Back to Journals » Open Access Emergency Medicine » Volume 11
Improving fluid resuscitation in pediatric shock with LifeFlow®: a retrospective case series and review of the literature
Authors Piehl M , Smith-Ramsey C , Teeter WA
Received 19 September 2018
Accepted for publication 28 February 2019
Published 24 April 2019 Volume 2019:11 Pages 87—93
DOI https://doi.org/10.2147/OAEM.S188110
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Hans-Christoph Pape
Mark Piehl,1–4 Cherrelle Smith-Ramsey,5 William A Teeter5
1Department of Pediatrics, Division of Pediatric Critical Care, WakeMed Health and Hospitals, Raleigh, NC, USA; 2410 Medical, Inc, Durham, NC, USA; 3Department of Pediatrics, University of North Carolina School of Medicine, Chapel Hill, NC, USA; 4Department of Pediatrics, Duke University School of Medicine, Durham, NC, USA; 5Department of Emergency Medicine, University of North Carolina School of Medicine, Chapel Hill, NC, USA
Abstract: Rapid delivery of an intravenous fluid bolus is commonly used in pediatric emergency care for the treatment of shock and hypotension. Early fluid delivery targeted at shock reversal results in improved patient outcomes, yet current methods of fluid resuscitation often limit the ability of providers to achieve fluid delivery goals. We report on the early clinical experience of a new technique for rapid fluid resuscitation. The LifeFlow® infuser is a manually operated device that combines a syringe, automatic check valve, and high-flow tubing set with an ergonomic handle to enable faster and more efficient delivery of fluid by a single health care provider. LifeFlow is currently FDA-cleared for the delivery of crystalloid and colloids. Four cases are presented in which the LifeFlow device was used for emergent fluid resuscitation: a 6-month-old with septic shock, a 2-year-old with intussusception and shock, an 11-year-old with pneumonia and septic shock, and a 15-year-old with trauma and hemorrhagic shock.
Keywords: hypotension, sepsis, septic shock, fluid therapy
Introduction
Children who present to the emergency department (ED) with shock have a 5–7% risk of mortality, and each hour of delay in shock reversal results in greater than a twofold increase in the odds of death.1 Children with decompensated shock (prolonged capillary refill plus hypotension) are at the highest risk, with over 30% mortality.1 Earlier fluid delivery targeted at shock reversal results in decreased morbidity,1–3 mortality,1,3–8 and hospital length of stay (LOS).3,7,9–12 For example, in a prospective cohort study evaluating adherence with guideline recommendations for fluid resuscitation in pediatric septic shock, patients for whom all aspects of the protocol were met had a 57% shorter hospital LOS.9 In two retrospective cohort studies of protocolized severe sepsis care, adherence to the protocol resulted in earlier initiation of rapid fluid boluses, a larger total volume of fluid administered in the ED, less organ dysfunction, and shorter pediatric intensive care unit and hospital LOS.2,3 In a separate study of a sepsis quality improvement initiative, a sepsis bundle was initiated that included intravenous (IV) fluid boluses directed at the rapid reversal of shock.7 The odds of death in this study were five times higher in children who did not receive bundle-compliant care.7
Rapid restoration of intravascular volume may be required to correct hypotension and reverse shock in a variety of pediatric emergencies. In children with decompensated shock from conditions such as hypovolemia, sepsis, hemorrhage, and anaphylaxis, cardiovascular collapse may be imminent and rapid fluid bolus therapy is essential.13,14 A variety of methods are currently used for fluid delivery in children, including gravity infusion, IV infusion pumps, pressure bags, mechanical rapid infusers, and the use of manual syringes (the push–pull technique [PPT] or disconnect–reconnect technique [DRT]). Gravity flow is universally slow, and while the addition of a pressure bag inflated to 300 mmHg may modestly speed the infusion rate, this technique requires constant re-inflation to achieve consistently increased speed.15,16 This method also carries the risk of air embolism.17 Infusion pumps deliver a maximum rate of 1,000 mL/hr and can achieve 60 mL/kg over 15 mins only in patients weighing <4 kg, but are still commonly used as a method of fluid bolus delivery.9,12 With PPT and DRT, providers may be able to achieve the guideline-recommended rates of infusion,17,18 but these methods are complex and labor-intensive, and both techniques may introduce bacterial contamination into the sterile stopcock.19–22 Mechanical rapid infusers are expensive, require highly trained staff, tend to be located only in larger EDs, and function best with large-gauge IV catheters. Finally, with most of these methods it may be difficult to quickly and efficiently deliver an accurate 10–20 mL/kg fluid bolus, quickly reassess patient response, and deliver an additional bolus if necessary.
LifeFlow is a novel, FDA-cleared device for delivering measured boluses of crystalloids and colloids. The device packages a 10 mL spring-loaded syringe, large-bore inlet tubing, and an automatic check valve into a lightweight ergonomic device which facilitates rapid, controlled fluid delivery by a single health care provider (Figure 1). In a simulation study comparing flow through common IV gauges, LifeFlow facilitated infusion two to four times as fast as standard techniques. (Figure 2).23 The device can be setup quickly in emergency situations, and may help avoid the nosocomial infection risks associated with PPT.19–22
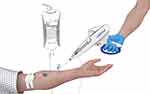 | Figure 1 LifeFlow® device. |
 | Figure 2 Speed comparison (mL/min) for IV-gauge size vs rapid fluid infusion method. |
In a recent study of LifeFlow at Yale New Haven Children’s Hospital, teams of providers were asked to treat a simulated 10 kg patient with septic shock. For the fluid resuscitation element of the scenario, teams were randomized to LifeFlow, PPT, and pressure bag for the delivery of three 20 mL/kg boluses of fluid. Completion of the 60 mL/kg of fluid was fastest with the LifeFlow device, and participants judged the complexity of fluid delivery to be the lowest with LifeFlow, as measured by the National Aeronautical and Space Administration Task Load Index (NASA-TLX).24 In a similar study, individual nurse and paramedic providers were asked to provide all patient care tasks for an adult-sized patient with septic shock, including assessment, fluid delivery, antibiotics, and documentation. Time to completion of three 500 mL fluid boluses required 7.8 mins with LifeFlow, compared to 20 mins with a pressure bag, and completion of all patient care tasks took 50% longer when a pressure bag was used as the infusion method (22.8 vs 36.3 mins).25
The following case series illustrates the use of LifeFlow in children with shock resulting from a variety of emergency conditions. In each of these diverse cases, the patient received early and rapid fluid resuscitation, resulting in significant hemodynamic improvement. All patients subsequently experienced full recovery and were discharged home with no further sequelae.
The reporting of these cases has been approved by the WakeMed Institutional Review Board, Raleigh, NC. The parents of each patient have given written and informed consent to allow the publication of patient case details.
Cases
Case 1
A 6-month-old boy with a 2-day history of viral symptoms was found to be gray and unresponsive in his crib. The caregiver started cardiopulmonary resuscitation and called 911. Emergency medical services (EMS) found patient to be mottled and unresponsive with a heart rate (HR) of 230 beats per minute (BPM) and a palpable pulse. An IV catheter was inserted, and two doses of adenosine were given for presumed supraventricular tachycardia (SVT) without effect. On arrival to the ED, the HR was 245 BPM and he remained unresponsive, with a capillary refill time of >4 s. After a third dose of adenosine was administered, the IV catheter infiltrated and several additional attempts were made to establish IV access. He then developed apparent seizure activity, with eye deviation and symmetric twitching of all extremities. Bedside ultrasound revealed a hyperdynamic heart with subjectively increased heart function and complete inspiratory collapse of the inferior vena cava (IVC). An arterial blood gas showed a pH of 6.7 and lactate of 9 mmol/L. Due to these findings and HR variability, the presumed diagnosis was changed from SVT to septic shock. After IV access was re-established, a bolus of 40 mL/kg of normal saline was infused with LifeFlow through a 22-gauge IV catheter in the right antecubital vein in <5 mins. This led to an immediate decrease in HR to 170 BPM. He was subsequently electively intubated due to shock, altered mental status, and presumed seizures. An additional 160 mL/kg of normal saline was infused with LifeFlow in 40 mL/kg increments, after which he achieved improved perfusion and stable vital signs. No vasopressors were required. Lactate decreased to <2 mmol/L in 4 hrs, and serum creatinine decreased from 1.1 to 0.4 mg/dL within 12 hrs. He was extubated within 48 hrs and was neurologically normal. He was subsequently diagnosed with hemophagocytic lymphohistiocytosis and septic shock.
Case 2
A 2-year-old previously healthy girl was brought to the ED with emesis, lethargy, and fever. Approximately 30 mins prior to arrival at the ED, she had presented to urgent care with a 2-day history of vomiting and poor oral intake. Because of her ill appearance, she was transported to the ED by EMS. No IV access could be obtained en route. On arrival to the ED, she was noted to be pale and lethargic. Her initial vital signs were temperature, 101.8°F; HR, 224 BPM; respiratory rate (RR), 57 breaths per minute; blood pressure (BP), 109/65 mmHg; and O2 saturation of 97% saturation on room air. She did not open eyes or withdraw to the painful stimulus of two IV cannulation attempts. Her skin was cool and mottled, capillary refill time was >3 s, and mucous membranes were dry. A 22 gauge IV catheter was placed in her left hand and two boluses of 250 mL normal saline (20 mL/kg each) were given via LifeFlow, each over approximately 90 s. Her HR decreased to 178 BPM with first bolus, and 162 BPM with the second. Capillary refill time improved to <2 s, BP Increased to 143/93 mmHg, RR decreased to 43 breaths per minute, and O2 saturation remained 100% on 2 L of oxygen. Mental status improved and she began responding to parents. Abdominal ultrasound revealed intussusception, and she was taken directly to the operating room in stable condition. She was found to have ileo-ileocolic intussusception, with poorly perfused but viable bowel due to a Meckel’s diverticulum, which was resected. She was admitted to the inpatient ward and subsequently discharged within 2 days.
Case 3
An 11-year-old previously healthy girl presented to the ED with fever of 106°F, cough, and left flank pain. Vital signs on arrival were temperature, 100.8°F; HR, 137 BPM; RR, 22 breaths per minute; BP, 83/44 mmHg. She received 20 mL/kg normal saline over 1 hr by infusion pump. Chest x-ray was negative for pneumonia. Renal ultrasound was also normal. White blood cell count was 22,000, and urinalysis showed moderate ketones. One hour after the initial fluid bolus she developed fever to 101.7°F and again became hypotensive to 84/47 mmHg. She received an additional 20 mL/kg normal saline over 1 hr via infusion pump, with only modest improvement in BP and HR. She then again developed tachycardia, tachypnea, and hypotension, with a BP of 73/35 mmHg. The patient became difficult to arouse, and O2 saturation dropped to 84%. High-flow nasal cannula oxygen was started at 15 L per minute. Bedside ultrasound demonstrated a left lower lobe pneumonia with small effusion, normal heart function, and complete inspiratory collapse of the IVC. A bolus of 500 mL normal saline was infused using LifeFlow through a 20-gauge IV catheter in approximately 2 mins. She subsequently became more alert, HR decreased to 109 BPM, and BP increased to 92/42 mmHg. Systolic BP again declined to 85 mmHg 30 mins later. IVC ultrasound demonstrated minimal inspiratory collapse, suggesting no further fluid boluses were required. A norepinephrine infusion was started and additional fluid was administered at maintenance rate via infusion pump. Within 12 hrs, she no longer required oxygen and was weaned from norepinephrine within 72 hrs. Repeat chest x-ray demonstrated a left lower lobe pneumonia, and she was treated with an antibiotic course for pneumonia and sepsis.
Case 4
A 15-year-old boy was an unrestrained passenger in the rear seat of a vehicle which struck a tree at high speed. He was found outside of the vehicle and was transported to the ED by EMS. On arrival to the ED, he was moaning and had a Glasgow Coma Scale of 8, facial abrasions, bleeding from both ears, diminished breath sounds on the left, cool extremities, and palpable pulses. Initial vital signs were HR, 141 BPM; RR, 35 breaths per minute; BP 140/69 mmHg; and O2 saturation, 81%. He was immediately intubated. Chest x-ray and focused assessment with ultrasound for trauma exam revealed hemothorax with tension pneumothorax on the left. Needle decompression was performed and a thoracostomy tube was placed with the return of fresh blood. He became hypotensive with a BP of 71/51 mmHg. Two liters of normal saline were infused by LifeFlow through a left antecubital 18-gauge IV catheter, each over approximately 5 mins, with an increase in BP to 110/56 mmHg. He was transported to the pediatric intensive care unit and did not require blood transfusion until hospital day 3. Additional injuries included traumatic brain injury with temporal bone fracture, rib fractures, and pulmonary contusion. He made a complete recovery and was discharged within two weeks.
Discussion
In each of the cases presented is this report, a child with shock required emergent fluid resuscitation to restore tissue perfusion, minimize end-organ injury, and prevent cardiovascular collapse. In several cases, the rapid reversal of hypotension may have prevented additional procedures, including the need for vasopressors or emergent endotracheal intubation. This in turn may have further decreased subsequent complications, as emergency intubation may exacerbate hypotension and hypoxemia, which are the most common risk factors for post-intubation cardiac arrest.11,26 The patients in this case series received a wide range of fluid volumes, from 10 mL/kg up to 200 mL/kg, and clinical response to the fluid bolus was immediately detected by improvements in vital signs, mental status, and/or skin perfusion. One patient had previously received a large volume of fluid via infusion pump and yet needed additional rapid fluid resuscitation for recurrent hypotension. All patients had good outcomes, and none developed clinically evident pulmonary edema or volume overload.
The Pediatric Advanced Life Support (PALS) Provider Manual specifically calls for a 20 mL/kg fluid bolus to be given over 5 mins for severe shock with hypovolemia or hypotension, noting that “early recognition and rapid intervention are critical to halting the progression from compensated shock to hypotensive shock to cardiopulmonary failure and cardiac arrest.”17 Similarly, the American College of Critical Care Medicine (ACCM) guidelines specify that 20 mL/kg of crystalloid fluid be administered within 5 mins of the recognition of septic shock and establishment of vascular access.18 Both resources advise that repeated 20 mL/kg fluid boluses be administered until tissue perfusion is restored, with careful reassessment after each bolus to ensure there are no signs of volume overload. When cardiogenic shock is suspected, smaller bolus volumes are recommended, with careful monitoring for rales and hepatomegaly or objective evidence of volume overload by bedside ultrasound.18
A number of barriers lead to inadequate resuscitation in pediatric shock. In fact, the PALS Provider Manual cautions clinicians that inadequate and delayed administration of fluids is common and should be carefully avoided.17 This is supported by studies showing that fluid administration guidelines are often not achieved.9,27 In one large academic center, perfect adherence to ACCM guidelines was achieved in 11% of children presenting with septic shock, and a modified goal of 60 mL/kg over 1 hr was achieved in only 37% of patients.9 Similarly, two simulation studies conducted with over 50 multidisciplinary teams across 30 EDs showed that teams were able to achieve 60 mL/kg of fluid resuscitation in 15 mins in approximately only half of the cases.28,29
Perhaps the most common early barriers to effective fluid resuscitation are the recognition of shock and establishment of vascular access.30 Once shock is recognized, lack of knowledge of fluid resuscitation guidelines and technical limitations of fluid delivery often delay adequate resuscitation.28,31 Current methods of fluid resuscitation, including gravity infusion, IV infusion pumps, pressure bags, and manual syringe techniques, all have drawbacks that limit the ability of providers to achieve fluid delivery goals.15,16,32,33
Another factor limiting effective early resuscitation may be the recent literature suggesting harm from fluid bolus therapy,34,35 leading to arguments against the use of early fluid bolus therapy in both adult and pediatric septic shock.36,37 The applicability of these studies to emergency pediatric care in the developed world has been questioned and their results should be interpreted with caution, though they have been used to argue against the use of early fluid bolus therapy in both adult and pediatric septic shock guidelines.36,37 The most well known of these is the FEAST trial, which randomized children in sub-Saharan Africa with severe febrile illness to fluid bolus therapy vs no fluid bolus. Children who received fluid boluses had increased mortality at 48 hrs. However, it is important to note that children with hypotension were not randomized to the no-bolus arm.34 In addition, approximately 60% of children were positive for malaria, 30% had severe anemia with hemoglobin <5 mg/dL, and supportive therapies such as high-flow nasal cannula oxygen, mechanical ventilation, and intensive care facilities were not available. For all of these reasons, the results of these studies should be interpreted with caution and are likely not applicable to the resuscitation of decompensated shock in the developed world. A more recent trial by Sankar et al showed an increased rate of mechanical ventilation among children who received their initial fluid bolus over 15 mins. However, this study had a number of methodologic limitations. Investigators enrolled children with low to moderate severity of illness, had a low threshold to determine the need for mechanical ventilation, did not use objective measures of intravascular volume.35,38 This study actually showed a trend toward decreased mortality in children who received fluids more rapidly.35
Conclusion
While the appropriate timing and volume of fluids for children with sepsis remain a matter of debate, and several ongoing trials are attempting to study this question,39,40 it is widely accepted that children with decompensated shock and hypotension require rapid restoration of intravascular volume. The available evidence suggests that earlier reversal of shock improves patient outcomes, and pediatric septic shock guidelines continue to recommend early recognition and treatment with IV fluids.
Given the current barriers to early and rapid fluid administration in critically ill patients, a new technique that offers improved speed, efficiency, and control of volume infused has the potential to improve outcomes. This case series demonstrates that the LifeFlow device can be safely and effectively used to reverse shock due to a variety of conditions, potentially reducing the need for further interventions, such as additional fluid bolus therapy, vasopressors, central venous catheters, and endotracheal intubation. The LifeFlow device improves upon standard techniques for the delivery of targeted rapid fluid resuscitation therapy. This device improves the speed and efficiency of care for children with sepsis and other forms of shock, potentially reducing the mortality, morbidity, and cost associated with these conditions. Prospective trials are currently underway to further evaluate the effects of this fluid resuscitation technique.
Disclosure
Mark Piehl is the inventor of the LifeFlow device discussed in this manuscript, is a shareholder, the Chief Medical Officer, and Co-Founder of 410 Medical, Inc., reports a salary from the company, and has a patent issued: 15/612,709; he reports no other conflicts of interest in this work. The other authors report no conflicts of interest in this work.
References
1. Carcillo JA, Kuch BA, Han YY, et al. Mortality and functional morbidity after use of PALS/APLS by community physicians. Pediatrics. 2009;124:500–508. doi:10.1542/peds.2008-1967
2. Balamuth F, Weiss SL, Fitzgerald JC, et al. Protocolized treatment is associated with decreased organ dysfunction in pediatric severe sepsis. Pediatr Crit Care Med. 2016;17:817–822. doi:10.1097/PCC.0000000000000858
3. Akcan Arikan A, Williams EA, Graf JM, Kennedy CE, Patel B, Cruz AT. Resuscitation bundle in pediatric shock decreases acute kidney injury and improves outcomes. J Pediatr. 2015;167:1301–1305 e1301. doi:10.1016/j.jpeds.2015.08.044
4. Carcillo JA, Davis AL, Zaritsky A. Role of early fluid resuscitation in pediatric septic shock. JAMA. 1991;266:1242–1245.
5. Han YY, Carcillo JA, Dragotta MA, et al. Early reversal of pediatric-neonatal septic shock by community physicians is associated with improved outcome. Pediatrics. 2003;112:793–799.
6. Oliveira CF, Nogueira de Sa FR, Oliveira DS, et al. Time- and fluid-sensitive resuscitation for hemodynamic support of children in septic shock: barriers to the implementation of the American College of Critical Care Medicine/Pediatric Advanced Life Support Guidelines in a pediatric intensive care unit in a developing world. Pediatr Emerg Care. 2008;24:810–815. doi:10.1097/PEC.0b013e31818e9f3a
7. Lane RD, Funai T, Reeder R, Larsen GY. High reliability pediatric septic shock quality improvement initiative and decreasing mortality. Pediatrics. 2016;138:e20154153.
8. Leisman D, Wie B, Doerfler M, et al. Association of fluid resuscitation initiation within 30 minutes of severe sepsis and septic shock recognition with reduced mortality and length of stay. Ann Emerg Med. 2016;68:298–311. doi:10.1016/j.annemergmed.2016.02.044
9. Paul R, Neuman MI, Monuteaux MC, Melendez E. Adherence to PALS sepsis guidelines and hospital length of stay. Pediatrics. 2012;130:e273–e280. doi:10.1542/peds.2012-0094
10. Larsen GY, Mecham N, Greenberg R. An emergency department septic shock protocol and care guideline for children initiated at triage. Pediatrics. 2011;127:e1585–e1592. doi:10.1542/peds.2010-3513
11. Long E, Sabato S, Babl FE. Endotracheal intubation in the pediatric emergency department. Paediatr Anaesth. 2014;24:1204–1211. doi:10.1111/pan.12490
12. Moresco BL, Woosley C, Sauter M, Bhalala U. Poor compliance with sepsis guidelines in a tertiary care children’s hospital emergency room. Front Pediatr. 2018;6:53. doi:10.3389/fped.2018.00053
13. Fuchs CS, Tomasek J, Yong CJ, et al;
14. Martin K, Weiss SL. Initial resuscitation and management of pediatric septic shock. Minerva Pediatr. 2015;67:141–158.
15. Reddick AD, Ronald J, Morrison WG. Intravenous fluid resuscitation: was Poiseuille right? Emerg Med J. 2011;28:201–202. doi:10.1136/emj.2009.083485
16. Stoner MJ, Goodman DG, Cohen DM, Fernandez SA, Hall MW. Rapid fluid resuscitation in pediatrics: testing the American College of Critical Care Medicine guideline. Ann Emerg Med. 2007;50:601–607. doi:10.1016/j.annemergmed.2007.06.482
17. Chameides L, Samson RA, Schexnayder S, Hazinski MF, editors. Pediatric Advanced Life Support Provider Manual. Dallas (TX): American Heart Association; 2016.
18. Davis AL, Carcillo JA, Aneja RK, et al. American College of Critical Care Medicine clinical practice parameters for hemodynamic support of pediatric and neonatal septic shock. Crit Care Med. 2017;45:1061–1093. doi:10.1097/CCM.0000000000002425
19. Blogg CE, Ramsay MA, Jarvis JD. Infection hazard from syringes. Br J Anaesth. 1974;46:260–262.
20. Olivier LC, Kendoff D, Wolfhard U, Nast-Kolb D, Nazif Yazici M, Esche H. Modified syringe design prevents plunger-related contamination–results of contamination and flow-rate tests. J Hosp Infect. 2003;53:140–143.
21. Loftus RW, Brown JR, Koff MD, et al. Multiple reservoirs contribute to intraoperative bacterial transmission. Anesth Analg. 2012;114:1236–1248. doi:10.1213/ANE.0b013e31824970a2
22. Spangler H, Lane A, Piehl M, Robertson G. Improving septic technique during the treatment of pediatric septic shock: a comparison of two rapid fluid delivery methods. J Infus Nurs. 2018;42(1):23–28. doi:10.1097/NAN.0000000000000307
23. Robertson G, Lane A, Piehl M, Whitefill T, Spangler H. Comparison of a novel rapid fluid delivery device to traditional methods. Available from:
24. Kline M, Crispino L, Bhatnagar A, Panchal RA, Auerbach M. A randomized single-blinded simulation-based trial of a novel method for fluid administration to a septic infant. Pediatr Emerg Care. 2018. doi:10.1097/PEC.0000000000001583
25. Piehl M, Spangler H, Robertson G, Chenet K. A novel technique for improving fluid resuscitation in septic shock. Ann Emerg Med. 2017;70:S150. doi:10.1016/j.annemergmed.2017.07.353
26. De Jong A, Rolle A, Molinari N, et al. Cardiac arrest and mortality related to intubation procedure in critically Ill adult patients: a multicenter cohort study. Crit Care Med. 2018;46:532–539. doi:10.1097/CCM.0000000000002925
27. Inwald DP, Tasker RC, Peters MJ, Nadel S;
28. Auerbach M, Whitfill T, Gawel M, et al. Differences in the quality of pediatric resuscitative care across a spectrum of emergency departments. JAMA Pediatr. 2016;170:987–994. doi:10.1001/jamapediatrics.2016.1550
29. Kessler DO, Walsh B, Whitfill T, et al;
30. Thompson GC, Macias CG. Recognition and management of sepsis in children: practice patterns in the emergency department. J Emerg Med. 2015;49:391–399. doi:10.1016/j.jemermed.2015.03.012
31. Paul R, Melendez E, Stack A, Capraro A, Monuteaux M, Neuman MI. Improving adherence to PALS septic shock guidelines. Pediatrics. 2014;133:e1358–e1366. doi:10.1542/peds.2013-3871
32. Cole ET, Harvey G, Urbanski S, Foster G, Thabane L, Parker MJ. Rapid paediatric fluid resuscitation: a randomised controlled trial comparing the efficiency of two provider-endorsed manual paediatric fluid resuscitation techniques in a simulated setting. BMJ Open. 2014;4:e005028. doi:10.1136/bmjopen-2014-005028
33. Toshniwal G, Ahmed Z, Sengstock D. Simulated fluid resuscitation for toddlers and young children: effect of syringe size and hand fatigue. Paediatr Anaesth. 2015;25:288–293. doi:10.1111/pan.12573
34. Maitland K, Kiguli S, Opoka RO, et al;
35. Sankar J, Ismail J, Sankar MJ, Suresh CP, Meena RS. Fluid bolus over 15–20 versus 5–10 minutes each in the first hour of resuscitation in children with septic shock: a randomized controlled trial. Pediatr Crit Care Med. 2017;18:e435–e445. doi:10.1097/PCC.0000000000001269
36. Gelbart B, Glassford NJ, Bellomo R. Fluid bolus therapy-based resuscitation for severe sepsis in hospitalized children: a systematic review. Pediatr Crit Care Med. 2015;16:e297–e307. doi:10.1097/PCC.0000000000000507
37. Marik PE, Malbrain M. The SEP- 1quality mandate may be harmful: how to drown a patient with 30 mL per kg fluid! Anaesthesiol Intensive Ther. 2017;49:323–328. doi:10.5603/AIT.a2017.0056
38. Russell MJ, Kanthimathinathan HK. Is there an optimum duration of fluid bolus in pediatric septic shock? a critical appraisal of “Fluid Bolus over 15–20 versus 5–10 mins each in the first hour of resuscitation in children with septic shock: a randomized controlled trial” by Sankar et al (Pediatr Crit Care Med 2017; 18: e435–e445). Pediatr Crit Care Med. 2018;19:369–371. doi:10.1097/PCC.0000000000001459
39. O’Hara CB, Canter RR, Mouncey PR, et al. A qualitative feasibility study to inform a randomised controlled trial of fluid bolus therapy in septic shock. Arch Dis Child. 2018;103:28–32. doi:10.1136/archdischild-2016-312515
40. Parker MJ, Thabane L, Fox-Robichaud A, Liaw P, Choong K;
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
