Back to Journals » Journal of Multidisciplinary Healthcare » Volume 13
Informed Consent Form Challenges for Genetic Research in Jordan
Authors Alkaraki AK , Khabour OF , Alzoubi KH , Al-Ebbini LMK , Altaany Z
Received 28 December 2019
Accepted for publication 13 February 2020
Published 5 March 2020 Volume 2020:13 Pages 235—239
DOI https://doi.org/10.2147/JMDH.S243669
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Almuthanna K Alkaraki,1 Omar F Khabour,2 Karem H Alzoubi,3 Lina MK Al-Ebbini,4 Zaid Altaany5
1Department of Biological Sciences, Faculty of Science, Yarmouk University, Irbid 21163, Jordan; 2Department of Medical Laboratory Sciences, Faculty of Applied Medical Sciences, Jordan University of Science and Technology, Irbid 22110, Jordan; 3Department of Clinical Pharmacy, Faculty of Pharmacy, Jordan University of Science and Technology, Irbid 22110, Jordan; 4Department of Biomedical Systems and Informatics Engineering, Hijjawi for Engineering Technology, Yarmouk University, Irbid 21163, Jordan; 5Department of Basic Medical Sciences, Faculty of Medicine, Yarmouk University, Irbid 21163, Jordan
Correspondence: Almuthanna K Alkaraki
Department of Biological Sciences, Faculty of Science, Yarmouk University, Irbid 21163, Jordan
Tel +962 2 72 11111 ext. 2833
Fax +96227211117
Email [email protected]
Background: Informed consent is an obligatory requirement for research engaging human subjects. Informed consent form (ICF) should be provided for human subjects to confirm their willingness for voluntary participation in a study. Ethical and legal obligations necessitate the presence of informed consent essential items to be built into the ICF.
Objective: To evaluate the content of ICFs obtained from different genetic studies accomplished in Jordan and their adherence to ethical guidelines proposed by the International Conference on Harmonization—Good Clinical Practice (ICHGCP).
Methods and Measures: A total of 44 ICFs obtained from master theses and grant proposals at two major universities in Jordan were analyzed according to the good clinical practice criteria proposed by ICHGCP. ICFs were scored for the presence or absence of ICF main items/categories.
Results: Results show inadequate information present in the examined ICFs. The highest information score was 17 out of 20, while the lowest score was one out of 20. The average score for all studied ICFs was 6.18± 3.65. Among essential items/categories that were absent from the majority of studied ICFs were a statement about voluntary participation, confidentiality of data, compensation to study participants, risk/benefits of the study, and researchers’ contact information.
Conclusion: The ICFs were missing a number of required items. This could reflect inadequate knowledge about minimal informed consent requirements among Jordanian investigators highlighting the need for research ethical training in the country.
Keywords: informed consent form, challenges, genetic research, Jordan
Introduction
Obtaining informed consent is one of the ethical values of the declaration of Helsinki, the Belmont report and the Nuremberg code.1 The procedure of obtaining informed consent from human subjects in medical research is firmly regulated.2 The informed consent form (ICF), which indicates the agreement of the human subject—or their guardian—to participate in the research project is part of the procedure.3,4 The International Conference on Harmonization—Good Clinical Practice (ICHGCP) outlined minimum requirements for the ICF, where it should include essential information to enable participants to make an informed decision.4,5 The main purpose of ICHGCP is to preserve the rights of human subjects participating in medical research. The outlined guidelines have a beneficial impact on research conducted on human subjects all over the world.6 Different consent models were reported in the literature; including verbal, blanket, broad, meta, dynamic, and waived consents.7 Among essential information are descriptions of the nature of the study, purpose of the study, specimen management procedures, confidentiality, voluntarily participation, possible benefits/risks, expectations, contact information, study procedures, and participant’s rights and responsibilities.3–5,8
Recent decades have witnessed a growing interest in conducting research involving human subjects in Jordan.9,10 Informed consent, privacy, confidentiality, data storage and bio-specimen collection, and further analysis are some of ethical challenges of genetic studies in Jordan.10–13 Despite numerous publications that address ethical issues related to informed consent in genetic studies, very little is known about consenting genetic studies in the Arab region.8,14 In this study, we aimed to assess the content of different ICFs from genetic studies conducted in Jordan to determine the degree of compliance according to essential requirements proposed by ICHGCP.5 To achieve this goal, ICFs from research grant proposals and master's degree theses involving human genetic studies in two Jordanian universities were analyzed according to responsible conduct of research criteria proposed by ICHGCP.5
Methodology
Samples, Measures, and Data Analysis
A total of 44 ICFs that involved human genetic studies were obtained from studies that were conducted in the years 2007 to 2019 from two major universities in Jordan, namely, Jordan University of Science and Technology, and Yarmouk University. The 2007–2019 period was chosen because it corresponds with the year following the establishment of the local IRB committee serving both institutions in 2006.
The ICFs were obtained from research grant proposals and master's theses. ICFs were analyzed and assessed for the presence or absence of the minimal requirement of the ICH-GCP informed consent guidelines. This framework and research instrument was adopted from a previous study.8 Six major categories were assessed including: purpose of the study, study procedures, potential benefits/risks from participation, confidentiality, and participant rights and responsibilities. These six categories were further organized into 20 sub-items that include all the minimum requirements (Table 1) of a comprehensive ICF.8 The adopted scoring system was one for each sub-item present in the ICF and zero for the absent sub-item. Accordingly, the top score was 20, and the lowest score was zero.8 To ensure methodological rigor, ICFs content were scored by two well-trained researchers. Inconsistency between the two researchers was solved by taking the opinion of a third one.
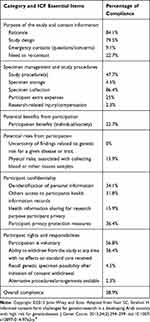 |
Table 1 Categories/Minimal Essential Items for all Informed Consent Forms. |
The study was approved by participating universities. The confidently of assessed ICFs, identity of researchers, grants sponsors, and university identity were protected. Genetic studies that involve human subject were considered eligible for assessment process. Data were analyzed using Statistical Package for Social Sciences, version 22.0 (IBM Corporation, Armonk, NY, USA). Data were expressed as percentage or as mean ± SD.
Results
ICFs (N=44) of genetic studies were analyzed according to the criteria proposed by ICHGCP. ICFs were previously approved by local IRB committees. Figure 1 Shows the histogram of ICFs scores of compliance out of 20 with their frequencies. The highest score was 17 out of 20, while the lowest score one out of 20. The normal curve was negatively skewed toward the low scores and only one ICF scored above 14 out of 20, indicating deficiency in the minimum requirement within the studied ICFs. The mean of the total scores for all ICFs was 6.18±3.65 (SD).
 |
Figure 1 ICFs compliance scores out of 20 (X-axis) according to the International Conference on Harmonization—Good Clinical Practice with their frequencies (Y-axis), N=44. |
Table 1. shows the categories/minimal essential items as percentage of compliance for all studied ICFs. Among the items assessed, rationale, specimen collection, consent model, subject name, and verbal information statement were available in more than 80% of the ICFs reviewed. Alternatively, items including study procedures, compensation, benefits/risk assessment, de-identification of personal information, access to participant’s health records, data sharing for research purpose, participant privacy/privacy protection measures, voluntary participation, ability to withdraw, and researcher name were often rarely considered in the ICFs (Table 1). Moreover, items such as emergency contacts, specimen storage, research-related injury compensation, uncertainty of findings related to genetic risk for a given disease or trait, recall genetic specimen possibility after initiation of consent withdrawal, and alternative procedures were not included in the vast majority of the ICFs reviewed. The overall compliance of the studied ICFs was 38.9% (Table 1).
Discussion
The number of genetic studies from Jordan increased within the last two decades. This could be due to increased research capacity; the prevalence of different genetic diseases, which were reported to be high among Jordanians as a result of consanguinity and high birth rate;15–17 and having a diverse population that contains many ethnic groups and minorities,18,19 along with the significant jumps in the census due to waves of immigration toward Jordanian territories from surrounding high tension countries. This increase in the number of genetic studies in Jordan should have been accompanied with an increase in awareness of the importance of applying ethical obligations and morals in the research process including proper informed consent process.10,13 Thus, the goal of the current study was to investigate the presence of the required items ICFs in genetic studies.
Different ethical challenges in genetic studies were addressed in previous studies.20,21 The newly emerging genetic information could affect patients’ clinical management and health services.20 Furthermore, genetic privacy has emerged as a challenging concern that need to be addressed carefully due to its familial sensitivity.22 One of the important requirements in establishing good ethical research is obtaining informed consent. The ICF should be adequate according to the standard guidelines that regulate the process of consenting subjects. However, studies that examined ethical challenges related to consent process in Jordan and the Arab countries were very limited. Recently, a research paper was published assessing the quality of ICFs in Jordan, however, the research paper was generally focused on biomedical research not genetic studies.23 Moreover, ethical challenges related to genetic research in developing countries were also explored earlier in other regions such as Africa.24 Another study was conducted in the UAE, addressing the ICF challenges in Arab developed countries.8
The current study has focused on ICFs from genetic studies conducted in Jordan. In the majority of examined studies inadequate information was detected as per the ICHGCP minimum requirements of ICFs. For example, critical items related to genetic research, such as uncertainty of findings related to genetic risk, recall genetic specimen possibility after initiation of consent withdrawal, and availability of alternative procedures were largely absent. In the current study, approximately one-third of the ICFs reviewed involved enough information to keep data confidentiality and to protect research participant privacy. These findings are similar to those of a previous study from the UAE, where these same items were also missing from most of the ICFs examined.8 However, this previous study showed that items such as compensation, benefits/risk assessment, and voluntary participation were present in all ICFs.8 Yet the current study found that majority of the ICFs from Jordan did not have these items present. Moreover, lower commitment to some important items was also noticed in our study such as, de-identification of personal information, the need to re-contact subjects, participant extra expenses and participant benefits/risks assessment. In some genetic studies, researchers are required to re-contact participants for any future use of the biological specimens; if the consent model was for a specific study.25 Repeated contact for re-use purposes seems an obstruction and a financial disadvantage to participation in research in the UAE, which could also be a problem in Jordan.8,10
The minimal essential items required to establish a complete an ICF vary between different ICFs studied indicating a lack of consistency among researchers. The dilemma of the absence of complete comprehensive ICFs could be due to the lack of knowledge of responsible conduct of research among researchers along with lack of appropriate ethics training programs in the universities. The adoption of ICF templates for various research that involved human subjects by IRBs might help in improving the informed consent process and uniformity of ICFs.
The present deficits in ICFs have a direct impact on the participants of studies, especially in developing countries, including Jordan. Subjects are being enrolled in studies without complete information presented, which could pose a risk to participants, and violate their autonomy and their ethical right of respect. Therefore, action is recommended involving the implementation of compulsory human research ethics/guidelines training to every researcher or IRB member before being involved in human research projects/committees, and not only relaying on researchers’ experience, hands-on training, or voluntary workshops and courses.
The current study has some limitations including the fact that it included only two universities in Jordan, and inclusion of only 12 years interval. A future study covering more institutions and larger time frame is recommended. Moreover, assessing compliance with other guidelines and regulations such as the Final Rule 2017 or the CIOMS 2016, in addition to the ICH GCP could that matter of future study.
In conclusion, the use of ICFs with adequate information to enable the participants to make an informed decision in genetic research is still a challenging issue in Jordan. The adoption of a standard ICF templates for different types of medical research might improve the quality of the informed consent process. Furthermore, academic institutions in Jordan should adopt training programs in responsible conduct of research to improve the quality of the research involving human subjects.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Nijhawan LP, Janodia MD, Muddukrishna BS, et al. Informed consent: issues and challenges. J Adv Pharm Technol Res. 2013;4(3):134–140.
2. Manti S, Licari A. How to obtain informed consent for research. Breathe (Sheff). 2018;14(2):145–152. doi:10.1183/20734735.001918
3. Neff MJ. Informed consent: what is it? Who can give it? How do we improve it? Respir Care. 2008;53(10):1337–1341.
4. Macklin R. Understanding informed consent. Acta Oncol. 1999;38(1):83–87. doi:10.1080/028418699431843
5. ICH. International Conference on Harmonisation of technical requirements for registration of pharmaceuticals for human use (ICH) adopts consolidated guideline on good clinical practice in the conduct of clinical trials on medicinal products for human use. Int Dig Health Legis. 1997;48(2):231–234.
6. Dixon JR
7. Thompson R, McNamee MJ. Consent, ethics and genetic biobanks: the case of the Athlome project. BMC Genomics. 2017;18(Suppl 8):830. doi:10.1186/s12864-017-4189-1
8. Nair SC, Ibrahim H. Informed consent form challenges for genetic research in a developing Arab country with high risk for genetic disease. J Genet Couns. 2015;24(2):294–299. doi:10.1007/s10897-014-9763-y
9. Khalaf I. Development of nursing research in Jordan (1986–2012). Int Nurs Rev. 2013;60(4):461–468. doi:10.1111/inr.2013.60.issue-4
10. Makhlouf H, Alrabadi N, Khabour OF, Alzoubi KH, Al-Delaimy W. Population’s perspectives toward biobanks in scientific research: a study from Jordan. Pharmacogenomics Pers Med. 2019;12:23–32. doi:10.2147/PGPM.S187657
11. Ahmad MI, Daradkeh J, Malkawi M, Al Delaimy WK. Challenges in environmental health research and sustainability in a less developed country: a case study from Jordan. Curr Environ Health Rep. 2019;6(4):327–337. doi:10.1007/s40572-019-00248-2
12. Ayoub NM, Qandil AM, McCutchan JA. Knowledge, attitudes, and practice regarding research ethics committees among health care faculty at two public universities in Jordan. J Empir Res Hum Res Ethics. 2019;14(4):372–382. doi:10.1177/1556264619851351
13. Khabour OF, Abu-Siniyeh A. Challenges that face the establishment of diabetes biobank in Jordan: a qualitative analysis of an online discussion forum. J Multidiscip Healthc. 2019;12:229–234. doi:10.2147/JMDH.S194161
14. Al-Riyami A, Jaju D, Jaju S, Silverman HJ. The adequacy of informed consent forms in genetic research in Oman: a pilot study. Dev World Bioeth. 2011;11(2):57–62. doi:10.1111/dewb.2011.11.issue-2
15. Dasouki M, El-Shanti H. Genetic disorders in Jordan. In: Teebi AS, editor. Genetic Disorders Among Arab Populations. Berlin, Heidelberg: Springer Berlin Heidelberg; 2010:325–352.
16. El-Shanti H. The impact of genetic diseases on Jordanians: strategies towards prevention. J Biomed Biotechnol. 2001;1(1):45–47. doi:10.1155/S1110724301000092
17. Hamamy HA, Masri AT, Al-Hadidy AM, Ajlouni KM. Consanguinity and genetic disorders. Profile from Jordan. Saudi Med J. 2007;28(7):1015–1017.
18. Zanetti D, Sadiq M, Carreras-Torres R, et al. Human diversity in Jordan: polymorphic Alu insertions in general Jordanian and Bedouin groups. Hum Biol. 2014;86(2):131–138. doi:10.3378/027.086.0201
19. Azab M, AL-Bashir N, Momani SN, Al-Nasser A, Alkaraki AK, Khabour OF. Comparison between frequencies of several STRs loci in Jordan with neighboring countries. J Med J. 2010;44(1):55–60.
20. El Mecky J, Johansson L, Plantinga M, et al. Reinterpretation, reclassification, and its downstream effects: challenges for clinical laboratory geneticists. BMC Med Genomics. 2019;12(1):170. doi:10.1186/s12920-019-0612-6
21. Ahmed E, Shabani M. DNA data marketplace: an analysis of the ethical concerns regarding the participation of the individuals. Front Genet. 2019;10:1107. doi:10.3389/fgene.2019.01107
22. Shi X, Wu X. An overview of human genetic privacy. Ann N Y Acad Sci. 2017;1387(1):61–72. doi:10.1111/nyas.13211
23. Ibrahim MA, Alshogran OY, Khabour OF, Alzoubi KH. The quality of consent form structure in biomedical research: a study from Jordan and Sudan. J Multidiscip Healthc. 2019;12:727–731. doi:10.2147/JMDH.S219316
24. Nyika A. Ethical and practical challenges surrounding genetic and genomic research in developing countries. Acta Trop. 2009;112(Suppl 1):S21–S31. doi:10.1016/j.actatropica.2009.07.034
25. McGuire AL, Beskow LM. Informed consent in genomics and genetic research. Annu Rev Genomics Hum Genet. 2010;11:361–381. doi:10.1146/annurev-genom-082509-141711
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
