Back to Journals » Clinical Ophthalmology » Volume 16
Expert Panel Consensus for Addressing Anti-VEGF Treatment Challenges of Diabetic Macular Edema in Spain
Authors Fernández-Vigo JI, Contreras I, Crespo MJ, Beckford C, Flores-Moreno I, Cobo-Soriano R, Pareja J, Martín MD, Moreno L, Arrevola-Velasco L
Received 15 May 2022
Accepted for publication 3 August 2022
Published 19 September 2022 Volume 2022:16 Pages 3097—3106
DOI https://doi.org/10.2147/OPTH.S374763
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Scott Fraser
José Ignacio Fernández-Vigo,1 Inés Contreras,2 María José Crespo,3 Carlos Beckford,4 Ignacio Flores-Moreno,5 Rosario Cobo-Soriano,6 Jesús Pareja,7 María Dolores Martín,8 Luis Moreno,9 Luis Arrevola-Velasco10
1Deparment of Ophthalmology, Hospital Clínico San Carlos, Instituto de Investigación Sanitaria San Carlos (IdISSC), Madrid, Spain; 2Deparment of Ophthalmology, Hospital Universitario Ramón y Cajal, Instituto Ramón y Cajal de Investigaciones Sanitarias (IRYCIS) and Clínica Rementería, Madrid, Spain; 3Department of Ophthalmology, Hospital Universitario Infanta Leonor, Madrid, Spain; 4Department of Ophthalmology, Hospital Universitario Príncipe de Asturias, Alcalá de Henares, Madrid, Spain; 5Department of Ophthalmology, Hospital Universitario Puerta de Hierro, Madrid, Spain; 6Department of Ophthalmology, Hospital Universitario Henares, Universidad Francisco de Vitoria, Madrid, Spain; 7Department of Ophthalmology, Hospital General Universitario Gregorio Marañón, Madrid, Spain; 8Department of Ophthalmology, Hospital Infanta Cristina, Madrid, Spain; 9Department of Ophthalmology, Hospital 12 de Octubre, Madrid, Spain; 10Department of Ophthalmology, Clinica Baviera Instituto Oftalmológico Europeo, Madrid, Spain
Correspondence: Luis Arrevola-Velasco, Department of Ophthalmology, Clínica Baviera Instituto Oftalmológico Europeo, P.° de la Castellana, 20, Madrid, 28046, Spain, Tel +34 917 82 03 60, Email [email protected]
Purpose: The treatment of diabetic macular edema (DME) has evolved rapidly in the past decade, highlighting the need to address the challenges of routine clinical practice decision-making through expert consensus agreements.
Methods: After a literature review and discussion of real-world experience on DME management, a group of ten retina specialists agreed on a consensus of recommendations for the most appropriate management of DME patients using vascular endothelial growth factor inhibitors (anti-VEGF) in Spain.
Results: The panel recommended early treatment initiation in DME patients with worse baseline visual acuity (VA) to maintain or improve outcome. For patients with good VA, an observation strategy was recommended, considering the presence of diabetic retinopathy, optical coherence tomography biomarkers, and impact on patient’s quality of life. Based on the available evidence and clinical experience, the panel recommended the use of anti-VEGF intensive loading doses with the objective of achieving anatomic and visual responses as soon as possible, followed by a Treat & Extend (T&E) strategy to maintain VA improvement. Aflibercept was recommended for patients with a baseline decimal VA < 0.5, followed by a T&E strategy, including the possibility to extend frequency of injections up to 16 weeks.
Conclusion: An expert panel proposes a consensus for the management of DME in Spain. Early treatment initiation with anti-VEGF in DME patients is recommended to maintain or improve VA; aflibercept is recommended for patients with a poor baseline VA.
Keywords: diabetic macular edema, clinical practice patterns, intravitreal injections, consensus
Introduction
Diabetes mellitus (DM) is a chronic disease with a high global prevalence.1 It has been estimated that in 2021, there were 61 million people with DM in Europe. In Spain, the prevalence of DM in subjects aged 20 to 74 years was reported to be 5.1 million in 2021, which accounts for 10.3% of the total population.1 Diabetic retinopathy (DR) is one of the major complications of DM, often leading to visual loss.2 Diabetic macular edema (DME), characterized by exudative fluid accumulation in the macula, is the most common complication of DR. It is a serious healthcare issue among patients with DM considering the increase in life expectancy.2 In the European context, the prevalence of DR and DME is estimated to be 25.7% and 3.5% of DM patients, respectively.3 Additionally, 20.0% of patients with DM type 1 and 25.0% of patients with DM type 2 are expected to develop DME during their life.4 In Spain, the prevalence of DME in DM patients ranges between 1.4% and 7.9% according to observational studies performed in different regions across the country.5,6
Although the pathogenesis of DR and DME is complex, with multiple disease pathways, the overexpression of vascular endothelial growth factor (VEGF) plays a key role, making intravitreal VEGF inhibitors (anti-VEGF) a cornerstone for the management of these diseases.4,7 Different clinical practice guidelines have been developed to address the management of DME and most place anti-VEGF drugs as the standard of care.8,9 However, the management of these patients must be adapted to the conditions of clinical practice in each country or context. Consensus documents seek to describe the best management scheme in these different settings.10–12 Additionally, there is an increase in available evidence on the management of DME, on the effectiveness of the available treatment options, and protocols focusing on anti-VEGF use are constantly evolving. All these facts must also be considered in the development of these country level consensus.13,14
In this regard, establishing an expert consensus on recommendations to optimize DME management in Spain is imperative. This will support in providing better quality of care for patients and aid the rational use of the available resources for the healthcare system, in alignment with the current clinical practice landscape in Spain.
Method
An expert panel of ten Spanish retina specialists formed a Working Group which seeked to analyze the available evidence on the treatment of DME with anti-VEGF and develop a consensus recommendation focusing on the management of this retinal disease, adapted to clinical practice patterns in Spain. The members of the Working group were retina experts with extensive experience in the management of DME patients, being considered as reference in diabetic retinopathy units or specialized care at national level. Because of the method employed to reach a consensus (Focus Group), a group of 8–12 experts was the most appropriate option.
The main topics addressed by the Working Group were related to the clinical management of DME patients with antiangiogenic therapies, including: i) evidence supporting anti-VEGF therapy, ii) treatment initiation, iii) loading dose and iv) long-term treatment strategies.
The literature review collected information related to: i) DME physiopathology; ii) efficacy of anti-VEGF in DME; iii) effectiveness of anti-VEGF in DME; iv) effectiveness of anti-VEGF in DME patients and their quality of life; and v) Clinical Practice Guidelines (CPG) for DME treatment. The literature search was performed in different sources, including Spanish references, to avoid potential language bias. First, a search in PubMed for all articles published from 2010 to September 2020 was performed using the search terms: “Diabetic macular edema” AND “Physiopathology” OR “Treatment” OR “Anti-VEGF” OR “Health-related quality of life” OR “Management” OR “Outcomes”. Relevant cited references in selected articles were also reviewed. Later, a search in evidence-based secondary databases (Cochrane Database) was also conducted to identify relevant CPG. The retrieved information was summarized in a draft document that was shared for discussion among the Working Group members.
The Working Group conducted an individual evidence review (September 2020), followed by an ad hoc meeting (October 16th, 2020) to discuss a draft document.
Based on the discussions and/or comments provided during the Working Group meeting, together with complementary evidence review, a consensus document draft was developed, which had to be reviewed and agreed upon by all members of the Working Group. The final document was validated by all the experts. Herein, we present a summary of the relevant evidence on DME and the proposed management approach for anti-VEGF therapy in DME.
Ethics committee approval is not required for this type of consensus document.
Results
Summary of Relevant Evidence on the Role of VEGF in DME Physiopathology and in Antiangiogenic Therapy
The metabolic changes brought about by DM in the retina promote inflammation, vascular permeability, and angiogenesis.4,7 Hyperglycemia leads to oxidative stress and retinal tissular damage, with an activation of cytokines and consequently, inflammation. Furthermore, the levels of the signaling protein related to angiogenesis, VEGF-A, and placental growth factor (PlGF), another member of VEGF family, are increased in DME patients. VEGF-A and PlGF activate VEGF receptors (VEGFR-1 and VEGFR-2) and play a crucial role in vascular permeability, inflammation, and angiogenesis. Thus, inhibition of VEGF is one of the pathways that can lead to improvement of DME.15–17
Currently, there are three anti-VEGF drugs available for use in DME patients in Spain (bevacizumab, ranibizumab, and aflibercept).18 Brolucizumab has just been approved for this indication but is still not employed routinely in clinical practice. The first trial that compared the efficacy and safety of the different anti-VEGF drugs (protocol T), showed that all three (aflibercept, ranibizumab, and bevacizumab) presented similar efficacy in improving vision when initial visual acuity (VA) loss was mild. However, when VA loss was moderate or severe, aflibercept resulted in a higher improvement of vision compared to the other anti-VEGF drugs.19
The RESPOND20 and BOLT21 studies also reported that ranibizumab and bevacizumab led to VA improvement. The evidence provided by the VIVID and VISTA studies22–24 indicate that the use of aflibercept, the only anti-VEGF that acts by blocking both VEGF and PlGF,25 resulted in a gain of around two vision lines during the first year of treatment compared to laser treatment; continued treatment with aflibercept could maintain visual improvement for up to 5 years.26
The evidence available in the real-world setting supports the good results shown by anti-VEGF clinical trials, leading to anti-VEGF27 being considered the reference drugs for the management of DME.8,28–30
The results of Protocol T19 and the real world data provided by the “Fight Retinal Blindness” Registry of Australia,31 show that DME patients with a baseline VA <69 letters treated with aflibercept achieve a higher improvement in VA compared to those treated with ranibizumab during the first year of treatment.26 In addition, the APOLLON study,27 a prospective, observational cohort study conducted in France, showed equivalent improvements in functional and anatomic outcomes in both treatment-naïve and previously treated patients with DME, who were treated with aflibercept, as per the results provided by the VIVID trial.22 These results collected in a real-world setting were also confirmed in other countries,32 in terms of VA gains.
The evidence currently available supports the recommendation for early treatment in DME patients. Data provided by the VIVID and VISTA studies show that aflibercept used as an early and intensive DME treatment achieved VA gains that were maintained during the first 3 years, including the possibility to reduce the number of yearly injections administered.22–24 The results of the ENDURANCE study confirmed this benefit up to 5 years from treatment initiation.26
Anti-VEGF treatment also improves patients’ quality of life. Patients report a higher limitation in their daily activities with DME progression.33 According to the AQUA study34 which assessed self-perceived quality of life, the visual improvements led to an improvement of 6.1 points in the overall score 52 weeks after treatment initiation with aflibercept according to the National Eye Institute Visual Function Questionnaire (NEI VFQ-25). These improvements were higher in near-vision activities (+11.4 score).34
In addition to the benefits shown in DME, anti-VEGF therapies have also demonstrated relevant benefits in terms of improvement and regression of disease severity in DR. This was evaluated in a subgroup analysis of the VIVID, VISTA, and Protocol T studies19,22–24 for aflibercept, as well as in the long-term results of the RISE and RIDE studies for ranibizumab.35 Moreover, aflibercept also showed efficacy in eyes with non-proliferative DR (NPDR) and proliferative DR (PDR) according to the results from CLARITY,36 PANORAMA37 and RECOVERY38 studies.
Anti-VEGF Treatment Initiation for Central DME Patients
Although the early initiation with antiangiogenic therapy is key to achieve the expected outcomes in DME patients, treatment initiation should take into account different factors such as DM evolution and patient characteristics.8
In accordance with other previous consensus documents,39 the decision to initiate treatment should be based on the patient’s need, the severity of the disease (functional and anatomical criteria), and the visual impairment, as the main decision-making factors. However, it is also important to consider other relevant factors such as the patient’s cardiovascular or cerebrovascular risk.39,40 Anti-VEGF therapy has been linked to a potential risk for systemic adverse events, especially in those patients who have suffered a cardiovascular or cerebrovascular event in the six months prior to drug administration.40,41 In this regard, it is important to balance risk and benefit in these patients before anti-VEGF drug administration.
Consensus Recommendations
- The treatment initiation with anti-VEGF, irrespective of the patient and number of affected eyes, needs evaluation and consideration of the following factors:- Functional criteria: degree of visual impairment, both objective VA and subjectively reported by the patient.- Anatomical criteria: central retinal thickness/volume, together with a qualitative evaluation of the edema, including serous retinal detachment, cyst size, and number and location and edema extension, as well as other relevant biomarkers such as integrity of the ellipsoid zone (EZ), disorganization of retinal inner layers (DRIL) associated with significantly lower final VA, serous macular detachment, or hyper-reflective spots, among others.10- Cardiovascular or cerebrovascular disease history in the 6 months prior to the anti-VEGF administration.- DM metabolic control.
Consensus Recommendations
- An analysis of the balance between benefits and risks of anti-VEGF therapy is required in patients with a high cardiovascular risk. The benefit may prevail over the risk, except in case of patients who have presented a cardiovascular or cerebrovascular event in the 6 months prior to treatment initiation.
In agreement with other DME consensus,42,43 outcomes should be measured in terms of functional and anatomic benefits. There is some evidence suggesting that baseline VA could be a relevant criterion having a significant impact on treatment results. According to the data provided by the Protocol V,44 VA could remain stable for more than 2 years in eyes with central involved DME and good vision. In these patients, the choice of starting treatment is based on the clinical criteria, as suggested by Bandello et al, an Italian consensus that recommended anti-VEGF therapy initiation even if decimal VA was ≥0.8, if patients met biomicroscopic, optical coherence tomography (OCT) and retinal fluorescein angiography findings.39 In case of patients with VA lower than 0.7, anti-VEGF therapy initiation could provide visual improvement,45 and an early treatment initiation with anti-VEGF is especially relevant, as recommended by DME consensus from Italy and UK.42,43 In those patients with borderline VA (0.6–0.7) and mild NPDR, European GPC (EURETINA) suggested that subthreshold laser treatment or observation might be an alternative to anti-VEGF.8
According to the available evidence and expert consensus, aflibercept should be the treatment of choice for patients with a baseline VA <0.5.19
Consensus Recommendations (Figure 1)
- Treatment initiation with anti-VEGF in all patients showing a baseline VA <0.7: in patients with a baseline VA <0.5, the recommended option for treatment initiation would be aflibercept.
- Consider additional factors, such as DR presence and severity, for treatment initiation decision-making in patients with a baseline VA between 0.7–1:
- - Immediate anti-VEGF treatment initiation in patients with contralateral eye affectation, especially in case of very aggressive PDR and/or severe macular edema.
- - In patients with DME in their single functional eye, immediate treatment initiation is recommended in:
i presence of PDR (panretinal photocoagulation together with co-adjuvant anti-VEGF therapy)ii presence of severe NPDR.- For patients with bilateral affectation, treatment initiation may not be immediately required if there is an option to improve the edema by improving metabolic control. In general, treatment decision-making would follow the same recommendations as in the case of patients with a single functional eye.
Figure 1 Initiation of antiangiogenic treatment algorithm for DME patients according to diabetic retinopathy severity.
- It is always recommended to conduct an assessment by OCT and biomarkers46 to decide the need for early treatment initiation.
- Although patients with good baseline VA would not require a standard early treatment initiation, the following factors to assess edema location and impact on patient’s quality of life are decision-making factors to be considered:
- - In patients at a working age or with an active lifestyle (patients with high daily activity or family responsibilities), early treatment is recommended in order to avoid negative impact on quality of life.
- - Adherent patients are also potential candidates for early treatment.
- - In patients with good vision and mild NPDR, subthreshold laser or observation may be considered.
Anti-VEGF Loading Dose Management
One of the current debates on anti-VEGF treatment is about the number of injections that are required during the loading phase before considering either a treatment switch if there is a limited response or an extension of the interval between injections if there is an excellent response. An Italian DME consensus, Avitable et al,42 and a consensus from UK, Pearce et al,43 recommended a loading phase of five monthly injections of anti-VEGF treatment, following the VIVID and VISTA studies. However, other expert consensus from Italy, Bandello et al,39 and Spain, Udaondo et al,10 recommended that anti-VEGF treatment should be initiated as a monotherapy with at least three consecutive monthly injections.
After the loading phase, an assessment of anatomic and visual response is mandatory. For patients with suboptimal response, Pearce at al suggested continuation of anti-VEGF therapy with monthly injections and to consider adding an additional treatment.43 In case of non-responders, Bandello et al and Pearce et al proposed the use of intravitreal corticosteroids39,43 and Udaondo et al recommended extending the loading phase to two more monthly injections.10,43
Consensus Recommendations (Figure 2)
- Standard loading dose of at least three anti-VEGF intravitreal injections administered at four weekly intervals.
- On the monitoring visit one month after the third injection, assess treatment response and depending on the visual and anatomic outcomes, consider the use of two to three additional injections, initiation of the long-term strategy (treat and extend strategy preferred), or treatment switch to more effective drugs, including non-anti-VEGF or discontinuation.49
 |
Figure 2 Antiangiogenic loading doses and treatment algorithm for central DME patients. |
Anti-VEGF Treatment Strategy
The most recent evidence available positions the treat and extend (T&E) strategy as the preferred option for the management of DME patients with anti-VEGF drugs.50–52 Bandello et al consensus recommended a pro re nata (as needed) anti-VEGF scheme in responders,39 whereas Avitable et al consensus proposed both a fixed bi-monthly anti-VEGF regimen and a pro re nata scheme.42 In the UK, Pearce et al recommended a T&E strategy.43 The possibility of extending the period between injections in the T&E strategy leads to a lower frequency of annual administrations with similar outcomes compared to fixed therapies, with the added benefit of improvement in treatment adherence.52
Consensus Recommendations
- After the loading dose, a T&E regimen strategy is recommended, starting at 16 weeks from treatment initiation in case of patients with excellent anatomic and visual response after loading phase completion, or at 24 weeks from treatment initiation if additional monthly injections are needed after the loading phase because of partial response (Figure 2).
- T&E strategy should be maintained up to stability achievement, understood as the maintenance of the maximum extension interval in a period of at least two consecutive treatment administrations, with evidence of stable anatomical and functional results (eg, for aflibercept, maximum interval was defined as 16 weeks, according to results of the VIOLET study)53 (Figure 2).
- In patients in whom treatment can be stopped, regular monitoring visits should be continued for disease evolution assessment. Re-treatment with anti-VEGF should be considered if there is anatomic worsening or fluid presence (Figure 3).
- No differences are identified in the proposed strategy with regards to unilateral or bilateral eye affectation. If bilateral treatment is required, the main recommendation is to act based on the requirements of the eye with the worst vision.
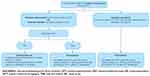 |
Figure 3 Follow-up of patients after successful treatment of DME. |
Conclusion
Our retina specialists panel considered all available evidence in anti-VEGF and DME management and their perspectives about reality of clinical practice in Spain. Although there are previous consensuses about anti-VEGF treatment in Spain (ie, Udaondo et al10), clinical practice criteria, especially the treatment strategy after the loading phase and management of non-responders, remain undefined. The present consensus provides specific treatment algorithms and decision-making criteria to be used as guidance for treatment initiation according to patient’s baseline situation, loading doses and treatment strategy for maintenance, according to the routine clinical practice of DME in Spain. The panel recommended early treatment initiation in DME patients with worse baseline VA to maintain or improve VA. In DME patients with a better VA, an observation strategy was recommended with evaluation of the presence of DR, OCT biomarkers, and patient quality of life, typically every 3–6 months or based on clinical criteria and disease evolution. Anti-VEGF loading doses recommended were intensive with the objective of achieving anatomic and visual response as fast as possible, followed by a treatment strategy of T&E with the purpose of maintaining improvement in VA for the longest time possible. Aflibercept was considered the recommended option for patients with a baseline VA <0.5, followed by a T&E strategy, including the possibility to extend injection frequency up to 16 weeks.
As a limitation of the present consensus, it must be mentioned that the discussion of anti-VEGF adverse events was limited to cardiovascular events, excluding intraocular events, which could be considered similar among anti-VEGF drugs. The current expert panel consensus is the first one to focus on DME and anti-VEGF in Spain and aims to provide practical guidance for the antiangiogenic treatment of DME patients according to the routine clinical practice at retina units in Spain.
In conclusion, early treatment initiation with anti-VEGF in DME patients is recommended to maintain or improve VA. An expectant management can be considered in selected patients with a better baseline VA whereas aflibercept is recommended as anti-VEGF treatment in those patients with worse VA. After a loading phase with anti-VEGF, a T&E strategy is recommended for DME patients.
Acknowledgments
The study has been supported by Bayer, facilitating the consensus meetings’ management and medical writing funding, supported by IQVIA.
Funding
Bayer facilitated the meetings of the panel of experts and financed the services of a medical writer provided by IQVIA. However, Bayer did not participate in the literature review or in the drafting of the consensus.
Disclosure
José Ignacio Fernández-Vigo has received honoraria for advisory boards, lectures, and travel costs from Bayer, Novartis, Roche and Allergan. Inés Contreras and Rosario Cobo have received honoraria for advisory boards, lectures, and travel costs from Bayer, Novartis, and Allergan. María José Crespo and Luis Arrevola-Velasco have received honoraria for advisory boards, lectures and travel costs from Bayer. Ignacio Flores-Moreno has received honoraria for advisory boards from Bayer and Novartis. Jesús Pareja has received honoraria for advisory boards, lectures and travel costs from Bayer and Allergan, and María Dolores Martín has received honoraria for lectures from Bayer and Pfizer. Dr Carlos Beckford reports non-financial support from Novartis, non-financial support from Allergan, non-financial support from Bayer, during the conduct of the study; non-financial support from Novartis, non-financial support from Allergan, non-financial support from Bayer, outside the submitted work. The rest of the authors received honoraria for starting the advisory board from Bayer. The authors report no other conflicts of interest in this work.
References
1. Factsheets | IDF Diabetes Atlas. Available from: https://diabetesatlas.org/regional-factsheets/.
2. Teo ZL, Tham YC, Yu M, et al. Global prevalence of diabetic retinopathy and projection of burden through 2045: systematic review and meta-analysis. Ophthalmology. 2021;128(11):1580–1591. doi:10.1016/J.OPHTHA.2021.04.027
3. Li JQ, Welchowski T, Schmid M, et al. Prevalence, incidence and future projection of diabetic eye disease in Europe: a systematic review and meta-analysis. Eur J Epidemiol. 2015;35(1):11–23. doi:10.1007/S10654-019-00560-Z
4. International Diabetes Federation. Clinical Practice Recommendations for Managing Diabetic Macular Edema.
5. Romero-Aroca P, Fernández-Alart J, Baget-Bernaldiz M, Méndez-Marín I, Salvat-Serra M. [Diabetic retinopathy epidemiology in type II diabetic patients. Effect of the changes in the diagnostic criteria and stricter control of the diabetes between 1993 and 2005 on the incidence of diabetic retinopathy]. Arch Soc Esp Oftalmol. 2007;82(4):209–218. Spanish. doi:10.4321/S0365-66912007000400005
6. Santos-Bueso E, Fernández-Pérez C, Macarro A, Fernández-Vigo J. [Prevalence of diabetic retinopathy in the city of Badajoz 2002 (Extremadura project to prevent blindness)]. Arch Soc Esp Oftalmol. 2007;82(3):153–158. Spanish. doi:10.4321/S0365-66912007000300007
7. Ndisang JF, Rastogi S, Vannacci A. Immune and inflammatory processes in obesity, insulin resistance, diabetes, and related cardiometabolic complications. J Immunol Res. 2014;2014:1–3. doi:10.1155/2014/579560
8. Schmidt-Erfurth U, Garcia-Arumi J, Bandello F, et al. Guidelines for the Management of Diabetic Macular Edema by the European Society of Retina Specialists (EURETINA). Ophthalmologica. 2017;237(4):185–222. doi:10.1159/000458539
9. Sociedad Española de Retina y Vítreo. Manejo de Las Complicaciones Oculares de La Diabetes. Retinopatía Diabética y Edema Macular. Guías de Práctica Clínica de La SERVC; 2019. Available from: www.serv.es.
10. Udaondo P, Adan A, Arias-Barquet L, et al. Challenges in diabetic macular edema management: an expert consensus report. Clin Ophthalmol. 2021;15:3183. doi:10.2147/OPTH.S320948
11. Chhablani J, Wong K, Tan GS, et al. Diabetic macular edema management in asian population: expert panel consensus guidelines. Asia Pac J Ophthalmol. 2020;9(5):426–434. doi:10.1097/APO.0000000000000312
12. Corcóstegui B, Durán S, González-Albarrán MO, et al. Update on Diagnosis and Treatment of Diabetic Retinopathy: a Consensus Guideline of the Working Group of Ocular Health (Spanish Society of Diabetes and Spanish Vitreous and Retina Society). J Ophthalmol. 2017;2017:1–10. doi:10.1155/2017/8234186
13. Bressler SB, Odia I, Maguire MG, et al. Factors Associated With Visual Acuity and Central Subfield Thickness Changes When Treating Diabetic Macular Edema With Anti–Vascular Endothelial Growth Factor Therapy: an Exploratory Analysis of the Protocol T Randomized Clinical Trial. JAMA Ophthalmol. 2019;137(4):382. doi:10.1001/JAMAOPHTHALMOL.2018.6786
14. Glassman AR, Wells JA, Josic K, et al. Five-Year Outcomes after Initial Aflibercept, Bevacizumab, or Ranibizumab Treatment for Diabetic Macular Edema (Protocol T Extension Study). Ophthalmology. 2020;127(9):1201. doi:10.1016/J.OPHTHA.2020.03.021
15. Whitcup SM, Nussenblatt RB, Lightman SL, Hollander DA. Inflammation in retinal disease. Int J Inflam. 2013;2013. doi:10.1155/2013/724648.
16. Daruich A, Matet A, Moulin A, et al. Mechanisms of macular edema: beyond the surface. Prog Retin Eye Res. 2018;63:20–68. doi:10.1016/J.PRETEYERES.2017.10.006
17. Grigsby JG, Cardona SM, Pouw CE, et al. The role of microglia in diabetic retinopathy. J Ophthalmol. 2014;2014:1–15. doi:10.1155/2014/705783
18. Virgili G, Lucenteforte E. Cochrane Database of Systematic Reviews Anti-Vascular Endothelial Growth Factor for Diabetic Macular Oedema: a Network Meta-Analysis (Review) Anti-Vascular Endothelial Growth Factor for Diabetic Macular Oedema: a Network Meta-Analysis. Anti-Vascular Endothelial Growth Factor for Diabetic Macular Oedema: a Network Meta-Analysis (Review). Ophthalmology. 2017;1:548. doi:10.1002/14651858.CD007419.pub5
19. Wells JA, Glassman AR, Ayala AR, et al. Aflibercept, Bevacizumab, or Ranibizumab for Diabetic Macular Edema: two-year Results from a Comparative Effectiveness Randomized Clinical Trial. Ophthalmology. 2016;123(6):1351. doi:10.1016/J.OPHTHA.2016.02.022
20. Berger A, Sheidow T, Cruess AF, Arbour JD, Courseau AS, de Takacsy F. Efficacy/safety of ranibizumab monotherapy or with laser versus laser monotherapy in DME. Can J Ophthalmol. 2015;50(3):209–216. doi:10.1016/J.JCJO.2014.12.014
21. Michaelides M, Kaines A, Hamilton RD, et al. A prospective randomized trial of intravitreal bevacizumab or laser therapy in the management of diabetic macular edema (BOLT study) 12-month data: report 2. Ophthalmology. 2010;117(6):1078–1086.e2. doi:10.1016/J.OPHTHA.2010.03.045
22. Korobelnik JF, Do D. Intravitreal aflibercept for diabetic macular edema. Ophthalmology. 2014;121(11):2247–2254. doi:10.1016/J.OPHTHA.2014.05.006/ATTACHMENT/5E022135-D183-4A95-9543-5DAA4E256223/MMC4.PDF
23. Brown DM, Schmidt-Erfurth U, Do D. Intravitreal aflibercept for diabetic macular edema: 100-week results from the Vista and VIVID studies. Ophthalmology. 2015;122(10):2044–2052. doi:10.1016/J.OPHTHA.2015.06.017/ATTACHMENT/40152B87-CA12-4FB3-968A-314077ED1034/MMC2.PDF
24. Heier JS, Korobelnik JF, Brown DM, et al. Intravitreal Aflibercept for Diabetic Macular Edema: 148-Week Results from the Vista and VIVID Studies. Ophthalmology. 2016;123(11):2376–2385. doi:10.1016/J.OPHTHA.2016.07.032
25. Carle M, Chu TG, Tabandeh H, Boyer DS. Intravitreal aflibercept use in the treatment of macular edema from central retinal vein occlusion. Ophthalmology. 2014;8(3):227–235. doi:10.1586/EOP.13.21
26. Wykoff CC, Ou WC, Khurana RN, Brown DM, Lloyd Clark W, Boyer DS. Long-term outcomes with as-needed aflibercept in diabetic macular oedema: 2-year outcomes of the ENDURANCE extension study. Br J Ophthalmol. 2018;102(5):631–636. doi:10.1136/BJOPHTHALMOL-2017-310941
27. Korobelnik JF, Daien V, Faure C, et al. Real-world outcomes following 12 months of intravitreal aflibercept monotherapy in patients with diabetic macular edema in France: results from the APOLLON study. Graefe’s Arch Clin Exp Ophthalmol. 2020;258(3):521–528. doi:10.1007/S00417-019-04592-9
28. Diabetic Macular Edema—Personalizing Treatment - American Academy of Ophthalmology. Available from: https://www.aao.org/eyenet/article/diabetic-macular-edema-personalizing-treatment.
29. Canadian Journal of Diabetes | diabetes Canada 2018 Clinical Practice Guidelines for the Prevention and Management of Diabetes in Canada | scienceDirect.com by Elsevier. Available from: https://www.sciencedirect.com/journal/canadian-journal-of-diabetes/vol/42/suppl/S1.
30. Cheung GCM, Yoon YH, Chen LJ, et al. Diabetic macular oedema: evidence-based treatment recommendations for Asian countries. Clin Experiment Ophthalmol. 2018;46(1):75–86. doi:10.1111/CEO.12999
31. Bhandari S, Nguyen V, Fraser-Bell S, et al. Ranibizumab or Aflibercept for Diabetic Macular Edema: comparison of 1-Year Outcomes from the Fight Retinal Blindness! Registry. Ophthalmology. 2020;127(5):608–615. doi:10.1016/J.OPHTHA.2019.11.018
32. Lukic M, Williams G, Shalchi Z, et al. Intravitreal aflibercept for diabetic macular oedema: moorfields’ real-world 12-month visual acuity and anatomical outcomes. Eur J Ophthalmol. 2020;30(3):557–562. doi:10.1177/1120672119833270
33. Rose MA, Vukicevic M, Koklanis K, Rees G, Sandhu S, Itsiopoulos C. Experiences and perceptions of patients undergoing treatment and quality of life impact of diabetic macular edema: a systematic review. Psychology, Health & Medicine. 2018;24(4):383–401. doi:10.1080/13548506.2018.1533249
34. Garweg JG, Stefanickova J, Hoyng C, et al. Vision-Related Quality of Life in Patients with Diabetic Macular Edema Treated with Intravitreal Aflibercept: the AQUA Study. Ophthalmol Retina. 2019;3(7):567–575. doi:10.1016/J.ORET.2019.03.012
35. Brown DM, Nguyen QD, Marcus DM, et al. Long-term outcomes of ranibizumab therapy for diabetic macular edema: the 36-month results from two Phase III trials: RISE and RIDE. Ophthalmology. 2013;120(10):2013–2022. doi:10.1016/J.OPHTHA.2013.02.034
36. Sivaprasad S, Prevost AT, Vasconcelos JC, et al. Clinical efficacy of intravitreal aflibercept versus panretinal photocoagulation for best corrected visual acuity in patients with proliferative diabetic retinopathy at 52 weeks (CLARITY): a multicentre, single-blinded, randomised, controlled, phase 2b, non-inferiority trial. Lancet. 2017;389(10085):2193–2203. doi:10.1016/S0140-6736(17)31193-5/ATTACHMENT/C1C5B6A0-5DA3-4F5E-BC2D-BEB009F6C58E/MMC1.PDF
37. Brown DM, Wykoff CC, Boyer D, et al. Evaluation of Intravitreal Aflibercept for the Treatment of Severe Nonproliferative Diabetic Retinopathy: results From the PANORAMA Randomized Clinical Trial. JAMA Ophthalmol. 2021;139(9):946–955. doi:10.1001/JAMAOPHTHALMOL.2021.2809
38. Wykoff CC, Nittala MG, Zhou B, et al. Intravitreal Aflibercept for Retinal Nonperfusion in Proliferative Diabetic Retinopathy: outcomes from the Randomized RECOVERY Trial. Ophthalmol Retina. 2019;3(12):1076–1086. doi:10.1016/J.ORET.2019.07.011
39. Bandello F, Midena E, Menchini U, Lanzetta P. Recommendations for the appropriate management of diabetic macular edema: light on DME survey and consensus document by an expert panel. Eur J Ophthalmol. 2016;26(3):252–261. doi:10.5301/ejo.5000736
40. Zarbin MA. Anti-VEGF Agents and the Risk of Arteriothrombotic Events. Asia-Pacific Journal of Ophthalmology (Philadelphia, Pa.). 2018;7(1):63–67. doi:10.22608/APO.2017495
41. Maloney MH, Schilz SR, Herrin J, Sangaralingham LR, Shah ND, Barkmeier AJ. Risk of Systemic Adverse Events Associated with Intravitreal Anti–VEGF Therapy for Diabetic Macular Edema in Routine Clinical Practice. Ophthalmology. 2019;126(7):1007–1015. doi:10.1016/J.OPHTHA.2018.09.040
42. Avitabile T, Azzolini C, Bandello F, et al. Aflibercept in the treatment of diabetic macular edema: a review and consensus paper. Eur J Ophthalmol. 2017;27(6):627–639. doi:10.5301/ejo.5001053
43. Pearce I, Bailey C, Fletcher E, et al. Translating evidence into practice: recommendations by a UK expert panel on the use of aflibercept in diabetic macular oedema. Eye. 2020;34(5):969–981. doi:10.1038/s41433-019-0615-8
44. Glassman AR, Baker CW, Beaulieu WT, et al. Assessment of the DRCR Retina Network Approach to Management With Initial Observation for Eyes With Center-Involved Diabetic Macular Edema and Good Visual Acuity: a Secondary Analysis of a Randomized Clinical Trial. JAMA Ophthalmol. 2020;138(4):341. doi:10.1001/JAMAOPHTHALMOL.2019.6035
45. Wykoff CC. Thresholds for Initiating Treatment of Eyes with Diabetic Macular Edema and Good Vision: consideration of DRCR.Net Protocol V Results. Ophthalmol Retina. 2019;3(11):917–919. doi:10.1016/J.ORET.2019.07.007
46. Busch C, Okada M, Zur D, et al. Baseline predictors for visual acuity loss during observation in diabetic macular oedema with good baseline visual acuity. Acta Ophthalmol. 2020;98(7):e801–e806. doi:10.1111/AOS.14390
47. Grzybowski A, Turczynowska M. Epidemiology of Endophthalmitis and Treatment Trend in Europe. Springer Singapore; 2018; doi:10.1007/978-981-10-5260-6_5
48. Burgués-Ceballos A, Barnés Ruz C, Cantal Portabella E, de Miguel Simó P, Moser Wurth C. Endoftalmitis en inyecciones intravítreas con y sin profilaxis con antibiótico tópico. Experiencia y manejo. Ann d’oftalmologia. 2020;28(1):14–21.
49. Madjedi K, Pereira A, Ballios BG, et al. Switching between anti-VEGF agents in the management of refractory diabetic macular edema: a systematic review. Surv Ophthalmol. 2022;1. doi:10.1016/J.SURVOPHTHAL.2022.04.001
50. Kim YC, Shin JP, Pak KY, et al. Two-year outcomes of the treat-and-extend regimen using aflibercept for treating diabetic macular oedema. Sci Rep. 2020;10(1). doi:10.1038/S41598-020-78954-3
51. Pak KY, Shin JP, Kim HW, et al. One-Year Results of Treatment of Diabetic Macular Edema with Aflibercept Using the Treat-and-Extend Dosing Regimen: the VIBIM Study. Ophthalmologica. 2020;243(4):255–262. doi:10.1159/000504753
52. Volkmann I, Knoll K, Wiezorrek M, Greb O, Framme C. Individualized treat-and-extend regime for optimization of real-world vision outcome and improved patients’ persistence. BMC Ophthalmol. 2020;20(1). doi:10.1186/S12886-020-01397-X
53. Efficacy and Safety of Three Different Aflibercept Regimens in Subjects With Diabetic Macular Edema (DME) - Study Results - ClinicalTrials.gov. Available from: https://clinicaltrials.gov/ct2/show/results/NCT02818998?view=results.
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
