Back to Journals » Drug Design, Development and Therapy » Volume 15
Effects of Sugammadex versus Neostigmine on Intraoperative Coagulation Profiles in Patients with Thyroidectomy
Authors Zhao D, Fang J , Xiong W, Lin J, Chen W, Wu C
Received 27 October 2020
Accepted for publication 13 January 2021
Published 25 February 2021 Volume 2021:15 Pages 829—834
DOI https://doi.org/10.2147/DDDT.S286803
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Professor Anastasios Lymperopoulos
Dizhou Zhao, Jieyu Fang, Wei Xiong, Jun Lin, Wanmei Chen, Chujun Wu
Department of Anesthesia, The First Affiliated Hospital of Sun Yat-Sen University, Guangzhou, People’s Republic of China
Correspondence: Jieyu Fang
Department of Anesthesia, The First Affiliated Hospital of Sun Yat-Sen University, No. 56 Zhongshan Road II, Guangzhou, People’s Republic of China
Tel + 86-13660121136
Email [email protected]
Background: Sugammadex has been a revolutionary reversal of neuromuscular blockade. It is known to be highly efficient. However, a change in the coagulation profile is one of the most dangerous potential complications which is a concern for both surgeon and anesthetist. Bleeding may cause hypovolemic shock, hematoma, and so on. To investigate the effects of sugammadex on coagulation profiles in patients with thyroidectomy, we compared patients that were treated with either sugammadex or neostigmine.
Patients and Methods: Eighty patients with thyroid neoplasms undergoing thyroidectomy were randomly allocated to sugammadex group (group S) or neostigmine group (group N). Induction of anesthesia was preformed using propofol, sufentanil, and rocuronium. Group S received sugammadex 2.0mg/kg after trachea intubation, similarly Group N received neostigmine 40 μg/kg, for reversal of rocuronium-induced neuromuscular blockade. The intraoperative coagulation profiles were monitored after the rocuronium injection (T0), 10 minutes after reversal (T1) and 30 minutes after reversal (T2) by testing activated partial thromboplastin time (APTT), prothrombin time (PT), fibrinogen (FIB), thrombin time (TT), and TEG-Haemonetics. Amount of bleeding was recorded during perioperative period.
Results: There was no significant difference in the thromboelastogram, APTT, PT, FIB, or TT measurements at each time point in Group N. The reaction time (R time) and kinetics time (K time) of Group S in T1 were significantly longer than the corresponding times at T0 and T2, and the R times were significantly longer than those in Group N at the same time points (P< 0.05). Additionally, in Group S, the APTT was prolonged in T1 and returned to normal in T2.
Conclusion: The result showed that sugammadex provided transient efficacy in prolonging the coagulation parameters, while neostigmine did not change the coagulation profile.
Keywords: sugammadex, neostigmine, TEG-Haemonetics, coagulation, thyroidectomy
Introduction
Maintaining a neuromuscular blockade is an important part of general anesthesia for the purpose of providing clear surgical field, ensuring endotracheal intubation or facilitating other surgical operations.1,2 Nowadays, some operations require a change in the level of intraoperative neuromuscular blockade; that is to say, it might be essential to reverse the neuromuscular blockade rapidly.3 In the past, an anti-cholinesterase drug, neostigmine, was chosen to achieve the reversal, even though it could lead to complications, and the speed of reversal was unsatisfactory.4 Complications related to neostigmine include increasing gland secretion, decreasing heart rate, and so on. Recently, sugammadex has achieved a revolution in neuromuscular blockade reversal. Sugammadex is known to have a rapid onset, and it is highly efficient. Currently, the use of sugammadex has increased.
In thyroidectomy, the electromyographic signal endotracheal tube (EMG Endotracheal Tube) has become popular, since it assists surgeons in locating the recurrent laryngeal nerve and then avoiding nervous damage by mistake.5 Applying sugammadex after anesthesia induction reverses muscle relaxant quickly, which ensures the effect of the EMG Endotracheal Tube.6 Nevertheless, a previous in vitro study reported that sugammadex might be associated with moderate hypocoagulation in whole blood of healthy subjects.7 Perioperative bleeding is one of the most dangerous complications in patients undergoing a thyroidectomy; thus, it is a serious concern for surgeons and anesthetists. Postoperative bleeding may cause dyspnea by obstruction of airway. Therefore, in the present study sugammadex or neostigmine was applied to patients to investigate the effects of sugammadex on coagulation profiles in patients undergoing a thyroidectomy. We aimed to use qLabs Electrometer (to test activated partial thromboplastin time [APTT], prothrombin time [PT], fibrinogen [FIB], and thrombin time [TT]) and TEG-Haemonetics to assess the real-time coagulation profiles change from the patients.
Methods
Our experimental protocol which was conducted in accordance with the Declaration of Helsinki was approved by Ethics Committee of the First Affiliated Hospital of Sun yat-sen University (number: [2019]153), and it was registered in China clinical trial registry (number: ChiCTR2000030083). All of the patients signed informed consent. Study inclusion criteria were: 1) patients with American Society of Anesthesiologists (ASA) physical status ASA Ⅰ to ASA Ⅱ; 2) age 18–65 years; and 3) scheduled for thyroidectomy. Study exclusion criteria were: patients with cardiac disease, hepatic failure, distant metastasis of a malignant tumor, and allergy to the test drugs. Eighty patients were included in the study.
For anesthesia induction, both groups of patients were administered propofol by target-controlled infusion of 4.0 µg/mL, sufentanil 0.5µg/kg iv, and rocuronium 0.6 mg/kg iv. After tracheal intubation, anesthesia was maintained with propofol target-controlled infusion of 2.0 ng/mL and remifentanil target-controlled infusion as 5.0 ng/mL. The time at which we administered rocuronium for the neuromuscular blockade was defined as T0.
Patients in the Group S received sugammadex 2.0mg/kg for reversal of rocuronium-induced neuromuscular blockade. The time 10 minutes and 30 minutes after the reversal were defined as T1 and T2. The Group N received neostigmine 40ug/kg for the reversal. Heart rate, blood pressure, and oxygen saturation (pulse oximeter) were monitored. If the heart rate declined to less than 50 beats per minute, a dose of 0.3 mg atropine was administered.
We collected 3 mL of peripheral venous blood sample from each patient at T0 and at 10 min (T1) and 30 min (T2) after the reversal. QLabs Electrometer (Micropoint Biotechnologies, Guangdong, China) was used to test the samples for four coagulation items including prothrombin time (PT), activated partial thromboplastin time (aPTT), Thrombin time (TT), and fibrinogen (FIB) and TEG-Haemonetics (thromboelastograph coagulation analyzer Model 5000, Haemoscope corporation, Boston, MA, USA) was used to test the other bleed samples for Reaction time (R time), the kinetics time (K time), α angle, and maximum amplitude (MA). 20µg CaCl2 and the test reagent were mixed with the blood samples in the the TEG-Haemonetics cup. After 30 minutes we received the TEG items values.
The amount of blood loss of surgery was recorded. The episodes of bradycardia were recorded. The tracheal tube was extubated when the patient woke up after the surgery.
Statistical Analysis
Statistical analysis was performed with SPSS 19.0 for Windows (IBM Corporation, Armonk, NY, USA). Continuous variables were presented as mean ± standard deviation (SD), and categorical variables were presented as frequency. Serial changes in coagulation profiles were analyzed with a repeated measures analysis of variance. Pairwise difference in coagulation profiles were analyzed with LSD-t-test. P-values <0.05 were considered to be statistically significant.
Results
In this study, 80 patients undergoing a thyroidectomy had been enrolled. Baseline characteristics are presented in Table 1. There was no significant difference in age, sex, body weight, or other general characteristics between the two groups (Table 1).
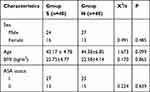 |
Table 1 Baseline Characteristics of Two Groups |
Coagulation Items
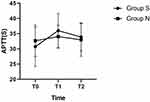
There was no statistically significant difference in the APTT, PT, TT, or FIB in each time of Group N. The APTT indexes in group S measured at T1 were significantly higher than that measured at T0 and T2. The T1 and T3 values were in the normal range for APTT. However, the APTT in group S at T1 was significantly higher than the R time in group N at the same time, and the results were statistically significant (P<0.05; Table 2, Figure 1).
 |
Table 2 Coagulation Items of Two Groups |
Thromboelastogram Items
There was no statistically significant difference in thromboelastogram indexes in each time of group N. The R time in group S measured at T1 was significantly higher than that measured at T0 and T2. The T1 and T3 values were in the normal range for R times. However, the R time in group S at T1 was significantly higher than the R time in group N at the same time (P<0.05). The K time in group S measured at T1 was significantly higher than that at T0. But the K times in group S at each time point were not significantly different from those in group N. There were no significant differences in the indexes of α angle or the MA in both groups at each time point (Table 3, Figures 2 and 3).
 |
Table 3 Thromboelastogram Items of Two Groups |
Bleeding and Other Adverse Events
There was no significant difference in blood loss between the groups. No postoperative hemorrhage was recorded in either group. During the reversal, 14 patients in group N experienced a decline in heart rate decrease. Among these, 10 patients received atropine 0.3 mg then heart rate increase over 50 beats per minute. The other four patients soon recovered spontaneously. Two patients in group N suffered heart rate decrease and recovered spontaneously.
Discussion
In this study, the effects of sugammadex were compared versus neostigmine on intraoperative coagulation profiles in patients that underwent a thyroidectomy. The results showed that a dose of 2.0 mg/kg sugammadex might prolong the APTT index and the R time, and K time in the thromboelastograph TEG test temporarily. While a dose of neostigmine used to reverse neuromuscular block did not affect the coagulation profile.
Non-depolarizing neuromuscular blocking agents (NMBAs) are widely used in anesthesia induction. Previously, for reversal, neostigmine used to be chosen to weaken the activity of acetylcholinesterase.8 However, application of neostigmine may be limited by the risk that excess acetylcholine might lead to complications, such as a decline in the heart rate and an increase in gland secretion.9
Sugammadex is one of the recent neuromuscular blocking antagonist. Sugammadex is a synthetic γ-cyclodextrin derivative, and the structure includes hydrophilic and lipophilic surfaces on different sides.10,11 This new drug works differently from neostigmine by binding up the NMBAs by the lipophilic inner cavity to compose chelate structure.12 Thus, NMBAs are inactivated. A previous study in vitro showed that sugammadex could prolong the APTT and PT.13
In fact, the effect of coagulation in sugammadex had different results in previous pharmacological research. A study by Carron et al showed that sugammadex produced a slight effect on coagulation in morbidly obese patients, without increasing the risk of postoperative bleeding.14 Additionally, Bosch et al reported that with sugammadex 16 mg/kg in surgical patients, anti-coagulant activity would remain below thresholds observed following treatment with standard anti-coagulant therapy; then, the activity decrease rapidly with declining plasma sugammadex concentrations.15
Patients that undergo a thyroidectomy typically require monitoring of the recurrent laryngeal nerve, which is aimed to make the surgical field clear. The technology of endotracheal tube really reduce the possibility of recurrent laryngeal nerve injury and helps avoid complications;16 thus, anesthetists need to reduce the dose of NMBAs or prepare to reverse neuromuscular block rapidly.17 Because of the special anatomic structure of thyroid, patients that undergo a thyroidectomy are at a higher risk of bleeding than other superficial operations. Meanwhile, acute bleeding probably cause neck hematoma and then lead to tracheal obstruction which lead to deadly dyspnea. Whether sugammadex can influence the coagulation profile, its use in patients undergoing a thyroidectomy remains controversial.
qLabs Electrometer is a machine which is able to detect coagulation items quickly by only a few drops of blood in 3 minutes. It is a point-of-care equipment, which can check coagulation items in operation room. APTT of 40 patients in group S showed a tendency to increase from 30.72±6.19 s to 35.99±5.37 s within 10 minutes; then, it came to 33.80±4.39 s within 30 minutes time after sugammadex administration. Other items did not change. APTT represent the function of the endogenous coagulation system. The prolongation might result from decreasing levels of plasma factor VIII, factor IX, and factor XI.
Furthermore, four coagulation parameters are insufficient to describe the complete coagulation process from platelet aggregation to fibrin clot formation. TEG-Haemonetics is supposed to describe the coagulation process more clearly. It analyzes the function of coagulation factors, fibrin, platelets and other factors in the process of coagulation. Samples in Group S and Group N got a different result in TEG R time and K time. As we know, R time emerge the incubation period before fibrin formation represent the procession of initial coagulation. It relates to the function of plasma factors. K time shows the strength of the fibrin block and it relates to the platelet function.
In this research, both rapid coagulation parameters and the thromboelastography indexes suggested that sugammadex might act on the function of plasma factors and the platelet to prolong coagulation profiles temporarily, which is consistent with previous reports. We assume that the distinctive structure of sugammadex might play a decisive role. When sugammadex binding up the NMBAs, some chelate with moderation effect have been produced. These chelated structures might have work on the plasma coagulation factors and the platelet as well. When the drug is metabolized, this moderation effect disappears, which result in a return of coagulation factors to normal levels. This moderation effect is so slight that it does not increase intraoperative blood loss.
However, this study only focused on the effects of patients with normal coagulation function before operation in a clinical dose of sugammadex. The effects of sugammadex on patients with abnormal coagulation function before operation, especially patients with coagulation dysfunction, needs further study.
Conclusion
In this study, sugammadex is associated with transient efficacy of prolongation of coagulation parameters after administration. The changes of coagulation are so slight that it hardly increases the risk of bleeding. However, the change of coagulation profiles return to normal after about thirty minutes. Furthermore, neostigmine does not change in coagulation profiles.
Abbreviations
APTT, activated partial thromboplastin time; PT, prothrombin time; FIB, fibrinogen; TT, thrombin time; TEG, thromboelastogram; R time, reaction time; K time, kinetics time; EMG, electromyographic; MA, the maximum amplitude; NMBAs, non-depolarizing neuromuscular blocking agents.
Data Sharing Statement
We intend to share all of the participant data on the ResMan public platform (website: http://www.medresman.org.cn/login.aspx). These data are available since October 2020.
Disclosure
There is no competing interest between authors and other individuality and organization.
References
1. Fuchs-Buder T, Schmartz D, Baumann C, et al. Deep neuromuscular blockade improves surgical conditions during gastric bypass surgery for morbid obesity: A randomised controlled trial. Eur J Anaesthesiol. 2019;36:486–493. doi:10.1097/EJA.0000000000000996
2. Kamen V, Vlassakov I, et al. A quest to increase safety of anesthetics by advancements in anesthesia monitoring: scientometric analysis. Drug design. Development Therapy. 2015;9:2599–2608.
3. Kim NY, Koh JC, Lee KY, et al. Influence of reversal of neuromuscular blockade with sugammadex or neostigmine on postoperative quality of recovery following a single bolus dose of rocuronium: A prospective, randomized, double-blinded, controlled study. J Clin Anesth. 2019;57:97–102. doi:10.1016/j.jclinane.2019.02.014
4. Gaver RS, Brenn BR, Gartley A, et al. Retrospective analysis of the safety and efficacy of sugammadex versus neostigmine for the reversal of neuromuscular blockade in children. Anesth Analg. 2019;129(4):1. doi:10.1213/ANE.0000000000004207
5. Moritz A, Schmidt J, Schreiner W, et al. Combined recurrent laryngeal nerve monitoring and one-lung ventilation using the EZ-Blocker and an electromyographic endotracheal tube. J Cardiothorac Surg. 2019;14(1):1–8. doi:10.1186/s13019-019-0927-6
6. Schepens T, Cammu G, Saldien V, et al. Electromyographic activity of the diaphragm during neostigmine or sugammadex-enhanced recovery after neuromuscular blockade with rocuronium: A study in anaesthetised healthy volunteers. Eur J Anaesthesiol. 2015;32(1):010201. doi:10.1097/EJA.0000000000000140
7. Kam PJD, Grobara P, Prohn M, et al. Effects of sugammadex on activated partial thromboplastin time and prothrombin time in healthy subjects. Int J Clin Pharmacol Ther. 2014;52(3):227–236. doi:10.5414/CP201976
8. Bailey J, Wilson M, Akuffo N, et al. Evaluation of sugammadex vs neostigmine in the reversal of neuromuscular blockade. Chest J. 2018;154(4):890. doi:10.1016/j.chest.2018.08.799
9. Kent NB, S S L, Phillips S, et al. Therapeutic doses of neostigmine, depolarising neuromuscular blockade and muscle weakness in awake volunteers: a double-blind, placebo-controlled, randomised volunteer study. Anaesthesia. 2018;73(9):1079–1089. doi:10.1111/anae.14386
10. Nguyen-Lee J, Moreland N, Sadoughi A, et al. Sugammadex: clinical Pharmacokinetics and Pharmacodynamics. Curr Anesthesiol Rep. 2018;4(8):168–177. doi:10.1007/s40140-018-0266-5
11. Welliver M, McDonough J, Kalynych N, Redfern R. Discovery, development, and clinical application of sugammadex sodium, a selective relaxant binding agent. Drug Des Devel Ther. 2009;6(2):49–59.
12. Abad-Gurumeta A. Evidence of residual neuromuscular block with sugammadex vs neostigmine. Br J Anaesth. 2018;120(3):603. doi:10.1016/j.bja.2017.12.020
13. Ok LI, Sung KY, Wone CH, et al. In vitro investigation of the effects of exogenous sugammadex on coagulation in orthopedic surgical patients. BMC Anesthesiol. 2018;18(1):56–62. doi:10.1186/s12871-018-0519-3
14. Carron M, Bertini D, Prandini T, et al. Effect of sugammadex on coagulation as detected by rotational thromboelastometry in morbidly obese patients. Minerva Anestesiol. 2017;84(2):178–188. doi:10.23736/S0375-9393.17.11856-0
15. Rolien B, van Lierop M-J, de Kam P-J. A PK-PD model-based assessment of sugammadex effects on coagulation parameters. European J Pharmaceutical Sci. 2016;84:9–17. doi:10.1016/j.ejps.2015.12.028
16. Calò PG, Medas F, Conzo G, et al. Intraoperative neuromonitoring in thyroid surgery: is the two-staged thyroidectomy justified? Int J Surg. 2017;41(Suppl 1):
17. Chen HK, Chen CL, Wen KS, et al. Application of transoral continuous intraoperative neuromonitoring in natural orifice transluminal endoscopic surgery for thyroid disease: a preliminary study. Surg Endosc. 2018;32(1):517–525. doi:10.1007/s00464-017-5656-0
 © 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2021 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.