Back to Journals » Neuropsychiatric Disease and Treatment » Volume 10
Improvement of gross motor and cognitive abilities by an exercise training program: three case reports
Authors Alesi M, Battaglia G , Roccella M, Testa D, Palma A, Pepi A
Received 29 November 2013
Accepted for publication 13 January 2014
Published 14 March 2014 Volume 2014:10 Pages 479—485
DOI https://doi.org/10.2147/NDT.S58455
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Marianna Alesi,1 Giuseppe Battaglia,2 Michele Roccella,1 Davide Testa,1 Antonio Palma,2 Annamaria Pepi1
1Department of Psychology, 2Department of Law, Social and Sport Science, University of Palermo, Palermo, Italy
Background: This work examined the efficacy of an integrated exercise training program (coach and family) in three children with Down syndrome to improve their motor and cognitive abilities, in particular reaction time and working memory.
Methods: The integrated exercise training program was used in three children with Down syndrome, comprising two boys (M1, with a chronological age of 10.3 years and a mental age of 4.7 years; M2, with a chronological age of 14.6 years and a mental age of less than 4 years) and one girl (F1, chronological age 14.0 years and a mental age of less than 4 years).
Results: Improvements in gross motor ability scores were seen after the training period. Greater improvements in task reaction time were noted for both evaluation parameters, ie, time and omissions.
Conclusion: There is a close interrelationship between motor and cognitive domains in individuals with atypical development. There is a need to plan intervention programs based on the simultaneous involvement of child and parents and aimed at promoting an active lifestyle in individuals with Down syndrome.
Keywords: disability, Down syndrome, gross motor abilities, cognitive abilities, physical activity
Introduction
Children with intellectual disabilities (ID) can show impaired development in a number of areas, such as cognitive, motor, adaptive, social, and emotional domains. For some years now, theories of intellectual disabilities have been taking an approach centered on a more complete description of development in individuals with ID, known as “the whole-child approach”,1 in which emphasis is placed on all the factors that characterize atypical development. In line with this perspective, there is good agreement among theorists that sport and leisure can play a crucial role in promoting well-being and social integration among children and adolescents with intellectual or functional disabilities2,3 and in elderly people.4,5 Recent studies support the hypothesis that regular physical activity is associated with improved reaction time6 and better working memory in children with ID.7 The literature to date supports a causal link between regular physical activity and brain development, particularly in the prefrontal cortical area. In more depth, physical activity could act by enhancing the production of neurotrophins aimed at controlling survival, growth, and differentiation of neurons, synaptogenesis, and angiogenesis, with consequent improvement in areas of cognitive performance, such as speed of processing, planning and control strategies, and working memory.8,9
However, little information is available on the structure of intervention programs aimed at simultaneously ameliorating motor and cognitive skills. Shin and Park10 undertook a meta-analysis to examine the effects of motor programs in individuals with intellectual disabilities. In summary, short-duration interventions (31–60 minutes) and programs running four times per week appeared to be the most effective. Moreover, the efficacy of the above-mentioned programs seems to be influenced by personal characteristics, such as age and level of ID. Younger individuals and those with borderline ID improve more than those with a mild level of ID after specific motor training. However, although there is good agreement among theorists that children with ID can benefit from physical programs, many barriers to involvement have been observed for persons with ID. One of the most significant barriers appears to be sedentary lifestyles associated with a lack of motivation and difficulty in maintaining a planned sporting activity protocol for adequate periods of time.11 On the other hand, involvement and participation in organized sporting activities is limited in people with ID by environmental factors, including accessibility of the gym, lack of expert teachers and coaches, and limited availability of training.12 These factors are often associated with other familiar barriers, ranging from dependence on transportation to beliefs regarding restrictive medical conditions linked to the specific disability or prejudices regarding reduced physical and behavioral skills. In the long term, all these factors can encourage overprotection on the part of families towards their children with ID and decrease or limit participation in sporting activity.13
In light of these theoretical considerations, the goal of this pilot study was to examine the efficacy of an integrated exercise training program (coach and family) in three children with Down syndrome in order to improve their motor and cognitive abilities, including reaction time and working memory. Children with Down syndrome were chosen because of their typically greater limitations in the verbal than visuospatial components of working memory and consequent poorer working memory performance in verbal tasks.14,15
Specifically, impaired memory is connected to abnormalities in the electrophysiological process of “long-term potentiation” in the dentate gyrus of the hippocampus and a reduced number of synapses.14 In turn, these developmental abnormalities of the nervous system contribute to neuronal degeneration.16 There is evidence from mouse models that a combination of physical exercise and environmental enrichment, a condition of augmented sensorimotor stimulation, decreases cortical inhibition and improves memory skills by increasing cell proliferation, neurogenesis, and gliogenesis in the hippocampus.17 Transgenic mouse models of Down syndrome have been generated by triplications of different segments of the murine chromosome,16 which has a large degree of synteny with human chromosome.21 Similarities were found between individuals with Down syndrome and the Ts65Dn murine model regarding a significantly reduced brain size and smaller cerebellum. In particular, the reduction in brain volume is closely linked to hypoplasia of the hippocampus, cerebral cortex, and white matter, with a significant reduction in the number of neuronal cells.18,19
The aim of this pilot study was to assess the improvement in gross motor and cognitive ability, such as reaction time and working memory, following an integrated exercise training program (coach and family) in three children with Down syndrome and mild to severe ID. It was expected that treatment would result in significantly more gross motor and cognitive improvements in children with a lower level of ID. We used a single-subject study design in which subjects served as their own controls, because such designs are used primarily to evaluate the effect of a variety of interventions in applied and clinical research. Moreover, these designs are more sensitive to individual differences than group designs, which are mainly sensitive to differences in group means.
Materials and methods
Subjects
The participants were three children with Down syndrome, of whom two were boys and one was a girl. The first boy (M1) had a chronological age of 10.3 years and a mental age of 4.7 years. The second boy (M2) had a chronological age of 14.6 years and a mental age of less than 4 years. The girl (F1) had a chronological age of 14.0 years and a mental age of less than 4 years. The first child had mild ID and the other two children had severe ID. All three subjects had been engaged in structured speech therapy and psychomotor activity from early childhood. The children did not attend any additional physical activity programs in or out of school.
All three subjects were from average socioeconomic backgrounds and attended primary school. They were recruited through a not-for-profit association that provides support and community resources for people with Down syndrome and their families (Associazione Famiglie Persone Down, Palermo, Italy). Members of the organization were invited to meet with researchers to become familiar with the goals of the study and its procedures. Prior to the start of the study, appropriate local ethics committee approval was obtained from the University of Palermo and written informed consent was provided by each participant’s caregiver.
Methods
Our experimental design included: a preliminary evaluation (T0) determining chronological and mental age, body weight, height, gross motor skills, working memory, and attention skills; a baseline evaluation (T1) after 2 months in which subjects were familiarized with the main exercises of the training protocol and with the coach, and were assessed for gross motor development, working memory, and attention tasks; the exercise training program; and a post-test evaluation (T2) after 2 months of training in which anthropometric measurements and tests for gross motor development, working memory, and attention were repeated.
Anthropometric measurements
Height and body weight were measured according to the standard practices recommended at the Airlie conference.20 Height was assessed using a stadiometer (maximum height recordable, 220 cm; resolution, 1 mm) with the subjects barefoot and standing upright. Body weight was measured using a Seca electronic scale (maximum weight recordable, 300 kg; resolution, 100 g; Seca Deutschland, Hamburg, Germany). Body mass index was calculated as body weight divided by height squared (kg/m2).
Assessment of mental age
The Organizzazioni Logiche (OL) test21 was administered to the participants in order to determine their mental age. The OL test consists of 18 items subdivided into three areas of logical operation, ie, ordering, numbering, and classification. Evaluation was binary for each item, with a mark of 1 being attributed to each correct item and 0 to each incorrect item. The raw data thus obtained were then transformed into a measure of mental age (range 4–8 years) using appropriate conversion tables. The OL test shows good validity, with a 0.68 correlation with Wechsler Intelligence Scale and a 0.78 correlation with the Columbia Mental Maturity Scale. The reliability of the OL test is 0.87.
Assessment of gross motor development
The subjects were assessed for locomotor ability and object control skills using a gross motor development test.22 This test investigates two different aspects of gross motor development, ie, locomotion (requiring subjects to run as fast as possible for 15 meters, gallop for ten meters, hop on one leg for five meters, jump forward, do a long jump, and take little jumps forward and laterally) and object control (requiring subjects to catch a ball with a tennis racket, bounce off the ball, catch a ball, kick the ball running, and throw a ball with the hand). The two subtests combined give a quotient of gross motor ability (QSGM). Participants’ performances were videotaped with a digital video camera that allowed us to analyze movement sequences separately and to assign scores. To obtain a higher validity, according to the handbook, the participant was required to repeat the trial three times and a score of 1 was assigned if the subject performed well twice or 0 if the subject was not able to perform the test. The sum of scores obtained for each criterion (maximum total score 48) was transformed into standard scores according to the age level of the child. We evaluated the gross motor development level based on QSGM scores suggested by the manual’s instructions, ie, 35–69 (very low motor ability, VL-MA); 70–79 (low motor ability, L-MA); 80–89 (under average motor ability, UA-MA); 90–110 (average motor ability, A-MA); 111–120 (over average motor ability, OA-MA); 121–130 (high motor ability, H-MA); and 131–165 (very high motor ability, VH-MA). The Cronbach’s alpha coefficient is 0.91 and the correlation coefficient for the test-retest is 0.96.
Assessment of working memory
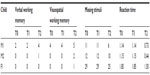
Verbal and visuospatial working memory was assessed by tests derived from working memory tasks.14 One verbal working memory test and one visuospatial working memory test at low level of information processing were administered. The first test, known as “forwards word recall”, consists of a list of eight sequences of words with increasing level of difficulty according to the length of each trial given by the number of words ranging from 2 to 5 units. The first two sequences are composed of two words each and so on until the last two sequences, which are composed of five words each. All the words are two-syllable and characterized by high levels of concreteness and familiarity, such as “mamma (mother), “papa” (father), “cane” (dog), “casa” (house), “palla” (ball), “gatto” (cat), “mela” (apple), and “luna” (moon). The child is required to repeat immediately and in the same order the list of words verbally presented at a rate of one word per second by the experimenter. The test is stopped when the child fails on both lists of the same length. Consequently the score is defined by the number of items correctly remembered. The visuospatial working memory test used was the “memory for positions” in which the child is required to remember within 10 seconds the path with the start and final position of a green frog within cells filled in green on a 3 × 3 or 4 × 4 chessboard. The task consists of eight trials with four levels of difficulty according to the path number to be remembered (from 2 to 4) and the size of the chessboard, ie, 3 × 3 or 4 × 4. Each level has two series of paths. The test is stopped when the child fails on both items of the same difficulty level. The score is then defined by the number of items correctly remembered. The range is 0–8. The Cronbach’s alpha reliability coefficient is 0.70.
Assessment of reaction times
Reaction time was assessed by a simple reaction time task derived from the “Attenzione e Concentrazione” test.23 Using this test, reaction time is measured by the amount of time between the appearance on a computer screen of a stimulus, given by a blue star, and the child’s response. The task comprises 30 stimuli and the child is required to place an index finger on the spacebar key and press the spacebar as fast as possible upon appearance of the stimulus. At the beginning, the experimenter presents the instructions and allows practice trials. Two parameters are evaluated, ie, missing items and reaction time (indicated in seconds). The reliability coefficient of the test is α=0.82.
Exercise training program
Participants in this study, known as male 1 (M1), male 2 (M2), and female 1 (F1), took part in a specific exercise training program which included several exercises to improve their locomotor ability and object control skills. The subjects trained twice a week for a period of 2 months. Training was done in a group setting and based on useful, goal-directed training, practicing specific activities of relevance to the child. Parents were involved in the goal setting process, were active participants in the exercise training, and cooperated with the group leader to carry over the knowledge and skills learned safely, to the child’s everyday life. Each training session (Table 1) lasted about 60 minutes and, in agreement with Battaglia et al, included the following stages:3 a social interaction phase between child, coach, and parents (about 5 minutes) to enhance the motivation to participate; a warm-up period (~5 minutes); a central training period (~40 minutes) including two nursery rhyme games and several activities aimed at improving basic motor abilities such as running, jumping, throwing, and rolling; a cool-down period (~5 minutes); and a feedback phase (~5 minutes) to explore the child’s satisfaction level. Each activity in the central phase was given initially for 6–10 repetitions; the number of sets and repetitions of each exercise was gradually increased when the children were able to perform it with ease. In particular, the workload volume was augmented in weeks 1–3 and in weeks 5–7, increasing the complexity and number of sets and repetitions for several exercises.
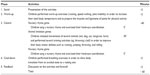  | Table 1 Model of exercise training program |
Results
The children did not show any relevant difference in body weight, height, body mass index, or QSGM after the familiarization period (T0 versus T1). However, all three children showed a decrease in body mass index and an increase in QSGM scores after the training period (T1 versus T2). With regard to gross motor abilities, based on QSGM scores suggested by the manual’s instructions, we found that male subjects increased their gross motor abilities from low to under average (L-MA, UA-MA) to average (A-MA). The female subject improved her QSGM score from very low (VL-MA) to under average (UA-MA) after the exercise period. Specifically, M1, M2, and F1 shifted their QSGM from 85 (UA-MA) to 103 (A-MA), from 79 (L-MA) to 109 (A-MA), and from 46 (VL-MA) to 88 (UA-MA), respectively, after the training program (Table 2 and Figure 1).
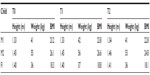  | Table 2 Values for body weight, height, and BMI |
  | Figure 1 Changes on Quotient of Gross-Motor (QSGM) ability for all children. |
With regard to cognitive profile, all measures, including verbal and visuospatial working memory, reaction time and omissions, showed no difference from T0 to T1 for each subject. Global differences were found when we compared pretest (T1) and post-test (T2) measures. In particular, subject M1 showed improvements in verbal and visuospatial working memory from T1 to T2, and his performance score on the “forwards word recall” task improved from 2 to 4. Similarly, his performance score on the “memory for positions” task improved from 4 to 5 for correctly repeated path sequences. Comparison of pretest and post-test results showed greater improvement in reaction time. Reaction time and omissions improved, showing a decrease from T1 to T2. Subject M2 showed less improvement in verbal and visuospatial working memory from T1 to T2. Greater improvements appeared in reaction time from T1 to T2 and in the omissions from T1 to T2. Finally, subject F1 did not show any improvement in verbal working memory from T1 to T2 and only limited improvement in visuospatial working memory from T1 to T2. More consistent was the decrease in reaction time from T1 to T2 nd in missing stimuli from T1 to T2 (Table 3).
Discussion
The aim of this study was to compare improvements in gross motor and cognitive abilities, such as reaction time and working memory, following an integrated exercise training program (coach and family) in three children with Down syndrome and mild to severe ID. Even though all three subjects appeared to show differences from pretest to post-test, the child with mild ID improved more than those with severe ID. This result is consistent with the hypothesis that the efficacy of motor programs is influenced by the severity of ID. Individuals with a lower level of ID are likely to improve more than those with a severe level of ID after specific motor training. Indeed, the impaired intellectual functioning of children with borderline and mild ID appears to be linked to their reduced physical performance.24–26
Specifically, with regard to gross motor abilities, all the children in this study showed improved QSGM scores after the training period. The male subjects increased their gross motor ability from a low to under average level (QSGM score 79–85) to an average level (103–109). However, the female subject improved her QSGM score from 46 (very low motor ability) to 88 (under average motor ability) after the exercise training period. Therefore, following 8 weeks of a specific exercise training program, all three children with Down syndrome were able to improve their gross motor ability. We found that organization of training units in several subphases (social, warm up, central, cool-down, and feedback phase) was a suitable way to improve the children’s participation, with the children attending at least 70%–80% of the training program. In particular, inclusion of a nursery rhyme game before and after the animal imitation games was innovative and original in our study. This phase, which is not included in usual training programs, was introduced to promote motivation and adherence with the training program.
With respect to working memory, also noteworthy are the differences in verbal and visuospatial performance. Visuospatial ability seems to be more sensitive to the beneficial effects of motor training and should improve to a greater extent. This is consistent with other research regarding memory in children with Down syndrome; more specifically, individuals with Down syndrome are reported to have more impairment in verbal than visuospatial components of working memory.14 Therefore, in our study, the visuospatial component would be expected to increase more than the verbal component. This was confirmed by the marked improvement in the memory for positions task shown by all three children. This task is traditionally considered to require the abilities of the ancillary visuospatial subsystem, such as the visuospatial sketchpad, according to Baddeley’s27 tripartite model of working memory.
Differences in the reaction time task from T1 to T2 appeared to be more consistent. All three subjects showed a decrease in the time interval between presentation of the stimulus and the child’s response. This result is consistent with a previous report by Yildirim et al,6 who found that young individuals with ID showed significant improvements in reaction time following a 12-week structured physical fitness training program when compared with a control group. Recent experiments provide evidence of changes in electroencephalographic activity and cognitive task performance in individuals with ID following a moderate running exercise. Specifically, a significant decrease was found in cortical current density in the regions of the frontal lobe, rectal gyrus, medial frontal gyrus, and orbital gyrus.7,9,10
Conclusion
Our results support the hypothesis that motor and intellectual domains are highly interrelated in individuals with atypical development. Moreover, our findings underscore the potential role of movement in cognitive development, starting in infancy. The benefits of regular exercise, such as improved well-being and physical and cognitive health, are also becoming increasingly relevant for individuals with ID. As argued by Hartman et al,24 intervention training directed at increasing ability in individuals with ID may further contribute to decreasing their motor impairment by increasing specific cognitive abilities, such as executive functioning and motor responses in more complex situations. The debate regarding the global approach to individuals with ID stems from the research reported by Ziegler1 and is now supported by the International Classification of Functioning, Disability, and Health.28 This multidimensional perspective points out the close interaction between the individual and context. More specifically, it involves an approach focused on the body, person, and society, which are considered to be the main components characterizing functioning, both in health and in disability.
Moreover, from an educational perspective, our results encourage the development of multifaceted intervention programs based on simultaneous involvement of children and their parents aimed at promoting an active lifestyle in individuals with Down syndrome. Researchers examining caregiver involvement in child play or leisure activities have reported a positive influence of the amount, duration, and complexity of child activities, both in typically developing children and in children with ID. This influences behaviors by providing adequate scaffolding during cooperation which involve more sophisticated behaviors and underlying mental skills resulting in more exploratory and symbolic activity. A positive correlation has been found between the quality of affective parent–child interaction and the exploratory and symbolic skills of children with Down syndrome.29–31 Nevertheless, it is important to emphasize that this is a pilot study based on a small case series and we recognize its shortcomings. First, we did not include a control group with typical development and we did not control for other physical or mental activity. This raises the possibility that some of the changes seen may partially reflect growth and maturation of the children participating in our study. Second, the short-term nature of this study may limit its generalizability. It would be interesting to carry out a follow-up study over 3 or 6 months to assess whether the improvements seen can be maintained. Additional research is needed to examine the effects of this exercise training program in larger samples and in individuals with deficits in other specific domains.
Acknowledgment
The authors thank the Associazione Famiglie Persone Down, Palermo, for its support and assistance during this study, as well as the children involved in the study.
Disclosure
The authors report no conflicts of interest in this work.
References
Ziegler E. The retarded child as a whole person. In: Adams HE, Boardmna WK, editors. Advances in Experimental Child Psychology. New York, NY, USA: Pergamon; 1971;1. | |
Tomporowski PD, Lambourne K, Okumura MS. Physical activity interventions and children’s mental function: an introduction and overview. Prev Med. 2011;52:1–15. | |
Battaglia G, Alesi M, Inguglia M, et al. Soccer practice as an add-on treatment in the management of individuals with a diagnosis of schizophrenia. Neuropsychiatr Dis Treat. 2013;9:595–603. | |
Bellafiore M, Battaglia G, Bianco A, Paoli A, Farina F, Palma A. Improved postural control after dynamic balance training in older overweight women. Aging Clin Exp Res. 2011;23:378–385. | |
Battaglia G, Bellafiore M, Bianco A, Paoli A, Palma A. Effects of a dynamic balance training protocol on podalic support in older women. Pilot study. Aging Clin Exp Res. 2010;22:406–411. | |
Yildirim N, Erbahceci F, Ergun N, Kenneth HP, Beets M. The effect of physical fitness training on reaction time in youth with intellectual disabilities. Percept Mot Skills. 2010;111:178–186. | |
Nagamatsu LS, Chan A, Davis JC, et al. Physical activity improves verbal and spatial memory in older adults with probable mild cognitive impairment: a 6-months randomized controlled trial. J Aging Res. 2013;33:861–893. | |
Best RJ. Effects of physical activity on children’s executive function: contributions of experimental research on aerobic exercise. Dev Rev. 2010;30:331–551. | |
Golubovic S, Maksimovic J, Golubovic B, Glumbic N. Effects of exercise on physical fitness in children with intellectual disability. Res Dev Disabil. 2012;33:608–614. | |
Shin I, Park EY. Meta-analysis of the effect of exercise programs for individuals with intellectual disabilities. Res Dev Disabil. 2012;33:1937–1947. | |
Hutzler Y, Korsensky O. Motivational correlates of physical activity in persons with an intellectual disability: a systematic literature review. J Intellect Disabil Res. 2010;54:767–786. | |
Kristen L, Patriksson G, Fridlund B. Conceptions of children and adolescents with physical disabilities about their participation in a sports programme. European Physical Education Review. 2002;8:139–156. | |
Barr M, Shields N. Identifying the barriers and facilitators to participation in physical activity for children with Down syndrome. J Intellect Disabil Res. 2011;55:1020–1033. | |
Lanfranchi S, Cornoldi C, Vianello R. Verbal and visuospatial working memory deficits in children with Down syndrome. Am J Ment Retard. 2004;109:456–466. | |
Pepi A, Alesi M. Attribution style in adolescents with Down syndrome. European Journal of Special Needs Education. 2005;20:419–432. | |
Rachidi M, Lopes C. Mental retardation and associated neurological dysfunctions in Down syndrome: a consequence of dysregulation in critical chromosome 21 genes and associated molecular pathways. Eur J Paediatr Neurol. 2008;12:168–182. | |
Begenisic T, Spolidoro M, Braschi C, et al. Environmental enrichment decreases GABAergic inhibition and improves cognitive abilities, synaptic plasticity, and visual functions in a mouse model of Down syndrome. Front Cell Neurosci. 2011;5:29. | |
La Grutta S, Lo Baido R, Calì A, Sarno L, Trombini E, Roccella M. People with Down’s syndrome: adolescence and the journey towards adulthood. Minerva Pediatr. 2009;61:305–321. | |
Vecchio D, Salzano E, Vecchio A, Roccella M. A rare unbalanced translocation 1;18 in a child with epilepsy, mild dysmorphology and mental retardation. Minerva Pediatr. 2012;64:365–367. | |
Lohman TG, Roche AF, Martorell R. Anthropometric Standardization Reference Manual. Champaign, IL, USA: Human Kinetics Books; 1988. | |
Vianello R, Marin ML. Organizzazioni Logiche e Conservazione. Dal pensiero intuitivo al pensiero operatorio concreto: prove per la valutazione del livello di sviluppo. [Logical Operations Test]. Bergamo, Italy: Junior; 1997. | |
Ulrich DA. Test of Gross Motor Development. Austin, TX, USA: PRO-ED; 1985. | |
Di Nuovo S. [Attention and Concentration]. Trento, Italy: Erickson; 2000. Italian. | |
Hartman E, Houwen S, Scherder E, Visscher C. On the relationship between motor performance and executive functioning in children with intellectual disabilities. J Intellect Disabil Res. 2010;54:468–477. | |
Bartlo P, Klein PJ. Physical activity benefits and needs in adults with intellectual disabilities: systematic review of the literature. Am J Intellect Dev Disabil. 2011;116:220–232. | |
Biddle SJ, Asare M. Physical activity and mental health in children and adolescents: a review of reviews. Br J Sports Med. 2011;45:886–895. | |
Baddeley AD. Working Memory. Oxford, UK: Clarendon Press; 1986. | |
World Health Organization. International Classification of Functioning, Disability, and Health. Geneva, Switzerland: World Health Organization; 2001. Available from: http://www.who.int/classifications/icf/. | |
De Falco S, Esposito G, Venuti P, Bornstein MH. Mothers and fathers at play with their children with Down syndrome: influence on child exploratory and symbolic activity. J Appl Res Intellect Disabil. 2010;23:597–605. | |
Berktas N, Yanardag M, Yilmaz I, Aras O, Konukman F, Boyaci A. The effects of inclusion class programmes on physical fitness for children with mental challenges. Dev Neurorehabil. 2011;14:389–393. | |
Esposito M, Gimigliano F, Ruberto M, et al. Psychomotor approach in children affected by nonretentive fecal soiling (FNRFS): a new rehabilitative purpose. Neuropsychiatr Dis Treat. 2013;9:1433–1441. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.