Back to Journals » Journal of Multidisciplinary Healthcare » Volume 13
Exploring Health Professionals’ Perceptions on Health-ID, an Electronic Integrated Patient Progress Documentation System: A Qualitative Study in Indonesia
Authors Kamil H , Rachmah R , Irvanizam I , Wardani E
Received 9 July 2020
Accepted for publication 28 October 2020
Published 19 November 2020 Volume 2020:13 Pages 1649—1656
DOI https://doi.org/10.2147/JMDH.S270740
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Hajjul Kamil,1 Rachmah Rachmah,1 Irvanizam Irvanizam,2 Elly Wardani1
1Nursing Leadership and Management Department, Faculty of Nursing, Universitas Syiah Kuala, Banda Aceh 23111, Indonesia; 2Department of Informatics, Faculty of Mathematic and Nature Sciences, Universitas Syiah Kuala, Banda Aceh 23111, Indonesia
Correspondence: Hajjul Kamil Email [email protected]
Background: Continuum of care relies on seamless communication across health professionals. Paper-based integrated patient care documentation is, therefore, obligated in hospitals in Indonesia to standardize information among health providers. However, there are several pitfalls with paper-based documentation. Reported issues regarding time, workload, incomplete patient charts, and delayed verification were seen as obstacles in the implementation of integrated patient progress notes. In an effort to tackle the issues, Health-ID (Health-Integrated Documentation) software was developed to resolve and organize health documentation to break communication boundaries between health professionals.
Aim: This study was part of a system evaluation of the software program after its implementation in a hospital in Indonesia. The aim was to explore health professionals’ perceptions of Health-ID.
Methods: A qualitative study involving in-depth face-to-face interviews with five key informants and two focus group discussions was conducted. Thematic analysis was used to analyze the data.
Results: Thematic analyses of the interviews and focus group discussion revealed several main themes for each of the two topics that were explored in the discussions and interviews: (1) Perceptions on the use of Health-ID: innovative intervention; useful tool. (2) Perceived barriers to the implementation of the Health-ID: workload; organizational support; millennial gaps.
Conclusion: The study revealed the potential of the Health-ID to generate effective communication and collaboration among health professions. Reported benefits were as follows: integrating technology in patient progress documentation has been shown to ease the work of health professionals, providing fast and reliable information on patient care updates.
Keywords: Health-ID, Indonesia, patient documentation, patient safety, qualitative
Introduction
Patient documentation is a major indicator to assess, monitor, and evaluate effective care delivery.1 It is a set of complex communications containing important day-to-day details about patients’ health, including medical and social history, current status, test results, diagnosis, treatment, and discharge plans.2 Earlier studies have revealed that meticulous patient documentation was associated with the quality of care.3–6 Information exchange between health care professionals can do harm if it is not conducted properly. Failures to address accurate communication affect the quality of patient care, potentially leading to patient safety incidents in the hospital.7
Cognizant that safety is a no compromise priority for patients, the Ministry of Health of Indonesia regulated the implementation of integrated patient progress documentation in 2012. This was intended to harmonize communication across health providers. Prior the integration attempt, each professional worked on their own notes without reference to other providers’ thoughts. This paper-based integrated documentation was expected to be among the initiatives to get rid of fragmented care practices by offering accurate and seamless patient progress reports. Unfortunately, there were continuous reported shortfalls with its implementation. Hospital staff stated that the responsibilities they have for patients made them less likely to have time to do proper documentation.8 In addition, inadequate competencies, lack of supervision, inaccuracy of timely documentation, and inconclusive yet irrelevant notes between health providers were among the issues found during the implementation of the integrated patient progress documentation sheets.8–10
The issues presented here with the use of paper-based patient documentation are prevalent in the literature. With paper-based documentation, standards and requirements for high-quality documentation and communication among health professionals are lacking. Paper-based documentation is time-consuming, repetitive, and inaccurate.11 A great deal of patient data can accumulate in a hospital in a 24-hour period.
Such accumulation of complex data makes managing information difficult, ultimately affecting the delivery of best care to patients. Retrieving information manually is considered labor-intensive. Therefore, the integration of technology to manage health documentation is more efficient.12,13 Computerized patient documentation systems are reported to be a necessary component to increase the quality of patient care.
The application of technology in managing health documentation has raised considerable interest globally, with the potential for use with regard to patient safety and communication between health care professionals.14 However, its application is reported to be low in developing countries.15,16 In the context of Indonesia, electronic documentation is still insufficiently implemented. Most documentation is still paper based, leading to more costs for paper and printing and more time needed to access old data.17
Cognizant of the problem, a group of nurse researchers collaborated with an information technology (IT) professional to develop technology-based integrated health care documentation in 2017, which was later copyrighted as Health-ID V.02 (Health-Integrated Documentation Version 0.2). Health-ID includes timely patient progress documentation used by health care professionals or Profesional Pemberi Asuhan (PPA) in Indonesia. The workflow within the Health-ID information system is shown in Figure 1.
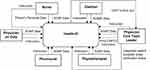 |
Figure 1 Health-ID workflow. |
The users include doctors on duty, nurses, a dietitian, a pharmacist, a physiotherapist, and a care team leader known as Dokter Penanggung Jawab Pelayanan (DPJP). Each user has distinct roles. Patient data entry is conducted separately by each profession. The nurses interact with the system by entering SOAP data (subjective, objective, analysis, planning) and instructions. Dietitians apply a similar process but noted in the form of ADIME (assessment, diagnosis, intervention, and monitoring/evaluation) data. The doctor on duty, pharmacist, and physiotherapist enter SOAP data as well as instructions into the system. These are then compiled in the same datasheets. The care team leader does the final check of the data and validates them, before printing the order. Health-ID enables the health professionals to have quick updates on patient progress by giving them electronic access to read and complete integrated documentation sheets. All data can be entered at the correct time and without further delay.
We developed the Health-ID in 2017. At the initial stage, manual or paper-based integrated documentation sheets within the medical records were carefully analyzed to identify problems within the patient progress documentation. The findings confirmed that the documentation was far from seamless and did not provide a conclusive picture of patient progress. In addition, mistakes such as incorrect procedure, missing names and signatures of the care provider, and delayed time of verification were also prevalent in the patient progress documentation sheets that were evaluated.8,10
Possible solutions using technology were agreed upon among the health professionals to tackle such problems.8 Before the software system design stage, several focus group discussions (FGDs) and interviews took place with various health professionals. We developed the system using a bottom-up approach, in preference to a top-down approach, to ensure that the software met the needs of the end users, the health professionals themselves. During the development of the program, we conducted approximately three rounds of FGDs and interviews with group of nurses, doctors, a pharmacist, dietitian, and physical rehabilitation team. The Health-ID software was tested in a hospital in 2019. At the beginning of the intervention, modifications and system adjustments were ongoing to ease its application. The aim of this research was to answer the following question: How do the health professionals perceive the Health-ID as electronic patient progress documentation?
Methods
Design
This is a qualitative study. This research was conducted using FGDs and in-depth interviews. Ethics approval for the study was obtained from the Faculty of Nursing Research ethics committee, Universitas Syiah Kuala and permission from the hospital where the study took place. Potential participants were provided with information sheets outlining the study’s objectives and procedures. Participant informed consent included publication of anonymized responses.
Participants
The Health-ID was implemented in a medical surgical ward at one hospital. Purposeful selection of participants was pursued for the study. Two FGDs with nurses (n = 16) and five face-to-face interviews with specialist doctors (n = 3), a dietitian (n = 1), and a pharmacist (n = 1) were performed to obtain data on their perceptions of the Health-ID system.
Data Collection
The FGDs took place in separate groups and the interviews took place with key informants. The FGDs and interviews lasted for 45 to 65 minutes. Sixteen nurses were involved in the nurses group and individual interviews were conducted at a time and place convenient for the participants. All interviews were recorded with prior consent from the participants. The FGDs and interviews with key participants were led by the first author as the principal investigator of the research. The FGDs with the nurses took place in two teams, A and B. The second and fourth authors assisted with the interview process, and the third author, the IT professional, also took part to assist with IT questions and requests for future system modifications. All of the research team were available to conduct the face-to-face interviews, also after prior consent. At the FGDs and personal interviews, the participants were arranged in a circle to create a non-threatening environment for the participants. The researchers had adequate experience in conducting qualitative studies. During the interview and FGDs, participation and open dialog were encouraged. The researchers reassured the interviewees and group discussion responses were clarified in a timely fashion.
Data Analysis
Data analysis was performed using thematic analysis.18 All interviews and FGDs were transcribed verbatim by two independent transcribers. The initial transcriptions were read and re-read to ascertain potential emerging themes. A code was applied to every line and sentence. Similar codes were classified into sub-themes and themes. This cycle was applied to the rest of the interview and FGD transcripts. The data from each interview were compared and contrasted with data from the other interview transcripts to ensure that all important pieces of information were gathered. The authors then had a meeting to consolidate the findings. When consensus was reached on the sub-themes and themes, two language experts at the host institution translated the results into English. These experts assisted to ensure that findings had the best semantic and meaning equivalent between Bahasa Indonesia and English.
Efforts to enhance the trustworthiness study were in place. We managed to discuss the emerging findings with another colleague who has extensive experience in conducting qualitative studies. This peer debriefing was done in an attempt to increase the credibility of the research.19
Results
Two FGD sessions were conducted with 16 nurses in total. Most of the participants were female staff nurses (n = 14) and most had an associate’s degree in nursing (n = 12). The nurses had been working in the hospital for 2 to 5 years. The interviewees included three specialist doctors, a pharmacist, and a dietitian who had been working in the hospital for more than 3 years. There was a general consensus that the Health-ID system introduced benefits in terms of communication among health professionals. However, some confirmed that the system fell short of their expectations. The participants’ understanding of the role of the Health-ID to digitally manage patient progress documentation was wide ranging.
The thematic analysis of the interviews and FGDs revealed several main themes for each of the two topics that were explored. However, the themes were not distinct because some of the statements applied to more than one theme. For topic 1, the main theme was perceptions of the use of Health-ID, with sub-themes innovative intervention and useful tool. For topic 2, the main theme was perceived barriers to the implementation of the Health-ID, with sub-themes workload, organizational support, and millennial gaps.
Perceptions on the Use of Health-ID
Innovative Intervention
There was consensus among the health professionals that the Health-ID was something new for them. They expressed their appreciation and happiness about the introduction of the system. A nurse said:
… wow, this is great. I am glad we have it, so, hopefully this will help us to work better not the other way around [smile and laughs] … (Nurse 4; Group A)
Appreciation for the invention was similarly expressed by the interviewees. As a doctor mentioned,
… I am glad the team came up with these brilliant ideas … yes, we should deal with technology. To my knowledge, other people are already away ahead of us. Of course, this should be well acknowledged, well done … (Doctor 2)
Useful Tool
In several discussions and multiple interviews, the participants agreed that the Health-ID system, to some extent, would be advantageous. A pharmacist said:
… I think the system flow is easy to follow. I would say that this will make a difference in the way we work and communicate with each other. (Pharmacist)
Excitement was clearly expressed by all participants when the researchers demonstrated the software. These health professionals showed optimism that the software would assist their daily patient documentation. This was well perceived as
… I feel it is convenient and friendly. This is much better than old ways of documentation. For me, I used to always make manual calculations. I might it get wrong [laughs], but this system facilitates me … (Dietitian)
Paper-based documentation was perceived as old fashioned. Missed communication and threats to safety were likely to be reduced or avoided with the IT intervention.
I do think it is quite advantageous for us. We have fast access to what other professionals say about the patient, so then quicker action for the patient … there is no need to wait for long as we do with paper notes … (Doctor 2)
Perceived Barriers to the Implementation of the Health-ID
Workload
Despite the agreement and positive reactions toward the Health-ID, several downsides were strongly voiced by participants. Health-ID was seen as an additional task and an interruption of their routines. This was strongly stated in the nurses group and in the personal interview with the doctors. One doctor said,
It is so hard, to be honest, dealing with the Health-ID. We have so many patients with so little time … Of course, I would be happy to fill it in with the help of assistant, but we don’t have one … (Doctor 1)
Resistance to the Health-ID due to workload was felt the most. On the one side, the doctor’s round needs to be conducted in a timely fashion, but it is rather more about getting to all patients than filling in the documentation. Paper-based notes are sufficient to document patient progress considering the extent of their duties.
Similar feelings were stated among the nurses. Health-ID was well acknowledged but used with caution. The main concern was the need for mandatory double documentation, both paper and electronic, which added to the daily work.
… It was so hard, though, we need to do the documentation twice: paper notes and the computer system … that was the hardest part. We have so many things to do for patients, not only documenting stuff, right … [smile] … (Nurse 4, Group B)
Organizational Support
The relationship between documentation and quality of care was well understood by the participants. However, the implementation of Health-ID implementation required more attention from the top leaders. As a nurse mentioned,
… For sure we, as the nurses, do most parts. Patients and documentation drain our energy. Under such condition, leaders need to be more supportive toward us, not just ask us to do stuff … ” (Nurse 7, Group A)
Lack of support provided since the trial launch of the Health-ID may have introduced the likelihood of motivational deficit among the health professionals. Nurses, as the largest user group, expressed their difficulty with the new system because appropriate support was not in place. Another nurse said,
… the system is okay, we agree. But, technical support needs to be here around the clock. The management should monitor regularly … sometimes we have problems with the system, and we don’t know what to do … (Nurse 2, Group A)
Unmet expectations about support and supervision in the organization were obstacles to applying the Health-ID as electronic documentation in the hospital. A doctor mentioned that
… the implementation would have been better if support systems were available to us, the users … local regulations need to be emphasized for the application of the Health-ID. It is hard work for both that hospital and us, the workers. (Doctor 3)
Millennial Gaps
Integrating technology in documenting patient progress was well received by all the participants involved in group discussions and interviews. On the other hand, concerns were raised by some potential users, particularly the older generation for whom digital application at work is not favored. This was strongly indicated by the nurses group. One nurse expressed:
… some of us are relatively old and not tech savvy at all [smile and laughs]. I think we are comfortable with paper documentation … Kind of hard to mingle with technology at work. I meant, it is just so hard to deal with Health-ID … like me, I made frequent mistakes when using it [laughs] … ” (Nurse 6; Group B)
Preference for paper-based patient progress notes was a result of some nurses feeling that dealing with the Health-ID was hard. The nurses admitted that they had limited digital literacy compared with the younger ones. A younger nurse explained,
… for us it is no big deal, but, I think the middle-age or older nurses find it difficult to cope and take the use of technology to another level, like the Health-ID. I respect them. I have helped them many times [smile] … probably more continuous training is needed … (Nurse 5; Group A)
Disruption to habitual actions from paper to Health-ID may have led to this negative perspective from some nurses. Some felt it was hard to move on from the paper routine because technology was initially perceived as an entertainment medium rather than a mode for effective work. Another middle-aged nurse said,
I like technology, but it is hard to imagine we will use it in our daily routine for work purposes [laughs] … maybe, we can get used to entertaining ourselves with those gadgets … (Nurse 1; Group B)
Discussion
Documentation is a reflection of the quality of care. It plays an important role in evaluating care delivery and bridging effective communication and cooperation between health care providers.20 Cognizant of the need for accurate and reliable patient progress documentation for quality assurance, electronic-based documentation has been introduced to deal with reported shortcomings with the use of traditional paper notes.
The Health-ID documentation technology software was created to facilitate integrated communication of patient progress information among health care providers. A bottom-up technology design was used to meet the best needs of the users. To the best of our knowledge, a very limited systems were available in Indonesia.
There was positive acceptance of the Health-ID from the participants in this study. The ease of use and efficiency of the system was acknowledged. The results were consistent with previous research suggesting that electronic documentation improves the performance of the hospital and health care professionals.12,21 This is not surprising, considering that studies have demonstrated that electronic documentation has a better structure than paper-based documentation.22,23 Misinterpretation of clinical notation and orders in manual systems are among the many potential sources of error that threaten patient safety.24,25 Accuracy in relation to clear writing, terminologies or abbreviations used, and recorded information is less likely to be achieved with a paper documentation system. Therefore, the Health-ID is expected to overcome the poor structure of manual notes due to the possibility of missing information.
Despite the positive views of the Health-ID, several barriers to its implementation were evident in this study. Health professionals involved in the study experienced frustration when dealing with the hybrid documentation whereby manual and digital notes were being made at the same time. This workload issue was prevalent and expressed frequently by the health professionals. The process of adjusting to the new system introduced another layer of tasks that could lead to cognitive exhaustion.26 Resistance to the transition and changes required in some processes must be dealt with in an institution.27,28 A change management strategy to mediate the transition must underpin the introduction of electronic documentation to minimize unintended consequences and to optimize improvements in safety and quality of care.29,30
Effective program implementation is linked to organizational factors. The lack of supervision and monitoring from administrators or the quality assurance department were obvious challenges in the application of the Health-ID. This was consistent with a previous study mentioning that barriers to facility and management support may impede the successful enactment of electronic documentation.31,32 Minimum leadership can mean that potential motivational aspects in embracing changes are overlooked.33 Leadership and the roles of the leaders in closely evaluating and monitoring staff attitudes and adaptation throughout the implementation of a system are pertinent during the transition trajectory.34,35
In addition to the stated obstacles to the use of the Health-ID, it was interesting that the generational factor had a significant impact when dealing with technology. In this study, the younger health professionals were eager to learn about new gadgets, whereas the older ones found it difficult to adjust to technology at work. This phenomenon is evident in the literature. The differences between millennials and previous generations are becoming more prevalent within the workplace36 with communication and technology as the biggest barriers to success. The millennials have the ability to utilize many tech-based devices simultaneously and therefore a strong technological culture has been established that influences the way they approach education and knowledge.37 Educational intervention and continuous training may facilitate positive attitudes to changes.38,39 This was emphasized in this study; more continuous training on this electronic documentation should be incorporated to mediate the generation gap.
Finally, this study has two limitations. First, the Health-ID was applied in one hospital. It would be interesting to investigate how staff in other hospitals assess the system. Second, the use of a convenience sample may not represent all the health professionals in the hospital. A future study would be enhanced by incorporating a rigorous mixed methodology and investigating it further using an adaptation theory model.
Conclusion
The current study explored health professionals’ perspectives on the Health-ID. Positive acknowledgment as well as challenges with the implementation of the system were found. Overall, the Health-ID was designed to ease health professionals into integrated documentation and was expected to increase the quality of multidisciplinary communication. Further intervention to improve the skills and attitude toward tech-based integrated documentation is required to pursue a smoother transition to the new system. Close supervision and unconditional support from hospital management are required to ensure future success with the implementation of Health-ID.
Acknowledgments
Our thanks to all health professionals involved for their time and knowledge in this study.
Funding
The research was funded by the Penelitian Unggulan Universitas (University Excellent Research) funding scheme (grant number, 276/UN11.2/PP/PNBP/SP3/2019), Universitas Syiah Kuala, Indonesia.
Disclosure
Hajjul Kamil reports a patent, CO1201704997, issued. Rachmah Rachmah reports a patent, Health-ID CO1201704997, issued. Elly Wardani reports a patent, Health-ID software, issued. The authors report no other potential conflicts of interest for this work.
References
1. Noureldin M, Mosollom R, Hassan SZ. Quality of documentation of electronic medical information systems at primary health care units in Alexandria, Egypt. East Mediterr Health J. 2014;20:105–111. doi:10.26719/2014.20.2.105
2. Scruth EA. Quality nursing documentation in the medical record. Clin Nurse Spec. 2014;28(6):312–314. doi:10.1097/NUR.0000000000000085
3. Harl FNR, Saucke MC, Greenberg CC, Ingraham AM. Assessing written communication during interhospital transfers of emergency general surgery patients. J Surg Res. 2017;214:86–92. doi:10.1016/j.jss.2017.02.069
4. Braaf S, Manias E, Riley R. The role of documents and documentation in communication failure across the perioperative pathway. A literature review. Int J Nurs Stud. 2011;48(8):1024–1038. doi:10.1016/j.ijnurstu.2011.05.009
5. Braaf S, Riley R, Manias E. Failures in communication through documents and documentation across the perioperative pathway. J Clin Nurs. 2015;24(13–14):1874–1884. doi:10.1111/jocn.12809
6. Jefferies D, Johnson M, Nicholls D, Lad S. A ward-based writing coach program to improve the quality of nursing documentation. Nurse Educ Today. 2012;32(6):647–651. doi:10.1016/j.nedt.2011.08.017
7. Coiera E. Communication systems in healthcare. Clin Biochem Rev. 2006;27(2):89–98.
8. Kamil H, Rachmah R, Wardani E, Björvell C. How to optimize integrated patient progress notes: a multidisciplinary focus group study in Indonesia. J Multidiscip Healthc. 2020;13:1. doi:10.2147/JMDH.S229907
9. Lasmani P, Haryanti F, Lazuardi L. Evaluasi implementasi rekam medis terintegrasi di instalasi rawat inap RSUP dr. Sardjito Yogyakarta [Evaluation of the implementation of integrated medical records for inpatients of RSUP dr. Sardjito Yogyakarta]. Jurnal Manajemen Pelayanan Kesehatan. 2014;17(1):3–8.
10. Kamil H, Rachmah R, Wardani E. What is the problem with nursing documentation? Perspective of Indonesian nurses. Int J Africa Nurs Sci. 2018;9:111–114. doi:10.1016/j.ijans.2018.09.002
11. Yu P, Zhang Y, Gong Y, Zhang J. Unintended adverse consequences of introducing electronic health records in residential aged care homes. Int J Med Inform. 2013;82(9):772–788. doi:10.1016/j.ijmedinf.2013.05.008
12. Nguyen L, Bellucci E, Nguyen LT. Electronic health records implementation: an evaluation of information system impact and contingency factors. Int J Med Inform. 2014;83(11):779–796. doi:10.1016/j.ijmedinf.2014.06.011
13. Ben-Assuli O. Electronic health records, adoption, quality of care, legal and privacy issues and their implementation in emergency departments. Health Policy (New York). 2015;119(3):287–297. doi:10.1016/j.healthpol.2014.11.014
14. Middleton B, Bloomrosen M, Dente MA, et al. Enhancing patient safety and quality of care by improving the usability of electronic health record systems: recommendations from AMIA. J Am Med Inform Assoc. 2013;20(e1):e2–e8. doi:10.1136/amiajnl-2012-001458
15. Hemmat M, Ayatollahi H, Maleki M, Saghafi F. Key health information technologies and related issues for Iran: a qualitative study. Open Med Inform J. 2018;12:1–10. doi:10.2174/1874431101812010001
16. Khan SZ, Shahid Z, Hedstrom K, Andersson A. Hopes and fears in implementation of electronic health records in Bangladesh. Electron J Inform Syst Dev Countries. 2012;54(1):1–18. doi:10.1002/j.1681-4835.2012.tb00387.x
17. Hariyati RTS, Yani A, Eryando T, Hasibuan Z, Milanti A. The effectiveness and efficiency of nursing care documentation using the SIMPRO model. Int J Nurs Knowl. 2016;27(3):136–142. doi:10.1111/2047-3095.12086
18. Braun V, Clarke V. Using thematic analysis in psychology. Qual Res Psychol. 2006;3:77–101. doi:10.1191/1478088706qp063oa
19. Lincoln Y, Guba EG. Naturalistic Inquiry. Newbury Park, CA: Sage; 2007.
20. Coffey C, Wurster LA, Groner J, et al. A comparison of paper documentation to electronic documentation for trauma resuscitations at a level I pediatric trauma center. J Emerg Nurs. 2015;41(1):52–56. doi:10.1016/j.jen.2014.04.010
21. Boonstra A, Versluis A, Vos JFJ. Implementing electronic health records in hospitals: a systematic literature review. BMC Health Serv Res. 2014;14(1):370. doi:10.1186/1472-6963-14-370
22. Akhu‐Zaheya L, Al‐Maaitah R, Bany Hani S. Quality of nursing documentation: paper‐based health records versus electronic‐based health records. J Clin Nurs. 2018;27(3–4):e578–e589. doi:10.1111/jocn.14097
23. Karp EL, Freeman R, Simpson KN, Simpson AN. Changes in efficiency and quality of nursing electronic health record documentation after implementation of an admission patient history essential data set. Comput Inform Nurs. 2019;37(5):260–265. doi:10.1097/CIN.0000000000000516
24. Pobocik T. Using an educational electronic documentation system to help nursing students accurately identify patient data. Int J Nurs Knowl. 2015;26(1):26–34. doi:10.1111/2047-3095.12032
25. Bruylands M, Paans W, Hediger H, Müller‐Staub M. Effects on the quality of the nursing care process through an educational program and the use of electronic nursing documentation. Int J Nurs Knowl. 2013;24(3):163–170.
26. Colligan L, Potts HWW, Finn CT, Sinkin RA. Cognitive workload changes for nurses transitioning from a legacy system with paper documentation to a commercial electronic health record. Int J Med Inform. 2015;84(7):469–476. doi:10.1016/j.ijmedinf.2015.03.003
27. Meehan R. Electronic health records in long-term care: staff perspectives. J Appl Gerontol. 2017;36(10):1175–1196. doi:10.1177/0733464815608493
28. Rantz MJ, Alexander G, Galambos C, et al. The use of bedside electronic medical record to improve quality of care in nursing facilities: a qualitative analysis. Comput Inform Nurs. 2011;29(3):149–156.
29. Kaminski J. Theory applied to informatics-Lewin’s change theory. Can J Nurs Inform. 2011;6(1).
30. Abbott AA, Fuji KT, Galt KA. A qualitative case study exploring nurse engagement with electronic health records and e-prescribing. West J Nurs Res. 2015;37(7):935–951. doi:10.1177/0193945914567359
31. Meißner A, Schnepp W. Staff experiences within the implementation of computer-based nursing records in residential aged care facilities: a systematic review and synthesis of qualitative research. BMC Med Inform Decis Mak. 2014;14(1):54. doi:10.1186/1472-6947-14-54
32. Alexander GL, Rantz M, Galambos C, et al. Preparing nursing homes for the future of health information exchange. Appl Clin Inform. 2015;6(2):248–266. doi:10.4338/ACI-2014-12-RA-0113
33. Gagnon M-P, Desmartis M, Labrecque M, et al. Systematic review of factors influencing the adoption of information and communication technologies by healthcare professionals. J Med Syst. 2012;36(1):241–277.
34. Williams F, Boren S. The role of the electronic medical record (EMR) in care delivery development in developing countries: a systematic review. Inform Prim Care. 2008;16(2):139–145.
35. Mutale W, Chintu N, Amoroso C, et al. Improving health information systems for decision making across five sub-Saharan African countries: implementation strategies from the African Health Initiative. BMC Health Serv Res. 2013;13(S2):S9. doi:10.1186/1472-6963-13-S2-S9
36. Gibson SE. Intergenerational communication in the classroom: recommendations for successful teacher-student relationships. Nurs Educ Perspect. 2009;30(1):37–39.
37. Gibson LA, Sodeman WA. Millennials and technology: addressing the communication gap in education and practice. Organ Dev J. 2014;32(4):63–75.
38. Sadoughi F, Kimiafar K, Ahmadi M, Shakeri MT. Determining of factors influencing the success and failure of hospital information system and their evaluation methods: a systematic review. Iran Red Crescent Med J. 2013;15(12):e11716.
39. Wakefield DS, Halbesleben JRB, Ward MM, Qiu Q, Brokel J, Crandall D. Development of a measure of clinical information systems expectations and experiences. Med Care. 2007;45(9):884–890. doi:10.1097/MLR.0b013e3180653625
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
