Back to Journals » Clinical Interventions in Aging » Volume 9
Help-seeking preferences in the area of mild cognitive impairment: comparing family physicians and the lay public
Authors Werner P , Heinik J, Giveon S, Segel-Karpas D, Kitai E
Received 7 January 2014
Accepted for publication 10 February 2014
Published 9 April 2014 Volume 2014:9 Pages 613—619
DOI https://doi.org/10.2147/CIA.S60248
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Perla Werner,1 Jeremia Heinik,2 Shmuel Giveon,3 Dikla Segel-Karpas,1 Eliezer Kitai4
1Center for the Research and Study of Aging, University of Haifa, Haifa, Israel; 2Margoletz Psychogeriatric Center, Ichilov Hospital, Sackler School of Medicine, Tel Aviv University, Tel Aviv, Israel; 3Clalit Health Services, Tel Aviv, Israel; 4Department of Family Medicine, Leumit Health Services, Sackler School of Medicine, Tel Aviv University, Tel Aviv, Israel
Background: Mild cognitive impairment (MCI) or mild neurocognitive disorder is a well-established clinical entity included in current diagnostic guidelines for Alzheimer's disease and in major psychiatric classifications. In all, a loosely defined concern obtained from conceptually different sources (the individual, a knowledgeable informant, or a clinician) regarding a decline in cognition and change in functioning constitutes a sine qua non for initiating diagnostics and providing therapy and support. This concern in practice may translate into complex proactive help-seeking behavior. A better understanding of help-seeking preferences is required in order to promote early detection and management.
Objectives: To compare help-seeking preferences of family physicians and the lay public in the area of MCI.
Methods: A structured questionnaire was used to collect data from 197 family physicians (self-administered) and 517 persons aged 45 and over from the lay public (face to face). Information regarding familiarity with MCI and help-seeking preferences was assessed.
Results: The vast majority in both samples reported that family physician, spouse, and children are the most highly recommended sources of help-seeking. In regard to professional sources of help-seeking, a higher percentage of the physicians than the lay public sample consistently recommended seeking help from nurses and social workers and psychiatrists, but a higher percentage of the lay public recommended turning to a neurologist for help.
Discussion: There were both similarities and differences between family physicians and the lay public in their preferences regarding help-seeking for a person with MCI. Most prominent is the physicians' greater tendency to recommend professional sources of help-seeking.
Conclusion: Understanding of help-seeking preferences of both physicians and lay persons might help overcome barriers for establishing diagnosis, receiving care, and improving communication between doctors and patients.
Keywords: lay persons, barriers, doctors, patients
Introduction
The alarming rise in the number of expected persons with cognitive problems and Alzheimer’s disease in future years due to the aging of the population has increased the amount of research devoted to early detection of these problems in general, and to the understanding of mild cognitive impairment (MCI) in particular.1 MCI is a clinical entity characterized by newly acquired cognitive decline beyond what would be expected for an individual’s age and education, maintaining independence in activities of daily living.2,3 MCI is currently included in the NIA-AA (National Institute on Aging and Alzheimer’s Association) diagnostic guidelines for Alzheimer’s disease,4 as well as in the fifth revision of the Diagnostic and Statistical Manual of Mental Disorders (DSM-5)5 under the term of “mild neurocognitive disorder.” In addition, the World Health Organization International Classification of Diseases (ICD) beta draft is suggesting mild neurocognitive disorder, separated from dementia syndrome and persistent amnestic disorder, for inclusion in its upcoming eleventh edition, ICD-11. The high prevalence of this syndrome, and the possibility that it may deteriorate into dementia, emphasize the importance of assessing the condition as early as possible.3,6,7
In all current diagnostic schemas for MCI,4,5 a concern regarding a decline in cognition and change in functioning constitutes a sine qua non condition for initiating a diagnostic process, establishing diagnosis, and providing therapy and support. However, this criterion is loosely defined, as it relies upon information obtained from conceptually different sources: the individual, a knowledgeable informant, and a clinician. In addition, no indications are provided regarding priorities, relative importance, identity, and mutual relations among the different sources of information.
Early detection and management of MCI requires proactive help-seeking, which has been defined as an active process of seeking (formal or informal) help, including several stages such as the identification and awareness of the problem or the need, the identification of the resources needed to alleviate the problem, the procurement of these resources from others, and the communication by the person in need with others (including physicians) about the problem.8
Although increased attention has been devoted in recent years in the area of subjective memory complaints and MCI to understanding the factors associated with the willingness to be screened for memory and other cognitive problems,9–11 only two studies have concentrated specifically on help-seeking patterns for MCI. In the first study, Begum et al9 conducted a qualitative study examining the experiences of nine persons who sought formal help for memory complaints to those of nine who did not seek such help. Their findings showed that concern, causation, and perceptions of the general practitioners were the main factors associated with help-seeking; however, this study did not empirically examine general practitioners’ perceptions. In an effort to expand this line of research, we have recently reported about family physicians’ preferences regarding help-seeking for MCI. In a quantitative study including 197 general practitioners, we found that family physicians and close relatives (spouse and children) were the most preferred sources of help in the case of a person with MCI.12
However, to the best of our knowledge, no comparative studies of lay persons’ and physicians’ help-seeking preferences in the area of MCI have been conducted. This is surprising, especially since studies in other conditions have stressed the importance of understanding and comparing physicians’ and patients’ or lay persons’ perceptions concerning the process of seeking help.13–15
Thus, the aim of the present study was to compare the help-seeking preferences of family physicians and the lay public in regards to MCI. Family physicians were selected for the comparison, since there is a wide agreement that they should be the first source for the detection and early intervention of MCI and dementia.16
Such an investigation is important for several reasons. First, help-seeking is a social action involving complex interactions between a person and his or her significant others.17 Since family physicians are usually the initial contact and play a central role in the managing of cognitive problems,18,19 it is of great importance to compare their help-seeking preferences with those of their patients or potential patients, especially since it has already been clearly established in the area of psychological help-seeking that primary care physicians’ attitudes towards help-seeking can influence their patients’ actions.15
Second, the roles of patients and physicians in the delivery of care in general, and in the process of help-seeking in particular, have been changing in recent decades. Indeed, we are witnessing the emergence of a less paternalistic and more participatory relationship20 in which each side will benefit by knowing the attitudes and expectations of the other side. Third, given the current efforts to increase awareness for early detection, primary care physicians would seem to be well positioned to convey information regarding the preferable sources for help-seeking in the case of cognitive problems. Finally, and more specifically to MCI, there is still no consensus regarding the benefits, detriments, and process of MCI screening,7 making it all the more vital to understand the viewpoints of all groups involved in the help-seeking process.
Methods
Participants
Two samples were used in this study. The first was a convenience sample of 197 family physicians working in one of the largest health maintenance organizations in Israel. As shown in Table 1, approximately half of the participants (48.5%) were male, with a mean age of 50.1 (standard deviation [SD] =9.2; range 28–67); 35% were Israeli born.
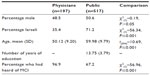  | Table 1 Comparisons between physicians’ and the lay public’s demographic characteristics and familiarity with MCI |
The second sample was a convenience sample of 517 community-dwelling adults aged 45 or older. This age was selected because of the relevance to the topic under study. Approximately half of the sample (50.6%) was male, with a mean age of 59.8 (SD =9.8) and a mean of 13.7 (SD =3.8) school years (Table 1). In addition, the majority of the participants in the lay public’s sample were born in Israel (71.2%). As can be seen from Table 1, the public’s sample was significantly older than the physicians’ sample and included a larger proportion of Israeli-born participants. These variables were later controlled for in the analysis.
Instruments
A questionnaire assessing physicians’ and lay persons’ knowledge, attitudes, and practice in regard to MCI was developed and piloted. The questionnaire opened with a short description of MCI. For the current study, the following measures were included.
Familiarity with MCI
Familiarity with MCI was assessed by asking participants whether they had heard of MCI (no/yes). Participants who reported not being familiar with MCI were excluded from the following analyses.
Help-seeking preferences
Participants were presented with a list of nine possible sources of help, derived from previous studies.21 Given the importance of involving nonprofessionals as well as professionals in the care of persons with MCI,7 the list of sources of help included spouse and children, friend, other family members, family physician, psychiatrist, psychologist, neurologist, nurse, and social worker. Each source was rated on a five-point Likert-type scale, ranging from 1= “would not recommend to seek help at all from this source” to 5= “would recommend to seek help to a great extent from this source.”
To examine whether help-seeking preferences reflected underlying dimensions, factor analysis using principal components and varimax rotation was performed. Tests of the suitability of the data for factor analysis proved satisfactory, with the Kaiser–Meyer–Olkin test value of 0.74 exceeding the recommended value of 0.60,22 and Bartletts’ test of sphericity23 reaching statistical significance (P=0.0001).
Inspection of the final solution showed two factors explaining 49.7% of the total variance: 1) professional sources (ie, social worker, nurse, psychiatrist, psychologist, neurologist, and family doctor), and 2) nonprofessional sources (ie, spouse and children, other relatives, and friends).
Two indices were derived by averaging the items in each factor. Internal reliability scores were very good for the professional index (α=0.80) and moderate for the nonprofessional index (α=0.56).
Procedure
The data were collected from two different surveys conducted among family physicians and the lay public in Israel during 2011, with the aim of assessing beliefs and perceptions regarding MCI. For family physicians, a self-administered, structured questionnaire was distributed during professional meetings and in continuing-education courses provided to family physicians. Questionnaires for the lay public were administered face-to-face by trained interviewers. All participants in the lay persons’ sample were recruited opportunistically from public places such as university campuses, places of work, and through personal contacts. They provided informed consent, and were assured of confidentiality and informed about the right to withdraw. Completion, of the questionnaire took approximately 20 minutes.
Participants in both surveys were not provided with any incentive. The protocols were approved by the ethics committee of the health maintenance organization for the physicians’ sample and by the University of Haifa for the lay persons’ sample.
Statistical analyses
Descriptive statistics (percentages, means, and standard deviations) were used to describe the samples and the main variables. Multiple analysis of covariance (MANCOVA) was used to examine the relationship between group membership (ie, physicians versus lay persons) and help-seeking preferences (separate items and overall indices), controlling for age, sex, and being Israeli.
Results
As could be expected, a higher percentage of the participants in the physicians’ sample reported hearing about MCI than the participants in the lay public sample (Table 1). Whereas 96.9% of the physicians reported to have heard about MCI, only 67.2% of the lay persons reported to have heard about MCI. Lay persons who had heard about MCI were more educated in comparison with those who had not heard about MCI (t(454)=2.4, P<0.05), and a significantly greater proportion of women reported to have heard about MCI (71.3% of women and 54.2% of men, χ2=14.1, P<0.001).
The following analyses regarding help-seeking preferences were conducted on those who had familiarity with MCI. Thus, the statistical models applied to analyze help-seeking were performed on 126 physicians and 292 lay persons.
As for the differences in help-seeking preferences for a person with MCI in both groups, some interesting similarities and dissimilarities emerged from the data. First, regarding the most preferred sources for help-seeking, spouse and children as well as family physician were the sources with the highest rates of preference, both for the lay public and for the physicians (Table 2).
Second, when examining the individual items, we observed an overall effect of group (F(1,413)=17.68, P<0.001). The univariate ANOVAs (analyses of variance) derived from the MANCOVA analysis for the separate items indicated that while there were no differences between the groups in their preferences for help-seeking from close relatives (spouse and children) or the family physician, there were statistically significant differences in the preferences to seek help from other sources. The most notable differences were the physicians’ greater preference for seeking help from nurses (F(1,413)=22.38, P<0.001) and social workers (F(1,413)=60.47, P<0.001), compared with lay persons. Surprisingly, lay persons showed slightly greater preferences than physicians to seek help from neurologists (F(1,413)=5.09, P<0.05) (Table 2).
Finally, comparing the overall indices of professional and nonprofessional sources of help-seeking, statistically significant differences were observed between the groups (F(1,413)=9.74, P<0.001). Overall, compared with the lay public, physicians reported greater tendency to seek help from professionals (F(1,413)=12.96, P<0.001). No statistically significant differences were found in the preferences to seek help from nonprofessional sources.
Discussion
Our results suggest that there are both similarities and differences between physicians and the lay public in their preferences regarding help-seeking for a person with MCI. First, close family members (ie, spouse and children) and the family physician were the most important sources for help-seeking for both lay persons and physicians, with both groups reporting similar levels of willingness to use these sources for help-seeking. Although previous studies assessing help-seeking for cognitive impairment and/or subjective memory problems in older adults reported family and primary care physicians to be the preferred help-seeking source by those seeking help,9,24,25 our study showed for the first time that these preferences are shared by family physicians as well. Given the still existing complexity in diagnosing and treating memory problems in general and MCI in particular,3,4 our findings are encouraging in that they suggest agreement in the preferred help-seeking trajectories between potential users and providers of care in the area of MCI.
Physicians were more inclined to suggest friends as a source for help, in comparison with lay persons, while lay persons were more inclined to suggest other close relatives as a source of help. These results may reflect a greater sense of embarrassment of the lay public, and therefore, a greater reluctance to share information about one’s cognitive functioning with others outside the family. Alternatively, it might be associated with the possibility that physicians’ friends are mostly physicians themselves. Indeed, recent findings stress the importance adjudicated by physicians to peer support for their physical and mental wellbeing.4
Despite these similarities, several important differences were found in the physicians’ and lay public’s perceptions regarding help-seeking for a person with MCI. Most notable is the overall greater willingness of physicians to seek professional help. Physicians reported nurses, social workers, and psychiatrists as more important sources for help-seeking than lay persons. This finding is encouraging, as it stresses family physicians’ recognition of these professionals as a prominent part of the health-care system, and their role in the diagnosis and treatment of cognitive impaired individuals, as suggested lately in the literature.26–28
It is interesting to note that, compared with physicians, lay persons reported higher levels of preference to seek help from neurologists. Several explanations are possible for this finding. First, it might be associated with the ongoing controversy regarding the roles played by primary-care physicians and specialists in the diagnosis and treatment of cognitive deterioration.29 Second, it might be a consequence of Israeli practice and models of care delivery. Indeed, a study assessing Israeli lay persons’ help-seeking preferences for Alzheimer’s disease showed neurologists to be the preferred professional source of help-seeking.30 Moreover, the conclusions and recommendations of the Israeli Consensus Conference conducted in 2002,31 as well as the Israeli Alzheimer’s Association website,31 suggest neurologists to be one of the first sources of help.
Interestingly, lay persons and physicians both preferred nonprofessionals as a source for help-seeking over professionals, although lay persons’ preference toward nonprofessional sources was more prominent than physicians’ preference. This inclination of the lay public might be associated with fatalistic beliefs reported to be a barrier to effective help-seeking among elderly persons.9,24,25
The present study has several limitations. First, both samples were based on convenience sampling rather than random sampling, and therefore the results should be generalized with caution. Second, the public survey was based on face-to-face interviewing, whereas an anonymous questionnaire was employed in the professional sample. This difference may have lessened the validity of the comparisons. However, we used a model based on identical study designs and questionnaires for all participating groups in an attempt to overcome this shortcoming. Third, we did not include information regarding the physicians’ length or type of experience in treating patients with cognitive deficits and regarding lay persons’ familiarity with dementia. Finally, we did not collect information regarding the number of years of education of the physicians, limiting our possibility to control for a potentially confounding variable. However, it should be noted that when the preferences of both groups were compared in a subsample of lay participants with high education (12 years of education and above), identical patterns to those reported here were found (data available from the authors).
Conclusion and clinical relevance
The importance and potential benefits of timely and adequate help-seeking behavior for cognitive problems have been well established.24 Recently, research has indicated the importance of physicians’ perceptions to the help-seeking response of persons with memory complaints.9,12 The present study expanded this line of research by comparing family physicians’ and lay persons’ preferences for help-seeking in the area of MCI.
Overall, greater consensus was found in the preferences for nonprofessional sources of help than in the professional ones. Regarding professional sources, our study demonstrates that family physicians expressed greater preference for professional sources that are not physicians, such as nurses and social workers.
Given the expected increase in the number of elderly persons with cognitive problems in future years, which is accompanied by increased efforts for early detection,1 primary-care physicians might be confronted with a concomitant pressure to advise and diagnose persons with cognitive problems in general and MCI in particular. However, the diagnosis and management of MCI is a complex process requiring clinicians to collaborate and partner with the elderly person and the caregiver to optimize the process.32 Accordingly, communication scholars have emphasized the need to identify and comprehend pre-diagnosis expectations33–35 to enhance comprehension and adequate management. However, these studies focused mostly on questions of whether patients wish to know the diagnosis or whether family members wish the patient to be informed. The present study stresses the importance of examining and comparing physicians’ and lay persons’ expectations regarding help-seeking preferences as well. This can be attained by developing public education interventions aimed at clarifying all available paths to help-seeking in the area of MCI. Such programs were proven beneficial for help-seeking in other diseases.36 These efforts should, however, be accompanied by appropriate training and education of professionals in the area, as well as by rigorous quantitative and qualitative research about help-seeking preferences.
In sum, understanding help-seeking preferences of both physicians and lay persons might help overcome barriers for establishing diagnosis, receiving care, and improving communication between doctors and patients in the complex process of diagnosis and management of MCI.
Disclosure
The authors report no conflicts of interest in this work.
References
Ferri CP, Prince M, Brayne C, et al. Alzheimer’s Disease International. Global prevalence of dementia: a Delphi consensus study. Lancet. 2005;366(9503):2112–2117. | |
Gainotti G. Origins, controversies and recent developments of the MCI construct. Curr Alzheimer Res. 2010;7:271–279. | |
Petersen RC. Mild cognitive impairment. New Engl J Med. 2011;364:2227–2234. | |
Albert MS, Dekosky ST, Dickson D, et al. The diagnosis of mild cognitive impairment due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimers Dement. 2011;7(3):270–279. | |
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders, Fifth edition (DSM-5). Arlington, VA: American Psychiatric Publishing; 2013. | |
Stewart R. Mild cognitive impairment – the continuing challenge of its “real-world” detection and diagnosis. Arch Med Res. 2012;43:609–614. | |
Werner P, Korczyn AD. Mild cognitive impairment: conceptual assessment, ethical, and social issues. Clin Interv Aging. 2008;3(3):413–420. | |
Rickwood D, Thomas K. Conceptual measurement framework for help-seeking for mental health problems. Psychol Res Behav Manag. 2012;5:173–183. | |
Begum A, Whitley R, Banerjee S, Matthews D, Stewart R, Morgan C. Help-seeking response to subjective complaints in older adults: toward a conceptual model. Gerontologist. 2013;53(3):462–473. | |
Boustani M, Watson L, Fultz B, Perkins AJ, Druckenbrod R. Acceptance of dementia screening in continuous care retirement communities: a mailed survey. Int J Geriatr Psychiatry. 2003;18(9):780–786. | |
Werner P. Knowledge about symptoms of Alzheimer’s disease: correlates and relationship to help-seeking behavior. Int J Geriatr Psychiatry. 2003;18:1029–1036. | |
Werner P, Heinik, J, Kitai E. Familiarity, knowledge, and preferences of family physicians regarding mild cognitive impairment. Int Psychogeriatr. 2013;25(5):805–813. | |
Arnou R, Frank M, Hagel T, Prebet A. Willingness to vaccinate with an intradermal seasonal influenza vaccine: a survey of general practitioners and the general public in France and Germany. Adv Ther. 2011;28(7):555–565. | |
De Nooijer J, Lechner L, De Vries H. Help-seeking behavior for cancer symptoms: perceptions of patients and general practitioners. Psychooncol. 2001;10(6):469–478. | |
Smith LD, Peck PL, McGovern RJ. Comparison of medical students, medical school faculty, primary care physicians, and the general population on attitudes towards psychological help-seeking. Psychol Rep. 2002;91:1268–1272. | |
Olazaran J, Torrero P, Cruz I, et al. Mild cognitive impairment and dementia in primary care: the value of medical history. Fam Pract. 2011;28:385–392. | |
Okello ES, Neema S. Explanatory models and help-seeking behavior: pathways to psychiatric care among patients admitted for depression in Mulago Hospital, Kampala, Uganda. Qual Health Res. 2007;17(1):14–25. | |
Lopponen M, Raiha I, Isoaho R, Vahlberg T, Kivela SL. Diagnosing cognitive impairment and dementia in primary health care: a more active approach is needed. Age Ageing. 2003;32(6):606–612. | |
Sadowsky CH, Galvin JE. Guidelines for the management of cognitive and behavioral problems in dementia. J Am Board Fam Med. 2012;25(3):350–366. | |
Boyer CA, Lutfey KE. Examining critical health policy issues within and beyond the clinical encounter: patient-provider relationships and help seeking behaviors. J Health Soc Behav. 2010;51 Suppl:S80–S93. | |
Werner P. Family physicians’ recommendations for help-seeking for a person with Alzheimer’s disease. Aging Clin Exp Res. 2007;19:356–363. | |
Kaiser H. An index of factor simplicity. Psychometrika. 1974;3:31–36. | |
Bartlett MS. A note on the multiplying factors for various chi-square approximations. J R Stat Soc Series B Stat Methodol. 1954;16:296–298. | |
Hurt CS, Burns A, Brown RG, Barrowclough C. Why don’t older adults with subjective memory complaints seek help? Int J Geriatr Psychiatry. 2012;27(4):394–400. | |
Werner P. Beliefs about memory problems and help seeking in elderly persons. Clin Gerontol. 2004;27(4):19–30. | |
Elliot AF, Horgas AL, Marsiske M. Nurses’ role in identifying mild cognitive impairment in older adults. Geriatr Nurs. 2008;29(1):38–47. | |
Kane MN, Hamlin ER, Hawkins WE. How adequate do social workers feel to work with elders with Alzheimer’s disease? Soc Work Ment Health. 2004;2(4):63–84. | |
Lin F, Vance DE, Gleason CE, Heidrich SM. Taking care of older adults with mild cognitive impairment: an update for nurses. J Gerontol Nurs. 2012;38:22–37. | |
Robinson L, Vellas B, Knox S, Lins K. Clinical practice patterns of generalists and specialists in Alzheimer’s disease: what are the differences, and what difference do they make? J Nutr Health Aging. 2010;14:545–552. | |
Werner P. Factors influencing intentions to seek a cognitive status examination: a study based on the Health Belief Model. Int J Geriatr Psychiatry. 2003;18(9):787–794. | |
Israeli Alzheimer’s Association [website on the Internet]. Available from: http://www.alz-il.net. Accessed August 16, 2013. | |
Bensadon BA, Odenheimer GL. Current management decisions in mild cognitive impairment. Clin Geriatr Med. 2013;29:847–871. | |
Carpenter B, Dave J. Disclosing a dementia diagnosis: a review of opinion and practice, and a proposed research agenda. Gerontologist. 2004;44(2):149–158. | |
Karnieli-Miller O, Werner P, Ajaron-Peretz J, Sinoff G, Eidelman S. Expectations, experiences, and tensions in the memory clinic: the process of diagnosis disclosure of dementia within a triad. Int Psychogeriatr. 2012;24(11):1756–1770. | |
Williams CM. Pre-diagnostic counseling with people with memory problems: what can we learn from HIV/GUM services? PSIGE Newsletters. 2004;87:11–16. | |
Gulliver A, Griffiths KM, Christensen H, Brewer JL. A systematic review of help-seeking interventions for depression, anxiety and general psychological distress. BMC Psychiatr. 2012;12:81. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.

