Back to Journals » Clinical Ophthalmology » Volume 14
Encircling Scleral Buckle with Chandelier Endoillumination and Endolaser for Repair of Rhegmatogenous Retinal Detachment
Authors Yannuzzi NA, Patel NA , Berrocal AM, Sridhar J
Received 12 November 2019
Accepted for publication 29 January 2020
Published 28 February 2020 Volume 2020:14 Pages 609—612
DOI https://doi.org/10.2147/OPTH.S238241
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Scott Fraser
Supplementary video of "Chandelier Buckle with Endolaser for Retinal Detachment" [ID 238241].
Views: 44504
Nicolas A Yannuzzi, Nimesh A Patel, Audina M Berrocal, Jayanth Sridhar
Department of Ophthalmology, Bascom Palmer Eye Institute, University of Miami Miller School of Medicine, Miami, FL 33136, USA
Correspondence: Jayanth Sridhar
Department of Ophthalmology, Bascom Palmer Eye Institute, University of Miami, Miller School of Medicine, 900 NW 17th Street, Miami, FL 33136, USA
Tel +1 305 326-6000
Email [email protected]
Purpose: To report a modified surgical technique for chandelier endoillumination-assisted scleral buckling using an endolaser.
Methods: A three patient case reports for demonstration of surgical technique.
Results: All patients underwent successful primary retinal detachment repair without any intraoperative or post-operative complications.
Conclusion: Endolaser can be employed during chandelier endoillumination assisted scleral buckling either as a standalone tool or in conjunction with cryopexy, especially in cases with posteriorly located retinal breaks.
Keywords: rhegmatogenous retinal detachment, scleral buckle, chandelier, endoillumination, endolaser
Introduction
Since its inception in the 1950s,1 and for subsequent decades, scleral buckling has been a useful surgical technique for the repair of rhegmatogenous retinal detachments (RRDs), especially in young, phakic patients,2 without a complete posterior vitreous detachment.3 Despite its long-standing track record, scleral buckling is being employed less commonly and accounts for only a small portion of the vitreoretinal fellowship training experience.4 Scleral buckling is conventionally performed under indirect ophthalmoscopic viewing but has also been described using chandelier illumination and a noncontact wide-angle microscopic viewing system, in conjunction with cryopexy or indirect laser photocoagulation.5 The purpose of this case presentation is to demonstrate a previously undescribed variation of the chandelier assisted encircling buckle technique, whereby an illuminated endolaser is used in addition to, or in place of, a cryotherapy probe to perform retinopexy.
Surgical Technique
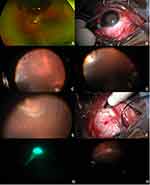
A 28-year-old man presented with vision loss for 2 weeks and a chronic macula involving inferotemporal RRD with retinal holes (Figure 1A). The decision was made to proceed with a primary scleral buckle. A conjunctival peritomy was performed and the rectus muscles isolated. A 25-gauge valved trocar was then placed 90 degrees away from the area of pathology to minimize risk to the phakic lens (Figure 1B, Supplementary video). The chandelier was held at all times rather than secured to allow for better safety, mobility, and visualization. Next, the periphery was inspected under scleral depression and retinal breaks were identified (Figure 1C). Cryopexy was then applied under direct supervision by the attending surgeon to the larger break (Figure 1D). Under scleral depressed exam, there was a smaller, more posteriorly located break noted (Figure 1E). Access to this break was limited with the bulkier cryopexy probe because of its more posterior location and its location under the inferior rectus muscle. The decision was instead made to perform laser retinopexy at the conclusion of the procedure. The most posterior break was then marked with a scleral depressor followed by a marking pen placed just posterior to the initial mark to account for parallax and to ensure that the break was supported by the encircling scleral band (Figure 1F). Buckle placement and drainage of subretinal fluid were then carried out in the normal fashion under direct visualization. Next, the peripheral retina was again examined under the microscope with the aid of the chandelier. As shallow residual fluid remained, indirect laser was felt to be challenging to achieve sufficient uptake. Thus, a curved illuminated endolaser probe was inserted through the same trocar in which the chandelier light had been introduced previously. A continuous laser, with power setting of 250–300 mW, was used to perform retinopexy (Figure 1G and H). Excessive insertion of the probe into the eye was avoided to minimize the degree of induced vitreous traction. The buckle height was then adjusted, and an anterior chamber paracentesis performed to normalize the intraocular pressure. The trocar was then removed and the sclerotomy and conjunctiva were closed with plain gut suture. The other 2 patients received scleral buckling with chandelier endoillumination and adjunctive endolaser in the same fashion for phakic RRDs.
Surgical Outcome and Follow-Up
After 6 months of follow-up, the retina has remained attached and there have been no intra or post-operative complications, iatrogenic breaks, vitreomacular traction, epiretinal membrane, or macular edema in all 3 patients.
Discussion
We describe the use of chandelier illumination scleral buckling with endolaser in addition to, or in place of, the current standards of cryopexy or indirect laser. While the method described may not be a first-line tool for the repair of RRDs, it can carry practical value as an option in certain circumstances.
Potential advantages reported of chandelier assisted buckling include improved visualization of the peripheral retina, direct viewing during external drainage of subretinal fluid, facility in conversion to pars plana vitrectomy, enhanced teaching capabilities, and improved ergonomics.5 Reported series of chandelier assisted buckling for the treatment of retinal detachment have traditionally achieved retinopexy with cryotherapy or indirect laser. Assi et al6 published a series of 25 eyes with RRD treated with endoillumination-assisted modified scleral buckling. In this technique, a chandelier was inserted via a 23-gauge valved trocar for direct non-contact wide-angle microscopic viewing and cryotherapy employed for retinopexy. The technique resulted in favorable anatomic outcomes and no entry site retinal breaks were detected. Likewise, Aras et al7 and Caporossi et al8 reported favorable anatomic results using a similar method, with the exception of employing 25-gauge and 27-gauge systems, respectively. A randomized controlled trial of RRDs treated with scleral buckle has demonstrated no difference in reattachment rates when comparing cryopexy and delayed indirect laser.9
Cryopexy in scleral buckling does have some drawbacks when compared to laser retinopexy. In cases where the retinal break is posterior, as in the case presented, or directly beneath the recti muscles, it may be technically challenging to position the probe for treatment.10 Collateral muscle damage might contribute to transient diplopia.10,11 Cryopexy is also considered to trigger inflammation. Studies have verified that cryotherapy treatment can cause the breakdown of the blood-ocular barrier and promote the dispersion of retinal pigmented epithelium (RPE) cells.12–14 It has been suggested that in certain cases, with horseshoe and giant tears, that cryopexy is a risk factor for PVR in comparison to laser.15
For the choice of using indirect laser for retinopexy, there are likewise some limitations. Treatment effect may be hampered by imprecise visualization of breaks when compared to the chandelier assisted wide-angle viewing system. In conditions where shallow subretinal fluid remains after drainage, or if there is vitreous debris or hemorrhage, it can be difficult to obtain uptake. Moreover, the routine use of indirect laser may be compromised by lack of availability in some surgical centers.
In our technique, the illuminated endolaser may be inserted through the same trocar as the initial chandelier illuminator, allowing for excellent laser uptake and clear visualization, without the need for further sclerotomies. It may also allow for more optimal angles between the retina around the laser site and the direction of laser delivery. The primary concern in this approach is the potential for vitreous traction and retinal breaks or dialyses caused by endolaser insertion into a nonvitrectomized eye. In order to mitigate this theoretical risk, care must be taken to avoid unnecessary manipulation or excessive insertion of the probe and to carefully examine the periphery for iatrogenic breaks. In all cases presented, no iatrogenic breaks were detected, but we recognize the potential risk or drawbacks of this technique. This method should be examined further in a prospective manner to assess its safety. An additional limitation of this technique is the added cost of the laser probe.
In this small case series, we find the use of the endolaser in endoillumination assisted scleral buckling as safe and effective in the treatment of rhegmatogenous retinal detachment. Although this approach is not advisable or necessary in all cases, it is an alternative option in circumstances where cryopexy or indirect laser pose technical challenges.
Ethics and Informed Consent
All patients in this case series provided written informed consent for their data, case details and any accompanying images to be published as part of a generalized imaging consent form. Institutional review board approval was not required for this study as it was a case report defined as three patients or fewer.
Funding
This study is supported in part by the Heed Foundation.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Schepens CL, Okamura ID, Brockhurst RJ. The scleral buckling procedures. I. Surgical techniques and management. AMA Arch Ophthalmol. 1957;58(6):797–811. doi:10.1001/archopht.1957.00940010819003
2. Heimann H, Bartz-Schmidt KU, Bornfeld N, et al. Scleral buckling versus primary vitrectomy in rhegmatogenous retinal detachment: a prospective randomized multicenter clinical study. Ophthalmology. 2007;114(12):2142–2154. doi:10.1016/j.ophtha.2007.09.013
3. Noori J, Bilonick RA, Eller AW. Scleral buckle surgery for primary retinal detachment without posterior vitreous detachment. Retina. 2016;36(11):2066–2071. doi:10.1097/IAE.0000000000001075
4. Bakri SJ, Alniemi ST, Chan RV. Experiences of vitreoretinal surgery fellows in the United States. Retina. 2013;33(2):392–396. doi:10.1097/IAE.0b013e31826b6700
5. Seider MI, Nomides RE, Hahn P, Mruthyunjaya P, Mahmoud TH. Scleral buckling with chandelier illumination. J Ophthalmic Vis Res. 2016;11(3):304–309. doi:10.4103/2008-322X.188402
6. Assi A, Abdelmassih Y, El-Khoury S. Endoillumination-assisted modified scleral buckling. Retina. 2018;38(2):320–324. doi:10.1097/IAE.0000000000001568
7. Aras C, Ucar D, Koytak A, Yetik H. Scleral buckling with a non-contact wide-angle viewing system. Ophthalmologica. 2012;227(2):107–110. doi:10.1159/000333101
8. Caporossi T, Finocchio L, Barca F, Franco F, Tartaro R, Rizzo S. Scleral buckling for primary rhegmatogenous retinal detachment using a noncontact wide-angle viewing system with a cannula-based 27-G chandelier endoilluminator. Retina. 2019;39:S144–S150. doi:10.1097/IAE.0000000000001891
9. Lira RP, Takasaka I, Arieta CE, Nascimento MA, Caldato R, Panetta H. Cryotherapy vs laser photocoagulation in scleral buckle surgery: a randomized clinical trial. Arch Ophthalmol. 2010;128(12):1519–1522. doi:10.1001/archophthalmol.2010.271
10. Govan JA. Prophylactic circumferential cryopexy: a retrospective study of 106 eyes. Br J Ophthalmol. 1981;65(5):364–370. doi:10.1136/bjo.65.5.364
11. Fison PN, Chignell AH. Diplopia after retinal detachment surgery. Br J Ophthalmol. 1987;71(7):521–525. doi:10.1136/bjo.71.7.521
12. Campochiaro PA, Kaden IH, Vidaurri-Leal J, Glaser BM. Cryotherapy enhances intravitreal dispersion of viable retinal pigment epithelial cells. Arch Ophthalmol. 1985;103(3):434–436. doi:10.1001/archopht.1985.01050030130038
13. Veckeneer M, Van Overdam K, Bouwens D, et al. Randomized clinical trial of cryotherapy versus laser photocoagulation for retinopexy in conventional retinal detachment surgery. Am J Ophthalmol. 2001;132(3):343–347. doi:10.1016/S0002-9394(01)01026-1
14. Arrindell EL, Wu JC, Wolf MD, et al. High-resolution magnetic resonance imaging evaluation of blood-retinal barrier integrity following transscleral diode laser treatment. Arch Ophthalmol. 1995;113(1):96–102. doi:10.1001/archopht.1995.01100010098027
15. Bonnet M, Fleury J, Guenoun S, Yaniali A, Dumas C, Hajjar C. Cryopexy in primary rhegmatogenous retinal detachment: a risk factor for postoperative proliferative vitreoretinopathy? Graefes Arch Clin Exp Ophthalmol. 1996;234(12):739–743. doi:10.1007/BF00189354
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.