Back to Journals » Clinical, Cosmetic and Investigational Dermatology » Volume 10
Effect of a lotion containing the heat-treated probiotic strain Lactobacillus johnsonii NCC 533 on Staphylococcus aureus colonization in atopic dermatitis
Authors Blanchet-Réthoré S, Bourdès V, Mercenier A, Haddar CH, Verhoeven PO , Andres P
Received 24 February 2017
Accepted for publication 13 April 2017
Published 3 July 2017 Volume 2017:10 Pages 249—257
DOI https://doi.org/10.2147/CCID.S135529
Checked for plagiarism Yes
Review by Single anonymous peer review
Peer reviewer comments 3
Editor who approved publication: Dr Jeffrey Weinberg
Sandrine Blanchet-Réthoré,1 Valérie Bourdès,1 Annick Mercenier,2 Cyrille H Haddar,3 Paul O Verhoeven,3 Philippe Andres4
1CUTIS (Clinical Unit for Tests and Imaging of Skin), Evaluation Department, Nestlé Skin Health/Galderma Research and Development, Sophia-Antipolis, France; ²Host Microbiome Interaction Group, Gut Ecosystem Department, Institute of Nutritional Science, Nestlé Research Center, Lausanne, Switzerland; 3Laboratory of Infectious Agents and Hygiene, University Hospital of Saint-Etienne and GIMAP (Mucosal Immunity and Pathogen Agents Group), Saint-Etienne, France; 4Medical Affairs Department, Galderma International, Paris, France
Objective: Staphylococcus aureus dominates the skin microbiota in patients with atopic dermatitis (AD), with bacterial loads correlating with disease severity. The aim of this exploratory study was to investigate the effect of a cosmetic lotion containing heat-treated Lactobacillus johnsonii NCC 533 (HT La1) on S. aureus colonization in AD patients.
Methods: This open-label, multicenter study was performed in AD patients in Germany. First, detection of S. aureus was performed in all patients using the swab or scrub-wash method of sampling, followed by quantitative culture or quantitative polymerase chain reaction. Repeatability and reproducibility of all method combinations were evaluated to select the best combination of sampling and quantification. Second, a lotion containing HT La1 was applied to lesional skin twice daily for 3 weeks. Scoring using local objective SCORing Atopic Dermatitis (SCORAD), measurement of S. aureus load, and lesional microbiome analysis were performed before and after the 3-week treatment period.
Results: Thirty-one patients with AD were included in the study. All sampling and quantification methods were found to be robust, reproducible, and repeatable for assessing S. aureus load. For simplicity, a combination of swab and quantitative polymerase chain reaction was chosen to assess the efficacy of HT La1. Following application of a lotion containing HT La1 to AD lesions for 3 weeks, a reduction in S. aureus load was observed in patients, which correlated with a decrease in local objective SCORAD. Interestingly, high baseline skin concentrations of S. aureus were associated with good responses to the lotion.
Conclusion: This study demonstrated that the application of a lotion containing HT La1 to the lesional skin of patients with AD for 3 weeks controlled S. aureus colonization and was associated with local clinical improvement (SCORAD). These findings support further development of topical treatments containing heat-treated nonreplicating beneficial bacteria for patients with AD.
Keywords: atopic dermatitis, S. aureus, heat treated La1, HT La1, L. johnsonii NCC 533, microbiology
Introduction
Atopic dermatitis (AD) is a chronic pruritic inflammatory skin disease that follows a relapsing course with recurrent eczematous lesions. The prevalence of AD has doubled or tripled in industrialized countries during the past three decades, with 15%–30% children and 2%–10% adults currently affected by this disease.1,2
It is well known that Staphylococcus aureus has a high prevalence on the skin of patients with AD,3 and that patients with AD are prone to S. aureus infection and skin colonization.3–6 Early studies have shown that 85% to 93% of lesional sites in patients with AD are colonized by S. aureus, with bacterial loads exceeding 104 colony forming units (CFU) per cm2 of skin. In addition, more recent studies have shown that S. aureus loads correlate with disease severity and that staphylococci represent 90% of the skin microbiota during untreated AD flares.7,8 However, in a recent meta-analysis of 95 selected observational studies, Totté et al concluded that patients with AD were more likely to be colonized with S. aureus on lesional skin than healthy controls but found high heterogeneity between studies in the prevalence and load of S. aureus colonization.9 Overall, these observations indicate that S. aureus might play a role in important aspects of AD pathogenesis and that strategies to decrease skin colonization by S. aureus in patients with AD would likely help to reduce the frequency and severity of flares.10
Lactobacillus johnsonii NCC 533 (hereunder designated as La1) is a member of the acidophilus group of intestinal lactobacilli that have been extensively studied for their “probiotic” properties that include pathogen inhibition, epithelial cell attachment, and immunomodulation.11 In vitro experiments on monolayer keratinocytes have shown that La1 can adhere to keratinocytes and impair S. aureus attachment to these cells and was one of the most effective among different Lactobacillus, Micrococcus, and Bifidobacterium strains (NRC patent, WO01/45721 A1). Interestingly, when inactivated by heat treatment, L. johnsonii La1 (HT La1) maintains its capacity to reduce S. aureus attachment on keratinocytes and its in vitro immune profile (Nestlé Research Center data). HT La1 displayed a concentration-dependent inhibitory effect on S. aureus adhesion and concentration of 0.3% (0.93×109 CFU/mL), which led to a 54% decrease in S. aureus adhesion, was selected for the clinical evaluation in this study. Additionally, our studies (Rosignoli et al, submitted) have shown that HT La1 can increase the gene expression and protein synthesis of certain antimicrobial peptides, including β-defensin 2, which is known to be altered in AD and to be a very important component of innate immunity.12 All these observations suggest that a topical formulation containing HT La1 may reduce S. aureus colonization in AD patients.
Swab sampling to determine skin S. aureus load is widely used. However, the scrub wash method described in 1965 by Kligman is unique to cutaneous sampling and may provide a more robust and sensitive technique to recover bacteria.13 Determination of skin S. aureus load by quantitative culture on a chromogenic medium is the gold standard. However, it is time consuming (24–48 h of bacterial growth), labor intensive, and requires fresh samples. Identification of S. aureus by quantitative (real time) polymerase chain reaction (qPCR) has already demonstrated excellent specificity and sensitivity for detecting S. aureus in nasal specimens 14 and is easier to implement in a clinical study as it can be performed on frozen samples.
Therefore, this study aims to first compare the robustness and reproducibility of two sampling methods of skin microbiota: swab and scrub wash, as well as to evaluate bacteria quantification methods using culture and qPCR. In the second part of this study, the effect of a topical lotion containing HT La1 on S. aureus colonization and its clinical efficacy in AD was assessed.
Materials and methods
Study design
This was an open label exploratory study in patients with AD conducted at three centers in Germany. The study consisted of two parts: 1) an assessment of S. aureus sampling and quantification methods and 2) evaluation of a cosmetic lotion containing a heat-treated probiotic. The first part of the study included all enrolled patients (Population 1, N=31) whereas the second part of the study included only those patients who were found to be carriers of S. aureus at the start of the study and presented with clinically visible lesions on Day 8 (Population 2, N=21). Both parts of the study are described in detail below. This study was carried out in accordance with the Declaration of Helsinki and in agreement with the ethical guidelines of the European Independent Ethics Committee. The protocol was submitted and approved by ethics committee of La Charité center (number EA1 7121/15) and the Freiburger ethik-kommision international (number 015/1154). All patients gave written informed consent to participate in this study.
Study population
Male and female patients aged 18–75 years diagnosed with AD of mild-to-moderate severity at baseline (Investigator’s Global Assessment scores of 2 or 3) who exhibited at least one AD lesion of >20 cm2 were eligible for inclusion in the study.15 The location of AD lesions had to allow sampling with the scrub wash method.
For the purposes of this study, lesional skin was defined as an active lesion of AD: an erythematous plaque with or without oozing, vesiculation, crusting, excoriations, or erosions but with no overt signs of infection, located within the antecubital or popliteal fossae, or other region typical of AD.
Exclusion criteria included severe fungal infection or other skin disease that could affect AD diagnosis, any uncontrolled or serious disease, or any condition that could interfere with data interpretation or put the patient at significant risk. Patients who did not respect the appropriate wash-out periods for topical and systemic steroids, topical and systemic antibiotics, and topical antiseptics–the use of which was prohibited during the study–before baseline (Day 1) were also excluded.
Evaluation of sampling and quantification methods
In the first part of the study, enrolled patients were assigned to one of the two groups to compare the swab (Group 1) and scrub wash (Group 2) sampling methods from a 3 cm diameter O-ring area of an AD lesion. At baseline, two swabs (first and second sampling) were taken from adjacent areas on one representative lesion (target lesion) of Group 1 patients (Figure 1) to assess repeatability. Similar scrub wash samplings were performed in patients assigned to Group 2. At Days 3 and 8 (before treatment), target lesions were sampled with both the swab and scrub wash methods from adjacent areas of the target lesion to evaluate the reproducibility of the methods.
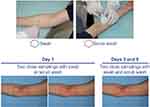  | Figure 1 Swab and scrub wash sampling techniques. |
The patients were instructed to avoid bathing for 24 h prior to all sampling time points and avoid showers and emollient on the day of the visit.
Swab sampling was carried out using a nylon flocked swab (eSwab 480CE [COPAN ITALIA spa, Brescia, Italy]) dipped in normal saline solution, in a 3 cm diameter O-ring. Skin microbiota was recovered in 1 mL Amies solution (COPAN ITALIA spa, Brescia, Italy). Scrub wash sampling was also performed using a 3 cm diameter O-ring. Briefly, 3 mL of buffer was added inside the O-ring then skin was scrubbed with a flat-ended rod and wash fluid was collected for S. aureus quantification. Both methods of sampling were performed by the study investigator or designee and samples were sent within 24 h at 4°C to an independent center (CHU, Saint-Etienne, France) for S. aureus quantification using both qPCR and quantitative plate culture. For qPCR, the Cepheid® Xpert SA Nasal Complete Assay was used with the GeneXpert® System (Cepheid, Maurens-Scopont, France). Quantitative plate culture was performed on selective chromogenic medium (BBL CHROMagar Staph aureus [Becton Dickinson, Le Pont de Claix, France]) using the EasySpiral dilute instrument (Interscience, Saint-Nom-la-Bretèche, France).
Clinical evaluation of HT La1 lotion
Strain La1 is a proprietary strain of the Nestlé Culture Collection. HT La1 was supplied to Galderma R&D in spray dried powder form, with an initial concentration of 3.1×1011 equivalent CFU/g (Nestlé PTC, Konolfingen, Switzerland).
For clinical assessment, a lotion (COS daily moisturizing lotion) containing HT La1 at 0.3% (w/w): designated as HT La1 lotion, was developed by Galderma R&D under good manufacturing practice conditions and was supplied to eligible participants. The lotion consisted of oil-in-water emulsion with oil phase being mainly composed of sunflower seed oil, caprylic/capric triglyceride, Butyrospermum parkii and the water phase of glycerin and xanthan gum. The complete composition is available in the pending patent PCT/EP2016/074065 (example 2).
On Day 8, patients included in the assessment of HT La1 lotion (i.e., S. aureus carriers on the target lesion identified at baseline and target lesion still present at the beginning of the treatment) were asked to apply HT La1 lotion on the target lesion in place of their usual moisturizer twice daily for 21(±1) days, leaving at least 6 h between applications. The contralateral lesion (if available) was either untreated or treated with the patient’s usual moisturizer.
For bacterial quantification, samples from target and contralateral lesions (if available) at Days 8 and 28 were analyzed using a combination of swab and qPCR. Samples were also collected from patients using the swab method on the target lesion at Days 8 and 28 and frozen at −20°C prior to analysis of microbiota profile by GenoScreen (Lille, France). Bacteria were identified at the genus level using 16S rRNA gene sequencing of the hypervariable regions V3–V4 with 454 sequencing technology on a GS FLX+ system (Roche, Basel, Switzerland). The efficacy of HT La1 lotion on disease severity was evaluated by local objective SCORing Atopic Dermatitis (SCORAD) on Days 8 and 28, which included assessment of erythema, edema, or papulation, oozing or crusting, excoriation, lichenification, and dryness of the treated lesion.16,17
Tolerability
Cutaneous tolerability of the sampling method (Population 1, N=31) and HT La1 lotion application (Population 2, N=21) was evaluated at each visit based on signs of erythema, induration or papulation, oozing or crusting, excoriation, lichenification, and pruritus in the target lesion or contralateral lesion (where available). All signs were classified according to intensity (0=none, 1=mild, 2=moderate, and 3=severe).
Statistical analysis
A sample size of 15 patients was deemed sufficient for this study. However, with an expected S. aureus carriage rate of 50% in AD patients, at least 30 patients needed to be included at Day 1 (where S. aureus carriage was determined) to ensure sufficient patients for HT La1 lotion assessment.
For the methodology part, all patients enrolled in the study from baseline to Day 8 (before treatment) (Population 1, N=31), were included in the corresponding statistical analyses. For HT La1 lotion assessment, patients from Population 2 (N=21) only (i.e., with S. aureus colonization at baseline) were included in statistical analyses.
The safety population included all patients who were included in the study.
Patient disposition, baseline characteristics, previous and concomitant therapies were summarized by descriptive statistics.
Pearson’s coefficient of correlation was calculated for comparison of quantification methods (qPCR vs culture) and sampling methods (scrub wash vs swab).
Differences in S. aureus load between Days 8 and 28 were tested using Wilcoxon signed rank test. A p-value of <0.05 was used to indicate significance. Statistical analysis on local objective SCORAD assessment was performed using the paired t-test.
Results
Baseline demographics and disease characteristics of all enrolled patients
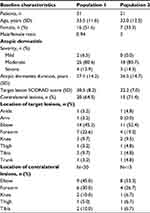
A total of 31 patients were enrolled and participated in the first part of the study (Population 1). The mean age of patients was 33.5±11.6 years and both genders were equally represented as 16 (51.6% of patients were females [Table 1]). The majority of patients (80.6%) had AD of moderate severity, with a mean target lesion local objective SCORAD of 30.5±8.2 and mean disease duration of 27.1±14.2 years. Target lesions were mostly located on the elbow (in 14 [45.2%] patients) and forearm (in 7 [22.6%] patients). Twenty patients (64.5%) presented with contralateral lesions. Similar to the target lesions, the majority of contralateral lesions were located on the elbow (in 9 [45%] patients) and the forearm (in 6 [30%]).
A total of 21 patients who were S. aureus-positive at baseline (for one sample, whatever the quantification method) and still presented clinically visible AD lesions on Day 8 were eligible for treatment and included in the second part of the study (Population 2). Baseline characteristics were similar between the two populations and no statistically significant difference was found between them, except that there was a majority (66.7%) of male patients in Population 2 (Table 1). All patients completed the study.
Evaluation of sampling and quantification methods
At baseline, skin samples (first and second sampling) were collected from the target lesion using the swab or scrub wash methods from a standardized surface (3 cm diameter O-ring area). Presence and levels of S. aureus on the target lesion at baseline are presented in Table 2.
More than 50% of the patients in Groups 1 and 2 of Population 1 were S. aureus carriers on the target lesion at Day 1 with mean bacterial loads ranging from 1.42 to 2.31 Log10 CFU/cm2, depending on the combination of sampling and quantification methods used (Table 2). The two methods of quantification yielded comparable S. aureus counts. A good correlation between qPCR and culture (Pearson’s correlation coefficient approaching 1 [0.92, p<0.001]) was observed despite a slightly higher bacterial load generally detected following culture compared with qPCR. Overall, no major differences were noted in terms of S. aureus concentrations between swab and scrub wash sampling, although there was less variability using the scrub wash method as shown by the smaller standard deviations.
A good correlation was also found between first and second samples taken from AD lesions of patients at Baseline using both sampling methods (swab or scrub wash) and both quantification methods (culture or qPCR), indicating good repeatability of the methods (Pearson’s correlation coefficient ≥0.83 [p<0.0001]; Figure 2). In the same way, analysis of the variance of S. aureus counts (CFU/cm2) at Days 1, 3, and 8 (before treatment) showed that there was no time effect for swab (p=0.340) and scrub wash (p=0.532) in S. aureus-positive patients, suggesting that both sampling methods were reproducible.
Since swab and scrub wash were performed in 2 groups of patients at Day 1 (Figure 1), the direct comparison of the two methods was performed on Day 3. Using scrub wash, the mean S. aureus load (2.08 Log10 CFU/cm2±1.70 for qPCR and 2.21 Log10 CFU/cm2±1.80 for culture) was slightly but significantly higher when compared with swab whatever the quantification method (1.83 Log10 CFU/cm2±1.77 for qPCR and 1.47 Log10 CFU/ cm2±1.66 for culture). Though, the Pearson’s coefficient of correlation was equal to 0.77 (p<0.0001), indicating that the two methods are strongly correlated.
In summary, we observed that qPCR and culture were very well correlated and not statistically different; likewise, the sampling methods (swab and scrub wash) were strongly correlated and all 4 couples of methods displayed a good repeatability and reproducibility. Since all methods of sampling and quantification were robust and reliable, the combination of swab and qPCR was selected to test the efficacy of the lotion containing the HT La1 as these techniques are easier to use.
Clinical evaluation of HT La1
COS daily moisturizing lotion containing 0.3% HT La1 was applied twice daily on the target lesions for 21±1 days. Following 3-week application, the lotion was found to control S. aureus load of the treated target lesions compared with contralateral lesions not treated with HT La1 lotion (−1 Log10 CFU/cm2, p<0.05). Indeed, in the 15 patients having a contralateral lesion, median S. aureus counts remained stable in the treated AD lesions (1.53 Log10 CFU/cm2 on Day 8 to 1.36 Log10 CFU/cm2 on Day 28, p<0.001) compared with contralateral lesions not treated with HT La1 lotion (1.9 Log10 CFU/ cm2 on Day 8 to 3.3 Log10 CFU/cm2 on Day 28) where an increase was observed (Figure 3). Using a logistic model to assess the role of S. aureus concentration at Day 8 in patient responsiveness to HT La1 lotion at Day 28, high S. aureus skin load at the time of lotion application was found to be a predictive factor of the microbiological response (point estimate: 3.117; Chi-square test: p<0.05). In those patients for whom S. aureus levels decreased in response to HT La1 lotion, the minimum S. aureus concentration at Day 8 was 2.89 Log10 CFU/cm2.
The 16S rRNA gene sequencing-based analysis of microbiota composition and diversity was performed on samples from the target lesions of 15 patients at Days 8 and 28. Considering the most common skin phyla (Actinobacteria, Firmicutes, Proteobacteria, and Bacteroidetes), the Firmicutes phylum was the only one significantly modified by the treatment. A noticeable reduction in the proportion of the Staphylococcaceae family was observed between Days 8 and 28 in AD lesions treated with HT La1 lotion (Figure 4) and was almost the only phyla modified. Also, a slight reduction of the Shannon diversity index was observed between Days 8 and 28, which was not statistically significant (data not shown).
  | Figure 4 Change in skin microbiota composition between Days 8 and 28 in target atopic dermatitis lesions treated with heat-treated Lactobacillus johnsonii lotion. |
Regarding the disease severity of the target lesion, the use of HT La1 lotion for 3 weeks led to a statistically significant decrease in mean SCORAD values of 4.93±8.23 between Days 8 (31.2±9.2) and 28 (26.2±7.9) (p=0.012; Figure 5).
Tolerability
When applied to the lesional skin of patients with AD, HT La1 lotion was found to be well tolerated.
Discussion
Several clinical studies have demonstrated that patients with AD are more likely to be colonized with S. aureus on lesional skin than healthy controls, although the prevalence of S. aureus colonization varies among studies.9 These variations are likely to be due to differences in the studied populations (e.g., age, ethnicity, disease severity), the control populations and in the sampling methods. Furthermore, patients with AD have higher S. aureus titers on their skin than healthy controls, with mean titers of around 104 CFU/cm2 on lesional skin that can reach up to 107 CFU/cm2 in the acute phase, and a correlation between S. aureus titers and disease severity has been reported in some studies.7,18,19 Moreover, the skin microbiota in AD is dominated by S. aureus, especially during flares.7
These findings support a role for S. aureus in the pathogenesis of AD, although the precise mechanism of its involvement remains to be determined. They nevertheless suggest that a reduction in S. aureus may improve the symptoms of AD.9,10
Previously, there have been many interventional trials aiming to decrease S. aureus in patients with atopic eczema. A Cochrane review evaluating these studies failed to find clear evidence that commonly used anti-S. aureus interventions are clinically beneficial.20,21 However, the studies included in the review were small and poorly reported, S. aureus load decrease was not documented in most studies and tested therapies (oral antibiotics, topical antibiotics, or antiseptics in combination with corticosteroids, bleach baths, and antibacterial bars) did not specifically target S. aureus.
In order to assess the efficacy of novel therapies that function by reducing S. aureus load on the skin of patients with AD, a reliable method for sampling and quantifying S. aureus is required. The swab and scrub wash methods of sampling have previously been shown to provide comparable recovery of bacterial species from the skin surface.22 This study showed that the swab and scrub wash methods of skin sampling are both robust, reproducible and repeatable methods of assessing the S. aureus load in patients with AD when coupled with either quantitative culture or qPCR. Since we found no major difference between the sampling and quantification methods for simplicity and speed, we elected to assess the effect of a lotion containing a nonreplicating probiotic strain on S. aureus levels using the combination of swab and qPCR.
The effect of probiotics on skin health is an interesting field of development and, although such studies generally make use of oral probiotics, there is increasing focus on the potential use of topical probiotics to modulate the cutaneous microbiota.23 In this study, we evaluated a lotion (COS daily moisturizing lotion) containing 0.3% La1 inactivated by heat treatment (HT La1 lotion) in patients with AD. Results demonstrated that after 3 weeks of twice daily application to target AD lesions, HT La1 lotion significantly lowered S. aureus loads compared with contralateral lesions that were untreated or treated with the patient’s usual moisturizer (p<0.001). This result is consistent with the antagonistic properties of HT La1 found in studies investigating the attachment of S. aureus to keratinocytes using the reconstructed human epidermis model (Nestlé patent, WO01/45721 and internal data [Rosignoli et al, unpublished data, 2017]).
Additionally, a noticeable reduction was found in the Staphylococcaceae family abundance on treated AD lesions between Days 8 and 28 using 16S rRNA gene sequencing for microbiota profiling. Actinobacteria, Firmicutes, Bacteroidetes, and Proteobacteria are the four dominant phyla of skin bacteria.24 Treatment with the HT La1 containing lotion mainly affected the Firmicutes phylum and, more precisely, the Staphylococcaceae family. This highlights the specificity of action of the HT La1 lotion when compared with antibiotics or bleach bath.
Interestingly, the control of S. aureus colonization was associated with clinical statistically significant improvement of the treated AD lesions (using local objective SCORAD). Of note, patients who “responded” best to treatment were those with higher S. aureus counts at the time the lotion was first applied (Day 8). Indeed, a level of 2.89 Log10 CFU/cm2 in the AD target lesion appeared to be the minimum S. aureus load required to observe a response to HT La1 lotion, suggesting that this lotion may be useful for patients with particularly high levels of S. aureus colonization. Incidentally, in a recent systematic review, the prevalence of S. aureus colonization was found to increase with disease severity.9 Although we still need to elucidate the mechanism underlying this effect of the HT La1 lotion, another study has shown that the Lactobacillus reuteri ATCC 55730 strain can compete with S. aureus for α5β1 integrin binding sites on the keratinocyte cell surface.25 However, this effect was only observed with viable L. reuteri cells. In this study, we have shown that a lotion containing heat-treated HT La1 can reduce S. aureus load in AD lesions and improve the severity of disease. Whether, HT La1 lotion improves AD by solely reducing the S. aureus load or by combining different modes of action (i.e., enhancement of the production of certain anti-microbial peptides) needs to be further investigated.
In our study, the in vivo effects on S. aureus were observed with a heat-treated nonreplicating probiotic strain, which is particularly encouraging and would support the development of a more user-friendly product that is easier to store and can be delivered in a standardized dose.
Although interpretation of the results presented in this study is limited by the small number of patients who were treated with HT La1 lotion, the limited study duration, effective control of S. aureus loads, and the associated improvement in local objective SCORAD warrant further investigation of topical treatments containing heat-inactivated beneficial bacteria.
Conclusion
The results of this study show that the HT La1 lotion is well tolerated and induces a clinical improvement of AD lesions in association with a control of SA colonization.
Acknowledgments
The authors thank Dr S Sres, PTC Konolfingen, Nestlé, Switzerland for the preparation of the HT La1 spray dried powder, Alexandra Lamquin, Nestlé Skin Health/Galderma R&D for the management of the study, Dr Anne Carricajo, University Hospital of Saint-Etienne, for her valuable advice regarding microbiology, and Anne Lebecq, Stateo, Monaco for the statistical analysis. Medical writing assistance was provided by Dr Kathryn Hall of Scinopsis Medical Writing, France. This research was funded by Galderma R&D (CUTIS), Sophia Antipolis, France. Nestlé (PTC Konolfingen) provided the optimized batches of processed and heat-treated La1 powder. The work included in this manuscript was presented at the SID 75th Annual Meeting, Scottsdale, AZ, USA, 2016 (poster only).
Disclosure
SB-R and VB are employees of Galderma R&D. PA is a former employee of Galderma R&D. AM is an employee of the Nestlé Research Center, Nestec Ltd. The authors report no other conflicts of interest in this work.
References
Weidinger S, Novak N. Atopic dermatitis. Lancet. 2016;387(10023):1109–1122. | ||
Bieber T. Atopic dermatitis. N Engl J Med. 2008;358(14):1483–1494. | ||
Leyden JJ, Marples RR, Kligman AM. Staphylococcus aureus in the lesions of atopic dermatitis. Br J Dermatol. 1974;90(5):525–530. | ||
Gloor M, Peters G, Stoika D. On the resident aerobic bacterial skin flora in unaffected skin of patients with atopic dermatitis and in healthy controls. Dermatologica. 1982;164(4):258–265. | ||
Higaki S, Morohashi M, Yamagishi T, Hasegawa Y. Comparative study of staphylococci from the skin of atopic dermatitis patients and from healthy subjects. Int J Dermatol. 1999;38(4):265–269. | ||
Goh CL, Wong JS, Giam YC. Skin colonization of Staphylococcus aureus in atopic dermatitis patients seen at the National Skin Centre, Singapore. Int J Dermatol. 1997;36(9):653–657. | ||
Kong HH, Oh J, Deming C, et al. Temporal shifts in the skin microbiome associated with disease flares and treatment in children with atopic dermatitis. Genome Res. 2012;22(5):850–859. | ||
Brussow H. Turning the inside out: the microbiology of atopic dermatitis. Environ Microbiol. 2016;18(7):2089–2102. | ||
Totte JE, van der Feltz WT, Hennekam M, van Belkum A, van Zuuren EJ, Pasmans SG. Prevalence and odds of Staphylococcus aureus carriage in atopic dermatitis: a systematic review and meta-analysis. Br J Dermatol. 2016;175(4):687–695. | ||
Nakamura Y, Oscherwitz J, Cease KB, et al. Staphylococcus delta-toxin induces allergic skin disease by activating mast cells. Nature. 2013;503(7476):397–401. | ||
Pridmore RD, Berger B, Desiere F, et al. The genome sequence of the probiotic intestinal bacterium Lactobacillus johnsonii NCC 533. Proc Natl Acad Sci U S A. 2004;101(8):2512–2517. | ||
Harder J, Dressel S, Wittersheim M, et al. Enhanced expression and secretion of antimicrobial peptides in atopic dermatitis and after superficial skin injury. J Invest Dermatol. 2010;130(5):1355–1364. | ||
Williamson P, Kligman AM. A new method for the quantitative investigation of cutaneous bacteria. J Invest Dermatol. 1965;45(6):498–503. | ||
Verhoeven P, Grattard F, Carricajo A, Pozzetto B, Berthelot P. Better detection of Staphylococcus aureus nasal carriage by use of nylon flocked swabs. J Clin Microbiol. 2010;48(11):4242–4244. | ||
Hanifin JMR, G. Diagnostic features of atopic dermatitis. Acta Derm Vener Suppl (Stockh). 1980;92:44–47. | ||
Severity scoring of atopic dermatitis: the SCORAD index. Consensus Report of the European Task Force on Atopic Dermatitis. Dermatology. 1993;186(1):23–31. | ||
Kunz B, Oranje AP, Labreze L, Stalder JF, Ring J, Taïeb A. Clinical validation and guidelines for the SCORAD index: consensus report of the European Task Force on Atopic Dermatitis. Dermatology. 1997; 195(1):10–19. | ||
Tauber M, Balica S, Hsu CY, et al. Staphylococcus aureus density on lesional and nonlesional skin is strongly associated with disease severity in atopic dermatitis. J Allergy Clin Immunol. 2016;137(4):1272–1274. e1271–e1273. | ||
Lipnharski C, d’Azevedo PA, Quinto VP, Bessa G, Bonamigo RR. Colonization by S. aureus increases the EASI and the number of appointments by patients with atopic dermatitis: cohort with 93 patients. An Bras Dermatol. 2013;88(4):518–521. | ||
Birnie AJ, Bath-Hextall FJ, Ravenscroft JC, Williams HC. Interventions to reduce Staphylococcus aureus in the management of atopic eczema. Cochrane Database Syst Rev. 2008;16(3):CD003871. | ||
Bath-Hextall FJ, Birnie AJ, Ravenscroft JC, Williams HC. Interventions to reduce Staphylococcus aureus in the management of atopic eczema: an updated Cochrane review. Br J Dermatol. 2010;163(1):12–26. | ||
Keyworth N, Millar MR, Holland KT. Swab-wash method for quantitation of cutaneous microflora. J Clin Microbiol. 1990;28(5):941–943. | ||
Al-Ghazzewi FH, Tester RF. Impact of prebiotics and probiotics on skin health. Benef Microbes. 2014;5(2):99–107. | ||
Grice EA, Segre JA. The skin microbiome. Nat Rev Microbiol. 2011; 9(4):244–253. | ||
Prince T, McBain AJ, O’Neill CA. Lactobacillus reuteri protects epidermal keratinocytes from Staphylococcus aureus-induced cell death by competitive exclusion. Appl Environ Microbiol. 2012;78(15):5119–5126. |
 © 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.
© 2017 The Author(s). This work is published and licensed by Dove Medical Press Limited. The full terms of this license are available at https://www.dovepress.com/terms.php and incorporate the Creative Commons Attribution - Non Commercial (unported, v3.0) License.
By accessing the work you hereby accept the Terms. Non-commercial uses of the work are permitted without any further permission from Dove Medical Press Limited, provided the work is properly attributed. For permission for commercial use of this work, please see paragraphs 4.2 and 5 of our Terms.





