Back to Journals » Clinical Ophthalmology » Volume 11
Five-year outcomes of pars plana vitrectomy for macular edema associated with branch retinal vein occlusion
Authors Nishida A, Kojima H, Kameda T, Mandai M, Kurimoto Y
Received 28 September 2016
Accepted for publication 23 December 2016
Published 17 February 2017 Volume 2017:11 Pages 369—375
DOI https://doi.org/10.2147/OPTH.S123419
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Akihiro Nishida,1,2 Hiroshi Kojima,1,2 Takanori Kameda,1,2 Michiko Mandai,1,3 Yasuo Kurimoto1,2
1Department of Ophthalmology, Kobe City Medical Center General Hospital, 2Department of Ophthalmology, Institute of Biomedical Research and Innovation, 3Laboratory for Retinal Regeneration, RIKEN Center for Developmental Biology, Chuo-ku, Kobe, Hyogo, Japan
Purpose: Long-term outcomes of pars plana vitrectomy (PPV) for macular edema (ME) associated with branch retinal vein occlusion (BRVO) have been previously reported, but the studies did not report the number of additional treatments after surgery. During 5 years of follow-up, we therefore investigated the efficacy and safety of PPV for BRVO and evaluated the incidence of additional treatments.
Methods: We retrospectively reviewed the medical records of 25 eyes of 24 patients who underwent PPV for ME associated with BRVO and were followed up for at least 5 years. Best-corrected visual acuity was measured, and foveal thickness was assessed by optical coherence tomography. Additional treatments were also investigated.
Results: The logarithm of the minimal angle of resolution (logMAR) improved from 0.53±0.23 at baseline to 0.16±0.25 at 5 years (P<0.0001). The foveal thickness decreased from 535±222 µm at baseline to 205±143 µm at 5 years (P<0.0001). For the eyes with residual ME, the following additional treatments were performed within 5 years of follow-up: sub-Tenon injection of triamcinolone acetonide in two eyes, intravitreal injection of bevacizumab in three eyes, grid laser photocoagulation in one eye, and direct photocoagulation of macroaneurysm in one eye. Additional surgeries were performed in two eyes: for one eye, phacoemulsification extraction of the ocular lens and intraocular lens implantation were performed because of cataract progression, and for the other eye, additional PPV was done for postoperative retinal detachment.
Conclusion: PPV was effective for resolution of ME associated with BRVO and improved visual acuity with a small number of additional treatments during long-term follow-up.
Keywords: branch retinal vein occlusion, macular edema, pars plana vitrectomy, 5-year outcomes
Introduction
Macular edema (ME) is a major cause of visual impairment in patients with branch retinal vein occlusion (BRVO). Many treatments for this disorder have been reported, such as photocoagulation,1,2 intravitreal or sub-Tenon injection of triamcinolone acetonide (STTA),3–9 intravitreal tissue plasminogen activator injection,10,11 and dexamethasone intravitreal implantation.12 It has also been reported that pars plana vitrectomy (PPV) is effective for reducing ME and improving visual acuity (VA) in patients with BRVO.2,13–18 Although the precise mechanism by which PPV reduces ME is unknown, it has been suggested that PPV may have beneficial effects on retinal ischemia by allowing oxygenated fluid to circulate in the vitreous cavity,19 releasing vitreomacular attachment in persistent ME,17,20 improving perifoveal microcirculation,21 and/or increasing the clearance of VEGF in the vitreous cavity.22 Recently, intravitreal injection of anti-VEGF drugs (eg, bevacizumab, ranibizumab, and aflibercept) has been widely used and reported to be effective against ME associated with BRVO.23–28 However, recurrence of ME was often observed. In these cases, patients needed repeated injections, which could lead to increased risk of surgical complications as well as economic burdens. Therefore, it would be of benefit to the patients suffering from BRVO if the resolution of ME and improvement in VA could be maintained with minimal additional treatments. In this study, we investigated 5-year results of PPV for ME associated with BRVO to evaluate the efficacy and safety of the treatment as well as the incidences of additional treatments.
Subjects and methods
All procedures conformed to the tenets of the Declaration of Helsinki, and the study design was approved by the institutional review board of the Kobe City Medical Center General Hospital. The review board waived the need for written informed consent because the study design consisted of a retrospective chart review.
We retrospectively examined consecutive nonrandomized patients who underwent PPV for BRVO from September 2003 to October 2007 and completed a 5-year follow-up. Inclusion criteria were ME associated with BRVO, and best-corrected visual acuity (BCVA) was ≤0.6 in decimal VA. Exclusion criteria were proliferative diabetic retinopathy, vitreous hemorrhage, severe cataract, and other eye diseases that could contribute to visual loss. Eyes that were treated with PPV prior to the surgical intervention for BRVO were excluded. Eyes with previous scatter photocoagulation were included, but those with previous grid pattern photocoagulation were excluded.
BCVA was measured using Landolt ring charts and converted into the logarithm of the minimal angle of resolution (logMAR). Optical coherence tomography (OCT) was performed to measure foveal thickness using an OCT 2 (Carl Zeiss, Oberkochen, Germany), 3D OCT-1000 (Topcon, Tokyo, Japan), or Spectralis OCT (Heidelberg Engineering, Dossenheim, Germany). A standard three-port PPV was performed using a 20-G system or a 23-G system. A posterior vitreous detachment was induced if the cortical vitreous adhered to the retina. If the ME showed no improvement within 3 months after surgery, additional treatments such as STTA, grid laser photocoagulation, and intravitreal injection of bevacizumab (IVB) were performed.
All values were presented as mean ± standard deviation. Paired t-tests were used to compare preoperative and postoperative BCVAs. To compare preoperative and postoperative foveal thicknesses, Welch’s t-tests were used because of missing values. Differences were considered statistically significant when the P-values were <0.01 following the Bonferroni correction.
Results
From September 2003 to October 2007, 61 eyes of 59 patients underwent PPV for ME associated with BRVO. Among these cases, 35 patients (36 eyes) withdrew before the 5-year follow-up visit. The change in BCVA of the dropped out patients is shown in Figure S1. As a result, 25 eyes of 24 patients with ME associated with BRVO were included in this study. All cases except one eye that had received STTA were treatment-naïve. The baseline characteristics of the study patients are summarized in Table 1. The mean age of the patients at surgery was 66.7±8.8 years (range, 51–87 years) and included 14 male (one case who underwent PPV in both eyes was counted as two) and 11 female eyes. The major branch of the retinal vein was occluded in 13 eyes, and the macular branch was occluded in 12 eyes. Fluorescein angiography revealed that 6 eyes were ischemic (≥5 disk areas of capillary nonperfusion) and 19 were nonischemic. The mean estimated elapsed time from the onset of the disease to surgery was 6.2±9.2 months (range: 0.5–36 months). The lens status before surgery was phakic in 23 eyes and pseudophakic in 2 eyes. For 22 of 23 phakic eyes, phacoemulsification of the ocular lens and intraocular lens (IOL) implantation were performed together with PPV to avoid postoperative nuclear sclerosis (Table 2). Intravitreal injection of triamcinolone acetonide (TA), arteriovenous sheathotomy, and internal limiting membrane peeling were combined with PPV in eight, four, and four eyes, respectively (Table 2). Endophotocoagulation was performed in five cases: four for intraoperative iatrogenic retinal tears and one for capillary nonperfusion (Tables 2 and 3). Temporary elevation of intraocular pressure (>21 mmHg) was observed in four eyes, which was controlled with temporary topical antiglaucoma medication in all cases (Table 3). In one case, rhegmatogenous retinal detachment (RD) developed 3 months after the initial PPV (Table 3). An additional PPV was performed, and the retina was reattached (case 2 in Table 4). For one eye in which the physiological lens was preserved during the PPV, phacoemulsification and IOL implantation were performed at 19 months after the initial surgery because of cataract progression (case 7 in Table 4). Five of the 23 eyes in which phacoemulsification and IOL implantation had been performed simultaneously or subsequently to PPV required Nd:YAG laser posterior capsulotomy within the 5-year follow-up (cases 1, 5, 7, 8, and 9 in Table 4). Five of the 25 eyes required additional treatments for persistent ME that lasted >3 months postoperatively: STTA in two eyes, IVB in three eyes, grid laser photocoagulation in one eye, and direct photocoagulation of a macroaneurysm in one eye (cases 3, 4, 5, 6, and 10 in Table 4). There were no eyes that underwent repeated STTA or IVB.
  | Table 1 Baseline characteristics of the patients |
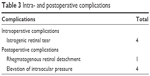  | Table 3 Intra- and postoperative complications |
The mean logMAR converted from the BCVA was 0.53±0.23 at baseline (Figure 1). Postoperatively, the mean BCVA changed to 0.43±0.29 (P=0.13) after 3 months, 0.33±0.27 (P=0.004) after 6 months, 0.32±0.30 (P=0.005) after 1 year, 0.26±0.29 (P=0.001) after 2 years, and 0.16±0.25 (P<0.0001) after 5 years (Figure 1). The mean BCVAs at the 6-month visit or later after surgery were significantly improved compared with baseline. The mean foveal thickness at baseline was 535±222 μm (n=23; Figure 2). Postoperatively, the mean foveal thickness significantly decreased to 315±94 μm (P=0.0003) after 3 months (n=15) and was maintained at a significant reduction until the 5-year visit: 370±112 μm (P=0.008) after 6 months (n=12), 327±161 μm (P=0.002) after 1 year (n=16), 257±139 μm (P=0.0003) after 2 years (n=10), and 205±143 μm (P<0.0001) after 5 years (n=19; Figure 2). Baseline and 5-year results of BCVA and foveal thickness with or without combined procedures such as intravitreal injection of TA, arteriovenous sheathotomy, and internal limiting membrane peeling were not significantly different, except for the baseline foveal thickness with or without internal limiting membrane peeling (Figure 3).
  | Figure 2 Changes in pre- and postoperative foveal thicknesses. |
Discussion
This study provided long-term results of PPV for ME associated with BRVO. Tachi et al17 reported that significant visual improvement was observed after PPV for BRVO in a follow-up period ranging from 12 to 32 months. Long-term outcomes of PPV with or without arteriovenous sheathotomy for BRVO have been previously reported.14,15,29 These reports showed improvement in VA from the baseline 31–48 months after PPV; however, they did not report the incidences of additional treatments after the initial surgical intervention. In this study, we investigated 5-year results of PPV for ME associated with BRVO to evaluate the efficacy and safety of treatment as well as the incidences of additional treatments. Resolution of ME and improvement in VA were achieved at 3 and 6 months after the initial surgery, respectively, and lasted as long as 5 years (Figures 1 and 2). The effects of combined procedures such as intravitreal injection of TA, arteriovenous sheathotomy, and internal limiting membrane peeling, albeit small numbers, were not clear on 5-year results of BCVA and foveal thickness (Figure 3). The most frequent additional treatment performed during the 5-year follow-up was Nd:YAG laser capsulotomy for posterior capsule opacification in 5 out of 23 eyes in which phacoemulsification and IOL implantation were performed simultaneously or subsequently to the PPV (22%; Table 4). The number of eyes that received additional treatments against residual ME, such as STTA, IVB, grid laser photocoagulation, and direct photocoagulation of macroaneurysms, was five (20%; Table 4), indicating that the majority of the eyes treated with PPV could maintain resolution of ME and improvement in VA without additional treatments for an extended period of time.
Recently, injections of anti-VEGF drugs such as bevacizumab, ranibizumab, pegaptanib, and aflibercept into the vitreous cavity have become a first-line treatment for ME associated with BRVO.23–28,30 Campochiaro et al31 reported 4-year outcomes for intravitreal injection of ranibizumab against BRVO and indicated that 50% of the patients had resolution of ME, defined as no intraretinal fluid without injection of ranibizumab for at least 6 months, with a mean follow-up of 50.2 months, suggesting that half of the patients could withdraw from anti-VEGF drugs longitudinally, while the other half still needed repeated injections, even in the fourth year.
Intravitreal anti-VEGF injections have been reported to have low complication rates. Recent studies reported that the incidences of rhegmatogenous RD after anti-VEGF injections were 0.013%–0.10%.32–34 Endophthalmitis occurred in 0.036–0.09% of the eyes after intravitreal injection of anti-VEGF drugs.32,35 On the other hand, Savastano et al36 reported that RD developed in 1.77% of the eyes that underwent 25-G high-speed PPV. A recent large-scale study reported that the incidences of postoperative endophthalmitis were 0.020% (4 of 19,865 eyes), 0.028% (3 of 10,845 eyes), and 0.021% (1 of 4,717 eyes) for 20-G, 23-G, and 25-G systems, respectively.37
Summarizing these reports, the risk of postoperative RD in PPV was 10- to 100-fold higher than that in intravitreal injection. Indeed, postoperative RD occurred in one case in the present study (Tables 3 and 4). In contrast, the incidences of postoperative endophthalmitis were not so much different between PPV and intravitreal injections. It is possible that multiple injections increased the risk of endophthalmitis, potentially more than that of a single PPV. Therefore, although the application of PPV should be restricted, it may have an advantage in cases that require repeated injections of anti-VEGF drugs for maintaining resolution of ME.
Limitations of this study involve the retrospective data collection and the relatively small number of cases. More than half of the patients did not complete 5-year follow-up. It is possible that the patients with poor VA stopped to come to hospital before 5-year follow-up. To minimize the bias, we analyzed the patients who had completed 5-year follow-up; however, we cannot eliminate the possibility described earlier. Nonuniformity of surgical procedure among cases, such as intravitreal injection of TA, arteriovenous sheathotomy, and internal limiting membrane peeling, is another drawback of this study. However, we believe that our study provides valuable insight into the long-term outcomes of PPV for BRVO.
Conclusion
PPV was effective for improvement in VA and resolution of ME associated with BRVO. The effects lasted at least 5 years with minimal additional treatments. Although the incidences of postoperative RD were higher than that in intravitreal injections, PPV may have an advantage in cases that require repeated injections of anti-VEGF drugs, because a smaller number of additional treatments can avoid the risks associated with repeated injections. Further investigation is required to clarify whether PPV is also effective for anti-VEGF-treated eyes.
Acknowledgment
The authors confirmed no financial support was received for this study.
Disclosure
The authors report no conflicts of interest in this work.
References
The Branch Vein Occlusion Study Group. Argon laser photocoagulation for macular edema in branch vein occlusion. Am J Ophthalmol. 1984;98(3):271–282. | ||
Harino S, Bessho K, Kida T. Prospective multicenter study of visual outcomes following three different treatments for macular edema associated with branch retinal vein occlusion: a study by the Japanese BRVO study group. Jpn J Ophthalmol. 2012;56(3):250–261. | ||
Cekic O, Chang S, Tseng JJ, et al. Intravitreal triamcinolone injection for treatment of macular edema secondary to branch retinal vein occlusion. Retina. 2005;25(7):851–855. | ||
Chen SD, Sundaram V, Lochhead J, Patel CK. Intravitreal triamcinolone for the treatment of ischemic macular edema associated with branch retinal vein occlusion. Am J Ophthalmol. 2006;141(5):876–883. | ||
Karacorlu M, Ozdemir H, Karacorlu SA. Resolution of serous macular detachment after intravitreal triamcinolone acetonide treatment of patients with branch retinal vein occlusion. Retina. 2005;25(7):856–860. | ||
Kawaji T, Hirata A, Awai N, et al. Trans-Tenon retrobulbar triamcinolone injection for macular edema associated with branch retinal vein occlusion remaining after vitrectomy. Am J Ophthalmol. 2005;140(3):540–542. | ||
Lee H, Shah GK. Intravitreal triamcinolone as primary treatment of cystoid macular edema secondary to branch retinal vein occlusion. Retina. 2005;25(5):551–555. | ||
Oh JY, Seo JH, Ahn JK, Heo JW, Chung H. Early versus late intravitreal triamcinolone acetonide for macular edema associated with branch retinal vein occlusion. Korean J Ophthalmol. 2007;21(1):18–20. | ||
Patel PJ, Zaheer I, Karia N. Intravitreal triamcinolone acetonide for macular oedema owing to retinal vein occlusion. Eye. 2008;22(1):60–64. | ||
García-Arumí J, Martinez-Castillo V, Boixadera A, Blasco H, Corcostegui B. Management of macular edema in branch retinal vein occlusion with sheathotomy and recombinant tissue plasminogen activator. Retina. 2004;24(4):530–540. | ||
Murakami T, Takagi H, Kita M, et al. Intravitreal tissue plasminogen activator to treat macular edema associated with branch retinal vein occlusion. Am J Ophthalmol. 2006;142(2):318–320. | ||
Haller JA, Bandello F, Belfort R Jr, et al; OZURDEX GENEVA Study Group. Randomized, sham-controlled trial of dexamethasone intravitreal implant in patients with macular edema due to retinal vein occlusion. Ophthalmology. 2010;117(6):1134.e–1146.e. | ||
Figueroa MS, Torres R, Alvarez MT. Comparative study of vitrectomy with and without vein decompression for branch retinal vein occlusion: a pilot study. Eur J Ophthalmol. 2004;14(1):40–47. | ||
Kumagai K, Furukawa M, Ogino N, Larson E, Uemura A. Long-term visual outcomes after vitrectomy for macular edema with foveal hemorrhage in branch retinal vein occlusion. Retina. 2007;27(5):584–588. | ||
Kumagai K, Furukawa M, Ogino N, Uemura A, Larson E. Long-term outcomes of vitrectomy with or without arteriovenous sheathotomy in branch retinal vein occlusion. Retina. 2007;27(1):49–54. | ||
Saika S, Tanaka T, Miyamoto T, Ohnishi Y. Surgical posterior vitreous detachment combined with gas/air tamponade for treating macular edema associated with branch retinal vein occlusion: retinal tomography and visual outcome. Graefes Arch Clin Exp Ophthalmol. 2001;239(10):729–732. | ||
Tachi N, Hashimoto Y, Ogino N. Vitrectomy for macular edema combined with retinal vein occlusion. Doc Ophthalmol. 1999;97(3–4):465–469. | ||
Yamamoto S, Saito W, Yagi F, Takeuchi S, Sato E, Mizunoya S. Vitrectomy with or without arteriovenous adventitial sheathotomy for macular edema associated with branch retinal vein occlusion. Am J Ophthalmol. 2004;138(6):907–914. | ||
Williamson TH, Poon W, Whitefield L, Strothidis N, Jaycock P. A pilot study of pars plana vitrectomy, intraocular gas, and radial neurotomy in ischaemic central retinal vein occlusion. Br J Ophthalmol. 2003;87(9):1126–1129. | ||
Takahashi MK, Hikichi T, Akiba J, Yoshida A, Trempe CL. Role of the vitreous and macular edema in branch retinal vein occlusion. Ophthalmic Surg Lasers. 1997;28(4):294–299. | ||
Noma H, Funatsu H, Sakata K, Mimura T, Hori S. Macular microcirculation before and after vitrectomy for macular edema with branch retinal vein occlusion. Graefes Arch Clin Exp Ophthalmol. 2010;248(3):443–445. | ||
Lee SS, Ghosn C, Yu Z, et al. Vitreous VEGF clearance is increased after vitrectomy. Invest Ophthalmol Vis Sci. 2010;51(4):2135–2138. | ||
Campochiaro PA, Clark WL, Boyer DS, et al. Intravitreal aflibercept for macular edema following branch retinal vein occlusion: the 24-week results of the VIBRANT study. Ophthalmology. 2015;122(3):538–544. | ||
Campochiaro PA, Hafiz G, Shah SM, et al. Ranibizumab for macular edema due to retinal vein occlusions: implication of VEGF as a critical stimulator. Mol Ther. 2008;16(4):791–799. | ||
Campochiaro PA, Heier JS, Feiner L, et al; BRAVO Investigators. Ranibizumab for macular edema following branch retinal vein occlusion: six-month primary end point results of a phase III study. Ophthalmology. 2010;117(6):1102–1112. | ||
Pai SA, Shetty R, Vijayan PB, et al. Clinical, anatomic, and electrophysiologic evaluation following intravitreal bevacizumab for macular edema in retinal vein occlusion. Am J Ophthalmol. 2007;143(4):601–606. | ||
Rabena MD, Pieramici DJ, Castellarin AA, Nasir MA, Avery RL. Intravitreal bevacizumab (Avastin) in the treatment of macular edema secondary to branch retinal vein occlusion. Retina. 2007;27(4):419–425. | ||
Stahl A, Agostini H, Hansen LL, Feltgen N. Bevacizumab in retinal vein occlusion-results of a prospective case series. Graefes Arch Clin Exp Ophthalmol. 2007;245(10):1429–1436. | ||
Oh IK, Kim S, Oh J, Huh K. Long-term visual outcome of arteriovenous adventitial sheathotomy on branch retinal vein occlusion induced macular edema. Korean J Ophthalmol. 2008;22(1):1–5. | ||
Udaondo P, Garcia-Delpech S, Salom D, Garcia-Pous M, Diaz-Llopis M. Intravitreal pegaptanib for refractory macular edema secondary to retinal vein occlusion. Clin Ophthalmol. 2011;5:941–944. | ||
Campochiaro PA, Sophie R, Pearlman J, et al; RETAIN Study Group. Long-term outcomes in patients with retinal vein occlusion treated with ranibizumab: the RETAIN study. Ophthalmology. 2014;121(1):209–219. | ||
Day S, Acquah K, Mruthyunjaya P, Grossman DS, Lee PP, Sloan FA. Ocular complications after anti-vascular endothelial growth factor therapy in Medicare patients with age-related macular degeneration. Am J Ophthalmol. 2011;152(2):266–272. | ||
Meyer CH, Michels S, Rodrigues EB, et al. Incidence of rhegmatogenous retinal detachments after intravitreal antivascular endothelial factor injections. Acta Ophthalmol. 2011;89(1):70–75. | ||
Wu L, Martinez-Castellanos MA, Quiroz-Mercado H, et al. Twelve-month safety of intravitreal injections of bevacizumab (Avastin): results of the Pan-American Collaborative Retina Study Group (PACORES). Graefes Arch Clin Exp Ophthalmol. 2008;246(1):81–87. | ||
Rayess N, Rahimy E, Storey P, et al. Postinjection endophthalmitis rates and characteristics following intravitreal bevacizumab, ranibizumab, and aflibercept. Am J Ophthalmol. 2016;165:88–93. | ||
Savastano A, Savastano MC, Barca F, Petrarchini F, Mariotti C, Rizzo S. Combining cataract surgery with 25-gauge high-speed pars plana vitrectomy: results from a retrospective study. Ophthalmology. 2014;121(1):299–304. | ||
Wu L, Berrocal MH, Arevalo JF, et al. Endophthalmitis after pars plana vitrectomy: results of the Pan American Collaborative Retina Study Group. Retina. 2011;31(4):673–678. |
Supplementary material
  | Figure S1 Changes in pre- and postoperative logMAR of the patients who withdrew before the 5-year follow-up visit. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.




