Back to Journals » International Medical Case Reports Journal » Volume 14
Hypothyroidism and Complicated Sick Sinus Syndrome and Acute Severe Psychiatric Disorder: A Case Report
Authors Huang R, Yan L, Lei Y, Li Y
Received 7 December 2020
Accepted for publication 28 January 2021
Published 19 March 2021 Volume 2021:14 Pages 171—176
DOI https://doi.org/10.2147/IMCRJ.S296071
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Ronald Prineas
Rui Huang,1,* Li Yan,2,* Yuhua Lei,1 Yuanhong Li1
1Cardiovascular Disease Center, Central Hospital of Tujia and Miao Autonomous Prefecture, Enshi Clinical College of Wuhan University, Enshi Prefecture, 445000, Hubei Province, People’s Republic of China; 2Pediatrics Department, Central Hospital of Tujia and Miao Autonomous Prefecture, Enshi Clinical College of Wuhan University, Enshi Prefecture, 445000, Hubei Province, People’s Republic of China
*These authors contributed equally to this work
Correspondence: Yuanhong Li No. 158 Wuyang Avenue, Enshi City, Hubei Province, People’s Republic of China
Email [email protected]
Background: Thyroxine is closely related to cardiovascular diseases, such as coronary heart disease, ventricular arrhythmia, atrioventricular block, myocardial systolic weakness, pericardial effusion, low cardiac output and hypertension. Previous studies have also found that hypothyroidism can also lead to mental disorders. Here, we present a rare case of severe hypothyroidism patient accompanied by sick sinus syndrome (SSS) as a cardiovascular manifestation needing cardiac pacing and severe mental disorders.
Case Presentation: A 42-year-old female patient, previously healthy, was referred to our hospital because of bradycardia complicated with sick sinus syndrome which requiring cardiac pacing and severe mental disorders. Her clinical features along with laboratory findings strongly suggested that the patient had severe hypothyroidism with sick sinus syndrome and mental disorders, both of which were reversible and successfully treated with levothyroxine.
Conclusion: This is the first reported case of hypothyroidism with sick sinus syndrome requiring pacemakers and psychiatric disorders, and the symptoms can be improved and reversed after thyroxine supplementation. This case highlights the importance of hypothyroidism screening when faced with unexplained psychosis or sick sinus syndrome, especially if combined.
Keywords: hypothyroidism, sick sinus syndrome, psychiatric disorder, case report
Background
Thyroxine is closely related to cardiovascular diseases, and in some cases it is recommended that patients with heart diseases should be routinely tested for thyroid function.1 As we all know, cardiovascular complications of severe hypothyroidism include coronary heart disease, ventricular arrhythmia, atrioventricular block, myocardial systolic weakness, pericardial effusion, low cardiac output and hypertension.2 Rarely, hypothyroidism can cause severe sick sinus syndrome requiring pacemaker treatment.2 Previous studies have also found that hypothyroidism can also lead to mental disorders.3,4 We herein report a rare case of hypothyroidism accompanied by sick sinus syndrome (SSS) as a cardiovascular manifestation and severe mental disorders, both of which were reversible and successfully treated with levothyroxine. We present the following case in accordance with the CARE reporting checklist.
Case Presentation
A 42-year-old female patient, previously healthy, was referred to our hospital because of bradycardia complicated with sick sinus syndrome and severe mental disorders. Her chief complaint was “general edema with fatigue for 4 years, aggravation with mental disorder and blackness for 1 month”. The patient developed generalized edema and discomfort 4 years ago, with fatigue and poor spirit, with anorexia, abdominal distension, constipation, with chills, with memory loss, with swelling of the hands and feet, with chest palpitations. One month prior to admission to our hospital, the patient developed black haze, syncope, and serious mental problems, such as auditory hallucinations, persecution delusions, and violent behavior. And she was admitted to the local psychiatric hospital, and considered the acute transient mental disorder: schizophrenia. In the hospital, electrocardiography (ECG) showed severe sinus bradycardia. And then she was referred to our hospital for further evaluation and treatment.
On physical examination, her height, body weight, and body mass index (BMI) were 155.5 cm, 58.4 kg, and 24.1 kg/m2, respectively. The patient had a cold expression, slow response, and rough skin. The heartbeat was 49 beats per minute and the heart rhythm was irregular. The heart sound was weak. There was no pathological murmur in each valve area. The face and limbs were slightly swollen. On psychiatric examination, the patient’s orientation was normal and the answer was to the point. She has auditory hallucinations, relationship delusions, exaggerated delusions, and persecution delusions. No comprehensive perception barrier was introduced. The patient was emotionally indifferent, lacked interest in surroundings. Her intelligence and calculation abilities were normal.
Admitted electrocardiography (ECG) showed significant sinus bradycardia and sinoatrial block (Figures 1 and 2). During hospitalization, electrocardiographic monitoring showed that the patient had frequent cardiac arrest, with a maximum time of 4.5 seconds at 3:20pm on the day of admission (Figure 3). On admission to our department, laboratory findings revealed severe hypothyroidism with a thyroid-stimulating hormone (TSH) level of higher than 98µIU/mL (normal range: 0.49–4.91), free T4 (FT4) of 0.12 ng/dL (normal range: 0.59–1.25), and free T3 (FT3) of 1.90pg/mL (normal range: 2.01–4.81). Antithyroglobulin antibody was negative (normal range: 0–75 IU/mL), thyroid peroxidase antibody was 993.70IU/mL (normal range: 0–18 IU/mL), thyroglobulin was 6.67ng/mL (normal range: 1.1–130.8) ng/mL, TSHR simulation-blocking antibody was >40IU/L (normal range<1.75 IU/L). Biochemical examination indicated that total cholesterol was 6.59mmol/L, triglyceride was 2.06mmol/L. Routine blood examination revealed that the patient had mild anemia, with hemoglobin 96g/L. Echocardiography showed a left ventricular ejection fraction of 65% with pericardial effusion and left atrial enlargement. Chest CT showed enlarged heart shadow with a small amount of pericardial effusion and pleural effusion on both sides of the chest. Her clinical features along with laboratory findings strongly suggested that the patient had severe hypothyroidism with sick sinus syndrome and mental disorders, and subsequent treatment also supported this hypothesis.
 |
Figure 1 Admitted ECG showed significant sinus bradycardia and sinus arrest. |
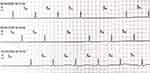 |
Figure 2 Admitted ECG showed significant sinus bradycardia and sinoatrial block. |
 |
Figure 3 He ECG showed that sinus arrest lasting 4.5 seconds occurred on the day of admission, specifically at twenty past three pm. |
From day1 to day 3, we kept giving the patient a dose of 25 ug of levothyroxine per day, and then gradually increased to100ug daily from the 14th day after admission. For the safety of the patient, a temporary pacemaker with a ventricular pacing rate of 60 beats/min was implanted on the first day of hospitalization. One week later, fT3 increased to 2.56μIU/mL. The number of episodes of mental and behavioral disorders decreased significantly during hospitalization. Because the patient’s heart rate was stable above 60 beats/min, the temporary pacemaker was removed on the 17th day. After two weeks of treatment with levothyroxine, the patient’s psychiatric symptoms improved significantly without another mental abnormality. After three months of subsequent follow-up, the ECG examination did not reveal severe bradycardia, and the patient no longer had symptoms of fatigue, dizziness, fainting, or any mental symptoms. And re-examination of thyroid function suggested that T3, T4, and TSH were returned to normal range. The patient’s clinical course is shown in Figure 4.
Discussion and Conclusions
To the best of our knowledge, it is the first time to report a case of severe hypothyroidism in a 42-year-old female patient that caused SSS requiring cardiac pacing and severe mental disorders. As far as the clinical process is concerned, the case is unique, with sick sinus syndrome and mental disorders recovered after thyroxine supplementation.
Thyroid hormones, especially the bioactive component T3, are closely related to cardiovascular diseases and are essential for cardiovascular diseases, which affect various functions of the heart, including cardiac contractility and electrophysiological remodeling.1 The mechanisms of T3 on cardiovascular system are diverse, mainly including the following integral aspects: 1. Binding to nuclear T3 receptors that affect the regulation of structure, contraction and gene expression; 2. Regulation of sympathetic nervous system; 3. Peripheral hemodynamic changes; 4. Direct regulation of ion channels, including Na+/K+ATP enzymes, Na+/Ca++ exchangers and L-type calcium channels.5
Hypothyroidism is known to be related with several ECG abnormalities including sinus bradycardia, prolonged QT interval, low voltage, prolonged the action potential duration of cardiomyocytes and heart block at varying degrees.2 Cardiac K+ and L-type Ca++ channels in patients with hypothyroidism are affected by serum T3 and as a result, ventricular repolarization anomalies develop, which is one of the reasons why hypothyroidism patients have been reported to have an increased risk of ventricular arrhythmias.7 Several studies have also confirmed that QT dispersion increases in dominant and subclinical hypothyroidism. It has been found that Tpe interval, which refers to the interval between the peak and end point of T wave on ECG and can be used as an index of transmural dispersion of ventricular repolarization, and has been used as a new index to predict the risk of arrhythmia and cardiovascular death, was significantly prolonged and could be shortened through levothyroxine treatment in patients with hypothyroidism.6,7 Previous cases have reported that hypothyroidism can also lead to significant bradycardia and even sick sinus syndrome and II and/or III degree atrioventricular block, usually requiring intravenous implantation of temporary or permanent pacemakers insertion in a majority of patients.8 However, even after the thyroid state is normal, reversible cases have been reported. To cite an example, Harada et al reported a case of hypothyroidism that caused SSS requiring temporary cardiac pacing, which was reversible and was successfully treated with levothyroxine without a need for a permanent pacemaker.2 Some scholars have reported an 87-year-old patient who developed high-grade atrioventricular block, which was successfully treated by supplementing thyroxine therapy and avoided the implantation of a pacemaker.9 Schoenmakers et al reported an elderly patient with severe hypothyroidism and complete atrioventricular block, who was recovered after levothyroxine supplementation.10 Our patient underwent intravenous temporary pacemaker because of severe bradycardia. Bradycardia recovered 17 days after levothyroxine replacement therapy and permanent pacemaker implantation was avoided.
Another feature of this case was that the patient was complicated with severe mental problems and had delusions of persecution, verbal auditory hallucinations and impulsive behaviors, symptoms similar to schizophrenia. Few patients with hyperthyroidism have mental disorders. It was thought that in previous studies hyperadrenergic is the main cause of mental symptoms, and β-adrenergic antagonist is an effective treatment.3 However, current researches have found that hypothyroidism can also lead to severe mental illnesses.4 Psychological symptoms caused by hypothyroidism include laziness, fatigue and mood swings, accompanied by mental retardation, behavioral disorders, hallucinations and delusions.3 Amann et al found that hypothyroidism was associated with an increased risk of mania and bipolar disorder, and higher basal thyrotropin (BTSH) levels were also associated with an increased risk of manic recurrence.11 It is suggested that it is important to routinely detect thyroid function in patients with mental disorders. Hockings et al described a case of hypothyroidism in an adolescent with psychiatric symptoms as the first onset of hypothyroidism.12 Mohamed et al reported a case of hypothyroidism complicated with acute psychosis and concurrent rhabdomyolysis gradually returned to normal mental symptoms after treatment with thyroxine and olanzapine.13
The mechanism of neuropsychiatric symptoms caused by hypothyroidism in humans is still unclear, and the current possible mechanisms are as follows: 1. Animal experiments have confirmed that triiodothyronine (T3) receptors are mainly concentrated in the amygdala and hippocampus, which plays a key role in the integration of emotions and behaviors.14 In addition, in the case of hypothyroidism, the conversion rate of thyroxine to t3 increased significantly.13 2. Hypothyroidism is associated with increased activity of brain neurotransmitters dopamine and adrenal catecholamines.13 3. Autoimmune thyroid disease (AITD) is the main cause of hypothyroidism, and the production of autoantibodies against the normal components of the thyroid axis is the main cause of mental disorders.15 4. T3 is not only important for neuronal development but also for the differentiation of astrocytes and oligodendrocytes, as well as for microglial development. In addition, T3 plays an important role in the mechanism of signal transduction factors that affect the function of microglia through complexes. Therefore, the dysfunction of thyroid hormones may damage glial function and therefore interfere with the brain, which may lead to mental illness.16
To our knowledge, this is the first reported case of hypothyroidism with sick sinus syndrome requiring pacemakers and psychiatric disorders, and the symptoms can be improved and reversed after thyroxine supplementation. This case highlights the importance of hypothyroidism screening when faced with unexplained psychosis or sick sinus syndrome, especially if combined.
Abbreviations
SSS, sick sinus syndrome; BMI, body mass index; ECG, electrocardiography; TSH, thyroid-stimulating hormone; AITD, autoimmune thyroid disease.
Data Sharing Statement
All relevant data supporting the conclusions of this article are included within the article.
Ethical Approval
The need for institutional ethics approval for this case report was waived. Written informed consent was obtained from the patient for publication of this case report and accompanying images.
Consent for Publication
The patient has provided informed consent for publication of the case. A copy of the written consent is available for review by the Editor-in-Chief of this journal.
Author Contributions
All authors made substantial contributions to conception and design, acquisition of data, or analysis and interpretation of data; took part in drafting the article or revising it critically for important intellectual content; agreed to submit to the current journal; gave final approval of the version to be published; and agree to be accountable for all aspects of the work.
Funding
This work was supported in part by the Health and Family Planning Commission of Hubei Province (CN) WJ2015MA021 and by the Graduate Education Innovation Project of Hubei Minzu University (MYG2020010) (Yuanhong LI). The funding bodies played no role in design of the study, collection, analysis, and interpretation of the data and in writing the manuscript.
Disclosure
The authors of this article declare that they have no conflicts of interest.
References
1. Khan R, Sikanderkhel S, Gui J, et al. Thyroid and Cardiovascular Disease: a Focused Review on the Impact of Hyperthyroidism in Heart Failure. Cardiol Res. 2020;1:68–75. doi:10.14740/cr1034
2. Harada K, Murakami S, Tokumasu K, et al. Myxedema coma accompanied by sick sinus syndrome and hypoventilation: a case report. J Gen Fam Med. 2019;20:206–208. doi:10.1002/jgf2.267
3. Fu J, Wei H, Li X, et al. Analysis on clinical characteristics of primary hypothyroidism-induced mental disorder. Zhong Nan Da Xue Xue Bao Yi Xue Ban. 2016;41:711–714. doi:10.11817/j.issn.1672-7347.2016.07.009
4. Zhao T, Chen BM, Zhao XM, et al. Subclinical hypothyroidism and depression: a meta-analysis. Transl Psychiatry. 2018;8:239. doi:10.1038/s41398-018-0283-7
5. Barbesino G. Thyroid Function Changes in the Elderly and Their Relationship to Cardiovascular Health: a Mini-Review. Gerontology. 2019;65:1–8. doi:10.1159/000490911
6. Findikli HA, Tutak AŞ, Aydin H, et al. The relationship between the TSH values and the Tpeak-Tend interval duration in hypothyroid patients receiving Levothyroxine treatment. Rom J Intern Med. 2019;57:175–180. doi:10.2478/rjim-2018-0042
7. Akın A, Unal E, Yıldırım R, et al. Evaluation of QT dispersion and Tp-e interval in children with subclinical hypothyroidism. Pacing Clin Electrophysiol. 2018;41(4):372–375. doi:10.1111/pace.13286
8. Ozcan KS, Osmonov D, Erdinler I, et al. Atrioventricular block in patients with thyroid dysfunction: prognosis after treatment with hormone supplementation or antithyroid medication. J Cardiol. 2012;60:327–332. doi:10.1016/j.jjcc.2012.05.012
9. Waseem H, Hashmi AT, Anser M, et al. A pacemaker that was avoided. Cureus. 2018;10:e2555.
10. Schoenmakers N, de Graaff WE, Peters RH. Hypothyroidism as the cause of atrioventricular block in an elderly patient. Neth Heart J. 2008;16:57–59. doi:10.1007/BF03086119
11. Amann BL, Radua J, Wunsch C, et al. Psychiatric and physical comorbidities and their impact on the course of bipolar disorder: a prospective, naturalistic 4-year follow-up study. Bipolar Disord. 2017;19:1–10. doi:10.1111/bdi.12495
12. Hockings CA, Cattaneo E, Sanka SK, et al. Auditory hallucinations in a 15-year-old boy: an unusual presentation of hypothyroidism. Case Rep. 2009;2009:
13. Mohamed MF, Mahgoub AB, Sardar S, et al. Acute psychosis and concurrent rhabdomyolysis unveiling diagnosis of hypothyroidism. BMJ Case Rep. 2019;12:1–5. doi:10.1136/bcr-2019-231579
14. Ruel J, Faure R, Dussault JH, et al. Regional distribution of nuclear T3 receptors in rat brain and evidence for preferential localization in neurons1. J Endocrinol Invest. 1985;8:343–348. doi:10.1007/BF03348511
15. Bunevicius R, Prange AJ. Thyroid disease and mental disorders: cause and effect or only comorbidity? Curr Opin Psychiatry. 2010;23:363–368. doi:10.1097/YCO.0b013e3283387b50
16. Noda M. Possible role of glial cells in the relationship between thyroid dysfunction and mental disorders. Front Cell Neurosci. 2015;9:1–7. doi:10.3389/fncel.2015.00194
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

