Back to Journals » OncoTargets and Therapy » Volume 13
Improvement in Pituitary Imaging After Targeted Therapy in Three Children with BRAF-Mutated Langerhans Cell Histiocytosis with Pituitary Involvement
Authors Yang Y , Wang D, Li N, Ma H, Lian H, Cui L, Zhang Q , Zhao X, Zhang L, Zhao Y, Wang C, Zhang L, Wang T, Li Z, Zhang R
Received 27 August 2020
Accepted for publication 13 November 2020
Published 1 December 2020 Volume 2020:13 Pages 12357—12363
DOI https://doi.org/10.2147/OTT.S279093
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Federico Perche
Ying Yang,1 Dong Wang,1 Na Li,2 Honghao Ma,1 Hongyun Lian,1 Lei Cui,2 Qing Zhang,2 Xiaoxi Zhao,1 Liping Zhang,1 Yunze Zhao,1 Chanjuan Wang,2 Li Zhang,1 Tianyou Wang,1 Zhigang Li,2 Rui Zhang1
1Beijing Key Laboratory of Pediatric Hematology Oncology; National Key Discipline of Pediatrics; Key Laboratory of Major Diseases in Children, Ministry of Education; Hematology Oncology Center, Beijing Children’s Hospital, Capital Medical University, National Center for Children’s Health, Beijing 100045, People’s Republic of China; 2Laboratory of Hematologic Diseases, Beijing Pediatric Research Institute, Beijing Children’s Hospital, Capital Medical University, National Center for Children’s Health, Beijing 100045, People’s Republic of China
Correspondence: Rui Zhang; Tianyou Wang
Beijing Children’s Hospital, Capital Medical University, National Center for Children’s Health, No. 56, Nanlishi Road, Xicheng District, Beijing, People’s Republic of China
Tel +86 010-13691156162
Fax +86 010-59617613
Email [email protected]; [email protected]
Abstract: Langerhans cell histiocytosis (LCH) is a rare myeloid neoplasia in children. BRAF mutations are associated with permanent diabetes insipidus (DI). The onset of clinical DI is always latent with imaging evidence of pituitary involvement. In this study, we reported three children with BRAF-mutated LCH with pituitary involvement who improved after targeted therapy (dabrafenib and trametinib). The results may indicate that pituitary involvement may be reversible in some patients with LCH if it is observed and treated before clinical DI. Targeted therapy may be an effective choice for LCH patients with early pituitary involvement who were irresponsive to first-line or second-line chemotherapy. However, a relapse after targeted therapy is completed in patients with persistently positive cfBRAFV600E mutations is still a challenge that needs to be resolved. The timing of introducing targeted therapy, its appropriate duration and effective combinations with chemotherapy or other targeted drugs should be explored further.
Keywords: Langerhans cell histiocytosis, BRAF mutation, pituitary, children, targeted therapy
Introduction
Langerhans cell histiocytosis (LCH) is a rare myeloid neoplasia. The annual incidence of LCH in children younger than 15 years old is approximately 5 to 9/106.1,2 LCH is more common in children than in adults. The accumulation of pathologic Langerhans cells (LC) in the skin, bone, liver, spleen, bone marrow, central nervous system and so on causes a spectrum of clinical manifestations.
Diabetes insipidus (DI) is a clinical syndrome characterized by polyuria and polydipsia with diluted urine due to the inability to concentrate urine,3 which is a permanent sequela of LCH. It has been reported that the cumulative incidence of DI among patients with LCH is approximately 20% over 10 years (13/70, 5 patients were treated with unspecified treatments, 7 patients with chemotherapy and 1 patient with radiotherapy).4 Some patients develop clinical DI several years after the initial diagnosis of LCH; on the other hand, some patients present with DI several years prior to the diagnosis of LCH.4 The onset of clinical DI is always latent with imaging evidence of pituitary involvement, including infundibular thickening and the lack of a posterior pituitary bright spot on the T1-weighted magnetic resonance imaging (MRI) sequences.5 Long-term use of vasopressin replacement therapy is required once clinical DI occurs.
Pathologic LC is related to activation of the MAPK pathway (RAS/RAF/MEK/ERK). BRAF mutations are found in 50–60% of patients with LCH, while BRAFV600E has been identified as comprising approximately 90% of BRAF mutations and is associated with permanent damage, including pituitary injuries.6 Other BRAF mutations, such as BRAFV600D and BRAFV600insDLAT, have been reported.7
Patients with LCH with central nervous system (CNS) risk lesions appear to be associated with reactivation and are at a high risk of developing permanent sequelae, including neurodegeneration and DI.4 Therefore, before permanent sequelae occur in LCH patients with an affected pituitary, targeted therapy is expected to be effective.6 Both BRAF kinase inhibitors (dabrafenib) and MEK inhibitors (trametinib) have been reported for use in the treatment of LCH patients.8,9 Here, we retrospectively reviewed three children with BRAF-mutated LCH with pituitary involvement who improved after targeted therapy, and we encourage clinicians to focus on the imaging findings of the pituitary and the efficacy of targeted therapy for LCH.
Subjects and Methods
Patients
We retrospectively analyzed all LCH patients who accepted targeted therapy with pituitary involvement (12 patients) and found three patients who had improved pituitary imaging after targeted therapy. The three patients we reported were diagnosed with LCH after histopathological examination with positive staining of CD1a and Langerin (CD207) of the skull (case 1), the shinbone (case 2) and a rash (case 3). BRAF mutations were detected in all of the patients from the biopsied tissues and/or circulation. They were followed up until July 1, 2020.
Study Protocol
All of the patients accepted first-line chemotherapy (vindesine + prednisone) after diagnosis and switched to targeted therapy due to a poor response or intolerance of the chemotherapy (Table 1). The dosages of dabrafenib and trametinib were, respectively, 2 mg/kg per treatment, once every 12 hours, and 0.5 mg per treatment, once every day, administered orally.10 The general duration of the course of the targeted treatment was 6 months to 1 year, adjusted according to the disease assessment and patient tolerance of the drug. If the patients had disease progression, increased or persistently positive cfBRAFV600E levels or severe adverse effects, targeted therapy could be discontinued.
 |
Table 1 Details of Each Patient’s Disease Characteristics |
After targeted therapy was completed, maintenance chemotherapy was given (6-mercaptopurine + vindesine + prednisone) for 0.5–1 year. The affected lesions, pituitary MRI and adverse effects were evaluated after 1 month, 3 months, and every 3 months thereafter, according to the Histiocyte Society LCH Evaluation and Treatment Guidelines.11 During the course of targeted treatment, circulating cell-free BRAFV600E (cfBRAFV600E) in cases 1 and 3 were monitored (using the QX200TM Droplet Digital PCR System (Bio-Rad, Hercules, CA), and cfBRAFV600E levels lower than 0.1% were regarded as negative). Currently, plasma cfBRAFV600D cannot be monitored in our center.
Examinations of Postpituitary Function
The levels of thyroid-stimulating hormone (TSH), adrenocorticotropin (ACTH), gonadotropin hormone (GTH) and prolactin (PRL) were measured in cases 1 and 3 before the targeted therapy. Only TSH was measured in case 2 (the other hormones were not measured). We were unable to measure the levels of antidiuretic hormone (ADH) and oxytocin due to the limitations of the technical conditions in our center. We also measured the amount of fluid intake and urine volume per day, urine specific gravity and serum sodium of all patients before and after targeted treatment.
DI is defined as a clinical syndrome characterized by polyuria (in excess of 2 L/m2/24 h) and polydipsia with diluted urine (urine specific gravity less than 1.005).3 A water deprivation test was not performed for any of the patients because they had no clinical signs or symptoms of DI.
Protocol of the Pituitary MRI
Pituitary MRI was conducted at least twice and the images were evaluated by two experienced radiologists. MRI studies were performed using T1 weighted sequences in the sagittal and coronal planes (repetition time, 500 ms; echo time, 8 ms; flip angle, 90°) on a Philips Achieva TX 3.0T scanner. The slices were 3 mm thick, with a 130 × 130 mm2 field of view and a 256 × 256 matrix. Imaging findings of the pituitary involvement included infundibular thickening, a mass lesion of the hypothalamic-pituitary axis and decreased or disappearing bright spots on the posterior pituitary on T1-weighted images (T1WI).5 The criteria for an improvement in the pituitary findings on MRI included a reappearance of the missing spots or a normalization of the attenuated bright spots. Maximum pituitary brightness using the signal intensity ratio of the neighboring cerebral gray matter was the quantitative evaluation. No contrast was used.
Results
Case 1
This patient was a 2.2-year-old boy diagnosed with multisystem-involved LCH (MS-LCH) with craniofacial involvement, ie, CNS-risk lesions. A lump on his head was the inaugural manifestation. The levels of BRAFV600E in skull biopsies and the plasma at diagnosis were 21.89% and 1.31%, respectively. He had a normal urine volume (less than 2 L/m2/24h) with a normal urine specific gravity and serum sodium. His levels of TSH, ACTH, GTH and PRL were also normal.
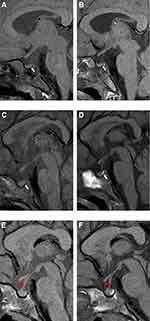
Because of a poor response to first-line chemotherapy (for 13 weeks) on his pituitary imaging (an absence of the normal posterior pituitary bright spot, Figure 1A; the other lesions were in a stable state), dabrafenib treatment was initiated at the age of 3.6, two weeks after completing the chemotherapy. After 3 months of dabrafenib treatment, the bright spot on the posterior pituitary on T1WI recurred with a higher signal intensity ratio compared with the gray matter (Figure 1B), and the other lesions also improved.
During targeted therapy, he experienced a mild skin allergic reaction, but the rash subsided after treatment with anti-allergic drugs. After the 9-month targeted therapy was completed, he was in an active disease (AD)-better state with a clear bright spot on the posterior pituitary on T1WI and then he was switched to second-line chemotherapy (cytarabine + vindesine + dexamethasone) because of being persistently positive for the cfBRAFV600E mutation. Conversion to negative detection of cfBRAFV600E was observed after 4 courses of second-line chemotherapy. At the end of follow-up, all therapy for LCH was terminated, and he was in an AD-better state without any clinical signs or symptoms of DI.
Case 2
In the second patient, MS-LCH was diagnosed at the age of 0.5 without polyuria or polydipsia. Fever was the main manifestation of the patient. Biopsied tissue from the involved shinbone showed BRAFV600D. The amount of fluid intake and urine volume per day, urine specific gravity and serum sodium and TSH (the other hormones were not measured) were measured, which were all at normal levels.
Because of a poor response to first-line chemotherapy (for 5 weeks) on pituitary imaging (an absence of the normal posterior pituitary bright spot, Figure 1C; the other lesions were in AD-better state), dabrafenib treatment was administered two weeks after completion of his chemotherapy. The brightness of the posterior pituitary on T1WI recovered after 1 month of dabrafenib treatment (Figure 1D). No target treatment-related side effects were observed. The duration of his dabrafenib treatment was 12 months. At the end of the observation period, the boy was followed up for 18 months without clinical DI, and no abnormality was observed on pituitary MRI. He has been off LCH treatment in an AD-better state.
Case 3
This patient was also a boy, and the age of his disease onset was 0.2 years. A rash was the initial presentation of the disease. His plasma cfBRAFV600E was 3.29% at diagnosis, but no remaining biopsied rash sample could be acquired for BRAFV600E detection. Before treatment, he also had normal hormone levels, urine volume, urine specific gravity and serum sodium.
After the 6th week of first-line chemotherapy, he developed a progression of his skin lesions and was switched to second-line chemotherapy (cytarabine + vindesine + dexamethasone). However, after 2 courses of second-line chemotherapy, he had a serious infection followed by hemophagocytic lymphohistiocytosis and intolerance of chemotherapy with myelosuppression and gastrointestinal reactions. Therefore, dabrafenib was used alone for 15 months followed by maintenance chemotherapy.
At the 8th month of maintenance therapy, he had new involvement of the pituitary with decreased bright spots on the posterior pituitary on T1WI and infundibular thickening (Figure 1E; his other lesions were in an AD-stable state) and he began to take dabrafenib combined with trametinib.
After a 3-month combination targeted treatment, his pituitary brightness was higher with a recovered infundibulum. His circulating cfBRAFV600E decreased from 0.41% to 0.24%, and his other lesions also improved. At the end of the observation, the boy had taken combination targeted treatment for 10 months and did not experience DI in an AD-better state with clearer bright spots on the posterior pituitary on T1WI and had a recovered infundibulum (Figure 1F). His plasma cfBRAFV600E had decreased to 0.21% at the research endpoint.
Discussion
Due to the high risks of pituitary biopsies, pituitary imaging can be used instead to observe pituitary lesions even if patients do not have evident DI. The bright spot on the posterior pituitary on T1WI is related to vasopressin secretion granules or liposomes in pituitary cells. If pathologic LCs involve the pituitary gland, permanent DI occurs when there is a loss of 80% or more of the hypothalamic magnocellular neurons.12 Imaging findings of pituitary involvement may include infundibular thickening, a mass lesion of the hypothalamic-pituitary axis and decreased or absent bright spots on the posterior pituitary on T1WI.5
In our cases, all patients had BRAF mutations and specific imaging findings of pituitary involvement. The improvement of the pituitary imaging after targeted treatment can also support the early involvement of the pituitary before permanent DI occurs. Moreover, two of them had CNS-risk lesions that had a higher cumulative incidence of DI compared with patients without CNS-risk lesions reported in other studies.4,11
Previous studies have shown that DI is a permanent sequela, and the absence of the normal posterior pituitary bright spot is correlated with a loss of hypophyseal function and it may indicate an early stage of occult local tumors.3,13 Therefore, it is essential to initiate early treatment for patients with CNS-risk lesions and abnormal imaging of pituitary involvement before clinical DI occurs. As BRAF mutations are associated with pituitary involvement and resistance to first-line therapy,6,14 targeted therapy may improve pituitary lesions in BRAF-mutated LCH patients, based on the successful improvement in our cases.
Some LCH patients have persistently positive cfBRAFV600E after targeted therapy, which is associated with a poor prognosis, especially relapses.14 We administered second-line chemotherapy or maintenance chemotherapy after targeted treatment was completed to decrease the level of cfBRAFV600E and reduce the recurrence rate. However, the timing of introducing targeted therapy has not achieved a consensus. Whether earlier administration rather than after first-line chemotherapy is more beneficial and the effectiveness and safety of long-term targeted treatment still need large-scale prospective studies.
Conclusion
In summary, these results may indicate that pituitary involvement may be reversible in some patients with LCH if it is observed and treated before overt clinical DI. Targeted therapy may be an effective choice for LCH patients with early pituitary involvement who are irresponsive to first-line or second-line chemotherapy. However, a relapse after targeted therapy is completed in patients with persistently positive cfBRAFV600E mutations is still a challenge that needs to be resolved. The timing of introducing targeted therapy, its appropriate duration and effective combinations with chemotherapy or other targeted drugs should be explored further.
Abbreviations
AD, active disease; ACTH, adrenocorticotropin; ADH, antidiuretic hormone; CNS, central nervous system; DI, diabetes insipidus; GTH, gonadotropin hormone; LCH, Langerhans cell histiocytosis; LC, Langerhans cells; MRI, magnetic resonance imaging; MS-LCH, multisystem-involved LCH; PRL, prolactin; T1WI, T1-weighted images; TSH, thyroid stimulating hormone.
Data Sharing Statement
The data that support the findings of this study are available on request from the corresponding authors.
Ethics Approval
Written informed consent (including informed consent to have the case details and any accompanying images published) was obtained from the parents or guardians of the children who served as subjects of the study. This study was conducted in accordance with the Declaration of Helsinki and approved by the Institutional Review Board (IRB) of Beijing Children’s Hospital, Capital Medical University (Number: 2019-k-109). The regimen has been registered as a clinical trial (ChiCTR2000032844).
Acknowledgments
This work was supported by the Capital's Funds for Health Improvement and Research (No. 2020-2-2093 and 2020-2-1141), the Special Fund of The Pediatric Medical Coordinated Development Center of Beijing Hospitals Authority (No. XTZD20180201), the National Natural Science Foundation of China (No. 82070202), the National Science and Technology Key Projects (No. 2017ZX09304029004), Beihang University & Capital Medical University Advanced Innovation Center for Big Data-Based Precision Medicine Plan (BHME-201912), and Funding for Reform and Development of Beijing Municipal health Commission (Genetic and immunological pathogenesis of pediatric histiocytosis and its guiding role in clinical diagnosis and treatment).
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Disclosure
The authors declare no conflicts of interest in this work.
References
1. Emile JF, Abla O, Fraitag S, et al. Revised classification of histiocytoses and neoplasms of the macrophage-dendritic cell lineages. Blood. 2016;127(22):2672–2681. doi:10.1182/blood-2016-01-690636
2. Allen CE, Merad M, McClain KL, Longo DL. Langerhans-cell histiocytosis. N Engl J Med. 2018;379(9):856–868. doi:10.1056/NEJMra1607548
3. Di Iorgi N, Napoli F, Allegri AE, et al. Diabetes insipidus–diagnosis and management. Horm Res Paediatr. 2012;77(2):69–84. doi:10.1159/000336333
4. Chow TW, Leung WK, Cheng FWT, et al. Late outcomes in children with Langerhans cell histiocytosis. Arch Dis Child. 2017;102(9):830–835. doi:10.1136/archdischild-2016-312185
5. Kaltsas GA, Powles TB, Evanson J, et al. Hypothalamo-pituitary abnormalities in adult patients with Langerhans cell histiocytosis: clinical, endocrinological, and radiological features and response to treatment. J Clin Endocrinol Metab. 2000;85(4):1370–1376. doi:10.1210/jcem.85.4.6501
6. Heritier S, Emile JF, Barkaoui MA, et al. BRAF mutation correlates with high-risk Langerhans cell histiocytosis and increased resistance to first-line therapy. J Clin Oncol. 2016;34(25):3023–3030. doi:10.1200/JCO.2015.65.9508
7. Durham BH. Molecular characterization of the histiocytoses: neoplasia of dendritic cells and macrophages. Semin Cell Dev Biol. 2019;86:62–76. doi:10.1016/j.semcdb.2018.03.002
8. Kieran MW, Geoerger B, Dunkel IJ, et al. A phase I and pharmacokinetic study of oral dabrafenib in children and adolescent patients with recurrent or refractory BRAF V600 mutation-positive solid tumors. Clin Cancer Res. 2019;25(24):7294–7302. doi:10.1158/1078-0432.CCR-17-3572
9. Arico M. Langerhans cell histiocytosis in children: from the bench to bedside for an updated therapy. Br J Haematol. 2016;173(5):663–670. doi:10.1111/bjh.13955
10. Yang Y, Wang D, Cui L, et al. Effectiveness and safety of dabrafenib in the treatment of 20 Chinese children with BRAFV600E-mutated LCH. Cancer Res Treat. 2020. doi:10.4143/crt.2020.769
11. Histiocyte society LCH evaluation and treatment guidelines [Internet]; 2009. Available from: https://histiocytesociety.org/document.doc?id=290.
12. Bellastella A, Bizzarro A, Colella C, et al. Subclinical diabetes insipidus. Best Pract Res Clin Endocrinol Metab. 2012;26(4):471–483. doi:10.1016/j.beem.2011.11.008
13. Adams NC, Farrell TP, O’Shea A, et al. Neuroimaging of central diabetes insipidus-when, how and findings. Neuroradiology. 2018;60(10):995–1012.
14. Cui L, Zhang L, Ma HH, et al. Circulating cell-free BRAF V600E during chemotherapy is associated with prognosis of children with Langerhans cell histiocytosis. Haematologica. 2020;105(9):e444–447. doi:10.3324/haematol.2019.229187
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.