Back to Journals » Psychology Research and Behavior Management » Volume 13
Emphasizing the “Cultural” in Sociocultural: A Systematic Review of Research on Thin-Ideal Internalization, Acculturation, and Eating Pathology in US Ethnic Minorities
Received 15 October 2019
Accepted for publication 18 January 2020
Published 1 April 2020 Volume 2020:13 Pages 319—330
DOI https://doi.org/10.2147/PRBM.S204274
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Mei-Chun Cheung
Cortney S Warren,1,2 Liya M Akoury3
1Department of Psychology, University of Nevada - Las Vegas, Las Vegas, NV, USA; 2Choose Honesty, LLC., Las Vegas, NV, USA; 3Walden Behavioral Care, Amherst, MA, USA
Correspondence: Cortney S Warren
Choose Honesty, LLC., 4044 N Lincoln Avenue, Unit 319, Chicago, IL 60618, USA
Email [email protected]
Abstract: A large body of research suggests that thin-ideal internalization is a robust predictor of eating pathology in women and, to some degree, in men. Recent research is exploring the relationships between thin-ideal internalization and culture-specific factors that may be salient to women and men who live in the US but are marginalized based on racial or ethnic background, such as acculturation. This systematic review summarizes published articles examining the relationships among thin-ideal internalization, acculturation-related constructs (including assimilation, marginalization, biculturalism, and acculturative stress), and eating pathology in US adults. Following the PRISMA method, 15 empirical studies met inclusion criteria. Although existing literature was sparse and conflicting in large part due to heterogeneity in acculturation measures, results yielded some support for positive correlational relationships between acculturative stress, thin-ideal internalization, and eating pathology for both men and women (in 4 out of 5 relevant studies). Research on other aspects of acculturation (eg, integration, assimilation) is mixed, with some existing research suggesting a positive relationship and other research finding no statistically significant relationship. Future research would particularly benefit from a gold-standard, multidimensional transcultural measure of acculturation to examine how the acculturation process relates to thin-ideal internalization and eating pathology in ethnic and racial minorities in the US.
Keywords: eating pathology, thin-ideal internalization, acculturation, acculturative stress, biculturalism, generational status
Introduction
A large body of research suggests that thin-ideal internalization is a robust predictor of eating pathology in women,1–4 and to some extent, in men.5,6 Defined as the personal acceptance and endorsement of thin cultural body ideal, research suggests that thin-ideal internalization is positively correlated with numerous aspects of eating pathology, including body dissatisfaction,7 disordered eating,3 binge eating,8 purging,9 and dietary restriction10 in adult samples of women. Furthermore, a recent meta-analysis3 found that thin-ideal internalization prospectively predicts disordered eating cognitions and behaviors, with small-to-medium effect sizes. Similar findings have emerged in studies using samples of children and adolescents.11
Research on thin-ideal internalization emerged from sociocultural models of eating disorder development (eg, the Tripartite Model) that describe how values and ideals of appearance prevalent in mainstream Western cultures perpetuate eating pathology (see12–14). In general, sociocultural models argue that living in a cultural climate that places paramount importance on physical appearance as a determinant of value and idealizes an unrealistically thin body, particularly for women, predisposes individuals to struggle with eating pathology as they unsuccessfully strive to attain the ideal appearance. As such, thin-ideal internalization emerges as individuals are exposed to Western values (through the media, family/parents, peers, and other culturally-influenced entities), become aware of cultural values and ideals of appearance, and feel pressure to attain these ideals (eg, through excessive dieting, exercise, use of make-up/plastic surgery).
Thin-Ideal Internalization in Racially and Ethnically Marginalized Groups
Given the powerful influence of thin-ideal internalization on the development of eating pathology and its etiological ties to Western cultural values and ideals of appearance, researchers and clinicians need to understand how thin-ideal internalization interacts with other culturally-salient factors to protect or put minorities at greater risk for eating pathology. To date, one of the most investigated topics is the direct and moderating roles of ethnicity and race on the relationships between thin-ideal internalization and eating pathology in samples of women in the United States (US).7,15,16 Race refers to self-identified belonging to one or more groups based on physical characteristics, such as skin color and eye shape (eg, Asian American); while ethnicity refers to self-identified belonging to one or more groups based on shared ancestry or culture (eg, Han Chinese or Chinese American17). This review focuses on ethnic/racial minority individuals in the US who are marginalized based on their race (eg, Black), ethnicity (eg, Armenian American women), or both.
Theoretically, ethnic/racial minority individuals may possess an array of culture-specific risk and protective factors for thin-ideal internalization and/or disordered eating as they move to the US. Ethnic/racial minorities in the US may: 1) experience thin-ideal internalization in the acculturative context of navigating their ancestral vs mainstream Western cultures;18 2) internalize alternative or additional beauty ideals (eg, a curvy, rather than thin physique; a larger body ideal for men and women) and/or place less value on physical appearance as a determinant of worth;7 and 3) experience mainstream Western appearance ideals as particularly unattainable (as the mainstream Western ideal is Eurocentric, as well as thin2). Taken together, disordered eating etiology in racial/ethnic minorities in the US may be more complex than in White samples of European descent; and retrofitting sociocultural models for disordered eating risk for ethnic/racial minorities may overlook key contributors to disordered eating etiology.
Unfortunately, these culture-specific considerations are absent from most thin-ideal internalization and disordered research focusing on ethnic/racial minority women;16 and, data on the role of race and ethnicity as it relates to thin-ideal internalization and disordered eating are mixed. On one hand, some research suggests that women of color are protected from eating pathology compared to White women of European descent.19 On the other hand, a recent longitudinal investigation found no significant ethnic differences in eating disorder prevalence, predictive risk prevalence, or future onset of an eating disorder.15
Thin-Ideal Internalization, Acculturation, and Eating Pathology
Instead of looking at the relationship between race or ethnicity to thin-ideal internalization and eating pathology, examining how culture-specific variables (eg, acculturation, acculturative stress) influence or correlate with thin-ideal internalization and disordered eating in ethnic/racial minorities in the US may be more meaningful because such variables are theoretically tied to the cultural values and ideals of a person. Acculturation is the process of simultaneous cultural and psychological change as a result of navigating two or more cultural groups.20,21 Specifically, individuals may identify predominantly with their acquired culture (ie, assimilation); identify predominantly with their native culture (ie, separation); identify with both cultures (ie, integration or biculturalism); or, with neither culture (ie, marginalization). In general, research indicates biculturalism is associated with the best mental health outcomes, while marginalization is associated with the worst.20,21
Furthermore, the relationship between acculturation and mental health outcomes may be mediated by acculturative stress, or the aggregate physical, biological, social, cultural, and psychological difficulties that individuals have to face as they encounter a new culture.22–24 Specifically, research on acculturative stress suggests that it negatively impacts general mental health22,25,26 and buffers/accounts for the association between biculturalism and overall mental health.22,23 With regard to thin-ideal internalization and eating pathology, as women of color from different cultural contexts adapt to Western cultural contexts (eg, US), they are confronted with a barrage of cultural messages promoting a thin, White, young ideal of beauty that is highly prized for women. Theoretically, as women acculturate immediately after immigrating (ie, first generation) or over many generations, the process can encourage or discourage women from internalizing a thin-ideal, thereby putting them at greater or lesser risk for eating pathology.
Thin-Ideal Internalization and Acculturation in Ethnic/Racial Minority Men
Although thin-ideal internalization is historically framed through a gender-based lens, emerging research suggests that men experience considerable sociocultural pressure to maintain a thin and fit physique.5,6 As men are exposed to Western values, they become aware of a largely unattainable thin, muscular, athletic societal ideal for men. Whereas women are generally focused on thinness (ie, thin-ideal internalization), men may focus on thinness and/or gaining muscle (referred to as athletic-ideal internalization27,28) as both reflect Western cultural values and ideals of appearance for men.
Some research suggests that thin-ideal or general-media internalization (which is associated with low body fat) is a predictor of eating pathology for men (eg, body dissatisfaction29,30). For example, in the development and validation of the SATAQ-4, Schaefer et al31 found that items reflecting internalization of a thin/low body fat ideal loaded on a separate subscale than items reflecting internalization of a muscular ideal (labeled muscular/athletic ideal internalization) in a sample of 271 US male college students. Furthermore, thin-ideal internalization was more strongly correlated with eating pathology (ie, EDE-Q scores, largely focused on shape concerns and a desire to lose weight) than athletic-ideal internalization, which may be more strongly related with muscle dysmorphia (or a desire to gain muscle mass and have low body fat).
In addition, some research suggests that ethnic and racial minority men endorse greater body dissatisfaction32 and use more extreme body-altering behaviors compared to White males.5,6 For example, in a recent study of 343 college men,33 Asian American and Hispanic/Latino men reported greater drive for muscularity, muscle dysmorphia, global eating pathology, body checking, binge eating, and driven exercise compared to African American and European American men. In addition, given that rates of overweight or obesity tend to be higher in ethnic minority groups in the US34 and are directly counter to US ideals of appearance for both men and women,35,36 adolescent boys and men from ethnic/racial minority groups who are overweight may be more likely to internalize a male thin-ideal and strive to lose weight. For example, high BMI is associated with increased disordered eating behaviors in Asian American men37 and increased body dissatisfaction and thinness expectancies in Latino boys.38 As such, further examination of acculturation, thin-ideal internalization, and eating pathology in ethnic or racial minority men in the US is warranted.
Current Study
Given the robust relationship between thin-ideal internalization and eating pathology, many scholars have specifically called attention to the need for research examining how culture-specific factors like acculturation and acculturative stress relate to internalization of the greater sociocultural context and eating pathology.15,23,39–42,44–48 Given that 30.9% of Americans are people of color or multiracial and 12.9% of Americans are first-generation,49 the lack of existing research in this area is noteworthy. Consequently, the overarching goal of this systematic review is to summarize empirical articles examining the relationships among thin-ideal internalization, acculturation, and eating pathology in US adults. Specifically, we reviewed published studies that measured internalization of a thin cultural ideal, eating pathology (broadly defined), and an acculturation-related construct by directly measuring cultural identity (eg, assimilation, biculturalism), using a proxy to approximate acculturation (eg, generational status), or measuring an important aspect of the acculturation process (eg, acculturative stress).
Methods
This review follows the PRISMA statement for reporting systematic reviews and meta-analyses. We used PubMed and SCOPUS to identify relevant papers for inclusion, conducting the search in June and August, 2019. The following seven dyadic and one triadic search terms were used: 1) “Thin-ideal internalization” and “Acculturation”; 2) “Thin-ideal internalization” and “Acculturative stress”; 3) “Internalization” and “Acculturation”; 4) “Thin-ideal internalization” and “Generational status”; 5) “Internalization” and “Generational status”; 6) “Thin-ideal internalization” and “Disordered Eating”; 7) “Eating pathology” and “Immigrants”; 8)“Acculturation” and “Eating disorders” and “Internalization.” The search was conducted by the two study authors. To be included, studies must have been published in peer-reviewed journals and written in English. In addition, studies must have used: 1) a sample of greater than 10 participants age 18 and older; 2) assessed for thin-ideal internalization; 3) assessed for acculturation (either directly using a measure of biculturalism or cultural identity or using a proxy like generational status) and/or acculturative stress; and 4) assessed for eating pathology (broadly defined).
While conducting our review, there were many studies that included constructs related to thin-ideal internalization (eg, drive for thinness, fat phobia) that were not specifically looking at personal acceptance and desire to attain a thin ideal based on cultural values and ideals. Consequently, we excluded studies that did not specifically measure sociocultural aspects of thin-ideal acceptance and internalization; did not have a thin-ideal internalization focus; did not focus on eating pathology of some type; did not include a measure of acculturation; focused on non-diaspora population (ie, Fijian adolescents in Fiji); or described a case study.
Results
General Literature Review Information
Figure 1 summarizes the PRISMA50 literature review procedure. Out of 175 unique identified records, 27 were included in the qualitative synthesis. Reasons for exclusion were: 1) record had no thin-ideal internalization focus; 2) record had no eating pathology or body dissatisfaction focus; 3) record had no acculturation focus; 4) record did not focus on an ethnic/racial minority population (ie, Taiwanese adolescents in Taiwan; deaf women in the US); 5) record described a case study; and 6) record did not include an adult US sample. Of them, 15 (9% of total) were included in the quantitative review and 12 (7% of total) were noted for qualitative overview only because they were reviews or commentaries.
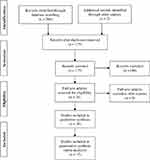 |
Figure 1 Overview of PRISMA literature review procedure. Notes: Adapted from Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group (2009) Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med 6(7): e1000097.50 Reasons for exclusion were: 1) record had no thin-ideal internalization focus; 2) records had no disordered eating focus; 3) record had no acculturation focus; 4) record focused on non-diaspora population (ie, Taiwanese adolescents in Taiwan); 5) record described a case study; and 6) record did not include an adult US sample. Among the 28 studies included in qualitative synthesis, 13 were excluded from the quantitative synthesis because they were reviews or commentaries. |
Overview of Included Studies
Sampled Populations
A total of 15 studies met inclusion criteria for this quantitative review. Among them, 12 studies included a female sample (see Table 1) and 5 included a male sample (see Table 2), with two of those studies including both men and women (Menon et al (2012)51 and Blow et al (2010)52 which are double listed in Tables 1 and 2). Of the 15 studies, seven focused on Latinx participants, seven focused on Asian American participants, and one study focused on White, Black, and Latina participants (ie, Gordon et al (2010)53). Most (13) examined college students and/or predominantly college-aged adults, with mean ages in the early 20’s. One study (Reddy and Crowther (2007)18) examined adolescents and adults, while another (Liao et al (2019)54) used a community sample of adults. All studies were correlational surveys, except Franko et al (2012)55 and Liao et al (2019),56 which were qualitative.
 |
Table 1 Studies Examining the Relationships Between Thin-Ideal Internalization, Acculturation, and Eating Pathology by Type of Acculturation Measured in Women |
 |
Table 2 Studies Examining the Relationships Between Thin-Ideal Internalization, Acculturation, and Eating Pathology by Type of Acculturation Measured in Men |
Thin-Ideal Internalization Measures
Of the quantitative studies that used a questionnaire to measure thin-ideal internalization, almost all used the original or a revised version of the Sociocultural Attitudes Towards Appearance Questionnaire (SATAQ31,57–59). The two exceptions were Reddy and Crowther (2007),18 who used the Ideal-Body Internalization Scale-Revised (IBIS-R60), and Gordon et al53 who used image ratings of cultural ideal body size.
Eating Pathology Measures
Among the quantitative studies, ten assessed for body dissatisfaction only, while four broadly assessed eating pathology (eg, restrictive eating, binge eating), and one study (Poloskov and Tracey, 201361) assessed both. Measures of eating pathology measures included the Eating Attitudes Test62 and the Eating Disorders Inventory.63 Measures examining body dissatisfaction (or body satisfaction) were: 1) Body Esteem Scale;64 2) Body Areas Satisfaction Questionnaire;65 3) Multidimensional Body-Self Relations Questionnaire;65 4) Drive for Muscularity Scale;66 5) Muscle Appearance Satisfaction Scale;67 6) Body Happiness Questionnaire;52 7) Body Shape Questionnaire;81 8) Body Parts Satisfaction Scale;68 and 9) the Body Comparison Scale.69
Acculturation Measures
The studies used a variety of measures of acculturation. Specifically, nine studies used culture-specific measures designed for a given ethnic or cultural group, including the Acculturation Rating Scale for Mexican Americans-II70 (ARSMA-II); Cultural Values Conflict Scale for South Asian Women71 (CVCS); Suinn-Lew Asian Self-Identity Acculturation Scale72 (SL-ASIA); Short Acculturation Scale for Hispanics73 (SASH); and the Asian Values Scale74 (AVS). An additional four studies used transcultural measures designed for participants moving from any cultural context, including the Riverside Acculturative Stress Inventory75 (RASI); Vancouver Index of Acculturation76 (VIA); American-International Relations Survey77 (AIRS); and the Stephenson Multi-Group Acculturation Measure78 (SMAS). Finally, one study used language spoken at home as a proxy for acculturation (Nouri et al, 201179), while one assessed acculturation qualitatively (Liao at al, 201956).
In terms of the kinds of acculturation studies aimed to measure (eg, assimilation, marginalization, biculturalism), almost all focused on assimilation, with two exceptions. First, Reddy and Crowther, 200718 measured cultural conflict (ie, the opposite of cultural integration; using CVCS). Second, Gordon et al, 201053 used the dominant society immersion (EDI) and ethnic society immersion (ESI) subscales of the SMAS,78 to measure assimilation and separation, respectively (but, unfortunately, did not measure their associations with thin-ideal internalization). In addition, two studies (ie, Cheng et al 2015 and Lau et al 2006)80,82 measured separation/marginalization (ie, attachment to Asian cultural values only) and three studies measured acculturative stress (ie, Menon et al 2012; Reddy and Crowther, 2007; Warren et al 2010).18,51,83
Thin-Ideal Internalization, Acculturation and Eating Pathology in Women
As shown in Table 1, existing empirical research yields conflicting evidence regarding the relationships among thin-ideal internalization, acculturation, and eating pathology. Of the 12 studies that examined the relationship between assimilation (ie, the degree to which individuals identify with mainstream American culture), thin-ideal internalization and eating pathology, three found positive relationships while six found non-significant results. In addition, of the three studies that measured acculturative stress, two found a significant positive relationship whereas one did not. No studies examined integration/biculturalism and only one study examined the relationship between thin-ideal internalization and separation/marginalization, making summative conclusions on these aspects of acculturation impossible.
Thin-Ideal Internalization, Acculturation and Eating Pathology in Men
As shown in Table 2, all of the studies that measured acculturative stress, thin-ideal internalization and eating pathology found a positive relationship (ie, three of three). Of the four studies that examined assimilation, two found positive relationships and two found non-significant results. No studies examined integration/biculturalism, and only one study examined the relationship between thin-ideal internalization and separation/marginalization, making summative conclusions on these aspects of acculturation impossible.
Discussion
This was the first known review of research examining the relationships among thin-ideal internalization, acculturation, and eating pathology among ethnic/racial minority women and men in the US. This review attempted to fill the gap in the literature identified by numerous previous reviews calling for more culturally-informed and acculturation-focused research on disordered eating etiology that examines how Eurocentric, Western values of appearance interact with the acculturation process.15,39–48
Primary Study Findings
Perhaps the largest take-home message from this study is that research on the relationship between acculturation and thin-ideal internalization in ethnic/racial minorities in the US is mixed and methodologically challenged. In particular, measurement of acculturation made comparisons with meaningful conclusions very challenging. For example, in the 15 studies identified that met inclusion criteria for this review, nine different quantitative measures of acculturation and one qualitative analysis were used. Of the quantitative measures, nine studies used culture-specific measures designed for a given ethnic or cultural group; four studies used transcultural measures designed for participants moving from any cultural context; and one used language spoken at home as a proxy. Furthermore, among the culture-specific measures used in this review, one assessed unique cultural attributes, non-transferable to other cultures (eg, filial piety; family recognition through achievement; ie, Asian Values Scale74) and the remaining culture-specific measures assessed transcultural attributes (eg, ARSMA-II:70 “My friends, while I was growing up, were of Mexican origin”).
To further complicate matters, almost all studies in this review used unidimensional measures of acculturation (eg, Suinn-Lew Asian Self-Identity Acculturation Scale72) that assessed assimilation to US culture rather than integration of both US and minority cultures (ie, biculturalism) or a more complex assessment of the acculturation process (eg, acculturative stress). Specifically, of the 12 studies that examined assimilation in this review using male or female samples, five studies found positive relationships and seven found non-significant results. Given that most existing research on acculturation and eating pathology focuses on assimilation, existing research may not be capturing aspects of acculturation that are particularly salient to thin-ideal internalization. For example, research suggests that biculturalism tends to be associated with mental health well-being among US minority individuals, such as a positive correlation with self-esteem84 and negative correlation with depression symptoms.85 Given these methodological challenges, it is unsurprising that research on thin-ideal internalization, eating pathology, and acculturation is so mixed and inconclusive.
Despite the overall inconclusive findings, the clearest empirical finding that emerged from this review is that acculturative stress was positively correlated with thin-ideal internalization and eating pathology in four of the five studies that measured it. For example, in a sample of 399 Latino college men and women, Menon and Harter (2012)51 found that acculturative stress was significantly positively correlated with body image disturbance after controlling for BMI, age, and gender; and, thin-ideal internalization mediated the relationship between acculturative stress and body image disturbance. Similarly, Liao et al56 described links between acculturative stress and athletic-ideal internalization, such as participants’ resignation of the “dream” of an athletic/Western physique, because they are Asian men. As such, researchers examining both male and female samples should include acculturative stress in their conceptualization of acculturation and its relationship to eating pathology.
Areas for Future Research
Specific recommendations for future research as suggested from these data are summarized in Table 3. In this review and as noted by other authors,40,46 analysis of extant acculturation research is made difficult by the lack of a gold-standard, multi-dimensional acculturation measure. Ideally, such a measure would include both culture-specific and transcultural aspects of the acculturation process and experience that are relevant to eating pathology and mental health outcomes. On one hand, measurement of acculturation should extend beyond language fluency, generational status and identification to examine culture-specific attributes relevant to identity (eg, cultural rites of passage, authoritarian vs egalitarian familial attitudes, gender roles). For example, the TRIOS scale of African American and Afro-Caribbean cultures87 measures five domains: Time, Rhythm, Improvisation, Orality, and Spirituality. These are key cultural features that are particularly salient to this cultural group, and that are not interchangeable with other cultural groups.87 Furthermore, a diminished reliance on language fluency as a proxy for acculturation allows for accurate measurement in cultures whose language was systematically erased by colonization (eg, Alaskan Natives). Similarly, the diminished reliance on generational status as a proxy for acculturation allows for more accurate measurement in cultures with high generational status but low assimilation into US culture (eg, Amish Americans). On the other hand, development of a gold-standard transcultural acculturation scale that captures aspects of the acculturation process (eg, acculturative stress) that are relevant to ethnic minority individuals from many backgrounds is also important. Such a measure would allow for empirical cross-cultural comparisons, enhancing the field’s understanding of cross-cultural differences in etiology and treatment of disordered eating.
 |
Table 3 Recommendations for Future Research on Acculturation and Thin-Ideal Internalization |
Until such a measure exists, future research should aim to measure not only assimilation but also other aspects of acculturation including integration and marginalization. For example, using a sample of 211 Mexican and Mexican American college women, Poloskov and Tracey (2013)61 found that thin-ideal internalization was significantly positively correlated with affiliation to White American culture and significantly negatively correlated with attachment to Mexican culture (as measured by the ARSMA-II Anglo Orientation Scale (0.21) and Mexican Orientation Scale (−0.39)). Furthermore, thin-ideal internalization was a significant mediator between dominant US orientation and body dissatisfaction. In addition, Reddy and Crowther (2007)18 was the only known study to both use a multi-dimensional, cross-cultural measure of acculturation (ie, the CVCS71), allowing for an assessment of integration/biculturalism (or, rather the lack of integration) in South Asian American women. These articles serve as good examples of how one can include various types of acculturation (eg, assimilation, integration, cultural conflict) as well as integrate culture-specific and transcultural aspects of the acculturation process into research.
Future research in this area should also continue to examine the role of acculturative stress as it relates to thin-ideal internalization and eating pathology. This review suggests that stress related to cultural adjustment and perceived conflict in ideals and values appears to be associated with increased thin-ideal internalization and eating pathology. As such, assessing for acculturative stress as well as other aspects of internalization of Western values and ideals of appearance, such as athletic-ideal internalization, is warranted. Examining these relationships across the lifespan (ie, from youth to older adulthood) and generations will be important to understand the interaction between acculturation of mainstream US values and ideals of appearance, stress related to the process of acculturation, and eating pathology.
Conclusion
This review of the literature on acculturation and thin-ideal internalization yielded a small and conflicting body of work. The findings are particularly inconclusive, due to the heterogeneity of acculturation measures, as well as the predominant focus on assimilation, rather than integration/biculturalism. One consistent finding was the positive association between thin-ideal internalization and acculturative stress, for both women and men. Future directions include the development of a gold-standard, multi-dimensional measure of acculturation, as well as the examination of acculturation and thin-ideal internalization in groups other than Latinx and Asian Americans.
Acknowledgments
We thank all research participants and researchers with continued devotion to understanding the acculturation process and its relationship to eating pathology over time.
Disclosure
The authors report no conflicts of interest in this work.
References
1. Llorente E, Gleaves DH, Warren CS, Pérez-de-Eulate L, Rakhkovskaya LM. Translation and validation of a Spanish version of the sociocultural attitudes towards appearance questionnaire-4 (SATAQ-4). Int J Eat Disord. 2014;48(2). doi:10.1002/eat.22263
2. Scharrer E. 15 Representations of Gender in the Media. In: Dill KE, editor. Oxford Handbook Media Psychology. 2013;267–273.
3. Culbert KM, Racine SE, Klump KL. Research review: what we have learned about the causes of eating disorders – a synthesis of sociocultural, psychological, and biological research. J Child Psychol Psychiatry. 2015;56(11):1141–1164. doi:10.1111/jcpp.12441
4. Keel PK, Forney KJ. Psychosocial risk factors for eating disorders. Int J Eat Disord. 2013;46(5):433–439. doi:10.1002/eat.22094
5. Ricciardelli LA, McCabe MP, Williams RJ, Thompson JK. The role of ethnicity and culture in body image and disordered eating among males. Clin Psychol Rev. 2007;27(5):582–606. doi:10.1016/j.cpr.2007.01.016
6. Douglas VJ, Kwan MY, Minnich AM, Gordon KH. The interaction of sociocultural attitudes and gender on disordered eating. J Clin Psychol. 2019;75:2140–2146. doi:10.1002/jclp.22835
7. Warren CS, Gleaves DH, Cepeda-Benito A, Fernandez MDC, Rodriguez-Ruiz S. Ethnicity as a protective factor against internalization of a thin ideal and body dissatisfaction. Int J Eat Disord. 2005;37(3):241–249. doi:10.1002/eat.20102
8. Racine SE, VanHuysse JL, Keel PK, et al. Eating disorder-specific risk factors moderate the relationship between negative urgency and binge eating: a behavioral genetic investigation. J Abnorm Psychol. 2017;126(5):481–494. doi:10.1037/abn0000204
9. Stice E, Gau JM, Rohde P, Shaw H. Risk factors that predict future onset of each DSM–5 eating disorder: predictive specificity in high-risk adolescent females. J Abnorm Psychol. 2017;126(1):38–51. doi:10.1037/abn0000219
10. Rodgers RF, McLean SA, Marques M, Dunstan CJ, Paxton SJ. Trajectories of body dissatisfaction and dietary restriction in early adolescent girls: a latent class growth analysis. J Youth Adolesc. 2016;45(8):1664–1677. doi:10.1007/s10964-015-0356-3
11. Clark L, Tiggemann M. Appearance culture in nine- to 12-year-old girls: media and peer influences on body dissatisfaction. Soc Dev. 2006;15(4):628–643. doi:10.1111/j.1467-9507.2006.00361.x
12. Keery H, Boutelle K, van den Berg P, Thompson JK. The impact of appearance-related teasing by family members. J Adolesc Heal. 2005;37(2):120–127. doi:10.1016/J.JADOHEALTH.2004.08.015
13. Thompson JK, Stice E. Thin-ideal internalization: mounting evidence for a new risk factor for body-image disturbance and eating pathology. Curr Dir Psychol Sci. 2001;10(5):181–183. doi:10.1111/1467-8721.00144
14. Shroff H, Thompson JK. The tripartite influence model of body image and eating disturbance: a replication with adolescent girls. Body Image. 2006;3(1):17–23. doi:10.1016/j.bodyim.2005.10.004
15. Cheng ZH, Perko VL, Fuller-Marashi L, Gau JM, Stice E. Ethnic differences in eating disorder prevalence, risk factors, and predictive effects of risk factors among young women. Eat Behav. 2019;32:23–30. doi:10.1016/J.EATBEH.2018.11.004
16. Soh NL-W, Walter G. Publications on cross-cultural aspects of eating disorders. J Eat Disord. 2013;1(1):4. doi:10.1186/2050-2974-1-4
17. Eriksen TH. Ethnicity and Nationalism: Anthropological Perspectives.
18. Reddy SD, Crowther JH. Teasing, acculturation, and cultural conflict: psychosocial correlates of body image and eating attitudes among South Asian women. Cultur Divers Ethnic Minor Psychol. 2007;13(1):45–53. doi:10.1037/1099-9809.13.1.45
19. Overstreet NM, Quinn DM, Agocha VB. Beyond thinness: the influence of a curvaceous body ideal on body dissatisfaction in black and white women. Sex Roles. 2010;63(1–2):91–103. doi:10.1007/s11199-010-9792-4
20. Berry JW, Phinney JS, Sam DL, Vedder P. Immigrant youth: acculturation, identity, and adaptation. Appl Psychol. 2006;55(3):303–332. doi:10.1111/j.1464-0597.2006.00256.x
21. Berry JW. Acculturation: living successfully in two cultures. Int J Intercult Relations. 2005;29(6):697–712. doi:10.1016/j.ijintrel.2005.07.013
22. Oh Y, Koeske GF, Sales E. Acculturation, stress, and depressive symptoms among Korean immigrants in the United States. J Soc Psychol. 2002;142(4):511–526. doi:10.1080/00224540209603915
23. Krishnan A, Berry JW. Acculturative stress and acculturation attitudes among Indian immigrants to the United States. Psychol Dev Soc. 1992;4(2):187–212. doi:10.1177/097133369200400206
24. Berry JW. Acculturative stress. In: Wong PTP, Wong LCJ, editors. Handbook of Multicultural Perspectives on Stress and Coping. International and Cultural Psychology. Boston, MA: Springer US; 2006. doi:10.1007/b137168.
25. Hovey JD. Acculturative stress, depression, and suicidal ideation in Mexican immigrants. Cultur Divers Ethnic Minor Psychol. 2000;6(2):134–151. doi:10.1037//1099-9809.6.2.134
26. Hovey JD, Magaña C. Acculturative stress, anxiety, and depression among Mexican immigrant farmworkers in the Midwest United States. J Immigr Health. 2000;2(3):119–131. doi:10.1023/A:1009556802759
27. Olivardia R, Pope HG, Mangweth B, Hudson JI. Eating disorders in college men. Am J Psychiatry. 1995;152(9):1279–1285. doi:10.1176/ajp.152.9.1279
28. Dakanalis A, Carrà G, Calogero R, et al. The developmental effects of media-ideal internalization and self-objectification processes on adolescents’ negative body-feelings, dietary restraint, and binge eating. Eur Child Adolesc Psychiatry. 2015;24(8):997–1010. doi:10.1007/s00787-014-0649-1
29. Blond A. Impacts of exposure to images of ideal bodies on male body dissatisfaction: A review. Body Image. 2008;5(3):244–250. doi:10.1016/J.BODYIM.2008.02.003
30. Thompson JK, Cafri G. The Muscular Ideal: Psychological, Social, and Medical Perspectives. Washington, DC, USA: American Psychological Association; 2007. doi:10.1037/11581-000
31. Schaefer LM, Thompson JK, Heinberg LJ, et al. Validation of the Sociocultural Attitudes Towards Appearance Questionnaire-4 (SATAQ-4) in Italian, British, and Australian Women.
32. Marais DL, Wassenaar DR, Kramers AL. Acculturation and eating disorder symptomatology in Black men and women. Eat Weight Disord - Stud Anorexia, Bulim Obes. 2003;8(1):44–54. doi:10.1007/BF03324988
33. White EK, Mooney J, Warren CS. Ethnicity, eating pathology, drive for muscularity, and muscle dysmorphia in college men: a descriptive study. Eat Disord. 2019;27(2):137–151. doi:10.1080/10640266.2019.1585717
34. Flegal KM, Carroll MD, Ogden CL, Curtin LR. Prevalence and trends in obesity among US adults, 1999–2008. JAMA. 2010;303(3):235. doi:10.1001/jama.2009.2014
35. Brewis A, SturtzSreetharan C, Wutich A. Obesity stigma as a globalizing health challenge. Global Health. 2018;14(1):20. doi:10.1186/s12992-018-0337-x
36. Puhl RM, Heuer CA. The Stigma of obesity: a review and update. Obesity. 2009;17(5):941–964. doi:10.1038/oby.2008.636
37. Nicdao E, Hong S, Takeuchi DT. Prevalence and correlates of eating disorders among Asian Americans: results from the national Latino and Asian American study. Int J Eat Disord. 2007;40(3):22–26. doi:10.1002/eat.20450
38. Ayala GX, Mickens L, Galindo P, Elder JP. Acculturation and body image perception among latino youth. Ethn Health. 2007;12(1):21–41. doi:10.1080/13557850600824294
39. Halliwell E. Future directions for positive body image research. Body Image. 2015;14:177. doi:10.1016/j.bodyim.2015.03.003
40. Shekriladze I, Tchanturia K. Acculturation to Western culture in the context of eating disorders ia. 2017.
41. Stice E, Becker CB, Yokum S. Eating disorder prevention: current evidence-base and future directions. Int J Eat Disord. 2013;46(5):478–485. doi:10.1002/eat.22105
42. Stice E, South K, Shaw H. Future directions in etiologic, prevention, and treatment research for eating disorders. J Clin Child Adolesc Psychol. 2012;41(6):845–855. doi:10.1080/15374416.2012.728156
43. Levine MP, Smolak L. Prevention of negative body image, disordered eating, and eating disorders: an update. Radcliffe Publishing; 2018:1–14.
44. Levine MP, Smolak L. Prevention of negative body image, disordered eating, and eating disorders: an update; 2007. Annual Review of Eating Disorders. Radcliffe Publishing, UK; 2007:1–13.
45. Bardone-Cone AM, Hunt RA, Watson HJ. An overview of conceptualizations of eating disorder recovery, recent findings, and future directions. Curr Psychiatry Rep. 2018;20(9):79. doi:10.1007/s11920-018-0932-9
46. Doris E, Shekriladze I, Javakhishvili N, Jones R, Treasure J, Tchanturia K. Is cultural change associated with eating disorders? A systematic review of the literature. Eat Weight Disord - Stud Anorexia, Bulim Obes. 2015;20(2):149–160. doi:10.1007/s40519-015-0189-9
47. Keel PK, Gravener JA. Sociological influences on eating disorders. Annu Rev Eating Disord Part 2. 2008:43–57.
48. Paxton SJ, Heinicke BE. Body Image. Annu Rev Eating Disord Part 2. 2008;69–83.
49. Trevelyan E, Gambino C, Gryn T, et al. Characteristics of the U.S. Population by Generational Status. US Dept of Commerce, Econ and Stat Admin, US Census Bureau. Washington, DC; 2016.
50. Moher D, Liberati A, Tetzlaff J, Altman DG, The PRISMA Group (2009) Preferred Reporting Items for Systematic Reviews and Meta-Analyses: The PRISMA Statement. PLoS Med 6(7): e1000097. doi:10.1371/journal.pmed.1000097
51. Menon C V, Harter SL. Examining the impact of acculturative stress on body image disturbance among Hispanic college students. Cultur Divers Ethnic Minor Psychol. 2012;18(3):239–246. doi:10.1037/a0028638
52. Blow JA, Taylor T, Cooper TV, Redfearn CK. Correlates of weight concern and control in a Hispanic college student sample. Eat Behav. 2010;11(1):6–10. doi:10.1016/j.eatbeh.2009.08.001
53. Gordon KH, Castro Y, Sitnikov L, Holm-Denoma JM. Cultural body shape ideals and eating disorder symptoms among White, Latina, and Black college women. Cultur Divers Ethnic Minor Psychol. 2010;16(2):135–143. doi:10.1037/a0018671
54. Liao Y, Knoesen NP, Deng Y, et al. Body dysmorphic disorder, social anxiety and depressive symptoms in Chinese medical students. Soc Psychiatry Psychiatr Epidemiol. 2010;45(10):963–971. doi:10.1007/s00127-009-0139-9
55. Franko DL, Coen EJ, Roehrig JP, et al. Considering J.Lo and Ugly Betty: a qualitative examination of risk factors and prevention targets for body dissatisfaction, eating disorders, and obesity in young Latina women. Body Image. 2012;9(3):381–387. doi:10.1016/j.bodyim.2012.04.003
56. Liao KY-H, Shen FC, Cox AR, Miller AR, Sievers B, Werner B. Asian American men’s body image concerns: a focus group study. Psychol Men Masculinities. 2019. doi:10.1037/men0000234
57. Heinberg LJ, Thompson JK, Stormer S. Development and validation of the sociocultural attitudes towards appearance questionnaire. Int J Eat Disord. 1995;17(1):81–89. doi:10.1002/1098-108X(199501)17:13.0.CO;2-Y
58. Cusumano DL, Thompson JK. Body image and body shape ideals in magazines: exposure, awareness, and internalization. Sex Roles. 1997;37(9–10):701–721. doi:10.1007/BF02936336
59. Thompson JK, van den Berg P, Roehrig M, Guarda AS, Heinberg LJ. The sociocultural attitudes towards appearance scale-3 (SATAQ-3): development and validation. Int J Eat Disord. 2004;35(3):293–304. doi:10.1002/eat.10257
60. Stice E, Agras WS. Predicting onset and cessation of bulimic behaviors during adolescence: a longitudinal grouping analysis. Behav Ther. 1998;29(2):257–276. doi:10.1016/S0005-7894(98)80006-3
61. Poloskov E, Tracey TJG. Internalization of U.S. female beauty standards as a mediator of the relationship between Mexican American women’s acculturation and body dissatisfaction. Body Image. 2013;10:501–508. doi:10.1016/j.bodyim.2013.05.005
62. Garner DM, Olmsted MP, Bohr Y, Garfinkel PE. The Eating Attitudes Test: psychometric features and clinical correlates. Psychol Med. 2009;12(04):871. doi:10.1017/S0033291700049163
63. Schoemaker C, van Strien T, van der Staak C. Validation of the eating disorders inventory in a nonclinical population using transformed and untransformed responses. Int J Eat Disord. 2010;15(4):387–393. doi:10.1002/eat.2260150409
64. Mendelson BK, Mendelson MJ, White DR. Body-esteem scale for adolescents and adults. J Pers Assess. 2001;76(1):90–106. doi:10.1207/S15327752JPA7601_6
65. Cash TF. Multidimensional Body–Self Relations Questionnaire (MBSRQ). In: Encyclopedia of Feeding and Eating Disorders. Singapore: Springer Singapore; 2015:1–4. doi:10.1007/978-981-287-087-2_3-1
66. McCreary DR. The drive for muscularity scale: description, psychometrics, and research findings. In Thompson J, Cafri G, editors. The Muscular Ideal: Psychological, Social, and Medical Perspectives. Washington: American Psychological Association; 2007:87–106. doi:10.1037/11581-004
67. Mayville SB, Williamson DA, White MA, Netemeyer RG, Drab DL. Development of the muscle appearance satisfaction scale: a self-report measure for the assessment of muscle dysmorphia symptoms. Assessment. 2002;9(4):351–360. doi:10.1177/1073191102238156
68. Petrie TA, Tripp MM, Harvey P. Factorial and construct validity of the body parts satisfaction scale-revised: an examination of minority and nonminority women. Psychol Women Q. 2002;26(3):213–221. doi:10.1111/1471-6402.00060
69. Thompson JK, Heinberg LJ, Altabe M, Tantleff-Dunn S. Exacting Beauty: Theory, Assessment, and Treatment of Body Image Disturbance. Vol. 396. American Psychological Association; 1999. doi:10.1037/10312-000
70. Cuellar I, Arnold B, Maldonado R. Acculturation rating scale for Mexican Americans-II: a revision of the original ARSMA scale. Hisp J Behav Sci. 1995;17(3):275–304. doi:10.1177/07399863950173001
71. Inman AG, Ladany N, Constantine MG, Morano CK. Development and preliminary validation of the cultural values conflict scale for South Asian women. J Couns Psychol. 2001;48(1):17–27. doi:10.1037/0022-0167.48.1.17
72. Suinn RM, Rickard-Figueroa K, Lew S, Vigil P. The suinn-lew Asian self-identity acculturation scale: an initial report. Educ Psychol Meas. 1987;47(2):401–407. doi:10.1177/0013164487472012
73. Marin G, Sabogal F, Marin BV, Otero-Sabogal R, Perez-Stable EJ. Development of a short acculturation scale for hispanics. Hisp J Behav Sci. 1987;9(2):183–205. doi:10.1177/07399863870092005
74. Kim BSK, Atkinson DR, Yang PH. The Asian values scale: development, factor analysis, validation, and reliability. J Couns Psychol. 1999;46(3):342–352. doi:10.1037/0022-0167.46.3.342
75. Miller MJ, Kim J, Benet-Martínez V. Validating the riverside acculturation stress inventory with Asian Americans. Psychol Assess. 2011;23(2):300–310. doi:10.1037/a0021589
76. Testa S, Doucerain MM, Miglietta A, Jurcik T, Ryder AG, Gattino S. The Vancouver Index of Acculturation (VIA): new evidence on dimensionality and measurement invariance across two cultural settings. Int J Intercult Relations. 2019;71:60–71. doi:10.1016/J.IJINTREL.2019.04.001
77. Sodowsky GR, Plake BS. Psychometric properties of the American-International Relations Scale. Educ Psychol Meas. 1991;51(1):207–216. doi:10.1177/0013164491511020
78. Stephenson M. Development and validation of the Stephenson Multigroup Acculturation Scale (SMAS). Psychol Assess. 2000;12(1):77–88. doi:10.1037/1040-3590.12.1.77
79. Nouri M, Hill LG, Orrell-Valente JK. Media exposure, internalization of the thin ideal, and body dissatisfaction: comparing Asian American and European American college females. Body Image. 2011;8(4):366–372. doi:10.1016/j.bodyim.2011.05.008
80. Cheng H-L, Mcdermott R, Wong YJ. Drive for muscularity in Asian American Men: sociocultural and racial/ethnic factors as correlates. Psychol Men Masculinity. 2015. doi:10.1037/men0000019
81. Cooper, PJ, Taylor MJ, Cooper Z, Fairburn CG. The development and validation of the Body Shape Questionnaire. International Journal of Eating Disorders. 1987;6(4):485-494.
82. Lau ASM, Lum SK, Chronister KM, Forrest L. Asian American college women’s body image: a pilot study. Cultur Divers Ethnic Minor Psychol. 2006;12(2):259–274. doi:10.1037/1099-9809.12.2.259
83. Warren CS, Castillo LG, Gleaves DH. The sociocultural model of eating disorders in Mexican American women: behavioral acculturation and cognitive marginalization as moderators. Eat Disord. 2010;18(1):43–57. doi:10.1080/10640260903439532
84. Cho H
85. Tobin J, Miller KA, Baezconde-Garbanati L, Unger JB, Hamilton AS, Milam JE. Acculturation, mental health, and quality of life among hispanic childhood cancer survivors: a latent class analysis. Ethn Dis. 2018;28(1):55–60. doi:10.18865/ed.28.1.55
86. Stark-Wroblewski K, Yanico BJ, Lupe S. Acculturation, internalization of Western appearance norms, and eating pathology among Japanese and Chinese international student women. Psychol Women Q. 2005;29(1):38-46. doi:10.1111/j.1471-6402.2005.00166.x
87. Jones JM. TRIOS: a Psychological Theory of the African Legacy in American Culture. J Soc Issues. 2003;59(1):217–242. doi:10.1111/1540-4560.t01-1-00014
88. Warren CS, Rios RM. The relationships among acculturation, acculturative stress, endorsement of Western media, social comparison, and body image in Hispanic male college students. Psychol Men Masc. 2012;14(2):192–201. doi:10.1037/a0028505
89. Benet-Martínez V, Haritatos J. Bicultural Identity Integration (BII): components and psychosocial antecedents. J Pers. 2005;73(4):1015–1049. doi:10.1111/j.1467-6494.2005.00337.
90. Lester R, Petrie TA. Personality and physical correlates of bulimic symptomatology among Mexican American female college students. J Couns Psychol. 1995;4(2):199–203. doi:10.1037/0022-0167.42.2.199.
91. Yoshimura T. Acculturative and sociocultural influences on the development of eating disorders in Asian-American females.. Eat Disord. 2005;3(3):216–228. doi:10.1080/10640269508249165.
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
