Back to Journals » Clinical Ophthalmology » Volume 8
Effect of dorzolamide/timolol combination on the visual field in glaucoma
Authors Takeda S, Mimura T, Matsubara M
Received 15 July 2014
Accepted for publication 29 July 2014
Published 25 August 2014 Volume 2014:8 Pages 1579—1590
DOI https://doi.org/10.2147/OPTH.S71162
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 4
Editor who approved publication: Dr Scott Fraser
Sakurako Takeda,1,2 Tatsuya Mimura,1 Masao Matsubara1,2
1Department of Ophthalmology, Tokyo Women’s Medical University Medical Center East, Tokyo, Japan; 2Department of Ophthalmology, Nippori Clinic, Medical Center East, Tokyo Women’s Medical University, Tokyo, Japan
Purpose: To evaluate the effect of treatment for 3 years with a dorzolamide/timolol (1%/0.5%) fixed combination (DTFC) on visual field progression in patients with open-angle glaucoma.
Participants: A total of 14 consecutive patients were enrolled who had been previously treated with monotherapy or any combination of a beta blocker, carbonic anhydrase inhibitor, and/or prostaglandin analog for primary open-angle glaucoma (POAG; n=4) or normal-tension glaucoma (NTG; n=10).
Methods: Patients were switched to DTFC from their prior glaucoma therapy. The IOP was measured at intervals of 4–6 weeks, and the visual fields were examined at least twice a year for 3 years. The annual change of mean deviation (MD slope) was used to quantify visual field loss.
Results: The mean MD value was –5.9±5.0 dB at baseline; it was –5.6±4.8 dB at 12 months, –5.9±5.0 dB at 24 months, and –5.6±5.1 dB at 36 months after switching. The mean MD slope was –0.2±0.8 dB/year before switching and 0.3±1.3 dB/year from baseline to 1 year, –0.3±1.1 dB/year from 1–2 years, and 0.3±0.9 dB/year from 2–3 years after switching. The mean MD slope from baseline to 36 months was correlated with the IOP reduction rate at 36 months after switching. Visual field progression was associated with the IOP reduction rate at 12 months after switching.
Conclusion: Switching to DTFC from prior glaucoma therapy improved the MD slope for at least 3 years. Reduction of the IOP after switching to DTFC was effective for delaying visual field progression. Although our study was not nonrandomized and was small in scale, the findings suggest that DTFC might have a beneficial effect on the visual fields in patients with open-angle glaucoma.
Keywords: dorzolamide/timolol (1%/0.5%) fixed combination, switch, visual field, MD slope
Introduction
Glaucoma is defined by the presence of a glaucomatous visual field defect. An increased intraocular pressure (IOP) is the most important risk factor for developing glaucomatous optic neuropathy that causes visual field defects.1–7 The Early Manifest Glaucoma Trial showed that each increase (or decrease) of 1 mmHg in the IOP was associated with approximately a 10% increase (or decrease) in the risk for progression of visual field loss.8 Thus, the primary goal of treating glaucoma is to reduce the IOP to the target pressure, and the options available for this purpose include ocular hypotensive agents, laser therapy, and surgery.9
Use of multiple medications for glaucoma may increase the risk for adverse effects, drug interactions, and nonadherence to treatment. Thus, we should aim to treat glaucoma with the minimum number of medications and the lowest doses required for IOP control. Combination therapy is expected to improve compliance and convenience for patients because it achieves fewer doses, lower costs, and fewer adverse effects because of a reduction of preservatives.10,11 Fixed combination drugs have several advantages.11,12 First, these drugs reduce the cost of treatment. Second, such drugs are more convenient and thus lead to better adherence because of less-frequent dosing. Third, a reduced decrease in the daily number of instillations will also reduce adverse effects. For instance, a fixed combination drug can potentially reduce repeated exposure of the ocular surface to ophthalmic preservatives compared with the use of two standard drugs. Fourth, fixed combinations sometimes show greater efficacy for reducing the IOP by avoiding the washout effect from administering a second eye drop after the first drop.
Recently, various combined ocular preparations have been successfully developed. The combination of dorzolamide (2%) and timolol maleate (0.5%) (Cosopt®; Merck & Co, Inc, Whitehouse Station, NJ, USA) contains a topical carbonic anhydrase inhibitor and a topical beta-adrenergic receptor blocking agent, which is the most widely used combination for glaucoma worldwide.11,13–15 In Japan, a combined drug with a lower concentration of dorzolamide (1%) and the same concentration of timolol maleate (0.5%) (Cosopt®; MSD, Tokyo, Japan; and Santen, Osaka, Japan) was developed and has been marketed since 2010. Mizoguchi et al reported that an IOP-lowing effect of adding this dorzolamide/timolol (1%/0.5%) fixed combination (DTFC) to a prostaglandin analog (PGA) was detected within 8 weeks in patients with normal-tension glaucoma (NTG).15 We have also evaluated the long-term reduction of IOP reduction and safety after switching to DTFC in patients with open-angle glaucoma. Our previous study showed that the mean IOP reduction rate was 12.8%±15.2% at 36 months after switching and that more than 10% reduction of the IOP from baseline was maintained for 36 months.16 However, there has been no report on the long-term effect of DTFC therapy on the progression of visual field loss. Accordingly, the aim of the present study was to evaluate the long-term effect of DTFC therapy on the IOP and visual fields in patients with open-angle glaucoma treated for 3 years. This report covers part of our investigation into the long-term beneficial effects of DTFC.16
Materials and methods
Study design
This was a prospective, longitudinal, uncontrolled, nonrandomized, and consecutive case series study conducted at the hospital of Nippori Clinic Medical Center East, Tokyo Women’s Medical University Hospital, and Tokyo Women’s Medical University Medical Center East Hospital in Japan. This study was performed in accordance with the Helsinki Declaration. This study was approved by the Tokyo Women’s Medical University Institutional Review Board for Clinical Research. There was no financial support or sponsorship from the pharmaceutical industry.
Subjects
The purpose and nature of the present study were explained in detail to all patients, and informed consent was obtained. Patients who fulfilled the eligibility criteria were recruited consecutively at routine hospital visits between June 2010 and September 2010. The present report covers the effect of DTFC therapy on IOP over 3 years, and the study population consists of the same subjects reported in a previous manuscript.16
The inclusion criteria were as follows: an age of 18 years or older who have the capacity to give informed consent; characteristic glaucomatous visual field loss and optic nerve head damage in at least one eye; treatment with a PGA, beta-blocker (BB), and/or carbonic anhydrase inhibitor (CAI) for at least 3 months; and best-corrected visual acuity of 20/200 or better (because visual impairment may affect test results of visual field).
The exclusion criteria were as follows: closed or barely open anterior chamber angle, a history of acute angle closure or ocular trauma, neovascular glaucoma, a history of ocular surgery including refractive surgery or glaucoma filtering surgery, a history of ocular inflammation or infection during the preceding 6 months, clinically significant dry eyes syndrome, or the inability to adhere to the plan for treatment and hospital visits.
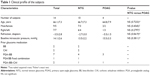
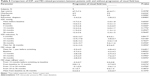
Nineteen patients who switched to DTFC were provisionally enrolled in this prospective clinical study. Five of these 19 patients were excluded because of lack of continuous visual field data during the observation period. As a consequence, the study population consisted of 14 patients with NTG (N=10) or primary open-angle glaucoma (POAG; N=4). The subjects were aged 66.1±7.3 years (mean ± standard deviation), with an age range of 52–81 years (Table 1). These patients were also included in our previous report.16 All patients were Asian (Japanese) and were residents of Japan. As prior antiglaucoma therapy, two patients were using BB (14.3%), two were using CAI (14.3%), seven were using PGA+BB (50.0%), one was using a PGA/BB fixed combination (7.1%), and two were using PGA+BB+CAI (14.3%) (Table 1).
Intervention
Patients were switched to DTFC (Cosopt®; MSD/Santen) without a washout period between the old and new treatments. Switching was performed at the attending physician’s discretion. The main reasons for switching to DTFC were insufficient control of the IOP and progression of visual field defects.17 The 4 patients with prior BB monotherapy (N=2) or CAI monotherapy (N=2) were switched to DTFC alone (28.6%), whereas the 7 patients with prior PGA+BB therapy were switched to PGA+DTFC (50.0%). One patient using a PGA/BB fixed combination drug was switched to DTFC alone (7.1%), whereas 2 patients receiving prior PGA+BB+CAI triple therapy were switched to PGA+DTFC (14.3%). To assess the efficacy of DTFC as a part of multidrug therapy (together with BB, CAI, and/or PGA) or as monotherapy (after switching from BB or CAI), patients were divided into two groups according to the change in the number of antiglaucoma medications: an increase group (switched from BB or CAI to DTFC or from PGA+BB to PGA+DTFC; N=11 [78.6%]) and a no-increase group (switched from PGA/BB fixed combination to DTFC or from PGA+BB+CAI to PGA+DTFC; N=3 [21.4%]). If both eyes fulfilled the eligibility criteria for this study, the eye with the higher baseline IOP was used for analysis. If both eyes showed the same IOP at baseline, the right eye was used for analysis.
Visual field analysis
Visual fields were examined at least twice a year, using the central 30 to 2 program of the Humphrey Field Analyzer (Humphrey Field Analyzer HFA-740i; Carl Zeiss Meditec, Inc, Dublin, CA, USA). The mean deviation (MD) was used to quantify visual field impairment, which was calculated from the program 30-2 test. The annual change of MD (MD slope, dB/year) was calculated in each subject by linear regression analysis, using the SLOPE function in Microsoft Excel 2010 (Microsoft Corporation, Redmond, WA, USA). MD values obtained from reliable visual field tests (<20% fixation errors, <33% false-positives, and <33% false-negatives) were used. To calculate the MD slope, data from 3 or more reliable measurements obtained on different days were used. Patients underwent an average of 3.4±0.6 visual field tests (range, 3–5 tests) before switching to DTFC therapy, as well as 6.1±0.8 visual field tests (range, 5–7 tests) after switching. Visual field progression was defined as deterioration of the visual fields according to the modified guideline proposed by the Early Manifest Glaucoma Trial; that is, at least 3 identical continuous points showing at least 3 dB of deterioration on glaucoma change probability maps, based on the changes of pattern deviation values in two consecutive tests.18,19
Main outcome
The age, gender, medical history, antiglaucoma medications, and ocular history of each patient were assessed at the baseline visit. All subjects underwent a complete ophthalmic examination (including anterior segment biomicroscopy and fundus examination) and refraction with an automated kerato-refractometer (RC-5000; TOMEY, Nagoya, Japan). The spherical power and cylindrical power were both measured, after which the spherical equivalent (sphere +1/2 cylinder) was used to calculate the refractive error.
Follow-up visits were scheduled at intervals of approximately 4–6 weeks for 3 years. If a patient cancelled a scheduled appointment, the data obtained at the visit closest to the scheduled time were used for analysis. At each visit, the IOP was measured by Goldmann applanation tonometry in the morning (between 9 am and 12 noon) by the same ophthalmologist (ST). The percentage decrease of the IOP (IOP reduction rate) was calculated as ([baseline IOP – mean IOP]/baseline IOP) ×100. MD values and the calculated MD slope were used to quantify changes of the visual fields. All data were entered into a computerized database at the time of each visit.
Statistical analysis
Continuous variables were compared between two groups by using the one-tailed or two-tailed paired or unpaired Student’s t-test; analysis of frequencies was performed with the χ2 test or Fisher’s exact test. Relations among variables were investigated by calculating Pearson’s correlation coefficients. Factors associated with the mean MD slope over the course of 3 years after switching to DTFC and factors associated with visual field progression were investigated by multivariate logistic regression analysis, with the explanatory variables including the age (years); sex (male/female); right/left eye; refraction (diopter); type of glaucoma (POAG/NTG); number of antiglaucoma medications after switching (no-increase group versus increase group); IOP at baseline and at 3, 12, 24, and 36 months; IOP reduction rates at 3, 12, 24, and 36 months; MD at baseline and at 12, 24, and 36 months; and MD slope before switching and at each time after switching. The level of significance was set at P<0.05. Statistical analysis was performed with SAS System software version 9.1 (SAS Institute Inc, Cary, NC, USA).
Results
The demographic profile of the subjects is summarized in Table 1. There were no adverse effects or toxicity during the treatment with DTFC. The mean IOP was 14.1±2.6 mmHg at baseline and 12.6±2.2 mmHg at 3 months, 12.2±2.2 mmHg at 6 months, 12.9±2.4 mmHg at 12 months, 12.4±3.0 mmHg at 18 months, 11.6±1.8 mmHg at 24 months, 12.1±2.0 mmHg at 30 months, and 12.4±2.9 mmHg at 36 months after switching (Table 2). There was a significant decrease of the IOP at 3, 6, 18, and 24 months after switching compared with baseline (P<0.05, paired two-tailed Student’s t-test; Table 2). There was no significant difference of IOP between the no-increase group and the increase group at all times of measurement (Table 2). After switching to DTFC, the POAG group tended to have a higher IOP than the NTG group, and there was a significant difference between the two groups at 12 months after switching (P=0.0020; Table 2).
The mean IOP reduction rate was 9.6%±11.8% at 3 months, 12.2%±12.2% at 6 months, 6.8%±16.8% at 12 months, 16.0%±11.7% at 24 months, and 11.4%±14.4% at 36 months after switching (Table 2). The mean IOP reduction rate tended to be higher in the increase group than in the no-increase group at all times of assessment, although there was no statistical difference between the two groups (unpaired two-tailed Student’s t-test; Table 2). The mean IOP reduction rate was higher in the NTG patients than in the POAG patients, although there was no significant difference between them (unpaired two-tailed Student’s t-test; Table 2).
The mean MD value was -6.0±4.5 dB before baseline, -5.9±4.8 dB at baseline, and -5.6±4.6 dB at 12 months, -5.9±4.8 dB at 24 months, and -5.6±4.9 dB at 36 months after switching (Figure 1). There was no significant difference of the mean MD value compared with baseline at 12 (P=0.4557), 24 (P=0.9715), and 36 (P=0.5546) months after switching (paired two-tailed Student’s t-test; Figure 1). Mean MD values were higher in the no-increase group than in the increase group at all times of assessment (-3.4±0.6 versus -6.7±5.1 dB [P=0.0728] before baseline, -3.7±0.7 versus -6.5±5.4 dB [P=0.1477] at baseline, -3.4±0.6 versus -6.2±5.2 dB [P=0.1228] at 12 months, -3.0±1.1 versus -6.6±5.4 dB [P=0.0789] at 24 months, and -2.7±0.7 versus -6.4±5.5 dB [P=0.0644] at 36 months after switching, unpaired two-tailed Student’s t-test). However, no significant differences were found between the two groups. Mean MD values also tended to be higher in the POAG patients than in the NTG patients at all times (-4.0±1.5 versus -6.8±5.3 dB [P=0.1939] before baseline, -3.8±1.7 versus -6.7±5.6 dB [P=0.1872] at baseline, -3.8±2.0 versus -6.3±5.3 dB [P=0.2495] at 12 months, -3.7±1.8 versus -6.7±5.6 dB [P=0.1885] at 24 months, and -2.8±1.6 versus -6.7±5.5 dB [P=0.0801] at 36 months after switching, unpaired two-tailed Student’s t-test), although no statistical differences were found between them.
The mean MD slope was -0.2±0.8 dB/year before switching to DTFC and 0.3±1.3 dB/year from baseline to 1 year after switching, -0.3±1.1 dB/year from 1–2 years after switching, and 0.3±0.9 dB/year from 2–3 years after switching (Figure 2). There was no significant difference of the mean MD slope from baseline to 1 year (P=0.3599), 1–2 years (P=0.8680), and 2–3 years (P=0.2268) after switching to DTFC compared with that before switching (paired two-tailed Student’s t-test; Figure 2). There were also no significant differences of the mean MD slope between the no-increase and increase groups or between the NTG and POAG patients throughout the observation period, except at 36 months after switching (P=0.0162, paired two-tailed Student’s t-test). Figure 3 shows pattern standard deviation and foveal sensitivity before and after switching to DTFC. Pattern standard deviation significantly increased from 7.3±4.6 dB at baseline to 7.8±5.0 dB at 12 months, 8.2±4.4 dB at 24 months, and 8.0±4.5 dB at 36 months after switching to DTFC (Figure 3A; P<0.05, paired one-tailed Student's t-test). Mean foveal sensitivity showed significant increase at 12 months (34.8±3.4 dB) compared with at baseline (33.5±4.1 dB; P=0.0315) and no significant decrease during observation after switching to DTFC (paired one-tailed Student’s t-test; Figure 3B).
Table 3 shows correlations among the mean MD values over the course of 1 year before switching to DTFC (dB, Pre-MD), the baseline MD value immediately before switching (dB, baseline MD), the MD slope for 1 year before switching (dB/year, Pre-MD slope), and the mean MD slope for 3 years after switching (dB/year, Post-MD slope). The mean Post-MD slope showed a negative correlation with the mean Pre-MD slope (R=-0.63; P=0.0150; Pearson’s product moment correlation coefficient; Table 3). Figure 4 shows a scatter plot with the regression line for the relation between the mean MD slope for 1 year before switching to DTFC (Pre-MD slope) and the mean MD slope for 3 years after switching (Post-MD slope). There was a significant correlation between the Post-MD slope and the Pre-MD slope (Post-MD slope =-0.1625 to 0.4896× Pre-MD slope, R2=0.4014, P=0.0150).
Table 4 displays the correlations of the mean MD slope for 3 years after switching to DTFC (Post-MD slope) with various factors and the multivariate odds ratios for the MD slope. Univariate and multivariate analyses showed there was no significant influence on the Post-MD slope of various factors before switching, including the age, sex, right/left eye, refraction, glaucoma type (NTG/POAG), no-increase group/increase group, and baseline IOP (Table 4). When factors after switching were assessed, such as the IOP, MD, and MD slope, the IOP reduction rate at 36 months was correlated with the mean Post-MD slope according to Pearson’s correlation coefficient analysis (R=0.67, P=0.0091; Table 4), but there was no significant association with the other parameters. In addition, multivariate analysis showed that none of the factors had a significant influence on the mean Post-MD slope (Table 4). Figures 4 and 5 show scatter plots and regression lines for the association between the mean MD slope for 3 years after switching to DTFC (Post-MD slope) and the IOP reduction rate at 3 years after switching (Figure 5A) or the mean IOP reduction rate for 3 years after switching (Figure 5B). There was a significant positive correlation between the Post-MD slope (-0.2651+0.0179×100 [%]) and the IOP reduction rate at 3 years (R2=0.2020, P=0.0091). However, the Post-MD slope showed no significant correlation with the mean IOP reduction rate for 3 years after switching to DTFC (Post-MD slope, -0.0894+0.0024×100 [%]; reduction of IOP for 3 years, R2=0.0020, P=0.8807).
Progression of visual field loss, which was defined as a 3 dB decrease of pattern deviation values at the same three points in two consecutive tests, was detected in five (35.7%) of the 14 patients. Table 5 shows a comparison of IOP- and MD-related parameters between the patients with and without visual field progression. The reduction of IOP at 12 months after switching (P=0.0160) and the MD slope from baseline to 12 months after switching were greater in patients with visual field progression than in those without progression (P=0.0027, two-tailed unpaired t-test; Table 5). Univariate analysis revealed a positive association between the progression of visual field loss and the IOP at 12 months after switching. However, no association was found between the IOP and progression of visual field loss by multivariate analysis (Table 6).
Discussion
This study provides the first evidence about the 3-year outcome of visual field progression after switching to DTFC therapy. MD values remained stable for 3 years, changing slightly from -5.9±4.8 dB at baseline to -5.6±4.9 dB at 3 years after switching. The MD slope improved from -0.2±0.7 dB/year at baseline to 0.3±0.9 dB/year at 3 years after switching, and the mean MD slope for 3 years was -0.1± 0.6 dB/year. In addition, the mean MD slope for 3 years was correlated with the IOP reduction rate at 36 months. These results suggest that switching to DTFC therapy contributed to the prevention of visual field defects, probably by reducing the IOP.
The MD value improved by +0.3 dB from baseline to 3 years after switching. The MD slope also improved by +0.5 dB/year from baseline to 3 years after switching. In addition, the mean MD slope over 3 years was -0.1±0.6 (dB/year), and the mean change of MD over 3 years from baseline was 0.1±0.4 dB per year. We cannot compare these results with those of other studies because there have been no other reports about MD changes after switching to DTFC therapy. Koseki et al compared the effect of oral brovincamine on the MD slope over 2 years between treated and untreated patients with NTG. The MD slope of the untreated patients was -0.778±0.178 dB/year, which was significantly steeper than that of the treated patients (-0.071±0.195 dB/year).20 Comparing the MD slope of the untreated patients in that previous study (-0.778 dB/year)20 with the slope in our study (0.1 dB/year over 3 years) suggests that switching to DTFC was effective for the prevention of progressive visual field loss. There are several reasons possible why we observed the further improvement of the MD slope after switching therapy. The first possibility is that the MD slope before switching was relatively gentle (-0.21 dB/year), resulting in a steeper MD slope after switching. However, our study demonstrated that the mean MD slope for 3 years after switching was negatively correlated with the MD slope before switching (Figure 4). Thus, the progression of visual field loss before switching to DTFC may not influence that after switching. Second, the study population included 11 patients in the increase group (78.6%) who received more active ingredients after switching to DTFC. Greater reduction of IOP by increasing glaucoma medications may be associated with the prevention of progressive visual field loss by switching to DTFC. However, we cannot confirm this because there were no significant differences between the no-increase and increase groups with respect to the IOP or the IOP reduction rate after switching (Table 2). Further studies on a larger scale will be needed to test these hypotheses.
The mean MD values of the no-increase and POAG groups were higher than those of the increase and NTG groups. In contrast, the MD slope showed no significant differences between the no-increase and increase groups or between the NTG and POAG groups. This discrepancy between MD values and the MD slope primarily arises because the baseline MD was lower in the increase group and the NTG group. Thus, switching to DTFC had a preventive effect on visual field progression regardless of prior medications (no-increase/increase groups) or the type of glaucoma (POAG/NTG).
The reasons why DTFC therapy could maintain better MD values and MD slopes for three years after switching are not clear from the present study. However, this may have been a result of the higher IOP reduction rate after switching (Table 2). The IOP reduction rate from the baseline was 11.4%±14.4% at 36 months after switching (Table 2). Sonty et al reported that the IOP was reduced from 21.4±2.5 mmHg at baseline to 17.9±3.5 mmHg at 12 weeks after switching to DTFC from latanoprost (n=57).14 Mizoguchi et al reported that the IOP was reduced from 15.6±2.0 mmHg at baseline to 13.7±2.2 mmHg at 8 weeks after adding DTFC to PGA monotherapy (n=40), and the percentage reduction of IOP from baseline was 11.7%±13.1% at 8 weeks.15 In our study, prior medications were switched to DTFC, whereas DTFC was added to latanoprost by Mizoguchi et al but the IOP reduction rate obtained in the present study was similar to those reported previously.14,15 Considering these results, an IOP reduction rate of 11.7% after switching to DTFC may be sufficient for protection against visual field progression.
In this study, univariate and multivariate analyses were employed to assess the association of the mean MD slope for 3 years with clinical variables. None of the factors before switching showed a significant association with the mean MD slope for 3 years (Table 4). Regarding factors after switching, the mean MD slope for 3 years was correlated with the IOP reduction rate at 36 months according to univariate analysis, but not by multivariate analysis (Table 4). Fukuchi et al reported that the MD slope was negatively associated with the mean follow-up IOP in patients with POAG, but this association was not observed in patients with NTG.21 These results suggest that the reduction of IOP after switching to DTFC is the most important factor influencing the progression of visual field loss, but some other potential factors must also be considered. The first possibility is the effect of DTFC on ocular blood flow.22 Systemic carbonic anhydrase inhibitors are known to increase retinal blood flow.23,24 A topical carbonic anhydrase inhibitor (dorzolamide) also increases retinal blood flow in patients with NTG.25 DTFC increases the arteriovenous passage time of fluorescein dye through the superior temporal artery compared with timolol in patients with POAG.26 DTFC also has a greater effect than latanoprost on pulsatile ocular blood flow in patients with POAG.22 Furthermore, DTFC raises the diastolic ocular perfusion pressure by counteracting the decrease of diastolic blood pressure with a substantial reduction of IOP.27 The results of these studies suggest that an increase of retinal blood flow with DTFC may delay or prevent the progression of visual field loss. The second possible factor is improvement of compliance by DTFC. In general, patients take their medicines in compliance with the directions just before seeing their doctor, whereas some patients may stop using medications before the next outpatient visit. During the interval between visits to the doctor or after discharge from hospital, compliance with medication normally declines.28 Fixed combination drugs are expected to improve compliance because they are more convenient for patients, with less potential for abuse, lower costs, and fewer adverse effects.10,11 Patient education for a clinical trial may also improve compliance with DTFC.14 Improvement of compliance can have a major effect on the reduction of IOP,29 and a lower IOP reduces the risk for progressive visual field loss.30
A number of study limitations should be considered when interpreting these results. First, our study was not randomized, and there was no control group, because all patients with insufficient control of the IOP and progression of visual field defects were switched to DTFC. Second, our study was small in scale (14 patients), and selection bias may have occurred. Third, switching to a medication generally improves adherence to treatment,13 so DTFC might appear to be more efficient than it really was. Fourth, our patients received many different antiglaucoma medications before switching to DTFC. Fifth, the IOP was measured only in the morning. Konstas and Quaranta reported that daytime peak IOP is clinically important in predicting long-term glaucomatous progression.31,32 Timolol is effective during the daytime, and dorzolamide is effective at night.33 For that reason, DTFC and dorzolamide increase mean 24-hour diastolic ocular perfusion pressure with a substantial reduction in IOP.34 Therefore, we need to measure IOP in the morning and evening. Sixth, we did not measure central corneal thickness, although greater central corneal thickness is associated with higher IOP.35
In conclusion, this study provided the first information about the progression of visual field loss over the course of 3 years after switching to DTFC. It demonstrated that DTFC prevented the progression of visual field loss and was well tolerated for 36 months in patients switched from other glaucoma medications. As well as decreasing the number of doses and improving adherence, DTFC protects against visual field progression.
Acknowledgment
This work was supported in part by a Grant-in-Aid for Scientific Research from the Ministry of Education, Culture, Sports, Science and Technology of Japan, and a Health Labour Sciences Research Grant from The Ministry of Health Labour and Welfare of Japan.
Disclosure
The authors report no conflicts of interest in this work. The authors alone are responsible for the contents and for writing this paper.
References
Collaborative Normal-Tension Glaucoma Study Group. The effectiveness of intraocular pressure reduction in the treatment of normal-tension glaucoma. Am J Ophthalmol. 1998;126(4):498–505. | ||
The AGIS Investigators. The Advanced Glaucoma Intervention Study (AGIS): 7. The relationship between control of intraocular pressure and visual field deterioration. Am J Ophthalmol. 2000;130(4):429–440. | ||
Drance S, Anderson DR, Schulzer M; Collaborative Normal-Tension Glaucoma Study Group. Risk factors for progression of visual field abnormalities in normal-tension glaucoma. Am J Ophthalmol. 2001; 131(6):699–708. | ||
Kass MA, Heuer DK, Higginbotham EJ, et al. The Ocular Hypertension Treatment Study: a randomized trial determines that topical ocular hypotensive medication delays or prevents the onset of primary open-angle glaucoma. Arch Ophthalmol. 2002;120(6):701–713, discussion 829–830. | ||
AGIS Investigators. The Advanced Glaucoma Intervention Study (AGIS): 12. Baseline risk factors for sustained loss of visual field and visual acuity in patients with advanced glaucoma. Am J Ophthalmol. 2002;134(4):499–512. | ||
Leske MC, Heijl A, Hyman L, Bengtsson B, Dong L, Yang Z; EMGT Group. Predictors of long-term progression in the early manifest glaucoma trial. Ophthalmology. 2007;114(11):1965–1972. | ||
Gordon MO, Torri V, Miglior S, et al; European Glaucoma Prevention Study Group. Validated prediction model for the development of primary open-angle glaucoma in individuals with ocular hypertension. Ophthalmology. 2007;114(1):10–19. | ||
Leske MC, Heijl A, Hussein M, Bengtsson B, Hyman L, Komaroff E; Early Manifest Glaucoma Trial Group. Factors for glaucoma progression and the effect of treatment: the early manifest glaucoma trial. Arch Ophthalmol. 2003;121(1):48–56. | ||
Gordon MO, Beiser JA, Brandt JD, et al. The Ocular Hypertension Treatment Study: baseline factors that predict the onset of primary open-angle glaucoma. Arch Ophthalmol. 2002;120(6):714–720, discussion 829–830. | ||
European Glaucoma Society. Terminology and guidelines for glaucoma. 3rd ed. Savona, Italy: European Glaucoma Society; 2008. Available from: http://www.eugs.org/eng/EGS_guidelines.asp. Accessed August 15, 2014. | ||
Rossi GC, Pasinetti GM, Sandolo F, Bordin M, Bianchi PE. From dorzolamide 2%/timolol 0.5% to brinzolamide 1%/timolol 0.5% fixed combination: a 6-month, multicenter, open-label tolerability switch study. Expert Opin Pharmacother. 2011;12(16):2425–2431. | ||
Syed MF, Loucks EK. Update and optimal use of a brinzolamide-timolol fixed combination in open-angle glaucoma and ocular hypertension. Clin Ophthalmol. 2011;5:1291–1296. | ||
Konstas AG, Bányai L, Blask KD, et al. Intraocular pressure and safety in glaucoma patients switching to latanoprost/timolol maleate fixed combination from mono- and adjunctive therapies. J Ocul Pharmacol Ther. 2004;20(5):375–382. | ||
Sonty S, Henry JC, Sharpe ED, et al. Success rates for switching to dorzolamide/timolol fixed combination in timolol responders who are insufficiently controlled by latanoprost monotherapy. Acta Ophthalmol (Copenh). 2008;86(4):419–423. | ||
Mizoguchi T, Ozaki M, Wakiyama H, Ogino N. Additive intraocular pressure-lowering effect of dorzolamide 1%/timolol 0.5% fixed combination on prostaglandin monotherapy in patients with normal tension glaucoma. Clin Ophthalmol. 2011;5:1515–1520. | ||
Nixon DR, Yan DB, Chartrand JP, Piemontesi RL, Simonyi S, Hollander DA. Three-month, randomized, parallel-group comparison of brimonidine-timolol versus dorzolamide-timolol fixed-combination therapy. Curr Med Res Opin. 2009;25(7):1645–1653. | ||
Hommer A, Kimmich F. Switching patients from preserved prostaglandin-analog monotherapy to preservative-free tafluprost. Clin Ophthalmol. 2011;5:623–631. | ||
Leske MC, Heijl A, Hyman L, Bengtsson B. Early Manifest Glaucoma Trial: design and baseline data. Ophthalmology. 1999;106(11):2144–2153. | ||
Bengtsson B, Leske MC, Hyman L, Heijl A; Early Manifest Glaucoma Trial Group. Fluctuation of intraocular pressure and glaucoma progression in the early manifest glaucoma trial. Ophthalmology. 2007;114(2):205–209. | ||
Koseki N, Araie M, Yamagami J, Shirato S, Yamamoto S. Effects of oral brovincamine on visual field damage in patients with normal-tension glaucoma with low-normal intraocular pressure. J Glaucoma. 1999;8(2):117–123. | ||
Fukuchi T, Yoshino T, Sawada H, et al. The relationship between the mean deviation slope and follow-up intraocular pressure in open-angle glaucoma patients. J Glaucoma. 2013;22(9):689–697. | ||
Janulevicienë I, Harris A, Kagemann L, Siesky B, McCranor L. A comparison of the effects of dorzolamide/timolol fixed combination versus latanoprost on intraocular pressure and pulsatile ocular blood flow in primary open-angle glaucoma patients. Acta Ophthalmol Scand. 2004;82(6):730–737. | ||
Maren TH. Carbonic anhydrase: general perspectives and advances in glaucoma research. Drug Dev Res. 1987;10(4):255–276. | ||
Rassam SM, Patel V, Kohner EM. The effect of acetazolamide on the retinal circulation. Eye (Lond). 1993;7(Pt 5):697–702. | ||
Harris A, Arend O, Kagemann L, Garrett M, Chung HS, Martin B. Dorzolamide, visual function and ocular hemodynamics in normal-tension glaucoma. J Ocul Pharmacol Ther. 1999;15(3):189–197. | ||
Harris A, Jonescu-Cuypers CP, Kagemann L, et al. Effect of dorzolamide timolol combination versus timolol 0.5% on ocular bloodflow in patients with primary open-angle glaucoma. Am J Ophthalmol. 2001;132(4):490–495. | ||
Quaranta L, Miglior S, Floriani I, Pizzolante T, Konstas AG. Effects of the timolol-dorzolamide fixed combination and latanoprost on circadian diastolic ocular perfusion pressure in glaucoma. Invest Ophthalmol Vis Sci. 2008;49(10):4226–4231. | ||
Kruse W. Patient compliance with drug treatment – new perspectives on an old problem. Clin Investig. 1992;70(2):163–166. | ||
Nebbioso M, Evangelista M, Librando A, Di Blasio D, Pescosolido N. Fixed topical combinations in glaucomatous patients and ocular discomfort. Expert Opin Pharmacother. 2012;13(13):1829–1835. | ||
Pescosolido N, Parisi F, Russo P, Buomprisco G, Nebbioso M. Role of dopaminergic receptors in glaucomatous disease modulation. Biomed Res Int. 2013;2013:193048. | ||
Konstas AG, Quaranta L, Mikropoulos DG, et al. Peak intraocular pressure and glaucomatous progression in primary open-angle glaucoma. J Ocul Pharmacol Ther. 2012;28(1):26–32. | ||
Quaranta L, Katsanos A, Russo A, Riva I. 24-hour intraocular pressure and ocular perfusion pressure in glaucoma. Surv Ophthalmol. 2013; 58(1):26–41. | ||
Quaranta L, Gandolfo F, Turano R, et al. Effects of topical hypotensive drugs on circadian IOP, blood pressure, and calculated diastolic ocular perfusion pressure in patients with glaucoma. Invest Ophthalmol Vis Sci. 2006;47(7):2917–2923. | ||
Quaranta L, Miglior S, Floriani I, Pizzolante T, Konstas AG. Effects of the timolol-dorzolamide fixed combination and latanoprost on circadian diastolic ocular perfusion pressure in glaucoma. Invest Ophthalmol Vis Sci. 2008;49(10):4226–4231. | ||
Doughty MJ, Zaman ML. Human corneal thickness and its impact on intraocular pressure measures: a review and meta-analysis approach. Surv Ophthalmol. 2000;44(5):367–408. |
 © 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2014 The Author(s). This work is published and licensed by Dove Medical Press Limited. The
full terms of this license are available at https://www.dovepress.com/terms.php
and incorporate the Creative Commons Attribution
- Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted
without any further permission from Dove Medical Press Limited, provided the work is properly
attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.