Back to Journals » Clinical Ophthalmology » Volume 14
GlaucoMap – Distribution of Glaucoma Surgical Procedures in the United States
Authors Ma AK, Lee JH , Warren JL, Teng CC
Received 8 April 2020
Accepted for publication 13 July 2020
Published 28 August 2020 Volume 2020:14 Pages 2551—2560
DOI https://doi.org/10.2147/OPTH.S257361
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Scott Fraser
Anthony K Ma,1 Jun Hui Lee,1 Joshua L Warren,2 Christopher C Teng3
1Yale School of Medicine, New Haven, CT, USA; 2Department of Biostatistics, Yale School of Public Health, New Haven, CT, USA; 3Department of Ophthalmology and Visual Science, Yale School of Medicine, New Haven, CT, USA
Correspondence: Christopher C Teng
Department of Ophthalmology and Visual Science, Yale School of Medicine, 40 Temple Street, Suite 1B, New Haven, CT, USA
Tel +1 203-785-3366
Fax +1 203-785-6220
Email [email protected]
Purpose: To understand the distribution of trabeculectomies, glaucoma drainage implants (GDI) and micro-invasive glaucoma surgeries (MIGS) performed in the United States through geospatial mapping.
Methods: We performed an observational cohort study to evaluate glaucoma surgeries in patients age ≥ 65. The most recently released data from Centers for Medicare Part B Carrier Summary Files were queried to determine the number of glaucoma surgeries performed per state during the year of 2017. We created choropleth maps, titled “GlaucoMap”, to characterize the rates of various surgeries performed across the United States, defined as the number of procedures performed per 10,000 individuals. A chi-squared analysis was further used to evaluate differences in surgical preferences across geographic region. Standardized residuals (SR) were calculated to determine regional influences on surgical distribution.
Results: There were 174,788 glaucoma surgeries performed: 22,862 trabeculectomies (13.1%), 19,991 GDI (11.4%) and 131,935 (75.5%) MIGS. The Northeast had the highest trabeculectomy rate, GDI was highest in the Southeast and MIGS were highest in the Southwest. There was a statistically significant difference in proportional use of conventional surgeries versus MIGS across various regions in the United States (p < 0.0001). Given the high trabeculectomy and GDI rates and relatively low MIGS adoption in the Southeast, we observed a +7.03 SR for conventional surgeries and − 4.01 SR for MIGS. The Southwest and Western states had the highest MIGS rate and contributed +3.29 and +3.24 SR toward disproportional MIGS preference, respectively. The preference for conventional surgeries in the Northeast (SR = +2.93) and MIGS in the Midwest (SR = +0.99) also contribute to the overall differences in glaucoma surgeries across the United States.
Conclusion: GlaucoMap is useful for visualizing the distribution of glaucoma surgeries in the United States. The heterogeneity in surgical preferences points to regional differences in glaucoma management.
Keywords: glaucoma, MIGS, trabeculectomies, GDI, heatmaps
Introduction
Glaucoma is a progressive optic neuropathy and is the leading cause of irreversible blindness and the second most common cause of blindness worldwide.1 According to the latest census and prevalence models, the number of people with open-angle glaucoma (OAG) and angle-closure glaucoma (ACG) worldwide has been climbing from 60.5 million in 2010 to 79.6 million in 2020 and a projected 111.8 million by 2040.2,3
Surgeries include trabeculectomy, glaucoma drainage implants (GDI) and micro-invasive glaucoma surgery (MIGS).4 MIGS allow for IOP reduction with minimal trauma, an overall higher safety profile, and quicker recovery.5,6 Their role within the glaucoma treatment algorithm has been gaining popularity as the philosophy of interventional glaucoma spreads. Interventional glaucoma involves performing MIGS at an earlier stage of disease to bridge the treatment gap between maximal medical therapy and more invasive surgeries. In effect, MIGS could reduce a patient’s reliance on drops and have an excellent safety profile with minimal side effects.7
Geospatial visualization tools have recently become widely popular in implementation and application for studies in public health, chronic diseases, and even ophthalmology.8–10 Applying methods in spatial epidemiology allow a better understanding of environmental factors that contribute to geographical variation in disease incidence and surgical management.11 Recent advances in data visualization technologies, both in the private sectors (ie, Tableau Software, Seattle, WA, USA) and open source software packages such as D3: Data Driven Documents (Stanford, CA, USA) and Plotly (Montreal, Quebec, Canada), facilitate such analyses to rapidly transform large numerical datasets into geospatial heatmaps that are intuitive in revealing novel patterns regarding disease and treatment progression.12–14 These maps, called choropleth maps, in which areas are shaded in proportion to the measurement of the statistical variable being displayed on the map, are highly intelligible and allow for better understanding of patterns that may not typically be visualized.
In this study, we aim to understand with geospatial heatmaps, how glaucoma is being managed in various states and regions across the United States.
Methods
Data Source
We obtained Part B National/Carrier Summary Data Files in the year of 2017 from the Centers for Medicare and Medicaid Services (CMS).15 The 2017 data set includes the most recent information available regarding the number of procedures performed under each carrier. Procedure counts at the carrier level were aggregated to compute the number of procedures performed in the individual 50 states and 5 regions of the United States. No directly identifiable patient population was utilized, and the study was exempted by the Yale Institutional Review Board. The Medicare Part B data includes information regarding both the number of procedures performed annually for a specified Current Procedural Terminology (CPT) code as well as demographic information of the patients who are Medicare beneficiaries. Overall, the CMS data provide a representative sample of the United States population ≥65 years and older, which corresponds to the age demographic most affected by glaucoma.
CPT codes were used to query the CMS database for common surgical procedures used for glaucoma management. The CPT codes used were 66170/66172 for trabeculectomy, 66180/66179 for GDI, 65820 for goniotomy, 66183 for Ab externo drainage device, 66174 for transluminal dilation, 66711 for Endocyclophotocoagulation (ECP), 0191T for iStent and 0253T for iStent Supra (Glaukos, San Clemente, CA, USA), 0449T for Xen Gel Stent (Allergan Inc, Irvine, CA, USA), and 0474T for CyPass (Alcon, Fort Worth, TX, USA). For each procedure, we collected the number of allowed services (ie, procedures paid for by Medicare Part B for all 50 states in the US.
We queried the American Glaucoma Society membership directory to determine the number of fellowship trained glaucoma specialists per state. Glaucoma specialist availability was defined as the number of glaucoma specialists in a state divided by 10,000 individuals ≥65 years of age.
Statistical Analysis
We first performed a qualitative analysis to understand the distribution of various glaucoma surgeries used in the United States. Surgery rate was defined as the number of procedures performed per 10,000 individuals in a state. These rates were plotted on a choropleth map visualization scheme with Plotly (Montreal, Quebec, Canada, 2015).13,16
To understand the degree of heterogeneity of glaucoma surgery types across the United States, we subdivided the procedure counts across the 50 states into 5 major regions: West (AK, CA, CO, HI, ID, MT, NV, OR, UT, WA, WY), Southwest (AZ, NM, OK, TX), Midwest (IL, IN, IA, KS, MI, MN, MO, NE, ND, OH, SD, WI), Northeast (CT, ME, MA, NH, NJ, NY, PA, RI, VT) and Southeast (AL, AR, DE, FL, GA, KY, LA, MD, MS, NC, SC, TN, VA, WV). Next, we performed a chi-squared analysis with calculated standardized residuals to understand whether there were regional variations in glaucoma surgery preference. The standardized residual (SR) was calculated as follows, SR = (O - E)/√E, where O and E are the observed and expected procedure counts for a particular glaucoma surgery respectively. Residuals of absolute value greater than 2.00 were considered major influencers on the significance of the chi-squared test statistic. A p-value < 0.05 was used to define the cutoff of significance in our study.
All data and statistical analyses were performed in Python (Amsterdam, Netherlands), R software version 3.5.1 (Auckland, New Zealand), and Excel v16.18 (Redmond, WA, USA).16,17
Results
Rates of Glaucoma Surgeries in the United States and by Region
In the year of 2017, the elderly population above 65 was 50.7 million and 174,788 glaucoma surgeries were performed under Medicare Part B. Of those procedures, 22,862 were trabeculectomies (13.1%), 19,991 were GDI (11.4%), and 131,935 were MIGS (75.5%).
There was notable variation in the proportion of a regional population receiving surgeries for glaucoma. The Northeast region of the United States has a population of 9.4 million people older than 65 years, and a total of 34,558 glaucoma surgeries performed through Medicare in 2017. This yields an overall surgery rate of 36.9 per 10,000 individuals, which was the highest of all regions. The Southwest had a slightly lower overall rate of glaucoma surgery, with 36.2 surgeries per 10,000 followed by the Southeast with 35.7 surgeries per 10,000 individuals. The West and Midwest had the lowest glaucoma surgery rate at 33.6 and 30.5 surgeries per 10,000 individuals, respectively (Table 1).
 |
Table 1 Distribution of Glaucoma Surgeries in the 50 States and 5 Regions of the United States. Total number of surgeries and rates (per 10,000 individuals). |
There was notable variation of glaucoma surgery rate per state within larger geographical regions. In the Northeast, where glaucoma surgery rate was highest of the regions at 36.9 surgeries per 10,000 individuals, New Jersey had the highest rate of 68.8 surgeries per 10,000 individuals as compared to Rhode Island with the lowest rate of only 3.8. The Midwest had the lowest overall glaucoma surgery rate amongst regions of 30.5, but there were large variations between individual states. South Dakota had the highest statewide glaucoma surgery rate across the entire United States of 103.0 per 10,000 individuals, whereas Minnesota had a rate of only 15.9 per 10,000. In the Southwest, the range of surgery rates spanned from 10.6 in New Mexico to 64.4 in Oklahoma. In the Southeast, West Virginia had a rate of 16.0 while Virginia had a rate of 60.1. In the West region, the surgery rates spanned from 16.9 in Oregon to 42.2 in Utah (Table 1).
Variation in Glaucoma Surgical Preference Across the United States
Surgical rates for all types of glaucoma surgery (ie, trabeculectomy, glaucoma drainage implants, and MIGS) were plotted to create geographical choropleth heat maps (Figure 1). There was notable variability in the numbers of trabeculectomies, GDI, and MIGS procedures performed per 10,000 individuals by region. The Northeast had the highest overall trabeculectomy rate of 5.58 per 10,000 individuals followed by 4.62 in the Southeast, 4.17 in Midwest and lower rates of 4.08 in West and 3.79 in the Southwest (Table 1). GDI had the highest rate of 4.66 in the Southeast, followed by 4.36 in the Southwest, 3.76 in the Northeast, 3.64 in the West, and 3.16 in the Midwest. MIGS were performed at the highest rate of 28.05 per 10,000 individuals in the Southwest, followed by 27.58 in the Northeast, 26.39 in the Southeast, 25.90 in the West, and 23.17 in the Midwest (Table 1).
Within each region, there was variation in preference for certain glaucoma surgeries over others. In the Northeast, trabeculectomies accounted for 15.1% of all glaucoma procedures as compared to 74.7% MIGS. The Southeast had the highest proportion of GDI utilization of 13.1% compared to 74.0% MIGS usage. The Southwest and West had the largest preference for MIGS of 77.4% and 77.0% respectively (Figure 2A).
 |
Figure 2 (A) Regional and (B) statewide preference for trabeculectomy vs GDI vs MIGS in glaucoma management. Columns indicate the percentage of surgeries performed per region for each procedure type. |
There was also considerable variation in surgical preferences at the state level. Rhode Island and Arkansas had the highest statewide preferences for trabeculectomy of 35.8% and 33.2% respectively as compared to zero cases being performed through Medicare in South Dakota. Rhode Island and Mississippi had the highest preference for GDI at 28.4% and 18.7% as compared to Wyoming, where zero were reported through this database. Given the high rates of trabeculectomy and GDI in Rhode Island, it lags behind as the state with lowest MIGS rate of 35.8%. The top three states where MIGS was the most highly preferred modality of glaucoma surgery were South Dakota, Wyoming, and Oklahoma with rates of 94.6%, 94.4%, and 94.3%, respectively (Figure 2B).
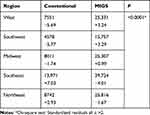
The heterogeneity in regional preferences for conventional surgeries (ie, trabeculectomy and GDI) versus MIGS was evaluated. A chi-squared test demonstrated a statistically significant difference in MIGS preference across the 5 regions of the United States (p < 0.0001). Standardized residuals (SR) were computed for each region and surgical category (conventional versus MIGS) and indicate the degree in which each region contributes to the overall variability of surgical preferences in the United States. As per convention, regions with absolute SR > 2 were considered significant contributors. In correspondence to high trabeculectomy and GDI surgery rates and relatively low MIGS rates in the Southeast, we observe a +7.03 SR for conventional surgeries and −4.01 SR for MIGS. Similarly, the Southwest and Western states have the highest MIGS surgery rate and contribute +3.29 and +3.24 SR toward the disproportional preference for MIGS surgeries respectively. Finally, the slight preference for conventional surgeries in the Northeast and MIGS in the Midwest corresponds to the SR contribution of +2.93 and +0.99, respectively, to the overall differences in surgical preference across the United States (Table 2).
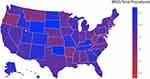
To assess the qualitative trends of glaucoma surgery preference, we generated a heatmap visualizing the proportion of MIGS to total procedures across all states (Figure 3). We observed large variations of MIGS preference across all states, with the highest rate of MIGS surgeries in South Dakota, Wyoming, and Oklahoma.
Finally, we explored the relationship between the availability of fellowship trained glaucoma specialists per state and MIGS usage. We computed the Pearson correlation between the number of glaucoma specialists in a state per 10,000 individuals and the MIGS usage rate per 10,000 individuals and got an R coefficient of −0.129 (p < 0.372) indicating a slightly negative correlation that was not statistically significant.
Discussion
The development of advanced data visualization software platforms facilitates analysis of geospatial datasets of unprecedented size and complexity. While data visualizations are traditionally used in business analytics, there has been an increasing popularity in applying these tools to clinical informatics and public health. In the field of ophthalmology and glaucoma, there have only been a handful of studies that have used geospatial heatmaps to investigate geographical and national trends on glaucoma prevalence and management strategies. Geographical variations in prescription rates for glaucoma and ocular hypertension have been studied in England.18 Cassard et al performed one of the largest national studies in the United States to elucidate the heterogenous distribution of glaucoma diagnosis across various regions.19 They found that there were substantial regional differences in diagnosed rates for all types of glaucoma, even after adjusting for patient characteristics and provider concentration, suggesting possible over diagnosis in some areas and/or under diagnosis in other areas.
With the advent of MIGS, there remain certain gaps in knowledge regarding how the landscape of glaucoma surgery preference looks across the United States. Prior studies have demonstrated an undeniable shift away from standard trabeculectomies to other alternatives. A Medicare study by Arora et al showed a national downtrend in trabeculectomy in exchange for mini-shunts done via external approach and periodic surveys of members from the American Glaucoma Society (AGS) between 1996 and 2008 have shown increased adoption of GDI over trabeculectomy.20,21 Furthermore, a recent study by Lee et al highlights a large drop in percentage of total Medicare payments attributed to trabeculectomy and GDI from 92.3% in 2007 to 21.2% in 2017.22 Payments for the iStent device alone represented 57.9% of the total payment in 2017, doubling that of conventional filtering surgeries.22 The rise in popularity of MIGS may also be attributed to their potential term cost-effectiveness in managing glaucoma as compared to SLT or medications alone.23 Berdahl et al reported that the projected cumulative cost at 5 years was lower in a two iStent treatment group compared to SLT or medications-only groups, with savings over SLT or medications-only of $309 and $1797. To complement these findings regarding trends in surgical management with visual analytics, our study provides visualization of the current landscape of glaucoma surgeries in the United States.
A recent Medicare database study performed by Khanna et al demonstrated high geographical variation in preference between trabeculectomy and GDI placement.24 Their study, based on data from 2014, demonstrated that GDI was used significantly more frequently than trabeculectomy within the South and Midwest regions relative to the Northeast. Our findings corroborate their results in that the Southeast and Southwest have the highest GDI surgery rates per capita. While we found the absolute GDI surgery rate for the Northeast in 2017 was the third highest of all regions, the trabeculectomy vs GDI rate was substantially higher in the Northeast than in all other regions, thus making the GDI to trabeculectomy preference the lowest and consistent with their study. Determinants of regional variations are likely multifactorial, and may be influenced by patient demographics and socioeconomic conditions, academic institutions which serve as investigational sites for studies, as well as the rigor and locale of training for regional physicians, who are mentored and taught similar techniques and preferences.24 Further studies performed on unified databases containing patient demographic and clinical data may elucidate more of the underlying drivers why MIGS adoption is faster in certain states than others.
The advent and growth of MIGS has largely impacted the way ophthalmologists are managing glaucoma patients in the United States. The transition from conventional surgeries to MIGS has not occurred at a uniform pace across all parts of the country. Our study elucidates how MIGS has altered the glaucoma treatment landscape. Our results show that MIGS is being performed at a higher rate in the Southwest and Northeast regions, but with the highest state-wide rates in South Dakota, Wyoming and Oklahoma. Even in the Southeast region, where MIGS usage is the lowest, MIGS still account for the overwhelming majority (74.0%) of all glaucoma surgeries performed.
We also examined if the number of glaucoma specialists per state was related to the number of MIGS being performed. There was a slightly negative correlation, but it was not statistically significant. This may indicate that MIGS are being performed by all ophthalmologists, not solely by glaucoma specialists. The number of glaucoma specialists in each state has no bearing on the number of MIGS being performed across the country.
There are limitations of this study. Medicare Part B is a database that only includes a certain subset of the population. We do not have data regarding glaucoma surgeries that were not charged under Medicare insurance. Furthermore, the publicly available data set is coarse in granularity as there is only aggregate information regarding the total number and charges for procedures for each state rather than individualized data regarding a patient’s demographic background. For instance, our data does not include clinical information regarding disease severity, intraocular pressure, peri-operative complication rates, patient co-morbidities, and long-term outcomes of vision preservation. Finally, it should be noted that the CMS Medicare Part B Carrier data are released a few years behind schedule. With the rapid advancements in MIGS, it should be taken into consideration that regional preferences in glaucoma intervention may have shifted since 2017.
It is also important to note, when performing future studies on underlying drivers for MIGS usage, that associations occurring at large aggregate levels may differ from associations measured at the individual scale. This phenomenon, better known as ecological bias, represents another limitation to be aware of when drawing inferences on correlations between MIGS utilization and underlying demographics. It is notable, however, that studies based solely on small regions or individual data may also potentially yield spurious patterns as a result of random variations across few events.25 To obtain a comprehensive understanding of the etiology behind MIGS geographical preference, one may need to combine the strengths of aggregate and individual level data through multi-levels modeling.26,27 Future work with richer databases with individual patient information regarding demographics and the course of glaucoma surgical management, such as the IRIS registry, may effectively build upon this study to identify definitive causative drivers of MIGS usage and elucidate the trends of glaucoma outcomes in relation to the evolving landscape of glaucoma surgical preference.28
We present “GlaucoMap”, a glaucoma choropleth map to visualize the distribution of glaucoma surgeries across the United States, and demonstrate the preferences for trabeculectomy, GDI and MIGS at the state and regional level. Our findings have multiple implications in understanding glaucoma treatment patterns. We provide the most recent snapshot of how glaucoma surgery has evolved in different states and regions. Visualizing trends and discrepancies are an important step to understanding the glaucoma landscape. This study also allows a visualization on the patterns of glaucoma surgery in the United States, and the different surgery rates in each state. We have characterized the regional preferences of both conventional and MIGS approach to glaucoma in the United States.
Conclusion
Micro-invasive glaucoma surgeries have greatly evolved the way in which ophthalmologists manage glaucoma. In this ecological study, we utilize heatmap visualizations to effectively demonstrate that the adoption of MIGS technology has not been occurring at an equal pace across various regions of the United States. We have characterized the regional preferences between conventional and MIGS approach to glaucoma surgeries.
Disclosure
Christopher Teng reports consulting fees from Neomedix and New World Medical, outside the submitted work. The authors have no other potential conflicts of interest to disclose.
References
1. Kingman S. Glaucoma is second leading cause of blindness globally. Bull World Health Organ. 2004;82(11):887–888. doi:/S0042-96862004001100019
2. Tham YC, Li X, Wong TY, et al. Global prevalence of glaucoma and projections of glaucoma burden through 2040: a systematic review and meta-analysis. Ophthalmology. 2014;121(11):2081–2090. doi:10.1016/j.ophtha.2014.05.013
3. Quigley HA, Broman AT. The number of people with glaucoma worldwide in 2010 and 2020. Br J Ophthalmol. 2006;90(3):262–267. doi:10.1136/bjo.2005.081224
4. Sharaawy T, Bhartiya S. Surgical management of glaucoma: evolving paradigms. Indian J Ophthalmol. 2011;59(Suppl):S123–30. doi:10.4103/0301-4738.73692
5. Khan M, Saheb H, Neelakantan A, et al. Efficacy and safety of combined cataract surgery with 2 trabecular micro bypass stents versus ab intern trabeculotomy. J Cataract Refract Surg. 2015;41(8):1716–1724. doi:10.1016/j.jcrs.2014.12.061
6. Rodriguez-Una I, Azuara-Blanco A, King AJ. Survey of glaucoma surgical preferences and post-operative care in the United Kingdom. Clin Experiment Ophthalmol. 2017;45(3):232–240. doi:10.1111/ceo.12846
7. Ahmed II. MIGS and the FDA: what’s in a Name? Ophthalmology. 2015;122(9):1737–1739. doi:10.1016/j.ophtha.2015.06.022
8. Kauh CY, Blachley TS, Lichter PR, et al. Geographic variation in the rate and timing of cataract surgery among US communities. JAMA Ophthalmol. 2016;134(3):267–276. doi:10.1001/jamaophthalmol.2015.5322
9. Raghupathi W, Raghupathi V. An empirical study of Chronic Diseases in the united states: a visual analytics approach. Int J Environ Res Public Health. 2018;15:3. doi:10.3390/ijerph15030431
10. Awalin S, Noh AS, Karol S, et al. Community health map: A geospatial and multivariate data visualization tool for public health datasets. Gov Inf Q. 2012;29(2):223–234. doi:10.1016/j.giq.2011.10.002
11. Elliott P, Wakefield J, Best N, Briggs D. Spatial Epidemiology: Methods and Applications. Oxford University Press;
12. Bostock M, Ogievetsky V, Heer J. D3: Data-Driven Documents. IEEE Trans Vis Comput Graph. 2011;18(12):2301–2309. doi:10.1109/TVCG.2011.185
13. Plotly Technologies Inc. Collaborative Data Science. QC: Montreal; 2015. Available from: https://plot.ly.
14. Tableau (version. 9.1). J Med Libr Assoc. 2016;104(2):182–183. doi:10.3163/1536-5050.104.2.022
15. Centers for Medicare & Medicaid Services. Limited Data Set (LDS) files; 2017. Available from: https://www.cms.gov/Research-Statistics-Data-and-Systems/Files-for-Order/LimitedDataSets/.
16. Python Software Foundation. Python language reference, version 2.7. Available from http://www.python.org.
17. R Core Team. R: A language and environment for statistical computing. R foundation for statistical computing. Vienna, Austria; 2018. Available from: http://www.R-project.org/.
18. Heng JS, Wormald R, Khaw PT. Geographical variation in glaucoma prescribing trends in England 2008-2012: an observational ecological study. BMJ Open. 2016;6(5):e010429. doi:10.1136/bmjopen-2015-010429
19. Cassard SD, Quigley HA, Gower EW, et al. Regional variations and trends in the prevalence of diagnosed glaucoma in the medicare population. Ophthalmology. 2012;119(7):1342–1351. doi:10.1016/j.ophtha.2012.01.032
20. Arora KS, Robin AL, Corcoran KJ, et al. Use of various glaucoma surgeries and procedures in medicare beneficiaries from 1994 to 2012. Ophthalmology. 2015;112(8):1615–1624. doi:10.1016/j.ophtha.2015.04.015
21. Vinod K, Gedde SJ, Feuer WJ, et al. Practice preferences for glaucoma surgery: a survey of the American Glaucoma Society. J Glaucoma. 2017;26(8):687–693. doi:10.1097/IJG.0000000000000720
22. Lee JH, Ma AK, Warren JL, et al. Impact of iStent microbypass shunt on medicare Part B glaucoma surgical expenditure. Ophthalmology Glaucoma. 2020. doi:10.1016/j.ogla.2020.05.004
23. Berdahl JP, Khatana AK, Katz LJ, et al. Cost-comparison of two trabecular micro-bypass stents versus selective laser trabeculoplasty or medications only for intraocular pressure control for patients with open-angle glaucoma. J Med Econ. 2017;20(7):760–766. doi:10.1080/13696998.2017.1327439
24. Khanna CL, Mahr MA, Hodge DO, et al. Variations in Trabeculectomy and Glaucoma drainage device use for the treatment of Glaucoma in the United States. Ophthalmology Glaucoma. 2018;1(2):139–143. doi:10.1016/j.ogla.2018.08.005
25. Rezaeian M, Dunn G, St Leger S, Appleby L. Geographical epidemiology, spatial analysis and geographical information systems: a multidisciplinary glossary. J Epidemiol Community Health. 2007;61(2):98–102. doi:10.1136/jech.2005.043117
26. Greenland S. Ecologic versus individual-level sources of bias in ecologic estimates of contextual health effects. Int J Epidemiol. 2001;30(6):1343–1350. doi:10.1093/ije/30.6.1343
27. Morgenstern H. Uses of ecologic analysis in epidemiologic research. Am J Public Health. 1982;72(12):1336–1344. doi:10.2105/AJPH.72.12.1336
28. Chiang MF, Sommer A, Rich WL, et al. The 2016 American Academy of Ophthalmology IRIS ((R)) Registry (Intelligent Research in Sight) database: characteristics and methods. Ophthalmology. 2018;125(8):1143–1148. doi:10.1016/j.ophtha.2017.12.001
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.