Back to Journals » International Journal of General Medicine » Volume 13
Evaluating the Usefulness of Lab-Based Test for the Diagnosis of Pneumonia in Children
Authors Tarhani F, Nezami A, Heidari G
Received 11 February 2020
Accepted for publication 14 May 2020
Published 27 May 2020 Volume 2020:13 Pages 243—247
DOI https://doi.org/10.2147/IJGM.S249221
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Fariba Tarhani, Alireza Nezami, Ghobad Heidari
Department of Pediatrics, Faculty of Medicine, Lorestan University of Medical Sciences, Khorramabad, Iran
Correspondence: Ghobad Heidari
Department of Pediatrics, Lorestan University of Medical Sciences, Khorramabad, Iran
Email [email protected]
Objective: The aim of this study is to determine the distribution of the results of routine laboratory tests for the diagnosis of pneumonia in children in Khorramabad.
Methods: This is a cross-sectional study and was performed on 650 children with pneumonia who were referred to Shahid Madani Hospital. From patients’ test results, the following data were recorded: whether the results were normal or not, age, sex, serotype, history of diabetes mellitus, and the presence of urinary and digestive tract symptoms.
Results: There was no difference in the prevalence of pneumonia, gender-wise, whereas 40% of the patients were under 2 years. In addition, 53.7% of the patients were presented with leukocytosis. From the blood test, blood urea nitrogen, creatinine, sodium, and potassium were normal in most of the patients. Stool examination, urine analysis, urine culture, erythrocyte sedimentation rate, C-reactive protein, and blood sugar were also normal in these patients.
Conclusion: Children under the age of 2 years are more susceptible to lung infections. Findings from blood tests such as leukocytosis are useful for making initial diagnosis other than computed tomography scan. Other lab tests might not give any useful results. In addition, a closer examination of the urinary system and digestive tract involvement is recommended, prior to urine or stool analysis.
Keywords: pneumonia, children, serum analysis, WBC count, blood glucose, digestive tract
Introduction
Acute respiratory infection, especially pneumonia, is one of the most common infections in childhood, including 30–60% of outpatient visits and 30–40% of hospital admissions.1 According to World Health Organization statistics, pneumonia is the most critical cause of death in children under the age of 5, where ~900,000 children under the age of 5 died due to pneumonia in 2015; which accounts for 16% of the deaths of children in this age group.2 The annual incidence of pneumonia in developing countries is 7–40%, whereas, 2–4% in developed ones, being highest among children under the age of 2.3 The causative agents of pneumonia are divided into two types: infections due to bacteria, viruses, fungi, and parasites, and non-infective causes such as gastric acid and hypersensitivity;4 however, bacteria are the leading cause of pneumonia. Chest radiography is a gold-standard for the diagnosis of pneumonia, where computed tomography (CT scan) is considered as a standard. Additionally, specimen-driven clinical features and culture aid the diagnosis.5 A number of lab-based tests are also exploited as the biomarkers to classify the type of pneumonia such as viral or bacterial. Additionally, urine analysis can be effective for detection of pathogen-specific nucleic acid and antigen.6 Korppi et al (1997),7 Prat et al (2003),8 and Khan et al (2010)9 found that the use of ESR (erythrocyte sedimentation rate), CRP, and CBC (complete blood count) in patients with moderate-to-severe pneumonia and inpatients are useful in determining how to respond to treatment and follow up patients. Similar findings are reported by Hutchinson et al, 2014,10 suggesting that blood tests to be a benchmark for identifying patients with severe pneumonia at early stages of the disease, where on-time treatment of patients and subsequent therapies could lessen mortality rate due to pneumonia. Clinical symptoms of severe pneumonia include; cough along with difficulty in breathing; as standardized by WHO (World Health Organization) and PERCH (Pneumonia Etiology Research for Child Health).11 Several studies have been conducted to rule-out unnecessary administration of antibiotics such as; monitoring symptoms and CRP testing.12 Similarly, clinical findings like ECR, WBC (white blood cell), and CRP can reduce the need for radiographic screening.13 To it, radiographic screening might also lead to misdiagnosis.14
The aim of this study was to evaluate the results of routine laboratory tests like ESR, blood culture (BC), blood urea nitrogen (BUN), creatinine (Cr), sodium (Na), and potassium (K), CRP, WBC, blood glucose (BS), urine analysis (U/A), urine culture (U/C), and stool examination (S/E) among pediatric pneumonia patients referred to Khorramabad Shahid Madani Hospital.
Methods
Type of Study and Sample Size
The present study is a cross-sectional study. The study population includes all children presenting pneumonia, referred to Shahid Madani Hospital in Khorramabad.
Patient Information
Among the patients in the children’s ward of the Shahid Madani Hospital during 2016–2017, who were admitted to the pediatric ward, samples for diagnosis of pneumonia were selected using simple random sampling. Written consent was obtained from the parents/guardians of all the children included in the study. Based on the sample size of 650 people, with the help of the information of the hospital registry system, the patients’ history was obtained during the years 2016–2017, and then the cases were handed over to the medical records section using the file number. Diagnosis of pneumonia was made based on chest X-ray (consolidation; presence of fluffy or dense opacity with or without air, pleural effusion or linear and patchy alveolar or interstitial opacities). Data were extracted from patients’ records and recorded in a checklist; the information extracted in this study included; age, sex, serotype, history of diabetes mellitus, and the presence of urinary and digestive tract symptoms, as well as data on the results of laboratory parameters such as WBC, ESR, CRP, B/C, BS, U/A, U/C, S/E, Na, K, BUN, and Cr.
Statistical Analysis
The extracted data were finally recorded in SPSS software and the data were analyzed using statistical indices. It is worth noting that this study is purely descriptive and does not have an analytical test.
Ethical Considerations
The instruction of this study has been approved by the Ethics Committee of Lorestan University of Medical Sciences. The extracted data from the patients' file were completely confidential without mentioning the patients’ names in accordance with the Declaration of Helsinki; therefore, patient parental consent was waived.
Results
This study was performed on 650 patients admitted in Shaheed Madani Hospital with diagnosis of pneumonia. Fifty-two percent of the patients were male and 48% were female (Figure 1). In terms of age, it was also found that most patients (260) were under 2 years of age (Figure 2).
 |
Figure 1 Frequency of patients based on gender. |
 |
Figure 2 The percentage of patients based on age. |
The findings from this study indicated that half of the patients (53.7%) had white blood cells (WBCs) higher than normal. BC was also reported as normal in most patients (84%). BUN, Cr, sodium, and potassium have also been reported as normal in all patients. Other laboratory tests include stool examination, urinalysis, urine culture, ESR, CRP, and blood glucose were also normal in most of the patients (Table 1).
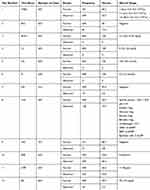 |
Table 1 Results of the Tests Checked in the Diagnosis of Pneumonia in Children |
Discussion
In parallel with the previous findings, most patients were diagnosed with abnormal WBC in this study.16 Hutchinson et al (2014) found that it is valuable to use blood tests as a benchmark for the identification of patients with severe pneumonia to obtain effective treatment results. The result of blood culture (BC) was only positive in a small number of patients (12.5%), which is consistent with Zar et al (2005).15 The researchers found that one of the diagnostic limitations of blood cultures in detecting childhood pneumonia is that it does not have positive outcomes in majority of the patient, which is consistent with our study.
Based on the findings, it was found that, among the tests performed in the studied patients, the highest rates of positive results were related to WBC, ESR, and CRP; in this regard, Korppi et al (1997), Nohynek et al (1995),16 Khan et al (2010), and Prat et al (2003) found that the use of ESR, CRP, and CBC in patients with moderate and severe pneumonia and hospitalized patients is helpful in determining how to respond to treatment and follow up patients. They reported that high levels of WBC, neutrophils, ESR, and procalcitonin correspond to the severity of the disease.
However, 63.8% of patients were under the age of 5 years, of whom 40% were under the age of two. These findings are consistent with the findings of the study by Barati et al (2010).17 The researchers found that the prevalence of pneumonia was higher in males than females; Yet, in this study, we could not conclude gender-based skew results. They also reported that most patients with bacterial pneumonia were under the age of 5 years. Similarly, Daniel et al (2005) found that children under 5 years of age are more likely to develop pneumonia than ages (ages 5 to 15).
The levels of BUN, Cr, Na, and K were normal in all patients. Blood glucose, stool testing, and urine culture were found abnormal in a low percentage of patients. Also, abnormal urine tests were positive in less than 20% of the patients, in regard to WBC, RBC, and bacteria.
Conclusion
These findings demonstrate the low value of these tests in diagnosing pneumonia. Urinalysis tests, urine culture, and stool testing have been studied in some patients without urinary and digestive tract symptoms, which might not be necessary. With regard to this and previous studies, it is suggested Na, K, BUN, Cr, and blood glucose might not be useful for screening patients suspected for pneumonia. Also, a closer examination of the history of the patient in terms of urinary and digestive tract symptoms can be useful before clinical examination, including urine and stool analysis, since the application of these tests imposes additional financial burden on the health system and can increase the occupancy of the health system staff and the field, compromising the accuracy of work and increasing the chances of medical errors. Chest radiography is a gold-standard for the diagnosis followed by the culture, and additional tests may not be necessary for diagnostic purposes. Signs and symptoms regarding other commodities might require the use of these clinical parameters.
Data Sharing Statement
Data sharing is not applicable to this article as no datasets were generated or analyzed during the current study.
Author Contributions
All authors contributed to data analysis, drafting or revising the article, gave final approval of the version to be published, and agree to be accountable for all aspects of the work.
Funding
No funding was secured for this study.
Disclosure
The authors deny any conflict of interest in any terms or by any means during the study.
References
1. Rudan I, Boschi-Pinto C, Biloglav Z, Mulholland K, Campbell H. Epidemiology and etiology of childhood pneumonia. Bull World Health Organ. 2008;86:408–16B. doi:10.2471/BLT.07.048769
2. Bryce J, Boschi-Pinto C, Shibuya K, Black RE, Group WCHER. WHO estimates of the causes of death in children. The Lancet. 2005;365(9465):1147–1152. doi:10.1016/S0140-6736(05)71877-8
3. McLuckie A. Respiratory Disease and Its Management. Springer Science & Business Media; 2009.
4. Tiewsoh K, Lodha R, Pandey RM, Broor S, Kalaivani M, Kabra SK. Factors determining the outcome of children hospitalized with severe pneumonia. BMC Pediatr. 2009;9(1):15. doi:10.1186/1471-2431-9-15
5. Makhnevich A, Sinvani L, Cohen SL, et al. The clinical utility of chest radiography for identifying pneumonia: accounting for diagnostic uncertainty in radiology reports. Am J Roentgenol. 2019;213(6):1207–1212. doi:10.2214/AJR.19.21521
6. Zar HJ, Andronikou S, Nicol MP. Advances in the diagnosis of pneumonia in children. BMJ. 2017;358:j2739. doi:10.1136/bmj.j2739
7. Korppi M, Heiskanen-Kosma T, Leinonen M. White blood cells, C-reactive protein and erythrocyte sedimentation rate in pneumococcal pneumonia in children. Eur Respir J. 1997;10(5):1125–1129. doi:10.1183/09031936.97.10051125
8. Prat C, Dominguez J, Rodrigo C, et al. Procalcitonin, C-reactive protein and leukocyte count in children with lower respiratory tract infection. Pediatr Infect Dis J. 2003;22(11):963–967. doi:10.1097/01.inf.0000095197.72976.4f
9. Khan DA, Rahman A, Khan FA. Is procalcitonin better than C‐reactive protein for early diagnosis of bacterial pneumonia in children? J Clin Lab Anal. 2010;24(1):1–5. doi:10.1002/jcla.20333
10. Apps L, Hutchinson S, Leary T, Perry L. Can laboratory blood tests be used to risk stratify patients admitted with pneumonia? Critical Care. 2014;18(1):P253. doi:10.1186/cc13443
11. Scott JAG, Wonodi C, Moïsi JC, et al. The definition of pneumonia, the assessment of severity, and clinical standardization in the Pneumonia Etiology Research for Child Health study. Clin Infect Dis. 2012;54 Suppl 2(Suppl2):S109–S16. doi:10.1093/cid/cir1065
12. Held U, Steurer-Stey C, Huber F, Dallafior S, Steurer J. Diagnostic aid to rule out pneumonia in adults with cough and feeling of fever. A validation study in the primary care setting. BMC Infect Dis. 2012;12:355. doi:10.1186/1471-2334-12-355
13. Ebrahimzadeh A, Mohammadifard M, Naseh G, Clinical MA. Laboratory findings in patients with acute respiratory symptoms that suggest the necessity of chest x-ray for community-acquired pneumonia. Iran J Radiol. 2015;12(1):e13547–e. doi:10.5812/iranjradiol.13547
14. Laushkina Z. The analysis of factors associated with misdiagnosis pneumonia in TB hospital. 2015;46(suppl 59):PA1524.
15. Zar H, Jeena P, Argent A, Gie R, Madhi S. Diagnosis and management of community-acquired pneumonia in childhood-South African Thoracic Society Guidelines. South Afr Med J. 2008;95(12):975–990.
16. Nohynek H, Valkeila E, Leinonen M, Eskola J. Erythrocyte sedimentation rate, white blood cell count and serum C-reactive protein in assessing etiologic diagnosis of acute lower respiratory infections in children. Pediatr Infect Dis J. 1995;14(6):484–490. doi:10.1097/00006454-199506000-00004
17. Barati M, Javad Mousavi S, Noorbakhsh S, Talebi Taher M, Ehteshami Afshar A, Tabatabaii A. Determination of pneumococcal pneumonia frequency through isolation of pneumococcal antigen from urine using immunochromatographic method (Binax NOW). Razi J Med Sci. 2010;17(71):34–40.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
