Back to Journals » Therapeutics and Clinical Risk Management » Volume 15
Hybrid graft vs autograft in anterior cruciate ligament reconstruction: a meta-analysis
Received 18 September 2018
Accepted for publication 17 January 2019
Published 14 March 2019 Volume 2019:15 Pages 487—495
DOI https://doi.org/10.2147/TCRM.S187979
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Deyun Wang
Lei Wang,1 Jian-gang Cao,2 Jun Liu1
1Department of Joint Surgery, Tianjin Hospital, Tianjin, People’s Republic of China; 2Department of Sport Medicine, Tianjin Hospital, Tianjin, People’s Republic of China
Purpose: We conducted this meta-analysis to evaluate the efficacy of hybrid grafts in anterior cruciate ligament reconstruction (ACLR).
Methods: We performed an electronic search of the Cochrane Library, PubMed, Embase, and ScienceDirect from the inception of these databases to February 2018, based on the terms “anterior cruciate ligament or ACL reconstruction”, “autograft”, “hybrid”, and “augment”. Relevant journals and conference proceedings were searched manually. Quality assessment, data extraction, and calculation of data from the included studies were conducted independently by two reviewers using RevMan 5.1.
Results: One randomized controlled trial and eight nonrandomized controlled trials met inclusion criteria. Larger graft diameters were found in the hybrid-graft group (mean difference -1.47, P=0.0001). There was no significant difference in failure rate (OR 2.13, P=0.21), retearing (OR 2.23, P=0.12), revision of ACLR (OR 1.05, P=0.87) or reoperation (OR 1.27, P=0.35). Subgroup analysis showed that hybrid-graft patients with meniscus injury suffered more revision (OR 4.10, P=0.02) and reoperation (OR 5.74, P=0.001). Both autografts and hybrid grafts performed similarly in most knee-score systems. However, autograft patients had better KT-1000 (mean difference 0.24, P=0.05) and quality-of-life results on the Knee Injury and Osteoarthritis Outcome Score measure (mean difference 7.23, P=0.05).
Conclusion: This meta-analysis of the current literature indicates similar performance of hybrid or autologous grafts in ACLR, though hybrid grafts had larger diameters than autografts. Other potential factors to influence failure, revision, or postoperative knee function, such as irradiation, age at reconstruction, meniscus injury/treatment, and hybrid-graft remodeling, should be investigated further.
Keywords: hybrid graft, autograft, anterior cruciate ligament, reconstruction
Introduction
The anterior cruciate ligament (ACL) is an important component to maintain knee-joint stability and is susceptible to injury during competitive sports.1 More than 100,000 patients per year need ACL reconstruction (ACLR) in the US.2 Autologous graft reconstruction is considered the gold-standard treatment, with better tendon–bone healing. However, evidence has shown that autografts of diameter <8 mm have no guarantee of better prognosis, especially for younger patients.3
Although allografts on their own have been reported to function similarly to autografts,4 the biomechanics of allografts are influenced by many factors, including irradiation and chemical processing, which is associated with the procession of tendon-bone healing and incorporation. Alvarez-Pinzon et al introduced hybrid-graft surgical techniques to permit the surgeon to customize the size of grafts.5 Allografts have been used in combination with autografts in the hope of increasing inadequate diameters and achieving better outcomes.
In a randomized trial, Li et al prospectively compared autografts, allografts, and hybrid grafts. The results showed similar objective and subjective clinical outcomes for patients undergoing primary ACLR with hybrid grafts or autografts. Both groups of patients had better KT-1000 measurements compared with the γ-irradiated (2.5 Mrad) allograft group.6 Another retrospective comparative study, however, noticed more failure or compromised ACLRs and worse Lysholm and IKDC scores after hybrid-graft reconstruction.7 Jacobs et al later reported more failures in autograft patients, and attributed the better results of hybrid grafts mainly to larger diameter.8 Several studies have been published about hybrid grafts vs autografts, with inconsistent results. Therefore, we conducted this meta-analysis to evaluate the efficacy of hybrid grafts in ACLR.
Methods
Search strategy
The literature was searched on the Cochrane Library, PubMed, Embase, and ScienceDirect databases for articles published from 1966 to February 2018. Secondary sources were identified from studies cited in the references. No studies were excluded based on the language used. The key search terms were “autografts”, “hybrid”, “allografts”, and “anterior cruciate ligament” in combination with the Boolean operators AND or OR. Also, research on the appraisal reference list was manually reviewed for other potential trials that should be included. The process was iterated until no further articles could be determined. The meta-analysis was based on acknowledged PRISMA guidelines.
Inclusion and exclusion criteria
Studies were considered eligible for inclusion if they met criteria of: 1) population – patients with ACLR; 2) intervention – hybrid graft (autografts augmented by allografts); 3) control – autograft only; 4) outcome measures – one or more of graft-failure rate, reoperation rate, complications, postoperative knee score, operation time, and other outcomes reported; and 5) study design – randomized controlled trials (RCTs) and non-RCTs. We excluded studies without control groups, articles without available full-text versions, and those with no available outcome data.
Data extraction
Data were extracted from the included trials by two researchers independently (LW and JGC). If article data were incomplete, the complete data were consulted from the corresponding authors of the articles. The following information: first author’s name, publication year, intervening measures, outcome measures, sample size, and comparable baselines were extracted. Other relevant parameters were also extracted from individual studies.
Quality assessment
The methodological index for nonrandomized studies (MINORS) form was used to assess non-RCTs. Quality assessment for RCTs was conducted according to the Cochrane Handbook for Systematic Reviews of Interventions. Literature-quality evaluation was conducted by two researchers independently (LW and JGC). Consensus was reached with the senior researcher (JL).
Data analysis and statistical methods
RevMan 5.1 (Cochrane Collaboration, Oxford, UK) was used for data analysis. Mean differences (MDs) and 95% CIs were determined for continuous outcomes. Dichotomous data were calculated using ORs and 95% CIs. Heterogeneity was estimated by I2 based on the standard χ2 test. When I2<50% and P>0.1, no significant heterogeneity existed and a fixed-effect model was used for analysis, while a random-effect model was used when I2>50% and P<0.1. Subgroup analysis was performed to investigate sources of heterogeneity.
Results
Search results
A total of 125 studies were identified as potentially relevant literature reports based on the search strategy. After titles and abstracts had been scanned, 116 reports were excluded according to the eligibility criteria. Kraeutler et al conducted two studies – in 20169 and 201810 – that both matched eligibility criteria with overlapped data. As such, the later study was included for further data pooling and analysis, because of the larger patient sample. One additional study by Pennock et al was obtained after the reference review.11 Ultimately, eight non-RCTs7,8,10–15 and one RCT6 were eligible for data extraction and meta-analysis, comprising 322 patients in the hybrid-graft group and 404 patients in the autograft group. The search process is shown in Figure 1.
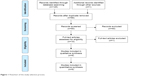  | Figure 1 Flowchart of the study selection process. |
Study characteristics
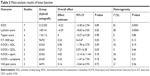
Demographic characteristics and details concerning literature type are summarized in Table 1. Statistically similar baseline characteristics were observed in both groups. Two studies focused on patients <18 years old.8,11 Most samples were 20–71 years old, while Kraeutler et al included 84 and 119 patients in the hybrid and autograft groups, respectively. However, only 36 matched pairs were evaluated for postoperative knee function. Insufficient autograft size was the main reason for extra allograft augmentation. Cutoff sizes for autografts were <7.5 mm7 and <8 mm.6,12–14 Xu et al added an allograft if the autograft could not restore the insertion site to at least 60% of the cross-sectional area or if the augmentation was able to result in better graft occupancy.15 Graft diameter and length, patient size, growth-plate status, and desired level of sport participation were the bases of decision for another study.11 Semitendinosus tendons were used solely as allografts to augment autograft hamstrings by Darnley et al12 and Jacobs et al.8 Tibialis anterior tendons alone were adopted by Li et al,6 Leo et al,13 Wang et al,14 and Xu et al.15 Both semitendinosus and tibialis anterior tendons were included in Burrus et al7 and Pennock et al.11 Posterior tibialis or peroneus longus tendons were the allografts in Kraeutler et al.10 High-dose irradiation (≥2.5 Mrad) was used in processing of allografts in three studies.6,14,15 Meniscus injury was included in four studies,6,7,11,12 while other studies excluded these patients.
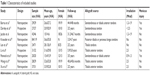  | Table 1 Characteristics of included studies |
Risk-of-bias assessment
Only one RCT had high methodological quality based on the Cochrane Handbook for Systematic Reviews of Interventions (Figure 2). For the eight non-RCTs, the MINORS score ranged from 18 to 24 (Table 2). Most studies were retrospective analyses, while only data were prospectively collected in Darnley et al12 and Leo et al.13 Prospective calculation of sample size was also performed in these two studies. No significant publication bias was noticed, based on the funnel plot for revision (Figure 3).
  | Figure 2 Risk-of-bias summary. |
  | Table 2 Quality assessment for nonrandomized trials |
  | Figure 3 Funnel plot for reoperation. |
Outcomes of meta-analysis
Six studies reported the diameter of grafts, and pooled data showed which was larger in the hybrid-graft group (MD −1.47, 95% CI 0.95–2.00; P=0.0001; Figure 4). The definition was a little different among the studies that reported the rate of failure. Therefore, we report failure, revision, and retear separately in this meta-analysis. Failure rate based on six studies did not show a significantly statistical difference between the two groups (OR 2.13, 95% CI 0.66–6.86; P=0.21; Figure 5). However, Jacobs et al8 reported more than double the rate of failure in the autograft group. After exclusion of their cases, a higher failure rate was noticed in the hybrid-graft group (21 of 144) than the autograft group (six of 136), with lower heterogeneity (OR 3.93, 95% CI 1.53–10.07; P=0.004). There was no significantly statistical difference in postoperative graft retearing (OR 2.23, 95% CI 0.82–6.10; P=0.12) or contralateral tearing (OR 1.00, 95% CI 0.27–3.70; P=1.00). Two damaged hybrid grafts and seven compromised ACLRs were also reported by Xu et al15 and Burrus et al.7 Eight non-RCTs reported revision and reoperation. We pooled only data related to grafts. No significant difference was noticed in either revised ACLR (OR 1.05, 95% CI 0.61–1.81; P=0.87; Figure 6) or reoperation (OR 1.27, 95% CI 0.77–2.11; P=0.35). Subgroup analysis showed that hybrid-graft patients with meniscus injury suffered more revision with lower heterogeneity (OR 4.10, 95% CI 1.28–13.10; P=0.02) and reoperation (OR 5.74, 95% CI 2.05–16.03; P=0.001). When patients without meniscus injury were investigated, no significant difference existed in either autograft or hybrid-graft patients.
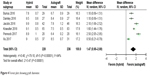  | Figure 4 Forest plot showing graft diameter. |
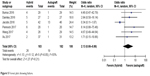  | Figure 5 Forest plot showing failure. |
  | Figure 6 Forest plot showing revision. |
Postoperative knee function was investigated in different studies based on different evaluation systems. Details of meta-analysis results of knee function are illustrated in Table 3. Both autografts and hybrid grafts performed similarly in most of these scores. Also, autograft patients had better KT-1000 test scores (MD 0.24, 95% CI 0–0.47; P=0.05), Lysholm scores (MD −4.29, 95% CI −8.60–0.03; P=0.05), and quality-of-life scores (MD 7.23, 95% CI 0.07–14.38; P=0.05) in the Knee injury and Osteoarthritis Outcome Score (KOOS) measure. Among the five studies reporting Lysholm scores, all patients in Pennock et al were younger than 18 years. Sensitive analysis excluding these cases surprisingly increased the heterogeneity, and again no significant difference existed (P=0.13). Subgroup analysis based on meniscus injury or not showed that no significant difference existed in normal-meniscus patients (MD −3.74, P=0.43), while the Lysholm score was different between the two groups in meniscus-injury patients (MD −4.74, P=0.05).
Discussion
Allograft tendons have been used to augment limited autograft size for ACLR in the past few years, and have achieved better results compared with the allograft solely. Based on the included studies, the current meta-analysis showed similar performance in failure, retearing, revision, and reoperation between hybrid-graft and autograft patients.
High heterogeneity existed in results of diameter, graft failure, revision, reoperation, IKDC score, and Lysholm score. For diameter, we did not perform further sensitivity or subgroup analysis, because it mainly depends on the surgeon’s preference in our opinion. Jacobs et al reported more than double the rate of failure in the autograft group, and they attributed this to the lower diameters of autografts. In a previous in vitro biomechanical study, Boniello et al showed increasing tensile strength for increased graft diameter.16 Clinical trials also supported the view that the diameter of hamstring autografts should be ≥8 mm to reduce the risk of revision ACLR, especially for younger patients.3 However, grafts showed a sequence of remodeling after implantation in the knee cavity.17 The biomechanics of hybrid grafts changed at different maturity times. It is not appropriate to attribute the better results only to larger diameters. Besides, larger diameters of hybrid grafts behaved significantly differently in revision and knee function in the included studies.
Kraeutler et al also reported much fewer revision cases in allograft patients (2.4% vs 8.4%), and they thought that nonirradiation of the allograft may be one major reason for the better results of hybrid grafts. Some previous studies showed evidence that γ-irradiation can damage the biomechanics of allografts. Using the Kaiser Permanente ACLR Registry, Maletis et al identified 14,015 cases and found a higher risk of revision in allografts with irradiation ≥1.8 Mrad after adjusting for age, sex, and race.18 A meta-analysis also reported a dose-dependent relationship between radiation and decreased mechanical tendon integrity. Low-dose radiation (<2.5 Mrad) showed graft weakening, with an average 4.3% decrease in load to failure.19 However, some other studies did not support this conception. A study using peroneus tendons at 1.5–2.5 Mrad γ-irradiation did not find major alterations in tendons’ biomechanical properties.20 In a systematic review, allograft ACL grafts appeared to be a reasonable alternative to autografts with γ-irradiation <2.2 Mrad.21 In our nine included studies, high-dose irradiation (2.5 Mrad) was used in three studies and subgroup analysis did not show more failure or revision in hybrid-graft patients.
Previous trials showed that younger patients were associated with more graft failure.22 Patients aged 25 years and younger had a significantly higher failure rate (16.5%) than patients >25 years (8.3%).23 For each 10-year decrease in age, the odds of graft retearing increase 2.3 times in patients with allograft reconstruction.24 The risk of revision decreased by 7% for each year increase in age.25 Three studies in our study included 32 revisions in 182 patients <25 years old and 27 revisions in 481 patients >25 years old. The revision rate decreased from 17.6% to 5.6%, with average age increased from >25 years to older. However, subgroup analysis showed no significant difference between hybrid grafts and autograft patients in any age range.
Meniscus injury/procedures were reported to be significant predictors of IKDC and KOOS scores 6 years following ACLR.26 Meniscus injury was included in four studies, and meniscus repair or meniscectomy was performed at the same time as ACLR. Subgroup analysis showed that hybrid-graft patients with meniscus injury suffered more revision and reoperation, with lower Lysholm scores. However, no significant difference was noticed in IKDC or Tegner activity scores. With limited detailed description on these procedures, we could not further estimate their effect on ACLR in our included studies.
Limitations
For full understanding of our research’s results, some limitations must be mentioned. First, only one RCT was included, which weakened our power to draw a definitive conclusion. Second, samples were small in most studies, so the relatively larger samples of Jacobs et al and Kraeutler et al had an important influence on the meta-analysis results. Third, many other potential factors can affect ACLR prognosis.
Conclusion
This meta-analysis of the current literature indicates similar performance of hybrid grafts in ACLR, even though hybrid grafts had larger diameters than autograft reconstructions. Irradiation, age at reconstruction, meniscus injury/treatment, hybrid-graft remolding, and other potential factors that influenced failure, revision, or postoperative knee function should be investigated further. Also, more RCTs with more patients and homogeneous design are needed to investigate predictive factors further.
Author contributions
LW and JGC conducted the literature search and determined studies for exclusion and inclusion. LW, JL, and JGC extracted data from the studies included, performed the meta-analysis, and drafted the manuscript. LW, JL, and JGC conceived the idea of the study, designed the study, and critically revised the manuscript for important intellectual content. All authors contributed to data analysis, drafting and revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Disclosure
The authors report no conflicts of interest in this work.
References
Wang H, Fleischli JE, Zheng NN. Transtibial versus anteromedial portal technique in single-bundle anterior cruciate ligament reconstruction: outcomes of knee joint kinematics during walking. Am J Sports Med. 2013;41(8):1847–1856. | ||
Mall NA, Chalmers PN, Moric M, et al. Incidence and trends of anterior cruciate ligament reconstruction in the United States. Am J Sports Med. 2014;42(10):2363–2370. | ||
Mariscalco MW, Flanigan DC, Mitchell J, et al. The influence of hamstring autograft size on patient-reported outcomes and risk of revision after anterior cruciate ligament reconstruction: a multicenter orthopaedic outcomes network (moon) cohort study. Arthroscopy. 2013;29(12):1948–1953. | ||
Mohan R, Webster KE, Johnson NR, et al. Clinical outcomes in revision anterior cruciate ligament reconstruction: a meta-analysis. Arthroscopy. 2018;34(1):289–300. | ||
Alvarez-Pinzon AM, Barksdale L, Krill MK, Leo BM. Hybrid graft anterior cruciate ligament reconstruction: a predictable graft for knee stabilization. Orthopedics. 2015;38(6):e473–e476. | ||
Li J, Wang J, Li Y, et al. A prospective randomized study of anterior cruciate ligament reconstruction with autograft, γ-irradiated allograft, and hybrid graft. Arthroscopy. 2015;31(7):1296–1302. | ||
Burrus MT, Werner BC, Crow AJ, et al. Increased failure rates after anterior cruciate ligament reconstruction with soft-tissue autograft-allograft hybrid grafts. Arthroscopy. 2015;31(12):2342–2351. | ||
Jacobs CA, Burnham JM, Makhni EC, et al. Allograft augmentation of hamstring autograft for younger patients undergoing anterior cruciate ligament reconstruction: clinical and cost-effectiveness analyses. Am J Sports Med. 2017;45(4):892–899. | ||
Kraeutler M, Kim S, Brown C, et al. A matched-pair comparison of patient-reported outcomes following primary ACL reconstruction with hamstring autograft vs hybrid graft. Arthroscopy. 2016;32(6):e6. | ||
Kraeutler MJ, Kim SH, Brown CC, et al. Clinical outcomes following primary anterior cruciate ligament reconstruction with hamstring autograft versus planned hybrid graft. J Knee Surg. 2018;31(9):827–833. | ||
Pennock AT, Ho B, Parvanta K, et al. Does allograft augmentation of Small-Diameter hamstring autograft ACL grafts reduce the incidence of graft Retear? Am J Sports Med. 2017;45(2):334–338. | ||
Darnley JE, Léger-St-Jean B, Pedroza AD, et al. Anterior cruciate ligament reconstruction using a combination of autograft and allograft tendon. Orthop J Sports Med. 2016;4(7):232596711666224. | ||
Leo BM, Krill M, Barksdale L, et al. Failure rate and clinical outcomes of anterior cruciate ligament reconstruction using autograft hamstring versus a hybrid graft. Arthroscopy. 2016;32(11):2357–2363. | ||
Wang HD, Gao SJ, Zhang YZ. Comparison of clinical outcomes after anterior cruciate ligament reconstruction using a hybrid graft versus a hamstring autograft. Arthroscopy. 2018;34(5):1508–1516. | ||
Xu H, Dong J, Xin D, et al. Second-look arthroscopic evaluation and clinical outcomes of anatomic anterior cruciate ligament reconstruction with autograft and hybrid graft: a retrospective study. Med Sci Monit. 2017;23:5564–5573. | ||
Boniello MR, Schwingler PM, Bonner JM, et al. Impact of hamstring graft diameter on tendon strength: a biomechanical study. Arthroscopy. 2015;31(6):1084–1090. | ||
Takeuchi H, Niki Y, Matsunari H, et al. Temporal changes in cellular repopulation and collagen fibril remodeling and regeneration after allograft anterior cruciate ligament reconstruction: an experimental study using Kusabira-Orange transgenic pigs. Am J Sports Med. 2016;44:2375–2383. | ||
Maletis GB, Chen J, Inacio MC, Love RM, Funahashi TT. Increased risk of revision after anterior cruciate ligament reconstruction with soft tissue allografts compared with autografts: graft processing and time make a difference. Am J Sports Med. 2017;45(8):1837–1844. | ||
Dibartola AC, Everhart JS, Kaeding CC, Magnussen RA, Flanigan DC. Maximum load to failure of high dose versus low dose gamma irradiation of anterior cruciate ligament allografts: a meta-analysis. Knee. 2016;23(5):755–762. | ||
Aguila C, Delcroix GJ, Kaimrajh DN, et al. Effects of gamma irradiation on the biomechanical properties of peroneus tendons. Open Access J Sports Med. 2016;7:123–127. | ||
Dashe J, Parisien RL, Cusano A, et al. Allograft tissue irradiation and failure rate after anterior cruciate ligament reconstruction: a systematic review. World J Orthop. 2016;7(6):392–400. | ||
van Eck CF, Schkrohowsky JG, Working ZM, Irrgang JJ, Fu FH. Prospective analysis of failure rate and predictors of failure after anatomic anterior cruciate ligament reconstruction with allograft. Am J Sports Med. 2012;40(4):800–807. | ||
Barrett AM, Craft JA, Replogle WH, Hydrick JM, Barrett GR. Anterior cruciate ligament graft failure: a comparison of graft type based on age and Tegner activity level. Am J Sports Med. 2011;39(10):2194–2198. | ||
Kaeding CC, Aros B, Pedroza A, et al. Allograft versus autograft anterior cruciate ligament reconstruction: predictors of failure from a moon prospective longitudinal cohort. Sports Health. 2011;3(1):73–81. | ||
Maletis GB, Inacio MC, Desmond JL, et al. Reconstruction of the anterior cruciate ligament: association of graft choice with increased risk of early revision. Bone Joint J. 2013;95-B:623–628. | ||
Cox CL, Huston LJ, Dunn WR, et al. Are articular cartilage lesions and meniscus tears predictive of IKDC, KOOS, and Marx activity level outcomes after anterior cruciate ligament reconstruction? A 6-year multicenter cohort study. Am J Sports Med. 2014;42(5):1058–1067. |
 © 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2019 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.