Back to Journals » Clinical Ophthalmology » Volume 15
Fear Associated with COVID-19 in Patients with Neovascular Age-Related Macular Degeneration
Authors Rozon JP , Hébert M , Bourgault S, Caissie M, Letartre L, Tourville E, Dirani A
Received 3 January 2021
Accepted for publication 19 February 2021
Published 16 March 2021 Volume 2021:15 Pages 1153—1161
DOI https://doi.org/10.2147/OPTH.S300239
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
Jean-Philippe Rozon,1,2 Mélanie Hébert,2 Serge Bourgault,2 Mathieu Caissie,2 Laurence Letartre,2 Eric Tourville,2 Ali Dirani2
1Faculty of Medicine, Université Laval, Québec, QC, Canada; 2Department of Ophthalmology, Centre Universitaire d’Ophtalmologie, CHU de Québec – Université Laval, Québec, QC, Canada
Correspondence: Ali Dirani
Department of Ophthalmology, Hôpital du Saint-Sacrement, 1050 Ste-Foy Street, Quebec City, QC G1S 4L8, Canada
Tel +1 418 525-4444
Fax +1 418 682-7557
Email [email protected]
Purpose: Since the beginning of the COVID-19 pandemic, news related to the pandemic has created a feeling of fear, particularly among high-risk groups including elderly patients. This study aimed to assess the fear associated with COVID-19 and to evaluate the fear of vision decrease related to the delay of treatment in neovascular age-related macular degeneration patients (nAMD) during the pandemic.
Patients and Methods: This is a prospective cross-sectional study of 160 actively treated patients with nAMD enrolled between September and November 2020 at a tertiary hospital in Québec, Canada. For each participant, demographic and clinical data were collected. The anxiety was rated in a questionnaire composed of two sections: the Fear of COVID-19 Scale (FCV-19S) and eight additional questions to assess ophthalmology-related COVID-19 statements.
Results: The mean ± standard deviation level of FCV-19S was 17.05± 4.38. In the multivariable analysis, it was significantly higher in women (p< 0.001) and lower in patients with a high school education vs elementary school (p=0.009). In the ophthalmology-related statements, 16% feared vision loss because of difficulties in maintaining regular follow-ups during the pandemic. The female gender was significantly associated with a higher tendency to postpone their appointment (p=0.03). No association was found between the patients’ underlying disease characteristics and higher fear of vision loss.
Conclusion: Despite the massive impact of the pandemic, anxiety related to COVID-19 and delaying ophthalmology treatments remained relatively low in nAMD patients. Greater explanations to address this fear may reduce anxiety level, especially among female patients and those with an elementary school education.
Keywords: vision loss fear, fear assessment, Fear of COVID-19 Scale, anti-VEGF
Plain Language Summary
Since the COVID-19 pandemic began, related news has created a feeling of fear, particularly among high-risk groups like elderly patients. However, this COVID-19 fear compared to the fear of vision loss due to treatment delay in ophthalmological patients has not yet been studied. Therefore, we performed a study to assess these elements in neovascular age-related macular degeneration patients, which are mainly elderly people who require regular follow-ups for assessments and treatments. We concluded that the fear related to COVID-19 and treatment delay remained relatively low in this population. Nonetheless, a special attention should be provided to female patients and less educated patients who are two subgroups with greater COVID-19 fear. No association was found between the patients’ underlying disease characteristics and higher fear of vision loss. Therefore, being aware of the fear of COVID-19 and its risk factors in ophthalmology patients can help eyecare professionals to better tailor their approach to patient expectations during the pandemic.
Introduction
On March 11, 2020, the World Health Organization (WHO) declared the coronavirus disease 2019 (COVID-19) a pandemic.1 In the following weeks, most governments announced the implementation of sanitary measures to slow the spread, including statewide lockdowns, bans on gatherings, indoor face masks, and limitations on large public gatherings. Further restrictions were incorporated in healthcare, such as limiting elective surgical procedures, prohibiting visitors, and implementing teleconsultations.2 Despite government reassurance, the rapid increase in cases and deaths around the world increased anxiety and fear of the disease, particularly among high-risk populations, such as the elderly and immunosuppressed people. Moreover, some important psychological problems (eg psychosis, anxiety, depression, and psychological trauma) are known to be caused by epidemics and pandemics, such as COVID-19 pandemics.3–5 Fear and anxiety of COVID-19 have changed our functioning in most aspects of life.
Age-related macular degeneration (AMD) is an acquired degenerative disease of the retina that causes significant central visual impairment. The neovascular form (nAMD) is currently the leading cause of legal blindness in the United States.6 This pathology mainly affects elderly people who are also at higher risk of morbidity and mortality due to COVID-19.7 These nAMD patients require regular follow-ups for assessments and treatment using intravitreal injections. As a result of implementing the necessary pandemic measures, ophthalmology departments have seen a significant drop in daily patient visits and an inability to maintain an optimal interval between treatments.8,9 The addition of all these factors could make nAMD patients at high risk of COVID-19 fear. The present study aimed to evaluate the fear of COVID-19 and the fear of vision loss in nAMD patients, as well as its risk factors.
Methods
This non-interventional cross-sectional study was approved by the Institutional Review Board of the Centre hospitalier universitaire de Québec – Université Laval and adhered to the tenets of the Declaration of Helsinki. It was performed in an ophthalmology tertiary care center (CHU de Québec – Université Laval) in Québec, Canada between September 17th and November 10th, 2020. It took place during the second wave of COVID-19 which led to new implementations of province-wide restrictions.
All consecutive patients treated for nAMD in the Hôpital du Saint-Sacrement were invited to participate in this study during the injection clinics. Eligible patients were adults diagnosed with nAMD receiving intravitreal injection of anti-vascular endothelial growth factor (VEGF). Exclusion criteria included history of diabetic retinopathy, patients with memory disorders, or patients who did not complete the questionnaire. Patients receiving intravitreal injections for other retinal diseases (eg diabetic macular edema, macular edema related to venous occlusions) and patients having additional causes of choroidal neovascularization (CNV) other than nAMD were not included in the study. Written consent was systematically obtained. All the questionnaires were completed in person. Among patients who were approached to participate in this study, the rate of enrollment was 82.9% (n = 160/193).
Data collection included demographic data (ie age, gender), highest education obtained (ie elementary school, high school, college, university, or other), type of residence (ie house, condo/apartment, retirement home, residential, and long-term care center or other), marital status (ie single, married, widowed, or other), disease laterality (ie unilateral or bilateral), duration since nAMD diagnosis, type of anti-VEGF (ie bevacizumab, ranibizumab, or aflibercept), total number of anti-VEGF injections since diagnosis, duration since the last injection, and visual acuity at the last injection before recruitment. Best-corrected visual acuity (BCVA) was converted to an Early Treatment Diabetic Retinopathy Study (ETDRS) letter score from an imperial scale (Snellen).
The questionnaire consisted of two sections: the seven-item Fear of COVID-19 Scale (FCV-19S) and eight additional questions to assess ophthalmology-related COVID-19 statements (Table 1).10 The FCV-19S is a quick and easy-to-use tool that underwent careful psychometric testing and is the most prevalent tool for the assessment of COVID-19 anxiety.2,10 In our study, the FCV-19S was translated to French. No additional validity and reliability test has been conducted except a pre-test to verify the good understanding of the questionnaire. The eight additional statements aimed to assess four specific aspects: fear of vision loss (statements 8–9), fear of COVID-19 compared to fear of vision loss (statements 10–11), fear of COVID-19 risks during follow-ups (statements 12–13), and confidence in in-hospital sanitary precautions (statements 14–15). The latter refers to all sanitary measures implemented and/or reinforced since the beginning of the pandemic at the hospital. These include measures to disinfect the examination rooms between patients, mandatory mask-wearing, handwashing before and after each patient interaction, physical distancing in the waiting rooms, and screening questionnaires for COVID-19 symptoms before appointments to assess the risk of infection.
Participants were asked to rate their level of agreement with each statement using a 5-point Likert scale, including “strongly disagree”, “disagree”, “neither agree nor disagree”, “agree”, and “strongly agree”. Each answer was converted into a scale from 1 to 5 in order of increasing agreement. Given the changes to the original FCV-19S (ie French translation and additional statements), a pretest was conducted among 25 participants across different age groups to assess the complete questionnaire. A 4-point Likert scale was used to test whether the individuals understand the item descriptions. Most participants (84.0%) had a good understanding of the statements, so no changes needed to be made. In addition, all patients were asked if they preferred to complete the questionnaire by themselves or have it read and explained by a member of the research team.
Statistical Analysis
Baseline demographics were summarized by presenting the frequency and percentage for categorical variables and the average ± standard deviation (SD) for continuous variables. The primary outcome was the FCV-19S score. This ranges from 7 to 35 points by adding the numerical results for each statement. A higher score corresponds to greater fear of COVID-19, and as in other studies, this score was treated as a continuous variable. Secondary outcomes were the ophthalmology-related statements, specifically on vision (statements 8–9), on COVID-19 (statements 10–11), on follow-ups (statements 12–13), and on hospital precautions (statements 14–15). Each pair of statements ranged from 2 to 10 points and was treated as an ordinal variable. Differences in scores were compared between demographic groups using Mann–Whitney U-test and Kruskal–Wallis test as appropriate for continuous variables. Spearman’s rho was used to evaluate the correlations between the FCV-19S and the ophthalmology-related statements. A Spearman’s rho of 0.00 to 0.29 was deemed a negligible correlation, 0.30 to 0.49 a weak correlation, 0.50 to 0.69 a moderately strong correlation, 0.70 to 0.89 a strong correlation, and 0.9 to 1.0 a very strong correlation.11
A multivariable linear regression model was built for FCV-19S score. All demographic characteristics were considered for inclusion in the model and variables that had an impact on FCV-19S score at the p<0.20 significance level in univariable analysis were included in the final model. A multivariable ordinal regression model was then built for each pair of ophthalmology-related statements using the same demographic variables used in the final multivariable linear regression model for the FCV-19S score to test whether the same risk factors influenced the agreement of patients on the ophthalmology-related statements.
Statistical analyses were performed using IBM SPSS Statistics for Windows, version 25 (IBM Corp., Armonk, N.Y., USA). Statistical significance was set at α = 0.05.
Results
Study Participants
A total of 160 patients were enrolled in the study (Table 2). There were 111 women (69.4%) and 49 men (30.6%), and mean ± standard deviation (SD) age was 82±8 years (range: 60–100). Most participants had a high school degree (44.4%). The “other” education category was mainly composed of patients that obtained a “commercial course” degree, which represented an alternative to high school, but this category remains heterogeneous.
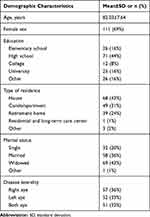 |
Table 2 Demographic Characteristics of 160 Study Participants |
FCV-19S
The results of the FCV-19S are presented in Table 1. Mean ± SD total FCV-19S score was 17.05±4.38 (range: 7–28). More than half of patients (54%) agreed that they were afraid of COVID-19, while other statements did not have a similar rate of agreement (Figure 1). The FCV-19S was significantly higher in female patients compared to male with 17.8±4.3 compared to 15.4±4.0, respectively (p<0.001). However, there were no significant differences in FCV-19S based on education, residence type, marital status, or bilateral disease. This was consistent with the results in the linear regression models for FCV-19S (Table 3). This analysis showed that female sex was a significant independent predictor for higher FCV-19S score (p<0.001), while patients with a high school education were more likely to have lower FCV-19S scores compared to patients with an elementary school level of education (p=0.009). The other demographic and disease characteristics were not independent factors influencing FCV-19S score.
 |
Table 3 Multivariable Linear Regression for Risk of Higher Score on “Fear of COVID-19 Scale” Adjusting for Baseline Patient Characteristics in Neovascular Age-Related Macular Degeneration Patients |
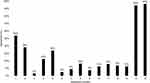 |
Figure 1 Percentage of patients who either “agree” or “strongly agree” with each statement in the questionnaire. |
Ophthalmology-Related Statements
Approximately one in six patients (16%) feared vision loss because of difficulties in maintaining regular follow-ups during the pandemic, while fewer patients (13%) would rather lose vision than risk getting infected by COVID-19 or postpone their appointments as a consequence (Table 1 and Figure 1). Almost all participants (96%) were confident in the sanitary and social distancing measures implemented at the hospital during their appointment. Female sex again led to a higher agreement with postponing follow-ups (male: 3.7±1.3 vs female: 4.5±2.0; p=0.03). Perception of hospital measures was also significantly different across education levels, specifically in pairwise comparisons between high school (8.2±1.2) and other levels (vs elementary school = 8.8±1.1, p=0.04; vs college = 9.0±1.0, p=0.02; vs university = 8.7±1.1, p=0.05). The multivariable ordinal regression models revealed few independent risk factors relating to the ophthalmology-related statements (Table 4). Female sex was an independent risk factor for fear of COVID-19 at the expense of vision (p=0.05). Indeed, female participants present a higher level of agreement towards these statements, meaning they would prefer sacrificing their vision in order to avoid contracting COVID-19. Finally, confidence in the in-hospital sanitary measures was lower in patients with a high school education compared to elementary school (p=0.04). This is consistent with the significant differences in agreement across education levels with high school being specifically lower than other levels.
The FCV-19S had a negligible but significant correlation with the ophthalmology-related statements on vision (r = 0.282, p<0.001), on COVID-19 (r = 0.188, p=0.02), and on follow-ups (r = 0.242, p=0.002), while it did not correlate with confidence in in-hospital sanitary measures (r = 0.032, p=0.69). This correlation means that patients with higher FCV-19S score also had a greater fear of vision loss, but preferred taking the risk of vision decrease rather than getting infected with COVID-19. The COVID-19 statements correlated with the vision statements (r = 0.187, p=0.02), but more so with the follow-up statements (r = 0.349, p<0.001). Patients who preferred taking the risk of vision decrease rather than getting infected with COVID-19 were also more likely to consider postponing their appointment. The statements on hospital measures did not correlate with any of the other pairs except for a negative correlation to follow-ups (r = −0.236, p=0.003). Patients who did not trust the hospital measures as much were, therefore, more likely to also favor postponing or cancelling their follow-ups.
Discussion
Anxiety and fear associated with COVID-19 and vision loss among nAMD patients have not yet been studied. However, since the elderly patients are vulnerable and mortality rates among them are higher than in a general population, they may experience greater fear of COVID-19.7 While most studies about COVID-19 fear were conducted among people between 20 and 50 years of age, the elderly were sparsely studied probably due to the recruitment method of most past studies (eg online survey).12,13 Thus, carrying out studies in older populations is crucial in order to have a better assessment of the current situation. In our study, we showed that COVID-19 fear is highly prevalent among this population. Moreover, we have found that the FCV-19S was higher in women and participants with an elementary school diploma as the highest education obtained. In general, the anxiety level is higher in female individuals than in male according to the literature.2 Indeed, this observation among female patients is consistent with previous studies about COVID-19 conducted in the general population.12–14 We have not found any significant differences in COVID-19-related anxiety regarding patients’ age, type of residence, marital status, and disease laterality.
A few questionnaires and scales were proposed to evaluate the fear of patients, but the first validated scale was FCV-19S.10 In our study, the mean score was 17.05±4.38 which is comparable to the reported mean levels in other studies (13.34 to 27.39).12,15 However, the direct comparison is difficult due to differences in time of assessment and study populations (eg mean age among study participants, specific populations). Moreover, our study was conducted almost 6 months after the beginning of pandemic measures in Canada. In comparison, most studies performed earlier in Iran, Italy, or Poland were within the first 3 months of the pandemic and reported similar levels of anxiety.2,12,13 For example, Soraci et al questioned 249 Italians from the general population (average age: 34.5 years) in mid-March 2020. They reported an average FCV-19S score of 16.86±6.06.13 In our study, we expected lower levels of fear because patients were dealing with the pandemic for more than 6 months. However, the similar levels of anxiety between our cohort and others who were questioned at the height of the pandemic suggest that the older age in our cohort may balance out this effect.
The infection rate is 1681 per 100,000 in Quebec compared to 2642 in Poland, 2681 in Italy and 3543 in Spain.16 However, the fatality rate is higher in Quebec (4.93%) as compared to most European countries: 1.76% in Poland, 3.48% in Italy and 2.75% in Spain.16 This may also contribute to the relative increase in the fear of COVID-19 in our population.
On the other hand, the evaluation of fear related to vision loss in this population is also highly important. The current treatment of nAMD using regular intravitreal injections requires an optimal compliance to preserve visual acuity. Therefore, patients must be confident about hospital precautions regarding COVID-19 to limit their anxiety and its negative impacts on follow-up adherence. In our study, we showed that the fear of pandemic-related vision loss is limited. This result may be explained by good management of injection clinics during the pandemic which could reassure patients about their treatments. Similar results were found regarding follow-ups though female patients were more prone to postpone them. This finding may be explained by their higher level of COVID-19 anxiety which encourages them to reduce their physical interactions as recommended by public health services. Surprisingly, no association was found between the ophthalmology-related statements results and patients’ underlying disease characteristics (eg worse visual acuity, status of the fellow eye and bilateral disease). Thus, monopthalmic patients or patients with low vision did not have a significantly higher level of anxiety compared to others. The personal demographic characteristics (especially sex and education) seemed to be the main determining factor for anxiety.
Due to a lower number of daily patient visits, the recruitment was realized over a 2-month period. However, the level of anxiety may have varied depending on the number of daily COVID-19 infections and deaths that had progressively increased over weeks in the province of Quebec. The moment of enrolment may have affected the results as the anxiety level was measured only once in our study.
No data were collected on concomitant medications, such as anxiolytics and antidepressants that could have a substantial impact on the emotional perception of anxiety. Moreover, the significant prevalence of visual disturbances among the participants may have slightly impacted the quality of answers. Indeed, statements might not have been perfectly read and understood by all, and consequently not reflect their state of mind entirely. In order to limit its likelihood, all patients were asked if they preferred to complete the questionnaire by themselves or have it read and explained by a member of the research team. Additionally, factors like socioeconomic status, news watching habits, and social media usage may affect anxiety levels.2,17,18 However, these were not evaluated in a measurable and objective manner. Moreover, since only patients who showed up for their appointment have been recruited, it is possible that patients with higher levels of anxiety did not show up to their appointment and therefore were not included in the study.
To the best of our knowledge, this is the first study to evaluate the fear of COVID-19 and vision loss in a population of nAMD patients during the pandemic. It is important to address these issues that impact the treatment adherence and subsequently visual acuity. Greater explanations to address this anxiety in ophthalmology during phone and in-person visits may reduce it further.19 A special attention should be provided to female patients and patients with an elementary school education who are two subgroups with greater COVID-19 fear. Likewise, being aware of this fear can help eyecare professionals to better tailor their approach to the patient’s expectations during the pandemic. In specific cases, telemedicine could also be used to perform a pre-visit to reassure patients and answer their questions, which could improve their compliance.
Abbreviations
AMD, age-related macular degeneration; COVID-19, coronavirus disease 2019; FCV-19S, Fear of COVID-19 Scale; nAMD, neovascular age-related macular degeneration; VEGF, vascular endothelial growth factor.
Data Sharing Statement
All data relevant to the study are included in the article. The datasets used and/or analysed during the present study are available from the corresponding author on reasonable request.
Ethics Approval and Informed Consent
The Institutional Review Board of the Centre hospitalier universitaire de Québec – Université Laval provided the ethical approval (Reference: 2021-5388). Direct written patient consent was obtained for data collection and analysis. All participants were ensured concerning the confidentiality and anonymity of their data. They were informed about their right to retract their data at any time.
Consent for Publication
Direct written patient consent was obtained for publication.
Acknowledgments
The authors would like to thank the Centre Universitaire d'Ophtalmologie clinical research team for their support of this research study (Marcelle Giasson and Johanne Doucet).
Author Contributions
All authors made a significant contribution to the work reported, whether that is in the conception, study design, execution, acquisition of data, analysis and interpretation, or in all these areas; took part in drafting, revising or critically reviewing the article; gave final approval of the version to be published; have agreed on the journal to which the article has been submitted; and agree to be accountable for all aspects of the work.
Funding
The authors did not receive support from any organization for the submitted work. Funded without commercial support by the authors.
Disclosure
The authors declare that they have no competing interests related to the work submitted. Serge Bourgault and Eric Tourville are consultants and members of ad-board for Bayer and Novartis, outside the submitted work. Eric Tourville is also a consultant to Roche. Ali Dirani is a member of the ad-board for Bayer and Novartis, outside the submitted work. Jean-Philippe Rozon, Mélanie Hébert, Mathieu Caissie and Laurence Letartre have nothing to disclose.
References
1. Cucinotta D, Vanelli M. Who declares COVID-19 a pandemic. Acta Biomed. 2020;91:157–160. doi:10.23750/abm.v91i1.9397
2. Sigorski D, Sobczuk P, Osmola M, et al. Impact of COVID-19 on anxiety levels among patients with cancer actively treated with systemic therapy. ESMO Open. 2020;5(5):e000970. doi:10.1136/esmoopen-2020-000970
3. WHO. Mental health and psychosocial considerations during the COVID-19 outbreak; 2020. Available from: https://apps.who.int/iris/handle/10665/331490.
4. Taylor MR, Agho KE, Stevens GJ, et al. Factors influencing psychological distress during a disease epidemic: data from Australia’s first outbreak of equine influenza. BMC Public Health. 2008;8(1):347. doi:10.1186/1471-2458-8-347
5. Tucci V, Moukaddam N, Meadows J, et al. The forgotten plague: psychiatric manifestations of Ebola, Zika, and emerging infectious diseases. J Glob Infect Dis. 2017;9(4):151–156. doi:10.4103/jgid.jgid_66_17
6. Soares RS, Mellen P, Garrigan H, et al. Outcomes of eyes lost to follow-up with neovascular age-related macular degeneration receiving intravitreal anti-vascular endothelial growth factor. Ophthalmol Retina. 2020;4(2):134–140. doi:10.1016/j.oret.2019.07.010
7. Zhou F, Yu T, Du R, et al. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet. 2020;395(10229):1054–1062. doi:10.1016/S0140-6736(20)30566-3
8. Hu VH, Watts E, Burton M, et al. Protecting yourself and your patients from COVID-19 in eye care. Community Eye Health. 2020;33(108):S1–S6.
9. Borrelli E, Grosso D, Vella G, et al. Impact of COVID-19 on outpatient visits and intravitreal treatments in a referral retina unit: let’s be ready for a plausible “rebound effect”. Graefes Arch Clin Exp Ophthalmol. 2020;258(12):2655–2660. doi:10.1007/s00417-020-04858-7
10. Ahorsu DK, Lin CY, Imani V, Saffari M, Griffiths MD, Pakpour AH. The fear of COVID-19 scale: development and initial validation. Int J Ment Health Addict. 2020;27:1–9.
11. Hinkle DE, Wiersma W, Jurs SG. Applied Statistics for the Behavioral Sciences.
12. Reznik A, Gritsenko V, Konstantinov V, et al. COVID-19 fear in eastern Europe: validation of the fear of COVID-19 scale. Int J Ment Health Addict. 2020;1–6.
13. Soraci P, Ferrari A, Abbiati FA. et al. Validation and psychometric evaluation of the Italian version of the fear of COVID-19 scale. Int J Ment Health Addict;2020. 1–10. doi:10.1007/s11469-020-00277-1
14. Evren C, Evren B, Dalbudak E, et al. Measuring anxiety related to COVID-19: a Turkish validation study of the coronavirus anxiety scale. Death Stud. 2020:1–7. doi:10.1080/07481187.2020.1774969
15. Caycho-Rodríguez T, Vilca LW, Cervigni M, et al. Fear of COVID-19 scale: validity, reliability and factorial invariance in Argentina’s general population. Death Stud. 2020;29:1–10. doi:10.1080/07481187.2020.1836071
16. Université Laval. Quebec: Quebec and the world; 2020. Available from: https://ulaval.maps.arcgis.com/apps/opsdashboard/index.html#/05990238bd6a4734b2d544e3143e57a7.
17. Bodas M, Siman-Tov M, Peleg K, et al. Anxiety-Inducing media: the effect of constant news broadcasting on the well-being of Israeli television viewers. Psychiatry. 2015;78:265–276. doi:10.1080/00332747.2015.1069658
18. de Hoog N, Verboon P. Is the news making us unhappy? The influence of daily news exposure on emotional states. Br J Psychol. 2020;111:157–173. doi:10.1111/bjop.12389
19. Fung THM, Kuet ML, Patel MK, Puri P. Addressing COVID-19 fear to improve clinic attendance for patients with wet age related macular degeneration. Acta Ophthalmol. 2020. doi:10.1111/aos.14520
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.


