Back to Journals » Clinical Ophthalmology » Volume 16
Examining the Relationship Between Diabetic Macular Edema, and Obstructive Sleep Apnea
Authors Kaba Q , Tai F , Al-Awadi A, Somani S
Received 15 December 2021
Accepted for publication 8 April 2022
Published 21 April 2022 Volume 2022:16 Pages 1215—1223
DOI https://doi.org/10.2147/OPTH.S354087
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Qayim Kaba,1 Felicia Tai,2 Ahmad Al-Awadi,3 Sohel Somani4– 6
1Cardiff University School of Medicine, Cardiff, UK; 2Faculty of Medicine, University of Toronto, Toronto, Ontario, Canada; 3Mayo Clinic School of Graduate Medical Education, Jacksonville, FL, USA; 4Department of Ophthalmology & Vision Sciences, University of Toronto, Toronto, Ontario, Canada; 5Uptown Eye Specialists, Brampton, Ontario, Canada; 6William Osler Health Centre, Brampton, Ontario, Canada
Correspondence: Sohel Somani, Uptown Eye Specialists, 401-7900 Hurontario Street, Brampton, ON, L6Y 0P6, Canada, Email [email protected]
Purpose: This prospective cohort study examined the relationship between diabetic macular edema (DME), diabetic retinopathy (DR) and obstructive sleep apnea (OSA) in patients after 1 year of treatment with anti-VEGF injection and/or continuous positive airway pressure (CPAP).
Patients and Methods: The study included adults with type 1 or 2 diabetes mellitus with diabetic retinopathy. Polysomnography metrics were measured at baseline. Ophthalmologic metrics were measured at baseline, six-month (6m) and twelve-month (12m) follow-up. All DME+ patients received standard care, and all OSA+ patients were advised continuous positive airway pressure (CPAP). Logistic regression between DR severity and OSA severity was performed. Analysis of variance (ANOVA) was performed between subgroups.
Results: Seventy-four eyes of 49 patients with DR were included. Prevalence of OSA was significantly higher in the DME+ group (70.7%) than DME- group (42.4%, p < 0.05). A significantly lower average minimum SaO2 was noted in OSA+DME+ (81.74%) than OSA+DME- eyes (88.23%, p < 0.05). Logistic regression analysis of ophthalmological and sleep metrics showed no correlation between DR and OSA severity. CPAP adherence was 20% (6/30) in the OSA+DME+ cohort and 36% (5/14) in the OSA+DME- cohort. At 12m, CPAP-adherent OSA+DME+ showed significantly lower DR severity score (1.00 ± 0.0) than CPAP non-adherent OSA+DME+ (1.36 ± 0.80, p = 0.042). No significant patterns were noted for visual acuity and mean central retinal thickness.
Conclusion: DME is associated with the presence of OSA. Minimum SaO2 is a significant OSA clinical variable for DME. DR severity is not associated with OSA severity. CPAP coupled with intravitreal anti-VEGF therapy may be helpful for reducing DR severity in DME+ eyes. Presence of OSA may diminish intravitreal anti-VEGF efficacy on anatomical (mean CRT) and functional (VA) outcomes of DME.
Keywords: diabetes mellitus, diabetic microvascular complications, anti-VEGF injections, continuous positive airway pressure, anti-VEGF, diabetic retinopathy
Introduction
Patients with diabetes mellitus (DM) often suffer from other comorbidities including obstructive sleep apnea (OSA),1 the prevalence of which may be up to 36%.2
OSA patients with moderate-to-severe OSA have a three-fold risk of developing microvascular diabetes-related complications including nephropathy, retinopathy, and neuropathy.3 DM patients with OSA are at a two-fold risk of developing diabetic retinopathy (DR) compared to those without.4 Underlying pathophysiological mechanisms of OSA also overlap with DR, such as oxidative stress, increased inflammation, and increased vascular endothelial growth factor (VEGF).5 Chronic damage to retinal microvasculature in DR may lead to development of diabetic macular edema (DME), a common cause of vision loss in patients with DM,6 with a 10-year cumulative incidence of 20–25%.7 Given the overlap in pathophysiologic mechanism, elucidating the clinical relationship between OSA and DME is an important next step in determining how patients with both conditions may be managed.
This study aims to further explore the association between DME and OSA diagnoses through a gold-standard polysomnography. Previous studies utilizing polysomnography were retrospective or cross-sectional studies.8–12 To our knowledge, we report the first prospective cohort study examining the relationship between DME and OSA polysomnography. Association between DR and OSA severity will also be explored by comparing functional and anatomic outcomes with a 12-month follow-up period.
Methods
Study Design
A prospective cohort study was conducted with patients diagnosed with type 1 DM (T1DM) or type 2 DM (T2DM), consecutively recruited from one ophthalmology outpatient clinic site located in Ontario, Canada, between March 2017 and November 2019. This study received Institutional Review Board approval prior to commencing (Institutional Review Board Services, Pro00018199) and adhered to the tenants of the Declaration of Helsinki. This study was registered with clinicaltrials gov (NCT03597815). Informed written consent was obtained from all study participants prior to study commencement.
Inclusion and Exclusion Criteria
T2DM patients aged 18 years or older with capacity to provide consent, with evidence of DR±DME, and willingness to comply with all treatment and follow-up procedures were included. Patients who had contraindications to intravitreal aflibercept (Eylea) injections including stroke within past 6 months, ocular or periocular infection, active intraocular inflammation, hypersensitivity to aflibercept; contraindications to continuous positive airway pressure (CPAP) including severe bullous lung disease, pneumothorax, pathologically low blood pressure, dehydration, cerebrospinal fluid leak, recent cranial surgery, or trauma; presence of any other retinal or macular disease (eg, retinal detachment, age-related macular degeneration); impaired capacity; pregnant or breastfeeding; and patients on any drug or device clinical investigation within 30 days prior to entry into the study were excluded.
For patients with two DME+ eyes, one eye was included at random using a randomizer. For patients with one DME+ eye and one DME- eye, only the DME+ eye was included to avoid confounding. For patients with two DME- eyes and unequal VA, the eye with the worse VA was included to avoid confounding. If both DME- eyes had equal VA, both eyes were included.
Outcomes
Gold-standard polysomnography testing obtained sleep metrics including apnea-hypopnea index (AHI), minimum oxygen saturation (minimum SaO2), mean SaO2, and sleep efficiency for each enrolled patient eye. OSA was defined as an AHI ≥15 (ie, moderate or severe OSA). DR severity was graded according to the International Clinical Diabetic Retinopathy Disease Severity Scale.13 Ophthalmologic metrics included mean central retinal thickness (CRT), logMAR best corrected visual acuity (BCVA), and DR severity scale. Eyes were defined to be DME positive (DME+) or DME negative (DME-) based on spectral-domain optical coherence tomography (sdOCT). DME was defined by central subfield retinal thickness >275 μm with evidence of intraretinal or subretinal fluid on sdOCT.
Throughout the twelve-month study period, all DME+ eyes received standard of care treatment with intravitreal aflibercept injections with five loading doses at monthly intervals followed by a treat-and-extend protocol.14 In addition, OSA positive (OSA+) eyes received continuous positive airway pressure (CPAP) treatment.
Statistical Analysis
Eyes were categorized into four groups based on measured parameters: OSA+DME+, OSA+DME-, OSA-DME+, or OSA-DME-. Analysis of variance (ANOVA) and two-sided t-test assuming equal variances with type I error controlled as 0.05 were used to compare polysomnography metrics and ophthalmologic metrics between the four subgroups at baseline, 6m, and 12m. Logistic regression analysis was used to assess correlations between DR severity, CRT, and logMAR BCVA with AHI, minimum and mean O2 saturation. Multivariate analysis was used to examine the association between DME and OSA.
Results
Demographics
Seventy-two patients were enrolled, with 23 patients dropping out prior to the polysomnography. Seventy-four eyes of 49 patients were enrolled after exclusion criteria were applied. 55.4% (n = 41) eyes were DME positive (DME+). 58.1% (n = 43) eyes were OSA positive (OSA+). There was a significantly greater prevalence of OSA in DME+ eyes (71%, n = 29) compared to DME- eyes (42%, n = 14; p<0.05).
Overall, 44 (59%) were male and 30 (41%) were female. Mean age of patients was 64±8.4 years, ranging from 56 to 72. Mean body-mass index (BMI) was 28.9±6 kg/m2. The ethnicity consisted mostly of Caucasian (50%, n = 37 eyes) followed by Asian (46%, n = 34 eyes). 95% (n = 70) of the study eyes were from patients with T2DM (Table 1). The duration of DM since diagnosis was 16±8 years. Follow-up cohorts at 6m and 12m comprised 69 eyes (93%) and 68 eyes (92%), respectively.
 |
Table 1 Baseline Characteristics |
Baseline Characteristics
Sleep metrics were obtained at baseline by polysomnography. Minimum SaO2 was significantly lower in DME+ (88±6%) compared to DME- eyes (82±11%, p<0.05) (Table 2). There was a trend towards higher mean AHI (32.43±11), higher number of apneas (6.37±11), and lower number of hypopneas (19.74±15) in DME+ eyes than in DME- eyes (27.39±27, p=0.22; 3.15±3, p=0.15; and 25.97±28, p=0.20, respectively). Sleep efficiency and mean SaO2 trended lower in DME+ (68.21±20 and 94.13±2, respectively) than DME- eyes (75.3±19, p=0.07; and 94.97±3, p=0.09, respectively).
 |
Table 2 Polysomnography Metrics Separated According to Presence of Diabetic Macular Edema |
Baseline ophthalmologic measures were compared between subgroups in Table 2. OSA+DME+ had significantly higher logMAR VA than other subgroups (0.67±0.57 [20/94], p<0.001) (Table 3). OSA-DME+ subgroup (0.34±0.13 [20/44]) had significantly higher logMAR than both OSA+DME- (0.19±0.14 [20/31], p<0.001) and OSA-DME- (0.22±0.16 [20/33], p=0.03) subgroups. Baseline mean CRT was significantly different between subgroups (p<0.0001) (Table 3). OSA+DME+ (433±156 µm) and OSA-DME+ (372±91 µm) groups were significantly greater than both OSA+DME- (262±27 µm) and OSA-DME- (289±109 µm) groups, although not significantly different from each other. DR severity score was not statistically significant between subgroups (p=0.29) (Table 3).
 |
Table 3 Baseline Ophthalmologic Metrics Separated According to Subgroup |
In a multivariate analysis adjusting for BMI, hypertension, age, and sex, OSA and DME were not found to be associated (p = 0.82; 95% CI: −0.024–0.393).
Severity of DR and Severity of OSA
Using logistic regression analysis, no correlation between any of the severity of diabetic retinopathy parameters (DR severity score, CRT, and logMAR BCVA) and the severity of OSA (AHI, minimum and mean SaO2) parameters were found (Table 4). DR severity and CRT were also analysed with AHI and minimum SaO2 at 6m and 12m using logistic regression analysis with no correlation between these parameters.
 |
Table 4 Regression Analysis of Ophthalmologic and Polysomnography Metrics |
CPAP Therapy Efficacy
While all OSA+ patients were offered CPAP therapy, patient adherence to this therapy was 20% (6/30) in the OSA+DME+ cohort and 36% (5/14) in the OSA+DME- cohort. As such, to delineate CPAP therapy efficacy, the following cohorts were analyzed: “CPAP adherent OSA+DME+” (n = 6) receiving anti-VEGF with treated OSA; “CPAP non-adherent OSA+DME+” (n = 24) receiving anti-VEGF with untreated OSA; and “OSA-DME+” (n = 11) receiving anti-VEGF without OSA-induced hypoxia. The presence of anti-VEGF is controlled for by separation of the analysis in DME+ and DME- patients. The total number of injections between OSA+DME+ and OSA-DME+ at 12m follow-up were identical (p = 0.63).
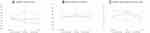
At baseline, the CPAP non-adherent OSA+DME+ cohort had significantly higher logMAR VA and mean CRT than other cohorts (Figure 1). CPAP adherent OSA+DME+ DR severity score (1.00±0.0) was significantly lower than CPAP non-adherent OSA+DME+ (1.36±0.80, p=0.042), and statistically equivalent to OSA-DME+ (1.18±0.4, p=0.166) at 12m. For logMAR VA, CPAP non-adherent OSA+DME+ (0.59±0.55) was significantly higher than OSA-DME+ (0.23±0.07, p=0.005), while CPAP adherent OSA+DME+ remained statistically similar to OSA-DME+ (0.33±0.16, p=0.192) at 12m. No significant trends were noted for changes in mean CRT at any time point, compared to baseline.
For OSA-DME+, significant improvements in logMAR VA, mean CRT, and DR severity score were seen at 6m and 12m when compared to baseline (Figure 1). However, for CPAP non-adherent OSA+DME+, significant improvements were only seen in mean CRT and DR severity score at 6m and 12m compared to baseline, while CPAP adherent OSA+DME+ only showed significant improvement with DR severity score at 6m and 12m.
CPAP therapy was analyzed in the same manner for DME- patients. The following cohorts were compared: CPAP adherent OSA+DME- (n = 5), CPAP non-adherent OSA+DME- (n = 9), and OSA-DME- (n = 19). No significant trends were noted in this analysis (Figure 2). LogMAR VA, mean CRT, and DR severity score remained equivalent across the three cohorts at all timepoints. There were also no significant improvements in logMAR VA, mean CRT, or DR severity score noted at 6m or 12m for any group.
Discussion
States of chronic hyperglycemia are known to predispose tissues to microvascular damage.15 Intermittent hypoxemia leads to vasoconstriction, increased advanced glycation end products, inflammation, and oxidative stress, resulting in further endothelial dysfunction, microvascular impairment, and VEGF production.15 In patients with DR, hypoxemic impact of OSA is magnified due to increased nocturnal retinal oxygen requirements.16 Nighttime hypoxemia was found to lead to an increase in VEGF,15 and elevated serum VEGF has been detected in hypoxic OSA patients.17
Polysomnography in this study reported a significantly higher prevalence of OSA+ patients (71%) in DME+ eyes, compared to DME- eyes. This agrees with previously reported values ranging from 31% to 76% when measured by home sleep study devices.16,18 Mason et al found a high prevalence of sleep disordered breathing when measured by a home sleep study device in patients with clinically significant DME.18 The same association was reported in patients with T1DM with OSA detected by polysomnography, indicating similar pathophysiologic mechanisms may still be at play.19 When examining the reverse association, DME was found to be similarly equal in OSA+ and OSA- eyes (p=0.20). Because DME is more likely to be found in eyes of OSA+ patients (p<0.05), and no difference in OSA status was found when looking only at DME+ eyes (p=0.20), this supports the previously proposed concept of OSA as an aggravator of DME.20
We found minimum SaO2 to be the only significant clinical variable of DME in patients with OSA, in agreement with other studies finding minimum SaO2 to be associated with DR. This suggests minimum SaO2 to be a sensitive marker for hypoxia in DR and DME.21 Hypoxia-inducible factor 1α (HIF-1α) pathways are activated under conditions of sustained hypoxia, leading to production of VEGF, while nuclear factor-κB (NF-κB) pathway is activated under conditions of intermittent hypoxia. Excess HIF-1α, Nf-κB, and VEGF are proposed to play a role in DR development and end-organ damage.22 Because minimum SaO2 is an index of hypoxia severity, including both intermittent and sustained hypoxia, DR-related DME may be associated with HIF-1α and Nf-κB pathways.21
Sleep metrics including AHI, AHI ≥15, apneas, hypopneas, mean SaO2 and sleep efficiency were found to be similar between DME+ and DME- eyes. Similar findings have been reported.8,9 Du et al conducted a cross-sectional study and did not find AHI, severity of OSA, ODI, and minimum SaO2 to be significantly associated with risk of DR, despite adjusting for thirteen confounding factors.10 No significant associations between DME and presence of OSA, AHI, total sleep duration, short sleep duration of <5 hours, and excessive daytime sleepiness have also been reported.8 Contrarily, a case-control study found mean AHI to be significantly higher in patients with DME compared to those without, indicating a greater prevalence of OSA in patients with DME in their study group.11
At baseline, logMAR BCVA and mean CRT values were significantly different among the four subgroups. With an equivalent number of aflibercept injections over 12m, DME+ groups showed significantly higher CRT and logMAR values at 12m, regardless of OSA status. This is not surprising given that logMAR BCVA and CRT are anatomical and functional outcomes of DME. Mason et al did not find sleep disordered breathing to be correlated to macular thickness,18 indicating that correlation to CRT thickness may be more prominent in patients with clinically significant sleep apnea. Overall, aside from being a marker of DME, CRT may not be an ideal independent marker for OSA severity.
To analyse CPAP efficacy, DME+ eyes without OSA (OSA-DME+), DME+ eyes with treated OSA (CPAP adherent OSA+DME+), and DME+ eyes with untreated OSA (CPAP non-adherent OSA+DME+) were compared. All patients in these three cohorts received anti-VEGF therapy in a treat-and-extend protocol. While OSA-DME+ patients showed significant improvement in logMAR VA and mean CRT at 6m and 12m, it appears that the presence of OSA may impact anti-VEGF efficacy on improving DME outcomes as both OSA+DME+ cohorts did not show significant improvement overtime. However, DR severity was significantly lower in CPAP adherent OSA+DME+ compared to CPAP non-adherent OSA+DME+ and statistically equivalent to OSA-DME+ DR severity. Interestingly, adherent CPAP therapy did not lower DR severity in OSA+DME- eyes over 6m or 12m. These patients did not receive anti-VEGF as there was no clinical indication. Altogether, these findings show that while CPAP treatment may not improve functional and anatomical outcomes of DME (VA and CRT, respectively), it may potentially reduce DR severity in DME eyes when used in conjunction with intravitreal anti-VEGF therapy.
Presence of OSA may diminish clinical efficacy of intravitreal anti-VEGF treatment of DME. Although serum VEGF levels were found to be significantly higher in DR patients with OSA,17 there are likely a significantly greater number of other inflammatory cytokines involved beyond VEGF alone, leading to more advanced pathology in OSA+ patients. This may include pro-inflammatory cytokines such as tumor necrosis factor-α (TNF-α), interleukin 8 (IL-8), intercellular adhesion molecule 1 (ICAM-1), and interleukin 6 (IL-6), which have been reported to be elevated in conditions such as OSA and DME.23–27
Mason et al have demonstrated improved VA after six-months of highly compliant CPAP usage.28 Contrarily, the Retinopathy and Concurrent Obstructive Sleep Apnea (ROSA) randomized control trial concluded that CPAP did not improve VA in patients with DR and DME.29 However, Smith et al point out that CPAP compliance is not as high in the ROSA trial compared to the study by Mason et al, and further demonstrates the efficacy of compliant CPAP usage in lowering the risk of DR and DME.30 Compliant CPAP usage in this study was defined to be at least 4 hours on 70% of nights.30
It has been demonstrated that prolonged anti-VEGF therapy in DME patients may present a theoretical risk for cardiovascular accident and mortality.31,32 Future studies investigating whether OSA may be a variable associated with cardiovascular events in DME patients treated with anti-VEGF may also be of interest.
When examining eyes with existing DR, we found patients with OSA have significantly higher DR severity scores. However, logistic regression analysis of specific OSA scores (AHI, minimum and mean SaO2) to DR severity score did not show any correlation. Contrary to our findings, Altaf et al reported a dose-dependent relationship between OSA severity and progression to advanced DR.20
The findings in this study are subject to limitations, such as enforcing CPAP adherence and treatment. Coupled with the drop-out of patients prior to completing a sleep study, the study sample size was significantly reduced. Given the low rate of CPAP utilization definitive conclusions may not be drawn from CPAP analysis. Furthermore, although our multivariate analysis showed no association between OSA and DME when adjusting for BMI, hypertension, age, and sex, this is likely largely due to the small sample size. It may instead show that variables of BMI and age are also significant determinants of OSA in our cohort. These variables are not independent of each other as older patients tended to have a longer length of DM presence, which is also associated with a greater chance of DME. Moreover, a higher BMI is a risk factor for DME.
To date, only a few studies have investigated the association between DME and OSA using gold-standard polysomnography.8–11 To our knowledge, we are the first to perform a prospective cohort study examining the relationship between DME and OSA polysomnography. In future studies, it may be of interest to further investigate the relationship between OSA and DME OCT angiography.33–35
Conclusion
In conclusion, our findings reaffirm that DME is associated with OSA, and minimum SaO2 is a significant OSA clinical variable in DME. Despite this, no correlation was found between measures of DR severity and measures of OSA severity. Whilst the presence of OSA may mitigate anti-VEGF therapy efficacy, larger controlled trials with sound CPAP adherence are needed to further elucidate the impact of OSA on DME.
Past Presentations
- Preliminary - Canadian Ophthalmology Society (COS), Quebec City, June 16th 2019
- American Society of Retina Specialists (ASRS), Paris, July 27th 2019
- Final – COS, Virtual, June 25th, 2021
Data Sharing Statement
The data that support the findings of this study are available from the corresponding author upon reasonable request.
Disclosure
The authors declare that there is no conflict of interest. The authors received no financial support for the research, authorship, and/or publication of this article.
References
1. Iglay K, Hannachi H, Joseph Howie P, et al. Prevalence and co-prevalence of comorbidities among patients with type 2 diabetes mellitus. Curr Med Res Opin. 2016;32(7):1243–1252. doi:10.1185/03007995.2016.1168291
2. Einhorn D, Stewart DA, Erman MK, et al. Prevalence of sleep apnea in a population of adults with type 2 diabetes mellitus. Endocr Pract. 2007;13(4):355–362. doi:10.4158/EP.13.4.355
3. Siwasaranond N, Nimitphong H, Manodpitipong A, et al. The relationship between diabetes-related complications and obstructive sleep apnea in type 2 diabetes. J Diabetes Res. 2018;2018:9269170. doi:10.1155/2018/9269170
4. Zhu Z, Zhang F, Liu Y, et al. Relationship of obstructive sleep apnoea with diabetic retinopathy: a meta-analysis. Biomed Res Int. 2017;2017:4737064. doi:10.1155/2017/4737064
5. Kato M, Roberts-Thomson P, Phillips BG, et al. Impairment of endothelium-dependent vasodilation of resistance vessels in patients with obstructive sleep apnea. Circulation. 2000;102(21):2607–2610. doi:10.1161/01.CIR.102.21.2607
6. Bandello F, Battaglia Parodi M, Lanzetta P, et al. Diabetic macular edema. Dev Ophthalmol. 2017;58:102–138.
7. Klein R, Klein BE, Moss SE, et al. The Wisconsin epidemiologic study of diabetic retinopathy. XV. The long-term incidence of macular edema. Ophthalmology. 1995;102(1):7–16. doi:10.1016/S0161-6420(95)31052-4
8. Chew M, Tan NYQ, Lamoureux E, et al. The associations of objectively measured sleep duration and sleep disturbances with diabetic retinopathy. Diabetes Res Clin Pract. 2020;159:107967. doi:10.1016/j.diabres.2019.107967
9. Chiang JF, Sun M-H, Chen K-J, et al. association between obstructive sleep apnea and diabetic macular edema in patients with type 2 diabetes. Am J Ophthalmol. 2021;226:217–225. PMID: 33529585. doi:10.1016/j.ajo.2021.01.022
10. Du C, He C, Dong L, et al. Associations of apnea hypopnea index and educational attainments with microvascular complications in patients with T2DM. Endocrine. 2020;67(2):363–373.
11. Vié AL, Kodjikian L, Agard E, et al. Evaluation of obstructive sleep apnea syndrome as a risk factor for diabetic macular edema in patients with Type II diabetes. Retina. 2019;39(2):274–280. doi:10.1097/IAE.0000000000001954
12. Chang AC, Fox TP, Wang S, et al. Relationship between obstructive sleep apnea and the presence and severity of diabetic retinopathy. Retina. 2018;38(11):2197–2206. doi:10.1097/IAE.0000000000001848
13. Wu L, Fernandez-Loaiza P, Sauma J, et al. Classification of diabetic retinopathy and diabetic macular edema. World J Diabetes. 2013;4(6):290–294. doi:10.4239/wjd.v4.i6.290
14. Pak KY, Shin JP, Kim HW, et al. One-year results of treatment of diabetic macular edema with aflibercept using the treat-and-extend dosing regimen: the VIBIM study. Ophthalmologica. 2020;243:255–262. doi:10.1159/000504753
15. Schulz R, Hummel C, Heinemann S, et al. Serum levels of vascular endothelial growth factor are elevated in patients with obstructive sleep apnea and severe nighttime hypoxia. Am J Respir Crit Care Med. 2002;165(1):67–70. doi:10.1164/ajrccm.165.1.2101062
16. Prudon B, Hughes J, West S. A novel postal-based approach to diagnosing obstructive sleep apnoea in a high-risk population. Sleep Med. 2017;33:1–5. doi:10.1016/j.sleep.2016.11.026
17. Kakhniashvili T, Tabagari-Bregvadze N, Dzvelaia S, et al. Serum vascular endothelial growth factor concentration decreases in correlation with glycated hemoglobin levels in patients with Type 2 diabetes. Georgian Med News. 2018;283:55–58.
18. Mason RH, West SD, Kiire CA, et al. High prevalence of sleep disordered breathing in patients with diabetic macular edema. Retina. 2012;32(9):1791–1798. doi:10.1097/IAE.0b013e318259568b
19. Manin G, Pons A, Baltzinger P, et al. Obstructive sleep apnoea in people with Type 1 diabetes: prevalence and association with micro- and macrovascular complications. Diabet Med. 2015;32(1):90–96. doi:10.1111/dme.12582
20. Altaf QA, Dodson P, Ali A, et al. Obstructive sleep apnea and retinopathy in patients with type 2 diabetes. A longitudinal study. Am J Respir Crit Care Med. 2017;196(7):892–900. doi:10.1164/rccm.201701-0175OC
21. Nishimura A, Kasai T, Tamura H, et al. Relationship between sleep disordered breathing and diabetic retinopathy: analysis of 136 patients with diabetes. Diabetes Res Clin Pract. 2015;109(2):306–311. doi:10.1016/j.diabres.2015.05.015
22. Arden GB, Sivaprasad S. The pathogenesis of early retinal changes of diabetic retinopathy. Doc Ophthalmol. 2012;124(1):15–26. doi:10.1007/s10633-011-9305-y
23. Carpagnano GE, Spanevello A, Sabato R, et al. Systemic and airway inflammation in sleep apnea and obesity: the role of ICAM-1 and IL-8. Transl Res. 2010;155(1):35–43. doi:10.1016/j.trsl.2009.09.004
24. Liu H, Liu J, Xiong S, et al. The change of interleukin-6 and tumor necrosis factor in patients with obstructive sleep apnea syndrome. J Tongji Med Univ. 2000;20(3):200–202. doi:10.1007/BF02886988
25. Rübsam A, Parikh S, Fort PE. Role of inflammation in diabetic retinopathy. Int J Mol Sci. 2018;19:4. doi:10.3390/ijms19040942
26. Adamiec-Mroczek J, Oficjalska-Młyńczak J, Misiuk-Hojło M. Proliferative diabetic retinopathy - the influence of diabetes control on the activation of the intraocular molecule system. Diabetes Res Clin Pract. 2009;84(1):46–50. doi:10.1016/j.diabres.2009.01.012
27. Bromberg-White JL, Glazer L, Downer R, et al. Identification of VEGF-independent cytokines in proliferative diabetic retinopathy vitreous. Invest Ophthalmol Vis Sci. 2013;54(10):6472–6480. doi:10.1167/iovs.13-12518
28. Mason RH, Kiire CA, Groves DC, et al. Visual improvement following continuous positive airway pressure therapy in diabetic subjects with clinically significant macular oedema and obstructive sleep apnoea: proof of principle study. Respiration. 2012;84(4):275–282. doi:10.1159/000334090
29. West SD, Prudon B, Hughes J, et al. Continuous positive airway pressure effect on visual acuity in patients with type 2 diabetes and obstructive sleep apnoea: a multicentre randomised controlled trial. Eur Respir J. 2018;52(4):1801177. doi:10.1183/13993003.01177-2018
30. Smith JP, Cyr LG, Dowd LK, et al. The veterans affairs continuous positive airway pressure use and diabetic retinopathy study. Optom Vis Sci. 2019;96(11):874–878. doi:10.1097/OPX.0000000000001446
31. Avery RL, Gordon GM. Systemic safety of prolonged monthly anti-vascular endothelial growth factor therapy for diabetic macular edema: a systematic review and meta-analysis. JAMA Ophthalmol. 2016;134(1):21–29. doi:10.1001/jamaophthalmol.2015.4070
32. Reibaldi M, Fallico M, Avitabile T, et al. Risk of death associated with intravitreal anti-vascular endothelial growth factor therapy: a systematic review and meta-analysis. JAMA Ophthalmol. 2020;138(1):50–57. doi:10.1001/jamaophthalmol.2019.4636
33. Moyal L, Blumen-Ohana E, Blumen M, Blatrix C, Chabolle F, Nordmann JP. Parafoveal and optic disc vessel density in patients with obstructive sleep apnea syndrome: an optical coherence tomography angiography study. Graefes Arch Clin Exp Ophthalmol. 2018;256(7):1235–1243. doi:10.1007/s00417-018-3943-7
34. Çolak M, Özek D, Özcan KM, et al. Evaluation of retinal vessel density and foveal avascular zone measurements in patients with obstructive sleep apnea syndrome. Int Ophthalmol. 2021;41(4):1317–1325. doi:10.1007/s10792-020-01690-0
35. Elnahry AG, Elnahry GA. optical coherence tomography angiography of macular perfusion changes after anti-VEGF therapy for diabetic macular edema: a systematic review. J Diabetes Res. 2021;2021:6634637. doi:10.1155/2021/6634637
 © 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2022 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.