Back to Journals » Journal of Blood Medicine » Volume 11
Effects of Alpha-Lipoic Acid Supplementation on Cardiovascular Disease Risk Factors in β-Thalassemia Major Patients: A Clinical Trial Crossover Study
Authors Jamshidi K, Abdollahzad H , Nachvak M, Rezaei M , Golpayegani MR, Sharifi Zahabi E
Received 2 March 2020
Accepted for publication 22 April 2020
Published 7 May 2020 Volume 2020:11 Pages 131—139
DOI https://doi.org/10.2147/JBM.S252105
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 2
Editor who approved publication: Dr Martin H Bluth
Khadijeh Jamshidi,1 Hadi Abdollahzad,2 Mostafa Nachvak,2 Mansour Rezaei,3 Mohammad Reza Golpayegani,4 Elham Sharifi Zahabi5
1The Student Research Committee, School of Nutritional Sciences and Food Technology, Kermanshah University of Medical Sciences, Kermanshah, Iran; 2Nutritional Sciences Department, School of Nutritional Sciences and Food Technology, Kermanshah University of Medical Sciences, Kermanshah, Iran; 3Department of Biostatistics and Epidemiology, School of Health, Kermanshah University of Medical Sciences, Kermanshah, Iran; 4Department of Pediatrics, School of Medicine, Kermanshah University of Medical Sciences, Kermanshah, Iran; 5Imam Khomeini Comprehensive Health Services Center, Kermanshah University of Medical Sciences, Kermanshah, Iran
Correspondence: Hadi Abdollahzad
Research Center for Environmental Determinants of Health, Health Institute, Kermanshah University of Medical Sciences, Kermanshah, Iran
Tel +98 83 3710 2008
Email [email protected]
Aim: Thalassemia is one of the most common genetic diseases, and cardiovascular disease (CVD) has been considered as the leading cause of mortality in more than 50% of β-thalassemia patients. The aim of this study was to determine the effects of alpha-lipoic acid (ALA) on CVD risk factors in β-thalassemia major patients.
Methods: Twenty β-thalassemia major patients participated in this randomized crossover clinical trial study. Participants were randomly assigned to ALA (600 mg/day) or placebo groups for two 8-wk interventions that were separated by a 3-wk washout period. The CVD risk factors including serum osteoprotegerin (OPG), homocysteine, lipoprotein-associated phospholipase A2 and trimethylamine N-oxide were measured at the beginning and the end of each intervention phase according to the standard protocol.
Results: Serum OPG reduced significantly in the ALA group in all participants (5.38 ± 2.79 to 3.27 ± 2.43 ng/mL, P= .003) and in the male subgroup (5.24 ± 2.56 to 3.13 ± 2.5 ng/mL, P= .015); this reduction was significant in comparison with the placebo group (P= .013). The changes in other CVD risk factors were not significant.
Conclusion: The results of this study showed that after 8-wk of ALA consumption, the serum OPG reduced significantly in β-thalassemia major patients. Therefore, controlling the serum OPG level with ALA consumption can be an important complementary therapeutic option to prevent the progression of CVD in β-thalassemia major patients.
Keywords: β-thalassemia major, alpha-lipoic acid, CVD risk factors
Introduction
Thalassemia is the most common hereditary diseases in the world, including in Iran. The frequency of disease varies from one region to another, so that the highest prevalence (10%) has been reported on the margins of the Caspian Sea and Persian Gulf, and in other parts of Iran it was 4%–8%. Currently, there are about 22,000 β-thalassemia major patients and more than 2 million carriers in Iran.1
This hereditary hemolytic anemia causes the body not to make the hemoglobin chains. β-Thalassemia major is the severe form of thalassemia, which begins with anemia and continues with apparent deformity, bone problems, weakness, and growth retardation.2 Therefore, in order to compensate for the lack of hemoglobin, an inevitable treatment is the continuous infusion of blood. This causes patients to have extra complications due to increased iron load and accumulation in various organs such as the liver and heart and eventually the risk of premature death.3 So cardiovascular disease (CVD) is one of the major complications of β-thalassemia major that could cause more than half of deaths in patients.4 Despite treatment with deferoxamine (an iron chelator), the most common cause of death in thalassemic patients (63% of all cases) is cardiac dysfunction including limiting pericarditis, heart failure, and arrhythmias.5 CVD is a multifactorial disease with a great number of traditional and modern risk factors such as osteoprotegerin (OPG), homocysteine (HCY), lipoprotein-associated phospholipase A2 (Lp-PLA2), and trimethylamine N-oxide (TMAO) are considered as the new risk factors and various studies have shown that the level of these new risk factors are high in β-thalassemia major patients.6–9
Alpha-lipoic acid (ALA), a potent antioxidant, can be used as an adjunct therapy for many diseases such as diabetes, CVD, neurological damages, autoimmune diseases, cancers, and AIDS.10 In addition to its antioxidant role, ALA has chelating properties for metals such as iron, copper, manganese, and zinc in both in-vitro and in-vivo conditions. Therefore, ALA can be used as an adjunct therapy to chelate iron in β-thalassemia major patients.11
Also, studies have shown that this antioxidant has beneficial effects in reducing serum lipids, inflammatory factors, oxidative stress, and CVD risk factors including HCY, OPG and Lp-PLA2.12–14
We examined the effect of ALA supplementation on traditional CVD risk factors including cholesterol, HDL-C, LDL-C, triglyceride, etc. in another study that is currently under review.
Considering the high prevalence of cardiac dysfunction and premature death, the high level of new risk factors in thalassemic patients, and the lack of specific nutritional interventions regarding new CVD risk factors in these patients, we aimed to evaluate the effects of ALA supplementation on new CVD risk factors including OPG, HCY, Lp-PLA2, and TMAO in β-thalassemia major patients.
Materials and Methods
Participants
According to available files in the Mohammad Kermanshahi Hospital, of 314 β-thalassemia major patients in this hospital, 85 individuals were assessed for eligibility, and 59 did not meet the inclusion criteria. In all, 20 eligible individuals were recruited to this randomized clinical trial (RCT). Furthermore, this number was adequate to cover potential losses during the study period, but we considered 26 individuals who had inclusion criteria (Figure 1).
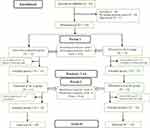 |
Figure 1 Flowchart of study progress. |
Inclusion criteria include age >15 yr; no history of hepatitis B and C, CVDs (include coronary artery disease, heart failure, limiting pericarditis, arrhythmia, myocardial infarction and cardiomyopathy), liver or kidney disease, cancer, allergy and digestive problems, not being pregnant or lactating, being non-smoking, and not adhering to a specific diet. Exclusion criteria included heart failure during the study, pregnancy, non-compliance with the study protocol, and the use of certain drugs (except routine drugs of thalassemic patients) and dissatisfaction with the continuation of the study. Before the start of the study, a questionnaire asking about demographic information, medical history, and medication use was completed. After the overview of the study course was given to the participants, they were asked to provide a written informed consent; for participants under the age of 18 years, informed consent was obtained from their parents.
All procedures performed in this study involving human participants were in accordance with the ethical standards of the institutional and national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Study Design
This double-blind clinical trial crossover study was conducted between August 2017 and May 2018 among β-thalassemia major patients referring to Mohammad Kermanshahi Hospital in Kermanshah, Iran. With regard to previous studies, the sufficient sample size was calculated by (N = (Z1-α/2+ Z1-β)2 × 2S2/(∆)2) formula15 based on serum level of HCY,16 in which α = 0.05 and β = 95%. The calculated sample size was seven individuals in each group. Due to attrition risk, 10 individuals were considered in each group.
The participants were randomly divided into two groups and randomly assigned to ALA group (600 mg/day) or placebo group (corn starch) by a third person who was not aware of the kind of capsules. Each phase of study was 8 weeks, separated by a 3-week washout period. Patients were asked to take a capsule per day for 8 weeks in addition to their routine chelating drugs. It was recommended that the ALA supplement should be consumed half an hour before dinner due to availability increment.17 Adherence to the study protocol was assessed by counting the returned capsules.
Five milliliters of fasting blood were drawn for biochemical assessment at four steps (baseline and at the end of each intervention phase: baseline and 8th, 11th, and 19th weeks). The participants completed a 3-day dietary record at the beginning and at 4-week intervals until the end of study. Participants were instructed how to complete the dietary records. In each intervention phase, they were asked to record their food intakes of two routine days and a weekend day. Nutritionist IV software was used for analyzing food intakes. Furthermore, participants were requested to record their daily physical activities at the beginning and by 4-week intervals until the end of the study. The recorded physical activities were multiplied by the relevant metabolic equivalents (MET) coefficients and finally converted to MET-h/d. (Figure 1).
Anthropometric Measurements
Anthropometric indices including weight, height, and body mass index (BMI) were measured baseline and at the end of each intervention phase (at baseline and 8th, 11th, and 19th weeks) by a trained expert. Using a Seca scale, weight was measured nearest to 0.1 kg. During weight measurement, participants wore light clothing and were barefoot. Height was measured with a Seca stadiometer without shoes, with 0.1 cm accuracy. BMI was calculated by dividing weight (kg) into the height square (m2).
Laboratory Analysis
12–14 h fasting blood samples were taken at the beginning of study (week 1) and at the 8th, 11th, and 19th weeks. Blood samples were centrifuged at 3000 rpm for 10 min and then frozen at 70 °C until performing analysis. ELISA kits were used to measure the serum level of HCY, Lp-PLA2, OPG, and TMAO (SHANGHAICRYSTAL DAY BIOTECH CO., CHINA).
Statistical Analyses
Normal distributions of all variables were assessed by the Kolmogorov–Smirnov test. Except dietary intakes, all variables had normal distributions. Therefore, paired t-test and Wilcoxon were used to compare dietary intakes. Paired t-test was used to compare baseline values of variables between the two groups, baseline and end values of variables within each group, and changes of variables between the two groups. ANCOVA was used to compare the end point values. In this analysis, end values were adjusted for baseline values of variables and monounsaturated fatty acids (MUFA), Vit E, and Vit B6. To determine the Pgroup, Ptime and Pgroup*time, repeated measure analysis of variance was applied. SPSS (SPSS Inc, Chicago, IL, USA, version 16) was used for all statistical analyses. P < .05 was considered as the significant level.
Results
The participants included 13 (65%) men and seven (35%) women. Baseline characteristics of the study population are presented in Table 1.
 |
Table 1 Baseline Characteristics of All Study Participants at Entry (N= 20) |
Dietary intakes of participants are presented in Table 2. Participants in the ALA group had higher intake of MUFA (P= .017) and lower intake of vitamin E (P= .037) and vitamin B6 (P= .017) compared with the placebo group.
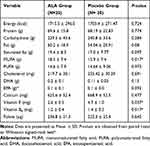 |
Table 2 Dietary Intakes of Individuals in ALA and Placebo Groups |
There was no statistical difference in the body weight and BMI between the two phases of intervention (P> .05). Also, there was no statistical difference in the amount of physical activity between the two phases of the study (31.65 ± 1.82 MET-h/d in ALA group versus 31.8 ± 2.15 MET-h/d in the placebo group; P= .726).
The effects of ALA on CVD risk factors are shown in Table 3. As shown, there was no significant difference according to baseline values of variables between ALA and placebo groups. In the ALA group the OPG levels significantly reduced during 8-wk intervention in all participants (P= .003) and in the male subgroup (P= .015); also in the ALA group, a significant difference was seen in regard to the endpoints of OPG values in comparison with the placebo group in all participants (P= .013) and in the male subgroup (P= .032). However, there was no significant difference in regard to the serum level of HCY, Lp-PLA2, and TMAO during the 8-wk intervention in the ALA group or between the two groups.
 |
Table 3 Baseline and End Values of CVD Risk Factors After 8-Wk of ALA Consumption |
The changes of CVD risk factors after intervention are presented in Table 4. Comparison of intragroup changes of variables between the ALA and placebo groups showed that only changes in serum OPG were significant (P= .006). Additionally, intragroup changes of serum OPG between the ALA and placebo groups in the male subgroup had a trend toward being significant (P= .059). Also, the interaction of group, time, and time×group for all CVD risk factors were not significantly different. For all variables, carry-over effect and period effect were not significant (P> .05).
 |
Table 4 Changes of CVD Risk Factors After 8-Wk of ALA Consumption |
Discussion
The aim of the present study was to determine the effects of ALA supplementation on CVD risk factors in β-thalassemia major patients. ALA significantly reduced OPG levels during the 8-wk of intervention in comparison with placebo group in all participants and in the male subgroup. However, it had no significant effect on serum level of HCY, Lp-PLA2, and TMAO.
In the present study, ALA significantly reduced serum OPG. Tumor necrosis factor-α (TNF-α) is one of the key intermediates of inflammatory processes which increases the secretion of OPG by stimulating the OPG-Von-Willebrand factor.10 Studies have shown that TNF-α decreases following nutritional interventions with ALA consumption. In a systematic review and meta-analysis of RCTs, findings showed that ALA supplementation decreased TNF-α, C-reactive protein (CRP), and interleukin-6 (IL-6) among patients with metabolic syndrome.12 In a study on obese people, a significant reduction in CRP and TNF-α concentrations was observed following ALA supplementation.18 In another study, ALA supplementation decreased TNF-α and IL-6 and increased adiponectin levels in obese subjects with impaired glucose tolerance.15
ALA intake may reduce inflammatory markers through scavenging free radicals, downregulating pro-inflammatory redox-sensitive signal transduction processes including nuclear factor kappa B translocation, leading to lower release of other free radicals and cytotoxic cytokines.19 Moreover, ALA improves cellular antioxidant capacity and phase 2 enzymes such as catalase, reduced glutathione, glutathione reductase, and glutathione-S-transferase.20
It can be said that ALA decreases serum OPG and inhibits vascular calcification by reducing inflammatory mediators such as TNF-α. Therefore, controlling the serum OPG level can be an important complementary therapeutic option to prevent the progression of CVD in β-thalassemia major patients.
Given that OPG is a new risk factor, there is still no reliable source to report the normal range of OPG. However, comparing postintervention OPG level in thalassemic patients with OPG level in healthy subjects in the studies, it was found that the OPG level in thalassemic patients after intervention in this study is similar to the OPG level in healthy subjects and it seems that this level of serum OPG would reduce CVD risk and thus can be considered beneficial to thalassemic patients’ health.21,22
Lp-PLA2 is a macrophage-derived enzyme that after oxidation of LDL can decompose oxidized phosphatidylcholine into lysophosphatidylcholine (LysoPC) and oxidized nonesterified free fatty acids (oxNEFA).23 These compounds significantly contribute to inflammation associated with atherosclerosis and can stimulate monocytes and macrophages to secrete cytokines, which in turn cause more liberation of Lp-PLA2 from macrophages.24 In the present study, ALA consumption had no significant effect on Lp-PLA2.
In Gajos et al's study, omega-3 reduced levels of Lp-PLA2 and ox-LDL in CAD patients. One of the potential mechanisms is that omega-3 protect LDL from oxidation and thereby reduce the substrate for Lp-PLA2.25 However, in the studies of Nelson et al and Pedersen et al, omega-3 did not have a significant effect on Lp-PLA2 in healthy subjects with normal lipid profiles.26,27 In the former study, participants were patients with atherosclerosis that had high level of low-dnsity lipoprotein (LDL); while in the latter study, the levels of lipid profiles were normal and baseline Lp-PLA2 level was lower than the borderline risk. In the present study, similar to Pedersen and Nelson groups' studies, baseline Lp-PLA2 level was lower than the borderline risk.
Chang et al did not find any significant difference in triglyceride or oxidized-LDL levels in diabetic patients who received 600 mg/day ALA compared to the control group.28 In the study of Skulas-Ray et al, a low dose of omega-3 did not affect Lp-PLA2 in hypertriglyceridemia individuals, while its high dose reduced Lp-PLA2 level.29 Also, in Jameel et al's study, ALA inhibited PLA2 in a dose–response manner in the laboratory environment.30 It sounds like Lp-PLA2 responds to the intervention as dose-dependent and in high prescriptive doses of ALA, while the applied dose in this study was the usual dose.
TMAO is produced from the TMA in the liver by the flavin-containing monooxygenase-3 (FMO3) enzyme. Various factors such as some foods, intestinal bacteria, and liver activity on FMO3 enzyme have an effect on TMAO concentration.31 Because TMA is produced from choline, betaine, and carnitine by intestinal microbial metabolism, the consumption of animal products such as egg, liver and meat, or L-carnitine supplementation are considered to be the main source of TMAO in humans.32
In Obeid et al's study, vitamin D alone or with vitamin B supplementation reduced TMAO.33 Vitamin D supplementation has been shown to reduce choline.34 Vitamin D can also alter the intestinal environment and stimulate bacteria to produce dimethylglycine as an alternative to TMA, or use betaine and thereby reduce TMAO.33 In an animal model, through affecting choline, a probiotic reduced the level of TMAO. Probiotics can reduce the production of TMAO by removing choline out of reach TMA-producing bacterial species.35 In Chen et al's study, resveratrol supplement reconstructed the gut microbial environment in mice, which resulted in decreased TMAO production.36
In the study of Boutagy et al, consumption of probiotic supplementation in healthy men for 4 weeks did not affect TMAO or L-carnitine, choline and betaine levels.37 In the study of Baugh et al, daily intake of 10 g of inulin for 6 weeks did not affect TMAO in individuals at risk for diabetes.38 In the present study, TMAO decreased in the ALA group and increased in the placebo group, but similar to Boutagy and Baugh’s studies the observed changes were not significant.
Considering that the intestinal flora plays a decisive role in the formation of TMAO from dietary choline,39 probiotics or other treatments that can alter the intestinal bacteria may affect the concentration of TMAO in clinical populations with high TMAO level compared to healthy individuals. In Boutagy and Baugh’s studies, the samples had low TMAO concentrations that are associated with a relatively low risk of CVD.
The present study did not investigate the changes in the composition of the intestinal bacteria that may be created during the interventional period; therefore, considering the role of intestinal flora in the production of TMAO,39 examination of intestinal flora and effective factors on its alteration is essential. Another factor that may affect any intervention is duration. Although it is known that TMAO is a biomarker that can be rapidly altered by food interventions,40 ALA may require more time to affect TMAO.
In the present study, the level of HCY in ALA and placebo group decreased, but the observed changes were not significant. Various studies have been done to evaluate the effects of supplements on serum HCY levels in different populations with different doses and different duration. In the study of Tayebi Khosroshahi et al, omega-3 significantly decreased the level of HCY in hemodialysis patients.16 In Pakfetrat et al's study, zinc supplementation significantly reduced the level of HCY in renal patients.41 In Hu et al's study, ALA inhibited HCY-induced cellular apoptosis in human aortic endothelial cells that play a key role in CVD, and suppressed HCY stimulation.14
One reason for the inconsistency of our findings with those of Tayebi Khosroshahi, Pakfetrat and Hu is that in these studies the level of HCY in the samples was higher than the normal level (5–15 μmol/L).9 However, the level of HCY in our study was normal at the onset of the study, which could be due to the use of folic acid, an essential supplement in the routine treatment program for thalassemic patients. Another reason for the normal level of HCY in the present study could be the relatively low age of thalassemic patients (23.5±5.47 y), as it has been shown that with increasing age the level of HCY increases.42
The limitations of the present study were low dose of supplementation, short-term intervention time and a relatively small sample size (20 subjects). Another limitation was the lack of measurement of serum ALA due to limited financial resources. Also, considering that there has not been a similar study in the field of ALA supplementation in thalassemia, inevitably we compared our results with other studies that evaluated the effects of ALA or other compounds in different diseases.
Conclusion
The findings of this study showed that 600 mg of ALA supplementation for 8-wk in β-thalassemia major patients resulted in a significant decrease in serum OPG. However, it had no significant effect on serum HCY, Lp-PLA2, and TMAO. To the best of our knowledge, this is the first study that has investigated the effects of ALA on CVD risk factors in β-thalassemia major patients; therefore, further studies are needed.
Abbreviations
ALA, alpha-lipoic acid; CVD, cardiovascular disease; OPG, osteoprotegerin; HCY, homocysteine; Lp-PLA2, lipoprotein-associated phospholipase A2; TMAO, trimethylamine N-oxide; BMI, body mass index; ELISA, enzyme-linked immunosorbent assay; ANCOVA, analysis of covariance; MUFA, monounsaturated fatty acids; TNF-α, tumor necrosis factor-α; RCT, randomized clinical trials; CRP, C-reactive protein; IL-6, interleukin-6; LDL, low-density lipoprotein; LysoPC, lysophosphatidylcholine; OxNEFA, oxidized nonesterified free fatty acids; Ox-LDL, oxidized-LDL; CAD, coronary artery disease; FMO3, flavin-containing monooxygenase-3.
Registration Number
This study was approved by the research deputy of Kermanshah University of Medical Sciences (Code No: IR.KUMS.REC.1397.192) and registered in the Iranian Clinical Trials Registry (registration number IRCT2017061714237N2).
Data Sharing Statement
The data sets used during the current study are available from the corresponding author on reasonable request.
Acknowledgments
This study was extracted from an MSc dissertation which was approved by School of Nutritional Sciences and Food Technology, Kermanshah University of Medical Sciences with the code number 97212. We hereby express our gratitude to all the staff working in the Mohammad Kermanshahi Hospital in the city of Kermanshah and the participants for their cooperation.
Funding
This study was funded by the Vice-Chancellor of Research in Kermanshah University of Medical Sciences.
Disclosure
The authors declare that they have no conflict of interest.
References
1. Haghi M, Poolady N, Hosseinpoor Faizi M, Hosseinpoor Faizi A. Beta thalassemia in Iran. J Shaheed Sadoughi Univ Med Sci. 2010;18(2):127–133.
2. Alhamdan NA, Almazrou YY, Alswaidi FM, Choudhry AJ. Premarital screening for thalassemia and sickle cell disease in Saudi Arabia. Genet Med. 2007;9(6):372–377. doi:10.1097/GIM.0b013e318065a9e8
3. Muncie HL, Campbell J. Alpha and beta thalassemia. Am Fam Physician. 2009;80(4):339–344.
4. Malik S, Syed S, Ahmed N. Complication in transfusion-dependent patients of B-thalassemia major. Pak J Med Sci. 2009;45(4):678–682.
5. Vechio C, Derchi G. Management of cardiac complication in patients with thalassemia major. Semin Hematol. 1995;32(4):283–296.
6. Mente A, Chalcraft K, Ak H, et al. the relationship between trimethylamine-N-oxide and prevalent cardiovascular disease in a multiethnic population living in Canada. Can J Cardiol. 2015;31(9):1189–1194. doi:10.1016/j.cjca.2015.06.016
7. Sherief LM, Dawood O, Ali A, et al. Premature atherosclerosis in children with beta-thalassemia major: new diagnostic marker. BMC Pediatr. 2017;17(69):1–8. doi:10.1186/s12887-017-0820-1
8. Ragab SM, Safan MA, Obeid OM, Sherief AS. Lipoprotein-associated phospholipase A2 (Lp-PLA2) and tumor necrosis factor-alpha (TNF-α) and their relation to premature atherosclerosis in β-thalassemia children. Hematology. 2015;20(4):228–238. doi:10.1179/1607845414Y.0000000180
9. Ozdem S, Kupesiz A, Yesilipek A. Plasma homocysteine levels in patients with β-thalassaemia major. Scand J Clin Lab Invest. 2008;68(2):134–139. doi:10.1080/00365510701516343
10. Wollin SD, Jones PJ. Alpha-lipoic acid and cardiovascular disease. J Nutrition. 2003;133(11):3327–3330. doi:10.1093/jn/133.11.3327
11. Valko M, Morris H, Cronin MT. Metals, toxicity and oxidative stress. Curr Med Chem. 2005;12(10):1161–1208. doi:10.2174/0929867053764635
12. Akbari M, Ostadmohammadi V, Tabrizi R, et al. The effects of alpha-lipoic acid supplementation on inflammatory markers among patients with metabolic syndrome and related disorders: a systematic review and meta-analysis of randomized controlled trials. Nutr Metab (Lond). 2018;15(1):39. doi:10.1186/s12986-018-0274-y
13. Fontani F, Marcucci G, Iantomasi T, Brandi ML, Vincenzini MT. Glutathione, N-acetylcysteine and lipoic acid down-regulate starvation-induced apoptosis, RANKL/OPG ratio and sclerostin in osteocytes: involvement of JNK and ERK1/2 signalling. Calcif Tissue Int. 2015;96(4):335–346. doi:10.1007/s00223-015-9961-0
14. Hu H, Wang C, Jin Y, et al. Alpha-lipoic acid defends homocysteine-induced endoplasmic reticulum and oxidative stress in HAECs. Biomed Pharmacother. 2016;80:63–72. doi:10.1016/j.biopha.2016.02.022
15. Zhang Y, Han P, Wu N, et al. Amelioration of lipid abnormalities by α-lipoic acid through antioxidative and anti-inflammatory effects. Obesity (Silver Spring). 2011;19(8):1647–1653. doi:10.1038/oby.2011.121
16. Tayebi-Khosroshahi H, Dehgan R, Habibi Asl B, et al. Effect of omega-3 supplementation on serum level of homocysteine in hemodialysis patients. Iran J Kidney Dis. 2013;7(6):479–484.
17. Ahmadi A, Mazooji N, Roozbeh J, Hasanzade J, Mazloom Z, Aliasghari F. The effects of dietary supplementation with alpha-lipoic acid and vitamin E, individually and combined, on insulin resistance and lipid profile in hemodialysis patients. Iran J Nutr Sci Food Technol. 2013;7(4):55–62.
18. Carbonelli MG, Di Renzo L, Bigioni M, Di Daniele N, De Lorenzo A, Fusco MA. Alpha-lipoic acid supplementation: a tool for obesity therapy. Curr Pharm Des. 2010;16(7):840–846. doi:10.2174/138161210790883589
19. Wong A, Dukic-Stefanovic S, Gasic-Milenkovic J, et al. Anti-inflammatory antioxidants attenuate the expression of inducible nitric oxide synthase mediated by advanced glycation endproducts in murine microglia. Eur J Neurosci. 2001;14(12):1961–1967. doi:10.1046/j.0953-816x.2001.01820.x
20. Cao Z, Tsang M, Zhao H, Li Y. Induction of endogenous antioxidants and Phase 2 enzymes by alpha-lipoic acid in rat cardiac H9C2 cells: protection against oxidative injury. Biochem Biophys Res Commun. 2003;310(3):979–985. doi:10.1016/j.bbrc.2003.09.110
21. Rozas Moreno P, Reyes Garcia R, Garcia-Martin A, Varsavsky M, Garcia-Salcedo JA, Munoz-Torres M. Serum osteoprotegerin: bone or cardiovascular marker in type 2 diabetes males. J Endocrinol Invest. 2013;36(1):16–20. doi:10.3275/8285
22. Buleu FN, Luca CT, Tudor A, et al. Correlations between vascular stiffness indicators, OPG, and 25-OH vitamin D3 status in heart failure patients. Medicina (Kaunas). 2019;55(6):309. doi:10.3390/medicina55060309
23. Macphee CH, Nelson JJ, Zalewski A. Role of lipoprotein-associated phospholipase A2 in atherosclerosis and its potential as a therapeutic target. Curr Opin Pharmacol. 2006;6(2):154–161. doi:10.1016/j.coph.2005.11.008
24. Zalewski A, Macphee C, Nelson JJ. Lipoprotein-associated phospholipase A2: a potential therapeutic target for atherosclerosis. Curr Drug Targets Cardiovasc Haematol Disord. 2005;5(6):527–532. doi:10.2174/156800605774962103
25. Gajos G, Zalewski J, Mostowik M, Konduracka E, Nessler J, Undas A. Polyunsaturated omega-3 fatty acids reduce lipoprotein-associated phospholipase A2 in patients with stable angina. Nutr Metab Cardiovasc Dis. 2014;24(4):434–439. doi:10.1016/j.numecd.2013.09.011
26. Nelson TL, Hokanson JE, Hickey MS. Omega-3 fatty acids and lipoprotein associated phospholipase A2 in healthy older adult males and females. Eur J Nutr. 2011;50(3):185–193. doi:10.1007/s00394-010-0126-7
27. Pedersen MW, Koenig W, Christensen JH, Schmidt EB. The effect of marine n-3 fatty acids in different doses on plasma concentrations of Lp-PLA2 in healthy adults. Eur J Nutr. 2009;48(1):1–5. doi:10.1007/s00394-008-0758-z
28. Chang JW, Lee EK, Kim TH, et al. Effects of alpha-lipoic acid on the plasma levels of asymmetric dimethylarginine in diabetic end-stage renal disease patients on hemodialysis: a pilot study. Am J Nephrol. 2007;27(1):70–74. doi:10.1159/000099035
29. Skulas-Ray AC, Alaupovic P, Kris-Etherton PM, West SG. Dose-response effects of marine omega-3 fatty acids on apolipoproteins, apolipoprotein-defined lipoprotein subclasses, and Lp-PLA2 in individuals with moderate hypertriglyceridemia. J Clin Lipidol. 2015;9(3):360–367. doi:10.1016/j.jacl.2014.12.001
30. Jameel NM, Shekhar MN, Vishwanath BS. Α-lipoic acid: an inhibitor of secretory phospholipase A2 with anti-inflammatory activity. Life Sci. 2006;80(2):146–153. doi:10.1016/j.lfs.2006.08.032
31. Koeth RA, Wang Z, Levison BS, et al. Intestinal microbiota metabolism of L-carnitine, a nutrient in red meat, promotes atherosclerosis. Nat Med. 2013;19(5):576–585. doi:10.1038/nm.3145
32. Fukami K, Yamagishi S, Sakai K, et al. Oral L-carnitine supplementation increases trimethylamine-N-oxide but reduces markers of vascular injury in hemodialysis patients. Cardiovasc Pharmacol. 2015;65(3):289–295. doi:10.1097/FJC.0000000000000197
33. Obeid R, Awwad HM, Kirsch SH, et al. Plasma Trimethylamine-N-oxide following supplementation with vitamin D or D plus B vitamins. Mol Nutr Food Res. 2017;61(2):1–24. doi:10.1002/mnfr.201600358
34. Han H, Cui M, You X, et al. A role of 1,25(OH)2D3 supplementation in rats with nonalcoholic steatohepatitis induced by choline-deficient diet. Nutr Metab Cardiovasc Dis. 2015;25(6):556–561. doi:10.1016/j.numecd.2015.02.011
35. Martin FP, Wang Y, Sprenger N, et al. Probiotic modulation of symbiotic gut microbial–host metabolic interactions in a humanized microbiome mouse model. Mol Syst Biol. 2008;4(1):157. doi:10.1038/msb4100190
36. Chen ML, Yi L, Zhang Y, et al. Resveratrol attenuates Trimethylamine-N-oxide (TMAO)-induced atherosclerosis by regulating TMAO synthesis and bile acid metabolism via remodeling of the gut microbiota. mBio. 2016;7(2):e02210–15. doi:10.1128/mBio.02210-15
37. Boutagy NE, Neilson AP, Osterberg KL, et al. Probiotic supplementation and trimethylamine-N-oxide production following a high-fat diet. Obesity (Silver Spring). 2015;23(12):2357–2363. doi:10.1002/oby.21212
38. Baugh ME, Steele CN, Angiletta CJ, et al. Inulin supplementation does not reduce plasma trimethylamine N-oxide concentrations in individuals at risk for type 2 diabetes. Nutrients. 2018;10(6):793. doi:10.3390/nu10060793
39. Tripolt NJ, Leber B, Triebl A, Kofeler H, Stadlbauer V, Sourij H. Effect of lactobacillus casei shirota supplementation on trimethylamine-N-oxide levels in patients with metabolic syndrome: an open-label, randomized study. Atherosclerosis. 2015;242(1):141–144. doi:10.1016/j.atherosclerosis.2015.05.005
40. Angiletta CJ, Griffin LE, Steele CN, et al. Impact of short-term flavanol supplementation on fasting plasma trimethylamine-N-oxide concentrations in obese adults. Food Funct. 2018;9(10):5350–5361. doi:10.1039/C8FO00962G
41. Pakfetrat M, Shahroodi JR, Zolgadr AA, Larie HA, Nikoo MH, Malekmakan L. Effects of zinc supplement on plasma homocysteine level in end-stage renal disease patients: a double-blind randomized clinical trial. Biol Trace Elem Res. 2013;153(1–3):11–15. doi:10.1007/s12011-013-9639-2
42. Beavers KM, Beavers DP, Bowden RG, Wilson RL, Gentile M. Omega-3 fatty acid supplementation and total homocysteine levels in end-stage renal disease patients. Nephrol (Carlton). 2008;13(4):284–288. doi:10.1111/j.1440-1797.2008.00934.x
 © 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2020 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
