public health non-communicable diseases section, 39–40, 2011.
2. Gurmu AE, Teni FS. Knowledge, attitude, and practice among diabetic patients on insulin therapy towards the disease and their medication at a university hospital in Northwestern Ethiopia. Int J Pharm Sci Res. 2014;5(10):685–692.
3. Daly JM, Hartz AJ, Xu Y, et al. An assessment of attitudes, behaviors, and outcomes of patients with type 2 diabetes. J Am Board Fam Med. 2009;22(3):280–290. doi:10.3122/jabfm.2009.03.080114
4. Roux ML, Walsh C, Reid M, Raubenheimer J. Diabetes-related knowledge, attitude and practices (KAP) of adult patients with type, 2 diabetes mellitus in the Free State province, South Africa. South Afr J Clin Nutr. 2019;32(4):83–90. doi:10.1080/16070658.2018.1468536
5. El-Khawaga G, Abdel-Wahab F. Knowledge, attitudes, practice, and compliance of diabetic patients in Dakahlia, Egypt. Eur J Res Med Sci. 2015;3(1):40–53.
6. Tewodros Y. Knowledge and attitude on insulin self-administration among type 1 diabetic patients at Metu Karl Referral Hospital, Ethiopia, Hindawi. J Diabetes Res. 2019;2019:1–7. doi:10.1155/2019/7801367
7. AACE. American Association of Clinical Endocrinologists medical guidelines for clinical practice for developing a diabetes mellitus comprehensive care plan. Endocr Pract. 2011;17(2):287–302.
8. Ichinose K, Kawasaki E, Eguchi K. Recent advancement of understanding pathogenesis of type 1 diabetes and potential relevance to diabetic nephropathy. Am J Nephrol. 2010;27(6):554–564. doi:10.1159/000107758
9. Beneby N, Isaacs C, King L, et al. Knowledge, attitude, and perception of the patients towards insulin therapy at primary care centers in Trinidad. J Community Med Public Health Care. 2015;2:004.
10. Moodley L, Rambiritch V. An assessment of the level of knowledge about diabetes mellitus among diabetic patients in a primary healthcare setting. S Afr Fam Pract. 2011;49:10.
11. Naglaa MA, Mohamed EM. Effectiveness of health education program for type 2 diabetes mellitus patients attending Zigzag University Diabetes Clinic, Egypt. Egypt Public Health Assoc. 2010;85(3):4.
12. Ramesh R, Kumar SV, Gopinath S, Gavaskar B, Gandhiji G. Diabetic knowledge of the rural community and drug utilization pattern in a tertian care hospital. Int J Pharm Life Sci. 2011;2(l):531–535.
13. Okolie VU, Ehiemere OI, Peace IN, Ngozi KI. Knowledge of diabetes management and control by diabetic patients at Federal Medical Center Umuahia Abia State Nigeria. Int J Med Sci Public. 2009;1(9):353–358
14. Voice Achienge, assessment of the level of knowledge, self-care, and glycemic control among patients with type II DM attending the diabetic clinic at Kenyatta national hospital. 2014.
15. Deere A, Rajalakshimi M, Yayehirad T, et al. Diabetes mellitus for the Ethiopian Health Center Team, 2010.
16. Kassahun CW, Mekonen AG, Ciccozzi M. Knowledge, attitude, practices and their associated factors towards diabetes mellitus among non diabetes community members of Bale Zone administrative towns, South East Ethiopia. A cross-sectional study. PLoS One. 2017;12(2):e0170040. doi:10.1371/journal.pone.0170040
17. Hadgu G, Admasu M, Birikity S, et al. Knowledge and attitude on insulin self administration among, type one diabetic patients in Mekele Hospital, Tigray, Ethiopia. Adv Surg Sci. 2015;3(5):32–36. doi:10.11648/j.ass.20150305.11
18. Rothman RL, Malone R, Bryant B, et al. The spoken knowledge in low literacy in diabetes scale: a diabetes knowledge scale for vulnerable patients. Diabetes Educator. 2005;31(2):215–224. doi:10.1177/0145721705275002
19. Toobert DJ, Hampson SE, Glasgow RE. The summary of diabetes self-care. Diabetes Care J. 25(1):14–17. The National Medical Journal of India,2012.
20. Navaneeth VM, Nazish F, Mamatha KA. Study on Knowledge, Attitude, and Practice (KAP) in diabetic patients attending endocrinology OPD at a Tertiary Care Hospital. RUAS SASTech J. 2018;11(1):53–56.
21. Alsous M, Abdel Jalil M, Odeh M, et al. Public knowledge, attitudes and practices toward diabetes mellitus: a cross-sectional study from Jordan. PLoS One. 2019;14(3):1–12, e0214479. doi:10.1371/journal.pone.0214479
22. Gawand KS, Gawali UP, Kesari HV. A study to assess knowledge attitude and practice concerning insulin use in adult patients with Diabetes Mellitus in the tertiary care center. Indian J Med Res Pharm Sci. 2016;3(9):36–40.
23. Niguse H, Belay G, Fisseha G, et al. Self-care-related knowledge, attitude, practice and associated factors among patients with diabetes in Ayder Comprehensive Specialized Hospital, North Ethiopia. BMC Res Notes. 2019;12:34. doi:10.1186/s13104-019-4072-z
24. Getachew F, Solomon D. Knowledge, attitude, practice and associated factors towards self-insulin administration among diabetic patients in Hawassa Referral Hospital, Southern Ethiopia. Recent Res Endocrinol Metab Disorder. 2019;1(1):10–17. doi:10.33702/rremd.2019.1.1.3
25. Sourav D, Somak K, Avijit H. Survey of knowledge-attitude-practice concerning insulin use in adult diabetic patients in eastern India. Indian J Pharmacol. 2014;46(4):425.
26. Ayele K, Tesfa B, Abebe L, Tilahun T, Girma E, Bacurau RFP. Self care behavior among patients with diabetes in Harari, Eastern Ethiopia: the health belief model perspective. PLoS One. 2012;7(4):e35515. doi:10.1371/journal.pone.0035515
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms
and incorporate the Creative Commons Attribution
- Non Commercial (unported, 3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
